Abstract
This paper presents findings from a cross-national study comparing frontline workers’ actual and potential responses to injecting drug use among minors (under 18) in Sweden, Switzerland, and Wales. We investigate if and how distinct drug policy contexts and child protection systems appear in front-line workers’ talk, and whether divergent policy settings might be associated with differential institutional responses. Attention is given to the different discourses which practitioners draw upon when depicting needs and suggesting appropriate measures. The data comprise six focus groups (two in each country) and vignettes serve as a basis for the discussion. Our analysis shows country differences and similarities; however, not always in line with policy expectations. Three country-specific patterns are identified: compulsory measures as default mode (Sweden), harm reduction as default mode (Switzerland), and drug use as secondary concern (Wales). A similarity across countries was a strong tendency to propose interventions that corresponded to already existing ones, originally developed for adults, whether these focused on abstinence or harm reduction. Our findings contribute to a limited empirically based knowledge regarding assessment processes and available services for children injecting drugs in Europe. It offers a starting point for reflection on how prevailing policy contexts influence everyday social welfare practices in the field of drug use.
Introduction
There are very few reliable country estimates on how many people under 18 inject drugs in Europe. Existing research indicates that they constitute a small, dynamic, and hidden population experiencing serious social, physical, and mental health issues (Barrett & Turner, 2024; Busza et al., 2013). While there has been a longstanding ethnographic engagement with injecting drug use among adults (e.g., Bourgois & Schonberg, 2009; Faupel, 1991), qualitative studies investigating the lives and perspectives of young people who inject drugs are rare (but see Krug et al., 2015). Research indicates that there are worse health and social outcomes for those with injecting debut prior to 18 when compared with those with debut while adults (Turner et al., 2023). In recent years, social work with adults using drugs has developed from a historically abstinence-oriented rehabilitation project to a more harm reduction-oriented practice (Lushin & Anastas, 2011; Richert et al., 2023; Vakharia & Little, 2017), but a similar trajectory has not been explored with minors.
In this article, we use the terms “legal minor” and “child” synonymously to bring to the forefront legal, ethical, and social issues that can be obscured when terms such as “youth” or “adolescent” are employed, with age ranges extending into the mid-20s. Unlike adults who inject drugs, legal minors are subject to child protection and child rights legislation and related institutions and systems. The UN Convention on the Rights of the Child (UNCRC), for example, applies to everyone under the age of 18, requiring reflection on how child rights standards apply to a behavior that is rarely associated with childhood, and to interventions that have been developed with much older participants in mind. Unlike with adults who inject, child protection standards must be factored into assessments and responses. Despite practical, ethical, and legal challenges involved in service provision for legal minors who inject drugs few studies focus on the legal and policy environment for harm reduction work with this age group (but see Watson et al., 2015).
In the present study, focus group interviews are used to analyze how frontline welfare practitioners in three high-income countries—Sweden, Switzerland, and Wales—discuss the needs of and make assessments regarding available and desirable interventions for people under 18 who inject drugs and who are still children from a legal and policy perspective. Attention is given to the different discourses which practitioners draw upon when depicting needs and suggesting suitable responses. We investigate if and how distinct drug policy contexts and child protection systems appear in front-line workers’ talk, and whether divergent policy settings might be associated with differential institutional responses. The goal is to contribute to a limited empirically based knowledge regarding assessment processes and available services for minors injecting drugs in contemporary European welfare practices.
Social Policy Contexts and Practices—An Overview
It is not known how many people under 18 currently inject drugs in each of the three countries. However, approximately 29% of people who inject drugs in Sweden and 23% in Switzerland report injection debut prior to the age of 18 (Barrett & Turner, 2024). The current figures are less clear in Wales due to age of injecting debut being removed as a variable in the relevant register. The best current estimate is only 5%‒9%, but when age of debut was collected previously it was estimated at 24% (Barrett & Turner, 2024). All three are high-income countries with relatively high levels of welfare provision. Child rights have a firm basis in national law across all three (e.g., Law 2018:1197 [Sweden]; Law on Childhood and Youth 2018 [Switzerland]; Rights of Children and Young Persons [Wales] Measure 2011), where a “minor” is anyone under the age of 18, conforming to the definition of a “child” under the UNCRC (Social Services Act 2001:453, 1 kap 2§ [Sweden]; Law on Childhood and Youth 2018, Art. 4 [Switzerland]; Social Services and Well-being (Wales) Act 2014, s. 3). However, the countries present different ways of organizing child welfare and child protection, and the structure of national drug policy and drug treatment services vary.
Sweden
In cross-national research on child welfare, countries are often categorized based on the distinction between a child-protection-oriented system, a family-service-oriented system and, more recently, a child-focused orientation (Schnurr, 2016). Regarding these distinctions, Swedish child protection has been labelled as family service-oriented, meaning that services and interventions aim to promote consensual measures and strengthen the care and capacities of the parents (Leviner, 2014). However, this overall characterization does not obviously translate to safeguarding in the context of injecting drug use, where Sweden's long-standing history of zero-tolerance drug policy and use of compulsory treatment measures must be considered. Regarding minors, according to the Swedish Social Services Act, authorities and staff working with children have a duty to report to social services if they have knowledge or suspect a child is being harmed or is at risk of being harmed (Social Services Act 2001:453, 14 kap 1§). Identification of injecting drug use would certainly trigger the duty to report (Prop 2016/17:15, p. 32). There is dedicated legislation on compulsory care for young people (Law 1990:52, abbreviated as “LVU”). Compulsory care can be applied if there is a risk of damage to health or other harm from drug use, criminality or other “social norm breaking” behaviors (Law 1990:52, 3§), and it can involve placement in a residential home run by the Swedish National Board of Institutional Care (SiS in Swedish). Before placement in such care, both the region and municipality should agree that the child's needs cannot be met in other ways. Approximately two-thirds of those in such institutional care are placed due to their drug use (SiS, 2022). Voluntary drug treatment for minors is primarily carried out via so-called “Maria” clinics run as part of regional health authority duties in collaboration with municipalities. However, register data show that very few minors who inject drugs appear in these clinics (Barrett & Turner, 2024). In terms of drug policy, Sweden remains strongly prohibitionist, with the policy goal of a drug-free society and the criminalization of possession and use of drugs. Nonetheless, harm reduction services have expanded in the form of opioid substitution therapy (OST), needle and syringe programs (NSP) and more recently naloxone distribution (SOU 2023:62, pp. 321–340). NSP are formally delivered through regional health clinics (Law 2006:323, 2§). Harm reduction is not envisaged as an approach for minors, however, and there is no national guidance on harm reduction for this age group. By law, under 18s are not permitted to access NSP (Law 2006:323, 6§). Needle purchase via pharmacies for anything but recognized medical conditions is not permitted for any age group (Law 2012:595, 4§).
Switzerland
Child protection in Switzerland has been described as a patchwork of 26 cantonal regimes (Schoch & Aeby, 2022). The country has been categorized as both child protection oriented, a risk-averse approach focusing on the rights of the individual child to protection from abuse or neglect, and family service-oriented, with child-focused elements introduced a decade ago (Müller et al., 2020; Schnurr, 2016). Since 2013, statutory child protection is the responsibility of Child and Adult Protection Authorities (CAPAs), which are multi-professional, court-like bodies responsible for processing information received about children at risk. Since 2019, all professionals with regular contact with children as well as “persons who learn of such cases in their official capacity” are “obliged to report [to a CAPA] if there are clear indications that the physical, psychological or sexual integrity of a child is at risk and that they cannot remedy the threat as part of their professional activities” (Schnurr & Gautschi, 2023, p. 268; Swiss Civil Code, 1907, Art 314c). Compulsory placements of minors at so-called secure institutions or psychiatric hospitals are possible, but this measure is not covered in statistics on decisions made by CAPAs. Nonstatutory services for children and families are the responsibility of cantonal social services agencies, and its provision and availability vary significantly across cantons (Schnurr & Gautschi, 2023).
Swiss drug policy has a long-standing harm reduction and public health orientation (Csete, 2010). Compulsory treatment for people who use drugs is possible but not a common practice, either for adults or minors. Provision of drug treatment varies between cantons and is delivered through a mix of public and private organizations. According to the Federal Office of Public Health, there is a service gap in that management of minors with problematic substance use often takes place in institutions that are not specialized in drug use disorders, such as care homes for children (foyer) or psychiatric services for children or adolescents (FOPH, 2019, p. 17). NSP is integrated into drug consumption rooms (DCR), mobile outreach services, and some hospital settings, but coverage varies across cantons. Pharmacy sales and automated vending machines are also available. Under 18s may not inject on site at DCRs but may obtain sterile injecting equipment from them. However, there are no national protocols for needle exchange for under 18s leading to variation between cantons and uncertainty as to applicable rules for minors (Csák, 2022).
Wales
Wales is governed by its own National Assembly, with various powers devolved from Westminster, including healthcare and social services. It has a child protection-oriented system. Needs assessments may be carried out by social services to determine if individuals need care and support, and if so to decide on which actions might be appropriate (Social Services and Well-being (Wales) Act 2014, pp. 21–23). There is a statutory duty for those providing care and support to report children at risk of harm (Social Services and Well-being (Wales) Act 2014, pp. 130 and 162). In relation to drug use interventions, children are categorized into four tiers based on behavior and substance use and risk, ranging from universal interventions for all children to inpatient care for those at greatest risk (Welsh Government, 2011a). It is likely that a minor who is injecting would be categorized into a high tier of risk (Welsh Government, 2011a, p. 37), triggering the duty to report, but as with Switzerland drug use alone would be unlikely to trigger compulsory care, which would be addressed under mental health legislation.
Welsh drug policy is strongly harm reductionist in orientation (South Wales Police, 2022; Welsh Government, 2019) including explicitly in relation to youth substance use (Welsh Government, 2024). Support for young people who use drugs is carried out through a mix of voluntary and statutory services, with specialized drug treatment being primarily run through Child and Adolescent Mental Health Services (CAMHS). NSP is provided through a mix of low threshold access points, including specialist statutory and voluntary NSP fixed sites, mobile outreach, and pharmacies, all of which are accessible to under 18s, albeit with certain additional rules that do not apply to adults, including the duty to report to social services, meaning the typical confidentiality of the service is not guaranteed for this age group. Wales is the only one of the three countries with national guidance on NSP for under 18s, with access for those under 16 being based on established judicial guidelines for determining consent (the “Fraser Guidelines”). The assessment for NSP for under-16s uses a standardized form that includes discussion of the child's drug use, injecting behavior, awareness of injecting-related health family context/family context (Welsh Government, 2011b, pp. 14–19).
Theoretical Framework
In this article, we depart from a social constructionist tradition and study the frontline practitioners’ discussions as “social problems work” (Holstein & Miller 1993), which highlights “the person-building activity entailed in the everyday construction of social problems” (Gubrium & Holstein, 2001, p. 11) such as drug use and mental illness. Constructionist-oriented research reminds us that language use is a basic element of social work practices, not only reflecting reality but actively constructing it (e.g., Hall et al., 2003; Jokinen et al., 1999). As Gubrium and Holstein (2001) point out, the societal contextualization—or discursive environments—of particular concerns set conditions for possible constructions of troubled selves. Previous studies on professional talk in drug service settings have provided important insights into how social and cultural contexts influence the perception and problematization of substance use (e.g., Heimdahl, 2018; Järvinen & Andersen, 2009; Selseng, 2017). For instance, Ekendahl et al. (2018) found that professionals in a Swedish outpatient drug treatment center for young people made use of logics that reinforced the prohibitionist view of cannabis as a serious and pressing issue and represented young cannabis users as in need of both protection and control. This resonates with a body of work within the field of childhood sociology and sociology of youth, where scholars highlight that casting children both as in danger and dangerous has a long history in politics and mass-media (e.g., Moran-Ellis, 2010; Wyn & White, 1997). Several studies have noted the importance attached to age when professionals assess to whom priority should be given in drug treatment (e.g., Wallander & Blomqvist, 2009) and Selseng (2015) argues that age constitutes a central component of contemporary discourses on drug use. Based on interviews with Norwegian substance use counsellors, Selseng shows how “young” (vulnerable and formative) and “adult” (agentic) constitute core categories for differentiating when counsellors assessed needs and made priorities among clients, underpinning a hegemonic “focus on the young ones” discourse. Following this tradition, we will study language used to describe children injecting drugs (for example as victims or untrustworthy) as expressions of locally available discourses that entail a moral positioning of the children (e.g., as pitiable or blameworthy).
The Comparative Methodology of the Study
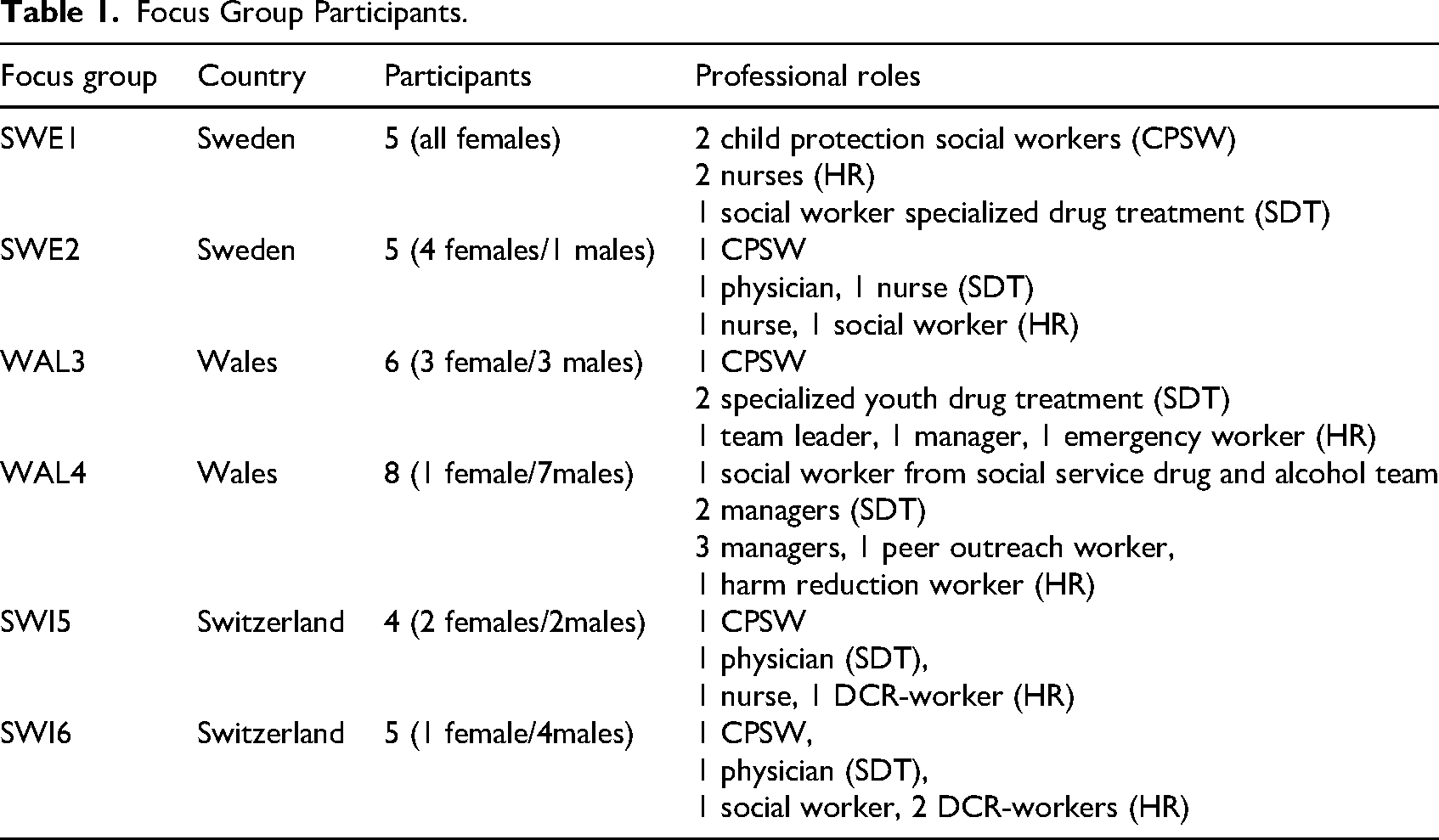
The data presented in this article consist of six focus groups with frontline practitioners in Sweden, Switzerland and Wales and is derived from a larger cross-national, multi methods research project. The focus groups (two in each country) were conducted online during 2022–2023. Participants were selected using purposive sampling procedures so that insights could be generated across several key areas (Quilgars et al., 2009). To enable comparative analysis each focus group was composed of frontline practitioners from three distinct welfare areas –child protection services, specialized drug treatment units for young people or that can accept young people, and harm reduction services (such as NSPs, DCRs, and Maria clinics). A key reason for our focus on frontline workers (as opposed to managers or policymakers) was that these are the hands-on people who directly interact with young people who use drugs, offering an opportunity to explore everyday welfare practices. On average, each focus group lasted 90 min. The focus group moderators varied across countries so that of the five researchers involved in the project, three acted as moderators on two occasions each. At each session, one of us filled a co-moderating role (acting as a recording technician, keeping track of time, etc.). Informed consent was obtained verbally from all participants prior to their participation, and these consents were audio-recorded (Table 1). 1
Focus Group Participants.
The research team was compiled of “national insiders” (Wendt, 2020, p. 245), a position here corresponding to linguistic skills, knowledge of the prevailing political and social conditions, and established connections with local social work and harm reduction communities. As highlighted by Fitzpatrick and Stephens (2014), to establish and interpret comparable results in cross-national studies the methodology, definitions, and selection of each national case need to be aligned. Also, differences in policies designed to deal with the problem at hand must be considered. The first set of questions was addressed by the development of a focus group guide that would be comprehensible across countries. We paid specific attention to language use to minimize possible translation bias, and to the moderator's role to decrease the risk of moderator bias. Given the cross-national design, comprising three countries with three different languages, an awareness of language issues and their possible impact became an essential part of the project (Frost et al., 2017). Challenges related to policy differences were addressed by incorporating a vignette methodology (Fitzpatrick & Stephens, 2014; Khoo et al., 2003). Vignettes may be described as “short stories about hypothetical characters in specific circumstances, to whose situation the interviewee is invited to respond” (Alexander & Becker, 1978, p. 94). By using vignettes, we aimed to “open up broader conversations about not only what would happen in particular circumstances, but also what should happen, highlighting the range of moral and normative ‘repertoires’ drawn upon by relevant stakeholders” (Fitzpatrick & Stephens, 2014, p. 220). To ensure validity, we strove to depict a set of scenarios that would be recognizable across the participating countries. All vignettes were based on data from our larger research project in the form of individual interviews conducted with young people who began injecting before turning 18, but built on several cases and with details amended to minimize the risk of identification (cf. Engwall et al., 2019). The vignettes, presented in Figure 1, represent three scenarios of severity and to capture various circumstances (family network, school attendance) to explore the range of responses in different settings. Each vignette has been labelled and given a fictional name to facilitate the reading.

The Vignettes.
Analysis
Initially, an open coding was conducted individually and for each country by all three authors. Transcripts were read closely, row by row, and concepts, descriptions, and events that recurred or stood out were noted. Focus during this phase was on what was said, and country-specific summaries were developed by each researcher. After this first reading, these summaries were discussed, identifying cross-country differences, but also striking similarities across contexts, notably with regard to how the vignettes were interpreted and the assessment of suitable interventions. The first and the second authors then reread the transcripts individually with a specific focus on the vignettes. We noticed that the material was imbued with varied moral reasonings and specific understandings of the depicted cases, offering an opportunity to explore discursive features in the data. Following Gubrium and Holstein (1997), we made an analytical distinction between “the whats” (content) and “the hows” (process) of the interviews. This meant analysis shifted from descriptions of events to how participants talked and how policy contexts were present and made sense of in the discussions (Hall et al., 2014). Moving back and forward between analytical closeness (detailed reading of each focus group) and analytical distance (zooming out for comparisons within and between countries), we compared and discussed our individual interpretations. Inspired by discourse psychology (Edley, 2001; Harré & van Langenhove, 1999), we explored categorisations and subject positions occuring in the material and focused on “collective voices,” rather than individual views, to analyse the discursive terrain of the focus groups (Smithson, 2000, p. 109). Analysis revealed four key discursive themes: medicine/addiction, psychology/trauma, youth at risk, and harm reduction. These four discourses are in line with larger-scale discourses identified in previous research. In the identified medical discourse, injecting drug use is manifested as a dangerous and incurable disorder that hijacks young people's brains, making them incapable of rational decision-making. This resonates with for example Rhodes’s (2002) influential work, that has highlighted the dominance of an addiction discourse within the public health domain. This discourse is based on the perception of drug use as a disease of the will, positioning drug users as “slave[s] to their addictions,” helplessly chasing the next hit (Rhodes, 2002, p. 86). The psychological discourse rests on assumptions that legal minors’ injecting arises from internally located causes, such as trauma, Post-Traumatic Stress Disorder , and emotional problems. This resonates with the psychological discourse in drug treatment identified by Kuusisto et al. (2023) which is characterized by “the prominent position of the individual's feelings and internal motivations when rendering behavioral addiction comprehensible” (Kuusisto et al., 2023, p. 221). A third prominent discourse in our data is the “youth at risk” where children injecting drugs are addressed as vulnerable minors in need of protection, either from themselves or from their environment. Within youth studies, several researchers has shown youth at-risk discourses to function as powerful truths that tend to individualise the troubles young people face while leaving structural barriers unaddressed. Kelly (2001, p. 30) argues that “[t]he discourse of youth at-risk mobilises a form of probabilistic thinking, about certain preferred or ideal adult futures” and through the present behavior of certain youths (in our case, injecting drugs) these preferred futures are jeopardized. Finally, the identified harm reduction discourse is characterized by addressing minor injectors as health-conscious actors capable of making rational decisions and taking responsibility of themselves and their lives. This resonates with what many scholars have articulated regarding contemporary harm reduction discourse, namely that the neoliberal drug-using subject constituted through the discourse is that of rational and autonomous health service consumer (e.g., Moore & Fraser, 2006). The harm reduction discourse manifests as destigmatizing and abstinence-oriented goals are not integrated part of the work at harm reduction services. However, scholars such as Andersen and Järvinen (2007) have described negative consequences of this understanding for clients not able or willing to live up to expectations of autonomy and risk management (e.g., lead to greater stigma, since failure to act in accordance with the harm reduction help and information offered may be seen as blameworthy). We return to these four discourses later in the text.
The identified country-specific themes have guided how we organized the below results section. For this article, excerpts from the Swedish and French language focus groups have been translated to English by the research team. In the excerpts, participants are identified as either social worker (SW), harm reduction practitioner (HR), or specialized drug treatment practitioner (SDT), followed by focus group identifier (SWE1, SWE2, WAL3, WAL4, SWI5, and SWI6). Transcription symbols: (…): Omitted part of text [indicate author addition]
Sweden: Compulsory Measures as Default Mode
Michael: Drifting at the Margins After Care Exit (Vignette 1)
There was a broad consensus among Swedish practitioners that this was a very serious case. A report to child protection services was presented as inevitable, as was the scenario that the report most likely would result in compulsory care. A shared opinion was that the boy “must be controlled immediately, and that is surely through a new placement, to break his addiction” (SDT, SWE2). The practitioners focused their discussion on the boy's drug use, which was construed as a serious addiction and the boy was positioned in line with a medical discourse, “as incapable of ‘rational’ or ‘reasoned’ decisions” (Rhodes, 2002, p. 86). Following on from this, the practitioners were positioned as agents with responsibility and a duty to act to protect the boy from himself. At the same time, the interviewees unanimously expressed concerns regarding the negative outcomes from compulsory care, and the detrimental environment at the special residential homes where this type of care is most often carried out. These institutions were described as “schools for future injecting careers” (SDT, SWE1), with insufficient specialist knowledge regarding young people who use drugs. “Usually nobody comes out better, it's not as if they get the level of treatment that is needed, rather it's storage” (SW, SWE2). Despite these concerns, what would happen in this specific case was also what the practitioners in general described should happen. “I think that is probably what should happen, that he should go back to SiS for another try” (HR, SWE1). The main motive described for a SiS placement of this boy was the depicted lack of other options available, and that the situation was assessed as urgent (cf. Ghazinour et al., 2021 on compulsory care placements of refugee minors). In this way the Swedish participants reflect a “last-resort” logic that has been seen to legitimate the use of extreme measures within a variety of social control settings (Emerson, 1981). The practitioners’ way of reasoning might also reflect the historically firm position of compulsory care in Swedish child protection as well as the drug treatment system (Palm & Stenius, 2002).
Sara: Living at Home and Planning to Inject (Vignette 2)
In relation to this girl, the tenor of responses in Sweden was alarm: “It goes without saying, as soon as this patient would come to us it would be a report to social services if she's under 18” (SDT, SWE2). Like the first vignette compulsory treatment was mentioned as a possibility. “It's very worrying, of course. It's surely time to take forceful action, to offer a lot of interventions, and it could be a question of compulsory placement based on that information” (SW, SWE2). In addition, interviewees agreed that a child protection investigation should be conducted. She would not be able to access NSP due to her age. Even though this girl is described as living with her parents, the issue of family did not come through very strongly in the practitioners’ discussion. When parents were mentioned, it was in relation to gaining information of relevance for a child protection investigation. “[W]e would find it necessary to contact the parents to talk about our concerns, and to get a picture of her needs. I don’t think we would specifically talk about injecting” (SW, SWE1). The primary goal for the suggested interventions in this case was to stop the girl from injecting. As one participant put it: “One has to investigate the situation and her needs more in-depth, but certainly not give information about safe injecting practices but rather try to motivate her to not try it” (SW, SWE1). This understanding was expressed also by NSP practitioners, but this was tempered by the harm reduction orientation of their work: “Then again, we would want to provide her with information to reduce risks, she's not going to stop injecting because we call social services” (HR, SWE2).
While harm reduction has gained acceptance in Sweden in recent years, the practitioners’ way of reasoning follows logically from a child protection perspective of drug use in which children are seen as having a right to a drug-free upbringing. Harm reduction in this context may not be seen as an appropriate pathway, even if accepted for those who are older. In the following excerpt, one interviewee justifies why the girl should not be admitted to a specialist ward: [B]ecause in our ward a young person like this would get loads of information and perhaps be tempted. There's substance abuse and self-harm, there's crime, and a troubled youth could probably learn a lot and go down all sorts of wrong paths. A youth who doesn’t attend school, feels bad, there's already a big concern, and then that she also has a desire to begin injecting, it feels very sick. (SDT, SWE2)
Unlike the boy in our first vignette, where a likely harmful institutional placement was deemed necessary to protect him from his drug use, this girl was constructed as in need of protection from destructive elements and detrimental aspects of the environment at specialized facilities for young people who use drugs. Focusing on discursive elements, the above excerpt highlights two prominent discourses in the Swedish data—youth at-risk and a psychological discourse. From this follows that practitioners’ responsibility becomes guiding the girl towards making the right choice and become a self-governing subject. In the psychological discourse, curiosity about injecting is interpreted as “sick” and focus is turned to the individual's internal world. Another interviewee said that “[i]t feels very unusual for a seventeen-year-old to ask those questions to health care practitioners in that way, so I think this case also involves a lot of mental illness and disability” (SW, SWE2), and another stated that “[a]ccording to my experience, when someone visits us and has never injected before, they have a psychiatric diagnosis” (HR, SWE2). The positioning of the girl produced by these two discourses—youth at risk and psychology—is that of weak and fragile, but not yet lost, in need of guidance and protection. When asked what they thought ought to happen in this case, Swedish interviewees in general shared the opinion that “[o]f course we cannot succeed with everyone, but we succeed with the vast majority. What should happen is roughly what would happen” (SDT, SWE2).
Ali: Injecting Before Class (Vignette 3)
Again, Swedish practitioners were highly concerned by the injection drug use, and all agreed that a report to social services would be a first response. We report to child protection services, it involves injecting. (…) This youth would be admitted to our ward, and we would try to get social services here as fast as possible and together with the family begin to investigate the situation further. Unlike the first vignette, this is a youth who is part of a family. Why has the family not noticed anything? (SDT, SWE2)
This vignette represents a more socially established position compared with the previous two. Some practitioners suggested compulsory care as a suitable intervention, but in this case coercive measures had to be balanced with the fact that the boy lived at home with his family and attended high school. Unlike the discussion on the previous two vignettes, this boy was positioned as part of a family and there was a stronger emphasis on parental responsibilities. But as one interviewee stated: “Nevertheless, I believe that compulsory placement would outweigh because injection drug use is regarded as very serious” (SW, SWE2). Following previous vignettes, the interviewees’ discussions and suggested interventions illustrate the importance attached to method of drug use in a Swedish context. When given the opportunity to reflect on what should happen in this specific case, the general suggestion made was further investigation into the boy's situation before putting in place more specific measures. Age and motivation were made relevant by some, if the boy's motivation was oriented towards abstinence, as illustrated in the following quote: One would consider this very seriously, perhaps it must be a placement, depending on the young person's attitude. But if he wants help it is better to try the voluntary route first, when it's a seventeen-year-old that wants this. (SW, SWE1)
While some practitioners raised additional questions regarding type of drug(s) injected and frequency, SiS-placement was not questioned as an adequate option for this boy, even if some hesitation was expressed in statements like “to end up at a special residential home might not be very positive, but that's just my thoughts” (SW, SWE2). In the practitioners’ discussions compulsory care was presented as a natural intervention following injecting drug use, assumed to be in the child's best interest, and potentially outweighing other protective factors such as family environment and school attendance.
Switzerland: Harm Reduction as Default Mode
Michael: Drifting at the Margins After Care Exit
In general, Swiss practitioners suggested a range of medical and harm reduction measures to address this boy's needs, in so far as the law permitted. We will probably help him to either go through withdrawal or propose an agonist treatment. All the while explaining how to inject properly, what the risks are, checking that he has a hepatitis B vaccination. Do all that we can that is prevention, and that we can normally do. At the moment, we would not be allowed to say “Go to [local DCR] to inject there.” (SDT, SWI5)
Embracing and advocating harm reduction measures was a mutual theme in the Swiss data, alongside a strong presence of medical and psychological discourses, as illustrated in statements such as: “He may be someone who is scared, fragile, fearful, and with lots of past traumas, who believed that things would change, who was disappointed, there may be lots of things” (SDT, SWI5). While a report to child protection services was described as mandatory by some interviewees, anonymity at NSPs rendered this duty irrelevant for several others. Many interviewees clearly believed that DCRs constitute a natural and legitimate harm reduction intervention that should be available also for persons under 18. The best thing would be for him to lie to us and tell us that he is 18 years old and for that to be believable. That he looks older, because that would enable us [at the DCR] to do our best work, in other words to accompany him in safe behaviours and the least dangerous practices possible and that with time, we manage to create a link and contact a network of care that would be adapted to him. (HR, SWI6)
As implied by the final part of the excerpt, harm reduction services were sometimes positioned by Swiss practitioners as part of a wider, long-term change process, involving other care agents and support systems. However, much discussion in relation to the first vignette revolved around the contradiction between anonymity granted for NSPs, but not for injecting on site at DCRs. Even in cantons where DCR operates according to the principle of universal access, staff retain the right to ask for identification when in doubt about the person's age. This difference regarding anonymity makes it possible for minors to retrieve needles and syringes, including from vending machines, but prevents them from injecting in supervised drug consumption facilities. One interviewee stated: [W]e had this case today. A young person came by, and he said “I’m soon 18” but in fact, I could tell he was much younger. He took the injecting equipment he needed and left. I have never seen him before; I don’t even know his name. (HR, SWI6)
The legal ambiguity was unanimously criticized since it was described as creating a more unsafe health situation for this group: The young users don’t go very far from our facilities to use, they inject in the forest [close by]. Generally, we make sure that they bring back the used equipment just afterwards, so that we can do a little evaluation of the health status of the person. (HR, SWI6)
Little attention was given to the boy's social situation in Swiss discussions, but one interviewee said that the ideal situation would be if he was in supported housing, because if so “one can assume that there are things that have more or less already been addressed.” (SW, SWI5)
In relation to what should happen in this specific case, Swiss participants expressed a shared critique of current legislation that without exception prevents legal minors from accessing DCRs. One interviewee stated that if meeting this boy, they would “effectively encourage him to lie to go to a place where he could use safely, also perhaps help him manage his use, use the right techniques” (SW, SWI6). On a discursive level, this way of reasoning signals a position of resistance characterized by criticism and opposition towards the current legislation and treatment system (Selseng & Ulvik, 2016). This resistance positioning—us against the system—cast practitioners as the boy's advocates, while the boy is positioned as in acute need of the protection and guidance from the DCR and its staff. However, beyond immediate health risks, a wider discussion as to if and how it might be in the boy's best interests to access a DCR was lacking.
Sara: Living at Home and Planning to Inject
Swiss practitioners made clear that the girl in our second vignette could access harm reduction services such as NSPs without any problems, where she would be offered information on injection hygiene and training in safe injection practices. [I]f it is not us as professionals who provide her with this information, she will go on the internet or on social networks to get the information, or it might even be someone else who would do the injection for her, so better she gets the answers from professionals. (HR, SWI6)
The justifying motive given for why harm reduction interventions are deemed suitable illustrates how the girl is simultaneously positioned as an active, competent agent (in relation to harm reduction services) and as a vulnerable, marginalized “youth-at-risk” (in relation to other sources of information/guidance). The practitioners are positioned with responsibility and potential to influence the girl's possible future injection practices. In sum, what would happen was also mainly what Swiss interviewees said should happen. The ideal situation matches the reality quite well in the sense that we have equipment to do exercises, we have fake arms to train on, and that, regardless of the person's age, we can do that, and we would do that. (HR, SWI6)
Adding to the harm reduction focus, there was also a strong presence of medical and psychological discourses in the Swiss discussion on suitable interventions: There is not this urgency of craving or withdrawal that adds itself to the situation, so there is perhaps room to take the person to a psychologist, see if she can be distracted from this need to use through injection. (…) [We must] find things to help provide answers and solutions to her suffering. Because there must be something psychological. (SDT, SWI5)
After making the medical assessment that no withdrawal symptoms are at hand, the frontline worker directs attention to Sara's internal motivations and assumed problems and the explanation is again psychological. The term “suffering” occurred frequently in the Swiss discussions and underpinned the depiction of the girl as being vulnerable and fragile, positioning her as passive and in need of having others intervene on her behalf. This psychological positioning conflicts with the parallel portrayal of the girl as a rational and competent actor, capable of deciding what is in her own best interests. The coexistence of these contradictory positions could be interpreted as reflecting and reproducing a larger discourse on harm reduction, based on independence, autonomy, and responsibility, alongside a discourse on “youth at risk,” based on vulnerability and paternalism. The Swiss interviewees did not mention reporting the girl to child protection services, nor did her social situation or family relations come up in the discussion.
Ali: Injecting Before Class
The Swiss practitioners’ discussion in relation to the final vignette described a scenario where a combination of contacts with professionals and interventions could be activated, depending mainly on the initial assessment made by the school nurse but also on Ali's wishes. While relational and social dimensions were mentioned, the concrete interventions that were suggested all focused on the boy as an individual. I think she [school nurse] would contact us. And then we would evaluate what is going on at the drug use level and then also evaluate the young person's reasons, whether he has a network and what resources are available and then, of course, put in place some medical treatment (…) To start with, harm reduction advice, but also surely to offer an alternative. Maybe discuss opioid substitution therapy. It all depends on where the young person is at. (SDT, SWI6)
In terms of discursive elements in the excerpt, it appears that the practitioner is articulating two different discourses, that of medicine (“and then, of course, put in place some medical treatment”; “discuss opioid substitution therapy”) and of harm reduction (“evaluate the young person's reasons”; “[give] harm reduction advice”). Given differences in the attribution of agency, this discursive combination ought to be paradoxical. However, as noted by Szott (2015) in relation to adult drug treatment services, practitioners may very well manage to strategically use these two approaches in their work with clients who use drugs. This seems to be case also for our Swiss practitioners in relation to our vignettes: I’ve experienced a similar situation (…) [T]hat young man was using while still living at home, so his environment was relatively secure. He couldn’t go to the drug consumption room, but he received treatment. In the end, he managed to finish high school. (…) We needed to respect his choices to inject, while at the same time, of course, trying to determine what the suffering behind him was all about because there was quite a lot. (SDT, SWI5)
This statement illustrates the Swiss tendency to define minors who inject as both competent actors, capable of deciding what is in their best interest, and as vulnerable persons who are suffering and therefore in need of professional support (cf. Andersen & Järvinen, 2007)
Wales: Drug Use as Secondary Concern
Michael: Drifting at the Margins After Care Exit
In contrast to the other two countries, Welsh practitioners’ primary concern when discussing our first vignette was the boy's unclear housing situation. This was related to a perceived lack of supported housing facilities accepting minors who use drugs, especially in rural areas. The first priority would be trying to get him into accommodation prior to starting to talk about substance misuse issues. The person would see that as their urgent issue. Ideally the public sector would take responsibility and meet the demands that are there (…) I would say we’d really struggle to deal with someone in that situation. That person has complex needs, not just substance misuse. We need to address some of the other issues prior to the substance misuse. (HR, WAL4)
This housing-oriented way of reasoning might be interpreted as a reflection of youth homelessness and a “housing first” approach been high on the policy and research agenda in Wales for many years (Gaetz et al., 2021). Housing first is based on the idea of homeless people as rights-bearers with legitimate entitlements, and harm reduction is a core principle within this approach. That Welsh practitioners’ discussions mainly revolved around the boy's social and relational situation, not his drug use, could be interpreted as stemming from this more rights-based housing-oriented approach. In addition to housing assistance, relational-based and social participation interventions were deemed appropriate. This was also presented as what should happen: Scenario says he has no family connections (…) We offer a programme about helping young people make connections while they’re in foster care. In a case like this when you’ve got a 16 year old who looks like he's on his way out of the care system, that plans are put in place for him to be developing connections. Whether that be with professionals, family members (…) Otherwise, he’ll be left in a B&B with a link worker who contacts him every couple of weeks, that should be avoided if possible. (SW, WAL3)
While clearly being viewed as “at risk,” suggesting a child protection orientation, Michael was simultaneously portrayed by the frontline workers as immersed in a social setting and positioned as a family member. Following logically from this, the suggested interventions all aimed to promote social interaction and relations. However, as indicated by the last sentence of the excerpt, this is not always guaranteed.
Sara: Living at Home and Planning to Inject
There was a clear focus on voluntary interventions as the most likely route of action in Wales for the girl in our second vignette. Suggested interventions were clearly linked to family and parental responsibilities in relation to meeting her needs, signaling a family-service oriented approach: [B]ecause she's living at home you’d need a whole family approach to any assessment or intervention taking place. There could be a tendency to focus on the young person as she's the one presenting with the issues, but clearly mum and dad if they’re on the scene, or carers, need to be very much involved in any type of intervention that was going on with that young person. (SW, WAL3)
Rather than focusing on the girl's potential inner state, Sara was positioned by Welsh frontline workers as a family member, and the parents were attributed responsibility for the care and well-being of their child. Still, practitioners shared the individualized understanding that a person-centered “harm reduction route” would be appropriate, “to inform her practice” (HR, WAL4). The harm reduction discourse turns the focus to the individual drug user as, to use Campbell's and Shaw's (2008) apt term, “ethical subjects” willing and able to change out of concern for their own health. References to judicial guidance on consent and capacity were frequently made when discussing Sara's case, “to understand that individual's capacity to have harm reduction conversations,” as one practitioner put it (HR, WAL4). As in both the Swedish and Swiss focus groups, some participants emphasized that “the harm reduction conversation” should “explore other means of consumption before injecting” (HR, WAL3). At the same time, the requirement for visitors to register to gain access to NSPs means that meeting a minor with plans to inject at a Welsch NSP would trigger a duty to inform child protection services. As one interviewee put it: “They can still walk out with needles but that's the policy” (HR, WAL4). Subsequently, minors either “lie about their age [at the NSP], or go straight to a pharmacy where they won’t be asked those questions” (HR, WAL4). In practice, this results in very few legal minors visiting specialized NSP in Wales, according to our interviewees.
Ali: Injecting Before Class
With the third vignette, once again, the primary focus of Welsh participants was not on drug use per se. In this case, they focused on school retention. The unanimous assessment was that the boy in our final vignette would be expelled from school: “Even a whiff of cannabis use, they’re out” (SDT, WAL3). The rising number of permanent school exclusions in Wales has been a subject of political and public concern for a long time (McCluskey et al., 2019) and participants all agreed that such exclusions were inappropriate: “They should be kept in school to get the support they need, get a warm meal and then the services should be reaching into the school,” as one interviewee put it (HR, WAL4). The desired scenario expressed was “support don’t punish” (HR, WAL3) and mainstreaming harm reduction in schools to mediate similar situations. The harm reduction discourse rests on the assumption that if informed on safer injection practices, people who use drugs will use this information to minimize harms and risks to which they are exposed. The discourse is articulated in the following excerpt where the frontline worker asserts that there is substantial scope for intervention in Ali's case. There's a massive piece of work we can do there, with the college and young person. Why does he feel the need to do it in college? What's going on in the home or wherever he's living, that he doesn’t feel safe enough to do it there? Minimise the risk when he does go into college. (SW, WAL3)
Family obligations or parental involvement were not raised in relation to meeting the needs of this boy. Instead, the question of age related to competence came through clearly in the practitioners’ discussion: “At 17 if the person didn’t want their parents to know, they’re at an age where they can make the decision not to have them involved” (HR, WAL3). This may be explained in part by the policy environment. In Wales, a 17-year-old has a right to access harm reduction services without parental consent, which is well known among frontline workers. This way of reasoning links not only to the autonomy implied by the harm reduction discourse, but also to the child rights principle of a right to be heard. Regarding the issue of child protection orientation, the discussions here suggest a child-focused, rather than a family-service or child protection, approach.
Discussion
This paper set out to explore if and how distinct drug policy contexts and child protection systems appear in front-line workers’ talk regarding children who inject drugs, and whether distinct policy settings might be associated with differential institutional responses. Across the three countries studied, injecting drug use among minors was framed in distinctly different ways. In Sweden, it was constructed as an alarming behavior warranting abstinence-oriented responses, while in Switzerland it was approached through a medicalized harm reduction lens. In Wales, by contrast, drug use was downplayed in favor of social and relational concerns. Common to all, however, was a tendency to propose interventions that largely mirrored existing practices. In making sense of the vignettes and deciding on appropriate measures, our analysis shows that workers in their discussions draw on culturally available discourses—medical, youth at risk, psychological, and harm reduction—representing differing and sometimes conflicting ways of understanding as regards to why minors inject drugs and the most appropriate way to deal with this issue. Country characteristics in terms of perceptions of the problem at hand, positioning of the child, and key interventions are summarized in Table 2.
Country Comparison: Summary of Key Characteristics.

In Sweden, the focus was squarely on drug use and injecting, a behavior that was assessed as very serious and alarming, irrespective of the child's social situation. Swiss frontline workers also focused on the minor's drug use, but with a firm medicalized harm reduction approach guiding their needs assessments. In Wales, on the other hand, drug use was seen as secondary in all three cases, with social context and relational dimensions being at the forefront of their harm reduction-oriented discussions. These different perceptions were linked to diverging institutional responses across settings. For example, in Sweden, there was little to no explicit role for harm reduction as applied to minors, and current age restrictions for NSP-access was not questioned, whilst in both Switzerland and Wales harm reduction services were considered an appropriate response to all three cases, albeit with different orientations. These diverging patterns were partly expected, given the previously described drug policy contexts. An unexpected finding, however, was the strong tendency in all countries to propose interventions that corresponded to those that already exist, largely supporting “business as usual,” whether strongly focused on harm reduction or abstinence. Indeed, while it may be fairly easy to critique compulsory measures as standard procedure, it is not obvious that a harm reduction approach—not developed with this age group in mind (Cook et al., 2010)—is appropriate for minors. For example, anonymity and low-threshold access are core harm reduction principles that may not self-evidently be in a child's best interests. As Järvinen and Andersen (2009) have argued, too much focus on short-term harm reduction goals may marginalize other priorities and long-term ambitions related to social integration in terms of education, family, and work. Our findings also indicate that broad policy decisions may limit the space for decision-making in individual cases by making rules applicable to all children of similar categories. This is the case with age restrictions on harm reduction in both Sweden (regarding NSPs) and Switzerland (regarding DCRs). Case-by-case best interests’ assessments, relying on the expertise of the practitioner and the wishes of the individual are precluded, given the wider policy decisions that were taken for all those under 18. As noted previously, given long-standing judicial guidance, Wales was the only one of the three countries with protocols allowing for a degree of legal discretion at the door of NSPs. Through that discretion the autonomy of the children could be respected and acted upon, although this clashed with mandatory reporting duties, resulting in very few legal minors visiting these harm reduction services. The need for discretion at DCRs was expressed in Switzerland, but it would currently require breaking the rules, which practitioners were more than willing to propose based on their interpretation of the best interests of those standing in front of them. In Sweden, on the other hand, the space for exercising expert discretion was much narrower and clearly linked to the prevailing legal and policy system, the existence of which was not questioned.
Regarding child protection orientations, our findings suggest that when injecting drug use is at play, institutional responses may not readily match conventional characterizations (cf. Berrick et al., 2017). Switzerland stands out as our vignette-based analysis reveals a noticeable absence of child protection discussions. Sweden, however, is most often positioned as family-service oriented, but in-home interventions were rarely mentioned by our Swedish participants. When it comes to drug use at the perceived severity represented by injecting, Swedish participants were more inclined to suggest compulsory measures and out of home-placements, signaling a child protectionist orientation. And, while Wales has been classified as having a child protection orientation, in cases regarding injecting drug use our results rather suggest a family-service approach, as well as child-focused orientation. The reasons for these differences are not easily explained and need further examination. One possible explanation could be each country's legal framework and practical guidelines on child protection, and that the directives to report are stronger and threshold for compulsory care lower in Sweden than in Switzerland and Wales. Previous research has observed that children's rights, service participation, and attention to family engagement have been firmly imbedded in micro-level social work practices in the UK (e.g., Duffy et al., 2018). Practice in Sweden, on the other hand, has been criticized for paying insufficient attention to participation (Heimer & Pettersson, 2023). As our comparison highlights, in Sweden and Switzerland, the children portrayed in our vignettes were mainly positioned within medical, psychological and “youth at risk” discourses. The need for protective measures became the focus for interventions. However, there were differences regarding the nature of these interventions, with Swiss participants highlighting the rational decision-making capacity of the individual to access harm reduction services and protect them from immediate health threats connected to injecting. Conversely, in Sweden, the need for compulsory measures was attached instead to diminished autonomy due to the seriousness of injecting drug use. Neither Swedish nor Swiss practitioners made any clear differentiation between cases with various degrees of severity when it came to suggested interventions (cf. Åström et al., 2013). Wales was the outlier here with discussions clearly focusing on children within their family and wider social settings, yet all the while emphasizing the need to respect their autonomy. In addition, references were continuously made to assessment tools and guidance protocols for practitioners in this area. Indeed, it was only in Wales that a strong focus on the views and preferences of the children in the vignettes consistently came through, which might signal a system that is both service-oriented and child-focused.
This paper adds to the limited literature on qualitative cross-country drug research and provides new knowledge to support the development of support services and treatment interventions tailored to minors who inject drugs. While responses to injecting drug use are a core harm reduction issue, how to address injecting among under 18s has not been subject of significant research or practice guidance. It is a very complex legal, ethical, and practical dilemma engaging child rights and child protection considerations that are not relevant to adults who inject. Our study was not evaluative, nor have we suggested that any one approach is “better” or “worse. Rather, through a comparative approach, lessons from similar yet distinct settings can open for reflection on local practices and policy frameworks around this rarely discussed challenge.”
Finally, a few last words about language use. Throughout this paper “child” and “legal minor” have been used interchangeably. While acknowledging previous scholarship focusing on possible shortcomings in lumping child and adolescent together within the category of “minor” (e.g., Heirro, 2006) we argue that this terminology is an important point to consider. We acknowledge that 16- and 17-year-olds are not always regarded as children, by others or by themselves. Nonetheless, under 18s in all three countries are children for the purposes of child rights and social welfare legislation. The participants’ compassion and concern for the individuals portrayed in our vignettes came through strongly in all focus groups, and this was clearly linked to the age of the characters in our three scenarios, but the label “child” was rarely used in the vignette-based discussions (only when asked specifically about “the best interest of the child” in a later part of the interview). Instead, terms such as “youth” and “young man/woman” were used. This may be seen as a process of adultification which has been problematized in other contexts, including criminal justice and migration (Dancy, 2014; Hlass, 2020). It is difficult to think of child rights, or the “best interest of the child,” in a consistent way if the word child is not used, if this label is seen as inappropriate, or if behaviors or situations position legal minors as outside of childhood. As Cordero Arce (2012, p. 386) asks, can a child hold rights “if she does not even belong to the category of children?”
Conclusion
This article has presented findings from focus groups with frontline workers actual and potential responses to working with legal minors who inject. Three vignettes served as base for discussion, and we explored if and how distinct drug policy contexts and child protection systems appeared in the workers’ talk, finding distinct defaults across the three countries. Four identified discourses—medical, youth at risk, psychological and harm reduction—were drawn upon when workers depicted needs and suggested suitable interventions. Beyond revealing discourses, the results from this qualitative cross-country comparative research provide new knowledge with the potential to support the development of support services and treatment interventions tailored to minors who inject drugs. This study offers an opportunity to gain an understanding of different countries’ systems regarding children that inject drugs, and to reflect on policy and practices which may otherwise be taken for granted.
Limitations
There is the possibility that those interviewed agreed to take part because they are the most engaged or interested in the topic, meaning that they do not fully represent the broader group of relevant professionals. This is not uncommon in qualitative interview methods. A survey may have produced a wider participant group but would not have allowed the in-depth discussion of the vignettes.
Footnotes
Acknowledgments
We wish to thank Rick Lines and Michelle Hughes at Public Health Wales for their help in setting up the Welsh focus groups, and Russell Turner for his assistance with moderation. Thanks also to Björn Andersson for insightful comments on previous version of the draft.
Ethical Approval
Ethical approval was given by the Swedish Ethical Review Authority (case number: 2021-03361), Commission Cantonale d’Ethique de la Recherche of the Cantons of Geneva and Vaud in Switzerland (case number: 2021-01444), and the Law & Social Sciences Research Ethics Committee, University of Swansea.
Consent to Participate
Informed consent was obtained verbally from all participants prior to their participation and these consents were audio-recorded.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Swedish Research Council for Health, Working Life and Welfare under grant number: 2020-0045.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data supporting the findings of this study are not available due to the sensitive nature of the information and, hence, legal restrictions in accordance with the Swedish Ethics Review Act.
