Abstract
The “Leave No One Behind” (LNOB) principle, a fundamental commitment of the United Nations’ Sustainable Development Goals, emphasizes the urgent need to address and reduce global health inequalities. As global health initiatives strive to uphold this principle, they face significant ethical challenges in balancing equity, resource allocation, and diverse health priorities. This narrative review critically examines these ethical dilemmas and their implications for translating LNOB into actionable global health strategies. A comprehensive literature search was conducted using PubMed, Scopus, Web of Science, and Semantic Scholar, covering publications from January 1990 to April 2024. The review included peer-reviewed articles, gray literature, and official reports that addressed the ethical dimensions of LNOB in global health contexts. A thematic analysis was employed to identify and synthesize recurring ethical issues, dilemmas, and proposed solutions. The thematic analysis identified 4 primary ethical tensions that complicate the operationalization of LNOB: (1) Universalism versus Targeting, where the challenge lies in balancing broad health improvements with targeted interventions for the most disadvantaged; (2) Resource Scarcity versus Equity; highlighting the ethical conflicts between maximizing efficiency and ensuring fairness; (3) Top-down versus Bottom-up Approaches, reflecting the tension between externally driven initiatives and local community needs; and (4) Short-term versus Long-term Sustainability, addressing the balance between immediate health interventions and sustainable systemic changes. To navigate these ethical challenges effectively, global health strategies must adopt a nuanced, context-sensitive approach incorporating structured decision-making processes and authentic community participation. The review advocates for systemic reforms that address the root causes of health disparities, promote equitable collaboration between health practitioners and marginalized communities, and align global health interventions with ethical imperatives. Such an approach is essential to truly operationalize the LNOB principle and foster sustainable health equity.
Keywords
The “Leave No One Behind” (LNOB) principle is a key goal within the United Nations’ Sustainable Development Goals, emphasizing the reduction of health inequalities. However, achieving LNOB in global health has been challenging due to ethical dilemmas, such as balancing equity with resource scarcity and varying capacities of health systems to implement inclusive policies.
This research critically explores the ethical and practical challenges of operationalizing the LNOB principle in global health. It introduces structured decision-making processes and robust community participation as essential strategies to navigate these ethical tensions, advancing health equity and informing more inclusive global health practices.
The review underscores the need for a nuanced approach to global health equity, advocating for systemic reforms prioritizing ethical frameworks and meaningful community involvement. These insights can inform the development of participatory methods and policies, influencing future global health initiatives to better address disparities and empower marginalized communities.
Introduction
The United Nations’ 2030 Agenda for Sustainable Development includes a pivotal commitment to “Leave No One Behind” (LNOB), central to Goal 10 of the Sustainable Development Goals (SDGs). 1 This principle emphasizes addressing inequalities marginalizing individuals and communities, particularly those traditionally excluded from progress. 2 Rather than focusing solely on national averages, LNOB advocates for reaching the “furthest behind first,” highlighting the need for targeted strategies that address intersecting factors like poverty, gender, disability, ethnicity, and geography, contributing to health disparities. 3 These principles call for a transformative approach to global health, aiming for both widespread improvement and targeted support for the most vulnerable.
Despite these commitments, achieving global health equity remains fraught with challenges. Marginalized populations continue to experience disproportionate disease burdens and limited access to healthcare.4,5 Health inequities are particularly acute in conflict zones, where violence disrupts healthcare services, increases preventable illnesses, and undermines access to essential resources like clean water and sanitation.6,7 Vulnerable groups, including women, children, and the elderly, are especially affected by malnutrition and untreated mental health conditions in these settings.8-15 Climate change further exacerbates these disparities, with extreme weather events disproportionately impacting marginalized communities by amplifying diseases like malaria and dengue fever and worsening food insecurity.16-20 The intersection of conflict, migration, and climate change creates a cycle of vulnerability perpetuating health inequities.21,22
Efforts to address these disparities through global health initiatives often encounter complex ethical dilemmas. Ensuring equitable, effective, and sustainable interventions requires a nuanced understanding of ethical considerations related to equity, resource allocation, community participation, and long-term sustainability.23-28 Navigating these challenges demands technical expertise and a steadfast commitment to social justice and cultural sensitivity, pushing global health efforts toward more just and inclusive solutions.
This literature review examined 3 critical questions to understand the ethical and practical dimensions of the LNOB approach in global health. First, it explores the inherent tensions between the ethical imperative of the LNOB and the practical realities of implementing international health programs. What are the challenges in ensuring equitable health access and outcomes, and how do existing health systems and policies support or hinder this ethical mandate? Second, this review considers whether a structured decision-making process can facilitate more equitable resource allocation in global health. Can a systematic approach align resource distribution more closely with the LNOB pledge, addressing health access and outcomes disparities? Third, it investigates the role of meaningful participation by marginalized communities in mitigating ethical tensions and ensuring that global health projects adhere to the LNOB principle. How does including these communities in planning and decision-making impact health interventions’ effectiveness and ethics?
Methods
A structured search strategy was conducted to review the literature on the ethical implications of the LNOB principle in global health. Searches were performed across PubMed, Scopus, Web of Science, and Semantic Scholar databases, using keywords and MeSH terms such as “Global Health,” “Ethics,” “ Social Determinants of Health,” “Health Equity,” “ Universal Health Insurance,” and “Sustainable Development.” The search was limited to English-language publications from January 1990 to April 2024.
Articles were included if they discussed ethical challenges, frameworks, or strategies related to LNOB in health and consisted of peer-reviewed articles, gray literature, or official reports. Exclusion criteria were non-English articles, non-health-focused studies, and opinion pieces. Screening involved initial title and abstract checks for relevance, followed by full-text reviews of selected articles. References of included studies were also reviewed to identify additional relevant literature.
The review employed a thematic analysis guided by a theoretical framework of health equity and justice, focusing on aligning global health initiatives with ethical imperatives to leave no one behind.29-32 This approach involved identifying and synthesizing key themes related to ethical challenges, proposed solutions, and the impact of strategies on marginalized populations.
Operationalizing “Leaving No One Behind”
Universalism Versus Targeting
Operationalizing the LNOB principle requires balancing universal health goals with the specific needs of marginalized groups. Rather than viewing universalism and targeting as opposing strategies, they should be considered complementary tools on a spectrum, adaptable to different contexts to achieve true health equity. A context-specific, community-driven approach, informed by ethical principles, can help global health practitioners navigate these complexities and work toward a world where socioeconomic or demographic circumstances do not determine health outcomes. However, putting these principles into practice reveals a dilemma between universalism and targeting: How can we balance the goal of improving health for everyone with the need to prioritize those who are most disadvantaged?
LNOB challenges policymakers, clinicians, and researchers to move beyond national averages to address disparities in health outcomes for marginalized populations. This creates a tension between universalism—aiming for health improvements for all—and targeting, which prioritizes those most disadvantaged. Universal Health Coverage (UHC) is often viewed as more equitable, reducing stigma and fragmentation compared to targeted programs.33-35 However, a purely universal approach may overlook the specific barriers faced by marginalized groups, such as social discrimination, geographic isolation, and extreme poverty, potentially conflicting with LNOB’s intent.36-42 Without targeted interventions, universal programs could inadvertently exacerbate existing disparities.43-45
Conversely, focusing solely on specific marginalized groups through targeted interventions can lead to inequities among other vulnerable populations who do not receive targeted support. This challenge becomes more pronounced in resource-limited settings where allocation decisions are tough. Over-reliance on targeted programs may also neglect the broader structural changes needed for sustainable improvements in health equity.46,47
A nuanced approach to resolving this tension is “proportionate universalism,” which combines universal health goals with targeted strategies proportionate to the level of disadvantage experienced. This could involve universal access to essential healthcare services, supplemented by targeted support like transportation vouchers, culturally tailored outreach, or language assistance for those most in need.48-51 Effective implementation of this approach requires a deep understanding of local contexts. Community-based participatory research (CBPR) can help identify the specific needs of those “furthest behind,” the barriers they face, and the potential unintended consequences of various interventions. 52 Balancing immediate efforts to alleviate suffering with long-term strategies to address the root causes of health inequities is essential for achieving sustainable health equity.
Resource Scarcity Versus Equity
The aspiration to LNOB faces the stark reality of limited resources in global health, presenting profound ethical dilemmas: How, with finite budgets, personnel, and technology, can we ensure the most marginalized benefit without sacrificing overall health gains for the broader population?
The ethical imperative of equity in healthcare requires that those facing the greatest disadvantages receive the necessary support to reduce health disparities. This often necessitates disproportionate funding for intensive interventions targeting marginalized groups in remote or high-need areas, such as providing antiretroviral therapy for HIV-positive individuals in remote settings.53-55 Although such measures may not be cost-efficient, they are essential from an equity standpoint. Research supports this approach, emphasizing the importance of targeted funding in areas like reproductive, maternal, and child health and the need to strengthen health systems and digital health services to reduce disparities.56-59
On the other hand, prioritizing efficiency in healthcare often means focusing on interventions that maximize health benefits for the largest number of people, favoring simpler and less costly initiatives. While this approach may achieve greater short-term returns on investment, it risks neglecting the most marginalized, who require sustained, often more expensive, support, potentially worsening health disparities.60-66 While strategies like linear programing models and cost-effectiveness thresholds can help optimize resource allocation, they may not always align with equity-focused public preferences, especially in low- and middle-income countries where failing to prioritize high-value healthcare interventions can exacerbate inequities.67-70
These competing priorities—equity and efficiency—pose significant ethical challenges for global health practitioners. Allocating resources solely based on equity could overwhelm limited programs while focusing only on efficiency risks perpetuating health disparities and denying essential care to those most in need. 71 To navigate this tension, decision-making must be guided by ethical frameworks that consider principles such as fairness, need, and potential benefits to ensure transparency and avoid arbitrary choices. 72 True efficiency should encompass long-term social and economic benefits, recognizing the broader societal gains from investing in marginalized populations’ health. 73
Addressing resource constraints while operationalizing LNOB also requires advocating for increased global health funding. Wealthy nations and institutions are ethically obligated to commit more resources to address the root causes of health disparities. Additionally, innovative approaches like cost-effective technologies, streamlined service delivery models, and new financial instruments, such as AI-driven health policy frameworks and Health Equity Bonds, can help maximize limited resources while prioritizing equity.74-83
AI-Driven Health Policy Frameworks for Dynamic Adaptation: The development of AI-driven health policy frameworks has been proposed to ensure that global health policies remain adaptive to rapidly changing population health dynamics.84-88 These frameworks (Figure 1) would utilize real-time data analytics and machine learning algorithms to predict emerging health trends and allocate resources dynamically to areas of greatest need. For instance, predictive models can forecast disease outbreaks in vulnerable regions, allowing for pre-emptive resource deployment and targeted interventions.81-83

Proposed model for an AI-driven health Policy Framework for Dynamic Adaptation in Global Health illustrates a potential AI-driven policy adaptation model that integrates real-time data from various sources—such as epidemiological surveillance, social determinants of health databases, and community feedback platforms. The model demonstrates how AI could dynamically adjust policy priorities and resource allocation based on predictive analytics, making global health interventions more responsive and equitable.
Health Equity Bonds: Financing the Future of Global Health: The concept of “Health Equity Bonds” is a novel financial instrument designed to attract private investment for public health initiatives promoting equity, 77 Table 1. These bonds would operate similarly to social impact bonds, where returns are linked to achieving specific health outcomes, such as reducing maternal mortality or increasing access to essential health services for underserved populations. Investors would receive dividends based on the social impact achieved, incentivizing them to fund interventions aligned with LNOB objectives.
Health Equity Bonds: Overview Outlining the Structure for Implementing Health Equity Bonds, Including Risk Assessment, Potential Returns, and Success Metrics.

Ultimately, balancing equity and efficiency in global health requires a multi-pronged approach, combining ethical advocacy, innovative financial solutions, and a commitment to ensuring that resource constraints do not compromise the goal of leaving no one behind.
Top-Down Versus Bottom-up Approaches
The LNOB principle challenges the traditional top-down approach in global health, where external experts, governments, or industries set priorities and interventions. Instead, LNOB emphasizes identifying and addressing the specific needs of those furthest behind. This shift raises a key question: How can global health initiatives genuinely reflect the voices of marginalized groups and ensure their meaningful participation?
Top-down approaches have been criticized for lacking community engagement and cultural sensitivity, often resulting in poorly adapted and unsustainable interventions. These approaches tend to rely on national-level data, which may overlook regional differences and the lived experiences of marginalized populations. In contrast, bottom-up approaches prioritize local ownership and participation, which are crucial for identifying and addressing the unique needs of the most disadvantaged. However, bottom-up methods can be difficult to scale due to power imbalances and the complexities of integrating diverse community perspectives.89-92
To address these challenges, global health research must adopt inclusive priority-setting practices that empower marginalized groups, share power, and consider local contexts.91,93-95 Achieving health equity requires democratizing processes and empowering communities to take an active role in decision-making. However, systemic barriers, such as limited funding, gender disparities, and the effects of globalization, continue to hinder meaningful participation from low- and middle-income countries.92,96-101
A collaborative model that integrates both top-down and bottom-up approaches is essential to fully realize the LNOB principle. Community-based participatory research (CBPR) is one method that facilitates this integration by fostering knowledge exchange and co-creating solutions between local communities and health experts. This process requires a conscious effort to address power dynamics, maintain continuous reflexivity, and shift decision-making power to local stakeholders.102-104 Transforming global health further involves decolonizing existing structures, dismantling paternalistic legacies, and ensuring diverse voices are included in decision-making processes. This includes institutional changes, revised funding models, and equitable partnerships that value non-Western knowledge systems.98,105,106
Ethical considerations are critical in this shift. While community engagement is essential, it must be conducted ethically to avoid exploitation and ensure fair compensation. Moreover, there is a need to proactively address how community participation could exacerbate existing inequalities if not managed carefully. Innovative solutions, such as blockchain-based decentralized health platforms, offer new opportunities for empowering communities by enabling them to manage their own health data and directly influence health priorities.107-109
Blockchain-Based Decentralized Health Platforms present a transformative approach to global health governance. These platforms allow communities to securely manage their health data, ensuring transparency, reducing data manipulation risks, and promoting trust and equity in health interventions (Figure 2). By decentralizing data governance, communities can have a stronger voice in shaping the health programs that affect them.107-109

Decentralized health data platform model where community data is anonymized, securely stored, and transparently shared among stakeholders, including healthcare providers, local governments, and non-governmental organizations (NGOs). This model empowers communities, enhances transparency, and reduces data manipulation risks, promoting trust and equity in global health interventions.
Ultimately, operationalizing the LNOB principle requires moving beyond purely top-down approaches that risk homogenizing diverse needs and perspectives. Shifting power dynamics in global health to center the voices of the most marginalized will involve challenging entrenched practices and building meaningful partnerships between experts and communities. While this is challenging, blending scientific rigor with local knowledge is crucial for designing equitable and sustainable global health interventions.
Short-Term Versus Long-Term Sustainability
The LNOB principle underscores the urgency of addressing the immediate needs of the most disadvantaged, those disproportionately affected by preventable diseases, malnutrition, and inadequate healthcare. However, while rapid responses such as emergency aid and medical care are essential in humanitarian contexts, there is also a need to balance these with long-term strategies for systemic change. The key tension in operationalizing LNOB is: How can global health initiatives sustainably integrate immediate interventions while fostering transformative, systemic change?
Short-term interventions, like emergency aid, temporary housing, and medical care, are critical in saving lives and alleviating suffering, particularly in conflict zones. They are ethical imperatives, providing immediate relief through vaccination campaigns, psychosocial support, and other urgent responses.110-112 However, these interventions come with challenges, such as the need for targeted planning and managing ethical concerns, including follow-up care and collaboration with local infrastructure.113-116 Despite these complexities, short-term humanitarian aid remains vital for resilience and recovery, as seen with the role of community health workers in delivering essential services and mitigating disaster impacts.117-120 Nonetheless, ensuring equitable support requires careful attention to social vulnerabilities during aid allocation. 120
To achieve lasting health equity, there must be a shift from short-term relief to long-term solutions that address root causes, such as poverty, discrimination, lack of education, and environmental degradation. Strengthening local health systems and focusing on the social determinants of health are crucial for fostering self-reliance and sustainable health outcomes in marginalized communities.121,122 However, these efforts face obstacles, including macroeconomic policies, governance issues, and resistance from those in power.123-131 Addressing these requires collaborative action across sectors to dismantle systemic barriers and promote health equity leadership that integrates science, policy, and practice.127-135
One key challenge for global health initiatives is balancing the need to address immediate needs with fostering long-term sustainability. Overemphasis on short-term projects can undermine local capacities and create dependencies. Ethical frameworks that emphasize collaboration, justice, and autonomy can help mitigate these risks by promoting community empowerment and self-sufficiency, even if they require greater initial investment.116,136,137 Building local capacity demands investment in infrastructure, education, ongoing support, and mechanisms to share decision-making power with communities to set research and policy priorities.138-142
Innovative mechanisms are essential to align immediate interventions with long-term sustainability. One such approach is an International Certification Program recognizing nations and regions successfully integrating short-term health responses with long-term Sustainable Development Goals (SDGs).143-150 This program would incentivize countries to align emergency health interventions, such as pandemic preparedness, with strategies that build long-term health resilience. Certification criteria focus on equitable access, sustainability, community participation, and alignment with ethical frameworks like LNOB. Table 2 outlines the framework for this certification program, including criteria such as ensuring equitable healthcare access, fostering community engagement, and integrating other relevant SDGs (eg, SDG 1: No Poverty, SDG 5: Gender Equality, SDG 13: Climate Action). Monitoring and evaluation processes would include data collection, regular assessments, impact evaluation, and community feedback mechanisms to ensure transparency and accountability. Certified countries would benefit from financial support, global recognition, technical assistance, and preferential access to resources during emergencies. Implementing this program would involve piloting in selected regions, capacity-building workshops, partnership development among key stakeholders, and continuous review to adapt to evolving global health landscapes. To foster continuous improvement, an Annual Global Health Summit could provide a platform for sharing best practices, lessons learned, and innovative solutions.143-150
Achieving lasting health equity requires a balanced approach, integrating short-term interventions with strategies that build resilient communities and systems. Prioritizing local capacities, community-led advocacy, and self-reliant solutions is critical to addressing immediate suffering while tackling systemic inequities. Transitioning from short-term responses to sustainable, community-driven approaches is essential for dismantling social and structural barriers and achieving the goals of the LNOB principle.
Potential Solutions and Frameworks
Can Structured Decision-Making Ensure Equity?
The LNOB principle requires a strategic and ethically sound approach to designing and implementing global health interventions. Structured decision-making processes, supported by ethical frameworks and practical tools, can help ensure equity. However, their effectiveness in addressing the complex realities of global health requires careful assessment.
Ethical frameworks provide a systematic approach to addressing equity concerns by analyzing interventions, identifying biases, and centering the needs of marginalized groups. Frameworks based on human rights, social justice, and decolonial ethics align well with LNOB’s core principles.151-153 Tools such as checklists, scoring matrices, and ethical analysis templates can help apply these frameworks consistently throughout the project lifecycle, enhancing transparency and accountability.154,155
Structured decision-making helps counteract the pitfalls of intuitive or urgency-driven decision-making by introducing objectivity and clarity in addressing ethical dilemmas in LNOB initiatives. Setting criteria, assigning weights, and evaluating trade-offs ensure that marginalized groups are explicitly considered alongside traditional effectiveness and efficiency measures.156-159
However, it is essential to acknowledge the limitations of such frameworks. Over-reliance on rigid quantification and objectivity can overlook social disadvantages’ complex, multifaceted nature. Ethical frameworks should complement—rather than replace—in-depth contextual analyses, community engagement, and ongoing reflection. Their true value lies in fostering dialog, revealing biases, and supporting continuous adaptation throughout a project’s lifecycle.116,160-162 Practitioners must use flexible, participatory methods to adapt these frameworks to new information and ensure that the “furthest behind” definitions reflect local realities and community priorities.
Research emphasizes incorporating local knowledge and social values when applying frameworks in specific contexts, particularly when addressing stigmas, disparities, and vulnerable groups’ agency in public health research.116,160-166 A culturally sensitive and balanced approach is essential, especially in mental health interventions and health inequities, where political and ethical complexities are prevalent.167-172
For ethical frameworks to be effective, systemic financing, power sharing, and knowledge production reforms are essential to create an environment conducive to equitable decision-making. These reforms empower marginalized communities, granting them greater autonomy and influence over their health outcomes. A shared ethical framework in global health governance should prioritize values like solidarity, innovation, and commitment to action, ensuring consistent application of ethical principles in health financing and policy decisions.30,71,173-175
Equitable research partnerships and funding practices are critical to advancing global health equity. This includes involving communities in decision-making, promoting equitable funding, and using ethical toolkits for priority setting. Addressing epistemic injustice in funding and overcoming challenges in evidence-based prioritization and culturally adaptive governance, particularly in indigenous health research, are vital steps toward empowering marginalized communities.92,142,176-178 Initiatives like logic models for locally led solutions in universal health coverage further highlight the need for systemic changes that enhance decision-making power and autonomy for these communities. 137
While structured decision-making and ethical frameworks have the potential to guide global health initiatives toward greater equity, their true value lies in promoting critical reflection, transparency, and flexibility rather than enforcing rigid formulas. When combined with meaningful community engagement and a commitment to systemic change, these frameworks can be powerful tools for advancing a more just and equitable global health landscape.
Community Participation as a Solution
The LNOB principle calls for a shift from “doing for” to “doing with” marginalized communities, emphasizing genuine participation and empowerment in shaping health outcomes.179,180 This requires overcoming barriers to participation faced by marginalized groups and using models like community development to reach those often excluded or hard to reach.181,182 Effective partnerships among governments, NGOs, healthcare providers, and communities are crucial for enhancing sustainability and ensuring culturally appropriate interventions.183-185
To facilitate genuine community engagement, it is vital to use participatory methods such as visual tools, capacity-building initiatives, and technology integration.186-189 Engaging communities in managing their health environments and using participatory research can help build more sustainable and healthier societies.190-193 However, authentic participation goes beyond tokenism and involves dismantling traditional power hierarchies in global health. Key strategies for achieving meaningful community participation include:
Global health practitioners must reflect on their biases, assumptions, and power dynamics. Recognizing and addressing unconscious paternalism is essential for building authentic partnerships based on trust and shared decision-making.
Redirecting funding to support community-based organizations directly fosters local ownership and self-determination. Investing in local leadership develops long-term capacity and promotes sustainable impact.
Challenging traditional research hierarchies involves valuing local knowledge and co-creating research that benefits academic institutions and communities.
While community participation is essential for equitable research and development (R&D), it must be carefully managed to avoid harm and exploitation. This involves ensuring fair representation of diverse voices within communities, avoiding manipulation or coercion, and providing fair compensation for community members’ time and expertise.194,195 Respecting community autonomy is critical, allowing individuals the right to refuse or withdraw participation without repercussions.
Special consideration is needed in research involving indigenous communities, where historical contexts and power dynamics are particularly significant. However, there is still a need for a more critical examination of how concepts like “community” and “participation” are applied in practice.196-198 Integrating community perspectives into research ethics reviews can help address the protection-inclusion dilemma, ensuring that vulnerable groups are protected and included meaningfully. 12
Community participation is not a quick solution; it requires time, resources, and a willingness from global health actors to share control. Power imbalances are deeply rooted and may resist change, demanding ongoing dialog, humility, and a commitment to structural reform. Embracing community participation is an ethical imperative under the LNOB principle and a practical necessity for achieving sustainable health equity. By employing participatory methods and actively shifting power dynamics, global health initiatives can better address unique community needs, enhance cultural appropriateness, and foster long-term improvements in health outcomes. While challenging, prioritizing community participation moves beyond mere good intentions to genuine collaboration, empowering those traditionally excluded and paving the way for a more just global health landscape.
Participation, Decolonization, and Shifting Power in Global Health Practice
The LNOB principle demands a fundamental re-examination of global health power dynamics, emphasizing marginalized communities’ voices and agency. Achieving ethical and effective interventions requires a practical focus on meaningful participation and critically examining colonial legacies. Community-based participatory research (CBPR) empowers communities as co-investigators, aligning research questions, methods, and interventions with local needs and priorities.184,199-203 Collaborative partnerships with community-based organizations should prioritize hiring local staff, investing in leadership development, and granting communities decision-making authority to promote self-sufficiency and resilience. Participatory evaluation tools like storytelling and community-led scorecards enable communities to define success beyond standard health metrics, ensuring culturally relevant and effective interventions. 199
Addressing power imbalances requires centering marginalized voices and sharing decision-making power.5,23-25,28,30,90,91,104,117,124,128,156,157,179,188,190,204 Tools and frameworks are available to tackle inequitable dynamics within CBPR, ensuring genuine participation and representation of marginalized groups in healthcare decision-making.205-208 These approaches underscore the need for both practical strategies and critical reflection on power imbalances to achieve LNOB’s goals.
The legacy of colonialism continues to shape global health, often manifesting in paternalistic attitudes and unequal power relationships between Western institutions and the Global South.15,56,104 Decolonizing global health requires critical reflexivity by practitioners and researchers to interrogate their biases, positionality, and power dynamics.102,104 Valuing local and indigenous knowledge equally and emphasizing co-creation are essential for developing holistic solutions. Transforming institutions through diversified leadership, revised funding models, and equitable partnerships is crucial for addressing structural power imbalances.102,209
This transformation involves moving away from charity models to true partnerships centered on capacity-building. Understanding global health in a globalized world from a systems perspective is vital to this shift.210-212 Decolonization is necessary to dismantle mechanisms perpetuating health inequities, and educational institutions play a key role by integrating colonial history into curricula and fostering equitable collaborations.213-215 Redistributing power is a complex process that may face resistance, especially from those accustomed to traditional structures. Challenges include navigating internal power dynamics within communities, avoiding tokenism, and ensuring equitable representation. Nonetheless, these are ethical imperatives in pursuing genuine LNOB implementation. Practical steps to operationalize LNOB by shifting power and control over resources include:
Allocating more funding directly to community-based organizations in the Global South fosters local autonomy and reduces reliance on external intermediaries.
Engaging marginalized communities in resource allocation ensures that funding aligns with local priorities and that the LNOB commitment is reflected on the ground.
Long-term investment in local research, leadership, and advocacy skills is essential to build sustainable local capacity and reduce dependence on external expertise.
Ethical guidelines and contractual agreements must ensure fair compensation, shared ownership of data, and recognition of traditional knowledge systems in global health partnerships.
The transformative potential of LNOB lies in embracing community participation and dismantling the colonial legacies entrenched in global health. Adopting methods involving communities at all stages, critical reflexivity, and institutional changes that redistribute power can create a more just and equitable global health landscape. This approach prioritizes co-creation over top-down solutions, respects local knowledge and priorities, and focuses on long-term capacity-building rather than short-term outcomes.
Advocacy for Increased Resources
The LNOB principle embodies a bold vision for achieving health equity globally. However, realizing this vision is challenged by resource scarcity in global health. While limited resources are a reality, increasing funding and support is desirable and ethically essential to transform LNOB from aspirational rhetoric into meaningful action for marginalized populations. The call for increased resources is grounded in the ethical principle of justice. Health is a fundamental human right recognized in the Universal Declaration of Human Rights. 216 Inadequate investment in the health of marginalized populations constitutes discrimination and perpetuates inequities. 217 The stark disparities in health outcomes between the Global North and South are a profound moral failure, exacerbated by significant gaps in funding that hinder low- and middle-income countries’ ability to implement effective interventions and build robust healthcare systems.218,219
Resource scarcity poses a dilemma for global health practitioners: maximizing efficiency with limited funds can perpetuate neglect of those with the most complex health challenges. Conversely, failing to allocate sufficient resources denies life-saving treatment to those in greatest need.72,220 Therefore, advocating for increased resources is both a practical necessity and a moral obligation. However, increased funding must be paired with transparency and accountability to ensure resources are used effectively. Concerns about donor fatigue and corruption make robust monitoring and evaluation mechanisms essential. Investments should focus on strengthening local health systems, fostering local ownership, and ensuring sustainable impact. 221
Several strategies can address resource scarcity in global health:
High-income countries must raise their Official Development Assistance contributions to meet internationally agreed targets, providing crucial support for global health initiatives. 222
Public-private partnerships, social impact bonds, and other innovative financial instruments can unlock additional funds for global health.223,224
Coordinated funding and collaboration are vital for addressing complex global health threats like pandemics or antimicrobial resistance.224,225
Improving governance and addressing global tax evasion can release significant resources for health, especially in resource-constrained settings.92,226
Wealthier countries have an ethical responsibility to reassess their spending priorities and allocate resources proportionate to the scale of global health inequities.92,224
While advocating for increased resources is crucial, ensuring their effective allocation and utilization is equally important. Investments in research and development, alongside efforts to improve access to essential medicines and technologies, can help maximize limited resources and enhance health outcomes. Transparent and equitable allocation mechanisms guided by distributive justice principles should be used to prioritize resource-constrained decisions. 227 Strengthening health research capacity and promoting the co-production of health research in low- and middle-income countries are also vital for sustainable progress. 228
Advocating for increased resources and ensuring their strategic and just allocation is fundamental to achieving LNOB’s goals. By aligning funding with equity, justice, and sustainability principles, global health initiatives can better address the needs of those furthest behind and make significant strides toward a more equitable world.
Context-Specific Innovations and Ethical Frontiers in LNOB Implementation
While existing LNOB frameworks offer valuable guidance, they often lack specificity for different socio-economic and cultural contexts. To be effective, LNOB strategies must be adapted to local realities through context-specific innovations that address unique challenges and ethical considerations.
In regions affected by conflict, mistrust in external interventions can undermine global health efforts. Integrating local conflict-resolution practices into health programs can help build community trust and facilitate participation. This requires partnerships with local leaders and community-based organizations to co-develop health interventions that resonate with the region’s socio-political dynamics. Aligning health initiatives with culturally accepted conflict-resolution norms can promote local ownership and the sustainability of intervention. 229
In settings with limited internet connectivity, offline-capable mHealth solutions can ensure that marginalized populations are included in digital health advancements. These solutions could offer essential health education, remote consultations, and access to digital health records without requiring continuous Internet access. Ethical considerations must address data privacy, digital literacy, and the risk of excluding digitally illiterate individuals. Developing these solutions should be driven by local needs assessments and user feedback to ensure they are relevant and effective. 230
While digital health tools have great potential to expand access to care, especially in under-resourced settings, they also present ethical challenges related to privacy, equity, and data governance. Robust ethical guidelines tailored to these contexts are urgently needed to address issues like informed consent, data security, and equitable access to technology. These guidelines must be adaptable to different cultural norms and values, ensuring digital health tools do not exacerbate existing inequities or create new forms of discrimination.231,232
Integrating technologies such as AI and blockchain into LNOB strategies brings new ethical dilemmas, including algorithmic bias, digital exclusion, and privacy breaches. A forward-looking framework that anticipates and mitigates these risks is essential for LNOB implementation. This framework must be dynamic, evolving with technological advancements and the changing needs of global health, to ensure ethical considerations keep pace with innovation. 233
Developing context-specific innovations that address these ethical frontiers is critical for effectively operationalizing LNOB. By tailoring frameworks to local realities and anticipating ethical challenges, global health initiatives can ensure they are both inclusive and effective, truly leaving no one behind.
Conclusion—A Call for Action and Continued Reflection
The LNOB principle, central to the Sustainable Development Goals, represents a significant ethical commitment to global health, demanding a shift from focusing on national averages to prioritizing those marginalized by poverty, discrimination, conflict, or lack of access to essential resources. However, operationalizing LNOB has exposed existing approaches’ inherent tensions and limitations.
Addressing these challenges requires more than technical solutions; it involves ethical commitments. Balancing universalism with targeted interventions, navigating resource scarcity while ensuring equity, and combining top-down and bottom-up approaches reflect deeper questions about how the global community values the well-being of those furthest behind. Progress depends on adopting ethical frameworks, enhancing community participation, advocating for increased resources, and challenging colonial legacies within global health systems.
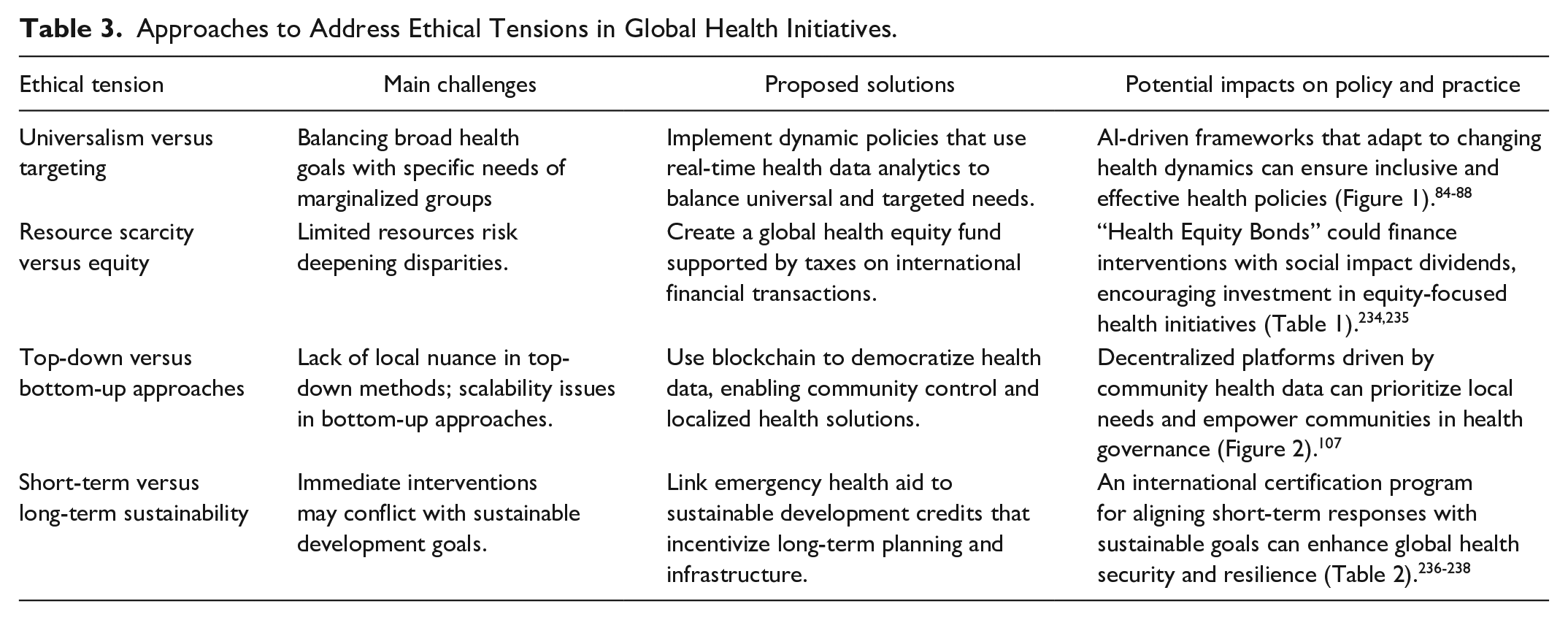
This transformative process demands humility and continuous adaptation. There are no simple or one-size-fits-all solutions. LNOB offers a roadmap toward a world where health is a universal right, not a privilege defined by circumstances. However, achieving this vision requires ongoing critical analysis, flexibility, and responsiveness to evolving contexts, Table 3.
Approaches to Address Ethical Tensions in Global Health Initiatives.
Turning this vision into reality requires embracing the ethical complexities of global health interventions, recognizing the limitations of current frameworks, and committing to ongoing dialog and collaboration. Achieving global health equity is a shared responsibility, calling for sustained efforts to prioritize the needs of the most marginalized. Continued research is essential to refine ethical decision-making, develop context-specific strategies, and identify best practices that ensure no one is left behind.
Footnotes
Author Contributions
DO was the principal author and initiator of the article and was responsible for its conception, drafting, and writing. PG contributed to the article by reviewing and revising it critically for important intellectual content. Both authors have read and approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.

