Abstract
Spider angioma is a benign vascular lesion reminiscent of a spider’s body characterized by peculiar dilatation of end vasculature. The lesion is characterized by a central spot and extensions which radiate outward like a spider’s body. Spider angiomas may appear as a solitary or multiple lesion that arises on the skin surface of the face, neck, chest, and arms; these lesions have been rarely observed in the sublingual mucosa and in the gut, and to date, they have never been reported in the nasal mucosa. In this article, we report a spider angioma of the nasal cavity found as an occasional finding during a narrow band imaging nasopharyngeal endoscopy in a 70-year-old male patient with hepatitis C virus-related liver cirrhosis and a history of total laryngectomy in 2013 due to laryngeal squamous cell carcinoma. The lesion was located in the mucosa of the pavement of the posterior portion of the left nostril; it was painless and asymptomatic.
Spider angioma, also known as spider telangiectasia or spider naevus, is a benign vascular lesion characterized by peculiar dilatation of end vasculature that arises on the skin surface of the face, neck, chest, and arms.1,2 The lesion presents a central red spot with extensions that makes it similar to a spider; in addition, it is possible to observe diffuse surrounding erythema. 2 Spider angioma can be solitary or multiple. 2 These skin lesions are often associated with cirrhosis, but they can be indicative of autoimmune diseases as rheumatoid arthritis or thyrotoxicosis. 2 Rarely, spider angioma can be a sign of pregnancy or severe malnutrition. Multiple spider angiomas are characteristic of chronic liver disease with a specificity of 95%. 1
The physiopathological mechanism that underlies spider angioma formation consists of a dilation of preexisting central arterioles from which numerous thin-walled capillary branches radiate like spider legs, carrying away freely flowing blood. 2 There are several hypotheses about the mechanisms that lead to arteriolar vasodilation; the most consistent hypotheses are direct vasodilatory effects of alcohol, substance P, hypoestrogenism, and inadequate hepatic metabolism of steroid hormones.2-4 Another possible cause is neoangiogenesis; in fact, patients with liver cirrhosis generally present elevated serum vascular growth factors, such as vascular endothelial growth factor (VEGF) and basic fibroblast growth factor levels that could be at the basis of this process. The excessive estrogen stimulation can also stimulate neoangiogenesis and be implicated in the development of the spider angioma. 5 Association between female gender and alcoholic abuse 3 can explain why women are more likely to present spider angiomas compared to men.
To date, the presence of spider angiomas in the nasal mucosa has never been reported in the literature, despite they have been observed in the sublingual mucosa 6 and gut. 7 To the best of our knowledge, we describe the first case of a spider angioma arising in the nasal mucosa.
A 70-year-old male patient with hepatitis C virus (HCV)-related liver cirrhosis and a history of total laryngectomy due to laryngeal squamous cell carcinoma presented to our hospital for a narrow band imaging nasopharyngeal endoscopy as annual clinical follow-up of his previous cancer. During the endoscopy, we observed, as an incidental finding, a gray spider angioma on the mucosa pavement of the posterior portion of the left nostril (Figure 1). Other vascular dilatations with hyperemia were observed. The patient did not refer any previous episode of epistaxis. The lesion was completely asymptomatic. Based on patient’s conditions and the state of the lesion, the patient was put on follow-up by nasal endoscopy for potential growth.
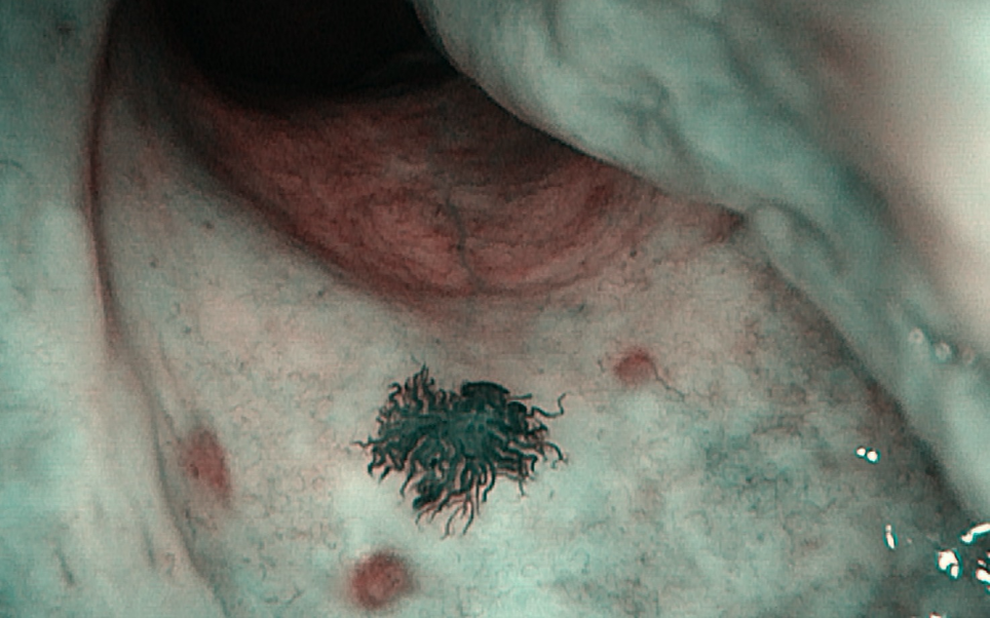
Spider angioma of the nasal mucosa. In this lesion, that is reminiscent of a spider’s body, we recognize the 3 specific characteristics of the spider angioma: a body, legs, and surrounding erythema. The body appears as a visible arteriole units; the lesion is surrounded by capillary vessels that radiate in a way from spider legs, with reduced dimensions toward the edges.
This case presents several interesting points; as first, it was located in the mucosa, a very uncommon site for spider angiomas. Additionally, it was in the nasal mucosa, a site where this type of lesion has never been reported. The lesion arose in a patient affected by liver insufficiency due to HCV infection, supporting the hypothesis that VEGF can impact the formation of the lesion.
In the absence of clear symptomatology, such as bleeding, mucosal spider angioma can be only an incidental finding. For similar cases, we suggest, even in the absence of symptoms, annual follow-ups to monitor the growth of the lesion and its potential transformation in a malignant lesion due to the inflammatory process that often accompanies these conditions.2,8
Footnotes
Authors’ Note
Dr Ralli and Dr Candelori conceptualized and designed the study, drafted the initial manuscript, and reviewed and revised the manuscript. Dr Di Stadio and Prof De Vincentiis reviewed, revised the manuscript, and critically reviewed the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work. The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
