Abstract
This article speaks to ongoing sociological debate around the fast-changing organisation of medicine and the implications for skills utilisation – with a specific focus on community pharmacy. While the professional status of pharmacists has been the subject of much debate, the closely related theme of skills deployment has been significantly overlooked. Any coverage of skills has largely been restricted to the deskilling effect of technology; analysis of the role other contextual factors might play has been piecemeal and fragmented. Drawing on qualitative data, this article aims to offer a more nuanced view of the skills trajectory, exploring employer and national policy and professional drivers of change. The results show these factors constrain and enable human agency, depending on the setting, opening up possibilities for both reskilling and deskilling. As such, the findings stress the important mediating influence exerted by ‘place’, i.e. the clinical setting on opportunities for skills development.
Introduction
In a seminal contribution Birenbaum (1982: 871) argued that ‘developments in technology, social organisation, and the division of labour’ have substantially threatened the traditional role of the pharmacist. Some claim an important component of this dynamic has been a drift towards the deskilling of the ‘profession’ (Edmunds and Calnan, 2001: 947; Harding and Taylor, 1997: 547) – a trend especially pronounced within community pharmacy (Edmunds and Calnan, 2001: 950): a sector which comprises independent proprietors and salaried pharmacists working in chains of chemists as well as supermarkets.
Coverage of skills utilisation amongst pharmacists has largely been restricted to the impact of technology and how this has altered fundamental aspects of pharmacy work and professional boundaries – an overall trend towards deskilling is a consistent theme. Birenbaum (1982: 872), for example, noted how developments in technology had imposed greater uniformity and predictability on the pharmacists’ work. More specifically, Harding and Taylor (1997: 557) referred to the way in which technological developments in the form of over-the-counter (OTC) dispensed medications, packaged for self-administration, ‘obviated the need for regulation and surveillance by experts’. The later work of Petrakaki et al. (2012) is significant in proffering a more subtle ‘agential view’ of technology. This suggests that technological artefacts constrain and enable human agency (Greenhalgh and Stones, 2010: 1285; Petrakaki et al., 2012: 435–436) without determining them. The discussion is thus framed around possibilities rather than certainties, the suggestion being the implications of technology for pharmacists are not unidirectional (Petrakaki et al., 2012: 430).
There is a need for a framework that can allow for a keener sense of interplay between context and agency. The theoretical aim of this study, then, is to extend this mode of analysis to a broader set of influences on skills utilisation beyond technology. Pharmacy operates in countries with differing institutional arrangements and varying degrees of state involvement and entrepreneurial focus (Nicolini et al., 2016). Within the UK the confluence of such factors exerts twin influences on skills deployment. First, there are employer drivers of change – an important dynamic here has been the ‘corporatization’ of community pharmacy (e.g. Bush et al., 2009), resulting in the ambiguous positioning of pharmacy as an occupation residing in-between medicine and retailing. A crucial issue is the impact of commercial demands on skills. The second area of attention is national, policy and professional levers of change. Developments here represent, at least in part, a reaction to the above commercial pressures: a broader state-sponsored re-professionalisation agenda, involving a search for new roles, marketable skills (Jesson and Bissell, 2006: 163) and expanded jurisdictions. Core features include role enlargement and an extended public health function via, for example, the New Medicine Service (Latif et al., 2016) and the Healthy Living Pharmacy Framework (NPA, 2023).
Hitherto, there has been little theoretical consideration of how these twin dynamics intersect and condition the applications of skills. More elusive still is any critical examination of complementarity or, conversely, interrelated tensions. Jesson and Bissell (2006: 167) have argued that attempting to ‘graft’ a public health mindset onto pharmacists operating within a commercial environment is contradictory. The implications of this assertion vis-a-vis skills deployment remain unexplored. Developing the agential approach, we demonstrate how key influences open up multiple possibilities for both deskilling and upskilling. As such the article speaks to broader sociological debate within medicine where professional roles are in a state of flux (Currie et al., 2010). While the thrust of the article is an examination of the implications of change for skills utilisation, this also takes in associated themes pertaining to role jurisdiction (e.g. Cain et al., 2021) and (de)professionalisation (e.g. Saks, 2021).
The article is structured accordingly. Initially an overview is provided of the relevant literature before we expound our analytical framework and research questions. This is superseded by a summary of the methodological approach underpinning the study. The main body of the article then applies the analytical schema to a rich, qualitative data set exploring evidence pertinent to the deskilling debate. The concluding section provides an overall analysis of the structural and agentive actions that can aid or confound deskilling.
Literature review
The changing structure of pharmacy
There are approximately 51,000 pharmacists in England (NHS, 2023), registered with their governing body, the General Pharmaceutical Council (GPhC). Recent diversity data show 61% are female. The racial and ethnic breakdown indicates the dominance of the Asian or Asian British group as a whole (43%), followed by the White group (33%) and Black or Black British (8%). The most common age band is 25 to 34 years old with a 37% presence (GPhC, 2023b).
Pharmacy, like most professions or ‘quasi professions’ (Denzin and Mettlin, 1968), does not comprise a homogeneous body of persons. Broadly speaking there are three strands to pharmacy – community, hospitals, and pharmacists in primary care networks (PCNs) or general practice. There are over 12,000 active community pharmacies in England (Trains, 2024). The market is made up of large multiples or chains (38%), small multiples (17%) and independents of various sizes (45%) (Connelly, 2023). The most significant recent trend has been the shift away from large multiples. The number of individual pharmacists working in PCNs has increased markedly (Burns, 2022) rising to 3294, with there being circa 7000 pharmacists based in hospitals (Royal Pharmaceutical Society, 2017).
In terms of functionality, community pharmacy is a patient-facing role with a focus on dispensing medicine and affording advice on their use – a range of auxiliary services are increasingly being provided, e.g. healthy lifestyle advice and immunisation. Hospital pharmacists, working as part of a broader healthcare team, are responsible for the care of patients and may specialise in particular areas, e.g. mental health and paediatrics. Pharmacists in PCNs function within multidisciplinary GP teams and offer patient-facing services including structured medication reviews, treatment and administrative support (Pharmacist Support, 2025; Pharmacy Careers, 2025).
Regardless of the precise branch of pharmacy, pharmacy students in England must undergo a four-year science degree leading to a Master’s in Pharmacy (MPharm). The foundation training year (formerly known as pre-registration training), which is in paid employment, is normally completed in a hospital or community setting (GPhC, 2023a). Pharmacists are required to use a range of technical and non-technical skills. In terms of the former, student pharmacists are expected to incorporate an expanding range of knowledge from their initial training into future practice beyond dispensing and pharmacokinetics, e.g. chronic disease management, immunisation, health and wellness screening and medication therapy management (e.g. Bullock and Horne, 2019). The most widely used definition of non-technical skills is ‘the cognitive, social and personal resource skills that complement technical skills, and contribute to safe and efficient task performance’ (Flin et al., 2008). While these are integral to task functionality, they are separate from the technical or practical skills required to do the job (Irwin and Weidmann, 2015). A generic list of non-technical skills would include inter alia situational awareness, decision making, leadership, teamwork and communication, managing stress and coping with fatigue (Flin et al., 2008). Pharmacists are required to utilise these skills to varying degrees in each of the aforementioned domains of pharmacy, although each branch will identify and prioritise how the skills are applied. It has been identified that non-technical skills may be used more frequently within community pharmacy than within hospital pharmacy (Irwin and Weidmann, 2015), for example.
Community pharmacy was traditionally typified by the high street chemist shop where prescriptions were dispensed and health-related items sold (Harding and Taylor, 1997: 548). The community and hospital branches of pharmacy have long held each other with ‘considerable mutual suspicion and hostility’ (Holloway et al., 1986: 329). This stems in part from the elevated status of the latter, who have been deemed to be more professional than their retail counterparts. The distinction revolves around the emphasis on entrepreneurialism (Holloway et al., 1986: 324) and ‘shopkeeping’ within community pharmacy. The implication is that the practice of pharmacy in this setting is guided by commercial interests which are at odds with the supposedly altruistic orientations of professions (Denzin and Mettlin, 1968). A broader, often unacknowledged issue is the matter of space whereby the co-location of hospital pharmacy alongside health practices with high status afford hospital pharmacy a degree of elevation.
Pharmacy and the loss of craft skills
Definitions of ‘deskilling’ abound. Within the context of the professions it has been expressed as the situation where the skills of workers that were once required to do the job are drawn from them, broken down and pre-defined at the level of conception. This results in the employee’s work being rationalised and their position transformed into an executor of other people’s plans (Apple, 1986). A lack of self-direction and autonomy is thus central.
The traditional starting point for theoretical discussions of deskilling is Braverman’s Labour and Monopoly Capitalism (1974), which used twentieth century America as its empirical backdrop. Braverman argued skilled factory work under capitalism had become progressively routinised and deskilled to the point where workers’ tasks were restricted to simple manual operations. A later account is provided by the work of Ritzer (2000), who identified McDonald’s as the modern prototype of Taylorised routinisation. Studies of trades (Haakestad and Friberg, 2020) and ‘quasi-professional’ occupations highlighted a similar trend towards ‘proletarianisation’. For example, Carey’s (2009: 512) study of social workers noted the way in which some likened their role to factory workers, ‘always moving from one procedure to the next’. As Lloyd and Payne (2016: 23) observe, debates have raged, particularly in the USA and UK, over how generalised these developments are and how they are to be weighed against counter-evidence of the upskilling of specific jobs. Here changes in the occupational structure of most countries whereby the numbers of managers, professionals and associate professionals and technicians have been increasing might suggest rising levels of skills. Lloyd and Payne (2016: 23) caution, however, that such an approach is unable to distinguish between the variable skills required within a job and the changes that may be taking place within an occupation over time. The completion of a four-year science degree for pharmacists could be viewed as a proxy indicator of high-skilled work but equally there is no guarantee that skills once formed will be put to effective use (Lloyd and Payne, 2016: 39) – especially so with overqualification rates being high across the world (Felstead, 2016: 239).
Echoing the broader labour process literature, extant research on community pharmacy has tended to focus on technology and the way this has altered fundamental aspects of pharmacy work and professional boundaries. The narrative conforms to the classical Bravermanian deskilling theme. Latif (2000: 345), for example, notes how pharmacy’s historic claim to professionalism rested with the experience of the pharmacist as a preparer of drugs. Traditionally, the pharmacist performed the craft-orientated role of apothecary where duties entailed procuring, preparing and evaluating drug products. Given the rise of premixed and pre-packaged drugs, the task of compounding was lost to industry (Trauslen and Bissell, 2004: 111). Denzin and Mettlin (1968: 378) accordingly noted how retail pharmacists increasingly viewed drugs as products to be sold, rather than objects to direct a service towards. This deterministic line of analysis can be overstated. While the pharmacists’ role is now less a ‘technicist’ (Blackburn and Mann, 1979) one, tied up with making medicines, this does not necessarily negate the importance of other skills. The above approach fails to acknowledge that skills contain a social dimension in addition to a technical one and thus elides the difference between drugs as material objects and drugs as a basis for social interaction (Dingwall and Wilson, 1995). Significantly, the passage of information around the drug to patients is a skill which has remained constant, albeit changed.
A more nuanced formulation is provided by Petrakaki et al. (2012). Taking an ‘agential’ rather than a ‘deterministic’ view of technology, it is argued that the consequences of new health technologies are not unidirectional (see also Findlay et al., 2017). Rather, the intrinsic properties of technology constrain and enable human agency for both good and ill (Greenhalgh and Stones, 2010: 1289). As such, ‘technology opens up a number of, often contradictory, possibilities for shaping healthcare professionals but does not determine them’(Petrakaki et al., 2012: 435). While technological automation is associated with attempts to deskill professionals, it may also provide the possibility to engage in more conceptual activities and facilitate the development of new capacities leading to reskilling (Petrakaki et al., 2012: 430). Unlike ‘de-skilling’ the concept of ‘re(up)-skilling’ has been afforded limited attention. Drawing on Martinaitis et al. (2021) it is defined here as continuous skill building. This refers to the opportunities of workers to learn new skills with workers having more occasion to perform complex tasks as well as have higher capacities to adapt to workplace innovations.
The current article moves beyond technological innovation, applying an agential view to two related and important but hitherto overlooked areas: (a) employer and (b) national policy and professional drivers for change. The relevant social and professional attributes of our analytical schema are explored below, along with a set of research questions to structure the findings.
Employer drivers of change
A potential factor influencing the skill requirements of community pharmacists is ‘growing corporatization’ (Bush et al., 2009) – i.e. pharmacy chains and supermarkets assuming a position of predominance over independent units. The former grouping has been described as a ‘sterile environment’ in which customers are rarely seen more than once (Tapster, 2003). This invasion of commerciality into pharmacy is thought to condition deskilling and standardisation, leading to the emergence of the ‘McPharmacist’ (Bush et al., 2009: 307). Taylor and Harding (2003; Harding and Taylor, 2000) have reviewed the above dynamic through the lens of Ritzer’s (2000) McDonaldisation thesis. Alluding to the ‘relentless pursuit of profit’, Taylor and Harding (2003: 2) plot the necessity for ‘efficient, rationalized and, above all, profitable delivery’ (Harding and Taylor, 2000: 602). The association of pharmacy with neo-Taylorist management principles and the ‘Mcjobs’ leitmotif is justified on the basis that ‘workers undertake simple, clearly defined tasks in accordance with written procedures’. Efficiency dictates that interactions between customers and employees are time limited. One consequence is that conversations ‘can be regulated using scripts, protocols and mnemonics’. This has the effect of precluding the practice of discretion with consultation limited to the asking of structured, formulaic questions (Harding and Taylor, 1997: 556), the overall effect being the commodification of healthcare.
A broader literature uses an ethical lens to offer some penetrative insights into the skills implications of corporatisation. Bartholomew (2009: 299) refers to the misalignment of professional duties to patients and the organisational requirements of employment. More specifically, noting pressures to link sell OTC medicines, Cooper et al. (2007: 106) explore the ethical problems driven by the inherently commercial and increasingly consumerist nature of medical sales. Skills issues are implicit in such accounts – clinical judgement is stymied because pharmacists cannot prevent sales of OTC medicines, notwithstanding reservations about their clinical appropriateness. The intrusion of a business orientation into community pharmacy thus imposes deskilling pressures emanating from both standardisation and the prioritisation of profit over clinical judgement and patient welfare. The extent to which corporatisation might allow pharmacists to develop new capacities effecting upskilling is a conspicuous gap within the literature.
Question: How far do employer priorities erode the skill base and autonomy of community pharmacists?
National policy and professional drivers of change
A number of significant reforms have been made to the pharmacy profession, as policy makers have recognised pharmacists possess a distinctive expertise (McDonald et al., 2010: 452). Such reforms to reshape the pharmacists’ role have been driven by the need to address skills shortages amongst clinicians; and significantly, a public policy desire to expand the role of community pharmacy in public health more generally amid growing health inequalities. Measures have accordingly been introduced to extend roles and functions which might simultaneously serve to upskill and open up more conceptual activities and new clinical capacities. This shift represents an attempt at state-supported re-professionalisation of the sector (Jesson and Bissell, 2006).
Such reforms have sought to encourage pharmacists to reduce their dependence on dispensing as a source of income (McDonald et al., 2010: 452) via the delivery of education and screening services (Latif et al., 2016). Examples include the introduction of Healthy Living Pharmacies (National Pharmacy Association [NPA], 2023) and, more recently, the Pharmacy First Strategy (C+D, 2023). While such interventions might conceivably enhance skills utilisation, allowing pharmacists to leave the ‘dispensing bench’ and provide patient-centred services (Latif et al., 2016: 987), research suggests an indeterminate set of outcomes. Consider here, for example, the New Medicine Service (NMS). Under this scheme patients with chronic conditions can obtain extra help and advice about medicine via contractual incentives afforded to pharmacists (Waring et al., 2016: 125). Latif et al. (2016: 983) note how general practitioners (GPs) viewed the NMS as potentially encroaching professional boundaries – duplicating the work undertaken by GPs. One outcome was the NMS had little if any effect on the relationship with the pharmacist, which continued with the ‘prescribing-dispensing’ pattern (Latif et al., 2016: 984).
An important issue is how the medical hierarchy and different types of licence affect skilling processes (Cain et al., 2021). The most significant government intervention in this regard is the independent prescribing (IP) right granted to pharmacists (and nurses) in 2006 following the Crown Report (Department of Health, 1999). This sought to modernise the UK National Health Service (NHS) and make better use inter alia of the skills of professional staff such as nurses and pharmacists (Weiss and Sutton, 2008: 407). From September 2026, all newly qualified pharmacists will be independent prescribers on the day of registration (NHS, 2024). Weiss and Sutton (2008: 407) suggest, ‘traditionally prescribing has been an indicator of the clinical autonomy and professional power of doctors within the wider structure of society’. While the intended reconfiguration of jurisdictions and boundaries in the social organisation of healthcare offers potential for the upskilling of pharmacists, possible tensions in boundary relationships again render outcomes far from certain.
Question: Do national-policy and professional drivers of change afford opportunities for upskilling?
Drawing on the above insights, this article applies an agential view to the above twin drivers of change, examining how they potentially constrain and enable human agency. We argue for a balanced assessment of possibilities across different settings that avoids an unhelpful unidirectional focus on deskilling. First, the research strategy is outlined.
Research method
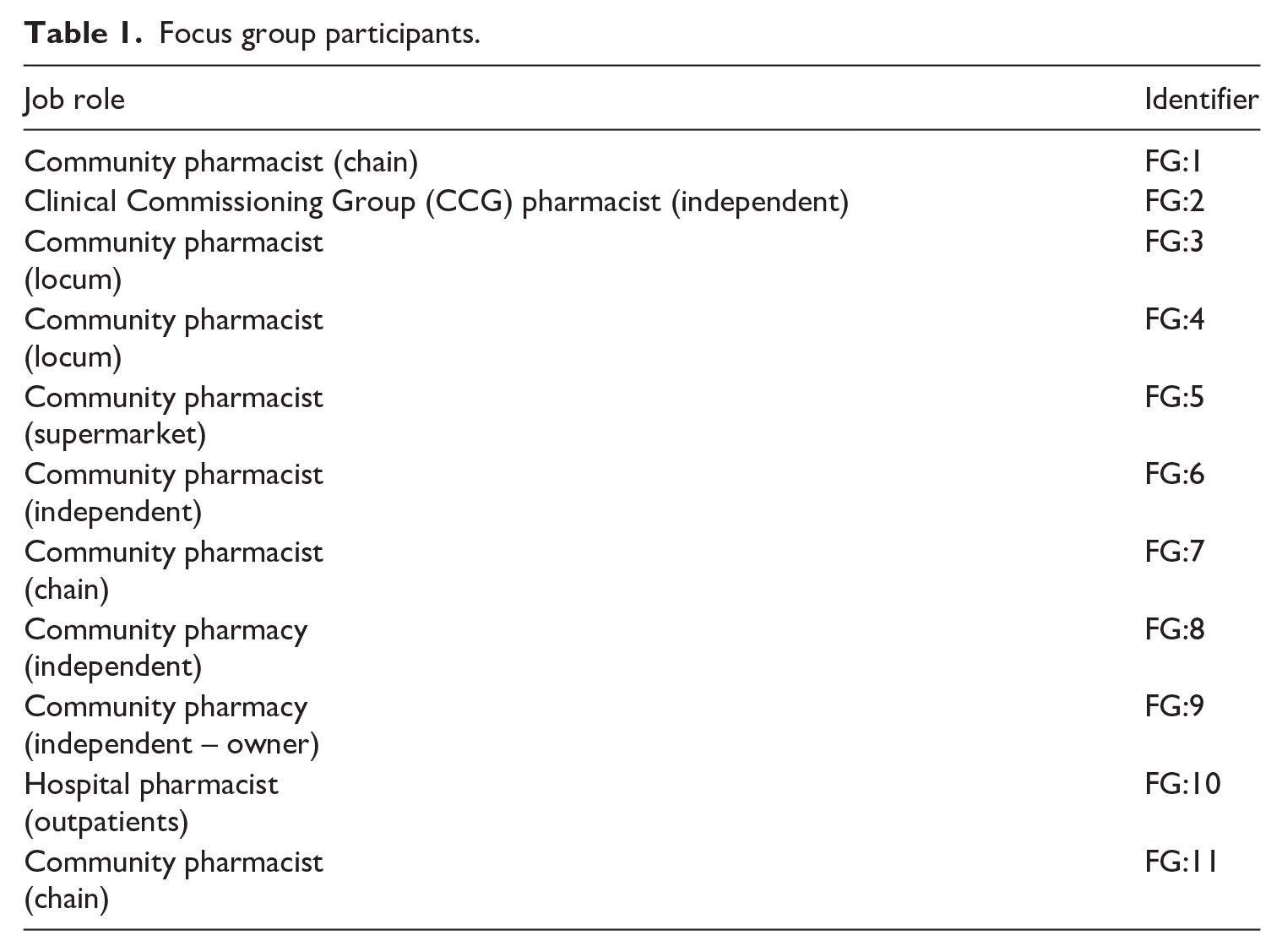
The broader research project from which the data are derived was initially designed by a multidisciplinary team researching applied clinical issues, pharmacy as a ‘public good’ and employment relations matters. The aim was to obtain an understanding of the key contemporary issues in each area. To facilitate access to research participants two focus groups (Table 1) were held with 11 practising community pharmacists studying for a Post-Graduate Diploma in Clinical Pharmacy at the lead author’s university. Focus groups are commonly prescribed for research that is exploratory (Stewart et al., 2007: 9) and as such they were deemed suitable for these early scoping discussions. By combining practitioners who were motivated to improve their professional and theoretical knowledge, the research team were able to draw on the practitioners’ varied skills to enhance the quality of the research data and findings. Both focus groups used the same research schedule, which explored their current role and experience and views on changes in professional practice. The theme of de(up)skilling emerged as the core employment relations issue and was subsequently investigated in greater depth by specialists in this field.
Focus group participants.
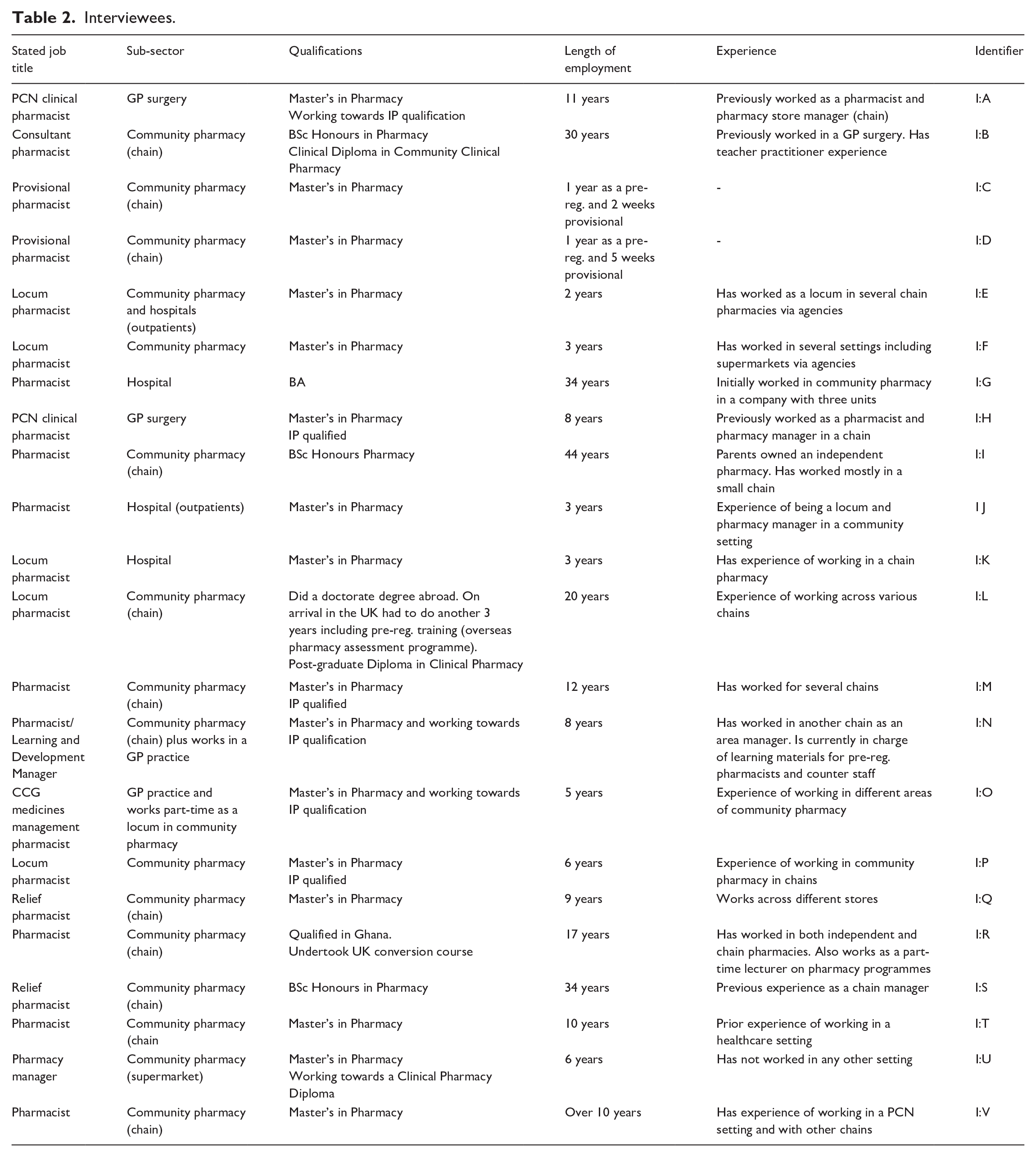
This article is concerned with the theme of skills utilisation in an ostensibly inhospitable environment – one in which the requirements of employment in a commercial and bureaucratic undertaking may come into conflict with pharmacists’ professional duties (Bush et al., 2009). There are subtle social processes at work and this tranche of the study accordingly adopted an in-depth, qualitative approach using semi-structured interviews to derive intricate details about the experience of employment. The extraction of such data concerning ‘feelings’ and ‘thought processes’ lends itself naturally to a qualitative approach (Strauss and Corbin, 1998: 11), given its sensitivity to the lived experience of individuals. Building on the foundations of the focus groups, a total of 22 interviews were held between August 2020 and May 2022 (Table 2) with a different set of practitioners. Five were conducted face-to-face, the remainder via telephone. Sampling was initially undertaken via a purposive approach, to identify participants ranging from newly qualified practitioners to those having a high degree of industry experience, allied to familiarity with working in various branches of pharmacy. Additional interviewees were endorsed through a snowballing method. In this way we were able to capture the thoughts of a breadth of pharmacists with varied experience of working in differing community settings (chains, supermarkets and independents) and beyond (i.e. PCNs and hospitals). As such, the study was well placed to explore how variation in clinical settings influenced skills deployment. While the research process was interrupted by the Covid pandemic, the spacing of the sessions over a two-year period lent itself to an iterative approach which involved the checking and building of knowledge in key areas, for example, work processes, skills acquisitions and clinical aspirations. All interviews were conducted by one or other of the research team.
Interviewees.
The discussions were wide ranging. The interview schedules were based on themes arising from the literature review, encompassing employer drivers of change (commercial pressures, job content, organisational culture and so forth) and national policy and professional matters (development opportunities, shifting boundary relationships and the expansion of services). The researchers were also keen to probe matters relating to human resource management including training, performance management, career mobility, voice and so forth. Consistent with academic guidelines, the researchers secured prior ethical approval from the lead author’s research ethics committee on 25 March 2018.
Epistemologically, this article falls within the sphere of abduction (Reichertz, 2007). Consistent with this, the work was guided by existing theory. An initial (a priori) coding schema was devised from the relevant literature. This comprised first-order codes reflecting key conceptual themes, for example, entrepreneurialism, pay, performance management, work intensity, decision latitude and quality of clinical service. In line with the principles of abduction (Reichertz, 2007: 225), the second step comprised the ‘intellectual jump’ that adds something new to the data. Higher order subcodes were added, capturing conceptual insights derived from a more fine-grained understanding of the data. Here, for example, codes relating to the mediating impact of ‘place’ or clinical setting on skills were identified from the research interviews. The overall process of designing the coding structure and its application was undertaken with care to ensure confirmability, consistency and authenticity (validity) of the data and its interpretation (see Miles and Huberman, 1994: ch. 10).
Findings
The research sought to examine how far employer drivers for change and national policy and professional levers have influenced the application and development of skills. The findings are accordingly structured into two sections. The concluding material will consider the theoretical implications of the data.
Employer drivers of change
Most of the pharmacists had experience of working in chains or supermarkets and there was widespread feeling that the focus on commerciality compromised autonomy and the ability to impart technical knowledge, invoking elements of deskilling. There were references to retail pharmacies being ‘warehouses’, staff being akin to ‘robots’ and organisations putting profits ahead of patients – ‘it’s all about targets. It’s not much about patient care. MUR [Medicine Use Review] targets. Sell this’ (I:B). It was suggested such pressures have been compounded in recent years due to reductions in NHS contractual funding. Indeed, some had moved out of community pharmacy due to frustrations around commercial pressures infringing on skills deployment. While there were several examples of community pharmacists moving across to hospitals or GP practice, what was striking was the number of newly qualified staff engaging in a process self-selection, viewing such a move as an immediate goal:
It doesn’t take you long. Usually by the second year you realise your job has become monotonous. It’s essentially the same thing that your are doing. (I:R)
Those who had made the move from a community to a hospital setting commented on the inferior clinical role within the former. Within the latter, the greater degree of dialogue with members of the healthcare team, and access to patient records, facilitated closer involvement in the direction of care, affording enhanced ability to operationalise and build on the skills and knowledge garnered during initial training:
There’s more dialogue with other members of the healthcare team. One huge factor has to do with the availability of information, the patient record. In community pharmacy until recently we didn’t have any access at all to patient healthcare records. That frustrates you because essentially to make judgments you need information.
Similar comments apply to GP practice. One interviewee working in a chain with aspirations to move across to this setting stated:
That [moving into GP surgery] would be quite appealing in the sense it would give me the opportunity to use my clinical knowledge a bit more. . . You don’t have the information ready to hand [in community pharmacy]. We don’t have clinical notes, we don’t have access to their blood samples. So, there is a lot of information we still don’t have. (I:U)
Pharmacists working in PCNs also referred to the broader impact of building a close rapport with doctors and other clinicians, including the ability to influence the purchasing of medicines, e.g. the use of generic medicines that might cost far less than brands.
A common theme was the fast-paced nature of community pharmacy and the sheer intensity of the working day with pharmacists ‘getting pulled in all directions’ (I:Q) and ‘spinning plates’ (FG:7). Work intensification was seen to frustrate the systematic application of clinical skills. There were comments vis-a-vis pharmacists signing off prescriptions without scrutinising them for drug interactions and instances reported of patients being given the wrong medication. All the locums interviewed acknowledged the stores were usually short staffed, leaving them no alternative but to serve on the till in between counselling patients and dispensing prescriptions – a function for which they were significantly overqualified.
Interviewees routinely referred to intensive systems of performance management and accountability. Targets were set in a myriad of areas including prescriptions delivered, medicine use reviews, flu jabs, vaccines, hair retention schemes and the sale of OTC products. In terms of the latter, the focus on commercial metrics hints at ‘Bravermanesque’ task degradation (Braverman, 1974: 127) and was a clear source of embarrassment. Some referred to the need to ‘link and upsell’, i.e. sell a product for every one of the patient’s concerns (I:A). This presented an ethical dilemma as it debarred the operationalisation of relevant skill sets where products were not considered clinically essential or useful:
It’s called link-selling. Somebody comes in and asks for some antihistamines [and] you have to make sure you sold a box of tissues to go with it! Have you got any face cream to sell [to put] on their sore nose – I personally hate it! (I:G)
Useful as such data are, it would be remiss to plot a deterministic denial of agency and narrowing of skill requirements. There was evidence that the expansion of services had extended the social aspect of the job, with some exhibiting pride in the development of an associated set of non-technical skills around encounters and communication. Consider here, for example, the support provided for those undergoing methadone treatment,
I do encourage them, I share their joy and excitement and say you’re doing really well. (FG:4) Just encouraging them. Showing them that it’s not impossible, maybe sharing stories confidentially of other patients that have come off it – [heroin] – being empathetic. (FG:2)
There were also data on conflicting trends with deskilling and upskilling coexisting. That is, the suppression of technical skills was paired with gains in the acquisition of other forms of human capital, i.e. non-technical skills. Pharmacists in large chains have a managerial/team leader role which involves reviews with subordinates, rostering, responsibility for general housekeeping (e.g. cleaning) and managing inventories of up to 50,000 items. This prompted one interviewee to note, ‘my main job was obviously to manage the team’, the implication being the clinical role was secondary (I:J). Another, who had subsequently moved into hospital pharmacy, was upbeat about their earlier experience of community pharmacy, noting that while the line-management function had moved them away from the clinical aspect of the job, the commercial setting had equipped them with ‘some very good’ people management skills (I:J), which were directly transferable to a hospital context. Others similarly referred to the acquisition of leadership capabilities which were seen to extend skill sets into a new domain. Interestingly, there was some criticism that the commercial aspect of the job could be taught better at universities, ‘what you learn in the ideal world at university is not always reflected in practice. It can be very different’ (I:U).
Broader forms of agency were also acknowledged. Far from being submissive victims of commercialisation, some felt there was significant scope for skills development within a commercially focused setting. One (I:B) with 30 years’ experience of working for a national chain, had recently completed a Covid vaccinator update, a flu injection refresher and training for an OTC contraceptive pill. Others sought to extend their skillsets by organising clinic days which potentially provided ‘a couple of quality hours’ (I:Q) to impart the theoretical knowledge acquired during training in a range of areas. Some alluded to the Healthy Living Pharmacy Framework, whereby community pharmacies seek to meet targeted local need to improve the health and wellbeing of the local population. For freelance locums, there were practical, instrumental reasons to keep their skill sets up-to-date to maximise the opportunity for, and revenue from, agency placements.
There was some discussion of the difference between working in chains/supermarkets and independent pharmacies. Some alluded to autonomy, with one (I:R) noting there was more ‘fluidity’ and freedom to ‘satisfy the patient’ in the latter with standard operating procedures being more rigid in the former. Within the former, the logic of bureaucracy and requirement for unyielding consistency in practice was seen to stifle the ability to impart clinical knowledge given there was little opportunity to influence procedures and processes – ‘it’s their way or the highway!’ (I:B). Another remarked:
The multiple – it’s all about accountability. The multiple would want to follow the letter of the law or the standard operating procedure even if it constrains your practice. It helps them to be consistent. And of course the price they would pay then is that the patient might suffer on some occasions in trying to maintain that consistency. (I:R)
One implication is commercialisation per se does not constrain skills utilisation, the setting is an important mediator that conditions outcomes.
National policy and professional drivers of change
National policy reforms have brought about a significant expansion of the services offered by pharmacists, extending the scope of their professional jurisdiction within the primary care setting. Policy makers have recognised that pharmacists possess distinct skills and expertise with reforms introduced to extend roles. Recent years have witnessed various government intervention to shift greater care into the community with patients being encouraged to seek advice and treatment from local pharmacists for common conditions. While fresh initiatives, e.g. Pharmacy First (Company Chemists’ Association [CCA], 2025), have expanded the scope of care that can be offered to patients, this trend was well under way when the research commenced in 2020. As one pharmacist working in a chain noted:
I think people find it more difficult to get into a GP. They will more often come to the pharmacy even if they think they need to go to the doctors just to ask your opinion and see if there is anything you can do to treat their condition. I think you’re kind of like a gatekeeper. (I:U)
The implications of such developments for the application of key skills are indefinite and contested and it is clear that national policy frameworks can invoke both upskilling and deskilling tendencies concurrently. A case in point was the use of medicine use reviews (MURs) which aimed to increase patients’ knowledge of their medicines. While the service was free to patients, pharmacies could claim reimbursement of £28 (Community Pharmacy News, 2020). The research period coincided with the ending of government funding in 2021 and as such their use sparked much comment. One view proffered was this initiative had provided pharmacists with the ability to operationalise core technical skills acquired at university, i.e. problem-based learning and the allied training conditioning them to view medication holistically (I:J). It was evident, however, that the aforementioned commercial pressures intervened to shape outcomes. One interviewee (I:A), who had formerly worked for a chain before moving into a PCN setting, noted that in the latter environment surgery time was allocated for MURs, whereas in their previous role ‘it was done as an add on, on top of your jobs’. The implication here was that work intensity and the need to conduct MURs alongside other daily activities (dispensing prescriptions, repeat dispensing, clinical governance and so forth) precluded a thorough review.
A further important way pharmacists can upskill themselves is by taking on the role of independent prescriber (IP). While IP status affords significant potential for pharmacists to relieve the pressure on doctors by extending their skills and responsibility, the ability to follow this route was again significantly coloured by the clinical setting. One working in a chain (I:M) suggested the qualification would be superfluous, actually heightening the degree of skills underutilisation, complaining ‘you would never be able to use your independent prescribing skills’. It was suggested this would require a move into a PCN. Another (I:P), who had also worked for a chain, demurred on this point, stating the organisation would have paid for the qualification. The actual problem was no assistance was given in sourcing a GP to provide the necessary 12 days of learning in practice. Now a locum, they described a tortuous process of initial rejections before securing a placement with a doctor recommended by a friend and fellow pharmacist. It was claimed some doctors were only prepared to offer the service for payment, with figures of £1500 and £2000 cited. However, even this ostensibly more hospitable context was seen as both enabling and constraining the use of skills. One interviewee (I:Q) alluded to abundant accounts from peers suggesting a lack of self-direction and autonomy, with independent prescribers ‘sitting in an office all day long, signing off regular scripts. . . doing all the doctor’s dog work’. This was seen as both a waste of their clinical skills and contrary to guidelines that pharmacists should only sign off prescriptions in areas in which they were competent.
Beyond jurisdictional changes with doctors, policy makers have sought to reshape the contours of the pharmacist’s boundary relationship with subordinates. Various accreditation processes have been developed for non-pharmacists to allow them to make better use of their skills. Dispensing pharmacists are required to perform a clinical check on prescriptions to assess the drug prescribed and the dose, but the task of dispensing can be delegated to accredited checking technicians (ACTs) and dispensing assistants. In theory the extension of junior roles should afford room for pharmacists to work ‘at the top of their licence’ (Russell-Babin and Wurmser, 2016) in a less pressurised environment, moving away from routine aspects of the job, labelling, for example, towards more cognitive and skilled functions. A problem, however, was lack of resources, not having enough ACTs and dispensers to free up the pharmacist’s time. Such problems are again related to commercial pressures and the lack of investment in support staff. As one interviewee based in a chain put it, ‘investment means money’ (I:B).
Discussion and conclusion
Our analysis of community pharmacy builds upon several areas in the sociology of healthcare work. Broader studies have emphasised the potential for the technological deskilling of clinicians (e.g. Aquino et al., 2023; Holt, 2011). The medical literature has similarly highlighted such tendencies (e.g. Edmunds and Calnan, 2001: 944; Harding and Taylor, 2000) amongst pharmacists, the implication being community pharmacists have become ‘over educated’ dispensers of medicines (Mesler, 1991: 312). However, as Vallas (1990: 387) has noted, skills theorists acknowledge that changes in skill requirements involve far more complex and contradictory processes than can be grasped using simple de(up)skilling dichotomies. Indeed, they may not be mutually exclusive possibilities, but rather conflicting trends than coexist with the same industry. Consistent with this position, this article adopted an agential view (Petrakaki et al., 2012) of levers of change beyond technological innovation, exploring how employer and national policy and professional drivers of change might constrain and enable human agency. This involved consideration of how pharmacists capture change in the process of remaking and retaining influence (Petrakaki et al., 2012: 430).
Turning to the first research question of how far employer priorities erode the skill base and autonomy of community pharmacists, there was clear evidence that pressures relating to corporatisation (Bush et al., 2009; Jesson and Bissell, 2006) exerted significant influence. The tension that has been noted between the twin demands of commercialisation and professional altruism (Harding and Taylor, 1997: 552) was very much to the fore. In some important respects the data chime with Harding and Taylor’s (2000) depiction of the ‘McPharmacy’, with the clinical role eroded by the need for efficiency and profitable service delivery. One outcome was the sheer intensity of the work, which on occasion frustrated the application of technical skills. Similarly, pervasive systems of performance management gave rise to ethical problems. In those situations where commercial priorities prevailed, this could act to stymie self-direction, clinical autonomy and judgements of whether the products were necessarily essential and complementary.
There are problematic consequences, however, of an uncomplicated application of Harding and Taylor’s (2000) ‘McPharmacy’ line of analysis which posits a straightforward neo-Taylorist tendency towards deskilling and the performance of routinised activities. One issue is the narrow interpretation of what skill means. Certainly, the data suggest ‘the corporatization of community pharmacy’ (Bush et al., 2009) may frustrate the application and development of technical skills. However, skills outcomes are far from determinate. The findings provided evidence of pharmacists upskilling by engaging in continuous skill-building (Martinaitis et al., 2021) through the attainment of non-technical skills including the managerial side of pharmacy, for example, business strategy and leadership. These were viewed by some as useful transferable skills, which might allow them to adapt to future workplace innovations.
In the same way that the issue of human agency has plagued Braverman (1974) inspired deskilling theory (Vallas, 1990: 382), uncritical ‘McPharmacy’ accounts create the sense of pharmacists as passive actors, unable to resist top-down control. Bissell et al. (2001: 289) have referred to the absence of sociological insight in relation to pharmacy. Certainly, the low level of engagement with sociological thought is especially striking in this regard. Evidence of proactivity, self-reliance and resistance cut through much of the data. While participants were cognisant of the impact of commercial pressures on their overall skill base and autonomy, they were far from passive actors. Some had crossed pharmacy sector boundaries (see also Rodrigues and Guest, 2015), moving into hospital pharmacy which afforded greater potential to both use technical skills and engage in further skills building via the execution of more complex tasks. Purposive agential action also came through in the way some sought to accumulate human capital. Emphasis was placed on professional development and building up a repertoire of competences related to Covid vaccinations, flu injections and the like. Whether this represents a strategy of genuine upskilling is a moot point. A critical reading of the data might suggest the routinised nature of the services provided amounts to ‘multi-tasking’ (e.g. Danford et al., 2005), i.e. an expansion of semi-skilled responsibilities horizontally, contributing to work overload and stress. Either way, the findings point to an indeterminate and contested set of outcomes.
Moving to the second research question, and whether national-policy and professional drivers of change afford opportunities for upskilling, an important issue to consider is whether the reconfiguring of occupational dominions and borders afford opportunities for role extension. The data relating to the independent prescribing rights granted to suitably qualified pharmacists in 2006 are informative. IP status grants the legal right to prescribe and involves pharmacists taking on formerly ‘entrenched’ (Edmunds and Calnan, 2001: 949) roles that were traditionally deemed part of the doctors’ medical terrain, for example, advice on drug therapy. This dynamic feeds into broader long-standing debates around boundary encroachment (Edmunds and Calnan, 2001: 949), ‘occupational imperialism’ (Larkin, 1983) and restriction of practice (e.g. Campbell and Haiven, 2011).
Many of the participants in the study supported the extension of their roles into the GPs’ traditional domain. This afforded clear opportunities for continuous skill building via the execution of complex tasks (Martinaitis et al., 2021). The ability to exercise these rights, however, was dependent upon ‘place’, i.e. the clinical setting. There was little incentive for those in chains and supermarkets to upskill, given the lack of opportunities to apply the qualification. For these, IP status would simply exacerbate the feeling of absence of self-direction – of being overqualified for the job. In any event, there was often no financial support or funding for study leave available. Any pull towards IP status lay in its currency as a passport into the less commercially pressured PCN setting, or – from the perspectives of freelance locums – the ability to maximise revenue from agency placements. The gaining of IP status was in any event fraught with barriers as obtaining the minimum of 90 hours or 12 days of learning in practice under a doctor could prove problematic. The reasons for this are unclear. While this could be related to exclusionary and demarcation strategies (Edmunds and Calnan, 2001: 954) or ‘social closure’ (Weber, 1947) amongst GPs, pharmacists did not see themselves as violating GPs’ territory and there was no direct evidence of ‘push back’ from doctors. There was, however, some anecdotal indication of routinisation with pharmacists who had made the transition to IP in PCN settings being given the task of signing off generic prescriptions. One interpretation might be ‘territorial skirmishes’ (McDonald et al., 2010: 456), i.e. GPs’ attempt to maintain the traditional division of labour via the delegation of mundane tasks. At the very least, the data suggest the PCN setting – which many aspire to – does not necessarily afford opportunities for significant upskilling and capacity for critical thinking.
Another policy and professional issue to consider is whether ‘medicines management’ (Pharmaceutical Journal, 2000), via the provision of specialised services such as the former MURs, affords clinical opportunities for upskilling. Ostensibly, this form of role extension in the delivery of primary healthcare (including the New Medicine Service and the Healthy Living Pharmacies Framework) gives pharmacists the opportunity to relinquish routine facets of the job (McDonald et al., 2010: 456), apply aspects of technical knowledge and expand non-technical social skills, for example, listening, questioning and influencing (Hargie et al., 1994). In terms of the latter, Waring et al. (2016: 128) note, one ‘rationality’ is that of patient education with the pharmacist identifying knowledge deficiencies and guiding behavioural change. Certainly, some suggested MURs served both an important clinical function – operationalising elements of earlier technical training in problem solving – and sharpened non-technical social skills. The majority, however, expressed doubts. As such, this and other ‘advanced services’ that have sought to expand the public health function of pharmacists simply compounded pressures around work intensification. Many in the sample described a tedious process involving performance targets, fractious interactions with line management and a wearisome treadmill of cursory consultations.
To sum up, the study has considered employer influences on skills allied to national policy and professional drivers of change. Consistent with an agential approach, the central argument is that the confluence of these factors opens up a field of multiple possibilities (Petrakaki et el., 2012: 435) for both reskilling and deskilling. However, a core finding is the potential for technical upskilling afforded by the national policy interventions is significantly mediated by employers’ commercial priorities. The two sets of findings support Jesson and Bissell’s (2006: 167) reference to the problems of attempting to graft a public health mindset onto a commercial environment. Developing this point, it is noted that ‘business practices are not necessarily incompatible with public health objectives’. Rather ‘the wider policy framework needs to address the fact that pharmacy is now corporatized’ (Jesson and Bissell, 2006: 167). As such, the closure of government fundings gaps (NPA, 2024) is necessary to ease commercial pressures and fund, i.e. incentivise, value-added service provision, for example, the roll-out of independent prescribing. As it stands, the full utilisation of technical knowledge derived from medicines management and IP status appears to require a decoupling from commercial pressures and the garnering of boundary management strategies (Rodrigues and Guest, 2015: 683), facilitating a move into a PCN or beyond. The findings thus stress the important local influence exerted by ‘place’. Ultimately, the more demanding extensions in function, for example IP status, are only logically beneficial in certain settings. Put another way, the findings indicate different types or tiers of pharmacy (supermarkets, chains, independent pharmacies, PCNs and hospitals) can act to close down or complement differing skills sets.
The findings speak more broadly to debates pertaining to (de)professionalisation (e.g. Saks, 2021). While this was not a focus in the current study, the data point to a series of ‘professional adjustments’ in the face of growing marketisation and corporatisation as reported elsewhere (Saks, 2021). The material similarly lends partial support to Saks’ (2021: 17) observation that ‘attempts to professionalise with the support of the state can fail as well as succeed’. Reflecting the earlier commentary, any potential for ‘success’ is significantly influenced by the clinical setting.
The data signal some apposite areas for future research. Scholars could usefully explore the issues of skills at an international level (e.g. Martinaitis et al., 2021). Countries exhibit varying degrees of marketisation and state involvement in pharmacy, and work is needed to map how the balance between ‘conflicting logics’ (Nicolini et al., 2016: 241) conditions skill levels. An obvious comparison would be between liberal (the UK and the USA) and Nordic social-corporate polities but studies could similarly map countries beyond this spectrum, e.g. China (Nicolini et al., 2016: 245).
Footnotes
Acknowledgements
The authors would like to thank two anonymous referees for their comments on an early version of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
