Abstract
Nurses in intensive care units (ICUs) face high levels of stress and emotional challenges, making it essential to understand the factors that influence their professional quality of life (ProQoL). This study aimed to investigate the relationship between work environment factors and ProQoL, particularly focusing on burnout, compassion satisfaction, and secondary traumatic stress, among ICU nurses. The Professional Quality of Life (ProQoL) Scale was used to measure these aspects, with an emphasis on the importance of a supportive work environment for enhancing staff well-being and organizational performance. This cross-sectional study was conducted between March and August 2024, involving 162 ICU nurses from hospitals in the southern West Bank. A stratified random sampling method was employed to ensure representativeness. Data collection involved surveys covering socio-demographic information, the Practice Environment Scale-Nursing Work Index (PES-NWI), and the ProQoL scale. Statistical analyses, including descriptive statistics and Pearson correlation, were performed using SPSS. The participants were predominantly young, with 61.7% less than 30 years old, and 65.4% were male. Most held a bachelor’s degree (54.9%). The survey indicated that the majority reported average levels of compassion satisfaction (90.7%), burnout (91.4%), and secondary traumatic stress (85.2%). The analysis showed that a moderately positive practice environment was significantly associated with lower levels of burnout and higher levels of compassion satisfaction. Additionally, there was a significant difference in mean Compassion Satisfaction scores according to sleep hours (F = 5.475, P < .05). Nurses who slept more than 8 h had significantly higher Compassion Satisfaction compared to those who slept less than 8 h or exactly 8 h (P < .05). ICU nurses generally perceived their work environment positively, though there are opportunities to improve their professional quality of life, particularly by addressing burnout. The findings highlight the need for targeted interventions and further research to enhance job satisfaction and well-being among ICU nurses.
Keywords
The professional quality of life (ProQoL) for nurses, particularly in high-stress environments like intensive care units (ICUs), is influenced by factors such as burnout, compassion satisfaction, and secondary traumatic stress. The work environment plays a crucial role in shaping these experiences, impacting nurse well-being, job satisfaction, and patient care outcomes.
This research provides a deeper understanding of the specific elements within the ICU work environment that affect ProQoL. By identifying the key factors that contribute to burnout, compassion satisfaction, and secondary traumatic stress, the study offers valuable insights for targeted interventions aimed at improving the well-being of ICU nurses and enhancing the quality of care they provide.
The findings have significant implications for nursing practice, organizational policies, and future research. They underscore the importance of fostering a supportive work environment in ICUs to mitigate burnout and secondary traumatic stress while enhancing compassion satisfaction. These insights can inform the development of policies and interventions designed to improve nurse well-being and patient outcomes, and contribute to theoretical models that explain the relationship between work environment factors and professional quality of life in high-stress settings.
Introduction
The worldwide nursing shortage, highlighted by the World Health Organization, 1 presents a critical challenge, particularly in areas with growing healthcare demands. This shortage jeopardizes the dignity and well-being of nurses, posing a significant issue for healthcare systems globally. Nursing is deeply grounded in the provision of holistic care, with an emphasis on cultivating strong nurse-patient relationships to improve health outcomes and overall well-being. 2 These relationships enable nurses to meet professional standards effectively, contributing to successful treatment outcomes and enhanced satisfaction for both nurses and patients.
Compassion, understood as the ability to empathize with and support others, is a fundamental aspect of nursing. In high-pressure settings such as intensive care units (ICUs), compassion plays a crucial role in shaping nurses’ professional quality of life (ProQoL). 3 ICUs, characterized by their intense and often traumatic environments require nurses to navigate complex emotional and ethical challenges, which directly impact their ProQoL.
The ProQoL scale measures Compassion Satisfaction (CS) and Compassion Fatigue (CF), where CS reflects the fulfillment derived from helping others, and CF encompasses burnout (BO) and secondary traumatic stress (STS). BO is associated with chronic workplace stress, leading to fatigue, cynicism, and diminished efficacy, while STS arises from exposure to patients’ traumatic experiences.4,5
The Nursing Work Environment (NWE), including factors such as staffing, management support, and work culture, is essential in understanding ProQoL, especially within the ICU context. Kanter’s Theory of Structural Empowerment suggests that work environments providing access to information, resources, support, and opportunities are key to enhancing nurses’ satisfaction and effectiveness. 6 A Healthy Work Environment (HWE) promotes patient safety, staff satisfaction, and the overall success of healthcare organizations.7,8 Given the high-stress nature of ICUs, the impact of NWE on ProQoL is profound. 9
While previous research has explored ProQoL among healthcare professionals, this study specifically focuses on ICU nurses, whose work environments are often more demanding due to the high-acuity patients they care for.10,11 This study aims to investigate ProQoL among ICU nurses, focusing on the relationship between their work environment and its influence on BO, STS, and CS. By employing Kanter’s Theory of Structural Empowerment, the study seeks to identify factors that contribute to burnout and secondary traumatic stress, with the goal of developing strategies to enhance ICU nurses’ well-being.
Review of Literature
The concept of Professional Quality of Life (ProQoL) is central to understanding the well-being of healthcare professionals, particularly within the nursing field. ProQoL encompasses both positive and negative aspects of a nurse’s experience, distinguishing between Compassion Satisfaction (CS) and Compassion Fatigue (CF). CS reflects the positive feelings derived from helping others, whereas CF includes 2 components: Burnout (BO) and Secondary Traumatic Stress (STS).4,12 Burnout (BO) involves emotional exhaustion, depersonalization, and a diminished sense of personal accomplishment, typically resulting from prolonged exposure to stress in demanding work environments. STS arises from direct exposure to traumatic events and can affect nurses emotionally and mentally, particularly in ICU settings.13,14
Research indicates that BO typically develops progressively due to chronic stress and job demands over an extended period, whereas STS can emerge more abruptly, often triggered by distressing or traumatic events involving patient care.15,16 This differentiation highlights the varying onset patterns and underlying mechanisms of these conditions. Understanding these differences is critical when addressing the professional quality of life of ICU nurses, as their unique work environment may expose them to both BO and STS. 17
The Nursing Work Environment (NWE) plays a critical role in influencing ProQoL. The International Organization for Standardization emphasizes that a supportive and well-structured NWE can enhance job satisfaction and reduces burnout; thereby positively affecting overall ProQoL. 7 This highlights the importance of optimizing the NWE for better outcomes in healthcare. NWE encompasses various factors, including physical conditions, organizational structures, social interactions, and cultural elements. Kanter’s Theory of Structural Empowerment suggests that work environments that provide access to resources, support, information, and opportunities for growth empower nurses and contribute to improved job satisfaction and effectiveness. 6
Previous studies have shown that positive work environments are strongly associated with lower levels of burnout and secondary traumatic stress among nursing staff. Additionally, such environments contribute to higher levels of compassion satisfaction (CS), which reflects improved emotional well-being and job satisfaction among nurses.13,17
The Intensive Care Unit (ICU) is particularly stressful due to the high acuity of patients and the emotionally charged nature of the work. ICU nurses are frequently exposed to life-threatening conditions, which can lead to increased job dissatisfaction, emotional exhaustion, and high levels of BO and STS.11,14 Studies have demonstrated that the demands of ICU environments can negatively impact nurses’ ProQoL, making it crucial to explore the interactions between these components in ICU settings. 18
However, despite the known challenges of ICU settings, research focusing on the specific interactions between ProQoL components and the Nursing Work Environment (NWE) remains limited.³ This gap in the literature underscores the need for targeted studies aimed at understanding and improving ProQoL among ICU nurses, with the ultimate goal of developing interventions to enhance their work environment and overall well-being.
Methodology
Design
This study employed a cross-sectional design, targeting nurses employed in Intensive Care Units (ICUs) across hospitals in the southern West Bank during the period from March to August 2024. The cross-sectional approach was selected for its ability to examine the relationship between the work environment and Professional Quality of Life (ProQoL) at a single time point. This design is particularly effective for identifying associations and generating hypotheses for future research, as it does not require prolonged follow-up, making it well-suited for analyzing variables within the dynamic ICU work environment.
Population and Sampling
The study focused on a population of over 194 nurses working in ICUs within the West Bank. The required sample size was calculated using the Raosoft online tool, based on parameters including a 5% margin of error, a 95% confidence interval, and an assumed response rate of 50%. The calculated sample size was 130, which was increased to 162 to account for potential attrition.
A stratified random sampling method was employed, ensuring that each hospital’s ICU contributed proportionately to the total sample size. The selection of hospitals was based on criteria such as size, ICU capacity, and geographic distribution within the region. The sampling frame consisted of a comprehensive list of ICU nurses, obtained from nurse managers at the selected hospitals.
The study included all nurses working in the selected ICUs during the data collection period, excluding those on medical leave, vacation, or other forms of absence. Part-time nurses and those on rotating shifts were excluded to maintain consistency in the assessment of ProQoL, as these factors could significantly impact the results.
Instruments
The research utilized a structured questionnaire comprising the following sections:
Socio-Demographic Information: This section collected data on variables such as age, gender, education level, work experience, shift type, and sleep hours. These variables were selected for their known influence on both the work environment and ProQoL. For instance, work experience and shift type are factors that can affect job satisfaction.
The Practice Environment Scale of the Nursing Work Index (PES-NWI), developed by Lake, 19 is widely used to assess nursing practice environments, identifying factors that either support or hinder high-quality care. 20 The tool consists of 31 items across 5 subscales and uses a 4-point Likert scale, where higher scores reflect more favorable environments. Endorsed by U.S. healthcare organizations, the PES-NWI is recognized as a key measure for improving nursing care, with a reliability range of .71-.84.21,22
The Professional Quality of Life Scale (ProQOL) Version 5 measures compassion satisfaction, burnout, and secondary traumatic stress through 30 items distributed across 3 subscales. 23 Using a 5-point Likert scale, respondents rate their experiences over the last 30 days, with scores categorized into low, average, or high levels. 24 In this study, Cronbach’s alpha for compassion satisfaction, burnout, and secondary traumatic stress were .88, .84, and .90, respectively, while the PES-NWI showed an alpha of .88, confirming high reliability. 25
The validity of both the ProQOL and PES-NWI in this study was assessed through an expert panel review. Nursing and psychometric experts evaluated the cultural and contextual relevance of the scales for the Palestinian healthcare setting, ensuring that the content, language, and applicability were appropriate for ICU nurses in Palestine. The feedback confirmed content validity, indicating that the instruments accurately reflected the work environment and professional quality of life in the region. Reliability was further confirmed by high Cronbach’s alpha values for compassion satisfaction (.88), burnout (.84), secondary traumatic stress (.90), and the overall PES-NWI (.88). While no prior psychometric validation studies of these tools had been conducted in Palestine, the expert panel’s assessment establishes a foundation for their construct validity in this context.
Data Collection
The study received ethical approval from the Institutional Review Board (IRB) of Palestine Ahliya University. The researcher coordinated with nurse managers at each hospital to obtain a list of ICU nurses and explain the study’s objectives. Nurses who agreed to participate provided informed consent, with participation being entirely voluntary and without impact on their professional standing.
The questionnaires were self-administered in English at the respective hospitals. To ensure anonymity and confidentiality, the researcher coded the questionnaires and securely stored the data. Given the sensitive nature of the ProQoL assessment in an ICU setting, measures were taken to minimize potential distress, including providing contact information for counseling services if needed.
Ethical Considerations
Ethical approval for this study was obtained from Palestine Ahliya University (CAMS/BSN/6/1228). Written informed consent was obtained from all subjects before the study. Participation was entirely voluntary, and participants were assured that their responses would remain confidential. Anonymity was maintained throughout the study, with all data being securely stored.
Data Analysis
Data analysis was performed using SPSS version 23. 26 Descriptive statistics were employed to summarize the data, including frequencies and percentages for categorical variables, and means and standard deviations for continuous variables. The socio-demographic variables were also analyzed in relation to the ProQoL scores to identify any significant patterns or correlations. Pearson correlation analysis was conducted to assess the strength and direction of relationships between continuous variables. Prior to the analysis, assumptions of normality, linearity, and homoscedasticity were checked to ensure the validity of the results. This study followed the relevant EQUATOR guidelines for cross-sectional studies and adhered to the appropriate checklist for reporting.
Results
Participants’ Characteristics
A total of 162 nurses participated in the study (see Table 1). The majority were 30 years old or younger (N = 100, 61.7%), and most were male (N = 106, 65.4%). Educational levels varied, with over half holding a bachelor’s degree (N = 89, 54.9%). Regarding work experience, the majority had less than 5 years of experience (N = 121, 74.7%). Most participants (N = 107, 66.0%) worked rotation shifts, and nearly half reported sleeping 8 h per night (N = 78, 48.1%).
Demographic Characteristics of the Participants (N = 162).

The distribution of participants based on their Professional Quality of Life (ProQoL) levels (see Table 2) revealed that most participants had average levels of Compassion Satisfaction (CS) (N = 147, 90.7%), with only a small proportion reporting low (N = 7, 4.3%) or high (N = 8, 4.9%) levels. Similarly, the majority of participants had average levels of Burnout (BO) (N = 148, 91.4%), with a minority reporting low levels (N = 14, 8.6%) and none reporting high levels. In terms of Secondary Traumatic Stress (STS), most participants were in the average range (N = 138, 85.2%), with a notable minority reporting low levels (N = 23, 14.2%) and very few experiencing high levels (N = 1, 0.6%).
Distribution of Participants Based on Level of Professional Quality of Life.

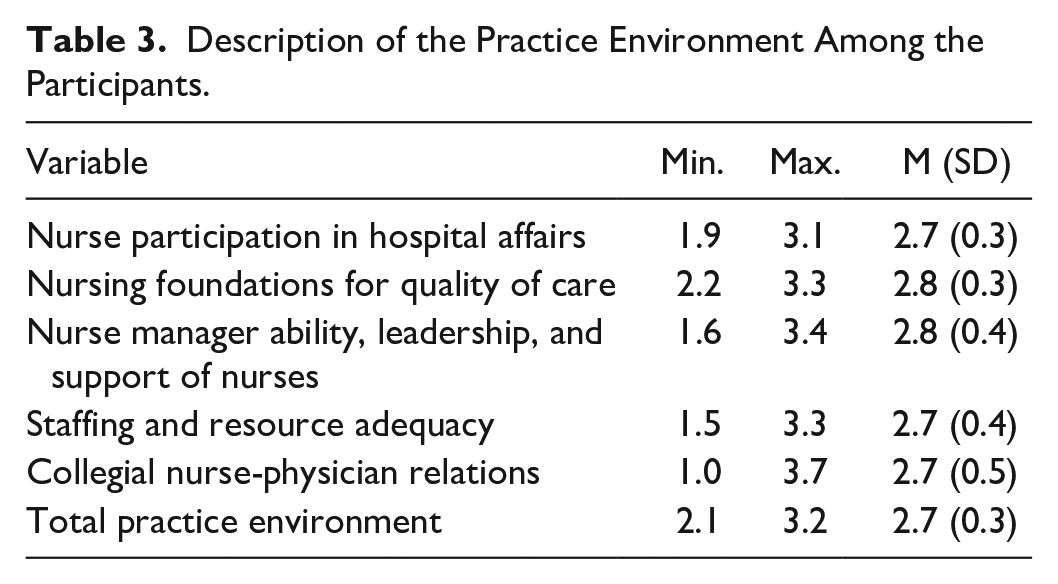
The overall practice environment score ranged from 2.1 to 3.2, with a mean of 2.7 (SD = 0.3), indicating a moderately favorable setting for the participants (see Table 3). Specific domains within the practice environment showed varying levels of favorability: Nurse Participation in hospital affairs had a mean of 2.7 (SD = 0.3), reflecting moderate involvement; Nursing Foundations for Quality of Care scored a mean of 2.8 (SD = 0.3), indicating a high foundation; Nurse Manager Ability, leadership, and support of nurses also scored highly with a mean of 2.8 (SD = 0.4). However, Staffing and Resource Adequacy scored slightly lower with a mean of 2.7 (SD = 0.4), pointing to moderate adequacy. Collegial nurse-physician relations had a relatively higher mean of 2.7 (SD = 0.5), indicating good interprofessional relationships.
Description of the Practice Environment Among the Participants.
As shown in Table 4, higher nurse participation in hospital affairs was found to be negatively correlated with burnout (r = −.32, P = .001). Similarly, Nursing Foundations for Quality of Care demonstrated a significant negative relationship with burnout (r = −.39, P = .001), as did Nurse Manager Ability, Leadership, and Support of Nurses (r = −.30, P = .001). Adequate Staffing and Resource Adequacy were postable
Relationship between Practice Environment and Professional Quality of Life among the Participants.

Significant at the .05 level.
Significant at the .01 level.
itively correlated with Compassion Satisfaction (r = .21, P = .007) and inversely related to burnout (r = −.29, P = .001). Furthermore, Collegial nurse-physician relations were positively associated with Compassion Satisfaction (r = .21, P = .007) and had a significant negative correlation with burnout (r = −.40, P = .001). Additionally, the overall practice environment score showed a positive correlation with Compassion Satisfaction (r = .18, P = .024) and a strong negative correlation with burnout (r = −.44, P = .001).
The analysis showed a significant difference in the mean Compassion Satisfaction scores according to sleep hours (F < 5.475, P < .05). The post hoc test indicated that nurses sleep more than 8 hours had significantly more Compassion Satisfaction compared to those sleep less than 8 hours and 8 hours (P < .05), as outlined in Table 5.
Difference in the Main Study Variables’ Scores According to Demographic Characteristics.

= P < .05, ** = P < .01.
Discussion
This study provides valuable insights into how the work environment impacts the professional quality of life (ProQoL) for ICU nurses, focusing on critical aspects that affect their overall well-being. The demographic profile of the study cohort reveals a predominantly young nursing workforce, with 61.7% of participants aged 30 years or younger. This observation is consistent with global trends toward a younger nursing workforce, as noted by Liu et al.27,28 Interestingly, the study uncovers a higher proportion of male participants (65.4%), which deviates from the traditionally female-dominated nursing profession. This deviation may reflect regional or institutional factors influencing gender distribution within the nursing workforce.
Educational levels among participants show that 54.9% hold a bachelor’s degree, underscoring a trend toward advanced nursing education aimed at improving patient care standards, as supported by Porat-Dahlerbruch. 29 This trend toward higher education reflects a broader commitment to enhancing the quality of care through improved knowledge and skills among nursing professionals.
The ProQoL analysis in this study indicates that the majority of nurses fall within the average range for burnout (BO), secondary traumatic stress (STS), and compassion satisfaction (CS). Specifically, 91.4% of participants report average BO levels, and 90.7% report average CS levels. These findings suggest that while nurses generally experience satisfaction with their caregiving roles, they are also susceptible to moderate levels of burnout. These results are consistent with earlier research by Cocker et al, 4 which also found that moderate burnout is common among nursing staff.
One key finding in this study was the lack of a significant relationship between Nursing Work Environment (NWE) and Secondary Traumatic Stress (STS). This may be explained by the unique nature of STS, which is typically linked more closely to exposure to traumatic patient events rather than structural or environmental workplace factors. STS can develop rapidly following specific incidents, making it less dependent on the broader NWE elements like nurse participation or staffing adequacy. Future studies should explore whether acute care settings or specific patient interactions are stronger predictors of STS, beyond general workplace conditions.
The study’s report of a relatively positive practice environment may serve as a protective factor, as evidenced by the very low percentage of participants reporting significant degrees of BO (0%) and STS (0.6%). These results align with findings from Hooper et al, 30 who noted similar trends in protective work environments.
Significant negative correlations were observed between various aspects of the practice environment and burnout. Notably, nurse participation in hospital affairs (r = −.32, P = .001) and the quality of nursing care foundations (r = −.39, P = .001) were inversely related to burnout. This finding underscores the importance of these factors in mitigating burnout, supporting the notion that increased involvement in decision-making and a strong foundation for quality care are crucial in reducing burnout. These results are consistent with the work of Laschinger et al., 31 who highlighted the significance of such factors in nursing practice.
Collaborative interprofessional relationships are also vital for reducing occupational stress, and the study found a substantial negative correlation between collegial nurse-physician relations and burnout (r = −.40, P = .001). This finding aligns with O’Leary et al., 32 who emphasized the role of positive professional relationships in mitigating stress among healthcare providers.
To enhance ProQoL, particularly in reducing burnout, healthcare organizations should focus on fostering strong nurse-physician interactions, ensuring adequate staffing and resources, and promoting active nurse participation in hospital decision-making. The significant positive correlation between the total practice environment score and compassion satisfaction (r = .18, P = .024) further emphasizes the need for a comprehensive approach to improving the work environment. This approach is consistent with the recommendations of Kutney-Lee et al, 33 who advocated for holistic improvements to the work environment to enhance overall ProQoL.
Despite its valuable insights, this study has limitations. The cross-sectional design limits the ability to establish causal relationships between the practice environment and ProQoL. Future research employing longitudinal studies could provide a deeper understanding of these correlations over time. Additionally, exploring these dynamics across various healthcare environments or geographical areas could offer a more comprehensive view of the factors influencing nurses’ work-related quality of life.
Strengths and Limitations
Strengths
This study provides a comprehensive analysis of professional quality of life (ProQoL) among ICU nurses, including compassion satisfaction (CS), burnout (BO), and secondary traumatic stress (STS), offering a holistic view of their work experiences; identifies significant correlations between various aspects of the practice environment and ProQoL outcomes, such as the impact of nurse participation and interprofessional relationships on burnout and job satisfaction; benefits from a high response rate and a diverse sample, enhancing the generalizability of the findings to similar healthcare settings; and delivers recent and relevant insights into the practice environment and its effects on ProQoL, reflecting current trends and conditions in the healthcare sector.
Limitations
The cross-sectional design of the study restricts the ability to establish causal relationships between the practice environment and ProQoL, capturing only a snapshot in time without accounting for changes over time; the sample may be influenced by regional or institutional factors affecting gender distribution and practice environments, limiting generalizability to other settings; the use of self-reported measures for ProQoL and practice environment variables may introduce response bias, with participants potentially providing socially desirable responses; and while several key aspects of the practice environment are examined, other potentially influential factors, such as organizational culture and management styles, are not addressed, which could offer a more comprehensive understanding of ProQoL.
Recommendations
Healthcare organizations should enhance supportive work environments by fostering positive nurse-physician interactions, ensuring adequate staffing, and providing resources that support nurses’ well-being; increase nurse participation in hospital decision-making and quality care initiatives, as higher involvement is linked to lower burnout; promote professional development and continuous training for ICU nurses to improve skills and resilience, mitigating burnout and stress; conduct longitudinal research to understand how changes in the practice environment affect ProQoL over time and identify long-term strategies; explore diverse healthcare settings and geographical locations to gain a comprehensive understanding of ProQoL factors and context-specific issues; and expand research to include additional practice environment factors such as organizational culture, leadership styles, and administrative support to provide a more complete picture of their impact on ProQoL.
Conclusion
In conclusion, this study highlights the vital importance of fostering a supportive and collaborative practice environment to enhance nurses’ Professional Quality of Life (ProQoL), particularly in the demanding settings of intensive care units (ICUs). By addressing the identified factors such as managerial support, adequate staffing, and collegial relationships, healthcare organizations can significantly improve job satisfaction among nurses, reduce burnout, and ultimately contribute to better patient care outcomes. These findings emphasize the need for targeted interventions and ongoing efforts to create a work environment that supports the well-being and professional growth of ICU nurses.
Footnotes
Acknowledgements
The authors would like to express their thanks to the nurses who participated in the study
Authors contributions
“AA initiated the study and collected the data. AA, along with MAE, drafted the manuscript and approved the final version submitted for publication. IA, MAE, and MF agree to be accountable for all aspects of the work, ensuring that questions related to accuracy or integrity are appropriately addressed and resolved. AB, IA, and MF made significant contributions to the design, analysis, and interpretation of the data for this study. Additionally, AB, IA, and MF provided critical revisions to the manuscript for important intellectual content. IA have reviewed and approved the final version submitted for publication. IA also agrees to be accountable for all aspects of the work, ensuring that any questions related to accuracy or integrity are properly investigated and resolved.”
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate
Ethical approval for this study was obtained from Palestine Ahliya University (CAMS/BSN/6/1228). Written informed consent was obtained from all subjects before the study.
Consent for Publication
We affirm that this work is original and has not been published elsewhere, except as noted in the manuscript.
