Abstract
The aim of this study is to review the prevalence of adverse reactions to cross-linked hyaluronic acid (HA) following injection laryngoplasty and discuss possible mechanisms. A retrospective chart review of patients who underwent injection laryngoplasty using HA was conducted. Demographic data included age, gender, etiology, site of injection, and amount injected. Adverse reaction was diagnosed by the presence of inflammatory reaction at the injection site. A total of 63 patients were included, divided into 41 males and 22 females with a mean age of 51.76 years. The most common etiology was vocal cord paralysis (n = 53), followed by postcordectomy, puberphonia, and vocal fold atrophy and bowing. The average amount injected was 0.56 (0.22) mL. Three cases out of 63 patients developed an adverse reaction and presented with airway symptoms, namely, progressive shortness of breath and globus 2 to 3 days postinjection. Adverse reactions following HA injection laryngoplasty may occur with life-threatening symptoms.
Introduction
Injection laryngoplasty is a commonly performed procedure for the treatment of glottic insufficiency. 1 Since its inception, several synthetic and biological injectable materials have been in use with various viscoelastic properties and duration of resorption. There is consensus that the ideal injectable substance must be biocompatible, readily available, offers the longest period of relief, and easy to use. 2,3 To that end, hyaluronic acid (HA) has gained marked popularity in view of its favorable properties as a naturally occurring component of the extracellular matrix of the lamina propria 2,4,5 and in view of its low rate of complications. 3,6
Since it became available in a commercial form (Restylane Q-Med AB, Uppsala, Sweden) and in more purified nonanimal forms, 7,8 HA has been commonly used with a very low incidence of adverse reactions that ranges between 0.06% and 0.08%. 7,9 Despite this low rate of reaction, there has been growing evidence of complications following its dermal use, namely, local erythema, angioedema, 10 granuloma formation, 11 ulceration, and tissue necrosis at the injection site. 12 More recently, mild adverse reactions to HA have been reported following injection laryngoplasty. Hertegård et al, in 2 studies on the safety of cross-linked hyaluronan as an augmentation substance for glottic insufficiency, have reported inflammatory reactions at the injection site in 3 patients, 2 of whom complained of hoarseness and cough but none had shortness of breath. 5,13 Similarly, Reiter and Brosch, in their study on the effectiveness of injection laryngoplasty using cross-linked HA in 19 patients with unilateral vocal cord paralysis, reported a case of edema of the false vocal fold and aryepiglottic fold at the site of injection 3 days after the procedure without any associated dyspnea. 14
More severe side effects with life-threatening sequel have also been described by a few. 8,15 -17 Halderman et al in their study on the safety and length of benefit of HA in injection laryngoplasty have reported 5 cases of adverse reaction out of 64 patients. Of those 5 cases, 2 had subepithelial plane injection of HA, 1 had recurrent atrial fibrillation at the end of the procedure, 1 had shortness of breath several hours after injection, and 1 developed hematoma of the arytenoid, aryepiglottic fold, and true vocal fold ipsilateral to the injection. 15 Shamanna and Bosch reported the case of a 53-year-old female who developed a severe compartment syndrome–like reaction after HA injection that resulted in ulceration and necrosis with eventual tracheostomy dependence. 7 Similarly, Dominguez et al, in their study on the rate of inflammatory reaction to HA in injection laryngoplasty (245 vocal folds were injected with HA in 186 patients), have reported 4 cases of severe reactions associated with dyspnea out of a total of 7 patients who had inflammatory reactions at the injection site. 16
In keeping with the aforementioned, the authors of this article have previously reported a case of a 23-year-old female with idiopathic pulmonary hypertension who underwent injection laryngoplasty with cross-linked HA for left vocal fold paralysis and subsequently developed severe edema of the left arytenoid, false vocal fold, and aryepiglottic fold with associated shortness of breath 2 days after the injection. 17
The purpose of this study is to cast more information on this subject by reviewing the prevalence of adverse reactions to cross-linked HA following injection laryngoplasty performed on 63 patients with glottal insufficiency. The possible mechanisms behind these adverse reactions will be discussed.
Patients and Method
After having obtained the institutional review board approval, a retrospective chart review of all patients who underwent injection laryngoplasty using HA during the period extending from June 2010 till August 2016 was conducted. A total of 63 patients were identified and enrolled in this study. All patients underwent injection laryngoplasty using cross-linked HA in the office under local anesthesia using the fiberoptic transnasal or transoral approach. 18,19
Demographic data included age, gender, etiology, site of injection, and amount injected. Adverse reaction to cross-linked HA was diagnosed by the presence of inflammatory reaction at the injection site or adjacent laryngeal structures, in the form of edema and/or erythema.
Statistical Method
Descriptive statistics was used to compute the means and the standard deviation of the continuous variables and the frequencies of the categorical variables. Statistical analysis was performed using IBM SPSS Statistics for Windows, version 22 (IBM Corp, Armonk, New York, Released 2013).
Results
Demographic Data
A total of 63 patients were included in this retrospective chart review. These were divided into 41 males and 22 females. The mean age of the total group was 51.76 years, with a range of 15 to 86 years. The most common etiology was vocal cord paralysis (n = 53), postcordectomy (n = 4), puberphonia (n = 4), and 2 cases of vocal fold atrophy and bowing. The injection material for augmentation used in all patients was cross-linked HA (Restylane Q-Med AB). The average amount injected was 0.56 (0.22) mL, with a range of 0.1 to 1.00 mL. The most commonly injected site was the left (n = 31), with bilateral injection being performed in 16 of the 63 cases (see Table 1).
Demographics.

Reaction to HA
Three cases of a total of 63 patients developed adverse reaction to the augmentation material used (cross-linked HA). Further description of these cases is illustrated below.
Case #1
A 23-year-old female with past medical history of idiopathic pulmonary hypertension presented with symptoms of hoarseness, vocal fatigue, aspiration, and dysphagia of 6 months duration. Perceptual evaluation showed grade 3 dysphonia with mild breathiness. Transnasal flexible laryngoscopy revealed left vocal cord paralysis in the paramedian position with signs of glottal insufficiency. Patient underwent office-based injection laryngoplasty of the left vocal fold with 0.7 mL of cross-linked HA (stabilized 20 mg/mL) via a fiberoptic 19-G needle under local anesthesia using the transnasal fiberoptic approach. The injection was made lateral to the vocal process and the procedure was well tolerated by the patient. Two days after the injection, the patient started complaining of progressive shortness of breath, dysphagia, and globus sensation, which eventually led her to the emergency department. Fiberoptic laryngoscopy revealed severe edema of the left arytenoid, false vocal fold, and aryepiglottic fold. Subsequently, the patient was started on intravenous dexamethasone, inhaled racemic epinephrine, and intravenous amoxicillin–clavulanic acid. Few hours after initiation of treatment, her symptoms improved and fiberoptic laryngeal examination revealed marked decrease in the extent of edema. Patient was monitored for 24 hours and was discharged afterward on prednisone 20 mg orally twice daily to be gradually tapered. Follow-up 10 days later revealed normal laryngeal examination with complete glottal closure during phonation.
Case #2
A 51-year-old healthy male sustained a motor vehicle accident, resulting in multiple extremity and facial fractures. He underwent multiple surgeries for his fractures along with a tracheostomy. Following extubation, the patient had aspiration and dysphagia. Flexible laryngoscopy revealed left vocal fold immobility with incomplete glottal closure. The patient eventually underwent injection laryngoplasty of the left vocal fold with 0.6 mL of cross-linked HA via the same approach described in case #1. On postoperative day 3, the patient presented with globus sensation and mild throat pain. Flexible laryngoscopy revealed left arytenoid edema extending to the aryepiglottic fold, but with no airway impediment. Patient was managed on an outside basis and was discharged on Augmentin 1 g orally twice daily for 10 days and prednisone 40 mg orally daily to be tapered over 5 days. Regular follow-up revealed significant decrease and eventual complete resolution of the endoscopic findings.
Case #3
This is the case of a 54-year-old female nonsmoker who underwent total thyroidectomy and parathyroidectomy in outside hospital complicated with bilateral vocal cord paralysis necessitating tracheostomy 1 year prior to presentation. In May 2017, patient presented to the Hamdan Voice Unit for further assessment and laryngeal endoscopic examination revealed bilateral vocal cord paralysis in the paramedian position. In July 2017, the patient was offered right transoral laser cordectomy in the office and was successfully decannulated 1 week later. On close follow-up in clinic, patient started complaining of dysphonia. Perceptual evaluation revealed grade 3 dysphonia with moderate breathiness, and laryngeal video-endo-stroboscopic examination revealed fixed vocal folds in the paramedian position with incomplete vocal fold closure on phonation with evidence of glottal gap. Subsequently, patient underwent right vocal fold augmentation using the transoral fiberoptic injection technique under local anesthesia as an in office procedure in February 2018. A total of 0.4 mL of cross-linked HA were injected posteriorly without compromising the airway. Patient’s voice markedly improved after the injection with no change in respiratory effort. Two days following the injection, patient started complaining of shortness of breath. Laryngeal video-stroboscopic examination revealed edema and redness of the right true and false vocal folds (see Figure 1). Patient was started on prednisone and was kept under observation for 48 hours till the edema and redness subsided completely. One week postinjection, the patient reported marked improvement in voice quality with no dyspnea or aspiration and laryngeal endoscopic examination revealed good glottal opening.
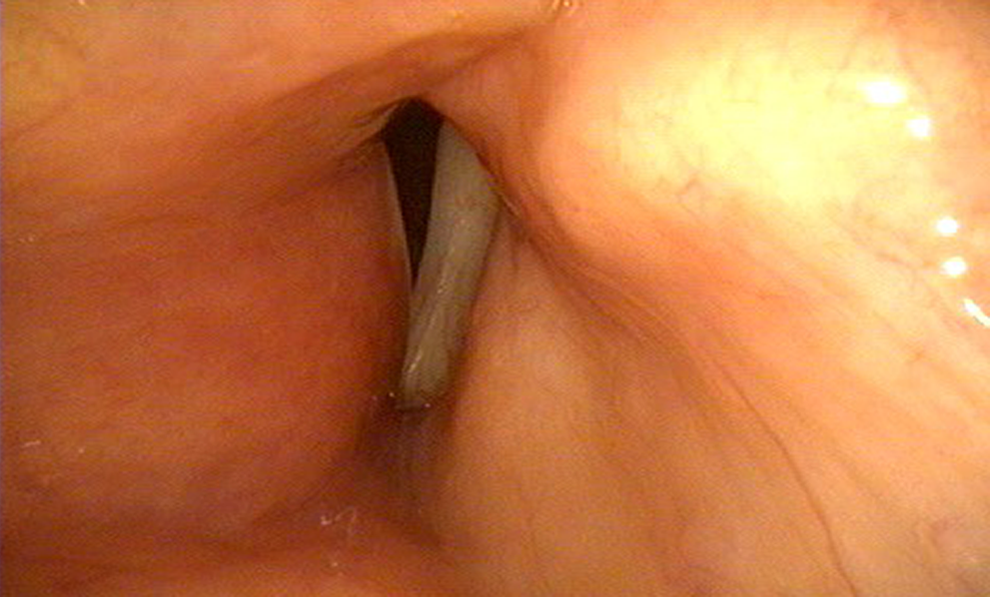
Flexible fiberoptic endoscopy revealing erythema and swelling of the right false vocal fold 2 days postinjection laryngoplasty.
Discussion
Hyaluronic acid is commonly used as a filling material in injection laryngoplasty. The results have been promising in view of its slow absorption rate, resistance to migration, and its ability to preserve the viscoelastic properties of the vocal cords. Despite the fact that HA used for injection is a biomedically engineered product, its usage carries some adverse effects ranging from mild hypersensitivity reactions, to odynophagia and airway obstruction. 3 -17 Based on this review of 63 cases of injection laryngoplasty using cross-linked HA, the rate of complications was 4.76%, which is comparable to the rates reported in previous publications. 13 -16 The clinical picture varies from minor side effects to life-threatening conditions as described in 2 of the 3 patients reported in this article. The most common symptoms are hoarseness, lump sensation in the throat, difficulty in swallowing, shortness of breath, and dyspnea. These symptoms are associated with various laryngeal findings, such as, edema of the false vocal fold, edema of the aryepiglottic fold, hematoma of the vocal fold, ulceration, and necrosis. In 2 of our patients, shortness of breath was the major complaint and was attributed to edema of the false fold and aryepiglottic fold.
Several theories have been described in an attempt to uncover the etiology of these reactions. A leading theory is local hypersensitivity to HA, with the sensitivity being attributed to the fermenting bacteria (streptococci) in the manufacturing process. This latter yields a certain amount of bacterial proteins that are considered as impurities by the microbiological engineering techniques. 2,8,14 What is not in favor of the hypersensitivity reaction theory is the normal level of immunoglobulin E (IgE) and IgG antibodies measured in patients injected with HA. 15 Histological behavior of vocal folds injected with HA in animal studies has shown mild inflammation but no cell-specific preference that would lean toward a hypersensitivity reaction. 20 What further opposes this theory is the longevity of the reaction and its unilaterality. In a study by Dominguez et al, the postinjection reaction lasted over 26 months, which refutes the possibility of hypersensitivity as HA lasts up to 6 months. In another case, the reaction to HA was unilateral while the patient had injection bilaterally. 16 Another theory behind the reported adverse reaction to HA is vascular compression or occlusion by the injected material. What is against this theory is the small diameter of the vessels in the human vocal fold and the lack or rarity of epithelial necrosis at the injection site. 21 A third possible theory that has been thoroughly discussed by several authors is contamination of the injector device. 13,16 This kind of reaction is not seen in other materials like steroid injections as these are injected at the superficial layer of the folds unlike HA that requires to be injected deeper in order to achieve the desired effect. Further evaluation using tissue culture is needed to substantiate this theory.
This study emphasizes the importance of diligent follow-up of patients undergoing injection laryngoplasty using HA and has deterred many from using it. In keeping with the aforementioned, this study alludes to the need for preventive measures and diligent follow-up of patients undergoing injection laryngoplasty. Preventive measures to reduce adverse reactions to HA must take into consideration both the type of molecule used and the technique adopted in injection. Selection of the right size of HA cross-linked particle, which can range between 20 and 1000 μm, may be an important factor in reducing the rate of vascular occlusion, which is one of the suggested hypothesis in the pathogenesis of these adverse reactions. 22 Moreover, recommendations advocated to prevent or reduce the rate of complications in dermal filler injections may well be adopted in injection laryngoplasty. These include the usage of small needles that can halt the speed of injection and the avoidance of overinjection because large injected volumes may compress neighboring vessels and lead to pressure necrosis. Other recommended measures may include voice rest and abstinence from high or low thermal ventilatory stimuli, as the latter has been incriminated in the exacerbation of inflammatory reactions following dermal filler injections. 23,24 The high rate of adverse reaction reported, similar to the rates previously described following the usage of Bovine collagen in the early 1980s and which has prompted skin testing prior to its usage, suggests to the need for skin testing. Although not recommended in facial injections, skin testing may be considered in injection laryngoplasty given the potential compromise in airway should a hypersensitivity reaction occur. 25
Worsening of the laryngopharyngeal signs and symptoms despite conservative medical treatment and close observation in patients with adverse reaction to HA should prompt the use of hyaluronidase. Similar to the benefits observed following its usage in the treatment of early complications of filler injections, hyaluronidase may be beneficial in reducing the surrounding edema and pressure on occluding vessels. 22 Nevertheless, hyaluronidase injection must be avoided early in the course of the reaction when infection is suspected because any manipulation of the infected field may cause further spread of the infection.
This study carries a main limitation and that is skin testing for HA to confirm the hypersensitivity reaction, which is the most plausible explanation for the occurrence of the adverse reaction. To that end, prior skin testing can be offered as an alternative to the close follow-up in patients undergoing the injection of this material, as discussed previously.
Conclusion
This review casts more information on a relatively poorly discussed topic in the literature, namely, the adverse reaction to HA. Despite the introduction of new form of HA with lower traces of proteins compared to the forms previously used, 19 adverse reactions following injection laryngoplasty still occur with life-threatening symptoms. The recommendation of the authors is close observation of patients for a period of 24 hours following the injection. Symptoms such as lump sensation in the throat, dysphagia, and/or shortness of breath should alert the physician for possible reaction to the injectable material and should prompt early therapeutic intervention.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
