Abstract
Necrotizing fasciitis is a rare and fulminant infection of the superficial fascia and subcutaneous cellular tissue. It is commonly polymicrobial, with the combination of aerobic and anaerobic bacteria, which contributes to the rapid progression and severity of the disease. The microbes commonly involved include group A streptococcus, Enterobacteriaceae, anaerobes, and Staphylococcus aureus. Over the past few years, skin and soft tissue infections, including necrotizing fasciitis, due to methicillin-resistant Staphylococcus aureus are increasing.
ENT Clinics
Necrotizing fasciitis is a rare and fulminant infection of the superficial fascia and subcutaneous cellular tissue. It is commonly polymicrobial, with the combination of aerobic and anaerobic bacteria, which contributes to the rapid progression and severity of the disease. 1 The microbes commonly involved include group A streptococcus, Enterobacteriaceae, anaerobes, and Staphylococcus aureus. Over the past few years, skin and soft tissue infections, including necrotizing fasciitis, due to methicillin-resistant Staphylococcus aureus (MRSA) are increasing. 2
A previously healthy 18-month-old boy presented with sudden onset of redness and swelling of the anterior aspect of the neck, which was followed by blackish discoloration of the skin. He also had fever, reduced oral intake, and was irritable. At the time of presentation to the ENT emergency, the skin overlying the anterior aspect of neck was necrosed and there was breakdown. His temperature was 101.4 °F. A complete blood count revealed hemoglobin of 6.5 g/dL; total leukocyte count of 16 200/mm3 with 75% polymorphonuclear leucocytes, 18% lymphocytes, 5% monocytes, 2% eosinophils; platelet count of 3 31 000/mm3. Peripheral smear and iron studies indicated iron deficiency anemia. He did not have any respiratory distress. A presumptive diagnosis of necrotizing fasciitis was made and the child underwent debridement. There was extensive necrosis of the skin and subcutaneous tissue over the entire anterior aspect of the neck, with fluid noted between the subcutaneous planes (Figure 1). The debridement was done till the presumed level of viable tissue, leading to a large defect on the anterior neck. The tissue specimen on histopathology revealed numerous bacteria, thrombosed vessels, acute inflammation and necrosis, consistent with necrotizing fasciitis. Culture of the debrided tissue grew S aureus resistant to penicillin and methicillin; and sensitive to vancomycin, linezolid, gentamycin, and teicoplanin. Accordingly, the patient was given injection vancomycin and gentamycin. Over the next week, the child underwent debridement 3 times (Figure 2). The final defect comprised the anterior part of the neck. Antibiotic treatment was continued for a total period of 3 weeks. The child also underwent blood transfusion for correction of anemia. Split skin grafting was done after that.
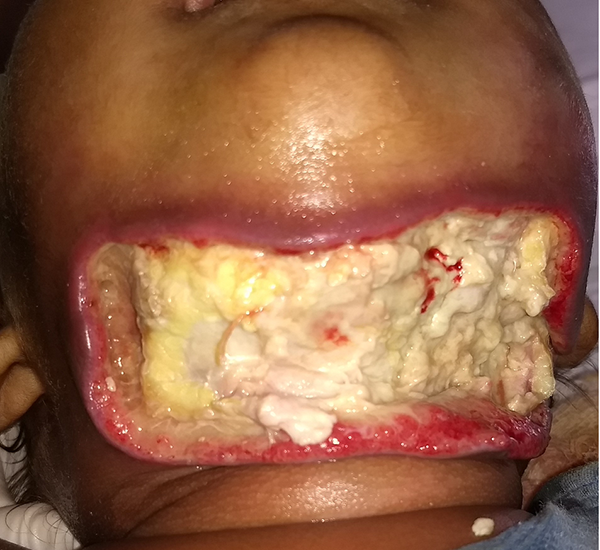
Necrotizing fasciitis involving the anterior neck in 18-month-old boy.
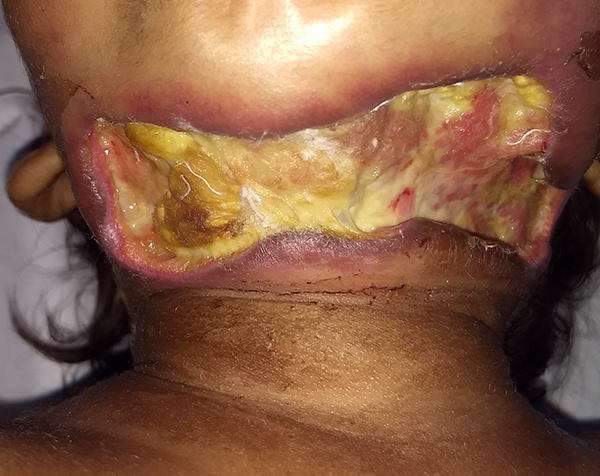
Following initial debridement.
Necrotizing fasciitis may be diagnosed by a combination of symptoms of systemic inflammatory response syndrome and skin symptoms—swelling, pain, erythema, and splinting. However, the initial subtle skin symptoms may be confused with cellulitis or may be ignored by the patient or caregivers, till there are more dramatic changes such as discoloration or necrosis, as in our patient. It most commonly affects the trunk, abdomen, perineum, and extremities. 3 Its occurrence in the head and neck is region is uncommon4,5 and may be associated with significant morbidity and mortality. Necrotizing fasciitis of the neck is uncommon, but involvement of the carotid artery and spread to the mediastinum can lead to high mortality. 6
Necrotizing fasciitis is associated with a high mortality rate, estimating around 38% to 50% in adults 6 and 25% in children. 7 Prompt diagnosis and aggressive treatment with surgical debridement and antibiotics is essential. Over the past few years, MRSA is assuming a more prominent role in skin and soft tissue infections, including necrotizing fasciitis. 8 Give its severity, a high index of suspicion is necessary and it is important to include vancomycin as a part of initial empiric therapy for all suspected cases.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
