Abstract
This study examines medication home delivery incidents reported in community pharmacies before and after the onset of the COVID-19 pandemic. Medication home delivery incidents are defined as medication errors that occur during the transportation of medication to patients outside the pharmacy through shipping, courier, or pharmacy delivery services. The objective was to analyze trends over time and identify contributing factors to inform patient safety improvements. A retrospective analysis was conducted on medication home delivery incidents reported to a national Community Pharmacy Incident Reporting system, Pharmapod (a Think Research company). Reports from 4091 community pharmacies across 10 provinces and 2 Territories were reviewed, covering the period from January 1, 2019, to January 27, 2022. A total of 156 medication home delivery incidents were identified and analyzed. Of the 156 incidents, 55 (35%) occurred pre-COVID and 101 (65%) post-COVID. The most frequent incident type was delivery to the incorrect patient, which decreased from 52.8% to 32.7%. In contrast, privacy breaches increased significantly from 29.2% to 41.6%. Contributing factors include staffing distribution, lack of quality control or independent checks, environmental distraction, operational workflow gaps, and insufficient staff training. Medication home delivery incidents increased following the onset of the COVID-19 pandemic, revealing emerging safety risks in pharmacy delivery practices. The shift in incident types and contributing factors highlights the need for improved verification protocols, enhanced privacy protections, and dedicated staff training. As home delivery services continue to expand, these findings underscore the importance of system-level interventions to safeguard medication safety in the community pharmacy setting.
Keywords
Introduction
The COVID-19 pandemic significantly impacted health service delivery, including medication distribution to patients. The rise in patient demands for non-pharmacy pick-up options, such as curbside and residential delivery, led to a substantial increase in medication home delivery services. These services involve transporting medications dispensed at community pharmacies to patients’ residences or their designated caregivers. 1
Pre-pandemic medication procurement methods included direct pharmacy counter pickup, drive-through windows, delivery to post offices or contactless lockers, and home delivery. The pandemic accelerated the growth of existing online pharmacy platforms and sparked the emergence of new ones, such as Amazon Pharmacy, 2 Pocket Pill, 3 and MedNow. 4 Many community pharmacies also expanded their prescription delivery services. These remote delivery options became crucial in reducing disease transmission by decreasing congestion at healthcare facilities. 5
Recent research has shown that home delivery of medications via mail order improved access, particularly for individuals with disabilities. This method has been associated with better health-related outcomes and reduced costs. 6 Researchers in Canada anticipate that this trend will continue. 7 with similar increases observed in countries like Qatar, 8 South Africa, 9 Spain, 10 and Saudi Arabia. 11 However, the rise in medication home delivery practices has raised concerns about an increased occurrence of medication incidents (MIs). Medication incidents (MIs) are defined as “any preventable event that may cause or lead to inappropriate medication use or patient harm while the medication is in the control of the healthcare professional, patient, or consumer.” 12 MIs also refer to medication errors that reach the patient (eg, incorrect drug, doses, quantity), in addition to medication errors that are intercepted before dispensing (ie, near misses). 1
Medication home delivery incidents specifically refer to errors occurring outside the pharmacy during the transportation of medication to patients via shipping, courier, or pharmacy delivery services. The UK-based National Pharmacy Association identified these errors as a growing patient safety concern in 2017. 13 Common types of incidents include medicines delivered to the wrong patient, wrong labeling in the delivered package, and inappropriate patient counseling. 6 More severe consequences have included drug overdoses, drug thefts, and consumption by family pets. 14
Recent research findings have identified critical areas in medication home delivery practice that can create the conditions leading to MIs. These include communication breakdowns between prescribers, pharmacies, and delivery services, 8 incomplete personal information such as home addresses, 15 and various delivery-related errors including non-delivery, dosing errors, wrong medication, unnecessary medication, incorrect formulation, and wrong patient. 10
Despite the pandemic-driven expansion of medication home delivery services, there is a lack of evidence regarding related incidents, particularly in the Canadian context. This study aims to address this gap by examining and identifying trends, contributing factors, and potential sources of medication home delivery incidents in Canadian community pharmacies, comparing pre- and post-COVID-19 pandemic periods.
Methods
We conducted a retrospective analysis of MIs reported to Pharmapod, a national Community Pharmacy Incident Reporting system. Pharmapod is used by 65% of Canadian community pharmacies. The study includes data from 4091 pharmacies across 10 provinces and 2 territories, spanning from January 1, 2019, to January 27, 2022.
MI data in Pharmapod reports include category of incident (eg, incorrect labeling, incorrect dose, incorrect patient, incorrect quantity), the stage of the incident (ie, step along the medication management process where the incident occurred such as the prescribing, dispensing, delivery), and contributing factors (ie, potential variables that were present in the moment of the incident and might have led to the incident). The categories of the medication incidents were already preset in the reporting system developed by Pharmapod, and the community pharmacist completing the incident report chose the best fit for the incident that was reported based on the preset categories. Incident categories for the study included any delivery outside the pharmacy via shipping, courier, or pharmacy delivery services. The research team accessed the anonymized data version, and all identifiable information had been removed before the analysis.
The coding was done manually by the first 2 authors, who thoroughly read and familiarized themselves with the data. The filtering process for identifying medication delivery incidents was as follows: A total of 56 422 MIs were reported. First, 182 medication incidents (MIs) were excluded due to incomplete data, leaving 56 240 incidents for screening. These were then filtered to identify delivery-related incidents, resulting in the exclusion of 55 970 non-delivery MIs. The remaining 270 delivery-related incidents were further reviewed in detail to confirm relevance, and 114 were excluded due to unclear classification or insufficient detail. Ultimately, 156 MIs met the inclusion criteria of having occurred during home delivery and were analyzed in this study.
Ethics approval was unnecessary because the research relied exclusively on the secondary use of anonymizedinformation in aggregates that did not contain identifiable information (as per TCPS2 Article 2.4). Confidentiality agreements were signed in the research partnership.
A descriptive analysis was performed for the event point or stage where the incident occurred, the category of the incident, and the frequency of reporting before and after the start of the COVID-19 pandemic (March 2020).
To specify incidents as before or after the World Health Organization’s declaration of the pandemic, the pre-COVID dates were January 1, 2019, to March 12, 2020, and the post-COVID dates were March 13, 2020, to January 27, 2022, helping to categorize the data analysis between pre-COVID and post-COVID.
This study followed the STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) reporting guideline for observational research. 16
To determine if there were statistically significant differences in the distribution of medication home delivery incidents before and after the onset of the COVID-19 pandemic, chi-square tests were conducted for the 4 most frequently reported incidents: Incorrect Patient, Breach of Privacy, Incorrect Drug, and Incorrect Label.
Results
A total of 56 422 MIs were reported between January 2019 and January 2022. Of the over 56 000 incidents reported, 156 incidents occurred during delivery to the addresses of the patients (home delivery) and were included in the present analysis. During the Pre-COVID period (January 1, 2019-Mar 12, 2020), there were 55 (35.3%) incidents reported, and during the Post-COVID period (Mar 13, 2020-Jan 27, 2022), there were 101 (64.7%) incidents reported. Note: Chi-square test comparing pre- and post-COVID incident frequency: χ² = 13.36, df = 1, P < .001
A statistically significant decrease was observed in the proportion of Incorrect Patient incidents post-COVID (χ² = 6.89, P = .0087), suggesting that while the absolute number increased slightly, it formed a smaller proportion of total delivery incidents in the post-pandemic period. A statistically significant increase was observed in Privacy Breaches after the pandemic (χ² = 4.73, P = .0296), indicating that this category became more prominent during the expanded use of home delivery services. The differences in Incorrect Drug and Incorrect Label incidents were not statistically significant, due to possibly smaller sample sizes in these categories.
Tables 1 and 2, and Figure 1 present the categorization of the medication home delivery incidents recorded by the pharmacist when entering the information about the event into the Pharmapod system. As can be seen in the tables, the 4 most recurring types of incidents were the delivery of the medication to the wrong patient, breach of patient privacy, delivery of incorrect medication, and incorrect labeling during the medication home delivery process (Table 1).
Frequency of Medication Home Delivery Incidents.

Chi-Square Test Results for the 2 Most Frequently Reported Incidents.

Note. Significance threshold: P < .05. Chi-square tests were applied only to categories with sufficient sample sizes (typically ≥ 5 in both groups). Categories with low frequencies were excluded from statistical testing or marked with (–).
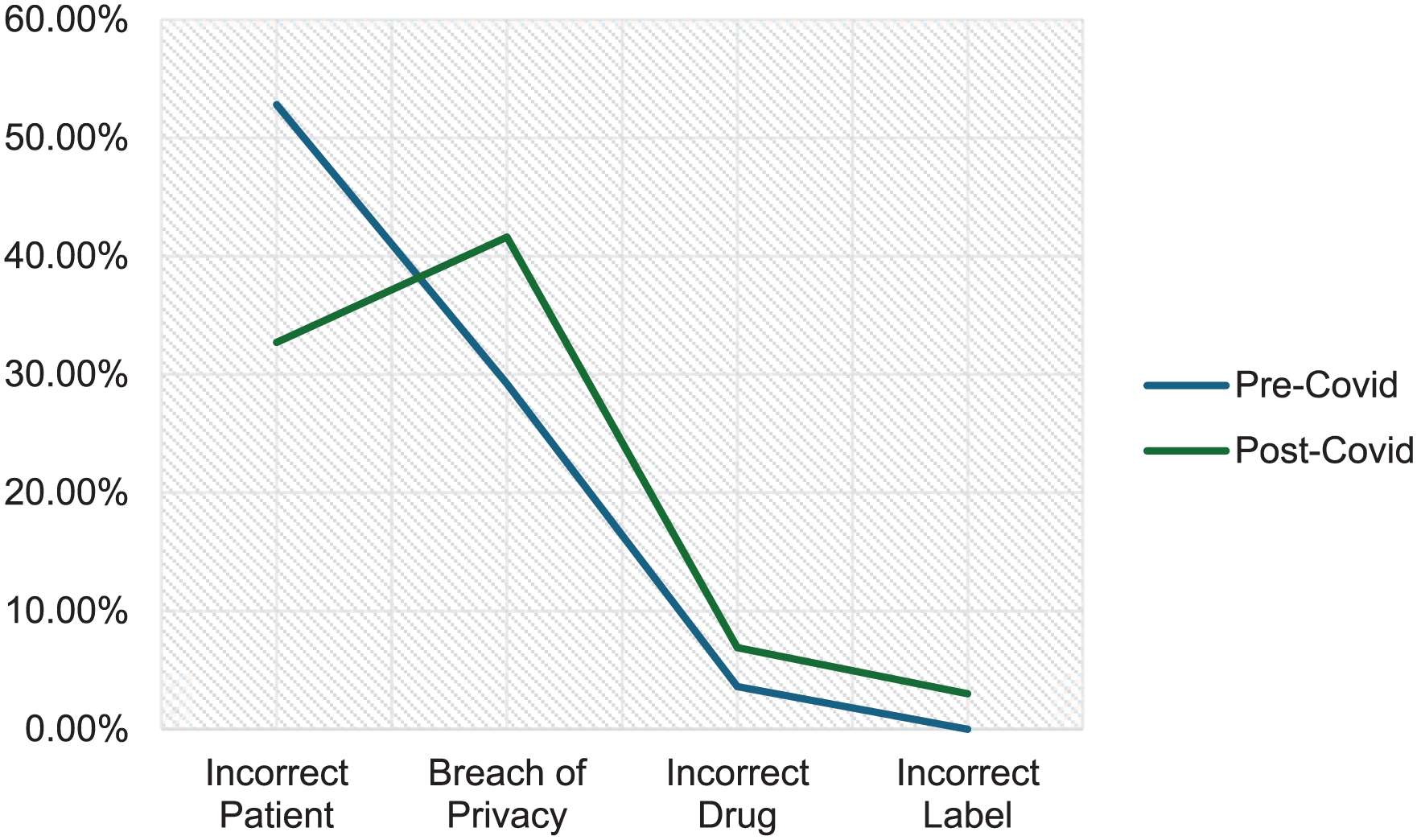
Trend of the top 4 medication home delivery incidents.
Discussion
This study examined trends in medication home delivery incidents in Canadian community pharmacies before and after the onset of the COVID-19 pandemic. The findings reveal a notable increase in the total number of incidents during the post-pandemic period, with 65% of all reported delivery-related medication incidents occurring after the onset of the pandemic. This increase likely reflects the substantial growth in demand for home delivery services as pharmacies adapted to public health restrictions and changing patient behaviors
Trends and Shifts in Incident Categories
The analysis of incident categories revealed important shifts over time. Incorrect patient incidents remained the most frequently reported category, increasing in absolute number from 29 to 33. However, their proportion of total incidents significantly decreased, from 52.8% pre-pandemic to 32.7% post-pandemic (χ² = 6.89, P = .0087). This suggests some improvement in preventing this type of error, possibly due to increased awareness or procedural adjustments.
In contrast, privacy breaches emerged as a growing concern, increasing significantly in both absolute (from 16 to 42) and relative terms (from 29.2% to 41.6%; χ² = 4.73, P = .0296). These findings suggest that maintaining patient confidentiality during delivery became more challenging.
Other categories, such as incorrect drug and incorrect label, showed increases, but these changes were not statistically significant and thus not included in the table. Nonetheless, they point to areas where continued vigilance is needed, especially as these types of errors can have serious clinical implications.
Contributing Factors and Delivery Challenges
The analysis of narrative reports revealed that delivery incidents often stem from upstream process errors within the pharmacy, such as incorrect labeling or packaging. These internal errors are contributing factors that, when combined with external delivery challenges, such as wrong address, lack of recipient verification, or environmental distractions, create major risks. For example, this report illustrated a lack of quality control and independent checks: “2 patients' IV medications were switched during delivery (Table 3).”
Contributing Factors of Home Medication Delivery Incidents.

Note. Staff distribution, education gaps, and quality control issues were the primary contributors in the report.
Delivery Driver
Delivery drivers play a critical role in maintaining medication integrity and ensuring proper delivery through verification processes. While pharmacies establish protocols for quality control, home delivery remains complex, and these measures do not prevent all incidents. External factors like traffic, weather, and navigation challenges further contribute to medication delivery errors. Data highlights that these non-dispensing factors, such as misreading an address, are significant contributors to home delivery incidents, emphasizing the need for improved oversight and operational safeguards.
This example from the MI report indicates a lack of quality control or independent checks:
Driver delivered medication to #17 instead of #17 1/2 on the same street. Error was discovered when (the) patient called to report that she had not received her delivery.
Another category of delivery incidents contributing to delivery person MIs is breach of privacy. Patient privacy is breached when the personal information or record of a patient, which is confidential, is given to other individuals, either by wrong labeling, mismatched delivery, or theft. For example, cases where the delivery driver was robbed were reported, therefore compromising the patient’s information, as seen in these MI reports:
"(The)Delivery driver’s vehicle was stolen. . .″ Delivery driver was robbed en route.
Sometimes, the delivery drivers were implicated not only in operational errors but in behaviors raising concerns about negligence or potential misconduct. For example, a situation where the delivery driver did not return an undelivered opioid medication to the pharmacy.
(The) delivery driver was given a codeine prescription to deliver for GK. The patient GK was not home at the time of the delivery - the Driver returned to the store and dropped off another patient’s medication but did not leave GK’s prescription with (the) pharmacy staff.
In another case, the driver urged the patient to take a medication despite her stating it wasn’t hers.
The driver took the package to house number 23 (the correct house number is 223). Both patients are our customers. The driver insisted that the customer take the package despite her telling him it was not her name. The driver also "waved" the charge because this patient usually (has) no charge. . .
Relationship Between Incidents Inside and Outside the Pharmacy
Medication home delivery incidents often stem from errors inside the pharmacy that carry over into the delivery process. Mistakes such as incorrect labeling, packaging, and patient mix-ups can lead to the wrong medication being delivered. Staffing shortages, 17 particularly during the pandemic, played a significant role in these errors, with increased workloads and pharmacist exhaustion contributing to mistakes. Additionally, a lack of quality control and independent verification exacerbated the issue, leading to mislabeled prescriptions, delivery mix-ups, and environmental distractions affecting operations.
To reduce errors in medication home delivery, pharmacies must first address internal challenges. Improving staff distribution, implementing stricter verification processes, and enforcing quality control measures at the preparation stage can prevent incidents before they reach patients. Strengthening these processes inside the pharmacy can significantly enhance accuracy and safety in home delivery services.
Implications and Recommendations
To improve patient safety and delivery reliability, pharmacies should implement
Pharmacies should leverage
Lastly, fostering a
Limitations and Future Research
This study had some limitations. First, the data relied on self-reported incidents, which may not have captured all occurrences. Second, the lack of detailed monthly or quarterly data limits our ability to analyze finer-grained trends over time. Although the study observed a post-COVID increase in medication home delivery incidents, the absence of delivery volume data limits conclusions about incident rates across the country. However, widespread expansion of pharmacy delivery services and greater patient reliance during the pandemic suggest that increased delivery activity may have contributed to the higher number of reported incidents.
Future research should aim to collect more granular time-series data to better understand the evolution of medication home delivery incidents throughout the pandemic and beyond. Additionally, qualitative research involving interviews with pharmacy staff and delivery personnel could provide valuable insights into the challenges and potential solutions for improving medication home delivery services.
Conclusion
The COVID-19 pandemic accelerated the adoption of medication home delivery services across Canada but also introduced new risks to patient safety. This study revealed both the scope of home delivery incidents and the need for structured interventions to mitigate them. The significant rise in privacy breaches, coupled with persistent delivery errors, signals the importance of enhanced systems, training, and protocols.
By implementing the recommendations outlined above, focusing on privacy, quality control, staffing, training, and technology, community pharmacies can strengthen their delivery services and reduce the risk of medication incidents. As home delivery becomes a permanent feature of pharmacy care, ongoing evaluation and adaptation will be essential to ensure that safety and quality standards keep pace with innovation.
Supplemental Material
sj-pdf-1-inq-10.1177_00469580251375868 – Supplemental material for Trends and Contributing Factors in Medication Home Delivery Incidents in Community Pharmacies Before and After COVID-19: A Retrospective Analysis
Supplemental material, sj-pdf-1-inq-10.1177_00469580251375868 for Trends and Contributing Factors in Medication Home Delivery Incidents in Community Pharmacies Before and After COVID-19: A Retrospective Analysis by Beatrice Onwuka, Paola A. Gonzalez, Benoit Aubert, Denis O’Donnell, Neil J. MacKinnon, Carla Beaton and James R. Barker in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Footnotes
Author’s Note
Neil J. MacKinnon is now affiliated to Central Michigan University, MI, USA.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by The Social Sciences and Humanities Research Council (SSHRC) in Canada. #430-2022-00683.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
