Abstract
Obsessive-compulsive disorder (OCD) is a chronic and impairing mental health condition that often begins in adolescence. OCD remains underdiagnosed and undertreated particularly in low-and middle-income countries where access to specialist mental health care is limited. Few qualitative studies have explored the lived experiences of adolescents with OCD, and none have incorporated both adolescent and parent perspectives, nor considered the additional impact of the COVID-19 pandemic. We sought to address this gap. Participants were South African adolescents (aged 12–18) living with OCD, and their parents. Eight adolescent-parent pairs participated in semi-structured, individual online interviews conducted between August 2022 and February 2023. Adolescents also completed the Children’s Florida Obsessive-Compulsive Inventory (C-FOCI). Interviews were transcribed and analysed using reflexive thematic analysis and ATLAS.ti. Five themes provided insight into participants’ subjective experiences: (1) Recognising and naming OCD, (2) impact on functioning, (3) influence on family and home life, (4) impact on social life, and (5) impact on school life. OCD symptoms were often hidden and misunderstood, leading to delayed help-seeking. Adolescents described significant disruptions to sleep, social interactions, and schoolwork. Mothers highlighted emotional and physical strain, family conflict, and limited support. The COVID-19 pandemic intensified symptoms for some while providing temporary relief from school-related stress and social demands for others. The study underscores the complex, multi-layered impact of OCD on adolescents and their families, exacerbated by the COVID-19 pandemic. Findings suggest the need for accessible, family-focused psychoeducation, early detection of OCD, and school-based mental health initiatives to reduce stigma and promote support.
Keywords
Introduction
Obsessive-compulsive disorder (OCD) is a chronic neuropsychiatric disorder characterised by recurrent, intrusive thoughts (obsessions) and/or repetitive behaviours or mental acts (compulsions) (American Psychiatric Association, 2013). Globally, OCD affects about 0.5%–3% of the population (Kessler et al., 2005; Stein et al., 2019) and among children is observed more frequently in boys than girls (Geller, 2006), but more common among adolescent and adult females (Mathes et al., 2019). In South Africa, the prevalence of OCD is still unknown, but similar rates (1.7%) are reported among secondary school students (n = 1090) in Nigeria (Adewuya et al., 2007). OCD typically begins in late adolescence or early adulthood (Heyman et al., 2001) and is significantly debilitating, impairing all aspects of daily functioning, and overall quality of life (QOL) (Piacentini et al., 2003; Valderhaug & Ivarsson, 2005).
OCD also impacts on the lives of relatives of those with OCD across numerous domains of functioning (Futh et al., 2012; Piacentini et al., 2003). For example, parents often engage and actively participate in their child’s OCD-related rituals (known as family accommodation), providing constant reassurance or modifying family routines, thereby maintaining the condition. Family accommodation further promotes tension between family members, family dysfunction and a lack of cohesion (Chessell et al., 2023; Lawrence et al., 2021).
Keyes et al. (2018) were the first to publish a qualitative study capturing the lived experiences of young people with OCD from their own perspectives. A forward citation search of this paper identified only two additional studies that specifically report adolescents’ perspectives of OCD (Sravanti et al., 2022, 2024). To our knowledge, this means that only three qualitative studies to date have centred the voices of children and adolescents (ranging in age from approximately 10 to 17 years) on their own experiences of living with OCD. In the first example, the research took place in the United Kingdom and involved a sample of 10 adolescents aged 14–17 with OCD. The findings revealed that OCD had a significant impact on participants’ academic performance, with time-consuming rituals interfering with their ability to complete schoolwork. In addition, their social lives were negatively affected, as feelings of shame and difference led to secrecy and social withdrawal (Keyes et al., 2018). In the second study, conducted in India, researchers explored the experiences of 10 young people aged 10–17 living with OCD. The results similarly highlighted the detrimental effects of OCD on academic functioning and peer relationships. Participants reported disruptions in their sense of self, school performance, and social standing, with several describing experiences of bullying and misunderstanding by peers (Sravanti et al., 2022). A follow-up study in 2024 further examined the barriers and facilitators to recovery in Indian children and adolescents (10–17 years) with OCD. This study emphasised internal barriers such as lack of awareness and perceived stigma, as well as external barriers including limited parental support, inadequate awareness in schools, and cultural myths about mental illness. Facilitators included supportive family members, positive therapeutic relationships, and improved mental health literacy (Sravanti et al., 2024). One additional qualitative paper published in 2016 explored adolescents’ (12–17 years) experiences of undergoing internet-delivered Cognitive Behaviour Therapy (ICBT) for OCD, including their positive and negative impressions, views on the treatment process, and perceptions of its usefulness. Participants also reflected on unmet expectations and offered suggestions for improving the programme. In South Africa, there are only two studies that have explored the lived experiences of OCD, and these have been explored in adults (Hathorn et al., 2022; Kohler et al., 2018). Across both studies, participants described major disruptions to daily life and a difficult, nonlinear process of recognising symptoms and seeking help. They also highlighted reduced quality of life and the value of supportive relationships. Studies that have included parent perspectives on OCD in adolescents are mostly quantitative in nature, and these report a discrepancy between the ways in which parents and their children report on the impact of OCD on home, social and school life (du Plessis et al., 2022; Piacentini et al., 2003; Valderhaug & Ivarsson, 2005). For example, in their South African study du Plessis et al. (2022) showed that among 26 adolescents with OCD (Mean age: 13.54 years), children reported the greatest OCD-related impairment in the school domain, while parents highlighted social difficulties. Furthermore, parent scores aligned more closely with clinician ratings and symptom severity than child self-reports. Parents are key role players in adolescent mental health help-seeking and treatment experiences. Hence, exploring adolescents’ experiences of OCD alongside parent narratives addresses an important research gap, and may inform clinical practice.
Given that this study was conducted in 2022–2023, during a period when the impact of the COVID-19 pandemic and lockdown measures were still profoundly felt we also sought to explore how the pandemic and its associated restrictions impacted adolescents living with OCD. Available research about COVID-19 and OCD among adolescents is quantitative in nature and findings are mixed. Some studies reported increased OCD severity during the pandemic (Kroon et al., 2022; Nissen et al., 2020), particularly highlighting exacerbations of contamination-related obsessions and cleaning compulsions (Tanir et al., 2020). Whereas others reported no significant worsening (Schwartz-Lifshitz et al., 2021).
Our review of the literature demonstrated that there is very little qualitative research that documents how adolescents understand and experience OCD and no qualitative work that explores how parent and adolescent accounts relate to or differ from one another. Furthermore, no South African study has captured adolescent experiences of OCD, and no qualitative studies to date have explored the influence of the COVID-19 pandemic on OCD experiences among adolescents with OCD and their parents. These gaps limit our ability to design developmentally and contextually appropriate interventions. South Africa is an upper-middle-income country within sub-Saharan Africa and faces substantial inequalities that shape knowledge of mental health conditions and access to mental health care. The country carries a high burden of unmet mental health needs (Herman et al., 2009), particularly among adolescents (Bantjes et al., 2025). Socio-political, structural and contextual factors likely influence how mental health is experienced by adolescents and supported by their parents in everyday life, and this study provides some initial insights into these experiences across various domains of life. Despite a new National Mental Health Policy Framework and Strategic Plan (2023–2030) (Department of Health, 2023), implementation remains poor, mostly due to limited or no budget allocations by provincial Departments of Health (Sorsdahl et al., 2023).
To address the gaps in the literature and utilising both parent and adolescent narratives our guiding research question was: How do South African adolescents aged 12 to 18 experience living with OCD, and how do they and their parents describe the influence of COVID-19 on these experiences across school, peer, and family settings?
Methods
Research design
We used an exploratory qualitative design within the interpretivist paradigm to explore the lived experiences of adolescents with OCD and their parents. This approach prioritises subjective meaning, allowing insight into how OCD affects various aspects of adolescents’ lives (Bryman, 2012; Silverman, 2020). A qualitative design was necessary because the study focused on subjective experiences that cannot be captured through structured measures alone. A brief quantitative component was included which consisted of measuring OCD symptom severity using the Children’s Florida Obsessive-Compulsive Inventory (C-FOCI). These data were used to better understand symptom severity among our adolescent participants, but answering the research question required an in-depth interpretivist approach.
Participants and procedures
We used purposive sampling to recruit adolescents with OCD and their parents. Purposive sampling is widely used in qualitative research because it helps identify participants who can offer detailed and meaningful accounts of the topic under investigation (Palinkas et al., 2015). This approach allowed us to intentionally select adolescents with lived experience of OCD and their parents who were well placed to contribute rich and relevant insights. To be eligible for this study participants had to be adolescents (12–18 years) with a formal OCD diagnosis, with or without comorbidities (excluding psychosis). Parents had to have a child with OCD between 12 and 18 years old. Recruitment occurred between August 2022 and February 2023. During this time, participants were recruited through several pathways to ensure a suitable sample size. Recruitment took place via clinical psychologists who work with adolescents with OCD, online mental health support groups, and a radio interview on Cape Talk. This process yielded seven adolescent-parent pairs, one adolescent whose parent declined to participate, and one parent whose adolescent did not participate, resulting in a total of 16 interviews. This number was appropriate for the aims of our exploratory qualitative study and was guided by the principle of information power. According to Malterud and colleagues (2016), when a study has a clearly focused aim, a relatively specific sample, strong interview dialogue, and an analytic approach that seeks thematic patterns across cases, a smaller sample can hold sufficient information to meaningfully answer the research question.
Interview schedules were semi-structured and grounded in the study’s aims and existing literature. Adolescent interviews explored the onset and diagnosis of OCD, its impact on daily life, school, family, and peer relationships, and how the COVID-19 pandemic influenced symptoms, routines, and access to support. Parent interviews explored when they first noticed symptoms, how OCD affected their child’s daily functioning, their approaches to managing compulsions, and the impact of the pandemic on home life, schooling, and social interactions. Participants also completed a demographic form and the C-FOCI to assess symptom severity (Sandoval-Lentisco et al., 2023; Storch et al., 2009). The measure has not been used or validated in South Africa.
Data analysis
Interviews were audio recorded (with permission from participants), conducted in either English or Afrikaans, transcribed verbatim and translated into English where needed. We used the six-step approach of Reflexive Thematic Analysis (RTA) to identify patterns of shared meaning across the dataset (Braun & Clarke, 2021), using ATLAS.ti. The data analysis was led by the researcher, with support from a supervisor and co-supervisor. Multiple strategies were used to ensure the trustworthiness of our research, focusing on credibility, transferability, dependability, and confirmability. Credibility was enhanced through member checking (checking interpretations with participants during interviews) and investigator triangulation, ensuring accurate interpretation of participants’ accounts. Transferability was addressed by gathering rich, detailed descriptions of participants’ experiences to make findings applicable to similar contexts, while dependability was ensured by providing clear, detailed documentation of the research process for potential replication. Confirmability was achieved by embedding direct quotes from participants to support findings, and linking findings to existing literature(Ahmed, 2024). Quantitative data (demographics and C-FOCI scores) were analysed using descriptive statistics (mean, standard deviation (SD), sum of scores for the C-FOCI, counts and percentages) in excel.
Ethical considerations
This study received ethics approval from Stellenbosch University’s Research Ethics Committee: Social Behavioural and Education Research (REC: SBE) (Approval reference number: 25076; 19 May 2022). Written informed consent and assent were appropriately obtained from all the participants and their parents. All gave written permission for publication in a peer-reviewed scientific journal. We protected the confidentiality of participants by ensuring that the interviews were conducted online an in a space that participants deemed safe and secure. We also ensured that the data were only shared among the authors included on this paper and that pseudonyms used in this paper to protect participants’ identities.
Findings
Participant characteristics
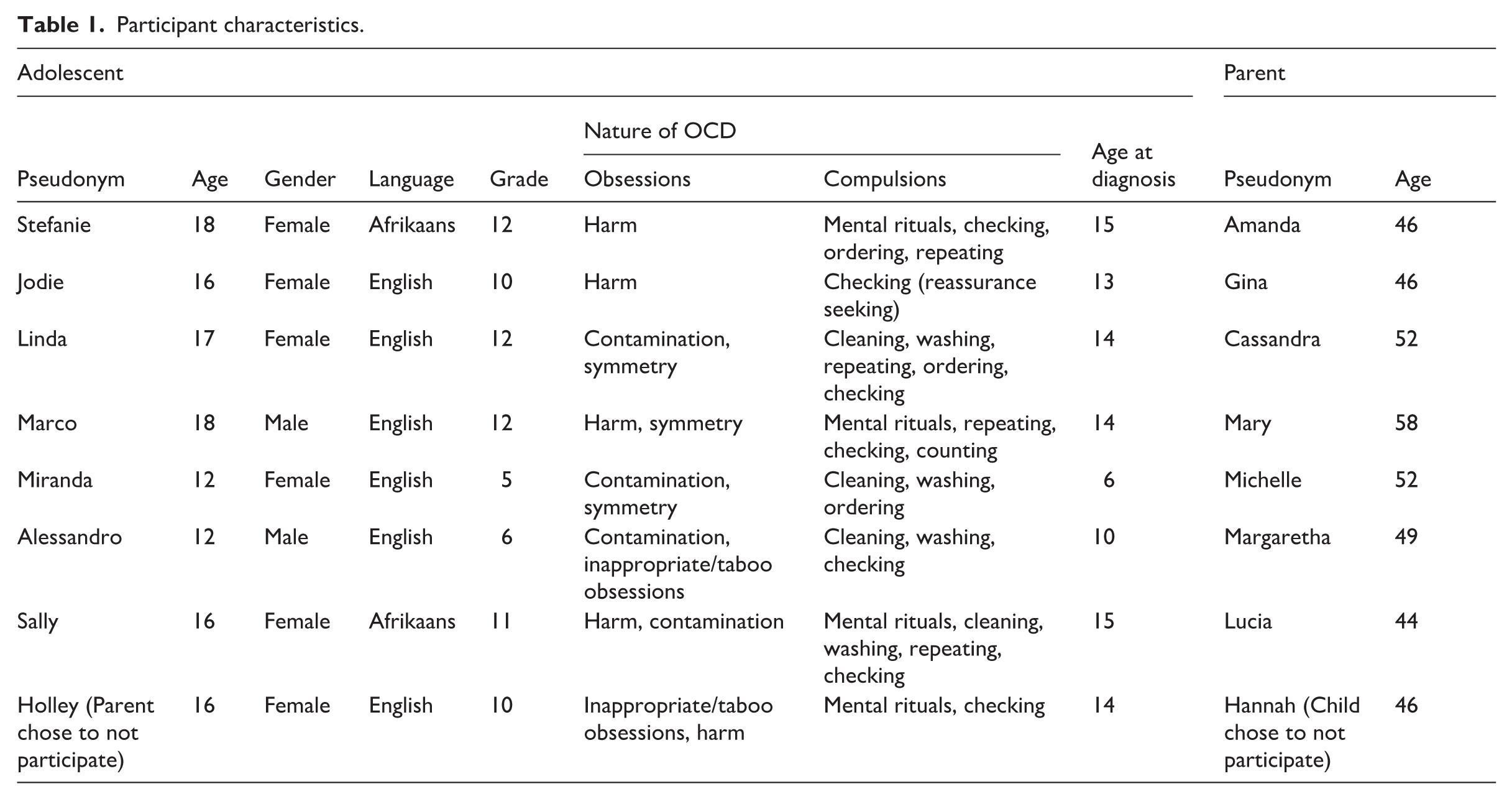
Eight adolescents (6 females and 2 males) and 8 mothers took part in the study (see Table 1). Adolescent participants were on average 15 years old (M = 15.63, SD = 2.387). Mean age of onset of OCD was 9.63 years. Most participants (N = 3; 37.5%) reported being diagnosed with OCD at the age of 14 years. The time since diagnosis varied among participants, ranging from one to six years. All participants attended school with three being in their last year of school (Grade 12). C-FOCI total scores ranged from 5 to 13 (M = 9.25, SD = 2.86), indicating moderate severity of OCD symptoms over the past month. Mothers’ ages ranged between 44 and 58 years (I = 49.12, SD = 4.64). Most of the participants came from suburban neighbourhoods (N = 12; 75.0%), and all had a family income of at least ZAR15 000 per month (~650GBP) and above.
Participant characteristics.
Themes and sub-themes
We identified five themes relevant to this study. Pseudonyms are used to protect participant identities throughout.
Theme 1: recognising and naming OCD
This theme explores how adolescents came to recognise and label their diagnosis. The process was initially marked by secrecy, confusion, and shame, followed by gradual disclosure and eventual diagnosis. Recognising OCD was a deeply emotional process, often compounded by distressing internal experiences shaping how young people perceived themselves and their symptoms.
Hiddenness of OCD
Mothers reported that they initially failed to notice that anything was wrong, as adolescent rituals were conducted in private. Amanda (46), mother to Stefanie (18), explained:
The actions that she was repeating and things like that was not things that were visible to us. It was more like her bedtime routine [. . .] having to do things in a certain order but I mean that’s done in private. It’s not something that we actually noticed.
Adolescents described feeling confused and ashamed about what they were experiencing, which led them to conceal their symptoms. As Holley (16) explained:
I thought I was a problem. I was fourteen. It [OCD] gradually in the two years became unliveable. At first when I was twelve, I was the only one who knew about it. I didn’t talk about it.
For many, the internal experience of OCD was not only isolating but also distressing. Sally (16) described a ‘constant feeling of. . . out of body’, and a sense of having no control over her thoughts or identity. This disconnection and confusion often contributed to self-stigma and emotional suffering. Some participants also reported intrusive sexual and harm-related thoughts, which were especially difficult to cope with and contributed to secrecy and deep feelings of guilt and shame. As Margaretha (49) shared about her son (Alessandro, 12):
. . .definitely sexual thoughts for sure and that’s what bothers him the most. . .that’s what makes him feel so horrible. Because he feels bad about the thoughts that he has that he doesn’t understand properly and that he thinks, in his book, are totally inappropriate to have at his age. . . that’s when the anger comes out. When there’s the guilt.
Disclosing symptoms to others
Due to the profound shame and fear associated with their experiences, adolescents struggled to openly discuss their symptoms. They worried they would be judged or misunderstood. Sally (16) wanted to disclose her struggles to her parents but was uncertain about how to approach them. Instead, she initially sought guidance and support from her school counsellor:
I approached our school counsellor and asked her for advice on how to approach my parents, and she said that she would call my parents herself. So, I did take the first step, but my counsellor was the person who told my parents that I might need help. . . I didn’t know how to bring it up to them and I was hoping the counsellor could give me advice.
Getting diagnosed with OCD
All adolescents eventually sought professional help for their symptoms, with many expressing mixed emotions about being diagnosed with OCD. While some felt relief, most initially struggled with feelings of grief, helplessness, and confusion. Both adolescents and their parents commonly lacked knowledge about OCD at the time of diagnosis, making it difficult to fully grasp what it meant or how to respond. For example, Stefanie (18) stated:
At first when I was diagnosed, I didn’t actually understand OCD. I was like completely unfamiliar with the whole idea because I mean I was 14/15 years old. I just didn’t know about mental illness. I didn’t know about OCD.
Similarly, Stefanie’s mother Amanda (46) stated:
She didn’t really understand exactly what it was, and we didn’t either. So, I wasn’t really capable of asking the right questions or trying to assist because I also didn’t really know the extent of it.
Access to appropriate services complicated the journey to diagnosis. Several mothers faced challenges in finding professionals specialising in OCD, and when they did, they desired greater involvement and education throughout the diagnostic process. Hannah (46) explained:
I really struggled to find a psychologist and a psychiatrist that really understands or knows how to handle him and, you know, the particular nuances of his situation . . . what we’ve discovered is that there is very few people who specialise in OCD in South Africa, um, you know, therapists and psychiatrists. And so, yeah, it did feel like we went round and round quite a lot. Um, and sort of a lack of definitive diagnoses. . . so it has taken a while, you know, for us to really get a proper diagnosis.
The process of diagnosis also raised concerns for mothers, some of whom felt unprepared to support their child. A few, like Cassandra (52), concealed the diagnosis to protect their child from stigma:
I try to protect her as a mother. . . I’ve never spoken to people about it. Not even my own family or my own siblings, because I don’t want them to see her and say, ‘oh, yeah, she’s carrying on like that because she’s got that’. I don’t want people to do that to her. So, I just keep it all to myself.
Theme 2: impact on functioning
This theme explores how OCD disrupted adolescents’ everyday functioning, including sleep, routine activities, and leisure, often contributing to their distress and social withdrawal. It also highlights how the COVID-19 pandemic amplified or, in some cases, temporarily eased these disruptions, depending on the individual’s circumstances.
Interference with sleep and bedtime routine
Adolescents reported how OCD interfered with their sleep, particularly preparing for bedtime, difficulty falling asleep due to disruptive thoughts and needing to constantly get up to perform OCD rituals, resulting in poor sleep quality. Participants reported that their sleep difficulties intensified following the onset of the COVID-19 pandemic, which in turn heightened bedtime OCD compulsions. Many reported feeling that if they failed to complete their rituals, their family members could contract the virus. For instance, Sally (16) said:
I think the biggest fear was that my family would catch it (COVID-19), and that something bad would happen to them. I think my OCD had just skyrocketed cause every night it was like, ‘Okay, I’m going to sleep. If I don’t say no this number of times. If I don’t walk on this many tiles, something is going to happen’. It was very bad. Some nights I couldn’t sleep, and if I did sleep, I had nightmares.
Interference with activities of daily living
Mothers and adolescents described how OCD interfered with everyday activities like cooking, eating, cleaning, and dressing for school. Several participants expressed uncertainty about whether COVID-19 directly influenced their OCD symptoms. Others reported that the pandemic worsened specific symptoms, such as contamination fears and compulsive cleaning. Conversely, some participants reported that the pandemic had a positive impact by offering the comfort of staying home, enabling avoidance of anxiety-provoking situations, and providing time for reflection and symptom management. Holley (16) said:
I’m going to say that I started my OCD/ depression before COVID-19 and people want to blame– people sometimes put the blame that I got worse on COVID, which I think that’s not true. It was going to happen either way, and staying home made it easier than going to school.
Interference with leisure activities
Adolescents reported that OCD severely disrupted their ability to engage in and enjoy their usual leisure activities and hobbies as these triggered OCD compulsions and obsessions. Marco (18) stated:
If I were, for example, putting on shoes to go for a run then I would have to kind of tie my shoelaces with a certain thought – the correct kind of feeling and everything. And if I didn’t get that right then I would do it over and over and over again.
Theme 3: impact on home and family
This theme explores the wide-ranging effects of OCD on family dynamics, caregiver well-being, and household functioning. While adolescents often underestimated the impact of their symptoms at home, mothers described emotional exhaustion, disrupted routines, and strained relationships.
Differing perceptions of family impact
Mothers reported that OCD in their child affected the entire family. In contrast, adolescents’ opinions about the impact of their OCD on family and home life were mixed with some reporting no influence, whereas others admitted significant impact. For example, Alessandro (12) stated that his OCD did not interfere with family functioning:
I don’t think it has affected my family life really, yeah. I think it just makes me, I get, oh, no it doesn’t really affect my family life, no.
In contrast, his mother, Margaretha (49), describes the challenging nature of having a child with OCD and its negative impact on her well-being:
He needs constant reassurance with everything as well as knowing that everything is going to be okay. It’s constant. So it’s exhausting. It’s draining! And when he has these thoughts that are darker than the ones he’d like to have or inappropriate, then it comes out as rage and anger that will usually be towards me because I’m the punching bag.
Disruption of family dynamics
Some participants recounted that OCD severely disrupted family dynamics, leading to increased conflict, distress, irritability, division and tension among family members. Especially during the COVID-19 lockdown, families spent more time together due to home confinement, which had mixed impact on family and home life. Some participants experienced improved communication and stronger family bonds and others reported heightened tension, conflict, and emotional outbursts. Marco (18) said:
I would say that it (the COVID-19 pandemic) brought us closer together, you know, we would obviously be spending a lot more time with each other. So, positively, it didn’t make anything more difficult, and the fact that I was sort of, you know, coming out (of) the rut I was in regard to OCD, um, made things easier as well.
Mothers, in particular, described the COVID-19 and lockdown periods as stressful, with some witnessing severe behavioural challenges in their children, including aggression and emotional distress related to OCD and depressed mood. Hannah (46), said:
He was so angry and like his temper was just really, really hectic. I mean that was the phase where it was just so scary because he was hitting me and breaking things and suicidal and – yeah, it was just really, really bad.
Impact on Caregiver
Mothers reported that their child’s OCD impacted on their mental and physical health, leading to physical or emotional exhaustion, grief, feelings of helplessness, depression, and anxiety. Mary (58) said:
I used to watch him and cry. It was terrible. It was so frustrating because you know what has to happen, but you cannot make it happen. That was the thing! There was nothing I could do to help you. . . You feel so helpless! You know, it’s like if your child is physically ill you know that you can help them, but with this, you just can’t do anything.
This led caregivers to try setting boundaries, a task that was particularly challenging. Some mothers feared that refusing to allow rituals would escalate conflict. Hannah (46), explained:
It’s like I haven’t really set good boundaries and I’ve kind of allowed myself to kind of be a co-conspirator in his rituals but just because it’s like so hard. I mean if I say no, it just escalates into an absolute nightmare really fast’.
Theme 4: impact on social life
This theme explores how OCD shaped adolescents’ social lives, often leading to withdrawal, isolation, and challenges in forming or maintaining relationships. It also highlights discrepancies between adolescent and mothers’ perceptions of social impact, as well as the varied influence of the COVID-19 pandemic on peer interactions and connectedness.
Social withdrawal
Adolescents with OCD often withdrew socially due to fears of stigma, acting on intrusive thoughts, or contamination, leading to isolation, difficulty maintaining friendships, and reduced self-esteem. While some mothers underestimated these social impacts, young people described feeling misunderstood and disconnected. For example, Stefanie (18) stated:
I distanced myself from people because I was scared they’d find out what a ‘monster’ I am. You know, because I thought badly about myself. I was so scared other people would see or know that was going on inside my head.
Mixed impact of COVID-19
As noted earlier, the COVID-19 pandemic had mixed effects. Some felt it worsened their isolation and symptoms, while others noted no significant change, attributing social challenges more to OCD itself than to the pandemic. Marco (18) said:
I don’t think that the fact that I had OCD, um, during the pandemic affected my relationships at all. I think just being in the pandemic affected it, you know, the fact that there was a lockdown, but I don’t think that it was different from other people who didn’t have OCD.
Michelle, mom to Miranda (12) said:
I don’t think it really made any much difference to her socialisation because at that stage when COVID did hit she was quite, um, she was not really the most social child. . . If there was COVID or no COVID it wouldn’t have made much of a difference.
Theme 5: impact on school life
This theme explores how OCD disrupted adolescents’ school experiences. Participants described struggles with attendance, concentration, and academic performance, compounded by anxiety, rituals, and a lack of understanding from peers and teachers. The shift to online learning during COVID-19 provided some relief but often worsened focus and productivity. Returning to school, however, intensified symptoms for many. Adolescents also reported experiencing bullying, social isolation, and feeling misunderstood, highlighting the need for greater awareness and support within schools.
Decline in school attendance and performance
Adolescents with OCD experienced significant challenges in attending and performing at school due to anxiety, distress, and time-consuming compulsions. Sally (16) said:
At some point, the OCD started to affect my mood a lot. I didn’t want to go to school because it would have physical symptoms, physical effects on my body. So, I would just get very, very sick, or cold, very numb at times because of the anxiety the OCD was causing me. And, um, I was always down at school. I could barely focus, and I just wanted to be home all the time.
Hannah (46), stated:
He wouldn’t be able to go to school quite a lot because it was just so hectic for him, um, it was just so intolerable being exposed to what he just felt was contamination everywhere. Often if he’s feeling very triggered or he’s got like things on his mind he won’t be able to work at school. He’ll often land up in the toilet crying, asking me to fetch him early.
While remote learning during the COVID-19 pandemic offered some respite from school-related stressors, it also led to reduced focus and productivity. For many, returning to in-person schooling was distressing further impacting their academic engagement. For example, Miranda (12) explained the impact of lockdown and COVID-19 on schoolwork:
I think yes because I didn’t actually have a time limit. . . so I could spend even more time perfecting my writing. . . I’d have the same amount of schoolwork, but it would just take much longer than if I was at school. It does take much longer. . . I would always get distracted with like my cat, and like my toys, and then after I would play with my toys I would spend more time putting it back.
Hannah (46) said:
[. . .] the first year was an absolute disaster because he just clocked out with online learning, so he just refused to participate. When he did go back for a few weeks, he was just so triggered. I mean, he was basically asked to leave because he was just so nasty to other kids there, but I think his new school is a lot more accepting and understanding of his challenges.
Social difficulties within school context
Adolescents with OCD often felt isolated and misunderstood at school, reporting bullying, few friends, and a lack of support from peers and teachers. Holley (16) stated:
I had no friends. I went to school and people would come to me and mock me [. . .] I guess I had like tics like (with) my head or doing things with my hands which people, um, made fun of me for that, which also didn’t help [. . .] I couldn’t do it anymore. It was just too much. Holley (16)
Mary (58), mom to Marco (18) expressed frustration at the schools’ limited awareness of OCD, contributing to socially isolating experiences for her child. She said:
They were shocking! They told us that Marco (pseudonym) was a disturbance to them and they are such a good, well-known, respected school they didn’t think he had a place there. I actually left. Got up and I just walked out of the meeting. I was crying and I couldn’t deal with it. They are one of [mentions place] best schools and they didn’t know how to deal with it.
Discussion
To our knowledge, this is the first qualitative exploration of the lived experiences of South African adolescents with OCD and their mothers, with an added layer of focus centred around the impact of COVID-19. Consistent with available literature our participants were female adolescents, and their biological mothers. Indeed, OCD is reported more commonly in adolescent and adult females (Mathes et al., 2019), and most of the research on adolescent experiences of mental health conditions, including OCD is reported by females and their mothers (Martin et al., 2025). As such, there is a notable gap in the literature regarding the perspectives of siblings, fathers, and other primary caregivers which warrants further exploration in future research.
Our findings echo several themes in the existing qualitative literature on adolescent OCD. For example, similar to the findings from the studies with adolescents in the United Kingdom (Keyes et al., 2018) and India (Sravanti et al., 2022), our study highlights the hidden nature of the condition, and delays in symptom recognition (Keyes et al., 2018; Sravanti et al., 2022). Furthermore, adolescents often experienced fear, shame, and isolation, viewing their symptoms as strange or shameful. Many kept symptoms secret, and when they did disclose, it was usually after significant distress. Like earlier studies, our findings emphasise adolescents’ reliance on caregivers for recognising mental health problems and facilitating help-seeking (Radez et al., 2022). However, mothers often lacked awareness of OCD symptoms and struggled to distinguish them from typical behaviour, likely due to limited mental health literacy and stigma. Even after diagnosis, some mothers reported receiving insufficient guidance from clinicians, mirroring findings from Sravanti et al. (2024). This lack of support undermined their ability to help their children effectively. Stigma remained a barrier to help-seeking for both adolescents and mothers (Belloch et al., 2009; García-Soriano et al., 2014). Family-focused psychoeducation may help reduce stigma, support early recognition, and enable timely intervention. Our study also revealed differing perceptions between adolescents and mothers regarding the life domains most impacted by OCD. Similar to the findings of a recent systematic review of parent experiences of a child with a mental health condition including OCD (Martin et al., 2025), mothers in our study emphasised family conflict, tension, and stress due to their involvement in compulsive rituals. Adolescents in our study, however, focused more on the influence of their OCD at school and in social relationships. As such, adolescents did not seem to recognise the toll their OCD took on their family relationships. This lack of insight, which in part may be developmental, could be an important focus for future interventions. Family accommodation, such as participating in rituals, was a major source of strain for mothers and has been shown to worsen symptoms and family functioning (Lebowitz et al., 2012; Stewart et al., 2017). At school, and in keeping with the available literature adolescents faced academic challenges as well as bullying, peer victimisation, and misunderstanding by teachers and peers (Keyes et al., 2018; Sravanti et al., 2022). School-based mental health awareness and support, which at present is limited in the South African context is an important focus of future research. Mothers expressed a strong desire to be more involved in their children’s treatment. While evidence for the effectiveness of parental involvement in therapy is mixed (Lawrence et al., 2021), it may enhance support at home and reduce unhelpful accommodations. Finally, the study highlighted the diverse impact of the COVID-19 pandemic on adolescents with OCD. For some, contamination fears worsened, while others found relief in the lockdown’s structure and reduced social demands, echoing other findings in the literature (Schwartz-Lifshitz et al., 2021; Tomczak et al., 2023).
Limitations
This study has several important limitations. The sample was drawn largely from middle- to high-income families who reported monthly household income levels of R15 000 and above, which is a broad bracket encompassing very different socioeconomic circumstances. In addition, all adolescents had already received a confirmed OCD diagnosis. As such, our findings reflect the experiences of a relatively small, distinct subset of families within the South African context, where access to specialist child and adolescent mental health services is highly unequal and higher-level public and private psychiatric care is disproportionately accessed by more socioeconomically advantaged families (Ataguba & McIntyre, 2013). All interviews were conducted online, which may have affected rapport and the depth of disclosure for some participants, particularly adolescents who may feel more comfortable engaging in person. Furthermore, we did not examine how digital access shaped who was able to participate. Because our recruitment and data collection relied on stable internet connectivity and familiarity with online platforms, adolescents and caregivers with limited digital access may have been unintentionally excluded. We also did not collect data on race or ethnicity, which limits our ability to consider how structural histories, cultural meanings, and racialised inequalities may shape young people’s experiences of OCD. Future research should include participants across diverse racial, cultural, linguistic, and socioeconomic backgrounds, including adolescents who have not yet accessed treatment. Future research is also needed to explore early help-seeking processes and the role of cultural beliefs about mental health, and to include the perspectives of fathers and other primary caregivers, as well as siblings, teachers, and peers. Future research is also needed to better understand how broader environmental and contextual factors, such as climate change, shape adolescents’ experiences of OCD.
Conclusion
This study provides important insights into the lived experiences of South African adolescents with OCD and their mothers, highlighting the multifaceted impact of the disorder on individual functioning, family dynamics, peer relationships, and school engagement. The findings underscore the importance of improving mental health literacy among caregivers, teachers, and health professionals to support earlier recognition and intervention.
Footnotes
Acknowledgements
We are grateful to all participants who contributed to this research. Aspects of the manuscript have previously appeared online, in a master’s degree thesis of author KP, with BC and CL as her study supervisors.
Ethical considerations
This study received ethics approval from Stellenbosch University’s Research Ethics Committee: Social Behavioural and Education Research (REC: SBE) (Approval reference number: 25076; 19 May 2022).
Consent to participate
Written informed consent and assent were appropriately obtained from all the participants and their parents. All gave written permission for publication in a peer-reviewed scientific journal.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Our ethics permission does not permit the data to be openly available but can be requested from the corresponding author upon reasonable request.
