Abstract
Historically, opioid use has been problematized to serve various socio-political interests. To understand the present construction and management of opioid “dependence,” across 2023, an Opioid Substitution Treatment service was assessed in Aotearoa, New Zealand. This article outlines the day-to-day work at this service, to assess how it is informed by treatment guidelines, and the interests of staff, service users, and policy makers. Using Institutional Ethnography, nine informants were interviewed from these groups, their work at the service was observed, and the texts that were activated through this work (such as treatment guidelines) were assessed. Findings are organized into a map of the treatment institution; informants’ work is connected by the associated texts. This map is described to show the interests that pervaded these, and how they were activated in informants’ work, and informed their understandings of opioid dependence. From these texts to the talk of the informants, there is a persistent understanding of “successful recovery” as requiring individuals to become self-responsible. However, though dominant (responsibilizing) modes of constructing opioid dependence and recovery are identified, these manifest paradoxically in practice, as service user autonomy is both promoted and restricted. How service users described themselves and their opioid use is equally varied, but also leveraged opportunistically by this group. It is argued that there is evidence of a complex performativity of dependence amongst the research informants. Service users understood themselves and their dependence in anticipation of the expectations of the service, but also in resistance to these, despite the service's seeming intent.
Introduction
From monomania of the will to the subject of criminalization, the trajectory of how opioid use has been conceived and managed shows it to be susceptible to appropriation—a locus at which various socio-political values and interests are constantly being negotiated (Bergschmidt, 2004; Fischer et al., 2004; Valverde, 1998). In modern treatment practices, though, the motivations behind categorizing those using opioids are obscured behind claims of objective, evidence-based practice, which target physiological issues such as withdrawal and tolerance (Campbell, 2012). Supported by Professor Peter Adams, and Associate Professors Bruce Cohen and David Newcombe, I (Dr Oliver Birch, the primary author and principal researcher) thus began an inquiry aiming to investigate claims that dependence could be solely the product of objective diagnoses; that these diagnoses identified a knowable, internal quality within the opioid user, similar to a disease, that could be located and treated through medicines. What, we wondered, could be learned from the latest treatment approach for managing opioid use? How were modern opioid treatment services set up, and what did this say about how people using opioids are perceived?
Through this article, we first cover the background and methodological development of this project. We then detail the key findings from my study of an Opioid Substitution Treatment (OST) service in Auckland, Aotearoa, New Zealand (NZ). Operated by a multidisciplinary team of medical and allied health staff, these services provide substitute opioids (such as methadone or buprenorphine) to those diagnosed with an opioid dependency. Through an Institutional Ethnography, we create an empirical account of how dependence is contested and acted upon in terms of informants’ talk and work at the service, and assess how this is shaped by various texts, such as standard operating procedures and treatment plans. We argue dependence to be “performative,” as informants’ constructions of opioid dependence were made with reference to (and sometimes, in resistance to) the OST service's modes of constructing this category through its practices and texts (Butler, 2000). In what follows, the occasional use of first-person pronouns is limited to passages that reflect the primary author's independent undertaking of data collection, analysis, and writing. In all other instances, to acknowledge supporting authors’ input into the study's methodological development and manuscript review, a collective or neutral voice is maintained.
Dependence Politicized: Framing the Inquiry
OST has been argued to create self-managing subjects who consume substances in ways that do not impede their ability to be productive (Niculescu, 2012; Oksala, 2013). The proliferation of medical experts in the “conduct of conduct” has been argued as decisive to this end (Miller & Rose, 2008, p. 149). At treatment services, experts such as psychologists and psychiatrists are argued to shape and inform patients’ self-regulation in relation to neoliberal norms of rational consumption and productivity. Individuals diagnosed as dependent are adjudged to have failed to manage the relations required by neoliberal modernity and are relegated to the status of the other (Reith, 2004). Rather than enriching their lives with moderate consumption—consumption that does not threaten autonomy and productivity—they have become overwhelmed by immoderate impulses. Through treatment, by recalibrating subjects in line with norms that are established (at least in part) by these clinics, the threat to modern social apparatuses of dysfunctional (unproductive, irrational, and so on) conduct is curbed (Rose, 1999).
Guerra-Barón (2017) suggested that OST achieves this through surveillance. Internationally, treatment regulations often mandate observed opioid medication dosing, regular (and random) urine testing, and general observation, establishing what Mendoza et al. (2019) called a “quasi-punitive ethos” (p. 244). This occurs in Aotearoa NZ, despite national treatment guidelines acknowledging it maintains “strong connotations of a surveillance agenda being valued over a therapeutic agenda” (Ministry of Health, 2014, p. 25).
According to Keane (2009), these processes create knowledge on service users and their opioid use, but also motivate self-policing. Regarding the creation of knowledge, Fischer et al. (2004) argued that OST clinics, through surveillance and subsequent pathologizing, “have mobilized an elaborate new moral code of what defines a responsible, well-behaved and safe drug user and have thus created a pervasive new moral enterprise enacting its own distinct set of norms and values” (p. 362). Through this, self-policing is secured; subjects reproduce their own capture, internalizing surveillance as they act in relation to these norms of “proper” behavior. Substance users’ aspirations, therefore, become aligned with those of the neoliberal state, as drug governance proceeds through this “responsibilization.” To be “good” service users, and more broadly, “good” citizens, they must follow the expectations of the service and become self-managing regarding their treatment, and also their lives more broadly (O’Malley, 2012).
However, despite the speculated intent of OST, Lancaster et al.'s (2023) recent longitudinal study of Australian opioid provision suggests that for service users, dependence might be a situated and relational becoming; their participants were made and remade socially as they enacted their dependence in various ways, in various scenarios. To explore this possibility, in my analysis of OST in Aotearoa NZ, it would have been disingenuous to overlook their constitution as instead resulting from a varied set of values and intentions (only some of which may be considered obviously neoliberal and responsibilizing) (Prince et al., 2006). My intent was not to “expose” a service as being constructed to subjugate its service users through its practices, as has been done elsewhere in literature; as will be shown through this article, OST services are not entirely coherent (and insidious) political machines. Instead, I sought to use this socio-political angle of analysis as a starting point to consider the various conceptions of dependence at an OST service, by whom they are constructed, how they are enacted, and how they are pervaded by conflicting socio-political values. I thus began with the material (the work, expectations, and guidelines) to assess the seeming intent of treatment, to then use this to assess how dependence was constructed at the boundaries of various value-conflicts between actors within the institution of OST.
Methods: Mapping OST
To do so, I adopted Dorothy Smith's Institutional Ethnography (IE), drawing on the conceptual guidance of all listed authors in applying this approach to the study (Smith, 2005). One who conducts IE explicates how those within an institution have their work coordinated by translocal ruling relations. “Translocal ruling relations” shape the socio-political contours of these individuals’ day-to-day lives; institutional interests are inserted into individuals’ activities as they activate institutional texts through their work (McKelvie, 2019). The “institution” is constituted by multiple local settings representing “sites of interface between individuals and a vast network of relations, discourses, and work processes” (McCoy, 1987, p. 105). IE thus seeks to access these networks by assessing individuals’ locally situated work within an institution and how it is organized by texts (McKelvie, 2019).
Within IE, “work” is broadly taken to mean any activity undertaken regularly by those within an institution (Ng et al., 2017). “Texts” are “the material forms of words, images, and sound that we can see, hear, and touch” (Turner, 2006, p. 139). Increasingly, complex organizations rely on texts to standardize work across varied settings (hence, “translocal” ruling relations) and by various individuals (Smith, 2001). Any project seeking to describe the apparent intent of an institution's practices would be remiss to not include an assessment of the texts that are activated by various actors as they undertake these. Within IE, texts must be replicable (Smith & Turner, 2014). They must be reproduced so that individuals may access the same texts in different settings, or at different times (or both). This, according to Smith (2006), organizes these individuals, “hooking up an individual's consciousness into relations that are translocal” (p. 66). Texts are seen as having no agency; the organizing of work is something the text could not accomplish without being activated (read, seen, or heard and consequently interpreted, then acted upon) by people (Dobson, 2001). What is critical is how the text is encoded with various interests, and how this encoding affects work when informants interact with the text. By approaching texts in this manner, the ethnographer is able to see the institution in motion.
In this research, the institution was that of OST provision in Aotearoa NZ. This included the local setting, at which I, and most of my participants were situated, but it also accounted for the external health care and social service providers associated with specialist services by the 2014 national OST guidelines in Aotearoa NZ (Ministry of Health, 2014). More broadly, the institution was the sum of any activities and interactions that functioned to treat opioid use nationally. It thus included the work of the policy makers who are tasked with creating the legislation that guides OST services, and a GP who had previously been involved with opioid provision.
Nationally, OST is one of two primary pharmacological responses to opioid use, alongside managed withdrawal (Ministry of Health, 2014). Barring exceptional circumstances such as court diversions, specialist services represent a voluntary entry point for those requesting treatment for opioid use (Ministry of Health, 2014). Since 2014, the Ministry of Health—in their opioid substitution practice guidelines—has sought to introduce a “recovery model” of service provision (Ministry of Health, 2014). According to these guidelines, “recovery is a broader and more complex journey that incorporates overcoming dependence, reducing risk-taking behavior and offending, improving health, functioning as a productive member of society and becoming personally fulfilled” (Ministry of Health, 2014, p. 36). Services are expected to: assess substance use and related concerns; develop individualized, recovery-oriented treatment plans; stabilize clients on substitution opioids; deliver harm-minimization interventions; provide psychosocial support to help clients and their whānau (the Māori word for one's extended family); transfer stabilized clients to primary care; and assist in withdrawal from OST when appropriate (Ministry of Health, 2014).
The service the study was situated at was operated by a multidisciplinary team of case workers, doctors, nurses, pharmacists (who operate an in-house pharmacy), and consumer liaison staff (who work on behalf of service users to advocate for their treatment needs). It is the largest service (in terms of enrollment) in the country (Schwarcz, personal communication, November 24, 2021). Induction to the service involves referral through another health service, agreement to an assessment by a prospective service user, and screening by service staff to determine suitability. This screening includes an assessment of one's health and social history, the conferral of a diagnosis (if appropriate), and the subsequent development of an individualized treatment plan. An in-house pharmacy (which makes this service unique compared to all others in Aotearoa NZ) was used to manage service users through induction and stabilization. Stabilization requires the service user to collect their medication from the in-house pharmacy, while staff find the appropriate dosage (to render the individual physiologically stable) through titration. Initially, service users are expected to collect their doses and consume them in front of available staff so that they may be monitored.
Eventually, service users may be offered takeaway doses. These are doses of opioids that are not consumed under clinical observation (at an OST center or at a pharmacy). To become eligible, service users must demonstrate “stability, reliability, and the ability to comply with the safety requirements of unsupervised consumption as specified by the individual specialist service” (Ministry of Health, 2014, p. 36). While the service manages the treatment of over 1,000 service users, the majority of these are in a “shared care agreement” with their GP and the specialist service, which can only begin after stabilization (and a period of “ongoing OST”) (Schwarcz, personal communication, November 24, 2021). Shared care requires the OST service to continue supporting service users and their respective General Practitioners (GP) regarding appropriate treatment delivery; however, it is the GP who will be prescribing the required opioids, and the service user is required to collect their medication from a community pharmacy. A service user may begin withdrawal from treatment when their treatment goals have been attained, as well as a level of stability that will give them a chance of maintaining their long-term use goals (Ministry of Health, 2014).
Across 2023, I moved iteratively between observations of work, interviewing informants regarding their work, and analyzing any texts I was directed to through my interviews and observations. I, as the primary author, conducted data collection and analysis. My aim was to understand how service texts were encoded (with values), and how actors within the institution interacted with these, and activated the texts through their subsequent work. My observations took place largely within staff meeting rooms to encounter how they talked about their work. I was also afforded opportunities to observe the service more generally, to see how staff work differed (if at all) from their talk of it in meetings, and to also witness service users’ work within the service. When I was able to see the rest of the service, I noted its layout and built structure, who could go where (and who could not), the work that was happening, and who was involved. More often, I attended monthly operational and governance meetings, in which staff discussed the day-to-day translation of service guidelines into work, as well as their responsibilities given their roles. Notes taken during these meetings were organized into several categories; these included examples of potentially noteworthy work, texts, plus my personal reflections on intangibles such as the atmosphere and tone of the meetings for broader context. I also noted any outstanding queries I had regarding what had been discussed during the meetings, to then follow these up in future interviews with staff.
When analyzing texts, it was their materiality that was of principal concern, as I aimed to understand how their encodings affected work. To do this, using a Microsoft Excel file, texts were read, and extracts from them were organized by the following categorizers, whereby to each, I asked (amongst other things), where it was found, who could access it, what metaphors and manners of framing were used in the text, and how it might inform future work. I was assessing the way the text was constructed, and the socio-political values and interests implicit in this. I was also looking at who used the text and where it could be found to see how it might be accessed by a variety of informants. Through analyzing texts in this way in combination with interviewing informants, I was aiming to examine through my informants’ accounts how texts directly organized their work, to show how values and interests pervaded what happened at the institution.
I interviewed three service users, three service staff, two treatment policy makers, and one GP (who had previously managed shared care agreements). The latter three were located outside of the service, but within the broader institution of OST provision. Each interview was around one hour in length. I began with service users due to my early observations of the service, and my initial engagements with service guidelines and Standard Operating Procedure (SOP) texts; much of the work and texts of the institution were seen to be directly affecting them, and I was primarily interested in the management of people using opioids (Melon, 2012). The decision to include the remaining informants emerged from insights gained during these initial interviews. This iterative approach is typical within IE (Turner, 2006).
After transcribing each interview, the data were organized within a Microsoft Word document for relevance. Transcripts were sorted by examples of institutional work, notable texts mentioned, my personal reflections on the interview, any additional noteworthy comments from informants, and any outstanding queries I had based on what they said, which I could then follow up on in the next interviews. After indexing each transcript, I updated my interview schedule to reflect my evolving understanding of the institution and to guide subsequent interviews. Later interviews and analyses were shaped by these early findings, as I examined how different groups’ work and understandings of dependence varied by their institutional position and how they activated key texts. Each interview directed me to the next, as each informant highlighted the texts that informed their work, while also implicating other prospective informants who were described as having their work organized through these texts as well.
Through this iterative process, a “map” of the institution was built, which then grounded the analysis (Turner, 2006). This is typical within IE; key work processes are linked by the texts that organize them. Work is shown to be occurring, texts are shown as being amended based on this work (such as when recovery plans—which will be discussed later—document service user “recovery” progress), actualities are abstracted by this documenting of work (as according to the encoding of texts), and others’ work is then informed by these amended texts. A map is a cartography of efforts to “follow the breadcrumbs”; within IE, one moves iteratively between findings from interviewing, completing observations, and analyzing texts, tracing textual sequences along the way (Turner, 2006). The map depicts a social landscape to make visible how informants are linked and organized. Mapping allowed me to visualize who undertakes what on behalf of texts, and why—relative to their position in the institution. Acknowledging textual sequences—how texts are perceived, acted upon, and amended—allowed for analysis of the ways by which socio-political values pervade work and therefore the management (and understanding) of opioid use. Through this, we describe how OST informed how those at the service have come to describe themselves, and in the case of the service users, their own opioid use.
In the following section, then, we offer the key findings from “a” map of the institution, rather than “the” map. These represent only the sum of encounters with texts and informants. The map was not exhaustive, nor representative. Our aim, though was not to argue that the institution is one, knowable monolith which consistently manages service users to a particular end. Rather, through my map, we uncovered examples of various texts organizing work (but also, failing to organize work) to a variety of ends. Mapping findings was merely a means of moving from scrutinizing individual examples of work and texts, to visualizing how both are related, so that we could then assess how and why they related to each other as they did; to see how work was textually mediated, and how texts are amended based on work. It is a way of moving my analysis from the local (what I noted while at the service), to the institutional (in terms of ruling relations), to begin to assess the socio-political values that pervaded texts, and how the work that was encountered was organized as the texts were activated.
Results and Discussion: Reading the Map
Here, we offer our results in two parts. First, we provide findings from a map of the institution, to then explicate the responsibilizing ruling relations that organize service users with reference to work and texts. Largely, the findings corroborate previous Foucauldian assessments of OST (Keane, 2009; Niculescu, 2012; Oksala, 2013). However, through contrasting my informants’ accounts (particularly those from staff versus those from service users), and through contrasting what was stipulated with regard to work that “should” be done in service texts, versus what was seen to be happening, we note an autonomy paradox. Though there was a seeming intent to create self-managing substance users in texts and staff talk, this was not routinely realized. Even as this intent was realized, there were several examples of work processes that instead limited the autonomy of service users to various ends. Second, we move the analysis from the institution to the individual (and how it is constituted in part by the institution). Given the seeming paradox, to understand how the institution therefore shapes how my informants constructed opioid use (and dependence) in varying and inconsistent ways, we will here argue dependence to be performative.
Mapping the Responsibilizing Institution
Figure 1 presents the created map. This map depicts the majority of texts analyzed as part of this research and the relevant work processes they inform. Texts are represented by boxes, whereas work is represented by circles. Some of the circles are visually differentiated through being filled to indicate work that is undertaken by service users (who are referred to as SU/SUs in this map), by staff, or jointly between the two (when the filling has a gradient). The circle in the top-right corner of the figure represents work undertaken by informants who worked outside of the service. Unfilled circles denote sub-processes of work; they are undertaken as part of a broader work process. Arrows can be taken to mean “informs,” or “leads to.” For example, the CADS—Medical Assessment AMS Detox (MAMI) text informs how an individual is screened by service staff for admission to the service. To give another example, a service user continuing OST after stabilization leads to other sub-processes of work.
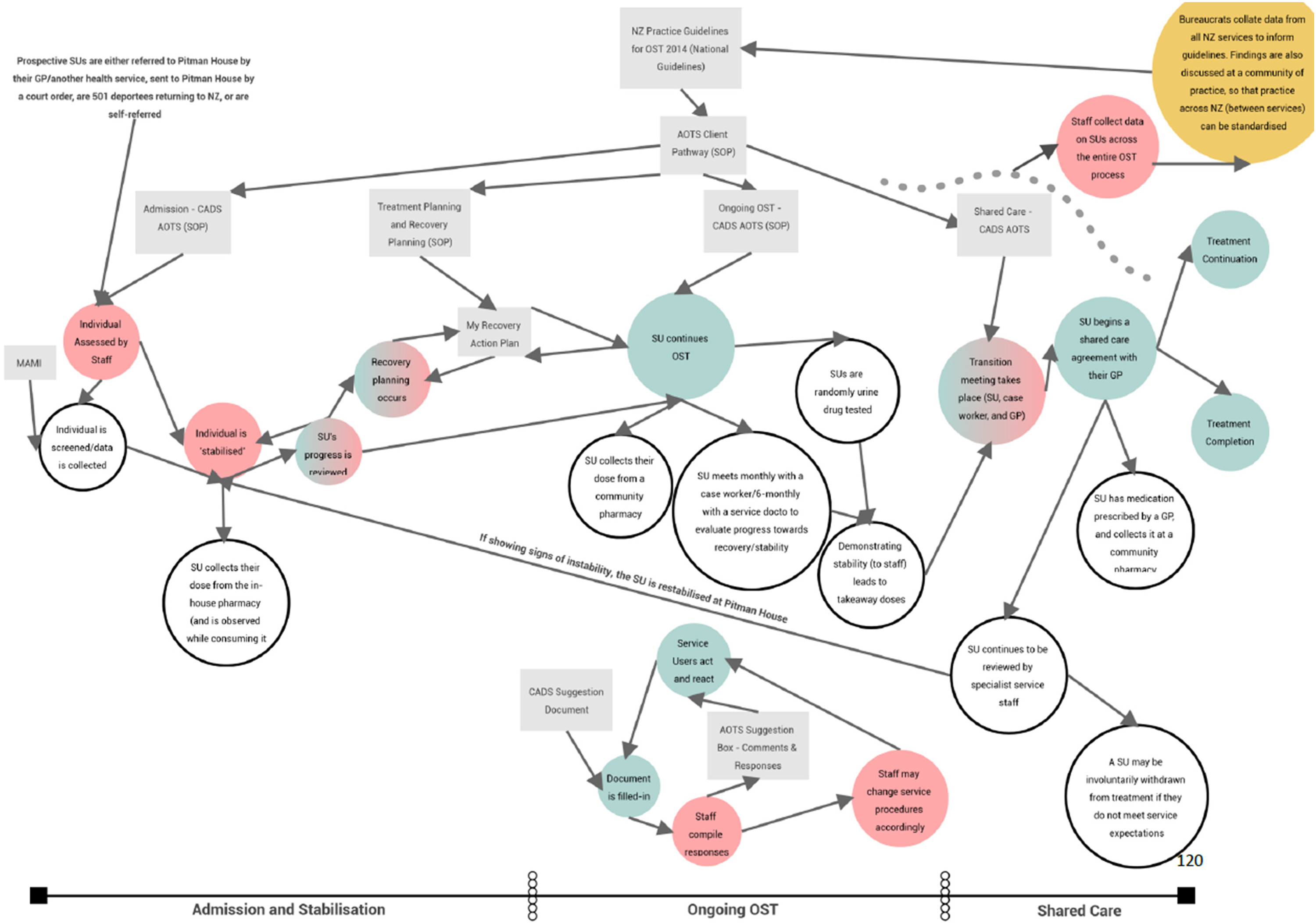
A Map of the Institution of OST.
Also, certain work is required before other work takes place; a service user must be assessed and admitted to the service by staff before they are “stabilized.” Given this, the map is roughly organized in line with the expected treatment trajectory of a service user. From left to right, the first examples of work and texts relate to the admission and stabilization phase, which occurs at the start of treatment. In the middle of the map, all work and texts shown are part of the “ongoing OST” phase. On the right is the shared care phase (though there is an acknowledgment here that the service users’ journeys are not necessarily linear, as they can be returned to the stabilization phase if staff are concerned regarding their progress). Note too the textual hierarchy, which is represented through the vertical organization of the texts. The national guidelines are shown to affect how SOPs are written and utilized, while those SOPs affect how texts such as the “My Recovery Action Plan” (assessed in detail subsequently) are written, and these then organize work.
Several textual sequences were acknowledged through the mapping process. For brevity, we focus here only on the sequence involving the “My Recovery Action Plan” text. We do so because this text was seen to coordinate a great deal of work (due to being revisited through regular case worker meetings), and was encoded with noteworthy expectations from the service, particularly regarding the recovery and self-responsibility of service users. A copy of it (refer to Figure 2) was accessed as it was included as part of the Treatment Planning and Recovery Planning SOP document, which was one of the first texts I reviewed. Used during regular meetings between service users and their assigned case worker, this recovery plan was described in the associated SOP as being essential to guiding these meetings and, therefore, the recovery process. As the SOP stated: Recovery plans are based on what the person actively wants for their future; are unique, influenced by each client's personality and values; and require the consumer to take personal responsibility for putting the plan into action. This talk of responsibilizing service users consequently runs through the recovery plan itself.
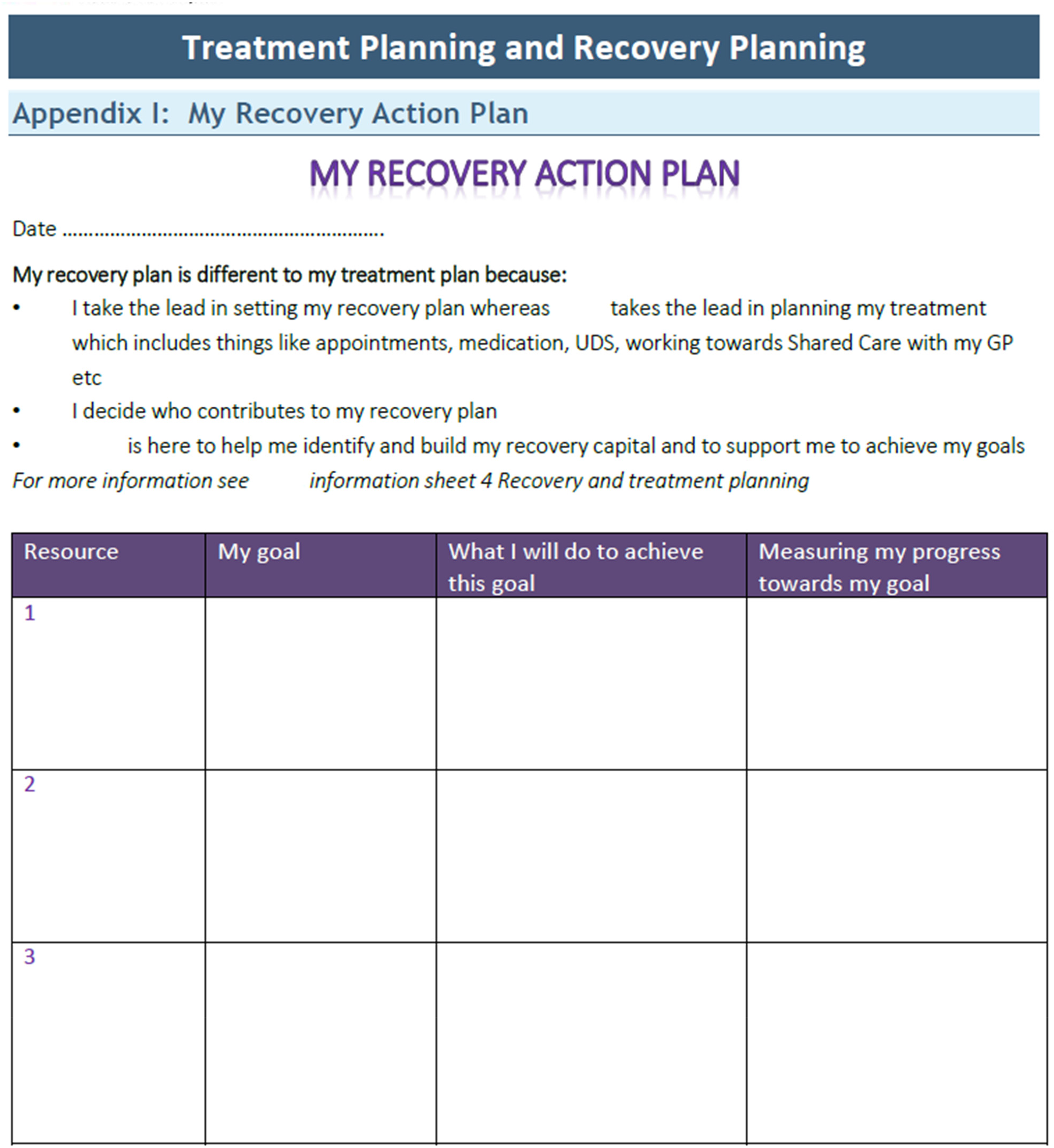

My Recovery Action Plan.
The text is primarily composed of a table, headed by “Resource,” “My goal,” “What I will do to achieve this goal,” and “measuring my progress towards my goal.” Above this table, what separates a recovery plan from an ordinary treatment plan is delineated by the following in bullet-point statements: I take the lead in setting my recovery plan whereas [the service] takes the lead in planning my treatment… I decide who contributes to my recovery plan … [the service] is here to help me identify and build my recovery capital and to support me reaching my goals….
This passage is worded as though it is from the perspective of a service user, implying the contract between service and service user: that compliance with this prescription of each party's responsibilities is required for treatment. [The service] outlines clearly that service users should work towards their own recovery, and that the responsibility of the service is to support this. In the way this text is written, the service user (and their responsibility) is foregrounded; the service itself appears to take a back seat, in a supporting role. How the table is framed reinforces this. Service users are directed to consider their own goals, then determine for themselves how they should achieve these. Space is then left so that in future case worker meetings, service users can be assessed on their progress. The purpose of the individual in attending the service is re-made into goals for improvement that the service user is responsible for actioning.
Relating this back to what is outlined in the associated SOP, this text should “steer the course of the client's engagement with the service” and includes the client's goals, but also the “service's goals” (i.e., that the client achieves stability on their OST medication, risk is managed, and harm is reduced). This text, therefore, organized what we call a “recovery loop.” It (as has been described) pervades with service expectations for service users, but also particular constructions of recovery and stability (as being self-managing). This text was used at case meetings (or at least SOPs stipulate that it should be), to inform service users’ work pertaining to their opioid use. Their work then followed on from this (as did their talk of themselves, as will be noted subsequently), until they have their next meeting again at the service. At this time, the plan could then be amended again to track the service user's progress and plan out further goals. Beyond this textual sequence, though, several key instances of responsibilizing work in my informants’ talk are noted. Generally, how my informants described OST corroborated other studies investigating similar services as sites for managing various interests—as institutions set up to render self-responsible subjects through various vehicles of surveillance and disciplining (and the associated self-disciplining by service users) (Foucault et al., 2008; Rose, 1999).
For example, the in-house pharmacy was observed by me and described by informants as a site for the surveillance of service users. Operating as a “pharmopticon” (following Foucault's interpretation of the “panopticon”), one staff member acknowledged that it provided an opportunity to “monitor” service users, and to “see people” (Foucault, 1995). It was also only open for 3 hr per day, with doses being withheld if not collected within these opening hours. Regarding this, another staff member said that “sometimes people do need a bit of routine,” and that the opening hours can give service users “a reason to get out of bed,” to “shower and get dressed.” Staff mentioned that from the “service's perspective,” there is a “mindset of no more than three takeaways [which are doses that do not have to be consumed onsite under observation],” so service users should “present at least three times a week” to the service, presenting ample opportunities to monitor service users. This was only true when service users were under the specialist care of the service, but when they had been deemed stable enough for shared care, they only had to “present … once a week.” When researching an overseas supervised injection site, Fischer et al. (2004) argued that observation fulfills the purpose of transferring responsibility for risk of harm to the service user (as the service has “done their bit,” so to speak).
Service users were subjected to further surveillance through random Urine Drug Screens (UDSs). Despite one service user describing UDSs as “going down to pee in a jar” and therefore “demeaning,” in a study of equivalent overseas services, Bennett (2011) suggested that these measures continue to be implemented to evaluate the degree to which the tested individual is being rendered compliant with reference to the objectives and regulations of OST; service users are subjected to the gaze of the institution with the intention being the reduction in use of unsanctioned drugs.
The institution of OST, and its complexities and strict regulations revolve around the provision of a controlled substance, which is, in turn, used to justify surveilling its service users. As one member of staff commented, “We're dealing with a controlled medication… A few people ruin it for everyone.” To avoid this, these tests are random. UDS samples were acknowledged by staff as not being regularly scheduled with service users, rather, “some of [the] doctors … will … just request them when the client's booked with [them].” Service users may be subjected to a test without prior knowledge, and so there is the threat of their illicit drug use being detected by the service
Following my mapping process and borrowing from Walby's (2005) Institutional Ethnography of surveillance, we also claim that the texts in action through OST mediate a surveillance circuit that operates to observe and therefore manage the behavior of service users, encouraging them to self-police. Through case notes on service users, recovery plans, and data collection for national treatment legislators, knowledge is generated about service users that pertains to everything from their participation in the service to their personal histories and current circumstances outside of the service. Data conveyed through these texts sustain distanciated surveillance relationships between local and extra-local informants (such as those setting policies and guidelines for OST services) (Walby, 2005). Here, we refer to the fact that the latter group is only able to see “trends at a national level” (as per one of my policy-making informants), which are used to affect reform in terms of how individual services work, and how their service users are treated. The data that extra-local informants receive are shaped by the texts being used, which are themselves “expressions of the organizational properties constitutive of the institution” (Walby, 2005, p. 161). Data are received in a manner that is framed by the interests of the institution, such as in terms of a service user's progress to “recovery” (through recovery plans), for example. Also, one staff member described having to document “people's smoking status,” as well as things like “unemployment,” employment,” and “housing status.” Service protocols may then be modified to better secure the interests of the institution if needed, and to better manage service users.
Given these surveillance practices, it is perhaps unsurprising that my informants would describe people using opioids as “chaotic” before attending the service, before then being corrected (and responsibilized) by OST. According to one staff member: There's … a lot of people when they come into treatment can be really chaotic… We talked about shared care and the needs of someone who's going to go out to shared care. They've got to be able to do it. They've got to be able to manage their scripts, et cetera. A lot of people can't… So … it's more about stability and … I think a lot of people that come in here are pretty chaotic and can't manage their lives so well… The whole thing with the doctors is just one aspect of it. It's probably all through their lives… Paying bills… Answering the phone, mowing the lawn… And … as you've mentioned, it's all through the guidelines, everywhere. There's references to helping clients manage themselves and sort of … be self-directing… Because that's one of the … of the symptoms of addiction. And especially … addiction to opioids is a sort of chaotic lifestyle… That's all part of the recovery journey… The service is very much focused on that and uses the language that constantly brings that up.
Individuals were described as coming to the service “chaotic,” and through the work of the staff, which follows on from “the guidelines and service documents,” service users could be responsibilized, in turn, “reach[ing] their potentials.” A service user's progress in this regard was “evident by their employment, by their ability to turn up, by how they’re dressed,” according to a policy-making informant, corroborating claims covered in the backgrounding section, that these services seek to create self-managing and productive subjects.
The Autonomy Paradox
However, we noted instances where the apparent intent of the institution was not being routinely realized. For example, staff conceded that recovery plans were not always used when meeting with service users. According to one, “the truth is that a lot of the case workers, especially the old timers, just haven't been using it [recovery planning] and they're more prone to just talk with their clients.” A service user also described the process of recovery planning as “a little unrealistic … and something over the top, and [that] it's just hard work trying to think up [resources for recovery] that you have.”
However, the scope of this paradox extends beyond expectations existing, but not being met. Critically, there were also contradictions in the seeming intent of the institution; while some processes and texts sought to responsibilize service users, autonomy restriction was also a feature of some work. When asked how much autonomy service users had over their treatment regime, a policy-making informant observed that: … autonomy is a really important aspect of a person's recovery, and services … the really clear message from the Director of Mental Health that he wants in the guidelines, is that services should use the least restrictive approach possible to maintain and preserve autonomy as much as possible. So, there's that tension between safety, but also maintaining, preserving autonomy, to the greatest extent possible.
Their description of having to balance autonomy against “safety” (presumably from the potential harms of using opioids) highlights the decisions that staff, and particularly the service doctors, must make regarding the freedoms they allow service users over their medication regimes, given staff's culpability for any potential risks incurred by these service users. Further, it seemed that service users were generally only afforded opportunities to be responsible for their treatment management when they were adjudged by staff to be ready and unlikely to be a risk to themselves or others. As one staff member said: … at one point there was this idea of people coming in and picking up their scripts on a monthly basis. The idea that they'd come in, they’d collect their script, and then they'd take their script to the pharmacy and there would be an active role, and being able to be part of their responsibility for their treatment, by clicking the script from the servers, giving it to the pharmacy, and then they get dosed… And, for some, that worked well. For others … their lives were so chaotic that they'd end up just going to the pharmacy and there'd be no dose there for them … they'd come in at a certain time, and so the script would be left in the file. And of course, they never turned up, and then we'd get the phone call from the pharmacy… But yeah, you know, I think that there is an important factor of people driving their, or feeling as if they are driving the treatment.
Critically, the staff member said that it is important for service users to at least be “feeling as if they are driving the treatment,” though not necessarily “driving” their treatment. Of course, though, the maintenance of this pretense was not supported by service users having to visit the in-house pharmacy during stabilization within strict hours, non-compliance with service expectations risking exclusion from treatment, and being required to submit urine tests at random. Even one's ability to choose to leave treatment was described as being limited in a sense; several informants commented that aspects of the treatment were like “liquid handcuffs,” whereby once one begins using methadone, it is “really hard to stop,” as “there's notoriously difficult withdrawals from methadone” (Frank et al., 2021). Discussing this idea, a staff informant said, that's one of the awful things about when people get angry with the service for whatever reason, and they say: right, I'm coming off [the OST programme]… it's easy to say that when you're not sick! But … when you're sick … it's tough.
Though SOPs and staff acknowledge that service users may choose to opt out of treatment at any time, the realities of using methadone can make this challenging, binding service users to treatment to an extent, further encouraging adherence to service rules, for fear of exclusion.
The (Sometimes) Responsibilised Self: Anticipating Dependence
Of course, my aim was to relate the treatment institution, with its work, texts, and seeming intent, to how opioid dependence is understood and enacted. We argue that in the findings, there is evidence of a performativity of dependence (as well as stability, recovery, being a “good” service user, and so on). Dependence was “real” for service users as they repeatedly performed it; how the service constructed them, and their use, became internalized, and informed how they interpreted their symptoms and situation. For Judith Butler, though her work is in reference to understanding gender, we anticipate an authority that prescribes a particular set of expectations, and our gender is performed based on our anticipation of these expectations (Butler, 2000). My informants’ constructions largely mapped onto (or were made through anticipation of) the dominant (responsibilizing, but also, medicalizing) modes of constructing these categories of being within the institution of OST. Certainly, this was the case when service users constructed their own opioid use and themselves through their accounts. However, service users would anticipate the expectations of the institution in varying ways based on their own interests and their position within the institution; dependence was constructed at the boundaries of various value-conflicts between actors within the institution.
To demonstrate this dynamic between institutional ruling relations and individuals’ conceptions of dependence, we will offer key examples of performativity, which largely fit under two categories. First, we will describe instances whereby service users, while anticipating the threat of exclusion from the service and the various (and sometimes contradicting) interests surrounding the nature and management of dependence, internalized these as they described themselves and their use of opioids. Second, we will describe the interviewed service users’ anticipations of each other, and the ensuing construction of other service users (but not themselves) as “scum,” “junkies,” and so on.
First, considering Butler's proposition that “anticipation conjures its object,” when asked how they thought exclusion from the service might work, two of my interviewed service users commented vaguely on the expectations of them as a service user, but believed that a misstep might lead to being dismissed from the care of the service (Butler, 2000, p. xv). According to one service user, when I asked whether the service's expectations were ever made clear to them, they said that “I think they [the staff] only told me about the… If you miss it [the methadone dose] three times, they'll cut it and you have to come in here [to the service, to be re-stabilised].” They also added that: …if you’ve got caught diverting it [that is, taking one's dose and selling it on illegally to someone else] from the pharmacy, then you … um … you can be taken off the programme … relatively quickly too… But… I don't really have to worry about that. But I do know some people that have been taken off it real quick. And after those three days, they've just … not had it at all after that…
A second service user commented to a similar effect, saying “you can tell there's kind of rules. It's like … you fuck up and we give you ‘x’ number of warnings or whatever. I mean, I've never been much of a bad boy.” Though neither were explicitly aware of what would count as circumventing service rules, both acknowledged they acted in a particular way that maintained their relationship with the service, based, to an extent, on the anticipation of what was acceptable behavior as a service user, and what was not (hence, making someone a “bad boy”). This anticipation then conjures its subject. Two service user informants described themselves, when in relation to the service and its expectations, as a “good boy,” “on the straight and narrow,” and so on. When I asked one service user how they spoke about their use with their case worker at the service, they said both parties called it “use” (rather than a dependence, for example), “because, ya know?… I think I'm pretty low-key. It's not, you know, I'm not coming in here with tales of selling my arse or whatever.” They were not dependent, they used, because they are “low-key.” Through narrow pharmacy opening hours, the threat of having takeaway doses changed to doses that must be consumed on the premises, and the expectation of turning up to the service as required for meetings and to collect doses, service users are responsibilized (and made to be self-responsibilizing) as “good boy[s],” through anticipating the consequences of not meeting these expectations.
From the perspective of staff though, some service users “know how to manipulate the system” and while they will “consider themselves good clients,” “there is evidence that could suggest they are using other things they’re not telling us about.” Importantly though, those who “consider themselves good clients” attended meetings, “always answer [their] phone” when staff called them to organize meetings, and then used this evidence of good behavior to ask for “more takeaways.” They, according to staff, navigate the expectations of the institution only to leverage their own interests. Where there was power, there was at times resistance; resistance here occurred through the reappropriation of institutional power differentials, as a sort of tactical reversal (Hartmann, 2003). Treatment expectations can be leveraged by service users to remake themselves in ways that benefit them.
Beyond this though, when I asked a service user whether they felt the treatment supported them to regain a sense of control over their substance use, they responded by saying that “it works for some people. That's the thing. You fucking be a junkie scum burglar, or prostitute, or whatever, and then you fucking change,” which, though they were being facetious, described a shaping of oneself based on an anticipation of the service's expectations. These expectations (and their pervasiveness) were best summarized by a staff member, who commented: … it's all through the [national treatment] guidelines, everywhere. There's references to helping clients manage themselves and … be self-directing. And all sort of language like that, it's all through the guidelines and service documents. Because that's one of the … symptoms of addiction. Addiction to opioids is a sort of chaotic lifestyle… An inability to manage some simple things that … other people just take for granted and do easily… So yeah, that's all part of the recovery journey, I think… The service is very much focused on that and uses the language that constantly brings that up.
Also, more abstract “authoritative disclosure[s] of meaning” than the service rules permeate the service and are anticipated by service users in different ways, such as the various constructions of opioid dependence, each a product of varying socio-political and personal interests (Butler, 2000, p. xv). Yes, service users may act according to what they anticipate is expected of them at the service, but also, how they talk about their opioid dependence and themselves appears to follow on more directly from their anticipation of dominant modes of constructing opioid dependence, as these are notable throughout the service's work and texts. Chiefly, service users described their opioid dependence as ingrained and inherited—typical features of a medicalized construction. One service user said, “I'm just an inveterate drug taker, I think. You know? Why the fuck can't I do that [take opioids]?”
Another informant consciously acknowledged their use as innate—this time as a “predilection,” the implications being that it is real, biological, and unavoidable. This should be unsurprising given OST constructs their use in the same way. For example, the first line of the New Zealand national OST practice guidelines begins: “Opioid dependence is a complex, relapsing condition requiring a model of treatment and care much like any other chronic health problem” (Ministry of Health, 2014). Dependence is here described as “relapsing” and “chronic,” and this construction was echoed in the talk of staff (and therefore, service users). According to one of my staff informants: … if they [service users] didn't have a dependency on opiates, obviously they wouldn't be steered towards our service… And if someone's depending on opiates, and it's a controlled medication, there's all those parameters that go with that treatment which they've got to be aware of too… There's a number of times that they'll be … going to the pharmacy and needing to come in for medical reviews… There is quite … a level of constraints that are put in place.
Here, they acknowledge service users anticipating (medicalizing) service expectations; because dependence is medicalized, service users must turn up for “treatment,” “come in for medical reviews,” and for treatment to be successful, they must be aware of these treatment “parameters.” Another staff informant, perhaps inadvertently, also acknowledged this anticipation by service users. They said: And it's one of the problems in OST. It becomes really heavily medicalized, you know? And it just becomes about the medication and that that's not the fault of the service… I mean, it's often that's the fault of the client. That's how the clients think about it… You know? It's about the medication, nothing else. “I don't wanna sit and talk to you … [and] talk about my problems or my relationships or anything else, and my aims and my goals”. But the truth is that … for someone to progress towards a proper recovery from addiction … they need to talk about those things.
Despite this, however, we wish to clarify that my intent is not to show that “dependence” is a product of medicalization. This has already been argued extensively (Kaye, 2012). Rather, we have shown that how my service user informants saw their consumption of opioids—the manner by which they constructed it and themselves—was made in relation to how they anticipated it being seen externally (by the institution of OST in this case). This connects the texts and work of the institution to how dependence was actually being conceived and enacted by participants. Because of this, how opioid dependence is constructed by service users can be appropriated by any number of socio-political interests, whether they be the intent of medicalization, or the intent of responsibilization (or a neoliberal interest more generally), for example.
Acknowledging performativity allows the analysis to extend beyond vindicating what has effectively already been argued in extant literature (namely, that the service is constructed to responsibilize its service users, as is described in the above excerpt). There is not just power, enacted by the “monolithic” institution, and service users’ uniform resistance to it. Instead, service users anticipate the expectations of the institution in varying ways (thus acting on, and understanding themselves, differently, given these) based on their own interests and their unique position within the institution. As above, service users thus constructed themselves and their own dependence to a variety of ends.
However, perhaps more interestingly, we also noted several examples of service users’ anticipations of one another within the service, which previous Foucauldian literature has not acknowledged. We argue that the way they talked about each other (compared to how they talked about themselves) betrayed a particular manner of thinking about people using opioids. Despite service users identifying themselves as a “good boy” or “easy” for staff, they commonly would describe others (despite having not necessarily encountered them) as “junkies” and “scum.” Previously, we described how particular dominant modes of thinking about opioid use came to constitute how service users understood themselves. Here, we argue there was evidence of other ways of constructing opioid use (and those using opioids) in the ways my interviewed service users understood each other, or at least, some abstract archetype of “the other.” According to one service user, they themselves “didn’t really need recovering” despite that being “the standard thing;” however, when describing other service users, they said, for example: It's just … a lot of bad fuckheads are attracted to this thing [OST programmes]. A lot of just… The criminal mentality; the person who blames everything on other people. You know? Just a criminal mentality. I guess it's … you just can't put up with it.
Describing other service users as those who blame everything on others, but themselves have a “criminal mentality,” this informant later added that the service had to maintain a “hard line” when enforcing its regulations, to contain this apparently challenging group. They concluded by saying: And that's just … that's not a method of social control. It's just like … you're here to get your shit together. That's how society and life works. If you say you're going to do something, you have to do it.…
This contempt for their fellow service user came up several times amongst my interviewees. Critically, though my service user informants regularly described their own use of opioids as a hereditary and medical issue, they were more skeptical regarding others. Describing fellow service users, one informant said: … at the end of the day these people have a “sickness” [while gesturing to insinuate that this is in inverted commas] and … so you’ve got to take a lot of shit from them. They can blame the disease or whatever to the “nth” degree … they've had terrible upbringings … yadda yadda… People can bring out a lot of cards…
In my encounters with each informant though, none of them appeared (at least in their own descriptions of themselves) to represent this described archetype of a “junkie,” or someone who has a “criminal mentality.” This was noted in the talk of one service user, who claimed that “junkies” circumvented service rules and failed to meet service expectations. As they said, regarding the initial stabilization period at the service: Yeah… You do a piss test, and you just get on like a certain, you know? They basically ask you … they give you a certain amount [of a prescribed opioid] and it's like … does this hold you? And all junkies are going to go, no, no, no, give me more, give me more, give me more.
They claimed that attempting to manipulate staff into prescribing a larger dose than is necessary is typical of “junkies,” though saying that they themselves are “not scummy enough” to attempt the same. This construction of “the abject other” service user was an odd, complicated abstraction, but was always, according to the accounts of my interviewed service users, made in relation to service expectations (Bergschmidt, 2004).
Conclusion
Given this, though there were dominant modes of constructing dependence (as a chaotic inability to self-manage, or as a medical issue) that pervaded the service, these manifested in paradoxical ways and were subject to resistance and opportunistic utilization by service users. Rather than drawing binaries—between the dominant service and the subjugated service user, or the chaotic dependent individual and the autonomous neoliberal subject—we have shown dependence to be neither an objective medical diagnosis, nor something which is installed without resistance into the bodies of service users to some ulterior end. Extending Lancaster et al.'s (2023) proposition, that dependence ought to be considered as a situated and relational becoming, we have instead shown dependence as being performative, but critically, made in relation to the materiality of the work and texts of OST; “real” insofar as it affects people's lives, but not as some objectively knowable internal essence. The dynamic, material relations that might afford “opioid dependency” its stigmatizing capacity have been rendered visible (Lancaster et al., 2023). In contrast to claims made elsewhere in the literature, stigmatizing language was not merely imposed from “the outside” or “above,” but was also reproduced and negotiated within the institutional context of treatment itself, structured by its rules, routines, and expectations (Link & Phelan, 2013; Treloar et al., 2022). Crucially, though, this could also be leveraged as a resource: one which service users could use to establish their own legitimacy in relation to an imagined deviant other.
Implications for Policy and Practice
Reflecting more broadly on the provision of OST, however, the sum of the involved work processes appears to follow a complicated, responsibilizing cycle. First, dependence is pathologized through the service's work, and service users are made responsible for managing their condition. This inadvertently justifies avoiding structural issues plaguing substance users’ lives, but certainly, further reaffirms dependence as an issue that should be addressed through medical intervention. Then, pathologizing problematic opioid use is vindicated (and thus repeated), as service users are adjudged to be “recovering” in line with the principles and expectations that already pervade the service.
Services are only “needed” as they maintain the “problem” which they aim to solve; people using opioids are created as “chaotic” and therefore in need of treatment to become self-managing. Regardless of whether this is routinely realized, OST, through its responsibilizing intent, appears to represent an attempted diversion from the need to address the myriad issues (relating to housing, relationship issues, and trouble with the law, for example) that those using opioids may face. Through OST, service users are positioned as “chaotic” before treatment (not disenfranchised), to employable, employed, and self-managing. This, in turn, de-responsibilizes the state from protecting and supporting a group that has become further marginalized through medicalization.
Some might argue that the work processes described are pragmatic; for example, the strict regulations around takeaway doses or who can go where within the service safeguard the safety of staff and service users. We do not deny this pragmatism. We appreciate the concern for the safety of all of those involved with methadone provision. Equally, we do not deny that OST services may reduce the spread of communicable diseases and substance-related deaths for those who attend them.
However, despite the alleged success of OST in reducing crime and the spread of disease, attention must be drawn to the propensity for these services to render opioid users as self-responsible subjects (Sheerin et al., 2004). It is not surprising that OST services are successful in managing these concerns; they pervade every aspect of how the institution is constructed. What must be acknowledged is the intent behind these arrangements. This is essential in advocating for the support of people who use drugs in ways that do not further pathologize, marginalize, or hold them individually responsible for managing the structural conditions that organize their lives.
To make recommendations for changes, even to broad drug policy, would thus be redundant; as it pertains to the provision of OST, drug policy can be seen as, at best, a compensatory measure for broader social and political mismanagement. If the broader management and understanding of substance use remained the same, but treatment for opioid use was stopped, it is to be expected that there would be more opioid-related deaths. However, these might be avoided in equal measure by a broader system of welfare and support that does not create subjugated classes. OST treatment might only be stopped when accompanied by a fundamental rewiring of the way illicit substances and those who use them are thought about and managed (if they are managed at all), more generally, an effort which this article has attempted to contribute to.
To begin to understand the depth to which medical discourses (and those which responsibilize those using opioids) have permeated how people think about opioid use, it would be useful to incorporate the accounts of those who use opioids, but do not attend OST. It would also be useful to consider those who are in the process of being admitted to the service. Both would provide comparison groups; seeing how their accounts of their use and themselves differ (if they do) from the accounts provided to me by my service users' informants would go some way in showing how OST services shape the way dependence is constructed. We have shown how opioid use is constructed within the institution, but how has the medicalization (and responsibilization) that these services propagate affected the construction of opioid use before people have even come into contact with these sorts of services?
An assessment of the broader public discourse could be hugely valuable; it could be inquired how dependence is constructed through films and other media, and how people engage with these media and discuss dependence through online discussions (for example), amongst other spaces. These inquiries could be approached by extending what has been begun here, with regard to understanding the performativity of addiction. We have argued for the usefulness of applying Judith Butler's work to this space, but exploring this with more informants, and with informants not necessarily involved with treatment services, will be essential in describing how those using opioids are now managed (and manage themselves) broadly.
Footnotes
Acknowledgments
We wish to acknowledge the service users and staff who provided their knowledge and support for this research project.
Ethical Approval
The research project referred to in this article was approved by the Health and Disability Ethics Committee (approval no. 2023 PR 12194). All participants provided written informed consent prior to enrollment in the study.
Consent to Participate
All participants provided written informed consent prior to enrollment in the study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
