Abstract

This article is in our series on social prescriptions
Healthcare systems are facing increasing need and demand because of aging populations, increasing chronic disease and multimorbidity, and new therapeutics and diagnostics being brought to market. These factors, when combined, require unsustainable levels of funding. 1 We must also acknowledge that a large proportion of chronic diseases that plague healthcare systems are preventable or can be brought into remission through lifestyle interventions and that 70% of health outcomes are determined by social factors that remain mostly unaddressed in healthcare systems predicated on the biomedical model. 2
There have been various attempts to look outside the biomedical box since the birth of social medicine in the 19th century, but none of the approaches has been able to challenge the dominance of the biomedical model. More recently, however, the rise of social prescriptions across European countries gives hope that there are non-biomedical means we can use to improve patient and population outcomes while optimising resource utilisation. Social prescriptions provide a way to connect individuals to sources of support within their community to address social determinants of health and encourage self-care for a variety of physical and mental health conditions. 2
Tech-enabled social prescribing: a ‘disruption from below’
The economic concept of ‘disruption from below’ describes a situation in which an organisation provides a cheaper solution to a problem that is less profitable for the incumbent. But more significant is that the new solution is better in some key ways that are important to the user. Typically, the margins of the new solutions are too low for the existing players, who prefer to stay with their more profitable solution rather than cannibalising their own market. Eventually, this novel solution becomes increasingly better and takes a larger share of the market and/or taps into a user base that did not use the services previously because they were too expensive.
The rise of the desktop computer versus the established mainframe computers is one example of such a disruption dynamic. The desktop computer was easier to use but it had fewer capabilities than a mainframe computer. The established mainframe manufacturers ignored the cheaper desktop computers only to find they improved quickly adding more functionality and they soon overtook the mainframes relegating them to a footnote in history. In healthcare, the pharmaceutical industry currently faces the ‘better than the Beatles’ problem: unlike a new song, novelty has no intrinsic value in pharmaceuticals. 3 New pharmaceuticals must significantly outperform the gold standard to justify the high prices charged to recoup their development costs, which typically lie in the billions.
Social prescriptions have the potential to affect our health at much lower cost and fewer side effects than most medicines. Social prescriptions are poised to become a key disruptive force in 21st century healthcare because they can: (a) be personalised and be highly adaptable to individual needs/expectations, which is currently largely impossible for most pharmaceuticals; (b) effectively address many health and care issues associated with lifestyle-related chronic conditions; and (c) address non-biomedical issues related to social determinants of health.
But there are several strategic, operational and tactical barriers that we must actively overcome to fully realise the disruptive potential of social prescriptions. The hope is that digital technologies will make it possible to scale social prescriptions because: (a) digital technologies make it easier and cheaper to obtain relevant information on individual patients, providers and the system; (b) they can increase flexibility outside of the traditional place-based care approach (e.g. online remote monitoring of vulnerable people and flagging changes in conditions that might require medication adjustments); and (c) they provide 24/7 interaction and automated functionality with the ability to provide nudges to patients and for the user to deliver frequent feedback as needed.
In this article, we argue that in order for social prescriptions to achieve their disruptive potential, they need to be informed by technological and lifestyle trends that influence our daily behaviour, particularly those that would allow social prescriptions to blend into what feels normal to patients’ regular lives.
Tech-enabled social prescriptions as a living service
‘Living Services’ are enabled by digitally connected intelligence and are defined as: sophisticated, contextually-aware digital services designed to anticipate and respond to your needs. They react in real-time to changes in the environment and patterns of behavior, in ways that will transform how we live, work and play.
Tech-enabled social prescriptions in practice
How digital technologies can deliver certain aspects of care relevant to social prescribing.
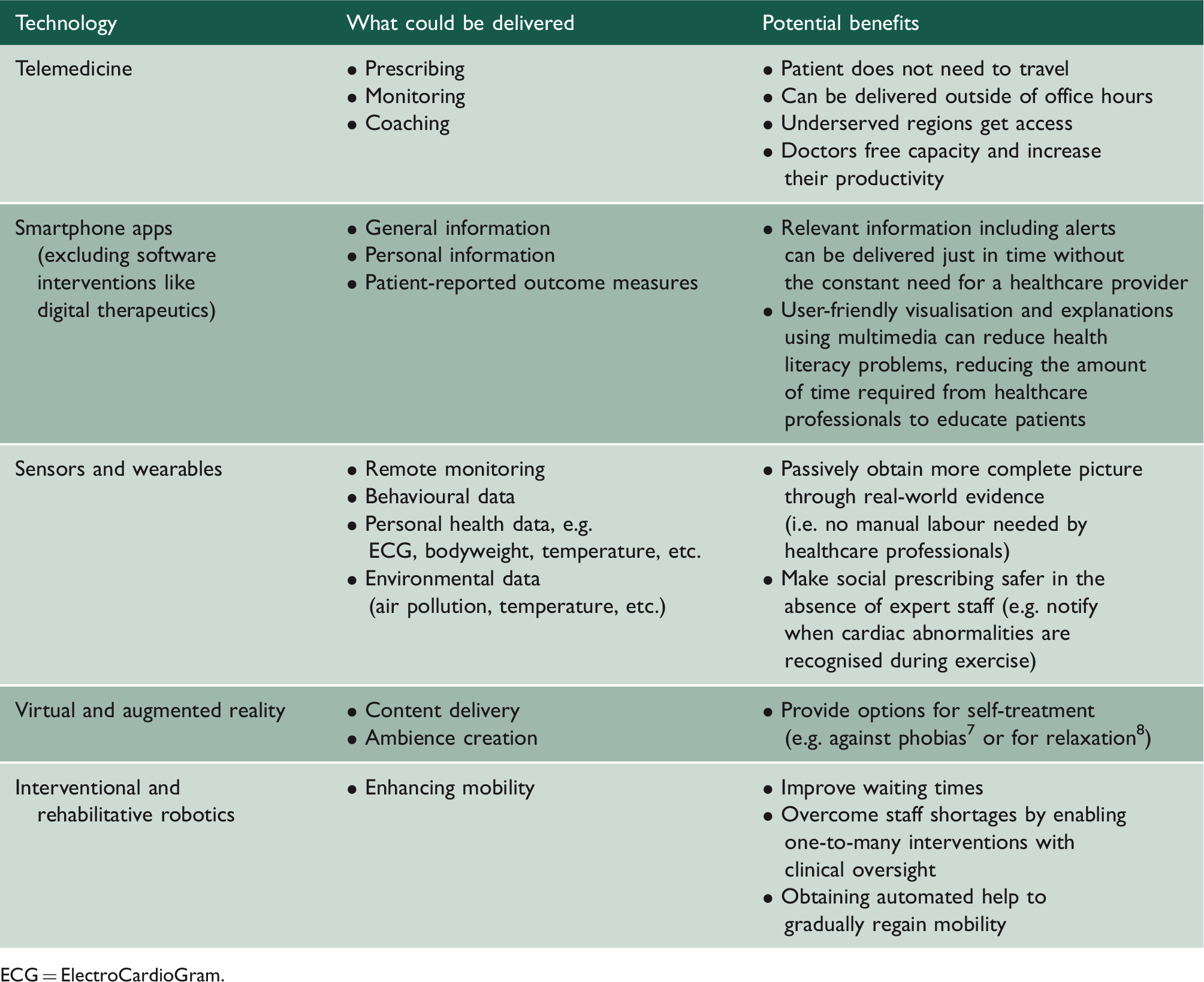
ECG = ElectroCardioGram.
As technologies improve, social prescriptions could have a stronger impact, particularly for chronic diseases that are driven by lifestyle issues and comprise a significant burden of disease in most countries. Tech-enabled social prescriptions could be made accessible at scale and can deliver more precise and faster adaptable interventions compared with pharmaceuticals, where precision medicine delivered via pharmacogenomics is still very expensive with a significant delay before novel drugs are available on the market.
Health and care’s shift towards tech-enabled social prescriptions is already happening at large and small scales. Platforms like Elemental 9 focus on coordination of logistics related specifically to social prescribing, while platforms like Intelligent Health 10 aim to create communities where individuals are connected with local services aimed at improving their health and wellbeing. The Royal College of General Practitioners is also in the pilot stages of a project to explore how Internet of Things could be used to support social prescriptions. 11 At a more global scale, large technology players like Apple are investing heavily into technology aimed at improving health, as evidenced by the recent US Food and Drug Administration approval of the newest version of the Apple watch as a medical device 12 ; and Haven, the joint initiative between Amazon, JP Morgan and Berkshire Hathaway aims to leverage ‘the power of data and technology to drive better incentives, a better patient experience, and a better system’ for its employees. 13
Further to this, as with other disruptive technologies, tech-enabled social prescriptions have the potential to deliver services to those who never had access to them previously. This is particularly important in resource-poor settings where tech-enabled social prescriptions could facilitate access to healthcare and also focus on lifestyle interventions to keep people healthy, rather than putting them at risk of developing preventable chronic diseases, as has happened in Western countries. One such example of this is Waves for Change (W4C), a South African non-governmental organisation which provides community-led physical activity programmes to disadvantaged youth that have been proven to prevent several physical and mental health challenges. Waves for Change has recently launched a platform called ‘Coach Assist’, which automates the recruitment, payment and tracking of community-based volunteers who launch activity-based community groups and receive payments for each individual engaged in their activities. 14
Scaling tech-enabled social prescriptions
To enable the health and care system to have functional social prescribing which is both sustainable and effective will require patients and health and care professionals to co-develop and be trained in using technology that removes barriers, manages huge quantities of data and supports all stakeholders to facilitate proactive management of patient care to reduce workload on the system and help the person be in control of their health.
Removing barriers
At its core, social prescribing supports the person to identify their personal goals and facilitates the use of community activities to meet these goals. General practitioners, link workers, allied healthcare professionals and community providers need to be able to share information and work as a team to help each person, which means information needs to be captured and shared effectively across organisations requiring improved standards and application programming interfaces for data sharing that facilitates ethical interoperability, which ensures patient safety and safeguarding of vulnerable people.
Managing data
Wearables and sensors can give information and insights that previously were not possible to collect. Through improved information flows and multiple measures of impact not only is it possible to capture the value of social prescribing but unintended consequences can also be monitored and mitigated through quality improvement approaches. But the active use of wearables and sensors means there will be a very high density of information flowing into systems, which will require effective and efficient data storage as well as facilitative tools to interpret the data and make it meaningful for all stakeholders.
Supporting stakeholders
Each member of the care team is interested in knowing the impact of the social prescribing through different lenses, so capturing information and presenting it to the relevant member of the team in the right way at the right time is essential. Stakeholders will need up-to-date information on what is available in the community, if patients are engaging with the intervention and whether it has been useful for them. Related to this is the transparency of the quality, evaluation and impact of digital tools which in turn will help build trust.
Let the health and care disruption begin!
To advance the use of social prescriptions, we need to incorporate digital tools and learn from other industries that are already deeply engaged with the everyday lives of their users. Social prescribing supported with technology has the potential to personalise care, bring the person in control of their health and address social determinants of health. While we must continue providing evidence of effectiveness and safety and address novel aspects of safety around data and privacy protection, a bigger mindset shift will be needed to ensure that technology-enabled social prescriptions should also be driven by good user experience and this will require that all of the players in the health and care ecosystem move beyond their existing siloes and adopt a more collaborative approach that sees seamless interfaces, a task particularly suitable to digital tools. As Fjord puts it, we live in the era of Liquid Expectations: When consumers engage with a brand today, such as an airline or a bank, they compare their experience not only with other airlines or banks but also with any service company, such as ride-sharing providers. Take the seamless and largely invisible payment systems these providers offer. Now consumers want payment experiences like this in every industry, consciously or subconsciously.
15
