Abstract

An 8-month-old infant with extensive petechial and purpuric rash was accepted to our pediatric intensive care unit (PICU). Patient’s purpuric rash involved the face, chest, and upper and lower extremities markedly (Figure 1A). The patient required intubation secondary to decompensated septic shock, and a purpuric lesion was noticed on the right side of the epiglottis during the initial attempt for intubation. A picture of the lesion was taken by video laryngoscopy (Figure 1B). This lesion was considered as a mucosal manifestation of purpura fulminans. Blood culture and cerebrospinal fluid polymerase chain reaction were positive for Neisseria meningitidis. The patient was treated with antibiotics, intravenous fluids, mechanical ventilation for 27 days, and plasma exchange for 7 sessions. The epiglottic lesion disappeared without any tissue loss, but although the skin lesion improved considerably, her feet and distal part of the legs needed amputation bilaterally. She was transferred to pediatric infectious diseases service without any neurological sequel on the 38th day of PICU admission.
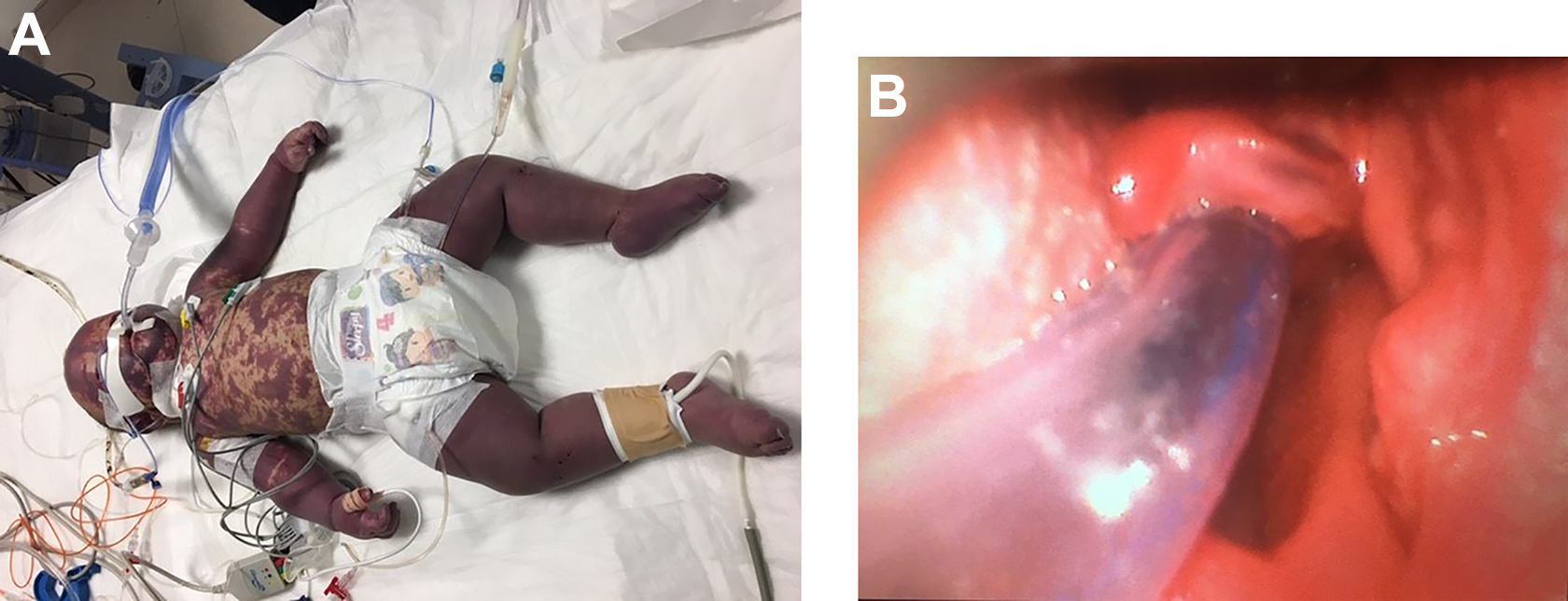
A, Patient’s whole body covered with purpuric rash due to purpura fulminans form of meningococcemia. B, Mucosal purpuric rash on the right side of epiglottis due to meningococcemia. Arrow shows the lesion. This image was taken by video laryngoscopy.
Meningococcemia is a severe sepsis which causes rapidly clinical deterioration, mental alterans, fever, petechial and purpuric rashes, disseminated intravascular coagulation, and multi-organ failure. Early antibiotic and fluid therapy is essential and lifesaving. 1 -3 Our patient was with severe form of purpura fulminans and it was destructive, especially affecting upper and lower extremities. Epiglottic purpuric lesion in meningococcemia is first time determined by us; there was not any report about the meningococcal involvement on epiglot or airway previously. This involvement resolved in follow, and we related to severe form purpura fulminans.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
