Abstract

A 45-year-old male presented to our clinic with known vascular lesions in the tongue, lip, and larynx. His lesions had been noticed for 4 years. He had experienced bleeding 1 to 2 times per month, usually due to biting the lesion in his tongue. The bleeding responded to pressure. There was no history of swallowing problems or airway compromise. He had undergone vascular malformation excision for lower back 9 years previously, and he had no other relevant medical history. On physical examination, he had soft contour abnormalities in the left neck and submental area consistent with the known underlying venous malformations (VMs). The findings were subtle and apparent only because of the knowledge that there was an underlying vascular anomaly. Laryngeal examination showed a purple mass arising from the laryngeal ventricle. The nasopharynx and hypopharynx did not have any lesions or masses. An outside magnetic resonance imaging of the neck dating back 18 months prior to presentation revealed multiple lesions in the neck and tongue with very slow flow, and the morphology was consistent with VMs. Many of these malformations were in locations that do not cause any apparent problem.
The main lesions of concern were located in the right retropharyngeal region and the right ventricle, as well as 2 right tongue lesions. The most symptomatic site was the tongue, which demonstrated 2 soft, nontender lesions, less than 1 cm in size. The patient also had long-standing hoarseness. Surgical therapy had not been offered previously because of the relatively mild symptoms that the laryngeal lesions were causing. However, the patient was interested in treatment and was therefore referred to the interventional radiology department in our institution to discuss minimally invasive sclerotherapy. His greatest fear was the possibility of bleeding from the laryngeal lesion, and he was afraid that he could have an airway emergency.
He was consented for the surgery including the possibility of an emergency tracheotomy. We decided to proceed with direct injection sclerotherapy under a combined otolaryngology/interventional radiology approach. He underwent microsuspension direct laryngoscopy. The lesion located in the right ventricle (Figure 1) under the microscope was punctured with a 21-G butterfly needle by the laryngologist (Figure 2). Subtraction venography was done to understand the venous drainage and assess adequacy of the needle access. Satisfactory needle placement was followed by administration of ethanolamine oleate 5% (Ethamolin; QOL Medical, LLC, Vero Beach, Florida) thoroughly mixed with air to prepare a sclerosant foam. Laryngoscopic observation of the foam replacing the blood in the abnormal venous spaces indicated completion of the treatment.
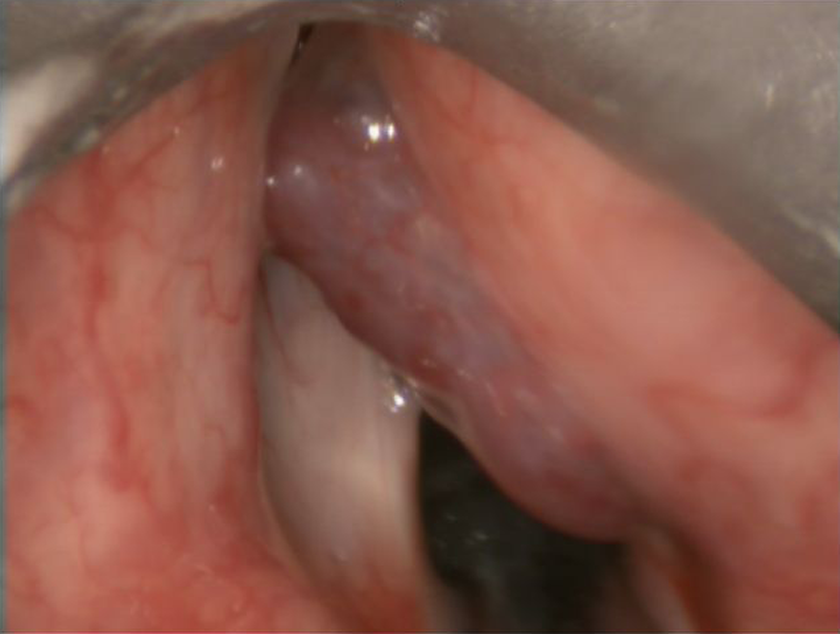
The intraoperative view of the vascular lesion in the right laryngeal ventricle.
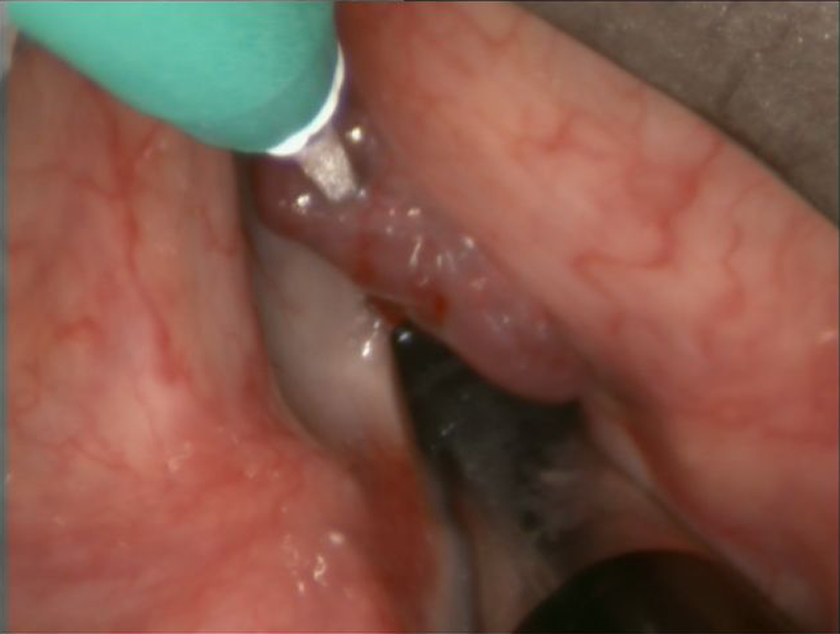
The ethanolamine was introduced with a 21-G butterfly needle to the lesion.
Discussion
Venous malformations are the most common slow-flow vascular malformations in the head and neck region. 1 They might occur anywhere in the body and show a predilection to the head and neck region. 2 When found in the upper airway, the patient might present with stridor, hoarseness, and difficulty breathing in the supine position. In such cases, the lesion itself or oozing/bleeding from the lesion might cause airway obstruction which might end up with life-threatening events. Thus, VMs involving the upper airway mandate prompt diagnosis and treatment. 3
Treatment of vascular malformations depends on the stage and type of the lesion. 4 The main treatment options include sclerotherapy, surgery, laser treatment, and embolization. 4 A clinical guideline for the treatment of vascular malformations is lacking. Optimal treatment is controversial, and these lesions often require a combination of treatments.
Sclerotherapy has been used as an adjunct or alternative to surgery. Several sclerosing agents are available including absolute ethanol, ethanolamine oleate, 5 sodium tetradecyl sulfate, 6 polidocanol, 7 bleomycin, 2,8 and OK 432, 9 and all have been reported to be effective. Currently, there is no consensus on the best sclerosing agent. Absolute ethanol is thought to be the most potent but also the agent most likely to be associated with complications such as soft tissue necrosis, sloughing, and nerve injury. Other sclerosants lack the same potency but are associated with less morbidity and postoperative swelling and pain. Edema is the most concerning local side effect in an upper airway lesion for all agents. In our case, ethanolamine oleate was chosen to minimize laryngeal edema and possible ulceration of the laryngeal mucosa that are more likely to occur when absolute ethanol is used.
Reports of laryngeal vascular lesions treated with sclerotherapy under direct laryngoscopy are scarce in the literature. In patients with laryngeal venous lesions, the management should be in cooperation with the anesthesiology team. The patient should be consented beforehand and all of the team members should be ready for urgent tracheotomy during the management of these lesions. Close follow-up of the patient in the immediate postoperative period is crucial.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
