Abstract
Community violence intervention and prevention (CVI) programs aim to reduce gun violence and its associated harms through community-driven strategies. Programs’ long-term sustainability is challenged by inconsistent and insufficient funding, however, which can be detrimental to the individuals who depend on these services as they navigate recovery from a violent injury. As states explore new funding mechanisms, Medicaid reimbursement has emerged as a viable option, however little implementation guidance exists specific to this policy option in the CVI context. This study combines the implementation science and public health infrastructure literatures with data from a recent multistate case study (n = 17 key stakeholder interviews) to produce a readiness assessment for funding CVI through Medicaid. The readiness assessment is organized by the stages of the EPIS (Exploration-Preparation-Implementation-Sustainment) framework and provides tangible guidance to states looking to improve their CVI infrastructure. The assessment includes recommendations that reflect key challenges and facilitators of implementation, as dictated by those who have recently navigated this process. Given the urgency of reducing gun violence and its harms, this study underscores the importance of structured policy planning to enhance CVI program viability and sustainability. This study contributes to the growing implementation science and public health infrastructure literatures by offering a theoretically grounded and evidence-informed tool to support policymakers in establishing sustainable funding mechanisms for CVI.
Keywords
Highlights
● States can leverage Medicaid to help sustain community violence intervention and prevention initiatives within the broader public health infrastructure.
● Lessons from early policy adopters are available and informative for future implementation.
● States should use the Readiness Assessment to inform their policy and implementation.
Introduction and Background
Gun violence has fluctuated considerably in many American cities in recent years. 1 Increases in gun violence are often met with policy shifts toward problem-oriented policing in high crime communities,2,3 however these responses have had negative collateral impacts on communities, including poor community-police relations, and crime displacement. 4 Not surprisingly, these collateral effects have led to considerable pushback against criminal justice-oriented responses to gun violence, shifting support to more community-driven strategies. 5
Community violence intervention and prevention (CVI) programs rely less on police intervention and leverage community resources and expertise to reduce gun violence and its harms. 6 Programs are typically community- or hospital-based and deploy violence interrupters—sometimes referred to by different names (eg, violence intervention specialists)—who hail from local communities and often have lived experience with violent injuries. Some CVI strategies have been used by grassroots community organizations since the 1960s 7 —however, they have received increased attention over the last decade due to the growth of programs like Cure Violence. 8 The Cure Violence model views violence as a communicable disease and uses strategies like detection, intervention, and social norm change to reduce violence (see https://sites.temple.edu/cureviolencephl/).
In 2021, former President Biden recognized CVI as an effective tool, leading to a swell of Federal funding and bipartisan support for such programs across multiple agencies. Especially notable was the provision of over 2 billion dollars of American Rescue Plan funding 9 and an additional 1.4 billion from the Bipartisan Safer Communities Act. 10 Despite this wave of financial and political support for CVIs, grant-based funding alone does not offer programs long-term sustainability and is highly contingent upon changes in political leadership and policy direction. Case in point, under the 2024 Presidential administration more than 350 grants awarded to CVI initiatives (valued at over $800 million) were recently ended midstream, forcing some grantees into layoffs and program closures. 11
CVI service delivery is resource intensive; it often requires staff to go into communities or hospitals around the clock, maintain frequent and sustained contact with participants as they recover, and address their complex immediate and long-term needs that are associated with violent injury. 12 When CVI programs lack sufficient resources, those most affected are individuals who suffer violent injuries—often young men of color, for whom gun violence is a leading cause of injury, and death. 13 Grant-based funding streams typically provide start-up funds to establish such programs but lack a plan for long-term sustainability. As a result, even though they provide essential support for these services, grants require programs to continuously monitor new requests-for-proposals (RFPs), complete labor-intensive applications, and report deliverables to remain in compliance with funders.
The challenge of sustainability in the public health space is by no means unique to CVI; similar challenges characterized the development of tobacco control programs, which are informative for more recent CVI efforts. While much attention was paid to evidence-based interventions relating to tobacco control, Lavinghouze et al 14 found that an equally if not more significant driver of the success and sustainability of such programs was the establishment of a solid public health infrastructure–including reliable long-term funding of surveillance programs through the U.S. Centers for Disease Control and Prevention (CDC). From this important research Lavinghouze et al 14 developed the Component Model of Infrastructure (CMI), which includes 5 interrelated core components that serve as a foundation upon which programs can build capacity and achieve public health outcomes: (1) guidance from leadership at all organizational levels (“multilevel leadership”), (2) diverse funding and personnel who reflect community needs and can implement best practices (“managed resources”), (3) data that are actively used to inform and motivate actions (“engaged data”), (4) strategic plans that are collaboratively developed and adapted to reflect evolving evidence and priorities (“responsive plans and planning”), and (5) strategic collaborations across local, state, and national levels (“networked partnerships”). Pilot study findings support that the CMI and its core components are measurable, have good face validity, and can produce data that enhance the sustainability of public health efforts via high quality evaluation and informed program planning. 15 The CMI and lessons learned from tobacco control programs are particularly salient to CVI today in that these programs also require a core public health infrastructure that is undergirded by reliable long-term funding.
Many states are currently considering or implementing policies that leverage state policymaking powers to fund and sustain CVI through Medicaid—a Federal program that is administered at the state level and designed to bring healthcare to low-income individuals (hereafter, “the policy,” see www.medicaid.gov/). 16 After Medicaid expansion under the Affordable Care Act (ACA) of 2010, a larger portion of the population became Medicaid-eligible, resulting in the program becoming the single largest payer of costs associated with gunshot wounds (GSWs). 17 Under the policy, those providing frontline CVI services can become Medicaid-certified providers and receive reimbursements for their time spent delivering case management, crisis intervention, and other essential services to victims/survivors of violence who are insured through Medicaid. To date, little specific guidance exists regarding the adoption and implementation of this specific policy. To address this gap, the authors build upon prior research 18 to develop a state readiness assessment that aids policymakers, stakeholders, and advocates in exploring, planning, implementing, and sustaining a Medicaid reimbursement policy for CVI.
Why Create a Readiness Assessment?
Readiness assessments are designed to measure the level of preparedness for undertaking a new technology, policy, or practice among an organized group of people, and are often used in management and business operations to assess organizational readiness. 19 Recent developments in the conceptualization of readiness have expanded beyond the individual and organizational levels to include the notion of “community readiness” for violence prevention. 20 In this context, “community” refers to the network of stakeholders who are directly or indirectly impacted by gun violence and the corresponding strategies aimed at its prevention, reduction, or response. Campie et al note that a lack of readiness among a single influential stakeholder may be sufficient to undermine the success of a given initiative, even when consensus exists among the broader stakeholder group. 20 For this reason it is essential to examine the interdependent readiness across all levels—individual, organizational, and community—to know the viability of leveraging Medicaid funding to address gun violence.
Specific to policymaking, readiness assessments can promote the success and sustainability of a given policy through leveraging prior knowledge from other contexts to ensure that new adopters are prepared for implementation. 21 There are a few examples of the development and use of applied readiness assessments for public policy implementation within a state, county, or local community.20,22 For example, Keefe et al developed a readiness assessment for road safety interventions that are intended to reduce traffic deaths and serious injuries. 21 Their tool evaluates the current level of concern and action regarding road safety, measures public awareness, attitudes, and perceptions of current road safety initiatives, assesses the role of community leadership, and identifies available resources for road safety efforts.
It is essential to create a readiness assessment specific to Medicaid reimbursement for CVI because of the complicated nature of this policy’s design and implementation, as outlined in prior research. 18 For example, state-level policymaking often involves an array of stakeholders at various levels, which brings its own set of challenges: competing priorities, differential access to resources, and “turf” considerations (ie, when a stakeholder or group of stakeholders feel ownership over the CVI policy and practice spaces). As articulated by Scaccia et al, these factors, which are highly relevant to stakeholders’ motivation and capacity to implement the policy, have important implications for their overall readiness to do so. 23 In addition, Medicaid-covered benefits are administered via a highly bureaucratic and oftentimes opaque system that many new classes of providers (eg, violence prevention professionals, violence intervention specialists) would not consider “user friendly.” As a result, few programs have successfully and consistently billed for services under this policy, citing a lack of guidance as a key concern.
Given the potential negative consequences of an under-resourced CVI ecosystem, it is even more important for states to leverage prior knowledge to “get it right” the first time, preventing unnecessary delays, or setbacks in implementing Medicaid reimbursement for CVI. The public health and implementation science literatures suggest that a well-informed implementation requires the inclusion of relevant stakeholders at all levels, maintains intervention or policy fidelity, and ultimately enhances the long-term sustainability of the model.14,24 The state readiness assessment for funding CVI through Medicaid was designed with consideration of these objectives.
Data and Method
The data used to create the readiness assessment come from a case study of the policy’s implementation across the first 3 states to adopt: Connecticut, California, and Illinois. Guided by a qualitative methodology and the emic perspective 25 , the case study prioritized stakeholders’ experiences to examine the policy in its natural context and provide deep insights enabling a cross-context application of the findings. The case study was approved by the Montclair State University Institutional Review Board (protocol #1103242200) and all research participants provided their informed consent prior to participating in the study. Data collection began on May 1, 2023, and concluded by April 30, 2024.
Data collection for the case study proceeded in 2 stages; in stage 1, the authors identified a sampling frame, systematically reviewed policy documents, and conducted pre-sample meetings with high-level policymakers to gather initial insights on the policy and its implementation. These insights were then used to design a semi-structured interview guide. Stage 2 included semi-structured interviews with high-level policy stakeholders and frontline implementers, with participants providing additional referrals and documentation. Sampling continued until data saturation was achieved (n = 17), at which time the interviews were manually analyzed for emergent categories. 26 The authors groups twenty to two categories into 7 overarching themes across the 3 participating states. Stakeholders confirmed and refined the findings via a member-checking process, enhancing the dependability and trustworthiness of the results. 27 Such collaborations between academic and practitioner/policymaker partners have been recognized as essential for the development of readiness tools in public health. 28
Results: A Readiness Assessment for Funding CVI Through Medicaid
Theoretical Model
We apply the Exploration-Preparation-Implementation-Sustainment (EPIS) framework as the model of theoretical change for the readiness assessment. 29 To our knowledge, no study to date has developed a readiness assessment from this model. In addition to EPIS, the Component Model of Infrastructure (CMI) lends an established evidence base and important supplemental insights on the importance of simultaneously developing a core public health infrastructure, which, as discussed previously, is essential for long-term sustainability in public health. 14
The EPIS framework recognizes that new policies are created and operationalized in distinct phases, each phase bringing its own challenges. In phase 1 (Exploration), stakeholders assess the need for and feasibility of adopting a policy. They then decide whether to adopt, and which adaptations may be needed to fit the policy to their context. It is during this initial phase that stakeholders should begin considering the status of their core public health infrastructure and its implications for implementation. In phase 2 (Preparation), stakeholders identify potential barriers and facilitators of implementation, develop a plan, and identify core infrastructure components to facilitate the use of a policy post-adoption. 22 In phase 3 (Implementation), a policy is enacted, and its implementation is guided by the supports established during the Preparation phase. During this time stakeholders need to monitor implementation and adjust their strategies as needed. In the last phase (phase 4, Sustainment), a policy continues to be used, with adaptations as needed.
The EPIS framework also suggests that there are 4 key components to consider across these phases: the innovation (or policy) factors, the inner and outer contexts of the policy, and the bridging factors between contexts. The EPIS framework is traditionally used to guide the adoption of evidence-based practices within organizational settings; however, it has recently been extended to state-level policy. 30 Continuing this line of inquiry, we apply the EPIS framework to Medicaid reimbursement for CVI in Figure 1 below.
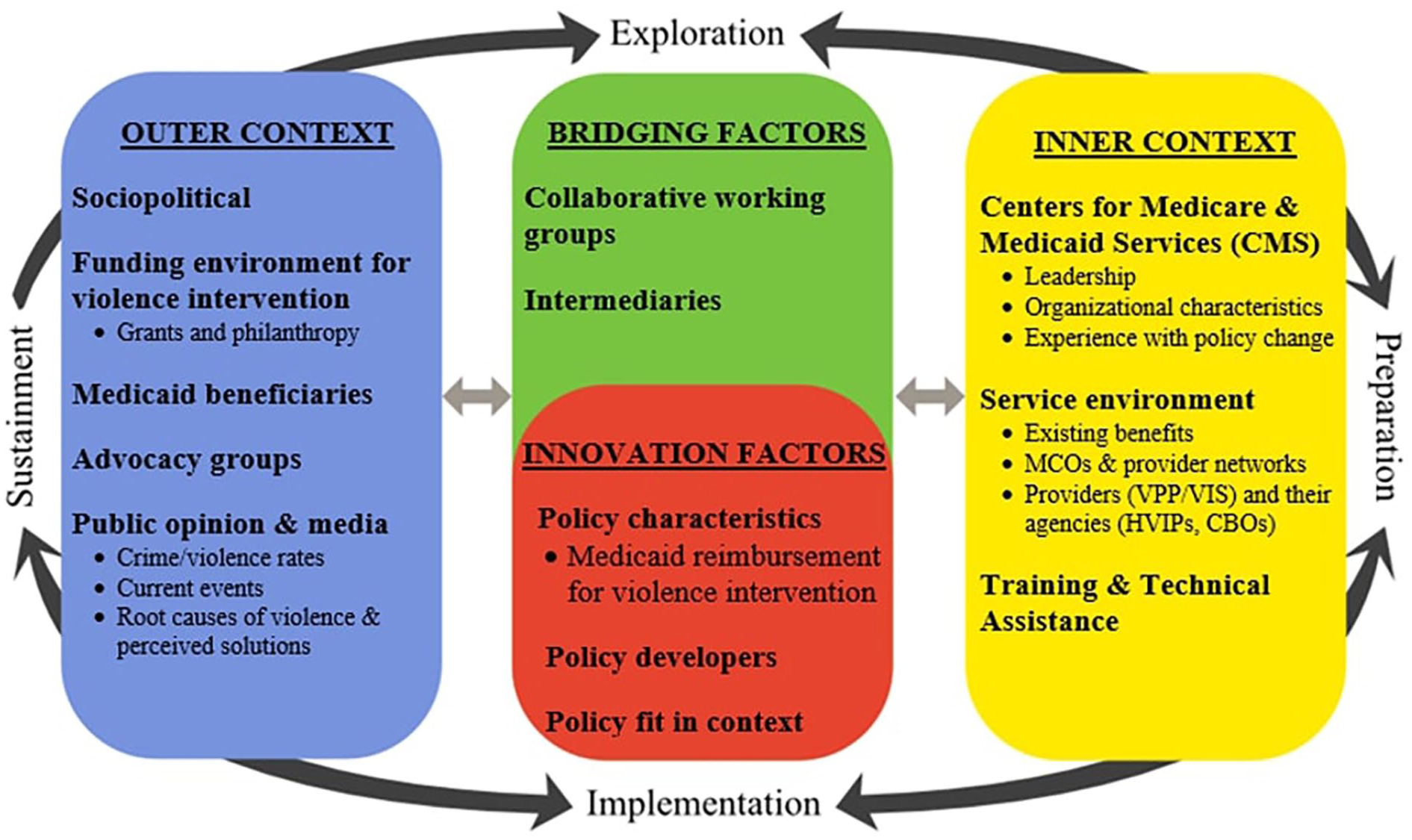
The EPIS framework for the statewide implementation of Medicaid reimbursement for CVI.
Structure and Application of the Readiness Assessment
The goal of the readiness assessment (Table 1) is to leverage prior research to help states successfully implement Medicaid reimbursement for CVI. It is designed for use by policymakers, administrators, and other CVI stakeholders who are considering their role(s) and/or planning to support a Medicaid reimbursement policy in their state. However, the tool is also valuable to those in states that have already adopted the policy, given that the implementation and sustainment phases are often lengthy and ongoing. Specific guidance on the structure and application of the tool appears below Table 1.
The Readiness Assessment.
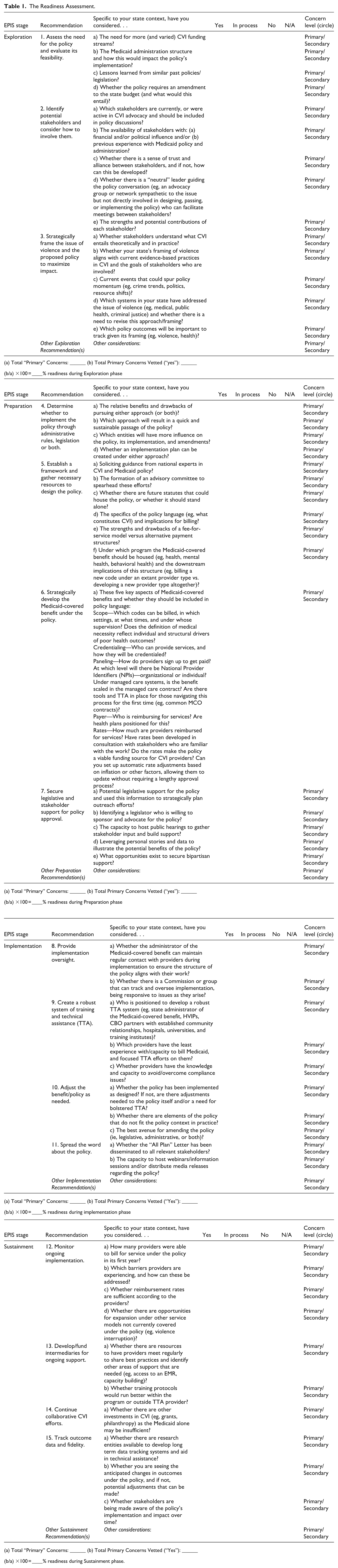
The tool is organized by EPIS phase (ie, exploration, preparation, implementation, and sustainment), and within each phase there are 3 to 4 recommendations listed. Recommendations need not be addressed in the specific order that they are listed; rather, stakeholders may (and perhaps should) address multiple recommendations simultaneously. Within each recommendation there are more specific considerations provided, and these can be ranked by the user according to whether they are “primary” or “secondary” given the state context. Primary considerations are fundamental to the policy’s success, whereas secondary considerations are designated as important and potentially beneficial, but not essential. While the readiness assessment is not yet statistically validated in terms of predicting long-term “success,” we emphasize that the recommendations that target the core components of the CMI, as defined above (ie, multilevel leadership, managed resources, engaged data, responsive plans and planning, and networked partnerships), should take priority. In measuring these evidence-based core components, the sustainability of the policy becomes predictable. 15
Users should focus their initial efforts on the primary considerations but revisit secondary considerations over time. There are 4 columns on the tool for users to indicate whether a given consideration: (1) has been thoroughly vetted (“Yes”), (2) is in the process of being vetted (“In process”), (3) has not yet been vetted (“No”), or (4) does not apply given the state context (“N/A”). A “thorough” vetting is characterized by the following: all relevant stakeholders have reviewed the consideration, provided feedback, identified their role regarding the consideration, and the resources needed to address the consideration.
Notably, there is no scoring threshold to indicate a specific point in which a state is ready to adopt the policy or move into the next phase of implementation; rather, users who have vetted more applicable considerations are better positioned than users who have vetted fewer applicable considerations. Absent scoring thresholds it is suggested that practitioners move forward with the next stage of implementation once all applicable primary considerations have been thoroughly vetted. “Readiness” under this definition might be measured as the proportion of vetted primary considerations to the proportion of un- or under-vetted primary considerations. For example, if a state indicates that they have 9 applicable primary considerations during the Exploration phase but has only thoroughly vetted 7 of these considerations (as indicated by a check in the “yes” column for these 7 items and a check in the “in process” or “no” columns for the remaining 2), then they will have achieved 78% readiness. They should consider thoroughly vetting all applicable primary considerations during a given phase (100% readiness) prior to transitioning to the next.
It is essential that users adapt the tool to their state contexts, as Medicaid—a state-administered Federal program—varies widely across states in terms of administrative structures, norms, and unique CVI ecosystems. Not all recommendations are applicable for each state, and users are encouraged to use the blank space provided at the end of each EPIS phase for their own recommendations and considerations not included in the current tool. The Exploration and Preparation phase recommendations are the most well-informed because the states represented in the case study had recently gone through these stages and were newly entering the Implementation phase. No states at the time of the study had reached the Sustainability phase, though stakeholders provided applicable information that was included in the tool. By including all 4 stages of the EPIS framework in the readiness assessment, however, users have the benefit of foresight in terms of future considerations. As stated previously, careful attention to the recommendations that align with strengthening the core components of public health infrastructure should increase sustainability as these components are rooted in a strong evidence base. 15 Users should reference their progress on specific recommendations and considerations from the tool in process and outcome evaluations for the policy, as these will provide important context for their findings.
Discussion
The state readiness assessment for funding CVI through Medicaid was built using case study data from early policy adopters. They offered many challenges and solutions to effectively implementing Medicaid reimbursement policies for CVI, most of which could be traced back to decisions made during the early phases of policy exploration and planning. These findings highlighted the importance of policy stakeholders thoroughly evaluating a range of factors rooted in the implementation science and public health infrastructure literatures prior to implementation.
This readiness assessment has important implications for bringing sustainability to CVI programs, namely through increasing the likelihood that they: (1) buy into the value of the policy, and (2) become certified providers who successfully and consistently bill for services. Most providers in the first states to adopt the policy have yet to consistently bill for services, and many attribute this to navigating this process with little guidance. Of note, the implementation strategies fundamental to policy success appear to ones that are both identified by the readiness assessment as well as align with core components of public health infrastructure as identified by others. 14 These include multilevel leadership, data collection and surveillance, responsive plans, and networked partnerships. Such strategies and the underlying infrastructure inherent to them allow for programs to continue harnessing data, cultivating champions, and maintaining partnerships so that programs can expand and hit the ground running when opportunities present themselves.
This readiness assessment should be considered in light of its limitations—namely, that it is based on data from only the first 3 states to implement the policy and is not yet validated to predict policy “success.” As such, the assessment does not likely include every relevant policy consideration, and the recommendations in the first 2 phases, Exploration and Preparation, are better informed than the latter 2. Future research should continue to develop the Implementation and Sustainment phases of the tool as states are bound to develop new and important knowledge as they continue to implement the policy over time. Even despite these limitations, this tool provides timely guidance for implementers given recent and sudden changes to the CVI funding landscape. While the tool was developed using data from a study that employed rigorous qualitative methods, future research can increase the tool’s validity through quantitative validation methods and through the inclusion of data from additional states.
CVI stakeholders need not navigate the implementation process alone, nor should this tool be the sole guidance for implementation. National experts in policy implementation for CVI (eg, the Health Alliance for Violence Intervention, Center for Healthcare Strategies, Giffords Center for Violence Intervention) regularly develop and disseminate guidance and technical assistance resources for using Medicaid to fund CVI. States that leverage multiple resources while preparing to adopt the policy will be better situated for a successful rollout, which has immediate implications for establishing new providers and successful billing/reimbursement, and downstream implications for CVI program sustainability.
Conclusion
With recent spikes in gun violence across American cities, CVI programs are charged with intervening to reduce violence and its associated harms. This is a monumental task in the face of inconsistent and insufficient funding. Medicaid reimbursement for CVI provides 1 avenue through which some states are increasing programmatic funding and sustainability. However, the complicated and often lengthy process associated with designing, adopting, and implementing a new Medicaid-covered benefit can seem insurmountable, and a lack of guidance during this time can contribute to reduced uptake of the policy. Readiness assessments that are rooted in implementation science and evidence-based concepts from the public health infrastructure literatures can help stakeholders to effectively implement the policy, measure its implementation, promote its long-term success, and foster an ecosystem that is better equipped to sustainably address community violence.
Footnotes
Ethical Considerations
Consent to Participate
All study participants provided their informed consent (see IRB protocol number above) prior to participating in the study.
Author Contributions
All authors contributed to the conceptualization and writing/editing of this paper. CS, SR, and KP contributed to the underlying case study data collection and analysis.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data from the underlying case study are not available for distribution.
