Abstract
We present a case of a 53-year-old female patient who was treated with 5-Fluorouracil (5-FU) after postsurgical contracture. A review of the literature regarding the use of 5-FU injections as a minimally invasive way to treat contracture was performed. We describe that the use of 5-FU injections is the preferred method for the effective treatment of contracture with minimal risk to the patient.
Introduction
5-Fluorouracil (5-FU) is a common chemotherapeutic agent that is used in many malignancies, as well as skin conditions. This medication is currently used in a variety of chemotherapy regimens and the reversal of recalcitrant hypertrophic and keloid dermatological issues. 1 Topical and injectable forms of 5-FU are additionally utilized in the treatment of skin contracture because of the ability to reduce the fibroblast and myofibroblast differentiation. 2 We now report a case of an individual who was treated with 5-FU for significant deep neck contracture due to postsurgical inflammation.
Case Presentation
A 53-year-old female patient had comprehensive facial surgery including forehead plasty with a brow lift, upper and lower blepharoplasty with fat repositioning, canthopexies, upper lip lift, corner lip lift, face-lift, neck lift, and CO2 laser resurfacing of the periocular and perioral regions. On day 7, the patient developed rapid swelling of the central neck extending from the cervical mental angle inferiorly. The area was red and bulging with a large collection that developed over the course of one night (Figure 1).
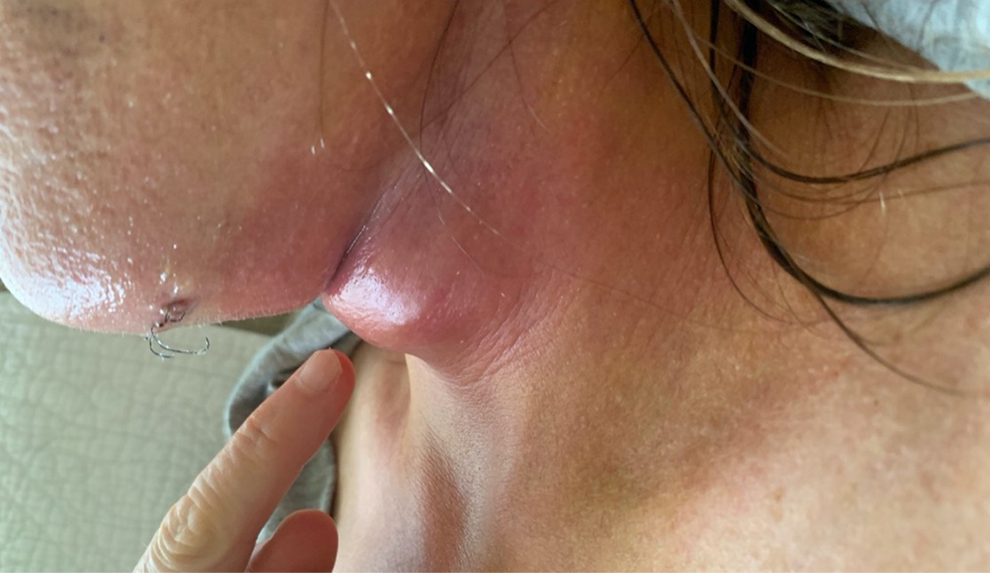
Abscess with erythema located at the cervical angle.
To treat the infection in the neck, 10mL of purulent fluid was drained from the cervical mental angle and irrigated with Dakin’s solution (sodium hypochlorite mixed with betadine) and vancomycin. The purulent fluid was cultured and the patient was given clindamycin and cefalexin to reduce the progression of the infection and prevent recurrent methicillin-resistant Staphylococcus aureus infection that she has experienced with a past surgery. The patient’s cultures came back positive for Klebsiella pneumoniae and Serratia marcescens. The patient was given levofloxacin and then cefdinir 3 times a week. Accordingly, the patient was advised at that time that she could develop a post-inflammatory course of contracture. On postoperative week 3, the skin of the cervical mental angle began to pull inferiorly. On postoperative week 5, there was no infection present, but the patient exhibited significant contracture with the inability to extend the neck normally (Figure 2).
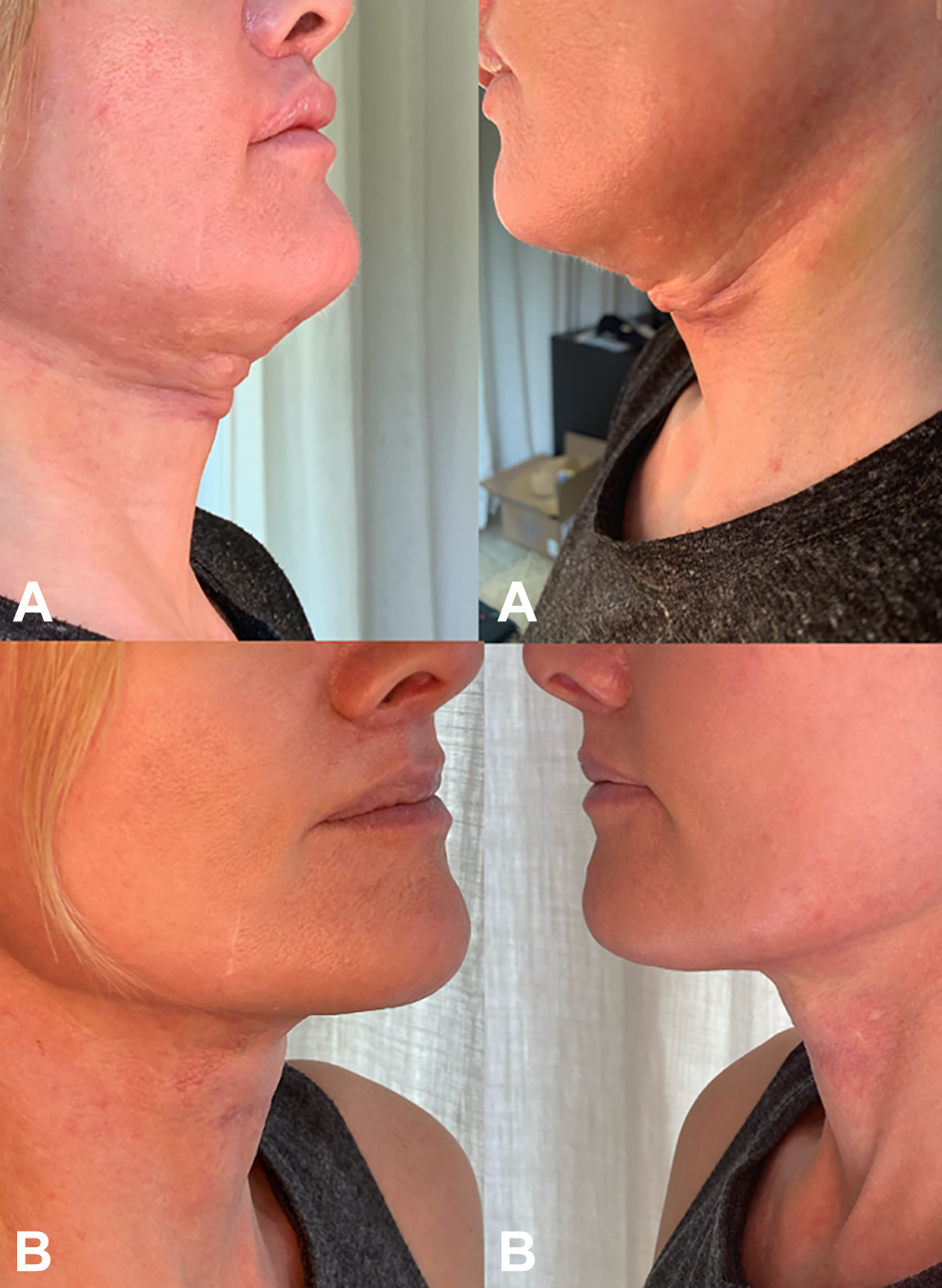
A, One-month postop induration with contracture of dermis and platysma. B, Nine-month postop following immune modulation injections of 5-Fluorouracil (5-FU).
Injections of 5-FU were recommended because they work well with deep contracture and seromas with little risk to the patient. The patient was injected with 25 mg (50mg/mL) of 5-FU combined with 0.5cc of 1% plain lidocaine, 2 to 3 weeks apart, up to 5 times, until resolution. The lidocaine is added as a dilutent and buffer, using the HCl in the lidocaine solution to lower the pH of 5-FU. Injections are placed into the indurated areas of the subdermis, platysma, and subplatysmal space using a 1mL syringe and 31 G needle. Dermal nd epidermal injections are only used for hypertrophic scarring and may cause skin irritation in various forms. Likewise, the patient was advised that triamcinolone acetonide (TACA) injection can be used for treatment, but there can be thinning of the skin with permanent banding in the neck due to the superficial nature of the platysma and sensitive nature of the dermis in the neck After the treatment discussion, the patient opted for 5-FU treatment.
Currently, the patient has a near resolution of the neck contracture after the treatment with 5-FU and may be followed up with a radiofrequency treatment to tighten the skin back to normal.
Discussion
Contractures of the dermis, subdermis and facial muscles can occur after procedures as a result of the thickening, tightening, and scarring of the skin cells in the region. This condition can present with functional difficulties through the formation of tight banding that can obstruct movement in the areas of the skin. There are multiple ways to treat a post-inflammatory course of contracture, but 5-FU treatment has been shown to have minimal risk to the patients. Potential side effects of 5-FU injections can include hyperpigmentation, pain, and ulcerations in the region. 1 In comparison to the other contracture therapies, such as radiotherapy and surgical interventions, 5-FU injections require less training, are easily stored, are lower in cost, and are practical treatments for at-risk individuals. 3 A study by Uppal et al displayed that treatment of scar excisions with 5-FU presented with significantly lower scar formation when compared with the control phosphate-buffered saline treatment. 4 Moreover, the studies done by Jemec et al using 5-FU as a topical treatment for Dupuytren’s contracture and nondiseased fascia revealed that the medication was able to inhibit the proliferation of fibroblast cultures and reduce high cell densities in the skin. 5 According to Ketchum and Donahue, the use of Kenalog (TACA) alone for treatment of contracture resulted in a resolution of 60% to 80%, but half of those patients experienced reactivation of contracture after their last injection. 6 Additionally, a study done by Khan et al treated 150 patients with 5-FU and Kenalog (TACA) showing fewer local side effects and better results than using corticosteroids alone. 7
Footnotes
Authors’ Note
This manuscript is original and has not been submitted elsewhere in part or in whole.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
