Abstract
The study examined the predictors of postpartum depressive symptoms among young mothers in rural Limpopo province in South Africa. Cross-sectional data of adolescents and young mothers aged 16 to 24 years from the DIMAMO Population Health Research Centre were used. The centre operates as a rural site of the South African Population Research Infrastructure Network’s Health and Demographic Surveillance System. A multivariate analysis using binary logistic regression was used to identify the predictors of postpartum depressive symptoms among young mothers in rural Limpopo. Postpartum depressive symptoms were experienced by 39.83% of the young mothers. Mothers from food-insecure households were more likely to experience postpartum depressive symptoms (adjusted odds ratio = 2.59; confidence interval = 1.33–5.07; p = .005) compared to those from food-secure households. HIV-positive mothers were more likely to experience postpartum depressive symptoms (adjusted odds ratio = 9.34; confidence interval = 1.56–55.72; p = .014) compared to those who are HIV-negative. Meanwhile, receiving financial support from the partner (adjusted odds ratio = 0.37; confidence interval = 0.20–0.70; p = .002) and a planned pregnancy (adjusted odds ratio = 0.19; confidence interval = 0.08–0.51; p = .001) reduced the likelihood of experiencing postpartum depressive symptoms. These findings highlighted the need for policies that address food security, integrate mental health care into HIV services, strengthen family planning education, and promote partner support among young mothers in rural South Africa.
Introduction
Postpartum depression (PPD), clinically referred to as depressive disorder with peripartum onset according to the DSM-V, is a major depressive episode that occurs during pregnancy or within 4 weeks after delivery (American Psychiatric Association, 2022; Serati et al., 2016). While the term PPD is widely used in public health, this study adopts this clinical framing to align with psychological practice. PPD is a public health concern worldwide, affecting women across diverse socioeconomic contexts. Most studies, however, have focused on adult mothers with fewer addressing adolescent and young mothers, despite evidence that the complexities surrounding early pregnancy may increase the risk of developing depressive disorder with peripartum onset (Ladores & Corcoran, 2019). Adolescent and young mothers in rural areas face additional challenges due to cultural and societal norms that view early motherhood as a deviation from traditional expectations, such as completing education and contributing to family responsibilities. These challenges, combined with limited access to health care and mental health services, place young mothers at higher risk of experiencing PPD compared to adult mothers. In South Africa, the prevalence of PPD among adolescent mothers is reported to be 47% (Gebrekristos et al., 2023), whereas the prevalence among adult mothers ranges from 16.4% to 42.5% (Mokwena & Modjadji, 2022; Mokwena & Mbatha, 2021; Ramchandani et al., 2009; Tomlinson et al., 2004).
Mothers experiencing depressive disorder with peripartum onset are more likely to face emotional distress that can impair their parenting abilities, and reduce their ability to engage with their children, which can negatively affect child development (Lovejoy et al., 2000; Nakić Radoš, 2021). Studies have linked maternal postpartum depressive symptoms during the peripartum period to adverse outcomes such as stunted growth, behavioural problems, and long-term psychological difficulties in children (Avan et al., 2010; Verkuijl et al., 2014). In South Africa, factors associated with PPD among adolescents include being a victim of intimate partner violence during pregnancy (Gebrekristos et al., 2023), while among adult women, additional factors include lack of financial and emotional support from the father, unplanned or unwanted pregnancies, and insufficient maternal support (Tomlinson et al., 2004).
Maternal mental health is often overlooked in South Africa, with depressive disorder with peripartum onset often underdiagnosed and routine screening rarely included in postpartum care (Hung et al., 2014). Consequently, several studies recommend the implementation of screening for PPD during postpartum visits to identify and support affected women early (Gebrekristos et al., 2023). Despite the high burden of adolescent pregnancies, research on symptoms of PPD among adolescent and young mothers in rural South Africa remains limited (Govender et al., 2020; Muthelo et al., 2024; Seakamela et al., 2023; Steventon Roberts et al., 2022). Most existing studies in the country have largely focused on women in general (Hung et al., 2014; Kathree & Petersen, 2012; Mokwena & Modjadji, 2022; Ramchandani et al., 2009; Stellenberg & Abrahams, 2015), with some studies examining HIV-positive women specifically (Mokhele et al., 2019; Mokwena & Mbatha, 2021; Peltzer et al., 2018; Peltzer & Shikwane, 2011). This limited research creates a gap in understanding the prevalence, risk factors, and context-specific predictors of depressive disorder with peripartum onset among young mothers, particularly in rural areas where access to mental health services is limited.
This study aimed to examine the prevalence and predictors of PPD symptoms among young mothers in rural Limpopo Province, South Africa. Specifically, it seeks to answer the following research questions: (1) What is the prevalence of PPD symptoms among young mothers in rural Limpopo Province, South Africa? (2) Which factors are associated with PPD symptoms among the young mothers in rural Limpopo Province? Understanding the factors contributing to PPD symptoms in this population, particularly in a rural setting with limited access to mental health services, will help inform targeted interventions to improve maternal mental health and child well-being. Given the limited research on postpartum mental health among adolescent and young mothers in South Africa, this study will contribute to public health policies and practices tailored to the needs of young mothers in these communities.
Methods
Dataset
We used data collected in 2022 from the DIMAMO Population Health Research Centre (PHRC), which operates as a rural site of the South African Population Research Infrastructure Network’s (SAPRIN) Health and Demographic Surveillance System (HDSS). It covers a population of 116,000 individuals, with a focus on population research in a rural and socioeconomically disadvantaged area. The survey captures information on births, deaths, migration, household demographics, and health issues. This makes it an important resource for understanding the dynamic structure of households and health issues in a rural setting. The findings derived from this setting can inform targeted interventions and policies designed to improve maternal mental health in rural, underserved regions of South Africa. The data were collected from 11 clinics providing services to residents within the DIMAMO HDSS area. The questionnaire was developed in English and translated into the local Sepedi language. Prior to data collection, field workers received training on questionnaire administration and research ethics. The dataset consisted of 360 adolescents and young mothers, including 121 who were pregnant, 7 who had terminated a pregnancy, and 232 who had given birth, all aged between 16 and 24 years. The final sample for this study was 232 young mothers who had given birth in the past 12 months.
Instrument
Postpartum depression was measured using the 10-item Edinburgh Postnatal Depression Scale (EPDS), which captures symptoms consistent with depressive disorder with peripartum onset as defined in the DSM-V. This scale has been validated in the South African context (De Bruin et al., 2004; Seakamela et al., 2023). The DIMAMO questionnaire comprises questions on respondents’ self-reports of PPD-associated symptoms during the past week. The respondents selected responses from a 4-point Likert-type scale. For most items, responses range from 0 (Yes, most of the time), 1 (yes, some of the time), 2 (not very often) and 3 (no, never). Responses are scored 0, 1, 2, and 3 based on the seriousness of the symptom. Items 3, 5 to 10 are reverse scored (i.e., 3, 2, 1, and 0). The total score is calculated by summing the scores for all 10 items, giving a possible range of 0 to 30. A score of 10 or more indicates a positive screening for PPD and suggests the need for further follow-up (Shuman et al., 2022). A cut-off score of ≥ 10 was used to indicate symptoms of depression (Horowitz et al., 2009; Kim et al., 2012; Mmasa et al., 2024). Cox et al. (1987) suggested using a lower cut-off score of 9/10 to minimise the risk of missing true cases of depression, reducing the proportion of missed cases to less than 10%. Some studies in the United States use a lower score of 9 or 10 with a cut-off of ≥10 to reduce failed detection to less than 10% (Kim et al., 2012; Nel et al., 2025). However, in South Africa, studies use a cut-off of ≥12 (Mokwena & Mbatha, 2021; Peltzer et al., 2018) or ≥13 (Gebrekristos et al., 2023; Hung et al., 2014) to indicate the presence of PPD. For robustness of results, this study will also use a cut-off of ≥13 to see if the results will differ from those using a cut-off score of ≥10. Using the two cut-offs, ≥10 and ≥13, supports sensitivity analysis that evaluates the consistency of the results across different cut-offs of PPD symptoms.
The independent variables in this study include several demographic, socioeconomic, and behavioural factors. Categorisation of the independent variables was informed by existing literature on maternal mental health research. Age is categorised into two groups: 16–19 and 20–24 years to reflect differences between mid-to-late adolescence and young adulthood, as younger adolescents are more vulnerable to mental health disorders (Kassa et al., 2024). Educational level is classified into three categories: less than high school, secondary education or below, and tertiary education. These different categories have been linked to differences in maternal mental health outcomes (Kotimäki et al., 2020). Employment status is a dummy variable indicating whether an individual is employed or not (1 = Yes, 0 = No), to capture the influence of employment on maternal mental health. Employment is a known social determinant of mental health (Gariépy et al., 2022; Hammarström et al., 2024; Muchemwa & Sodi, 2025b). Parity is categorised into primiparous (women who have given birth for the first time) and multiparous (women who have given birth two or more times), as first-time mothers are more likely to experience mental health challenges (Dol et al., 2021). This variable will help assess whether primiparous or multiparous mothers are likely to experience PPD.
Food security is measured as a categorical variable with two categories: food secure and food insecure. Food security was assessed using the validated Household Food Insecurity Access Scale (HFIAS), which includes nine items capturing household food access over the past 12 months. If a respondent answered yes to any of the questions, they were classified as belonging to food-insecure households represented by ‘1’; if they answered no, they were classified as from food-secure households represented by ‘0’. This categorisation helps examine how living in food-insecure or food-secure households influences mental health (Kassa et al., 2024). The respondents were asked whether they drink alcohol or not; a dummy variable was created, where ‘1’ represents individuals who consume alcohol and ‘0’ represents those who do not. Alcohol consumption was categorised like this to assess whether consuming alcohol is linked to depressive symptoms. Considering that alcohol consumption has been linked to an increased risk of depressive symptoms (Seakamela et al., 2023). Similarly, smoking status is also a dummy variable, with ‘1’ indicating individuals who smoke cigarettes and ‘0’ indicating those who do not. Smoking has been associated with adverse mental health outcomes (Muchemwa & Sodi, 2025a; Peltzer & Pengpid, 2020). By categorising it as a dummy variable, we can assess its association with PPD symptoms. Pregnancy planning status is represented as a dummy variable, with ‘1’ indicating that the pregnancy was planned and ‘0’ indicating that it was not, since unplanned pregnancies are associated with increased risk of depressive symptoms (Mbawa et al., 2018; Seakamela et al., 2023; Stellenberg & Abrahams, 2015). HIV status is another dummy variable, with ‘1’ representing HIV-positive individuals and ‘0’ representing those who are HIV-negative. This was done due to HIV status’ association with increased vulnerability to mental health disorders (Seakamela et al., 2023; Steventon Roberts et al., 2022). Partner financial support is also measured as a dummy variable, with ‘1’ indicating those who are financially supported and ‘0’ indicating no financial support. This was done to examine whether financial support protects mental health (Seakamela et al., 2023). Finally, the respondents were asked whether they experienced violence from their partners, for partner violence, a dummy variable was created, with ‘1’ representing individuals who experienced partner violence and ‘0’ representing those who have not, consistent with the literature violence has a strong association with adverse maternal mental health outcomes, including postpartum depression (Gebrekristos et al., 2023).
Analysis
A reliability test was conducted for the 10-item EPDS, which demonstrated high internal consistency in our sample (Cronbach’s α = .88), indicating that the items reliably measured PPD. We first conducted a univariate analysis to describe the characteristics of the sample, and a bar chart was produced to illustrate the prevalence of PPD symptoms. Bivariate associations between each predictor variable and PPD were examined using chi-square tests. To identify independent predictors of PPD, we conducted a multivariate logistic regression to model the relationship between independent variables and the probability of the outcome (PPD) occurring, providing estimates of adjusted odds ratios. Unlike linear regression, logistic regression was appropriate for this study as it does not assume a normal distribution of the dependent variable. In the main regression analysis, PPD used a cut-off of ≥10 for PPD symptoms. To assess the robustness of the results, two additional sensitivity checks were performed. First, employment status, educational level, and smoking were excluded from the regression models because some categories had few observations (see Appendix 1, Table 4). Second, we repeated the multivariate analysis using an EPDS cut-off of ≥13 (see Appendix 1, Table 5).
Ethical considerations
The study used secondary data; permission to use the dataset was sought from DIMAMO. Access was granted to the authors for the complete anonymised dataset, which did not contain any personal identifiers such as names or contact details. Ethical approval for the secondary analysis was not required, as ethical clearance had already been granted for the primary study by the Turfloop Research Ethics Committee (TREC) at the University of Limpopo. DIMAMO adhered to all required ethical protocols during data collection.
Results
Table 1 presents the background characteristics of the young mothers. The majority of the mothers (78.88%) were aged between 20 and 24 years, while 21.12% were aged between 16 and 19 years. Most mothers (86.64%) had completed secondary education, tertiary education was completed by (10.78%), with only 2.59% having less than high school education. The majority of the mothers were unemployed (98.27%), with only 1.73% employed. The sample was predominantly primiparous (91.34%), with only 8.66% being multiparous, indicating that most respondents were experiencing their first childbirth. More than half of the respondents (62.07%) were food insecure, while 37.93% were food secure. Most participants (85.34%) reported not drinking alcohol, while 14.66% reported alcohol use. The majority of mothers did not smoke (98.70%), with only 1.30% smoking. The majority (79.74%) reported that their pregnancy was unplanned, compared to 20.26% with planned pregnancies. Most respondents (95.61%) were HIV-negative, and 4.39% were HIV-positive. Almost two-thirds (64.50%) of the respondents received financial support from their partners, while 35.50% did not receive partner financial support. A small proportion of participants (8.70%) reported experiencing partner violence, whereas the majority (91.30%) did not experience.
Background characteristics of the young mothers.
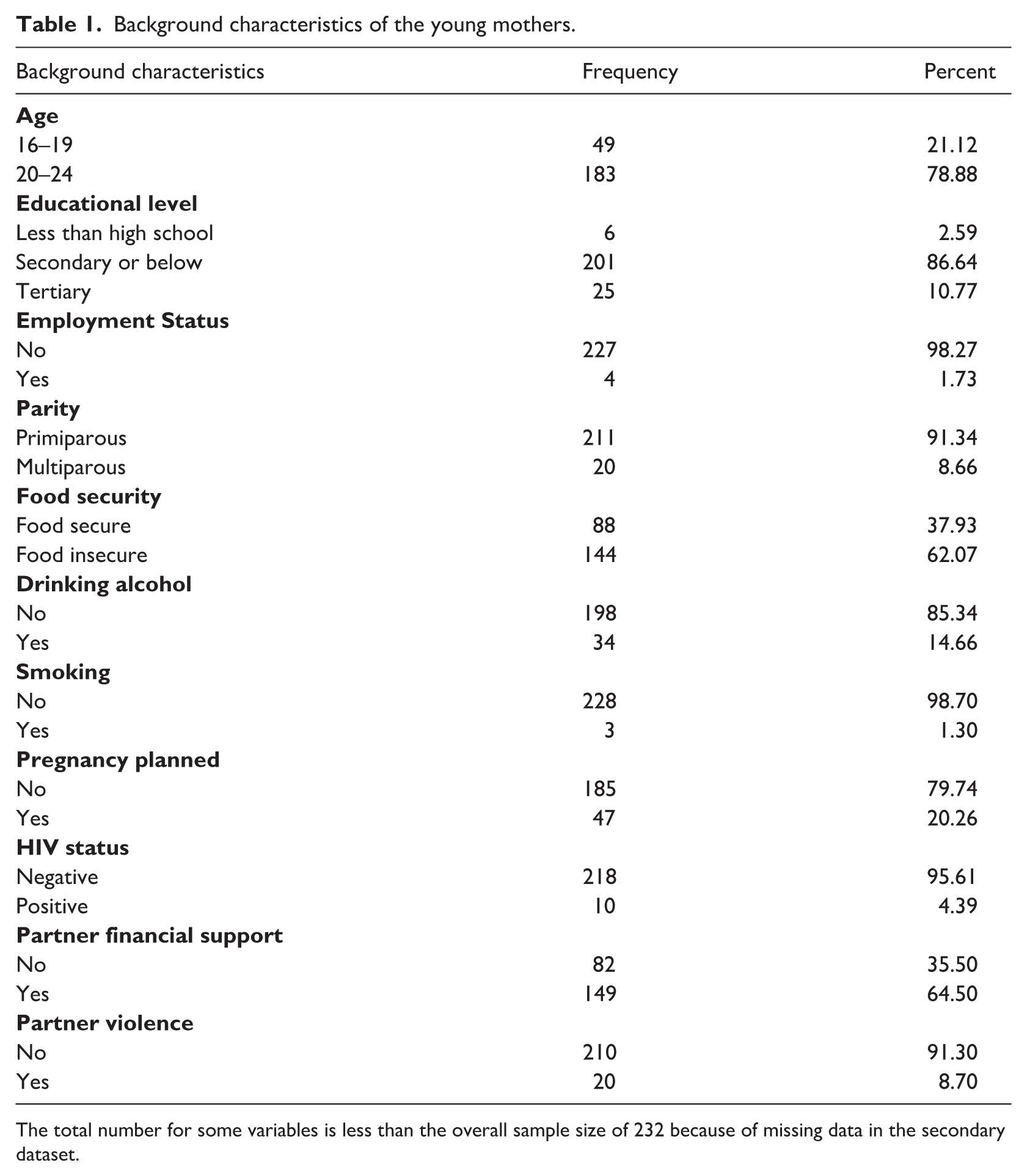
The total number for some variables is less than the overall sample size of 232 because of missing data in the secondary dataset.
Figure 1 indicates the prevalence of PPD symptoms among young mothers; 39.83% (n = 92) reported experiencing depressive symptoms. While the majority were symptom-free 60.17% (n = 139), the prevalence of depressive symptoms (40%) is relatively high compared to global estimates.
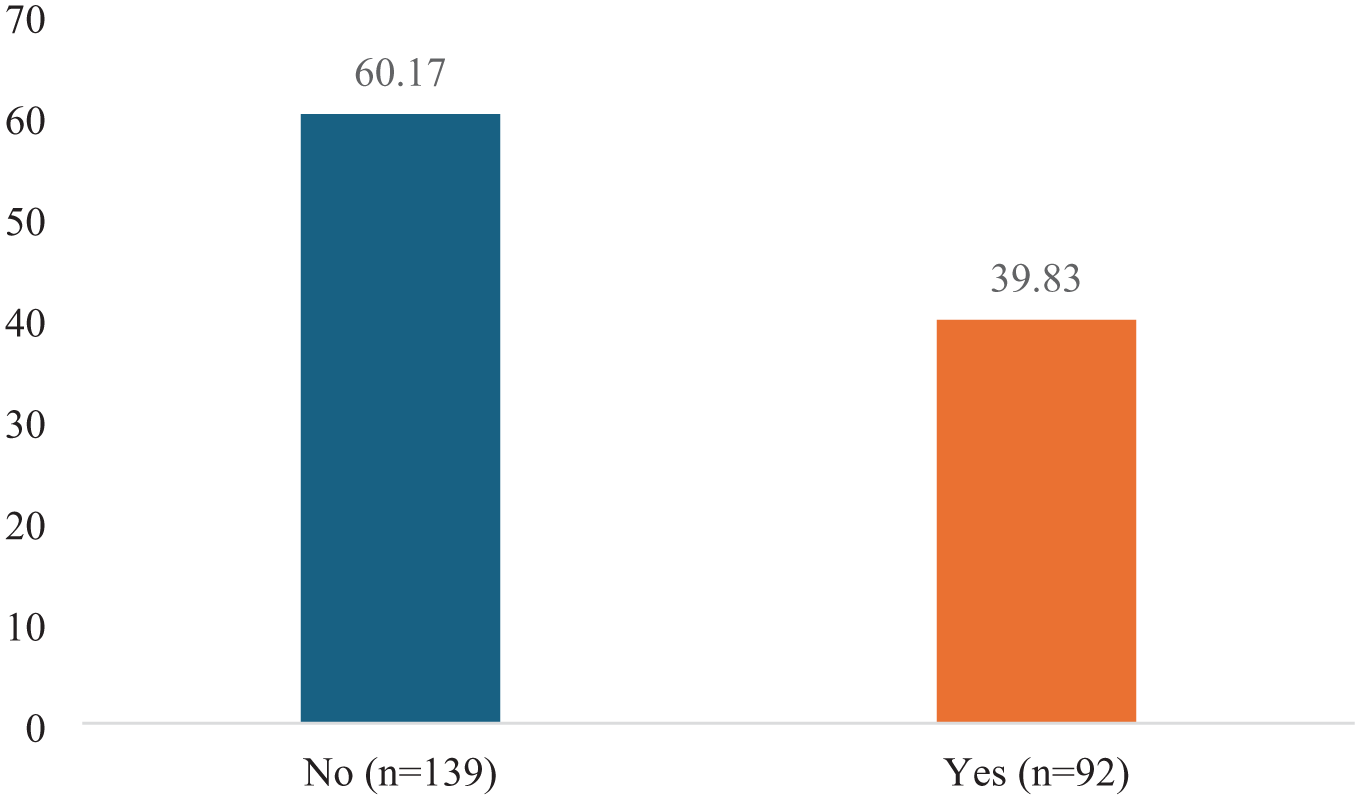
Percentage of young mothers who experienced PPD.
Table 2 indicates the results from Chi-square analyses showing the bivariate association between each predictor variable and PPD symptoms among mothers. Food security and HIV status were significantly associated with reports of PPD symptoms. Young mothers from households which are food insecure had higher reports (48.61%) of PPD symptoms compared to those from food-secure households. Those whose HIV status was positive had higher reports (80%) of PPD symptoms compared to those with negative HIV status. Mothers who planned their pregnancy (14.89%) and those whose partners financially supported them (29.05%) had lower reports of PPD symptoms compared to those who did not plan their pregnancy (46.20%) and those whose partners did not financially support them (59.76%), respectively.
Percent distribution of young mothers with PPD symptoms by background characteristics.
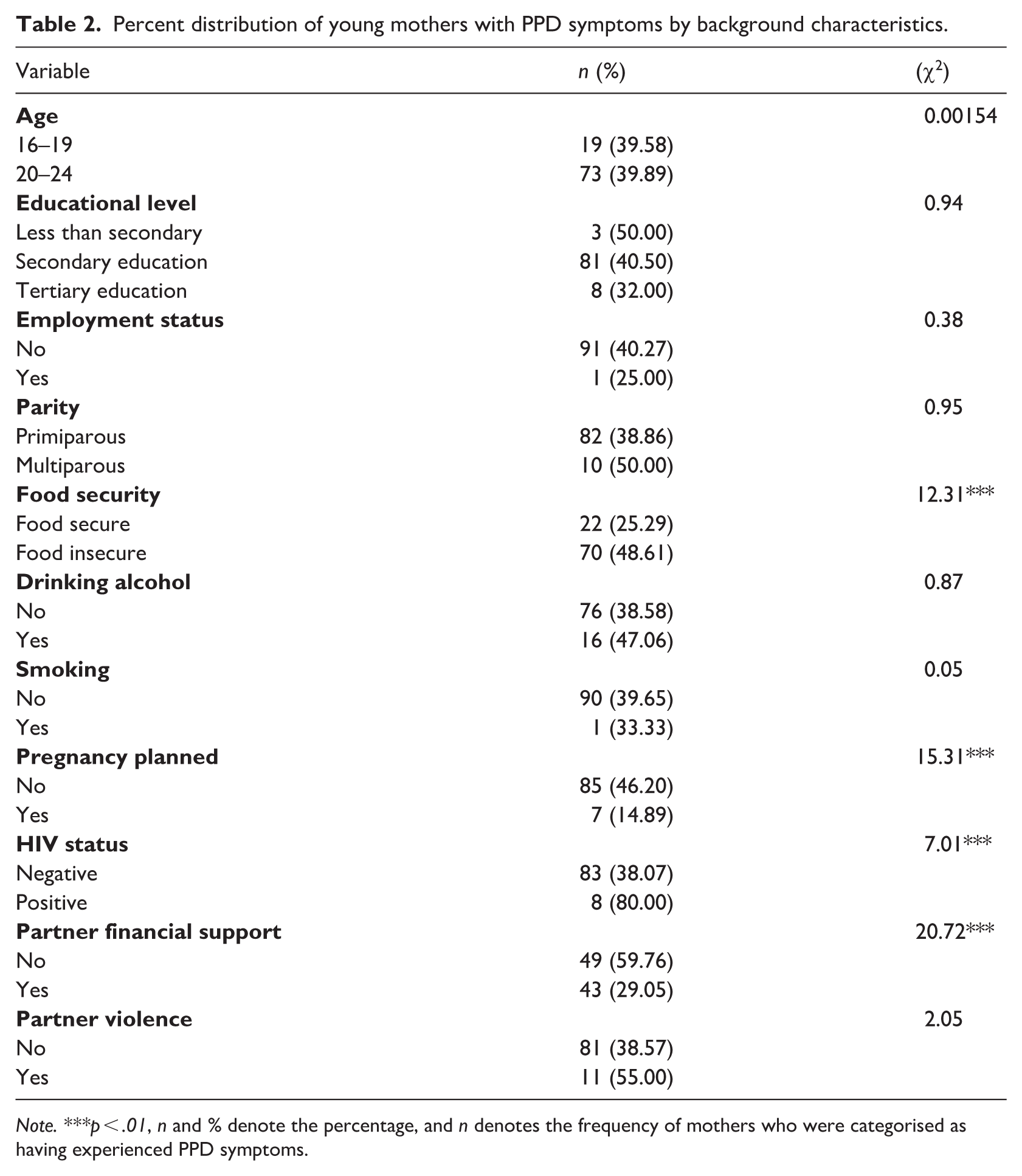
Note. ***p < .01, n and % denote the percentage, and n denotes the frequency of mothers who were categorised as having experienced PPD symptoms.
Table 3 indicates the adjusted odds ratios of the logistic regression, conducted to examine the predictors of PPD symptoms. Young mothers from households who are food insecure were significantly more likely to experience PPD symptoms (adjusted odds ratio [AOR] = 2.59; confidence interval [CI] = 1.33–5.07; p = .005) compared to those from households who are food secure. Young mothers who are HIV positive were significantly more likely to experience PPD symptoms (AOR = 9.34; CI = 1.56–55.72; p = .014) compared to those who are HIV negative. Meanwhile, receiving financial support from the partner significantly reduced the likelihood of experiencing PPD symptoms (AOR = 0.37; CI = 0.20–0.68; p = .002) compared to not receiving financial support from the partner. Having planned the pregnancy significantly reduced the likelihood of experiencing PPD symptoms (AOR = 0.19; CI = 0.08–0.51; p = .001) compared to an unplanned pregnancy. Educational level, age, parity, partner violence, and drinking alcohol were statistically insignificantly associated with PPD symptoms.
Multivariate results for the association between all predictor variables with PPD symptoms.
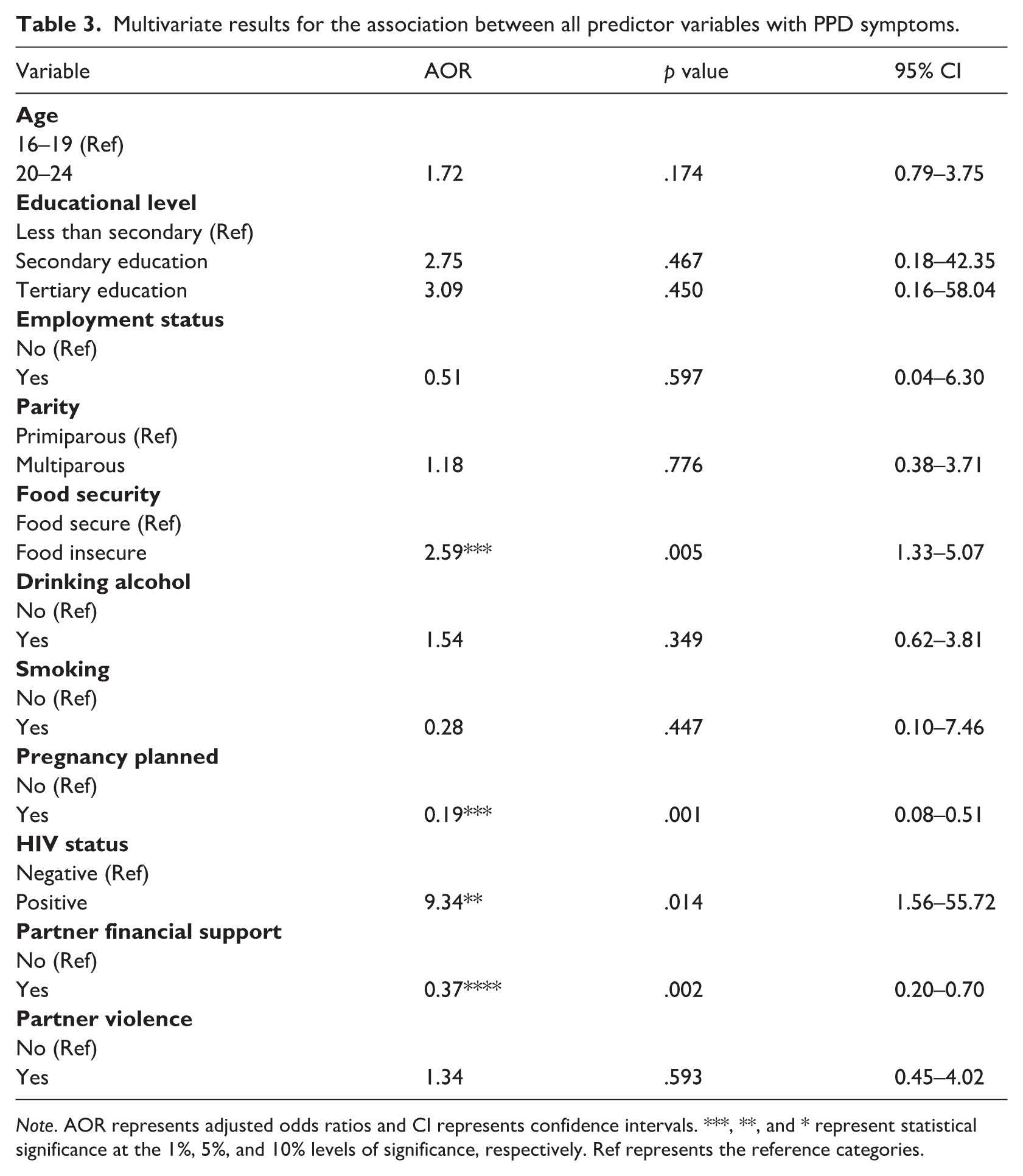
Note. AOR represents adjusted odds ratios and CI represents confidence intervals. ***, **, and * represent statistical significance at the 1%, 5%, and 10% levels of significance, respectively. Ref represents the reference categories.
As mentioned in the methods section, for robustness, we also used a cut-off score of ≥13 to indicate the presence of PPD, considering that other studies in South Africa have used it (see Appendix 1, Table 5). The findings are qualitatively the same, except for the variable HIV status, which became insignificantly associated with PPD symptoms. The ≥10 cut-off captures more mothers at risk, which is essential for early intervention in rural settings where PPD may be underdiagnosed due to limited resources. Also, this shows that the ≥10 cut-off can still be valid and beneficial in South Africa, as it broadens the scope for identifying at-risk mothers.
Robustness tests
To assess the robustness of our findings, two additional sensitivity analyses were conducted. First, we re-estimated the multivariate logistic regression model after excluding educational level, employment status, and smoking, as these variables had very few observations in certain categories. The results were consistent with the main model, with food insecurity, unplanned pregnancy, HIV-positive status, and lack of partner financial support remaining significant predictors of PPD symptoms. Second, we repeated the analysis using a higher cut-off of ≥13 on the EPDS to define the PPD symptoms, instead of the main threshold of ≥10. The overall pattern of results was largely unchanged, with food insecurity, unplanned pregnancy, and lack of partner financial support remaining significantly associated with PPD symptoms. However, in this stricter model, HIV status was no longer statistically significant. These robustness checks suggest that while the strength of association for some predictors may vary depending on the specification, the core findings, particularly food insecurity, pregnancy planning, and partner financial support, are robust.
Discussion
In this study, 39.83% of young mothers in rural Limpopo experienced PPD. A study conducted in rural Mpumalanga indicated that 35.6% of mothers experienced PPD (Peltzer et al., 2018), while another study in a rural setting in KwaZulu-Natal found a prevalence of 42.5% for depressive symptoms among mothers (Mbatha et al., 2020). However, both studies focused on women in general rather than specifically on young mothers. In contrast, a study focusing exclusively on adolescent mothers in urban areas of KwaZulu-Natal reported an even higher prevalence of 47% (Gebrekristos et al., 2023). The findings indicate the burden of PPD symptoms among rural young mothers, particularly when compared to broader populations of women. The high prevalence of PPD in our study may reflect the unique vulnerabilities of adolescent and young mothers, who often face socioeconomic instability, lack of financial independence, and limited social support. These challenges are common in rural Limpopo, where access to mental health services is limited, health facilities are distant, and poverty and unemployment are widespread. In addition, the stigma associated with young motherhood may lead to feelings of isolation and stress, which increases the risk of PPD symptoms. The findings indicate that young mothers from food-insecure households had a greater likelihood of experiencing PPD symptoms compared to those from food-secure households. This is consistent with previous studies in South Africa, which have shown that food insecurity and food insufficiency are associated with increased risk of PPD (Kathree & Petersen, 2012; Tsai et al., 2016). Tsai et al. (2016) further highlight the heterogeneity in depression severity, showing that food insufficiency has a stronger impact on women already experiencing high levels of depression compared to those with milder symptoms.
These findings suggest that the effects of food insufficiency are not uniform but are particularly more pronounced among those most vulnerable to severe depression. Similar to our study, Tsai et al. (2016) used the EPDS to measure PPD; however, their focus was on women in general rather than young mothers, and their research was not conducted in rural settings. Evidence from rural contexts outside South Africa indicates that adolescent mothers with PPD are more likely to report food insecurity (Kassa et al., 2024). Our findings are likely due to the challenges young mothers face in the absence of stable income and financial independence, where the inability to provide adequate nutrition for themselves and their infants may contribute to feelings of guilt and hopelessness, increasing the risk of PPD symptoms. Furthermore, rural areas such as Limpopo are characterised by high levels of poverty and limited employment opportunities, which can worsen the psychological impact of food insecurity.
Being HIV positive increased the likelihood of experiencing PPD symptoms among the young mothers. These findings are consistent with previous studies showing that HIV-infected women are more likely to experience PPD compared to their HIV-negative counterparts (Atuhaire et al., 2021), due to stigma associated with both pregnancy at a young age and HIV, alongside experiences of discrimination and limited social support. Also, HIV-positive mothers face additional stressors, such as concerns about vertical transmission, managing antiretroviral therapy during pregnancy and breastfeeding, and financial constraints, all of which contribute to psychological distress (Fords et al., 2017; Ogueji, 2021; Payán et al., 2019). However, a study in Malawi indicated a similar prevalence of PPD between HIV-infected and HIV-uninfected mothers; however, it was higher among women with HIV-infected infants (Dow et al., 2014). These findings highlight the importance of monitoring PPD in mothers with HIV-positive infants. Young mothers in rural areas, such as Limpopo, may have limited access to mental health and social services, increasing their vulnerability. These findings highlight the importance of integrating mental health screening and support into antenatal and postpartum care for HIV-positive mothers, as well as targeted interventions to address stigma and improve access to psychosocial support.
Young mothers who were financially supported by their partners were less likely to experience PPD symptoms than those who were not financially supported. This is consistent with studies which have shown the importance of partner financial support in raising children. A lack of financial support from the father of the baby is a risk factor for PPD (Kathree & Petersen, 2012; Mokwena & Modjadji, 2022). The findings could be attributed to the role of financial support in reducing stress and improving mental well-being among young mothers. Financial support from partners reduces the economic burden associated with parenting, enhances access to basic needs, and fosters a sense of security and stability. This, in turn, may reduce the risk of PPD by mitigating financial stress and promoting a more supportive environment for the mother and child.
Having planned the pregnancy reduced the likelihood of experiencing PPD symptoms compared to an unplanned pregnancy among the mothers. This is consistent with a study conducted in South Africa, which indicated that mothers in the Free State province who planned their pregnancy were less likely to experience PPD (Mokwena & Modjadji, 2022). Having an unplanned pregnancy increases the risk of experiencing PPD, potentially due to emotional distress and reduced social or partner support (Mbawa et al., 2018; Stellenberg & Abrahams, 2015). Young mothers who plan their pregnancies may be more emotionally prepared and supported, as planning often involves readiness for the physical, emotional, and financial responsibilities of motherhood. In rural contexts, planned pregnancies may align with cultural or societal expectations, reducing the stigma and stress associated with young motherhood.
In our study, educational level, age, employment status, parity, partner violence, drinking alcohol, and smoking were not associated with PPD symptoms. These findings align with a study conducted in Mpumalanga, South Africa, where age, marital status, education level, employment status, and number of own children were also statistically insignificant predictors of PPD (Peltzer & Shikwane, 2011). However, unlike some previous studies that report alcohol use and partner violence as significant risk factors for PPD (Gebrekristos et al., 2023; Seakamela et al., 2023), we did not observe these associations. This discrepancy may be due to the small sample size and limited variability in alcohol consumption and experiences of partner violence within our rural sample, which may have reduced the statistical power to detect significant associations. Furthermore, social desirability bias may have led to underreporting of alcohol use or partner violence, particularly among young mothers in rural communities. These findings highlight that while alcohol consumption and partner violence are recognised risk factors in the literature, their impact may vary across populations and contexts, emphasising the need to examine predictors of PPD within specific settings.
However, the study is not without limitations. The cross-sectional design limits the ability to establish causal relationships between predictors and PPD symptoms. Some variables had categories with relatively few observations, which may reduce statistical power. The secondary dataset did not include detailed psychosocial variables such as birth-related trauma, quality of family support, mother–child interaction, or experiences of obstetric violence. These factors are known to influence postpartum mental health and could provide a more nuanced understanding of the experiences of young mothers (Bay & Sayiner, 2021; Martinez-Vázquez et al., 2022; Taylor et al., 2022). Future primary research should aim to collect such data to better capture the complex psychosocial context of pregnancy and early motherhood in South Africa. The survey did not distinguish between live births and stillbirths. As a result, our analysis included all participants who reported having given birth within the past 12 months, regardless of infant outcome. Future studies should differentiate between live and stillbirths, as maternal mental health experiences may differ depending on birth outcomes. In line with epidemiological studies on PPD, our sample included participants who had given birth within the past 12 months; however, this timeframe extends beyond the DSM-5 definition of peripartum onset (within 4 weeks after delivery). As such, the prevalence estimates in this study may capture a wider spectrum of depressive symptoms experienced across the first postpartum year. The reliance on self-reported measures, such as the EPDS, may introduce recall or social desirability bias. Due to the small number of observations available in the secondary dataset, some variables included in the analysis had small cell counts (employment status, educational level, and smoking), which meant that the chi-square assumption of expected frequencies of at least five was not met. As a result, the chi-square findings for these variables should be interpreted with caution, as statistical reliability may be reduced. Finally, the study’s focus on a rural population in Limpopo Province may limit the generalisability of findings to other regions or urban settings with different socio-economic and cultural contexts.
Conclusion
The study examined the predictors of PPD symptoms among young mothers in rural Limpopo, South Africa. This study highlights that food security, HIV status, financial support from partners, and pregnancy planning were associated with PPD symptoms among young mothers in rural South Africa. Young mothers from food-insecure households and those living with HIV are at a higher risk of experiencing PPD symptoms while receiving financial support from partners and having planned pregnancies reduces this risk. Support services, including mental health care, should be integrated into HIV management programmes. Also, routine screenings for PPD during the mother’s first 6 and 10 weeks after giving birth can be done when they are taking their babies for the 6- and 10-week immunisation to help identify young mothers who require help or treatment. Programmes such as the Perinatal Mental Health Project (PMHP) at the University of Cape Town provide a useful model for integrating mental health care into routine antenatal and postnatal services. Incorporating similar approaches in primary health care facilities in Limpopo could ensure early detection and support for young mothers at risk of postpartum depression. We recommend longitudinal studies to establish causal relationships between food security, HIV status, and PPD symptoms among young mothers. Other studies could examine the intersection of partner support and broader family support in mitigating PPD among this vulnerable group.
Footnotes
Appendix 1
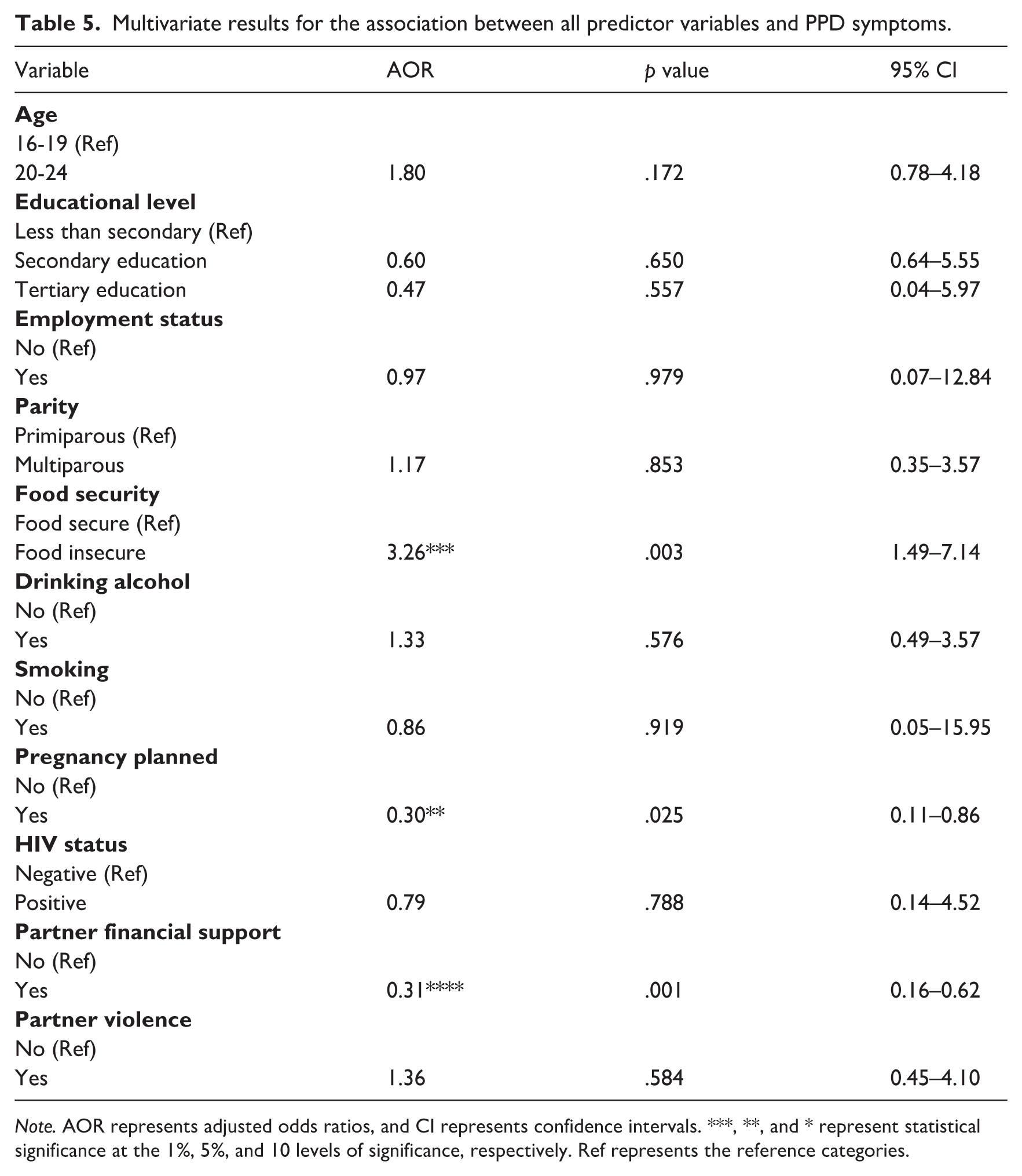
Multivariate results for the association between all predictor variables and PPD symptoms.
| Variable | AOR | p value | 95% CI |
|---|---|---|---|
|
|
|||
| 16-19 (Ref) | |||
| 20-24 | 1.80 | .172 | 0.78–4.18 |
|
|
|||
| Less than secondary (Ref) | |||
| Secondary education | 0.60 | .650 | 0.64–5.55 |
| Tertiary education | 0.47 | .557 | 0.04–5.97 |
|
|
|||
| No (Ref) | |||
| Yes | 0.97 | .979 | 0.07–12.84 |
|
|
|||
| Primiparous (Ref) | |||
| Multiparous | 1.17 | .853 | 0.35–3.57 |
|
|
|||
| Food secure (Ref) | |||
| Food insecure | 3.26*** | .003 | 1.49–7.14 |
|
|
|||
| No (Ref) | |||
| Yes | 1.33 | .576 | 0.49–3.57 |
|
|
|||
| No (Ref) | |||
| Yes | 0.86 | .919 | 0.05–15.95 |
|
|
|||
| No (Ref) | |||
| Yes | 0.30** | .025 | 0.11–0.86 |
|
|
|||
| Negative (Ref) | |||
| Positive | 0.79 | .788 | 0.14–4.52 |
|
|
|||
| No (Ref) | |||
| Yes | 0.31**** | .001 | 0.16–0.62 |
|
|
|||
| No (Ref) | |||
| Yes | 1.36 | .584 | 0.45–4.10 |
Note. AOR represents adjusted odds ratios, and CI represents confidence intervals. ***, **, and * represent statistical significance at the 1%, 5%, and 10 levels of significance, respectively. Ref represents the reference categories.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is based on the research supported by the South African Medical Research Council (SAMRC) and National Research Foundation (NRF) of South Africa (Grant Number: 150571).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
