Abstract
Background:
Untreated traumatic tympanic membrane perforations (TMPs) may lead to permanent perforations and hearing loss. There are many materials that have been previously used for repairing the TMPs.
Aims and Objectives:
The purpose of this study is to evaluate the clinical and histological effects of Vivosorb (Vv) and Epifilm on healing of TMPs in a rat model.
Material and Methods:
The posterior-inferior quadrant of the tympanic membranes (TMs) in right ears of 14 rats was perforated using a 20-g needle and then the animals were randomly divided into 2 equal groups (n = 7). The perforated right TMs were treated with either Vv (Vv group) or Epifilm (Ep group). The left TMs of 7 rats were perforated in same way and allowed to close spontaneously without any topical material applications (spontaneous closure group as sham control, SC). The left tympanic membranes of the other 7 rats were not perforated and used as normal controls (NC group). On postoperative 15th day, tympanic bullas were extracted from killed rats and examined morphometrically and histopathologically.
Results:
Perforation closure rate was 85.7% (6/7) in both Vv and SC groups. Perforations of Ep group closed in 7/7 (100%) ears. The thicknesses of the perforated membranes were increased in SC and especially Vv groups. Also, connective tissue fibrosis, blood clots, and epithelial degenerations were detected in SC and Vv groups. The mean fibroblastic reaction scores of Vv, Ep, and SC groups were 2.14(+), 0.57(+), and 1.71(+) respectively, on comparison with NC group. The mean neovascularization score was 1.42(+) in Vv group, 0.14(+) in Ep group, and 0.57(+) in SC group.
Conclusion and Significance:
Vivosorb and especially Epifilm can improve the healing process in traumatic TMPs and additionally, Epifilm might be more preferred for the treatment of TMPs because of causing lesser fibrosis.
Introduction
Tympanic membrane perforation (TMP) which is commonly seen in otolaryngology clinics occurs as the result of various traumatic situations such as blast injuries, interpersonal violence, barotrauma, and the removal of foreign bodies. 1 The pathogenesis of TMPs is not fully understood and if it is left untreated, it may lead to hearing loss or permanent TMPs. There is an increasing interest on the studies of healing mechanisms using surgical materials. 2,3 The spontaneous closure rate of the traumatic TMP is approximately 90%. 2,4 Although most of the traumatic TMPs heal spontaneously, they need to be treated especially in larger perforations.
In acute TMPs, the surgical materials approximate the perforation of edges, prevent the distortion of the edges toward the inner endodermal epithelium and play a role as a scaffold for the regenerating epithelium. 5 In previous studies, some biomaterials such as growth factors and stem cells showed improving effects in the cell regeneration. 6 Furthermore, many materials, such as paper, silk patch, gel foam, micropore strip, alloderm, and water-soluble chitosan band have been used to close traumatic TMPs.
Vivosorb (Vv) is made of 100% synthetic bio-resorbable material which is called poly (
Although there are many studies assessing the impacts of Epifilm on traumatic TMPs in the literature, there has not been yet a study assessing the effectivity of Vv in these cases. This experimental study presents an evaluation of the effects of Epifilm (HA ester) and Vv (polymer) in TMPs and makes a comparison on the outcomes with a spontaneous healing and intact TM.
Materials and Methods
Animals and Ethical Approval
Fourteen healthy adult female Wistar albino rats weighing were between 200 g and 260 g were used after performing a power analysis and receiving an ethical permission from the local Board of Ethics (KOU HAYDEK 6/5-2013). All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. Tympanic membranes were evaluated by clinical examinations and the rats those had healthy TMs without plug in the outer ear way were included in the study.
Materials
Vivosorb (Polyganics BV L.J. Zielstraweg 1 9713 GX, Groningen-Netherland) and Epifilm (Xomed-Medtronic, Jacksonville, Florida) were used for surgical applications to traumatic TMPs of rats.
Surgical Procedure
A traumatic perforation was created using a 20-gauge 25 mm × 1 mm needle in the postero-inferior quadrant of the TM after ensuring the anesthesia of rats via 45 mg/kg intramuscular ketamine hydrochloride (Ketalar vial, Pfizer Pharmaceutical Co Ltd, Ketalar; İstanbul, Turkey) and 5 mg/kg xylazine HCI (Rompun vial, Bayer, Shawnee Mission, Kansas).
Experimental Groups
At the beginning of the experiment, the posterior-inferior quadrant of the tympanic membranes (TMs) in right ears of 14 rats were perforated. The animals were randomly divided into 2 equal groups (n = 7). Immediately following the surgery on day 0, Vivosorb was laid on the right TMPs of the Vv group (n = 7) after cutting it slightly larger than the size of the perforation. The left TMs of the rats in the Vv group were untouched and used as normal (intact) controls (NC group, n = 7). In the other group bilateral surgery was applied on the both TMs of the rats. Then, Epifilm (Xomed-Medtronic) was laid on the right TMPs by cutting slightly larger than the size of the perforation (Ep group, n = 7 rats). The left TMs of the rats among to Ep group were used as sham controls those were allowed to close spontaneously (sham control [SC] group, n = 7 rats). No packing or supporting materials were used to prevent graft displacement. However, the position of the graft was re-evaluated at third, seventh, and 10th day postoperatively.
Tissue Harvest
On the postoperative 14th day, animals were killed by intraperitoneal pentobarbitone injection (160 mg/kg). After being dissected, the bilateral bulla was left to fixation by being placed into 10% formaldehyde solution. Then, the specimens were followed by decalcification in 5% nitric acid solution (pH 7.2) at 22 ± 2°C. Decalcified TMs were dehydrated in a series of graded alcohols, embedded in paraffin wax, and transversely sectioned at the thickness of 5 μm. After that, they were placed on slides which were stained with hematoxylin-eosin and Masson Trichrome stain kit (Merck chemicals, Darmstadt; Germany), the histopathological values were examined and photographed using light microscope (Olympus BX53F, Incekaralar Tibbi Cihazlar Ticaret A. S.; İstanbul; Turkey; Figures 1 –5).
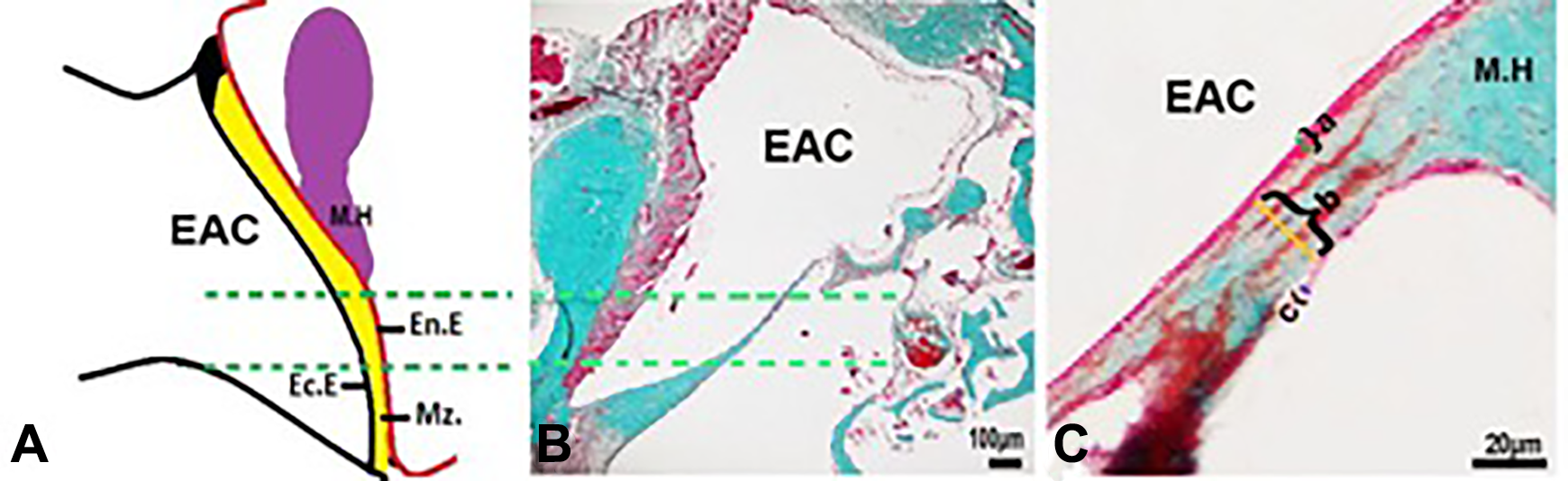
The illustration shows the measurements about the thickness of the layers in TM specimens. En.E, endodermal epithelium; Ec.E, ectodermal epithelium; Mz., mezodermal layer; M.H, malleus handle; green lines show measurement distance used for determining the thicknesses of the layers. C, The measurement area that between the green lines was shown at high magnification. A-C show thicknesses of ectodermal epithelium; mezodermal layer and endodermal epithelium, respectively. scale bars: 40 µm. TM indicates tympanic membranes.
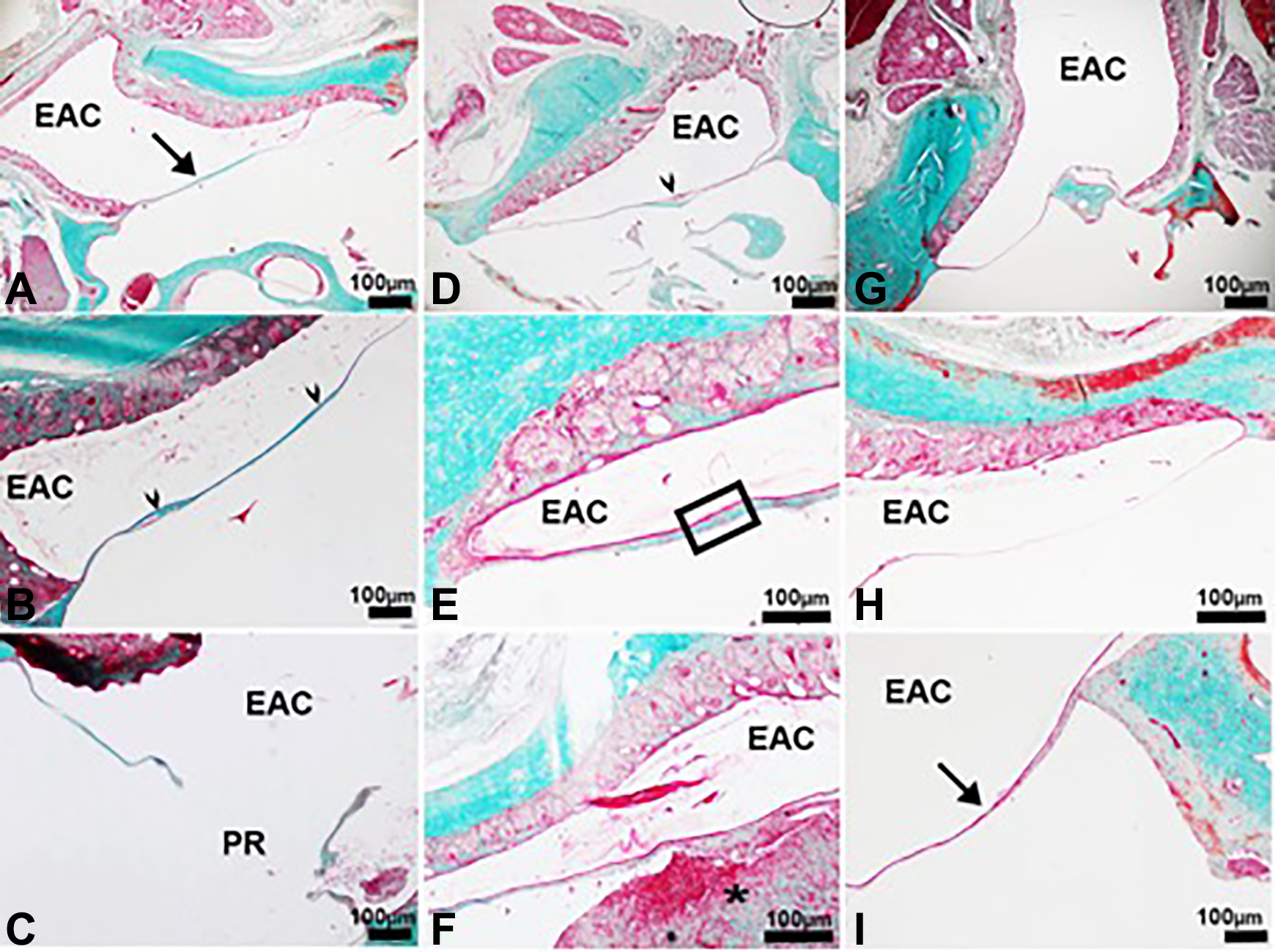
A-I are the light micrographs of the tympanic membranes in the all groups. A, Among to NC group; (B and C) among to SC group; (D-F) among to Vv group; (G-I) among to Ep group. EAC, external ear canal; PR, persistant perforation; arrow in A and I, TM with healthy appearance; asterisks, fibrosis cellular debris and hemorrhage in Vv group; arrowheads, TM with dense connective tissue and irregular appearance in SC and Vv groups, respectively; box shows thicker TM than those of the other groups in Vv group. Stain: Masson trichrome. TM indicates tympanic membranes
Morphometrical Evaluation
For the morphometrical evaluation, 10 slides from each TM specimens were used. Each area including TMs was photographed at ×40 magnification of the light microscope. Following, the thicknesses of the ectodermal epithelial layer (outer), mezodermal layer (lamina propria), and endodermal epithelial layer (mucosa) were measured using the Image-J program, (NIH, Maryland). In all TM specimens, this assessment was performed at a distance between 400 and 600 µm from the malleus handle. The thicknesses were taken from 3 different points of each area at the distance with 150 µm interval. Then, the average of these 3 values was used as mean thickness value (Figure 1). Hence, approximately 100 to 150 measurements were done for each TM specimen.
Histopathological Scoring
Histopathological scoring was done in SC, Vv, and Ep groups. The application details of the scoring are summarized in Figures 2 and 3. Subjective scoring was carried out according to the fibroblastic reaction (Figure 2) and neovascularization (Figure 3) degree between 0 and 3. Histopathological examination was done by 2 different histopathologists and results were compared.
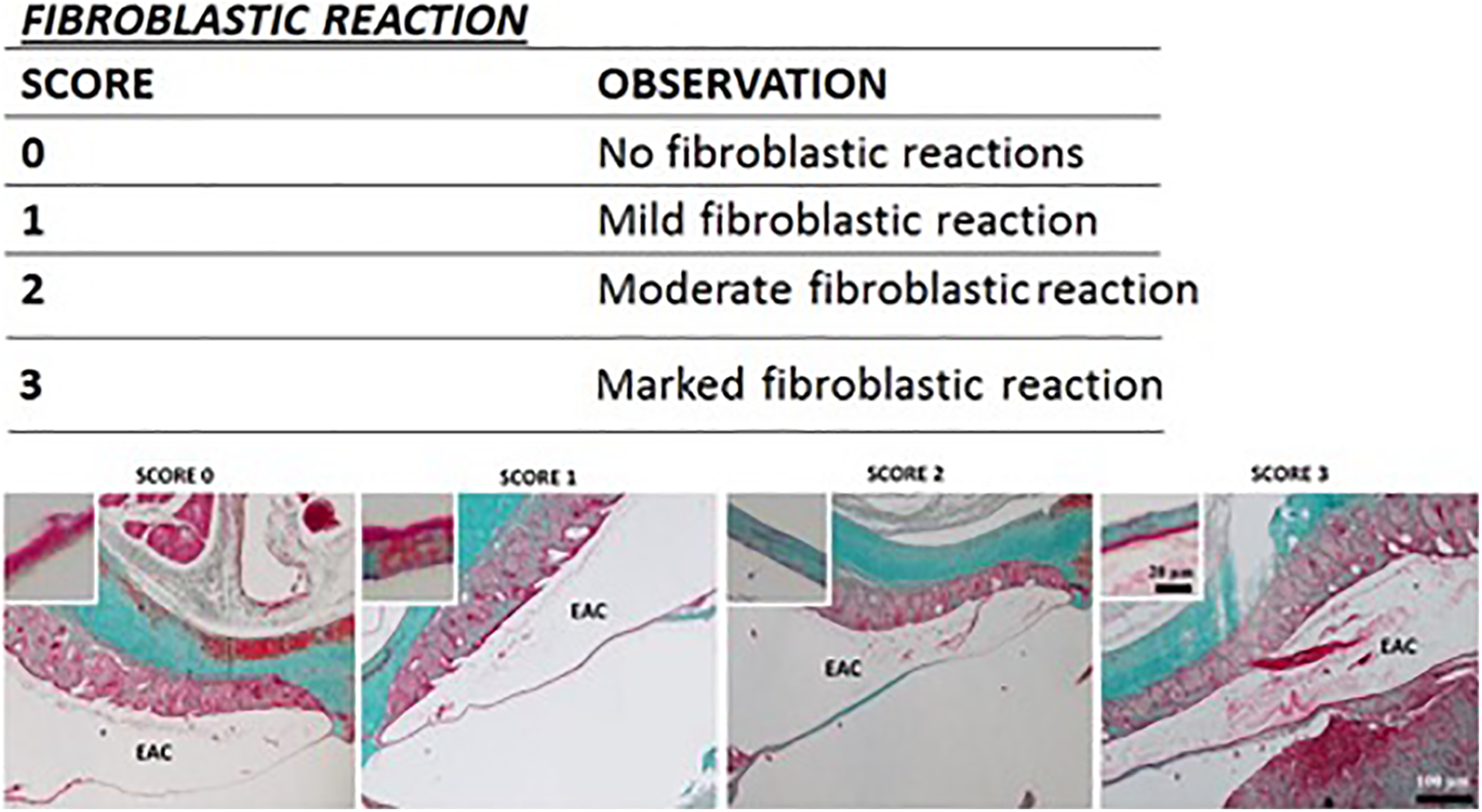
The illustration shows the characterization of the fibroblastic reaction in TM specimens. The table shows the scoring system used to evaluate the fibroblastic reaction in the tm perforations. EAC, external ear canal. Light microscopic figures show examples about marked scores. The insets indicated sample TM areas at high magnification. The fibroblastic reaction was evaluated based on Masson trichrome staining of collagen fibers performed at day 14 after TM perforation. TM indicates tympanic membranes.
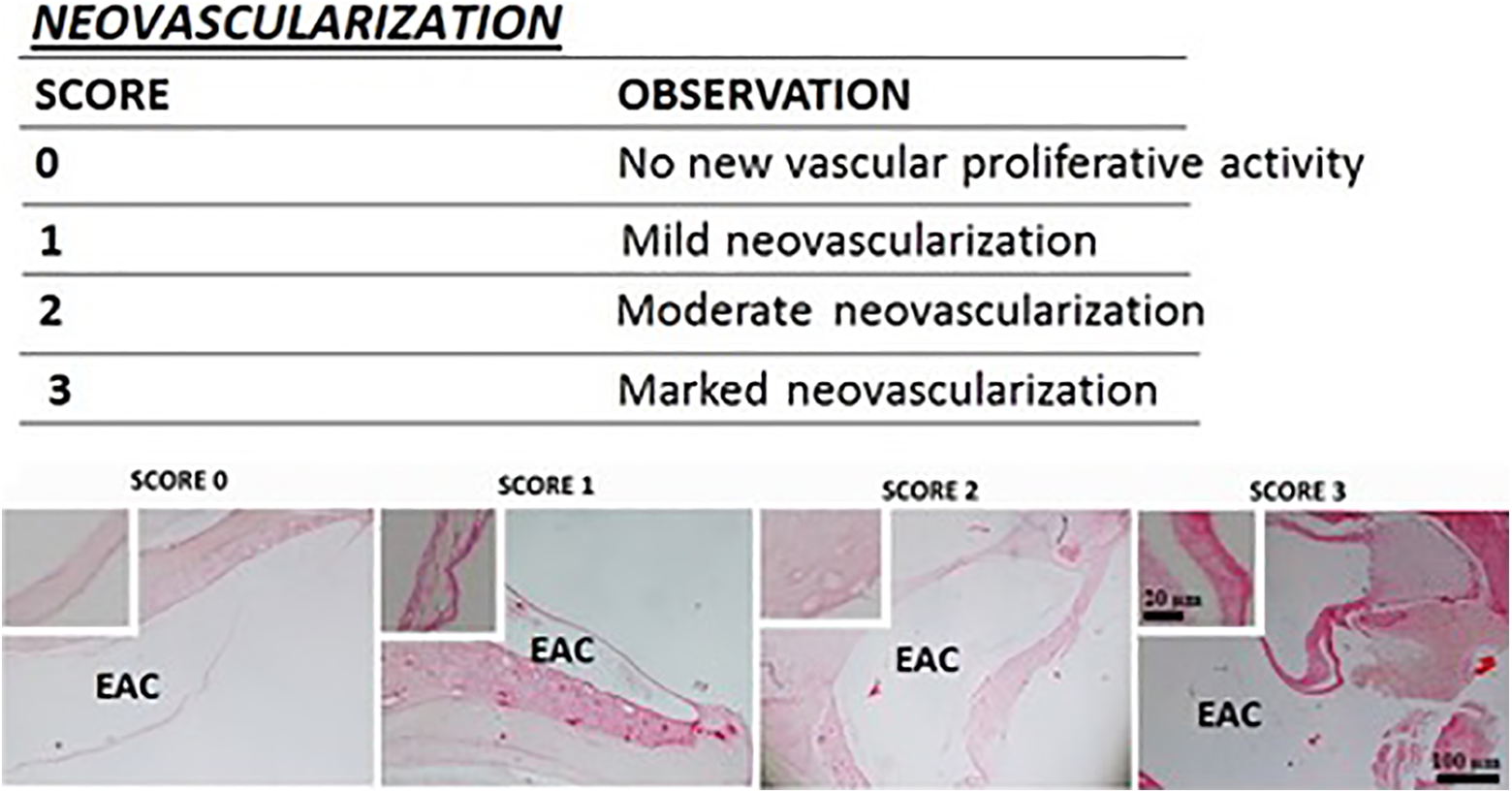
The illustration shows the characterization of the neovascularization in TM specimens. The table shows the scoring system used to evaluate the neovascularization in the TM perforations. EAC, external ear canal. Light microscopic figures show examples about marked scores. The insets indicated sample TM areas at high magnification. the neovascularization was evaluated based on hematoxylin-eosin staining of routine histological structures of TM samples including blood vessels performed at day 14 after TM perforation.
Statistical Analysis
Histopathological data of the groups were performed with one-way analysis of variance and χ2 tests using commercially available software (IBM SPSS Statistics version 20, SPSS Inc, an IBM Co, New York). Also the differences between the histopathological scores of the observers were statistically analyzed by paired samples t test (Wilcoxon signed rank test). All P values under .05 were considered as statistically significant.
Results
Thickness Measurement
Total thickness of the TM was significantly increased in SC (P < .05) and especially in Vv group (P < .01) as compared to that of the NC group. Thickness of the ectodermal epithelium was significantly increased in SC and Vv group when compared to the NC group (P < .05). Thickness of mesodermal layer was significantly increased in SC (P < .05) and especially in Vv group (P < .01) when compared to the NC group. There was not any statistical significance in terms of the TM layers between Ep and Nc groups (P > .05; Table 1).
The Mean Thicknesses (μm) of the Ectodermal and Endodermal Epithelia and Mesodermal Lamina of the Tympanic Membrane Were Summarized.
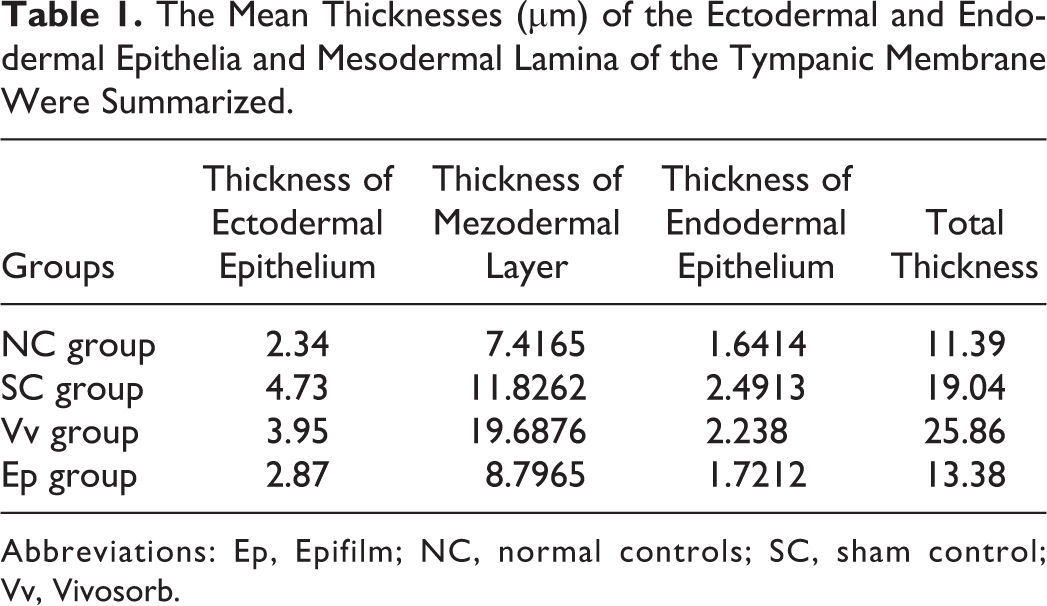
Abbreviations: Ep, Epifilm; NC, normal controls; SC, sham control; Vv, Vivosorb.
Histological Results
The TMs of the normal control group had a trilaminar membrane. In the outer, an ectodermal epithelium (the stratified squamous epithelial tissue) consisted of 1 to 2 rows of flattened epithelial cells throughout the length of the TM (Figure 2). In the middle, the connective tissue is present and organized with occasional fibroblasts and collagen fibers. The collagen fibers were connected to the malleus handle and in the tympanic annulus region; such fibers formed the fibrocartilaginous ring of the tympanic annulus. A few capillaries were located near the malleus handle. The inner endodermal epithelium (mucosal layer) had one row of flattened cells. Fourteen days after the perforation, in one of the animals of untreated group and Vv-treated groups, TM was still perforated. In some TM areas of these groups, irregular membrane organization, fibrosis, and cellular debris were detected. A significant thickening of the TM, epithelial membrane damage, dilated blood vessels, and clots were observed in different parts of the slides about untreated controls and Vv-treated groups. In the epifilm group, thickness of the TM didn’t increase; connective tissue, and epithelial structures of TM were normal (Figures 4 and 5).
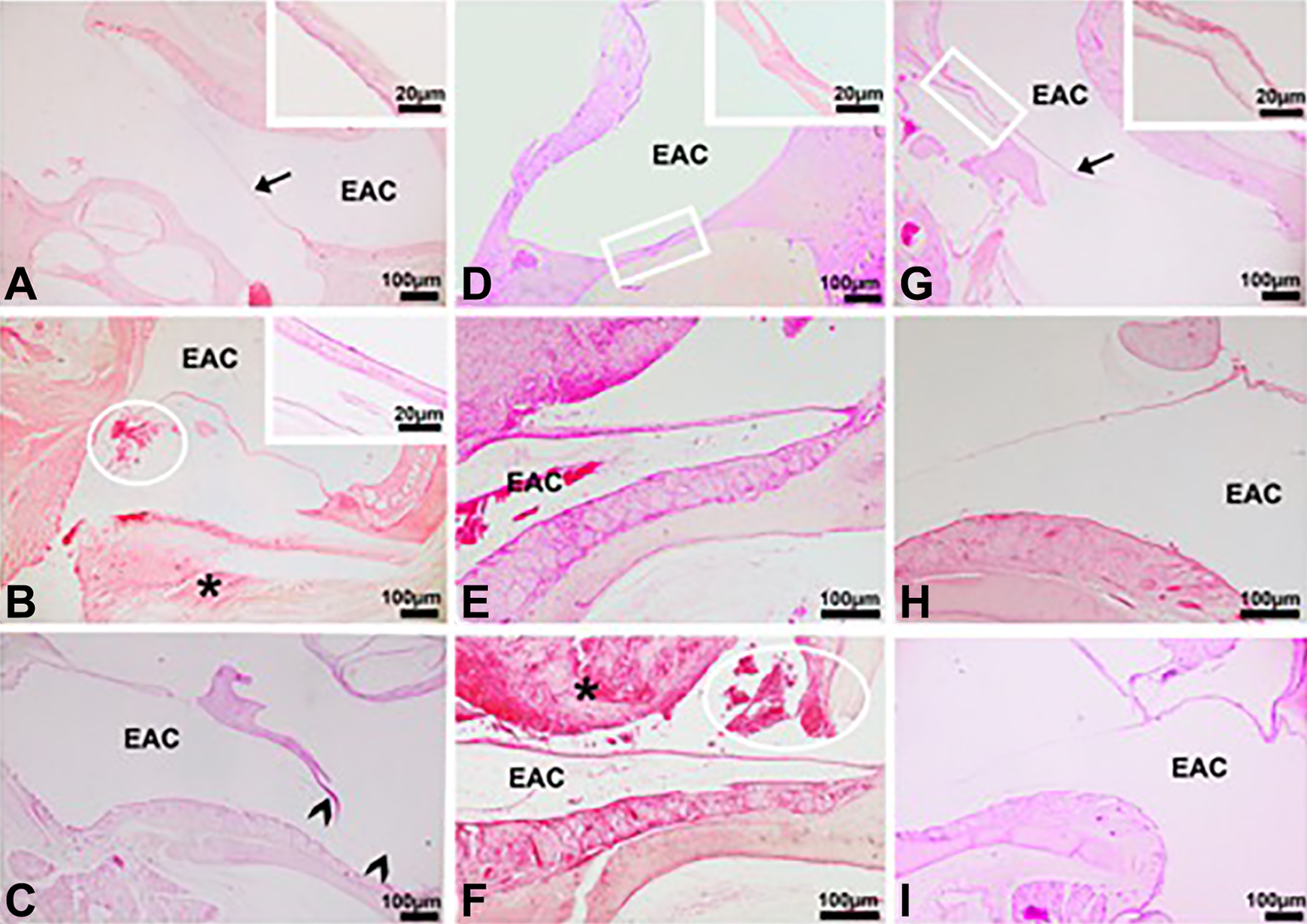
A-I are the light micrographs of the tympanic membranes in the all groups. A, Among to NC group; (B and C) among to SC group; (D-F) among to Vv group; (G-I) among to Ep group. eac, external ear canal; arrow and inset in A, TM with healthy appearance; asterisks, fibrosis, and cellular debris in SC and Vv groups; arrowheads, epithelial membrane damage in SC group; boxes in D and G show TM with dilated and normal vessels, respectively. Insets in D and G show boxes in high magnification. Circles in B and F show hemorrhage in tympanic cavities of SC and Vv groups, respectively. Inset in B shows TM with thick mucosa and dense connective tissue in SC group. Stain: hematoxylin-eosin.
Histopathological Scores
On the 14th day postoperative, the closing rate was 85.7% (6/7) in both the Vv and SC groups while all TMPs were closed in the Ep group (7/7). However, there was not a significant difference between the groups in terms of the closure (Table 2).
The Closure Rate at the End of the 15th Day Postoperative in the Groups.
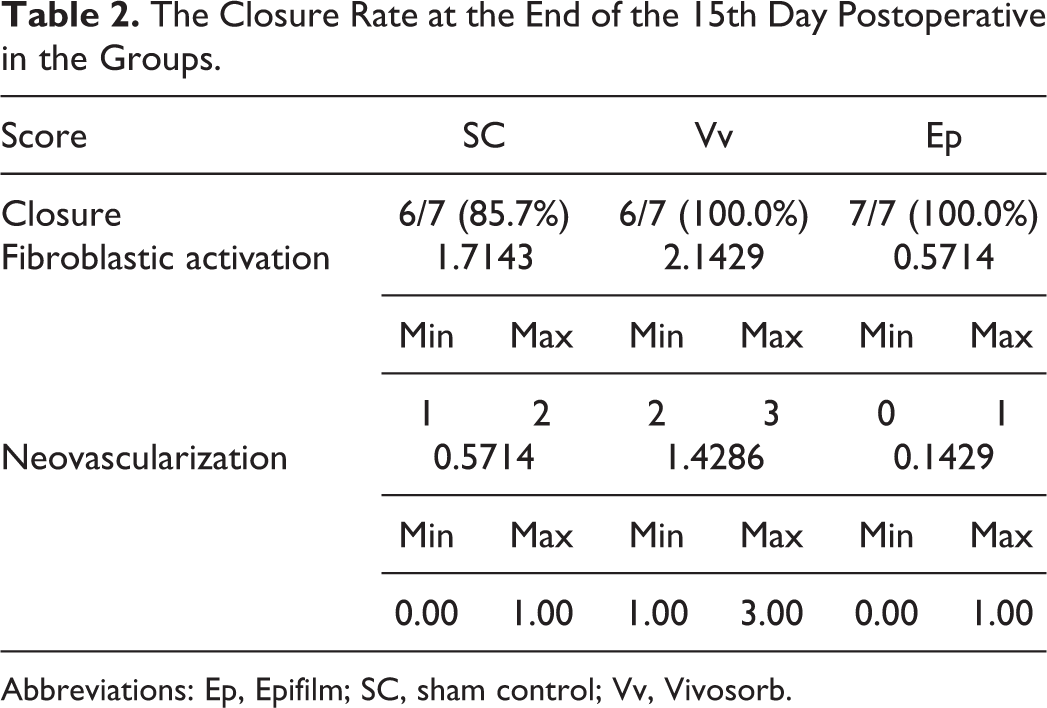
Abbreviations: Ep, Epifilm; SC, sham control; Vv, Vivosorb.
Fibroblastic Reaction
There is no significant difference between the observers in terms of the scores of the fibroblastic reaction (P > .05). The average fibroblastic reaction scores were 2.14 ± 0.37 (+), 0.57 ± 0.53 (+), and 1.71 ± 0.48 (+) in Vv, Ep, and SC groups, respectively. There was no significant difference between the Vv and SC groups whereas significantly less fibroblastic reaction was observed in Ep group compared to the other groups (Table 2).
Neovascularization
There is no significant difference between the observers in terms of the scores of the fibroblastic reaction (P > .05). The average neovascularization scores were 0.14 ± 0.37 (+) and 0.57±0.53 (+) in Ep group and SC group, respectively. There was no statistically significant difference between these 2 groups. Besides the average neovascularization score was 1.42 ± 0.78 (+) in Vv group and it was found statistically significant when compared to the other groups (Table 2).
Discussion
Most of the traumatic TMPs heal spontaneously. 2,4 The healing of the TM generally occurs on the 7 to 10 days following perforation and the healing process fully completes until the 14th day of the perforation. After the trauma, the repair process starts which is thought to be controlled by the epithelial layer. After 48 hours, the epithelial hypertrophy starts and the edges of the TM begin to close, and then these are followed by the development of the fibrous component of the lamina propria. 9 The closure rate of the perforation is affected by many factors. The 2 main factors that affect the recovery of the perforation are the size of the perforation and the secondary developed infections. 10 The small perforations have better closure rates and close earlier as expected. 2 Park et al evaluated 87 patients who had 50% or even larger perforations and compared the steri-strips, paper patches, and spontaneous closure. 3 They found that steri-strips and paper patches had closed earlier however closure rates were not statistically significant among the 3 groups. Orji and Agu reported that 94% of 53 patients aged between 2 and 86 with TM recovered in 12 weeks. They showed that the closure was inversely proportional to the age and the size of the perforation and the location of the perforation did not affect the closure. 5 Amadasum compared the spontaneous closure to the gentamicin application and to the cellophane film patches. While the closure rates of the cellophane film and the spontaneous closure were similar, higher closure rates were observed in both groups compared to the gentamicin group. 7 Huang et al compared the spontaneous closure and the gelfoam patches in 107 patients and found higher closure rate (94.5%) in the gelfoam patch-treated group than the spontaneously healing group (90.4%), however difference was not statistically significant. 2
Vivosorb is a copolymer consisting of poly (lactic acid) and of poly (∊-caprolactone) (PCL). Since they have hydrophilic structures, PCL membranes allow the passage of water which is required for the transport of metabolites from the nutritional control and environmental recovery tissues. Aldini et al used the PCL tubes in a study and recognized only the giant foreign body cells in the surrounding tissues. No local or general toxicity was observed and the regeneration of the nerve fibers was allowed in the lumen. 11 In another study conducted on rabbits it was proved that PCL was biocompatible in the subconjuctival region and could be used safely. 12 The previously performed in vitro studies showed that the PCL membranes were biocompatible with the nerve cells of the tube guides and they facilitated the binding, differentiation, and growth of the nerve cells. 13 -15 Our study was the first study evaluating usability of Vv for otologic surgery in the literature and in terms of the recovery parameters; we found that the fibroblastic reaction and the neovascularization increased significantly in the Vv group compared to the other groups. Also in morphometrical analyses, it was detected that total thickness of the TM in terms of the mesodermal layer indicating fibrosis occurrence in the Vv group. Hence, fibrosis of the TM could negatively affect hearing.
Hyaluronic acid is a polysaccharide which is naturally located within the extracellular matrix of the human tissue and composed of N-acetyl-
Conclusion
In terms of the closure rate of TM, no significant difference was observed among 3 groups. However, Epifilm recovered with a thinner epithelial and fibrous layer comparing to untreated Vv-treated rats. Nevertheless, Vv caused more fibroblastic reaction and neovascularization. As a result, we believe that especially Epifilm is useful than Vv for healing of the traumatic membrane perforation. But, further studies should be done to obtain detailed information about the effect mechanism of these materials.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
