Abstract
Objective
To report the reasons why doctors are considering leaving medicine or the UK.
Design
Questionnaire survey.
Setting
UK.
Participants
Questionnaires were sent three years after graduation to all UK medical graduates of 2008 and 2012.
Main outcome measures
Comments from doctors about their main reasons for considering leaving medicine or the UK (or both).
Results
The response rate was 46.2% (5291/11,461). Among the 60% of respondents who were not definitely intent on remaining in UK medicine, 50% were considering working in medicine outside the UK and 10% were considering leaving medicine. Among those considering working in medicine outside the UK, the most commonly cited reasons were to gain wider experience, that things would be ‘better’ elsewhere and a negative view of the National Health Service and its culture, state and politics. Other reasons included better training or job opportunities, better pay and conditions, family reasons and higher expectations. Three years after graduation, doctors surveyed in 2015 were significantly more likely than doctors surveyed in 2011 to cite factors related to the National Health Service, to pay and conditions, to their expectations and to effects on work–life balance and patient care. Among those considering leaving medicine, the dominant reason for leaving medicine was a negative view of the National Health Service (mentioned by half of those in this group who commented). Three years after graduation, doctors surveyed in 2015 were more likely than doctors surveyed in 2011 to cite this reason, as well as excessive hours and workload, and financial reasons.
Conclusions
An increasingly negative view is held by many doctors of many aspects of the experience of being a junior doctor in the National Health Service, and the difficulty of delivering high-quality patient care within what many see as an under-funded system. Policy changes designed to encourage more doctors to remain should be motivated by a desire to address these concerns by introducing real improvements to resources, staffing and working conditions.
Introduction
After completing their undergraduate courses, medical graduates in the UK undertake a two-year broad-based foundation programme designed to prepare them for an entry to specialist training in hospital practice or general practice (family medicine). 1 Although there have always been some who have taken time out at the end of foundation training, for various reasons, the great majority have proceeded immediately to specialist training. However, the picture is changing. The percentage of doctors who have progressed immediately from foundation training to specialty training in the UK has declined steadily from 71% in 2011 to 50% in 2016. 2 The numbers of doctors applying for Certificates of Good Standing (which enable UK-based doctors to work abroad) have increased in recent years: by 12% between 2008 and 2013. 3 A 40-year study of doctors’ careers found that, surveyed three years into their careers, 90% said that they would ‘definitely or probably’ practise medicine in the UK in 1977–1986, 81% in 1996–2011 and 64% in 2015. 4 Therefore, there is a clear trend towards leaving UK medicine, at least for a period, and/or delaying specialty training in the UK.
A study of UK-trained doctors who had emigrated to New Zealand found that the reasons doctors gave for leaving the UK included lifestyle, to be with family, to travel and dissatisfaction with the NHS. 5 Job satisfaction among the New Zealand-based doctors was higher than among UK-based doctors working in the NHS. 5
We know from surveys of senior doctors who work abroad that over two-thirds of them do not intend to return to UK medicine and that they would only consider returning to the UK if changes were made to the clinical–political interface, funding, pay, working hours, work–life balance and management. 6
In addition to the usual push and pull factors for leaving UK medicine, there are new factors at play. Doctors are currently in a period of contractual uncertainty with the UK government. 7 Junior doctors surveyed two years after graduation indicated that, in some cases, contractual issues had been a factor in a choice to switch specialty, and many doctors said that they now felt less valued. 8 Doctors also face an uncertain economic outlook in the light of the UK’s impending exit from the European Union. 9
Our aim in this paper is to report the reasons doctors gave, in two recent surveys undertaken three years after graduation, for considering leaving medicine or the UK. We report data from doctors who graduated from UK medical schools in 2008 and 2012, surveyed respectively in 2011 and 2015.
Methods
The UK Medical Careers Research Group surveyed the UK medical graduates of 2008 and 2012. We sent postal questionnaires three years after qualification (in 2011 and 2015). Up to four reminders were sent to non-respondents. Further details of the methodology are available elsewhere. 10
Our surveys were multipurpose and covered many aspects of the doctors’ career intentions, career progression and views. Among these questions we asked doctors: ‘Apart from temporary visits abroad, do you intend to practise medicine in the United Kingdom for the foreseeable future?’ (with the options being Yes-definitely, Yes-probably, Undecided, No-probably not and No-definitely not). Those doctors, who did not answer ‘Yes-definitely’, were asked if they were considering: ‘practising medicine abroad’, ‘leaving medicine but remaining in the UK’ or ‘leaving medicine and leaving the UK’. Doctors who indicated that they were considering one of these options were asked: ‘What is your main reason for doing so?’ (with the doctors being asked to respond in their own words).
We analysed the quantitative data by cohort, sex and specialty group using cross-tabulation and χ2 statistics (reporting Yates’s continuity correction where there was only one degree of freedom). Respondents were grouped for analysis into four specialty groups: hospital medical specialties; hospital surgical specialties; general practice; and other hospital specialties combined (paediatrics, emergency medicine, obstetrics and gynaecology, anaesthetics, radiology, clinical oncology, pathology and psychiatry).
In order to analyse the responses to the open question ‘What is your main reason for doing so?’ (that is, considering leaving medicine and/or the UK), we first divided the doctors into those who were considering leaving the UK and those who were considering leaving medicine (Appendix 1 contains details about how these were allocated). We used content analysis, 11 identifying themes raised and their context, to develop a coding scheme for the responses given by each group of doctors. We did not use an entirely inductive approach, but instead began with the knowledge of themes from our similar research in this area and added deductively from within the data: a hybrid approach. 12 Each scheme reflected the themes and sub-themes raised within the answers. Two researchers independently coded the answers, which were presented for coding in random order and without knowledge of which survey each comment corresponded to, with differences in coding being resolved through discussion. We found that by assigning each comment up to three codes, we were able to adequately encode the richness of the responses. We protected the anonymity of the doctors by redacting references to hospital trusts, medical schools and other identifying information.
Results
Response rates
We surveyed 12,200 UK doctors. The aggregated response rate from contactable doctors, over both surveys, was 46.2% (5291/11,461). Responses to the surveys were 49% (3228/6540) in 2011 and 42% (2063/4921) in 2015 (Appendix 1). Of 5291 doctors who responded, 78 completed a short questionnaire which did not include any questions about intentions to leave medicine or the UK: these are excluded from the analysis. The rest of this paper focuses upon the remaining 5213 respondents.
Intentions to practise medicine in the UK
In response to the question ‘Apart from temporary visits abroad, do you intend to practise medicine in the United Kingdom for the foreseeable future?’, 39.4% replied ‘Yes-definitely’ (Appendix 1). A full analysis of this question is contained in our companion paper. 4 Of the remaining 60.6% of doctors, 83.4% were considering ‘practising medicine abroad’, 17.0% ‘leaving medicine but remaining in the UK’ and 7.3% ‘leaving medicine and leaving the UK’.
Intentions to leave the UK
Of the 3145 doctors who said that they were not definitely intent on remaining in UK medicine, 2523 doctors provided comments about their reasons for considering leaving the UK (Appendix 1).
Comments about reasons for considering working in medicine outside the UK, percentages and numbers: by survey year.
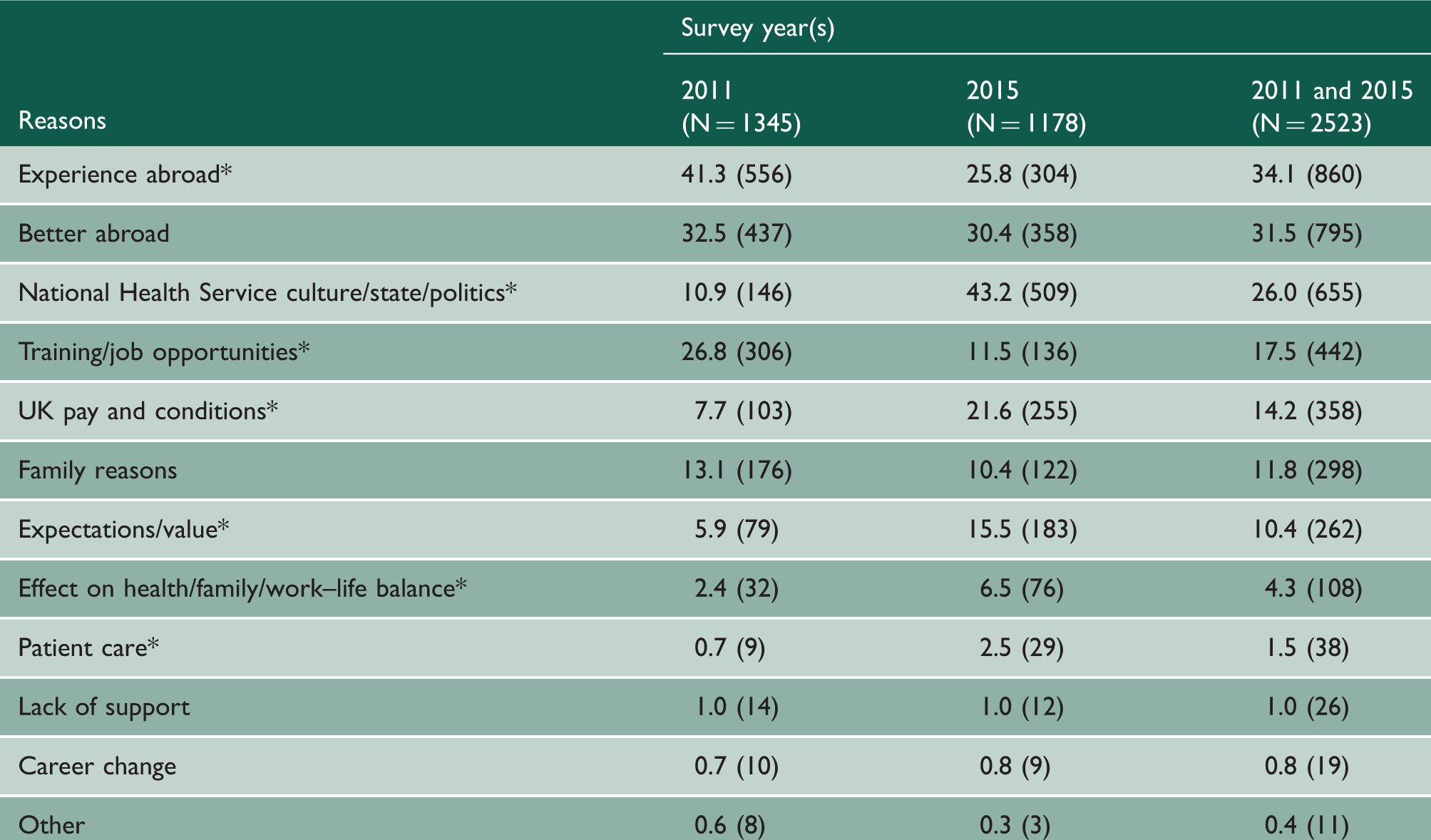
Percentages in each column add to more than 100% because some doctors cited more than one reason.
p < 0.001; significance tests, comparing 2011
and 2015:
Three years after graduation, doctors surveyed in 2015 were significantly (p < 0.001) more likely than doctors surveyed in 2011 to cite ‘National Health Service culture/state/politics’ (43.2% in 2015, 10.9% in 2011), ‘UK pay and conditions’ (21.6%, 7.7%), ‘expectations/value’ (15.5%, 5.9%), ‘effect on health/family/work–life balance’ (6.5%, 2.4%) and ‘patient care’ (2.5%, 0.7%). Doctors surveyed in 2011 were significantly more likely than doctors surveyed in 2015 to cite ‘training/job opportunities’ (26.8% in 2011, 11.5% in 2015) and ‘experience abroad’ (41.3%, 25.8%).
Gender differences in the reasons given were generally modest. Women were more
likely than men to cite ‘family reasons’ (14.6% women, 7.7% men;
Selected quotations about reasons for considering leaving the UK.

Quote number cross-refers to the ‘Results’ section.
Experience abroad
Many doctors wanted to work abroad to gain experience of another country and a different health system (Box 1, quotes 1 and 2). For some doctors, there was a desire to help people in developing countries, perhaps for charity work, and sometimes for religious reasons (Box 1, quotes 3 and 4). Some doctors wanted to develop career interests which could not be pursued in the UK (e.g. tropical medicine, international health; Box 1, quote 5). A few doctors said that they would be travelling abroad as part of their armed services job (Box 1, quote 6).
Better abroad
Doctors considered the lifestyle offered by other countries, such as Australia and New Zealand, to be better than that offered by the UK. Doctors believed that there were many reasons why living abroad would be better: lifestyle, work–life balance, working conditions, pay, economic prospects and climate (Box 1, quotes 7–9). Some doctors had favourable experience of working abroad or were already living abroad at the time of the survey (Box 1, quotes 10 and 11).
National Health Service culture/state/politics
Many doctors bemoaned the state of the National Health Service and expressed uncertainty around proposed new contracts (Box 1, quotes 12 and 13). This issue was raised in the 2011 survey, but was much more frequent in the 2015 survey. Many doctors complained about political factors, and uniquely in our experience, some even named the current Health Secretary for the National Health Service in England as the reason for their desire to work abroad (Box 1, quotes 14 and 15).
Training/job opportunities
Several doctors wanted to enhance their training and skills, and many felt that they could not do so in the UK (Box 1, quotes 16 and 17). There was concern that training in the UK was too rushed and that doctors were forced to specialise too early (Box 1, quotes 18 and 19). Several doctors believed that training opportunities in the UK were too limited, involved being sent around the country and that posts were also limited at the end of training (Box 1, quotes 20 and 21).
UK pay and conditions
Many commenters said that working conditions in the UK were too difficult. This included excessive working hours and workload, and too much stress. Several doctors considered pay to be too low (Box 1, quotes 22 and 23).
Family reasons
Several doctors wanted to work abroad because their family and friends lived abroad, or because their partner was going abroad and they would like to accompany them (Box 1, quotes 24–26).
Expectations/value
Many doctors, especially those surveyed in 2015, felt undervalued and talked about low morale (Box 1, quote 27). Doctors were unhappy about images of doctors within the media and felt that these images were influenced by the government and then filtered down to the public resulting in low public esteem for doctors (Box 1, quote 28).
Effect on health/family/work–life balance
Several doctors were concerned that their job was affecting their health or their family and that their work–life balance was poor or getting worse (Box 1, quotes 29 and 30).
Patient care
Some doctors felt that patient safety was compromised by proposed contract changes (Box 1, quote 31). A few doctors talked about ‘sub-optimal’ or ‘sub-standard’ conditions for patients (Box 1, quotes 32 and 33).
Lack of support
A few doctors complained about a lack of support from their seniors, and from management. Some doctors were also affected by bullying or harassment (Box 1, quotes 34 and 35).
Career change
A few doctors had doubts about medicine as a career or disliked the job content (Box 1, quotes 36 and 37).
Intentions to leave medicine
Of the 3145 doctors who said that they were not definitely intent on remaining in UK medicine, 476 doctors provided comments about their reasons for considering leaving medicine (Appendix 1).
Comments about reasons for considering leaving medicine, percentages and numbers: by survey year.
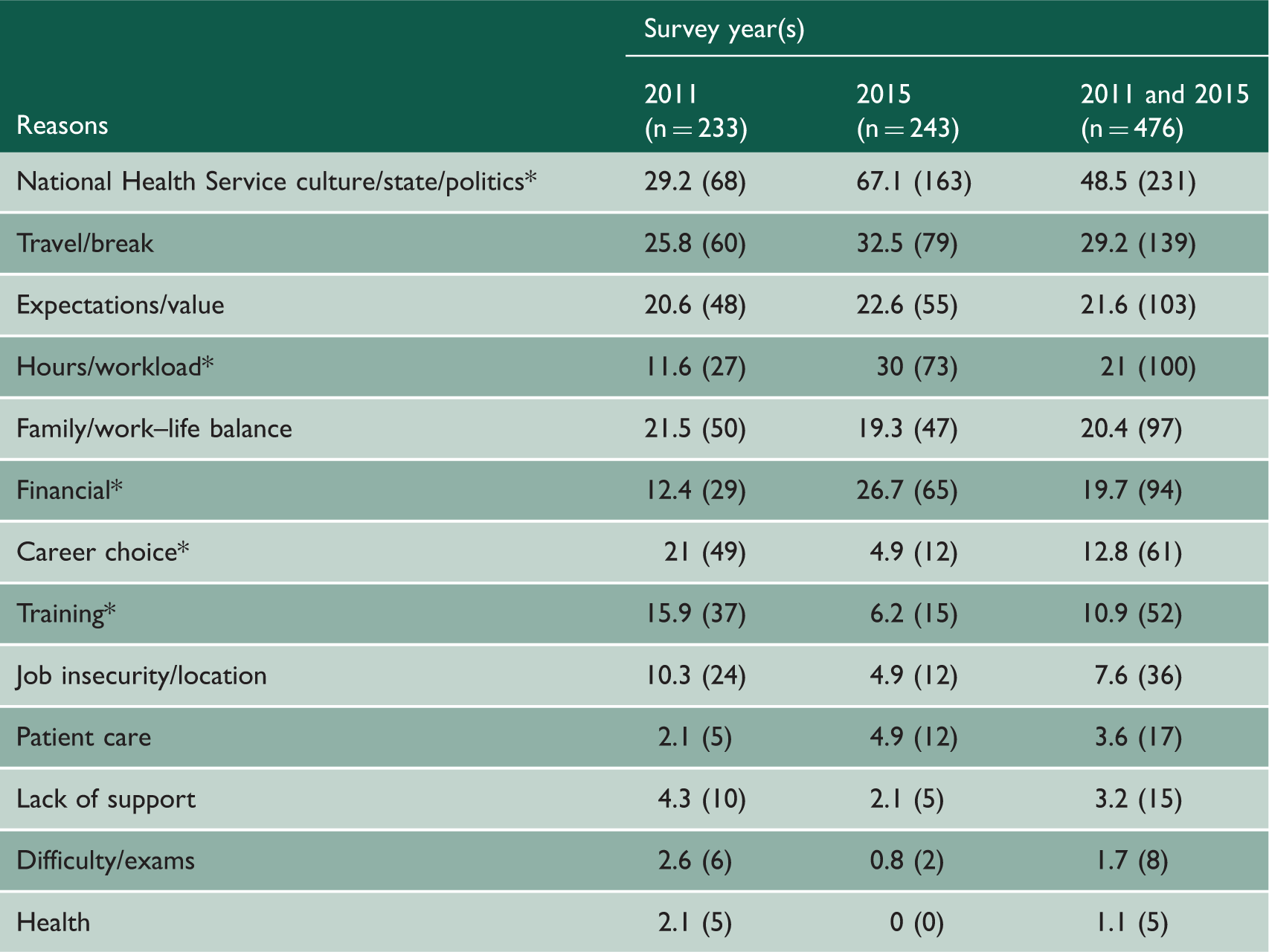
Percentages in each column add to more than 100% because some doctors cited more than one reason.
p < 0.001; significance tests, comparing 2011
and 2015:
Three years after graduation, doctors surveyed in 2015 were significantly more
likely than doctors surveyed in 2011 to cite ‘National Health Service
culture/state/politics’ (67.1% in 2015, 29.2% in 2011;
Women were significantly more likely than men to cite ‘family/work–life balance’
(25.5% women, 12.1% men;
Selected quotations about reasons for considering leaving medicine.

Quote number cross-refers to the ‘Results’ section.
National Health Service culture/state/politics
Many doctors said that the reason they were considering leaving medicine was because of the state of the National Health Service, and uncertainty around future contracts (Box 2, quotes 1 and 2). Many of these doctors blamed the government for ‘damaging’ the National Health Service (Box 2, quotes 3 and 4). This issue was raised more frequently in 2015 than in 2011 survey.
Travel/break
Many doctors expressed a desire to travel to experience another culture (Box 2, quote 5). Some doctors wanted to have a break from medicine (Box 2, quote 6). Others were leaving medicine to stay with their partners (Box 2, quote 7).
Expectations/value
Many doctors felt undervalued, unappreciated and felt that their professional status was being eroded (Box 2, quotes 8 and 9). Doctors talked about low workforce morale (Box 2, quote 10).
Some doctors also felt a lack of respect, and some hostility, from patients (Box 2, quote 11).
Hours/workload
Another topic raised more in 2015 than in 2011 was excessive working hours and workload (Box 2, quotes 12 and 13). Many considered the workload to be unsustainable (Box 2, quote 14).
Family/work–life balance
Many doctors were unhappy with the small amount of time they could spend with their families and were leaving medicine in order to achieve work–life balance (Box 2, quotes 15 and 16).
Financial
Some doctors believed that they were not paid enough for the hours they worked (Box 2, quotes 17 and 18). A few doctors compared their profession with other professions and concluded that they would be better paid elsewhere (Box 2, quotes 19 and 20).
Career choice
Many doctors, especially those surveyed in 2011, were unsatisfied with medicine (not just for financial reasons) and wanted to change career (Box 2, quotes 21 and 22).
Training
Several doctors complained of poor quality, or restrictive and inflexible training (Box 2, quotes 23 and 24). A few doctors felt that there were fewer training opportunities for less-than-full-time doctors (Box 2, quote 25). Doctors often described training as being too dominated by service provision (Box 2, quote 26). A few doctors felt that there was a lack of training posts (Box 2, quote 27).
Job insecurity/location
Several doctors were concerned about job shortages and excessive (or unfair) competition (Box 2, quotes 28 and 29). Many doctors also felt that it was difficult to obtain a medical job in their desired location (Box 2, quote 30).
Patient care
A few doctors described ‘unsafe’ working conditions, and target-based not patient-focused medicine (Box 2, quotes 31 and 32).
Lack of support
Some doctors felt that they did not receive enough support, respect or encouragement from their seniors (Box 2, quotes 33 and 34).
Difficulty/exams
A few doctors described unreasonably high expectations, and found the exams onerous (Box 2, quotes 35 and 36).
Health
Some doctors mentioned that their health had made them consider leaving medicine. For one doctor, this involved deteriorating mental health, but some doctors simply said ‘for health reasons’ (Box 2, quote 37).
Discussion
Main findings
Almost two-thirds of junior UK-trained doctors surveyed in 2011 and 2015 were not definitely intent on remaining in UK medicine. Half of these doctors were considering working in medicine outside the UK and 10% were considering leaving medicine.
Among those who were considering working in medicine outside the UK, comments which we have characterised as saying that respondents felt life would be better abroad, and comments relating family reasons for leaving, were made in roughly equal measure both in 2011 and 2015. However, comments we characterised as relating to the state of the National Health Service, UK pay and conditions, expectations and values, work–life balance and adverse effects on patient care were all made much more frequently by doctors in 2015 than in 2011. In sharp contrast, reasons relating to opportunities for better training, job opportunities and experience abroad were mentioned much more frequently by doctors in 2011 than in 2015.
A similar pattern was observed in the reasons doctors gave for considering leaving medicine altogether. In 2015, the dominant reason for leaving medicine was the state of the National Health Service as respondents saw it. Excessive hours and workload, and financial issues, were also strong factors in decisions to leave medicine. In 2011, the reasons given were more diverse, with concerns about training, career choice and job security being more common than they were in 2015.
Strengths and limitations
This was a large-scale national study of doctors who graduated from UK medical schools in 2008 and 2012. The response rate was 49% and non-responder bias may have been present.
Not everyone gave us reasons for considering leaving medicine or the UK. However, four-fifths of respondents who were not definitely intent on remaining in UK medicine provided comments about their reasons for considering leaving the UK. Fewer respondents provided comments about their reasons for considering leaving medicine, but fewer doctors were considering this option; therefore, fewer comments were to be expected.
Comparison with existing literature
In our study, there was a sharp fall between 2011 and 2015 in the percentage who were definitely going to practise medicine in the UK. This trend is mirrored in the decreasing numbers of doctors moving into specialty training over recent years. 2
Our respondents were considering leaving UK medicine to gain experience of a different country and health system, due to perceptions that things were ‘better abroad’, to avoid National Health Service culture/state/politics, and for better training and job opportunities. These reasons were also found in a study of UK-trained doctors working in New Zealand, 5 but our more recent survey has found that dissatisfaction with the National Health Service, and with the politics surrounding it, is now more of a push factor: especially for doctors surveyed in 2015. A more recent study of UK-trained doctors in New Zealand found that, as with our study, younger doctors were more likely to say that their motivation for leaving the UK was to leave the National Health Service. 13
UK pay and conditions also became more influential for doctors surveyed in 2015, compared with those surveyed in 2011. A study of health professionals who had emigrated from Ireland, surveyed in 2014, found that their main reasons for emigrating were difficult working conditions. 14
Implications/conclusions
The reasons doctors gave for considering leaving UK medicine were many and varied. Within that, comparison of the 2011 and 2015 results shows an increasingly negative view is held by many doctors of many aspects of the experience of being a junior doctor in the National Health Service, and the difficulty of delivering high-quality patient care within what many see as an under-funded system. Policy changes designed to encourage more doctors to remain should be motivated by a desire to address these concerns by introducing real improvements to resources, staffing and working conditions. Effort should also be made, at the level of senior staff and employers, to change culture and make junior doctors feel valued.
