Abstract

Extracranial schwannomas are uncommon neoplasms arising from the peripheral nerve sheath. Prior reports have listed the lack of a capsule as a distinctive feature of schwannomas of the sinonasal tract. We report a case of an encapsulated schwannoma arising in the nasal sidewall.
A 21-year-old male with no significant past medical history presented to clinic with a 3-year history of progressive right-sided nasal obstruction. Physical examination revealed a firm subcutaneous mass and visible deformity of the right nasal sidewall (Figure 1). His computed tomography scan demonstrated a 2.0 cm × 1.5 cm × 1.7 cm mildly enhancing mass in the right lateral nasal wall with central hypointensity and no apparent septal or bony involvement (Figure 2).
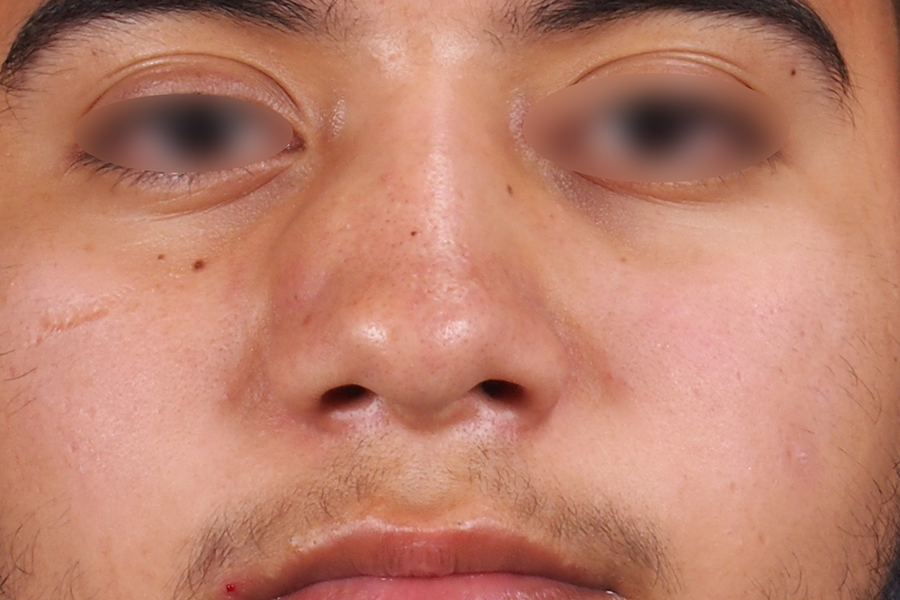
Photograph demonstrating the right nasal sidewall deformity.
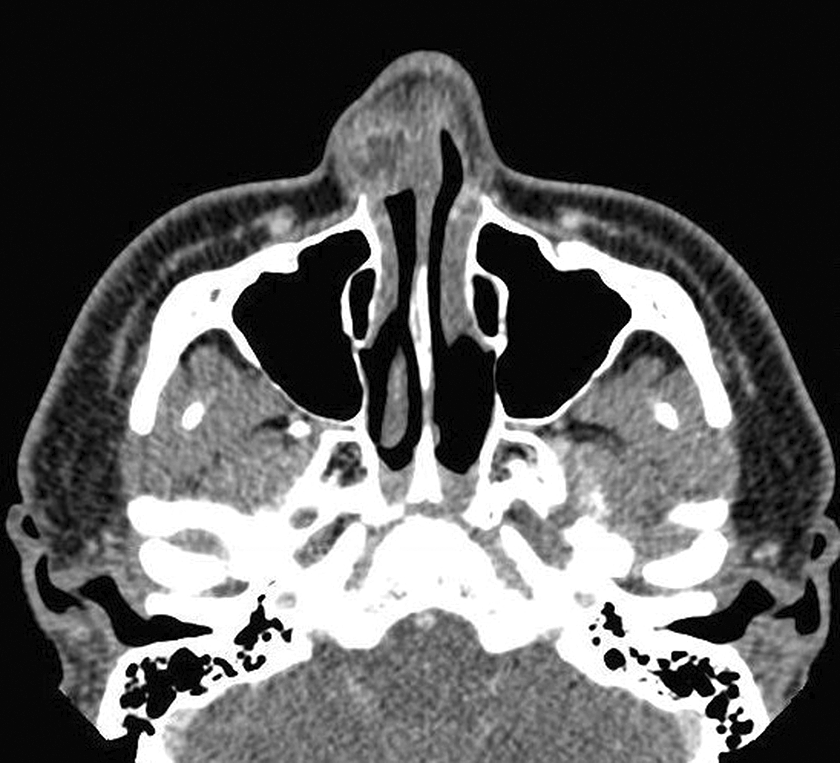
CT scan, axial slice demonstrating a mildly enhancing mass in the right lateral nasal wall. CT indicates computed tomography.
The patient was taken to the operating room for resection and reconstruction using an open septorhinoplasty approach. The right upper lateral cartilage (ULC) was collapsed but intact, and the scroll region had been separated. A spreader graft was used to support the right nasal valve, and the ULC was resuspended to the midvault. The lower lateral cartilage was sutured to the caudal edge of the ULC. A columellar strut was also used.
On gross examination, the mass was gelatinous, yellow-gray, and appeared encapsulated. Histologic examination revealed a well-encapsulated schwannoma (Figure 3). At 6-month follow-up, his nasal obstruction had resolved, there was excellent nasal sidewall symmetry, and there was no evidence of recurrence.
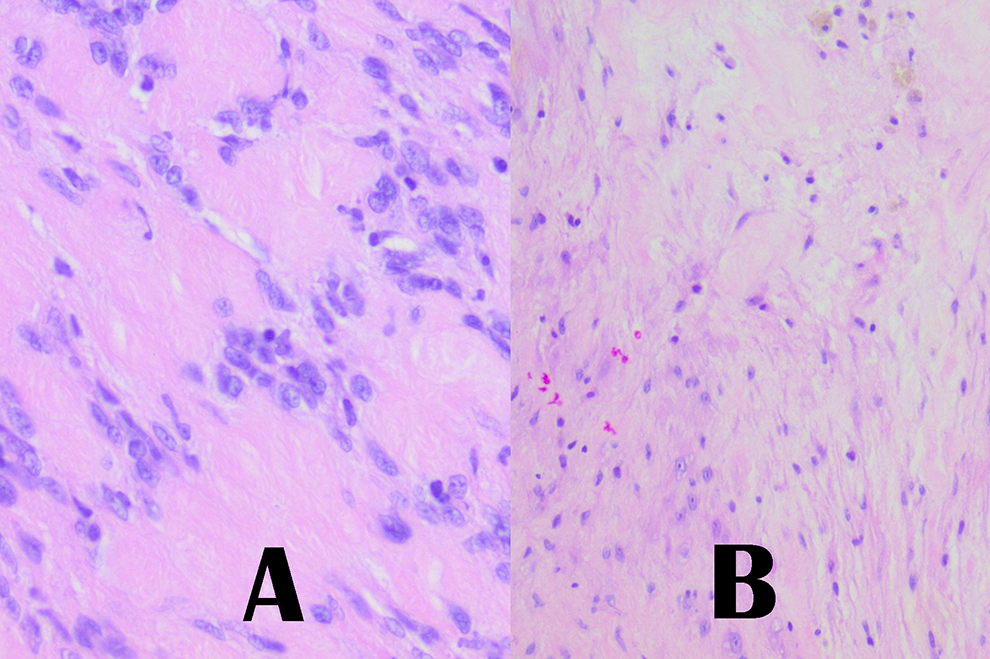
Tissue specimen with H&E staining demonstrating (A) Antoni A morphology at ×40 magnification and (B) Antoni B morphology at ×20 magnification. H&E indicates hematoxylin and eosin.
Discussion
Schwannomas are rare benign tumors that arise from Schwann cells, which compose the myelin layer of the peripheral nerve sheath. Although the true incidence is unknown, in a study at one of the largest medical centers in the United States, only 85 schwannomas were diagnosed over a 20-year period at all head and neck sites (excluding skin and the acoustic nerve). 1
Schwannomas may occur in any myelinated nerve, with a predilection for the sympathetic trunk and cranial nerves. Most tumors arise in individuals between 40 and 60 years old with equal frequency in either sex. 1,2 The most commonly diagnosed sites are neck soft tissue, parapharyngeal space, and oropharynx. 1 Reports of schwannomas limited to the nasal cavity are exceptionally rare, with approximately 16 reported cases in the literature. 2
Definitive diagnosis of schwannoma requires a tissue specimen, which demonstrates the classic histologic features; a heterogeneous appearance with areas of densely packed spindle cells with palisading nuclei surrounding acellular verocray bodies (Antoni A) and hypocellular areas with loose spindle cells in a myxoid stroma. 3
A classic feature of head and neck schwannomas is a well-defined capsule, with the exception of tumors of the nose and paranasal sinuses, which have been reported in all prior cases, with one exception, as being acapsular. 1 -4 Other authors have theorized that the lack of a capsule could be attributed to these tumors deriving from autonomic nerves of the sinonasal mucosa which lack perineural cells. 3 In contrast, our patient was found to have an encapsulated tumor; to our knowledge, this is only the second reported case of an encapsulated sinonasal schwannoma. 1 -4 In contrast to our patient who had a lateral sidewall soft-tissue mass, the other case of an encapsulated sinonasal schwannoma presented with a pedunculated intranasal mass. 4
Footnotes
Authors’ Note
This article was presented at the American Academy of Facial Plastic and Reconstructive Surgery Annual Meeting, October 2018, Dallas, TX, USA.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
