Abstract

A 76-year-old man presented with recurrent, mild right-sided epistaxis and nasal obstruction of 8 years duration. The patient had also noticed a small nodular lesion on the soft palate 3 years ago which progressively increased in size and numbers with difficulty in swallowing. Previously he had received empirical antitubercular therapy for 9 months, based on a nasopharyngeal lesion biopsy revealing granulomatous inflammation. However, he continued to have worsening symptoms. He had no known comorbidities and denied any history of trauma.
Nasal examination of the patient revealed granular mucosa on the right side with a fleshy mass involving inferior turbinate (Figure 1). Similar granular lesion was noted involving the soft palate, uvula, both tonsils, and left retromolar trigone (Figure 2).
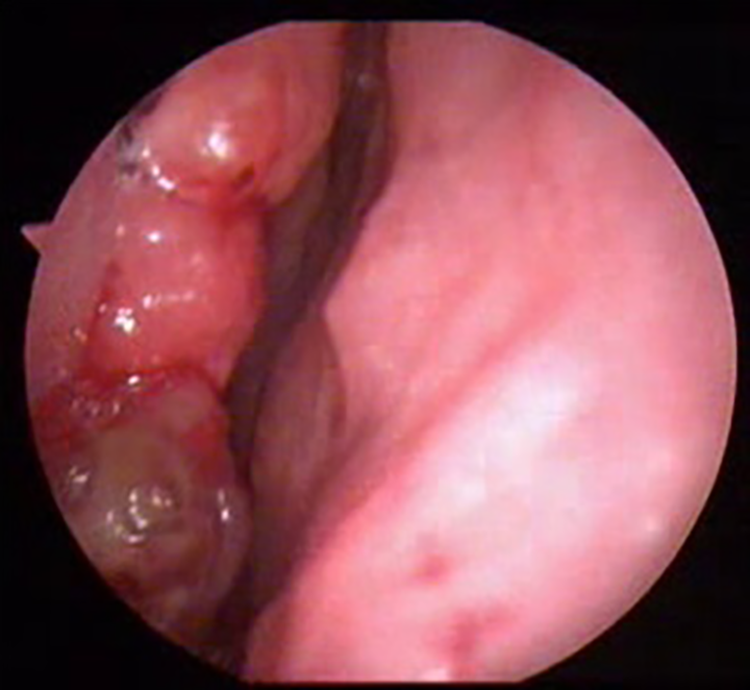
Right nasal cavity with granular mucosa and a fleshy mass involving inferior turbinate.
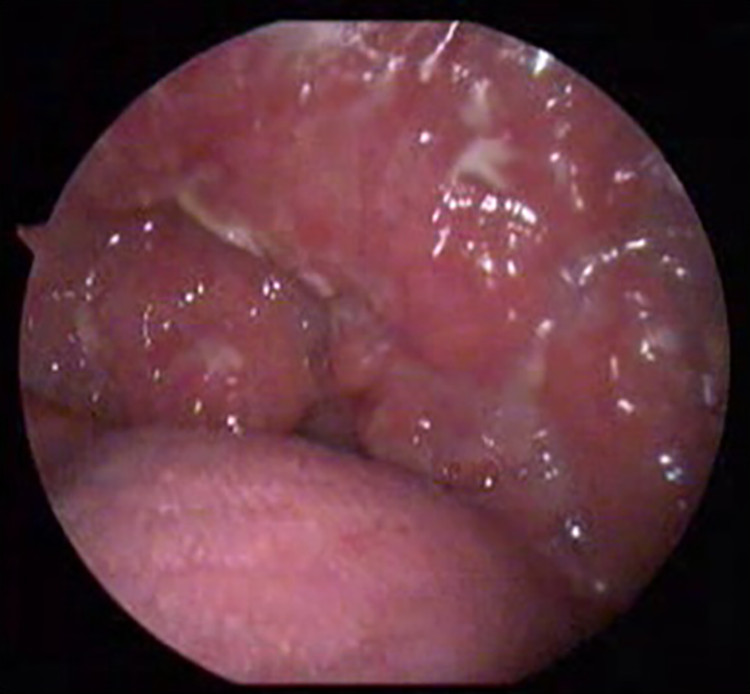
Granular lesion involving the soft palate, uvula, and both tonsils.
Computed tomography revealed an ill-defined enhancing soft tissue lesion in oropharynx extending down to hypopharynx and a heterogeneously enhancing well defined mass with calcific densities in right nasal cavity attached to inferior turbinate extending to middle meatus.
The histopathology of the mucosal lesions revealed dense subepithelial infiltrates of lymphocytes, plasma cells, few eosinophils, histiocytes, and nonnecrotizing granulomas. However, special stains for acid-fast bacilli and fungal organisms were negative. Leishmania ITS1 polymerase chain reaction (PCR) followed by sequencing and LD1 PCR on the nasal mucosal tissue identified Leishmania donovani and the serum was positive for anti rK39 antibody.
A diagnosis of mucosal leishmaniasis was established and treatment with intravenous liposomal amphotericin B to achieve a cumulative dose of 20 mg/kg of body weight was given. The patient showed significant improvement and had complete resolution of symptoms and regression of the mucosal lesions on 3 months follow-up.
Mucosal leishmaniasis caused by L donovani is a rare but increasingly reported entity from the endemic regions.1,2 Leishmania donovani usually causes visceral leishmaniasis with fever, splenomegaly, and systemic manifestations also known as kala-azar. Patients with a past history of visceral leishmaniasis can occasionally present with cutaneous manifestations many years later, called post kala-azar dermal leishmaniasis, and a minority of them may have mild mucosal involvement. 3 The mucosal involvement is classically seen in New World leishmaniasis. In areas known for Leishmania braziliensis transmission, almost 5% of patients with cutaneous leishmaniasis concomitantly or subsequently develop mucosal disease. 4 However, the mucosal involvement is also a possible presentation of Old World leishmaniasis, due to L donovani or Leishmania major infections rarely. 2
The mechanism by which the mucosal involvement occurs in L donovani infection is unclear and is difficult to study given the infrequent number of cases. The probable routes of spread of protozoa to reach mucous membranes could be a direct extension of contiguous facial skin lesions or lymphatic/hematogenous spread from a distant site. 5
Immunodeficiency and mucosal immunosuppressive factors, like tobacco smoke, corticosteroid therapy (systemic and inhaled), and so on, predispose to the development of mucosal leishmaniasis (ML). 6 Interestingly all these were notably absent in our patient. The fact that rarely isolated ML is seen in immunocompetent patients may reflect the attempt of the immune system to confine the disease rather than result of uncontrolled progression of the disease. It is possible that the L donovani presenting with mucosal disease without systemic manifestation may have an altered tropism and are genetically distinct from visceral strains similar to the recent reports from Sudan. 7
The most common symptom of ML is persistent nasal congestion. Clinical examination may reveal florid inflammation of the nasal mucosa with lesions varying from fine granular lesions, superficial ulcerations and granulomas to erosion of underlying tissue, and local progression of the disease. 8 Common sites of involvement are anterior septum, inferior turbinate, and the floor of the nasal cavity. Lesions may also affect the palate, pharynx, and larynx causing palatal dysfunction, nasal regurgitation, dysphagia, dysphonia, and aspiration.
Demonstration of leishmania parasites in infected tissues by culture or PCR is gold standard for diagnosis. The histopathology usually shows nonspecific granulomatous changes. The standard treatment of leishmaniasis with L donovani with liposomal amphotericin, using a cumulative dose of 15 to 20 mg/kg of body weight in 3 to 4 doses, results in excellent outcomes in immunocompetent patients.
Although mucosal leishmaniasis due to L donovani is exceedingly uncommon, patients from the endemic region with nasal and oropharyngeal mucosal lesions should be evaluated for the possibility of leishmaniasis, particularly in those with persistent disease. This case highlights the possibility of primary mucosal leishmaniasis caused by L donovani in an immunocompetent individual and demonstrates the importance of confirming the diagnosis and initiating appropriate treatment resulting in good outcome.
Footnotes
Declaration of Conflicting Interests
The author (s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
