Abstract

A 73-year-old female presented to the emergency department with a one-week history of bilateral nasal swelling and congestion that was associated with anosmia and pain. Her congestion and pain were worsening in intensity.
She denied any history of trauma or foreign body insertion. She reported it as starting with a pimple that she scratched it.
Her comorbidities included hypertension and a previous history of right breast cancer which was treated with resection and adjuvant chemotherapy.
Anterior rhinoscopy revealed a mucosal covered purplish mass bilaterally obstructing the nasal cavity (Figure 1). It was fluctuant on palpation. There were no signs of cellulitis of the surrounding tissue. The rest of the clinical examination was satisfactory.
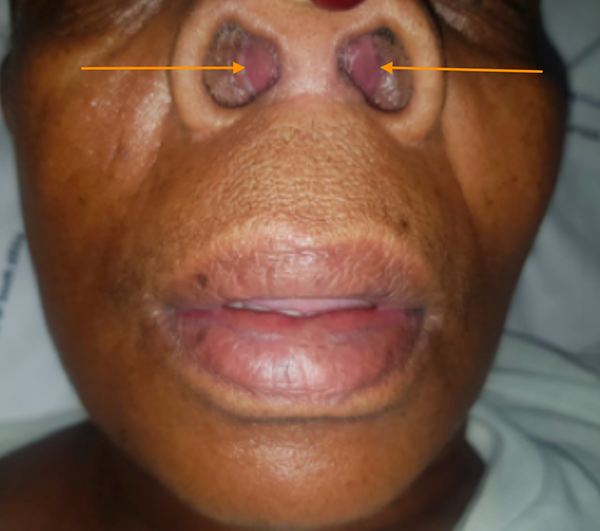
Nasal septal abscess (orange arrows).
Septic markers at the time of admission included C-reactive protein of 36 and a white cell count of 11.21. A diagnosis of a nasal septal abscess was made, and intravenous analgesia (paracetamol 1 gram every 8 hours) and broad-spectrum antibiotics (Co-Amoxiclav 1,2 grams every 8 hours) were commenced.
The patient consented to an incision and drainage of the abscess. A 7.5 mL of pus was drained and sent for microscopy and culture. Bilateral nasal packs were inserted for 24 hours to prevent reaccumulation of pus. Staphylococcus aureus was cultured and the antibiotic was changed to oral cloxacillin 500 mg 4 times a day. The patient was thus discharged and upon 2-week outpatient review, the abscess had completely resolved.
Discussion
Nasal septal abscess is defined as a collection of purulent material between the cartilaginous or bony septum and the mucoperichondrium or mucoperiosteum. Nasal septal abscesses secondary to a furuncle is a rare occurrence. A nasal septal abscess in the immunocompromised setting usually occurs secondary to insulin and non-insulin-dependent diabetes, human immunodeficiency virus, hematological malignancies, and chemotherapy. 1
The nasal septum is the main support structure of the nose. It is made up of cartilaginous and bony components. It is covered on either side by mucoperichondrium–mucoperiosteal membrane. Blood supply to the nasal septum is derived from branches of the external and internal carotid artery. The septum has many submucosal vessels supplying it. The mucoperichondrium itself has various arteriovenous anastomosis. The cartilaginous nasal septum gets it blood supply via the mucosa covering it. The cartilage itself is avascular.2,3
Therefore, any instance where there is a separation of the mucoperichondrium from the cartilage or expansion and obstruction of the blood vessels supplying the cartilage, it will result in compromise of its blood supply and progressive avascular necrosis within 3 days. If a hematoma does occur, it is an ideal medium for colonization and growth of bacteria.
Nwosu and Nnadede presented a prospective study detailing management and outcomes of septal hematomas/abscess. They found of 53 patients in the study only 4 patients were secondary to furuncles. With the average presentation to a health care facility being 2 weeks, the major presenting symptom being nasal obstruction. All had successful outcomes with incision and drainage. 4
Matsuba and colleagues presented an unusual case of septal abscess secondary to isolated sphenoid sinus information. The most common pathogen isolated in most studies was Staphylococcus aureus. This was on Gram stain culture of the pus. 5
The most common pathogen identified is Staphylococcus aureus. The less common are Streptococcus and other anaerobes. In the pediatric population, haemophilus influenzae is more common. Other rare pathogens that have been reported are pseudomonas and klebsiella. Fungal causes have also been described in immunocompromise individuals.
A computed tomography scan is recommended when there is facial/periorbital cellulitis, significant headache, symptoms of meningitis, altered consciousness or localizing neurological signs, and failure to improve clinically post incision and drainage. Computed tomography scan is also indicated especially if the underlying cause is uncertain. If the patient is suspected of having Wegener’s granulomatosis, tuberculosis, syphilis, sarcoma, or lymphoma especially in spontaneous onset of hematomas.6,7
Conclusion
Management of septal abscess requires prompt identification and surgical drainage, with intravenous or oral antibiotics. Most commonly, a hemitransfixion incision is used. With 0.9% saline washout, quilting sutures and nasal packing can be used to prevent reaccumulation of pus/blood. If at the time of incision and drainage marked destruction of the cartilage is noted, a decision for reconstruction can be made.
Complications of septal abscess include destruction of cartilaginous septum with resultant saddle nose deformity, intracranial complication including meningitis, cerebral abscess, subarachnoid empyema, and cavernous sinus thrombosis. It may also result in functional disturbance of the nasal airflow.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
