Abstract
Auricular perichondritis is a severe bacterial inflammation of the cartilaginous part of the external ear sparing the lobule and the tragus. Prompt diagnosis and treatment are necessary to avoid necrosis of the underlying cartilage and permanent auricular deformity. Management includes antibiotics and nonsteroidal anti-inflammatory drugs. Surgery to control the inflammation is sometimes necessary. Wide cartilage and subcutaneous tissue debridement with preservation of the helical rim to minimize the resulting auricular deformity is necessary.
Case Description
An 85-year-old male presented to our emergency department with a red, swollen, and tender left pinna for the last 3 weeks (Figure 1). No history of penetrating or blunt trauma was reported. The patient was on oral antibiotic therapy (quinolone) for one week without significant improvement. His past medical history included hypertension, insulin-dependent diabetes mellitus, and a stroke. On physical examination, severe inflammation and abscess of the pinna sparing the lobule were noted, and a clinical diagnosis of auricular perichondritis was made. Laboratory tests showed serum glucose levels at 160 mg/dL with normal white blood cells 8.03 K/µL and an elevated erythrocyte sedimentation rate 25.12 mm. He underwent incision and drainage of the abscess and pus was sent to microbiology. The presence of Staphylococcus epidermidis was confirmed. Intravenous antibiotic therapy with ceftaroline fosamil and quinolone was initiated for 7 days. He was discharged with improvement and he continued treatment with oral antibiotics for a further week. Three weeks later, even though serum glucose was well controlled, inflammation recurred and appeared resistant to long-term intravenous antibiotic therapy. An immunological cause such as relapsing perichondritis (first episode) was suspected but antinuclear antibodies and rheumatoid factor were negative, and immunologists did not recommend further investigations. After discussion with the patient, surgical resection of the antihelical and scaphoid cartilage with the overlying subcutaneous tissue was delivered (Figure 2). The wound was packed externally with antibiotic-impregnated ribbon gauze and a Penrose drain was inserted. Two weeks later, an additional minimal resection near the root of the helix was successful in containing the inflammation and alleviating the patient’s symptoms. The helical cartilage appeared normal and was preserved to minimize the auricular deformity. The pathological examination of the specimen confirmed chronic extensive necrosis of the cartilage and subcutaneous tissue and ruled out lymphocytic infiltration, a feature of lymphoproliferative or Kimura disease. The patient is well at the 6-month follow-up. Minimal deformity of the pinna is noted (Figure 3).
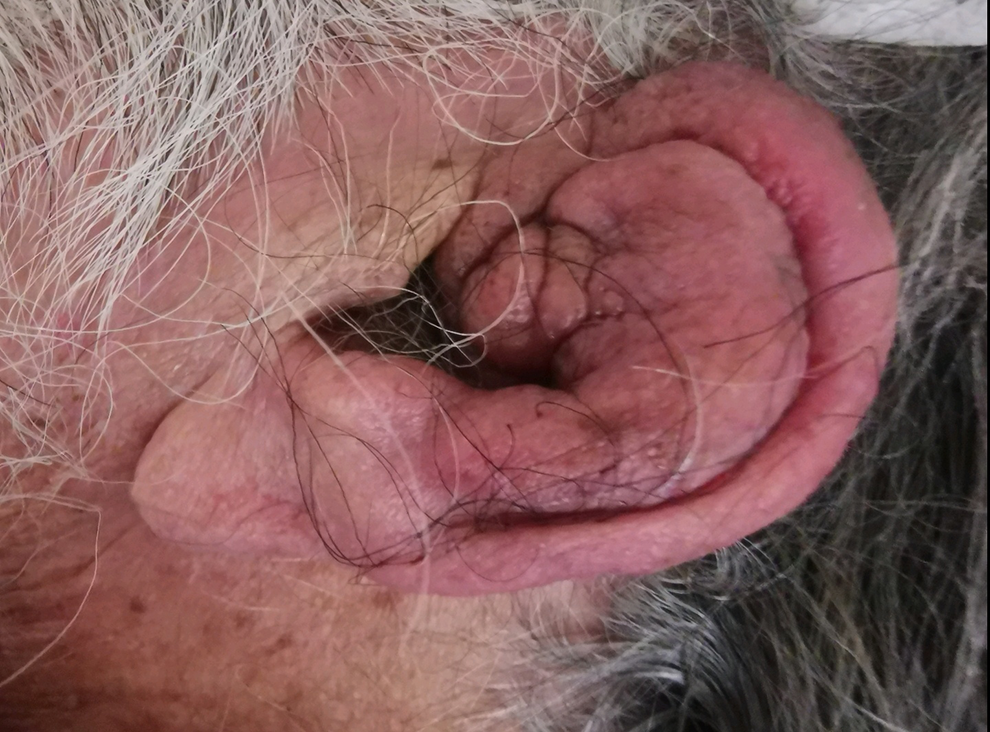
Preoperative acute perichondritis with extensive inflammation of the auricle.
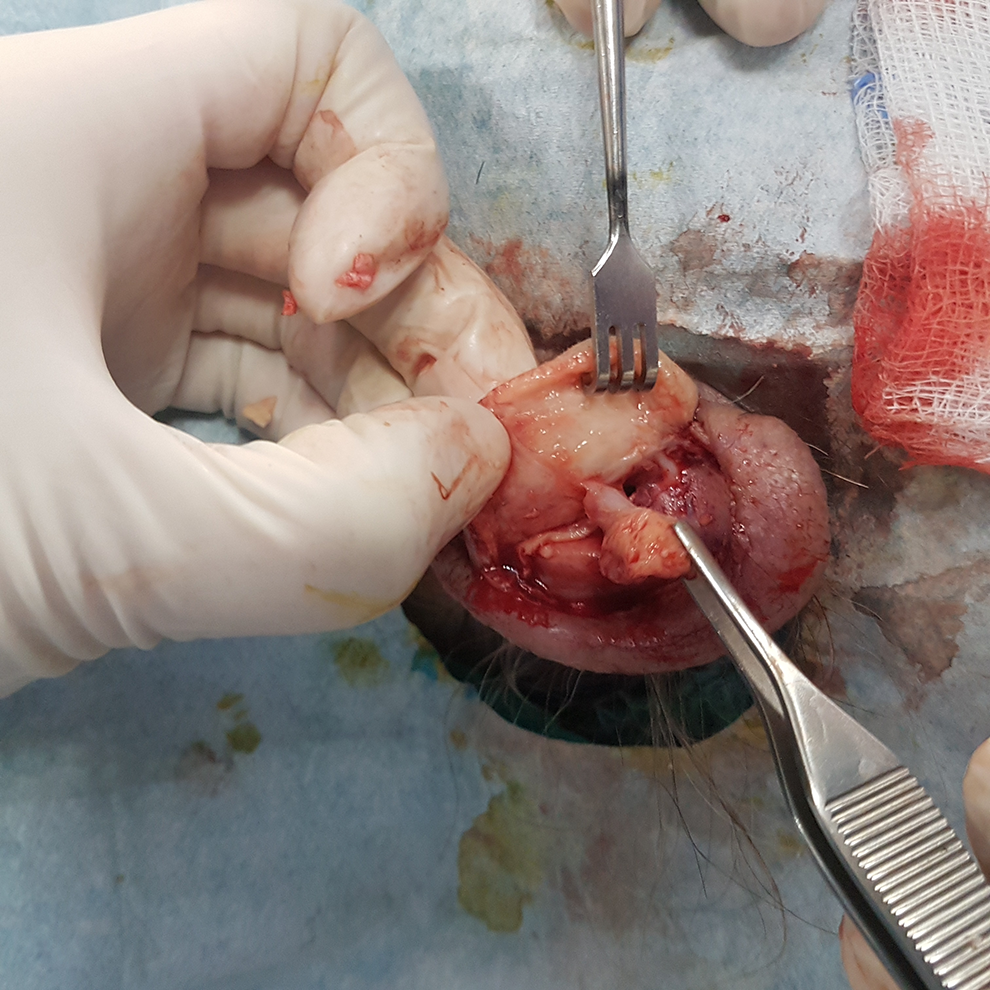
Removal of thickened subcutaneous tissue and necrotic cartilage.
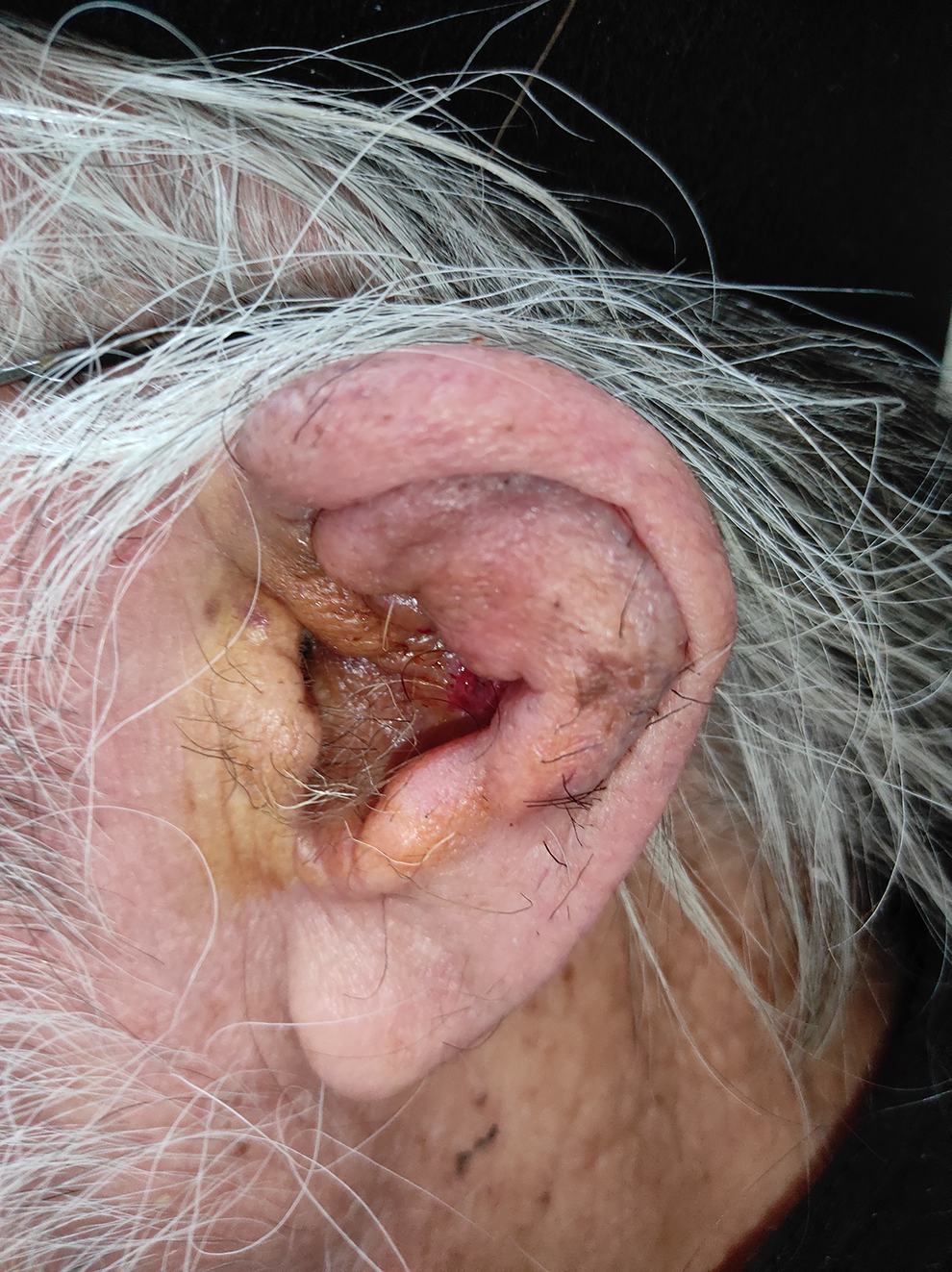
The final outcome. Complete resolution of the inflammation with minor deformity.
Discussion
The main symptoms of auricular perichondritis are erythema, edema, and tenderness. 1 Predisposing factors include trauma, auricle piercing, insect bites, and autoimmune diseases. 2 Immunocompromised and diabetic patients are prone to auricular perichondritis due to their susceptibility to infections. Untreated or persistent inflammation may easily result in necrosis of the cartilage and eventually in a deformed auricle (the so-called cauliflower ear). 3
Pseudomonas aeruginosa and Staphylococcus aureus are the most common causative bacteria. 4 Treatment consists of culture-oriented antibiotics (oral or intravenous) and if an abscess is present, then surgical drainage is warranted. However, Pseudomonas cases seem to require longer hospitalization due to their strong resistance against common wide-spectrum antibiotics. Therefore, the early initiation of empiric antipseudomonas treatment is strongly recommended, especially in cases where comorbidities exist. 5
According to the literature, surgical incision or wound debridement should be performed when conservative treatment fails with mixed results in cosmetic sequelae. 6 Our case supports the necessity of surgical intervention in persistent or recurring cases. Surgical debridement with preservation of unaffected cartilage eradicates the inflammatory foci and accelerates the curative process.
Footnotes
Authors’ Note
The authors declare that written informed consent for patient information and images to be published was provided by the patient.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
