Abstract
Internal branch of superior laryngeal nerve (ibSLN) provides sensory innervation mostly to the supraglottic part of the larynx and thus prevents aspiration during ingestion. Normally, it is distributed to the larynx after piercing the thyrohyoid membrane above the superior laryngeal artery. Multiple anatomical variations in the course of ibSLN have been reported. An early ibSLN bifurcation and course through double thyroid foramen constitutes an interesting anatomical variation that may easily lead to an injury during procedures in the thyroid gland and the larynx. Knowledge of the anatomical variability is essential in order to prevent surgical complications that could potentially impact the patient’s quality of life.
Case Presentation
An anatomical variation of the internal branch of superior laryngeal nerve (ibSLN) was observed during the dissection of a 64-year-old Caucasian female formalin embalmed cadaver, from Northern Greece. The cadaver was donated to the Department of Anatomy, Aristotle University of Thessaloniki. Cardiac arrest was documented as the cause of death. Dissection of the specimen did not reveal any gross pathology in the head and neck region. Left ibSLN was identified and dissected meticulously. The distribution of the nerve was abnormal (Figure 1). The ibSLN bifurcated shortly after branching from the main trunk of the superior laryngeal nerve and before reaching the larynx. Both branches crossed the laryngeal framework through 2 distinctive thyroid foramina. These foramina were located in the left lamina of the thyroid cartilage. Consequently, double thyroid foramen was recorded on the left side. The distance between the foramina was 0.6 cm.
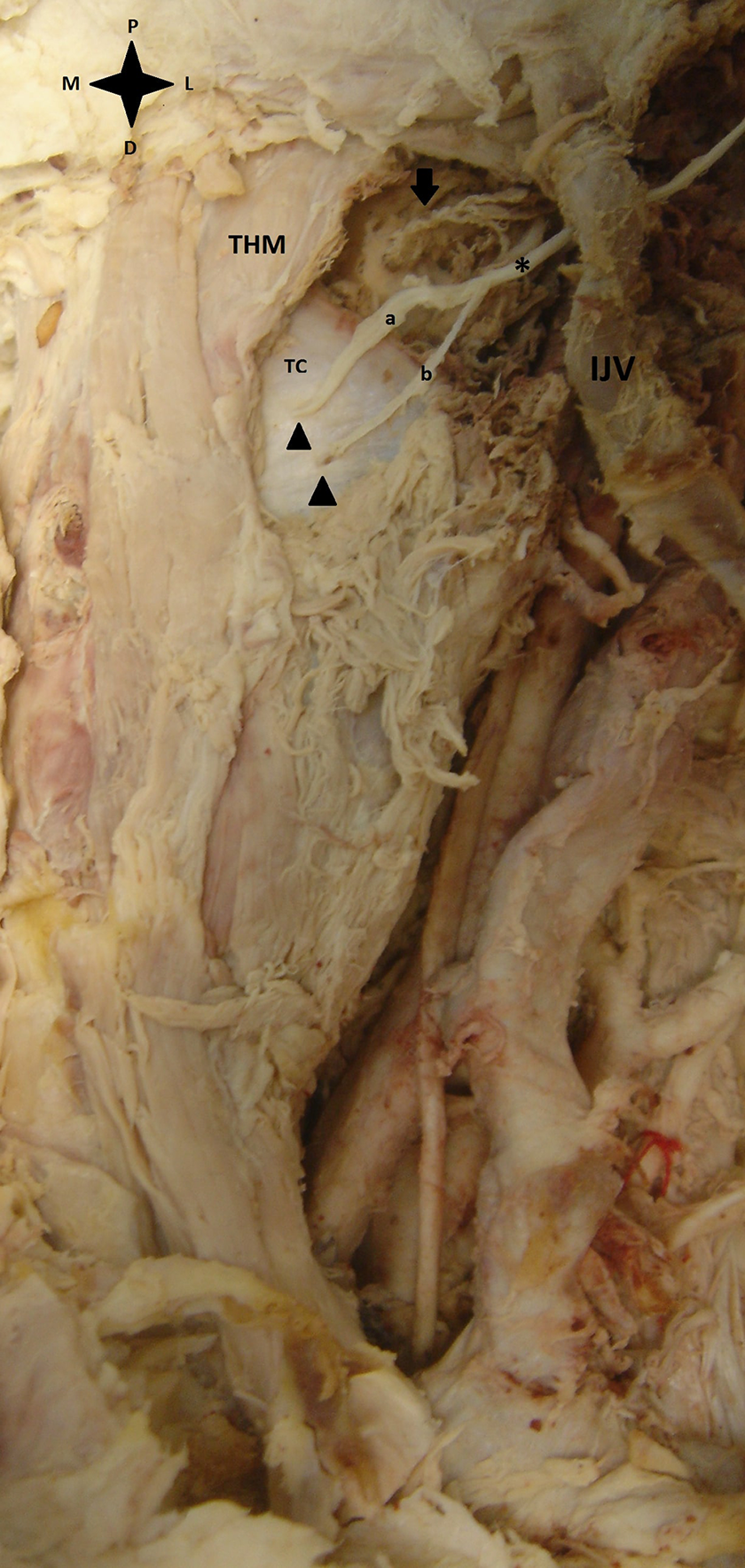
Cadaveric dissection. THM: thyrohyoid muscle, TC: thyroid cartilage, IJV: internal jugular vein, asterisk: internal branch of superior laryngeal nerve, a: upper branch, b: lower branch, arrowheads: thyroid foramina, arrow: superior laryngeal artery. D: distal, P: proximal, M: medial, L: lateral.
The upper branch of ibSLN run horizontally and was found to supply the mucosa of laryngeal vestibules, valleculae, epiglottis, and part of the pharyngeal mucosa. The lower branch headed downward in a vertical fashion. Its course included the medial wall of the piriform recess and provided innervation to the aryepiglottic fold, and the mucosa of the arytenoid cartilage. Finally, it united with the ascending branch of the recurrent laryngeal nerve to form “Galen’s anastomosis.” The superior laryngeal artery of our specimen pierced the thyrohyoid membrane, separately from the ibSLN. To the best of our knowledge, this is a rather rare anatomical variation and only a few cases have been reported in the literature.
The presence of thyroid foramen—a deficit in the thyroid cartilage—was first described in 1847. 1 Dimensions, incidence, and content vary. 2 -4 The presence of bilateral foramen was observed in 9% of studied specimens, whereas double thyroid foramen (on the same side) was detected only in a few occasions with its frequency ranging from 0.6% to 3.3% across studies. 4
Awareness of the possible presence of a thyroid foramen is extremely beneficial to the head and neck surgeon. The ibSLN’s bifurcation occurs either before or after piercing the thyrohyoid membrane (37.5% distal and 62.5% proximal to the thyrohyoid membrane, respectively). 5 Superior laryngeal artery may not accompany the superior laryngeal nerve while piercing the thyrohyoid membrane. 6 As a result, it could supply the larynx independently through the thyroid foramen. In such cases, there is a potential risk of an unexpected and unexplained laryngeal bleeding. In addition, the aberrant course of the ibSLN can lead to complications during surgical interventions in the larynx or the thyroid gland. Injury of the ibSLN leads to sensory loss of the larynx, which could increase the likelihood of aspiration.
In cases of laryngeal trauma, the presence of thyroid foramen can easily mislead radiologists, who may not be aware of this entity. Therefore, it can be considered as a fracture, a diagnosis that drastically changes the treatment algorithm. 4
Thyroid foramen was originally considered a weak spot in the thyroid cartilage that may be associated with the rapid spread of a tumor to surrounding structures. 7 However, the presence of connective tissue free of neoplastic infiltration in laryngectomy specimens provided conclusive evidence that this hypothesis was mistaken. 8
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
