Abstract
Extrapulmonary tuberculosis in the head and neck region accounts for 10% of all tuberculosis cases. Cervical lymph nodes are the most common sites of head and neck tuberculosis and often mimics neck metastasis leading to overstaging and overtreatment. Fine needle aspiration has proven effective in diagnosing cervical tuberculosis. If a diagnosis of tuberculosis is confirmed, then the first-line treatment is oral antituberculosis medication.
Case Report
A 59-year-old female visited our clinic to assess a nonpainful left neck mass that had been present for 3 months. Physical examination revealed multiple enlarged left neck lymph nodes without obvious tenderness. Sonograms and computed tomography revealed bilateral thyroid tumors and multiple left neck enlarged lymph nodes at levels II, III, IV, V, and VI. Extracapsular extension of left thyroid cancer with strap muscle invasion was strongly suspected. Fine needle aspiration (FNA) was performed on one left thyroid tumor and one enlarged lymph node. Cytological analysis revealed clusters of atypical cells in the thyroid tumor and nonspecific lymphoid cells in the lymph node. Based on suspicions of left thyroid cancer with left neck metastasis, the patient underwent bilateral total thyroidectomy with central neck dissection and left lateral neck dissection at levels II, III, IV, and V. Despite multiple severe adhesive lymph nodes, the surgeon was able to preserve the sternocleidomastoid muscle (SCM), internal jugular vein (IJV), and spinal accessory nerve (SAN). The results revealed papillary thyroid carcinoma involving bilateral thyroid lobes (3 foci) with left strap muscle invasion (Figure 1). One lymph node presented metastasis (level V; Figure 2), while more than fifty lymph nodes presented tuberculosis-related caseating granulomas (Figure 3). This led to a diagnosis of bilateral thyroid papillary carcinoma with left lateral neck metastasis and left cervical tuberculosis. No evidence of pulmonary tuberculosis was observed during the survey. Following surgery, the patient underwent radioactive iodine ablation and oral antituberculosis medication. Regular surveillance revealed no recurrence of thyroid cancer or tuberculosis.
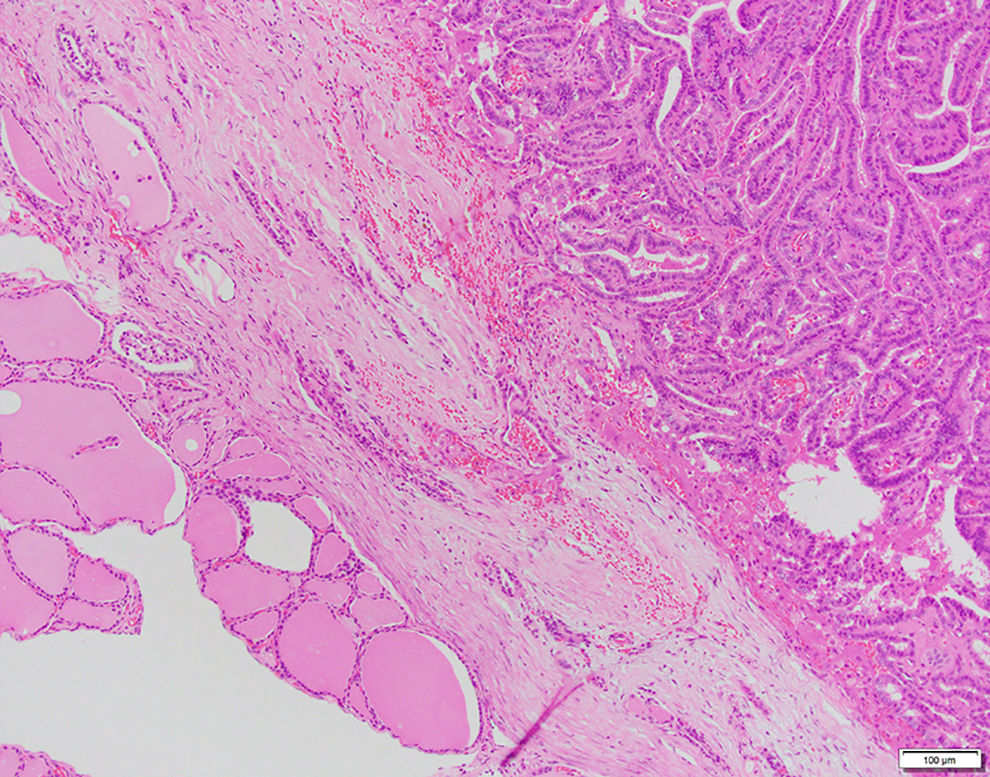
Microscopic examination revealed papillary thyroid carcinoma.
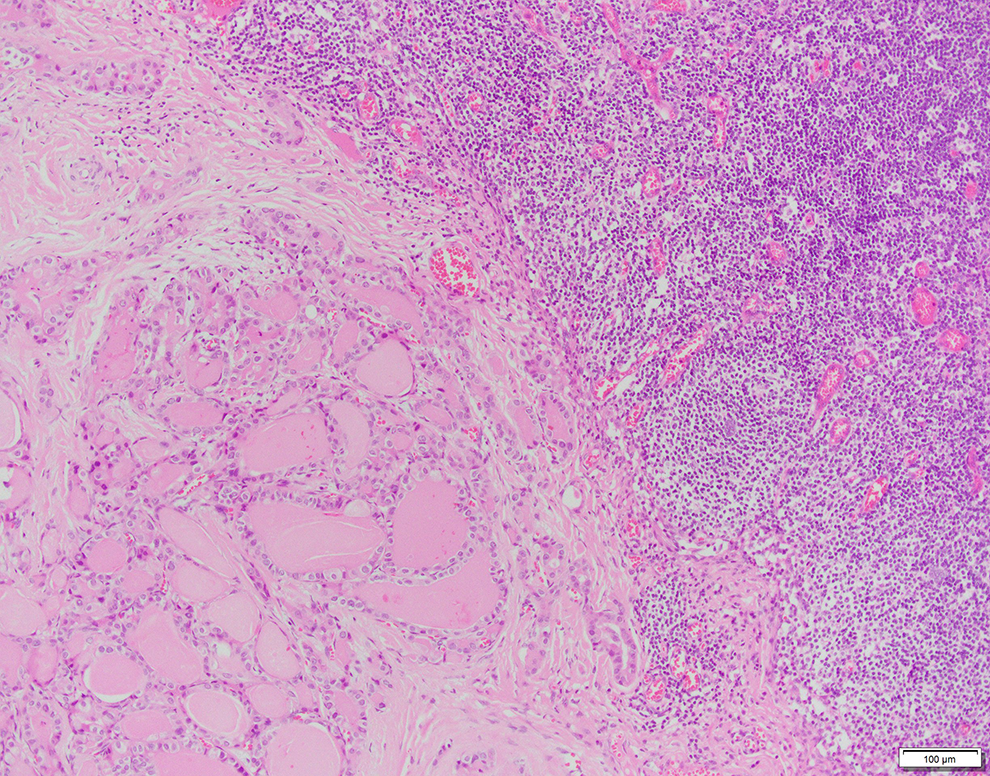
Microscopic examination revealed lymph node metastasis of papillary thyroid carcinoma.
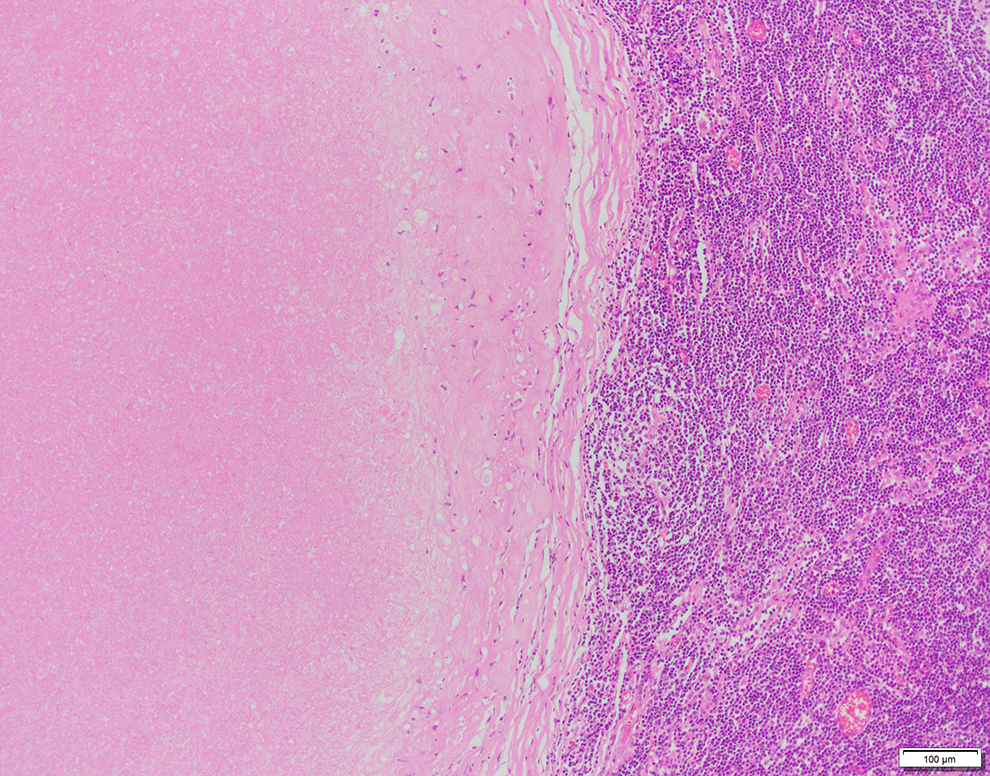
Microscopic examination revealed tuberculosis-related caseating granulomas in lymph nodes.
Discussion
Extrapulmonary tuberculosis accounts for 20% to 30% of all tuberculosis cases,1,2 and tuberculosis in the head and neck region accounts for 10%. 2 In a review article covering 5881 patients, the larynx (39%), cervical lymph nodes (38%), and oral cavity (10%) were the 3 most common sites of head and neck tuberculosis. 2 In that study, only 40 (0.6%) patients presented comorbidities with different types of tumors. 2 In another study of 410 patients, the incidence of tuberculosis in dissection specimens for head and neck cancers was 2%. 3
Therapeutic neck dissection is a routine procedure for locally advanced head and neck cancers; however, the value of prophylactic neck dissection in early stage cancers remains controversial. Nonetheless, cervical tuberculosis often mimics neck metastasis leading to overstaging and overtreatment. Satoh et al reported a case involving bilateral total thyroidectomy with central neck dissection and right lateral neck dissection at levels II, III, IV, and V, based on a preoperative diagnosis of right thyroid cancer with right lateral neck lymph node metastasis. 4 The SCM and IJV were killed during the surgery due to severe lymph node adhesion. The pathology report described right follicular thyroid carcinoma with right cervical tuberculosis without metastatic lymph nodes. Clinical course analysis in that case and the current study indicates that the only way to identify cervical tuberculosis preoperatively via FNA of neck lymph nodes for cytology or pathology evaluation. Fine needle aspiration has proven effective in diagnosing cervical tuberculosis in 32% to 79% of cases. 5 Note however that only nonspecific lymphocytes were observed in the case reported by Satoh et al and the current case. If a diagnosis of tuberculosis is confirmed, then the first-line treatment is oral antituberculosis medication. 2 In the current study, this could have delayed therapeutic lateral neck dissection for lymph node metastasis, which is strongly recommended by the American Thyroid Association. 6 Our decision to perform neck dissection for the removal of cervical tuberculosis and metastatic lymph node without killing the SCM, IJV, or SAN was fortunate. Nonspecific cytology analysis of the lymph nodes could be seen as a fortunate event.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
