Abstract
Ear, Nose & Throat Journal's Web site is easy to navigate and provides readers with more editorial content each month than ever before. Access to everything on the site is free of charge to physicians and allied ENT professionals. To take advantage of all our site has to offer, go to www.entjournal.com and click on the “Registration” link. Once you have filled out the brief registration form, you will have full access. Explore and enjoy!
Inverted papilloma is a benign epithelial tumor of the nasal cavity. It is known to coexist with malignancy in 5 to 13% of cases, with squamous cell carcinoma being the most common malignancy. Another associated malignancy, one that is extremely rare, is verrucous carcinoma. To the best of our knowledge, no case of verrucous carcinoma occurring alone or in association with another neoplasm has been described in the nasolacrimal system. We report a case of synchronous verrucous carcinoma and inverted papilloma of the lacrimal sac in a 47-year-old man. The patient presented with epiphora, nasal obstruction, swelling of the left medial canthus, and drainage of a foul-smelling fluid from the left nostril. Computed tomography and magnetic resonance imaging detected the presence of a large mass occupying the left nasal cavity and sinuses with extension into the nasopharynx. In addition, bony invasion of the anteroinferomedial wall of the left orbit was noted with extension of the tumor into the orbit itself, which resulted in lateral displacement of the left medial rectus muscle. The patient underwent endoscopic debulking of the left sinonasal lesion. Of note, the surgery had to be completed in stages because of excessive blood loss. Histopathologic examination of the intranasal component of the tumor identified it as an inverted papilloma. One month after the intranasal resection, a left dacryocystectomy was performed; histopathologic examination revealed that an invasive verrucous squamous cell carcinoma had arisen within the inverted papilloma.
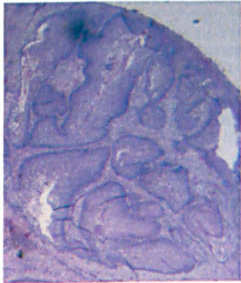
Esthesioneuroblastoma (ENB) is a rare tumor of the olfactory mucosa. We treated a 50-year-old man with an ENB in the right ethmoid sinus who had been diagnosed 16 years earlier with syndrome of inappropriate antidiuretic hormone secretion (SIADH) of unknown cause. When the ENB was surgically removed, the patient's osmoregulation returned to normal—that is, his SIADH resolved completely, which suggested that the SIADH was paraneoplastic in nature. These events prompted us to review the literature to determine if there is an association between our patient's ENB and his SIADH in general and between long-standing SIADH that precedes ENB in particular. Based on our review and an extrapolation of data, we have estimated that 1,300 cases of ENB have occurred since it was first described in 1924. Of these cases, SIADH was reported in 26 cases, including ours, which represents an estimated prevalence of 2% (although we believe this is actually an underestimation of the true prevalence). Of the 26 cases, SIADH had already been present in 14 patients (54%) prior to their diagnosis of EBN for a median duration of 3.5 years. We recommend that patients with newly diagnosed EBN be evaluated for SIADH. In those who are SIADH-positive, a resolution of SIADH should be expected once the ENB has been removed. If this does not occur, one should suspect that the ENB was not completely removed. If SIADH resolves but later recurs during follow-up, then a relapse should be suspected. In long-standing SIADH of unknown etiology, nasal sinus imaging should be considered.
Reports of delayed presentation of foreign bodies in the frontal sinus are infrequent and likely to become rarer with the widespread availability of computed tomography in the last 2 decades. We present a case in which glass from a road traffic injury was found in the frontal sinus, causing symptoms of frontal sinusitis 28 years after the initial injury. We also present a review of the literature.
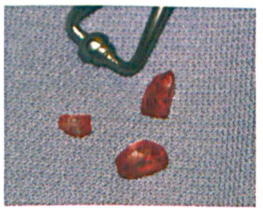
Paraneoplastic syndromes include a variety of disorders that affect the neurologic, endocrine, mucocutaneous, hematologic, and other systems as a result of neoplastic disease. Although their presentations vary, syndromes occur when tumor antigens exhibit cross-reactivity to similar antigens expressed by these systems. The antigens in the nervous system are called “onconeural” antigens. Although many disorders are associated with a comparatively high incidence of paraneoplastic neurologic syndromes, only a few cases have been associated with squamous cell carcinoma (SCC) of the tonsil. We report the case of a 69-year-old man who initially presented with weakness and spastic gait. He was subsequently found to have a characteristic paraneoplastic tractopathy on thoracic magnetic resonance imaging. The subsequent workup and operative intervention identified a T2N0M0 SCC of the tonsil. Following resection, the patient's overall symptoms were significantly alleviated, and his gait improved. A thorough literature search yielded no other report of a tonsillar SCC with associated paraneoplastic thoracic spine tractopathy.
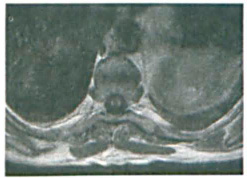
We present a case of diffuse sphenoid bone cavernous hemangioma in a 22-year-old primigravid woman. Her disease first manifested clinically as progressively decreasing vision in her left eye during her third trimester of pregnancy. We also discuss the known causes and some theoretical causes of cavernous hemangioma enlargement during pregnancy.
Hoarseness is a common presenting symptom in patients referred to the otolaryngology clinic. An arteriovenous malformation (AVM) in the neck is a previously unreported cause of hoarseness. We describe the case of a 61-year-old woman who presented with hoarseness and vocal fold paralysis, which was caused by an AVM. She was successfully treated with endovascular embolization. Devascularization of the AVM resulted in symptomatic relief of the hoarseness and resolution of the vocal fold paralysis, presumably secondary to interval reduction in edema and venous congestion.
We report 3 cases of rare, life-threatening intracranial and internal jugular vein (IJV) thrombosis that were caused by common ENT infections. These infections included otitis media in a 6-year-old girl, tonsillitis in a 21-year-old woman, and odontogenic sepsis in a 56-year-old woman. All 3 patients were treated with culture-directed systemic antibiotics; 2 of them also required surgical drainage (the child and the older adult). The 2 adults also received therapeutic anticoagulation, which was continued until venous recanalization was documented; the duration of combined antibiotic and anticoagulation treatment was 6 weeks. All 3 patients made uneventful recoveries. Significant morbidities associated with intracranial and IJV thrombosis were avoided as a result of prompt diagnosis and judicious treatment.
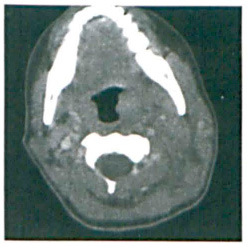
A frontocutaneous fistula is a rare sequela of frontal sinus pathology. Management via an endoscopic approach is not frequently reported in the literature. We describe such an approach with the aid of still photography and imaging plus videoendoscopy, and we discuss the current literature.
