Abstract
Although South Africa has high rates of child and adolescent trauma exposure and associated mental health difficulties, there is a poor evidence base for trauma interventions with youth in this setting. In a resource-constrained context, there is a need for brief evidence-based trauma treatments. However, abbreviated interventions may reduce the acceptability and tolerability of treatment for clients and impact treatment delivery by providers. We developed an abbreviated eight-session version of trauma-focused cognitive behavioural therapy. Using a sequential mixed-methods design, we piloted this intervention with 10 adolescents and their caregivers to assess the acceptability and tolerability of the abbreviated trauma-focused cognitive behavioural therapy model for participants, the degree of counsellor fidelity to the abbreviated treatment manual and counsellor experiences of implementation. The treatment completion rate was 90% and post-traumatic stress disorder symptoms reduced over the course of treatment for all treatment completers. Although there was flexibility in timing and dosing of delivery, counsellor fidelity to treatment components and treatment length was high. Thematic analysis of interviews with participants and counsellors indicated that, within this abbreviated trauma treatment, the therapeutic alliance was able to provide a solid foundation for trauma processing, there was adequate time to practice coping skills and the compressed trauma processing component was difficult but tolerable. Counsellors indicated that a degree of flexibility within fidelity to the abbreviated treatment model enhanced their implementation of the treatment. The findings provide evidence to support a formal evaluation of the abbreviated trauma-focused cognitive behavioural therapy treatment protocol.
South Africa has high levels of child maltreatment (Ward et al., 2018) and community violence (Foster & Brooks-Gunn, 2015). The majority of South African youth experience multiple forms of violence during their development (Richter et al., 2018), with polyvictimisation rates exceeding those reported in both high-income countries (HICs; Finkelhor et al., 2007) and other low- and middle-income countries (LMICs; Le et al., 2016). Trauma exposure creates a high risk for post-traumatic stress disorder (PTSD) among South African youth, and the odds for this disorder increase with higher levels of exposure (Stansfeld et al., 2017). There is therefore an urgent need for child and adolescent mental health services (CAMHS) in South Africa to provide effective interventions targeting PTSD.
However, ongoing trauma exposure both during and after treatment can compromise the effectiveness of trauma interventions in the South African context. It may therefore be necessary for treatment to include coping and safety strategies to enhance young people’s resilience to ongoingly violent environments. In addition, high rates of poverty and unemployment in South Africa create a context of multiple family adversity that can compromise parenting capacities (Lakind & Atkins, 2018), in turn hindering young people’s recovery from traumatic events (Williamson et al., 2017). Furthermore, local CAMHS are scarce and under-resourced (Mokitimi et al., 2018). There is therefore a critical need to develop trauma interventions that are brief enough to be implemented in an over-burdened CAMHS, yet robust enough to effectively address traumatic stress in a context of ongoing violence and adversity. Unfortunately, the evidence base for youth trauma treatments in South Africa is poor. Only one randomised controlled trial (RCT) has been conducted to date, which found that prolonged exposure therapy (previously mainly used with adults in HICs) was more effective than supportive counselling in reducing PTSD symptoms among high school learners in Cape Town (Rossouw et al., 2018). While this is encouraging, there is as yet no local evidence for other youth trauma interventions.
Trauma-focused cognitive behavioural therapy
In systematic reviews, trauma-focused cognitive behavioural therapy (TF-CBT; Cohen et al., 2006) is consistently identified as the first-line treatment for PTSD in children and adolescents, with the strongest RCT evidence base (Bennett et al., 2021; Mavranezouli et al., 2020). TF-CBT is a conjoint intervention that includes the child/adolescent and a caregiver. The counsellor spends 45 min with each, except for one session that is conducted conjointly if this is judged by the counsellor to be appropriate. It is a phased intervention where psychoeducation affect regulation skills and cognitive coping skills are followed by reprocessing of traumatic memories through prolonged exposure (involving repeated retellings of the traumatic event in the safety of the therapeutic relationship) and reworking dysfunctional trauma-related beliefs (Cohen et al., 2006). It also includes a focus on safety planning to reduce risk of re-exposure to trauma. TF-CBT has been effective in treating children, younger, and older adolescents exposed to a variety of single as well as multiple traumas (Cary & Curtis McMillen, 2012; Murray et al., 2013). While most of the TF-CBT evidence-base comes from HICs, it has also been found to effectively treat PTSD in some LMICs (Dorsey et al., 2020; McMullen et al., 2013; Murray et al., 2015).
With parenting, coping and safety components that supplement trauma processing, and evidence to support its use in LMICs, TF-CBT could be well-suited to addressing the needs of South African youth. However, TF-CBT was developed as a 12–15-session intervention (Cohen et al., 2006), which is too long for scale up in the over-burdened South African CAMHS. Even when TF-CBT has been adapted for LMIC contexts, there has been little reduction in treatment length. For example, in African settings, TF-CBT has been implemented in 12 (Dorsey et al., 2020), 15 (McMullen et al., 2013), and an average of 11 (Murray et al., 2015) sessions. Although PTSD interventions have recently been abbreviated for treating adults in primary care settings in HICs (Rauch et al., 2020), similar initiatives to abbreviate existing youth PTSD interventions are lacking. There is, however, some evidence that TF-CBT can be successfully abbreviated while retaining all of its core components: an eight-session TF-CBT format was effective in reducing traumatic stress symptoms in children exposed to sexual abuse (Deblinger et al., 2011) and intimate partner violence (Cohen et al., 2011) in the United States. To date, this abbreviated format has not been evaluated outside the United States or with youth exposed to multiple, ongoing forms of violence.
While abbreviated youth trauma interventions can be more cost-effective, they may reduce the acceptability and tolerability of treatment for both clients and counsellors, as anxiety-provoking trauma memories must be processed in a compressed time frame. Tolerability of exposure-based PTSD treatment for youth is a concern even in standard-length treatment formats, with drop-out rates ranging from 20% to 77% (Eslinger et al., 2014; Wamser-Nanney, 2020). The acceptability and tolerability of abbreviated TF-CBT for young clients therefore needs to be established, particularly in contexts of ongoing danger and adversity. In doing so, it is important to include the voices of young clients through qualitative research (Neelakantan et al., 2019). This is particularly vital in the South African context, where youth have had little exposure to CBT interventions.
Research also indicates that many counsellors have concerns about implementing evidence-based treatments in general, and exposure-based PTSD treatments specifically, resulting in low fidelity to treatment protocols and reduced treatment effectiveness (Ascienzo et al., 2020). For example, a study of standard-length TF-CBT implementation in the United States found that only 66% of counsellors reported being likely to use all the treatment components (Allen & Johnson, 2015). Counsellor concerns include fear of increasing client distress through eliciting trauma narratives, lacking skills to reprocess trauma-related thoughts and feelings, and struggling with how to engage caregivers in the treatment (Ascienzo et al., 2020). Abbreviated PTSD treatments, where there is a compressed time frame for implementation, may increase these challenges to counsellor confidence and fidelity, potentially compromising treatment effectiveness.
Given these previous findings, we aimed to assess client and counsellor experiences of an abbreviated version of TF-CBT in the South African context.
Adapting the intervention
Through collaboration with researchers at Johns Hopkins Bloomberg School of Public Health Department of Mental Health who had conducted a TF-CBT RCT in Zambia (Murray et al., 2015), an abbreviated eight-session TF-CBT treatment manual was developed. This manual included all the treatment components from the original TF-CBT protocol, but with a reduced time frame for completing each component, as follows: Session 1 for assessment and psychoeducation about PTSD, Session 2 for developing relaxation and other emotion modulation skills, Session 3 for modelling cognitive coping skills, Sessions 4 and 5 for conducting prolonged exposure through retellings of the trauma narrative, Session 6 for cognitive reprocessing of unhelpful trauma-related beliefs, Session 7 for a conjoint meeting between participant and caregiver (if indicated), and Session 8 for safety planning. As in the original TF-CBT model, each session is split between time spent with the adolescent followed by time spent with the caregiver (45 min with each), except for the conjoint session. Sessions with caregivers focused on teaching and rehearsing positive parenting skills and demonstrating the coping skills that the adolescent was learning, so that caregivers could support these practices. The adapted manual emphasises asking participants to generate examples from their own life on which to practice the various skills, to ensure that practice examples are contextually relevant for South African participants. It also focuses on problem-solving of contextual barriers to implementing the practice exercises in the South African context (e.g., lack of a private or safe space, or time constraints for over-burdened caregivers).
During a 2-day training workshop, five counsellors were trained in the abbreviated treatment protocol by the fourth author (SS), who was one of the developers of the abbreviated manual. Three were registered counsellors and two were clinical psychologists. Counsellors had been qualified for a period of between 1 and 5 years, and all had previous experience of providing counselling to children and families who had experienced trauma. Counsellors for the abbreviated TF-CBT intervention were selected based on the level of skill they had displayed in a prior training workshop on the standard-length version of TF-CBT.
Study aims
We first aimed to explore whether participants in the pilot study (both adolescents and their caregivers) found the abbreviated TF-CBT model to be acceptable and tolerable. We assessed treatment attendance and drop-out rates as indicators of acceptability: patterns of non-attendance or premature termination of therapy can signal structural barriers to treatment (e.g., the practical burden placed on clients to attend weekly sessions for 8 weeks despite work/school commitments) or a low level of treatment engagement. We also examined whether PTSD symptoms worsened between the beginning and end of treatment, which would indicate poor tolerability. While symptoms may increase during the trauma processing phase of treatment, they should reduce by the end of treatment. In addition, we aimed to qualitatively explore participants’ experiences of the abbreviated intervention.
Second, we aimed to assess counsellor experiences of delivering the abbreviated TF-CBT intervention, including their degree of fidelity to the treatment manual and their self-reported experiences of implementation.
Method
We used a sequential mixed-methods design. Descriptive statistics on treatment attendance, treatment tolerability, and treatment fidelity were gathered in the first stage of the study. This was then supplemented by post-treatment qualitative interviews with participants and counsellors, to further explore experiences of the abbreviated intervention.
Participants
As the pilot study was unfunded, with counsellors giving of their free time to provide the intervention, only a small sample could be included. Ten trauma-exposed adolescents and their caregivers were recruited from a youth traumatic stress clinic at a tertiary institution in Cape Town, South Africa. The clinic receives referrals of trauma-exposed adolescents (aged 11–19 years) from schools, hospitals, the legal system (e.g., in cases of child abuse) and non-governmental organisations. Trauma-exposed adolescents who met a Diagnostic and Statistical Manual of Mental Disorders (5th ed.; DSM-5) diagnosis of PTSD (assessed by a clinical psychologist) or had at least moderate symptoms on the Child PTSD Symptom Scale for DSM 5 (CPSS-5; Foa et al., 2017) were eligible for inclusion.
Participants’ ages ranged from 11 to 17 years, eight were female and five of the participants were ‘coloured’, while the remainder were White (while race is a socially constructed category on which the apartheid system in South Africa was based, it continues to be closely associated with unequal access to resources in post-apartheid South Africa and, as such, remains an important indicator of social and economic experiences in present-day South Africa). All were either English or Afrikaans speaking and were allocated to counsellors who were proficient in their preferred language. The number of traumatic events to which participants had been exposed ranged from two to six, with a mean of 3.6, and included domestic violence, witnessing a murder, sexual assault, and traumatic bereavement. Caregiver involvement was based on caregiver availability (with regard to work commitments and living arrangements). In three of the cases, both parents attended sessions, in two cases, only the father attended, in three cases, only the mother attended, in one case, the sessions were attended by the maternal aunt with whom the participant lived (both parents were deceased), and in the case of a participant who lived in a children’s home, their residential child-care worker attended.
Instruments
Treatment attendance rates
Client attendance data were extracted from the electronic clinical databases of the five counsellors. Counsellors had recorded whether the participant and caregiver attended each scheduled session and the stated reasons for cancelled sessions.
Tolerability
Counsellors administered the CPSS-5 at each session to monitor whether PTSD symptom severity worsened by the end of treatment.
Counsellor fidelity to treatment manual
Counsellors used an electronic database to record which treatment components they delivered in each session and how these were delivered. The clinical supervisor then elicited further details of each session from the counsellor during weekly supervision. If a component was missed or not completed, the supervisor requested completion in the next session and delivery of this component was then recorded in the electronic database. The supervisor therefore monitored the counsellors’ self-reports of fidelity on a weekly basis. For analysis of counsellor fidelity, we extracted the components that were delivered in each session, as recorded on the counsellors’ databases and checked by the clinical supervisor.
Interviews
Semi-structured interviews were conducted with participants and counsellors by a research assistant once treatment was completed. Counsellors were asked about how they experienced implementing the different components of the model, their observations of how participants had engaged in each of the treatment components, and their recommendations for adaptations to the treatment protocol. Participants were asked about their perceptions of each component of the eight-session model, logistical difficulties with attending treatment, and their recommendations for adaptations to the treatment.
Procedure
The first 10 adolescents referred to the clinic who met the inclusion criteria for the study were invited to participate. All 10 eligible participants and their caregivers accepted the invitation and were allocated to one of the five counsellors. Each counsellor saw two participants and received weekly online supervision from a clinical supervisor. Caregivers received a small standard reimbursement for transport costs for each session. Participants were invited to an interview within 1 month of their last TF-CBT session. Six of the ten families agreed to be interviewed. The remaining four families could not be contacted after therapy was completed (e.g., their mobile number was no longer active, or they did not respond to telephone messages inviting them to be interviewed). Only caregivers who had participated in the intervention were interviewed. This included both parents in two cases, only the mother in two cases, and only the father in the other two cases. We therefore conducted interviews with six adolescents and eight caregivers (14 interviews in total).
Ethical considerations
Ethics approval was obtained from the Universities of Cape Town and Stellenbosch and informed consent and assent were obtained from all participants.
Data analysis
We generated frequencies and percentages for the attendance and fidelity data. We checked for possible symptom worsening (lack of tolerability) by calculating the percentage of change in PTSD symptoms on the CPSS between the first and last sessions. Interviews with counsellors and participants were audio-recorded, transcribed, and then analysed using the six-step thematic analysis approach of Braun and Clarke (2006). Initial codes were assigned to each unit of analysis in the interview transcripts and these were used to build a list of codes. Thereafter, codes were compared to identify commonalities and organised into higher order categories. Conceptually related categories were then combined into broad themes.
Results
Treatment attendance
Nine of the ten adolescent participants (90%) completed treatment, while one participant terminated treatment after the fourth session. The clinical records indicated that the participant who terminated therapy prematurely (aged 14 years) was both heavily pregnant and living in a residential care home at the time of treatment. Her circumstances may have been too unstable to allow brief-term trauma exploration to be tolerable at that time. Of the nine participants who completed treatment, eight completed within eight sessions as per the treatment manual, while in one case, treatment was extended to nine sessions. For this latter case, the clinical records indicate that more time was needed for trauma processing due to very high levels of avoidance of traumatic reminders. Caregiver attendance was also high, with a caregiver co-attending 86% of appointments.
Missed or cancelled sessions that had to be rescheduled were common. Only two participants attended every scheduled session and completed treatment within eight chronological weeks. The remainder re-scheduled at least two sessions and took between 10 and 14 chronological weeks to complete eight sessions. Reasons provided by clients or caregivers for missed and cancelled sessions included school exams, school functions or sports events, caregiver work commitments, illness, and transport difficulties.
Tolerability
While there was some minor fluctuation in PTSD symptoms across sessions, as would be expected in exposure-based treatments, PTSD symptom severity decreased by between 39% and 100% for all participants between their first and last sessions, with an average reduction of 80% (see Figure 1).
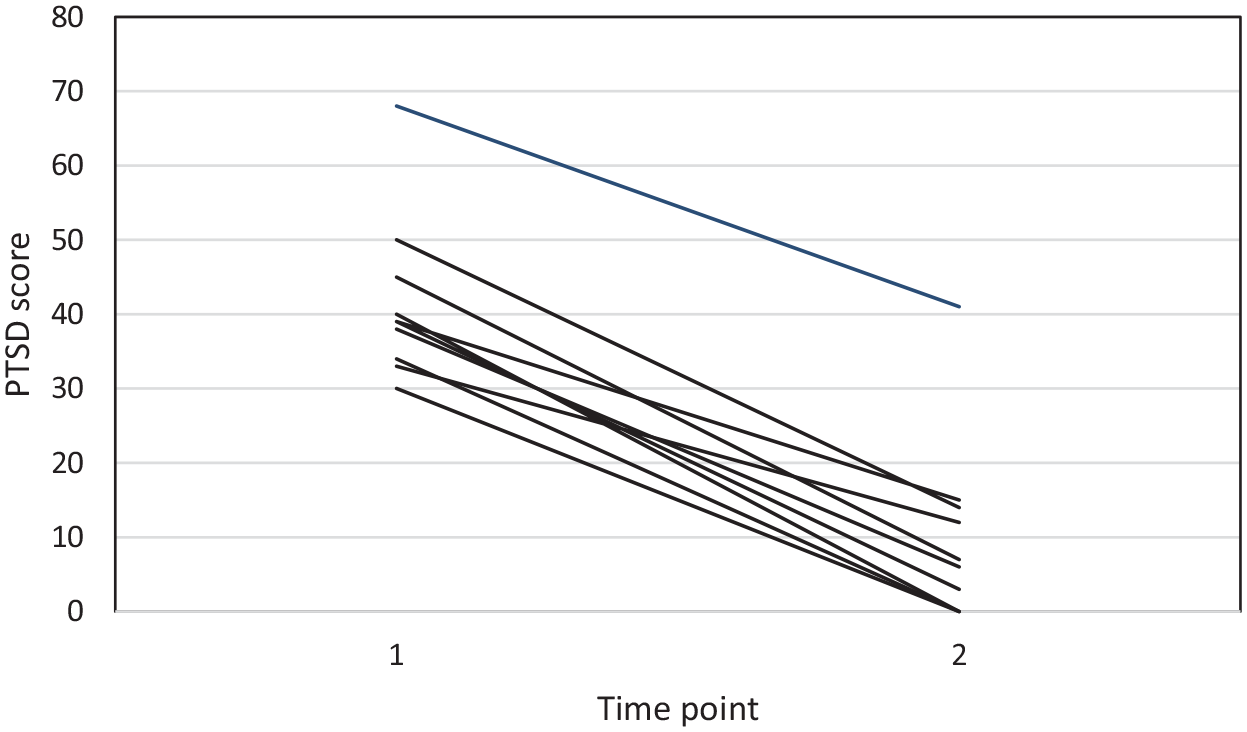
Change in PTSD scores from first to last session for individual participants.
Treatment adherence
In Sessions 1–4, there was 100% adherence to the treatment protocol, with all counsellors delivering psychoeducation in Session 1, relaxation/emotion modulation in Session 2, cognitive coping in Session 3, and starting the trauma narrative in Session 4. As noted previously, one client discontinued therapy after Session 4 and the remaining components could therefore not be delivered. Eight of the remaining nine clients completed the trauma narrative in Session 5 and worked on cognitive reprocessing in Session 6, as specified in the manual. In the ninth remaining case, the counsellor focused on enhancing safety in Session 5, due to a safety issue that arose in that session, and then picked up again on the trauma narrative in Session 6.
A conjoint session (Session 7 in the abbreviated treatment manual) is only conducted if the counsellor judges it to be appropriate for the adolescent–caregiver dyad in each case. In our study, a conjoint session was conducted in only five of the nine completed cases. According to the clinical records, in the remaining cases, the counsellor and supervisor judged that a conjoint session would not be appropriate, due to caregiver mental health status or to concerns about a caregiver’s ability to constructively engage with the adolescents’ needs. In these cases, Session 7 was used instead to consolidate previous treatment components.
Finally, there was some minor variability in the timing of the enhancing safety component. For the nine clients who completed all eight sessions, in six cases, enhancing safety was conducted in the last session, as per the manual. In three cases, it was introduced in a previous session due to safety and risk issues that arose at that stage of therapy (e.g., substance use, risky sexual behaviour, or environmental dangers, such as gang violence or domestic violence), and enhancing safety was then revisited and reinforced in Session 8.
Counsellor and client perceptions of the eight-session TF-CBT model
The most common themes emerging from the 19 interviews with counsellors (n = 5) and participants (n = 14) are presented below.
Importance of the therapeutic alliance
A good therapeutic alliance, allowing for the development of trust and safety, is essential to trauma-focused CBT (Cohen et al., 2006) and to the successful implementation of prolonged exposure therapy for PTSD in general (Capaldi et al., 2016). We were concerned that an abbreviated version of TF-CBT may not allow sufficient time for the development of a strong therapeutic alliance prior to embarking on trauma exposure components. Although not asked directly about the quality of the therapeutic relationship, in the interviews, four caregivers and five adolescent clients spontaneously described the importance of their relationship with the counsellor in overcoming their initial anxieties about attending treatment and enabling a sense of safety and trust that scaffolded the treatment. Similarly, all five counsellors described the development of trust and rapport as the foundation of their work with all the participants.
Obviously, it was hard in the beginning. I am a person who has trust issues . . . She showed me that I don’t have to be so hard-headed all the time and have my guard up all the time. (Participant 4) She showed me it’s a safe space and that I can trust her and what we will share will stay between us. (Participant 6) The therapist, she brings out a lot of things that I had inside me that I didn’t even know about. (Caregiver 2)
A systematic review of user perceptions of TF-CBT found that uncertainty and anxiety about starting therapy are common among youth embarking on TF-CBT and that the development of a therapeutic alliance can alleviate these concerns and enhance therapeutic engagement (Neelakantan et al., 2019). Furthermore, a positive working relationship is critical for involving young people in the various skills-based tasks required by TF-CBT (Ormhaug et al., 2014). Our qualitative findings indicate that even in the abbreviated version of TF-CBT, where the active work of skills development starts immediately after the first session, counsellors were able to establish a collaborative relationship with their clients. Participants and counsellors perceived that this alliance provided a solid foundation for moving through the different treatment components. Although we cannot comment on the experience of those participants who did not respond to the invitation to be interviewed, for interview participants, the abbreviated model did not appear to compromise the quality of the therapeutic relationship.
Value of coping skills
Nine of the interviewed participants reported that the coping skills components (relaxation/emotion modulation and cognitive coping) challenged them with new skills that took some practice to learn.
It was weird because I would never think of that . . . It took quite a while, I mean, I wasn’t used to it. (Participant 6) At first it was a little bit hard . . . I just didn’t understand it . . . but then it got better. (Participant 3) I began to understand it better as it went along and how it must be done. (Participant 1)
Despite this, all five counsellors, all six adolescents and three of the caregivers reported that the coping skills were useful in participants’ everyday life to cope with stressors at home, work, or school.
Sometimes when I wake up in the middle of the night I do it, it helps me to relax and to feel better. (Participant 5) Like when I was at work then I would have the managers being rude at me, so I would use the triangle and see where they coming from and maybe they’re stressed so I shouldn’t get angry or stressed over it. (Caregiver 6) He was using the skills set we taught, the relaxation . . . Talked about doing it on the bus one day on the way from school. (Counsellor A)
The acceptability and usefulness of CBT coping skills for youth living in a context of ongoing trauma exposure combined with multiple socioeconomic adversities have not been well established. Furthermore, in an abbreviated TF-CBT model, participants may not have sufficient time to develop and consolidate new coping skills. However, the interview respondents indicated that the coping skills components, though challenging, were both acceptable and useful to them and that they had adequate opportunity to practice these skills until they became more familiar. These reported benefits of the coping skills components are in line with user perceptions of longer versions of TF-CBT (Neelakantan et al., 2019), indicating that the abbreviated TF-CBT model did not significantly compromise participants’ ability to engage with coping skills.
Trauma narrative process as challenging but beneficial
All the counsellors and all the adolescent clients experienced the trauma narrative component as the most challenging and anxiety-provoking aspect of the treatment.
It was very hard . . . the hardest part of coming to therapy. (Participant 4) It was hard because I didn’t want to tell . . . Because the story was scary. (Participant 5) She was incredibly resistant and avoidant once we started to talk about the story. You could see she just didn’t want to engage anymore. (Counsellor E)
Anxiety about approaching traumatic memories is common both among traumatised youth in TF-CBT treatment (Neelakantan et al., 2019) and among counsellors who are delivering exposure-based trauma interventions (Ascienzo et al., 2020). In an abbreviated model of TF-CBT, the reduced time frame for completing the trauma narrative component may further reduce acceptability and tolerability of this component. However, in the interviews, all the counsellors and all six adolescent participants reported that the trauma narrative component, while difficult, was helpful in addressing the participants’ symptoms.
When he read it over and all the feelings came up again . . . It helped me. (Participant 1) When I wrote the story I felt better. (Participant 3) Once I’ve gotten past the trauma narrative there seems to quite an improvement in there’s a symptom reduction on the one hand so sometimes a lot will spike at that time and will drop quite rapidly after that. (Counsellor B)
It therefore appears that the abbreviated trauma narrative process, while challenging, was experienced as tolerable to both counsellors and participants, and was perceived to be valuable in addressing traumatic stress symptoms, in the same way as it is perceived to be challenging but beneficial to users of standard-length TF-CBT (Neelakantan et al., 2019).
Flexibility within fidelity
All five counsellors reported that they liked the balance between structure and flexibility within the abbreviated TF-CBT intervention. Counsellors indicated that having a ‘road map’ for each session in the treatment manual was a helpful foundation but the dosage (duration) and order of components could be adapted somewhat depending on the needs and capacities of the specific client. For example, in some cases, enhancing safety had to be delivered earlier than the last session if there were significant risk factors, as would be expected in a context of ongoing violence and multiple adversity. The counsellors recognised that, while it is important to achieve certain treatment goals within a session, how those goals are implemented can vary somewhat according to the clients’ needs.
I think a programme is a nice grounding and you have to adapt the programme to the case you work with, to their individual needs. But having the manual as something to go to is very helpful. (Counsellor D) I think that it’s not so heavily manualised that you can’t be flexible . . . We get to balance the whole thing of having adherence to certain goals and things that needs to happen versus being flexible enough to individualise it. (Counsellor E)
The abbreviated TF-CBT model therefore appears to have been acceptable to the counsellors as it provided a clear structure and also allowed sufficient scope to tailor the model to participants’ individual needs. These views affirm the argument by Kendall and Frank (2018) that flexibility within fidelity is vital to implementation of protocol-based treatments.
Discussion
Abbreviated TF-CBT has not been evaluated outside the United States, or with youth living in contexts of ongoing trauma exposure. This study aimed to assess client and counsellor experiences of an abbreviated version of TF-CBT in the South African context, using a mixed-methods approach.
While drop-out rates are a concern in implementing trauma-focused therapies for youth (Eslinger et al., 2014; Wamser-Nanney, 2020), the high rates of treatment completion by participants and caregiver attendance at sessions are quantitative indicators that our abbreviated TF-CBT treatment was acceptable to the participants and their caregivers. The reduction in PTSD symptom severity by end of treatment for all participants supports treatment tolerability, although the actual effectiveness of the abbreviated intervention can only be determined in an RCT. Sample heterogeneity with regard to both number of trauma exposures and age did not appear to impact on either completion rates or tolerability, however, these potential moderators would need to be explored in a larger evaluation.
These quantitative indicators of acceptability and tolerability were supported by qualitative findings. Interviewed participants expressed that a good therapeutic alliance was an important component of treatment acceptability and was successfully established even within the abbreviated treatment process. The individual components of the treatment also appeared to be acceptable to participants, despite being abbreviated into a shorter time frame than the original TF-CBT model. Adolescents and caregivers reported that, while the coping skills needed some practice, they were able to start implementing these skills to address daily stressors in their lives. Adolescent interview participants all experienced the trauma narrative component to be very difficult, as would be expected, but all reported that it was helpful and that they experienced notable symptom relief once this component was completed. These qualitative findings closely replicate those found in a systematic review of user perceptions of standard-length TF-CBT (Neelakantan et al., 2019), indicating that our abbreviated treatment model did not compromise user experience.
Low levels of counsellor fidelity to evidence-based PTSD treatments, reported in some previous studies (Allen & Johnson, 2015; Ascienzo et al., 2020) were not replicated here. While there was some flexibility in the dosage and timing of treatment components to match individual client needs, counsellor adherence to the treatment manual was high. Regardless of their level of qualification, counsellors were able to deliver the full intervention within eight sessions for all but one of the treatment completers. This may reflect the benefits of regular clinical supervision after the initial TF-CBT training, which has been linked to better TF-CBT treatment fidelity (Ascienzo et al., 2020).
However, the high rate of missed or cancelled sessions that had to be rescheduled suggests that it in the South African context, it may not always be feasible to deliver treatment in eight consecutive weeks. Allowance needs to be made for this when planning a formal evaluation and later possible scaling up of the intervention. The conjoint session may be the one component that was negatively affected by the abbreviated treatment time frame. With a more extended treatment duration, there may have been more time to prepare both participants and caregivers for a conjoint session and to work through any barriers or concerns, allowing for a conjoint session to be included in more of the cases.
This study demonstrates the value of collecting both quantitative and qualitative data when adapting an evidence-based PTSD intervention for youth in LMICs. There are very few qualitative studies on young people’s experience of TF-CBT, particularly in LMICs (Neelakantan et al., 2019). Our findings confirm that youth have valuable perspectives to offer and their voices should be included in future research on adapting trauma interventions for South Africa and other LMIC contexts.
The study had several limitations. First, the sample was small and not fully demographically representative of the Western Cape population as it did not include indigenous African language speakers, who constitute about one third of the provincial population. Second, treatment fidelity was assessed through counsellors’ clinical records and there were no independent raters of counsellor adherence. However, the clinical supervisor checked the weekly clinical records against her detailed case discussion with each counsellor in weekly supervision and would have noted and addressed any inaccurate recording of session procedures on the clinical records. Third, those families who could not be contacted for interviews may have had different experiences of the treatment. However, the high rate of treatment completion in the full sample suggests that the treatment was acceptable to most participants. Fourth, the provision of transport reimbursement to participants may have enhanced attendance and treatment completion; in real world treatment settings in South Africa, transport costs may present a barrier to treatment attendance and completion. Finally, without a control group, this study cannot draw conclusions about the efficacy of the abbreviated TF-CBT treatment. This can only be evaluated by a larger RCT.
Conclusion
While TF-CBT is recommended as a first-line intervention for PTSD in youth, there is a lack of research on abbreviated TF-CBT outside of the United States. This study indicates that an eight-session TF-CBT protocol is acceptable and tolerable to participants and, with adequate training and supervision, can be implemented with fidelity by counsellors. These findings support the feasibility of proceeding with a formal evaluation of the effectiveness of the abbreviated eight-session TF-CBT model with trauma-exposed South African adolescents, to add to the limited local evidence regarding treatment of youth traumatic stress.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is based on research supported in part by the National Research Foundation of South Africa (Grant Number 93568).
