Abstract

Angiosarcoma has a high mortality rate and is encountered infrequently. It most commonly occurs sporadically with the highest incidence in the head and neck. 1 -3 It also can occur in the context of known risk factors including prior radiation therapy. 1 -5 There is a limited number of reported cases of angiosarcoma in the head and neck after radiation therapy. 3 -6 Treatment consists of wide local excision, when anatomically feasible, with possible adjuvant radiation therapy. 1,3,6 Most authors quote 5-year survival less than 35%. 1,4 -6
We present a case of a 72-year-old male who presented to our facility in July 2017 with a chief complaint of shortness of breath. His past medical history included total laryngectomy with left pectoralis major muscle local flap reconstruction for recurrent laryngeal cancer in 2010. He had a primary tracheoesophageal puncture (TEP) placed. His initial laryngeal cancer was treated with cordectomy but unfortunately returned and invaded through thyroid cartilage into his anterior neck. He underwent adjuvant radiation therapy. Specific dosing record of his radiation treatment was not available, but standard adjuvant radiation therapy dosing is at least 60 Gy for head and neck malignancy.
On admission, computed tomography (CT) imaging of his chest revealed bilateral masses, with the largest in the left perihilar region measuring 7.4 cm × 4.9 cm (Figure 1), and bilateral pleural effusions. Pulmonology consulted our service to evaluate his TEP.
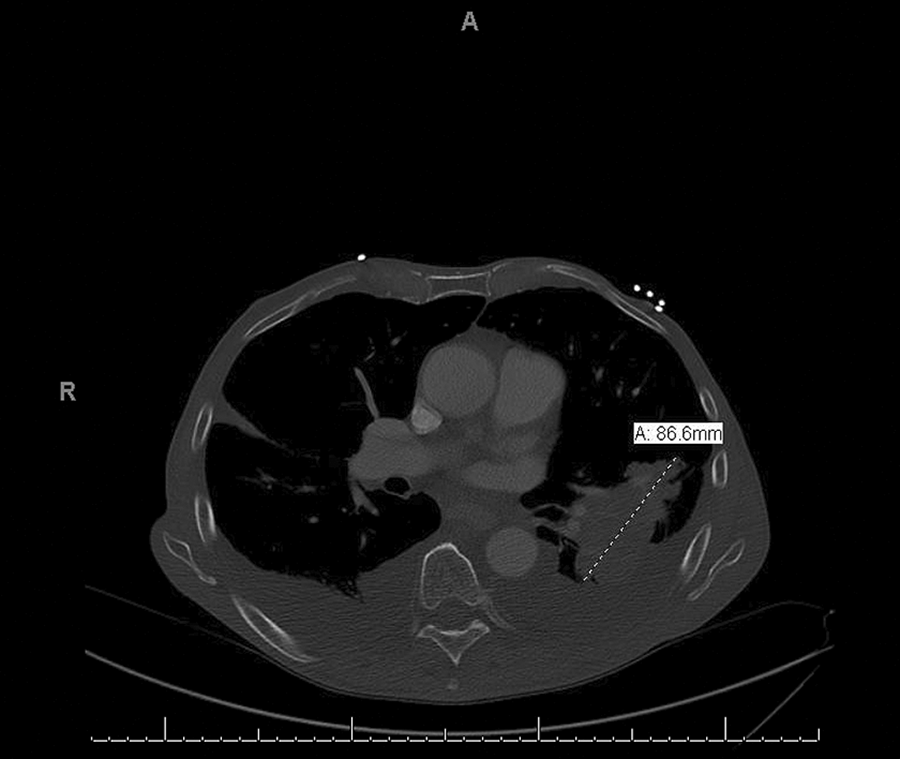
On admission, the patient had bilateral lung masses and effusions. The largest lesion was on the left and is shown here on axial CT image. CT indicates computed tomography.
During the initial consultation, deep purple, raised, firm, neck lesions were readily apparent on physical examination (Figure 2A and B). He reported that they had been present for approximately 2 months and that he had noticed progressive shortness of breath and weight loss over that time. He had not sought medical attention prior to his emergency department presentation. A bedside incisional biopsy was performed without complication. Pathology revealed low grade, angiosarcoma with immunohistochemical staining positive for vascular markers CD31 and CD34 which highlight the vascular proliferation within the dermis. Hematoxylin and eosin preparations revealed an intradermal infiltrate of atypical vessels with irregular anastomosing profiles and nuclear atypia.
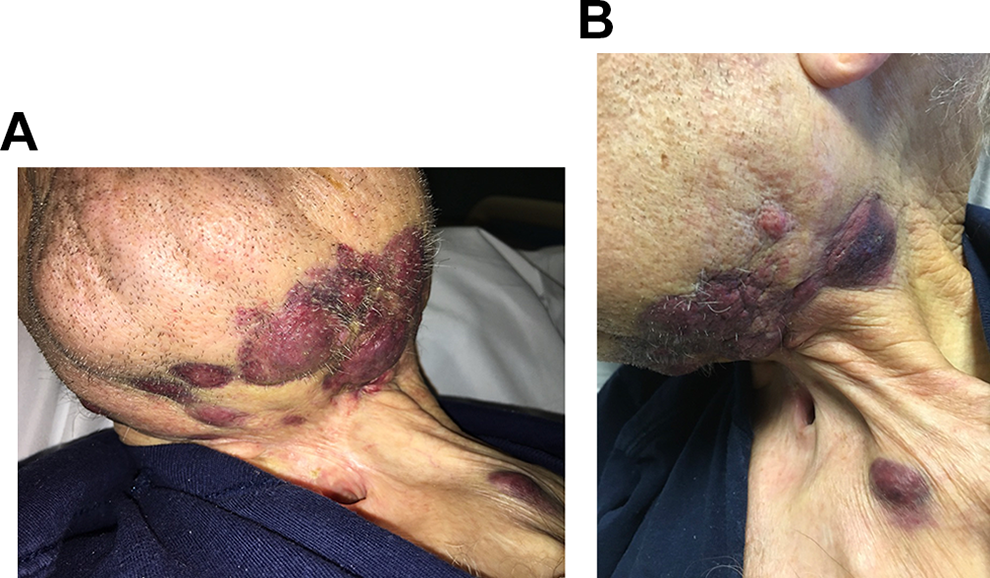
A, Large cutaneous angiosarcoma present on the patient’s left neck and supraclavicular region. His laryngectomy stoma is visible. B, Lateral view of patient’s left neck with angiosarcoma and laryngectomy stoma visible.
Neck CT revealed a 5.4 cm × 5.3 cm × 4.5 cm vascular mass in the left submandibular region and a 3 cm × 2.2 cm × 2.2 cm mass to the left of the stoma (Figure 3). Computed tomography of the chest was unchanged and no adenopathy nor masses were identified in neither the abdomen nor pelvis. The patient elected to be discharged home on comfort measures only. He died within a month of discharge.
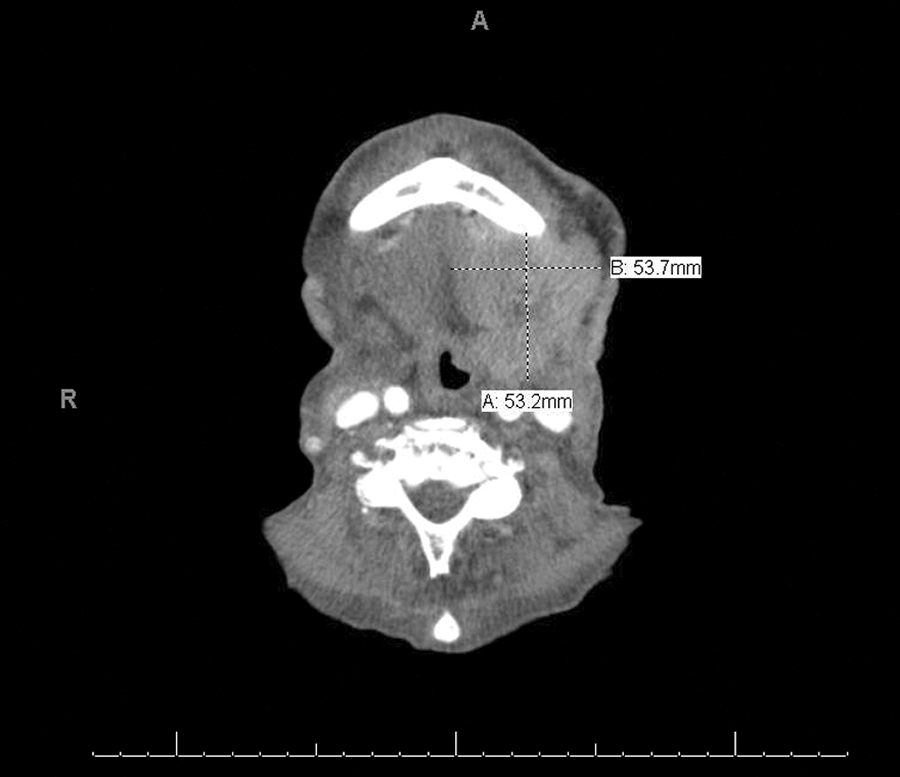
Angiosarcoma seen on axial CT images of the neck in the left submandibular region. CT indicates computed tomography.
Angiosarcoma is an aggressive malignant proliferation of endothelial cell origin that can arise from vascular or lymphatic vessels. They represent a subset of about 5.4% of all cutaneous soft tissue sarcomas. 1 The incidence has increased in the last 30 years and may be due to increased use of radiation therapy, longer survival after treatment, and better surveillance. 1 The majority of angiosarcomas arise spontaneously. Known risk factors include radiation therapy, chronic lymphedema, chemical exposure, and a limited number of familial syndromes. 1 -5 Elderly patients, white men in their eighth decade of life, are at increased risk of developing an angiosarcoma.1 Although 50% of angiosarcomas arise in the skin and soft tissue of the head and neck, most commonly on the scalp, only 0.1% of head and neck malignancies are angiosarcoma. 2
Survival is widely reported to be poor with a 5-year survival rates ranging from 10% to 35%. 1, 4–6 Pulmonary metastasis is the most common cause of death. 5 Treatment consists of wide local excision, when possible, with adjuvant therapy. Various combinations of chemotherapy and radiation therapy have been described for metastatic disease.1–5
This case underlies the importance for long-term follow-up for patients with cancer. It also demonstrates the need for proper patient education to seek medical evaluation of any new lesions or atypical symptoms that arise after cancer treatment, particularly in the irradiated field. Furthermore, a low threshold for biopsy is necessary for any atypical lesions followed by radiographic staging if pathology returns malignant.
Footnotes
Authors’ Note
Poster Presentation at UPMC Hamot Research Days April 11-12, 2018.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
