Abstract
The Maricopa County Department of Public Health (MCDPH) Sexually Transmitted Disease (STD) Clinic remained operational during a 6-week statewide Coronavirus Disease 2019 (COVID-19) Stay-at-Home Order. The present study sought to evaluate the effect of the Stay-at-Home Order on countywide STD reporting and uptake of sexual health services. We compared countywide daily median STD reporting and MCDPH STD clinic attendance across 3 timeframes; (1) Pre-Lockdown (01/01/2020–03/30/2020); (2) Lockdown (03/31/2020–05/15/2020); and (3) Post-Lockdown (05/16/2020–12/31/2020). STD reporting was characterized as incident chlamydia, gonorrhea, and primary and secondary syphilis. Clinic attendance was characterized as clients visiting through express testing or provider visits. Differences in STD reporting and clinic attendance were evaluated using non-parametric testing. Comparing Pre-Lockdown to Lockdown, we observed significant declines in the daily median chlamydia case reporting (−22%) and clinic express testing attendance (−29%). Comparing Lockdown to Post-Lockdown, we observed significant increases in daily median chlamydia and gonorrhea case reporting (+20%, +15%; respectively) and clinic express testing and provider visits (+42%, +20%; respectively). No significant difference was observed in countywide syphilis reporting across the 3 timeframes. Declines in STD reporting were observed countywide during the lockdown and were concurrent with declines in attendance observed at the MCDPH STD Clinic. Maintenance of clinic operations during the lockdown allowed for continued uptake of STD testing, diagnosis, treatment, and partner services. This study of sexual health care utilization at the public STD clinic in Maricopa County, Arizona, found reduced testing and provider visits contributed to lower countywide STD reporting during the Arizona COVID-19 Stay-at-Home Order.
• Declines in STD clinic attendance and STD reporting have been observed within the United States during the COVID-19 pandemic.
• The research in this article describes the differences in the uptake of services among symptomatic and asymptomatic STD cases using both countywide and clinic specific data.
• As the COVID-19 pandemic continues to evolve, changes in the uptake of sexual health services and STD reporting may inform opportunities to improve the uptake of prevention and treatment services.What do we already know about this topic?
How does your research contribute to the field?
What are your research’s implications toward theory, practice, or policy?
Introduction
Since declaration as a national emergency on March 13, 2020, the Coronavirus Disease 2019 (COVID-19) pandemic has significantly disrupted health care operations in the United States. Both the accessibility and delivery of sexual health services have been affected by unprecedented social isolation measures. In response to the pandemic, many sexual health clinics nationwide reduced services by restricting patient eligibility, reducing hours of operation, or entirely suspending clinic activities.1,2 Although Maricopa County, the fourth largest county in the United States, experienced similar disruptions in routine health care due to high morbidity of COVID-19, the only government-run sexual health facility has maintained all in-person sexually transmitted diseases (STD) clinical services during the pandemic.
Following the COVID-19 national emergency announcement, the governor of Arizona announced a 6-week Stay-at-Home Order in the State effective March 31, 2020 through May 15, 2020. The Order limited Arizona’s residents time away from home except when involved in essential activities or functions. 3 Early speculation suggested that lockdown interventions may reduce the opportunity for sexual encounters and therefore reduce transmission of STDs. However, increasing evidence suggests social isolation measures may result in decreased testing, treatment, and reporting of cases.4‐6
Throughout the COVID-19 pandemic, the Maricopa County Public Health Department (MCDPH) STD Clinic has maintained sexual health services fully operational, including Monday through Friday in-person express STD testing and medical provider visits. To understand the effect of COVID-19 isolation measures on sexual health care utilization and case reporting, we analyzed temporal trends of STD clinic attendance and STD morbidity in Maricopa County in relation to the COVID-19 Arizona Stay-at-Home Order.
Methods
Countywide Study Population
The countywide study population consisted of incident COVID-19, gonorrhea, chlamydia, and primary and secondary syphilis cases reported within Maricopa County. STD cases included were those reported between January 1, 2019 and December 31, 2020. Similarly, COVID-19 cases consisted of those reported between January 1, 2020 and December 31, 2020. Case definitions used are in accordance with those provided by Arizona Department of Health Services (ADHS). 7 Laboratory case reporting requirements for communicable diseases in Arizona are outlined in A.A.C. R9-6-204. 8
Clinic Study Population
The MCDPH STD Clinic study population consisted of clients attending the MCDPH STD Clinic between January 1, 2019 and December 31, 2020. As a proxy for symptomatic and asymptomatic clients, attendance was examined by type of visit including: (1) provider visits and (2) express STD testing. Express visits at the STD clinic were established in 2008 to provide serum-based HIV and syphilis, and urogenital and extragenital chlamydia and gonorrhea STD testing for persons that denied symptoms and were not referred or presenting as contacts to cases. Provider visits are reserved for persons with symptoms consistent with chlamydia, gonorrhea, or syphilis, or persons that are either known positives (diagnosed at outside clinics and referred to MCDPH) or are contacts to cases. 9 Based on self-report, patients are referred accordingly by clinic staff to express testing or a provider visit.
Data Collection
Countywide STD morbidity, testing, and treatment data were extracted from the Patient Reporting Investigation Surveillance Manager (PRISM). COVID-19 countywide case counts were extracted from the Medical Electronic Disease Surveillance Intelligence System (MEDSIS). Both PRISM and MEDSIS databases are hosted and supported by ADHS. MCDPH STD Clinic morbidity and attendance data were extracted from eClinical Works, an electronic health record software. Data were imported into SAS Enterprise Guide 8.2 for analysis.
Primary Analysis
To assess the temporal trends of countywide reported STDs, COVID-19, and isolation measures, rolling averages were produced using Microsoft Excel (V2008, Redmond, WA). For COVID-19 data, a 7-day rolling average was calculated for cases reported between 01/31/2020–12/31/2020. For STD data, a 21-day rolling average was calculated for cases reported between 01/31/2019–12/31/2020. Results were stratified by year and STD and overlayed with COVID-19 data.
Median distributions of countywide STD reporting and MCDPH clinic attendance were examined during 3 timeframes: (1) Pre-Lockdown (01/01/2020–03/30/2020); (2) Lockdown (03/31/2020–05/15/2020); and (3) Post-Lockdown (05/16/2020–12/31/2020). Lockdown was defined as the duration of the Arizona Stay-at-Home Order. Differences between timeframes (Pre-Lockdown, Lockdown, and Post-Lockdown) were examined using Kruskal–Wallis tests. For analyses in which the overall test was significant, pairwise comparisons were performed using the Mann–Whitney test.
Secondary Analysis
As an additional proxy for symptomatic STDs, a secondary analysis using gonorrhea in males was performed to assess incident STD transmission and access to services for symptoms. MCDPH STD Clinic provider visits among gonococcal males were examined during (1) Pre-Lockdown, (2) Lockdown, and (3) Post-Lockdown. The Kruskal–Wallis test was used to assess differences between timeframes. These analyses were conducted as part of public health surveillance activities and thus considered non-research according to Title 45 Code of Federal Regulations 46.102(I). 10
Results
Temporal Visualization
Countywide chlamydia, syphilis, and gonorrhea case reporting declined near the start of and during the Stay-at-Home Order marker. Following this stark decline, all 3 STDs trended upward before a short decline simultaneous to Maricopa County’s first peak in COVID-19 cases in early-July 2020. Following a steep steady decline in countywide COVID-19 cases, STD case reporting consistently increased from late-July until mid-October. Near mid-October, STD case reporting declined slightly coinciding with the second COVID-19 peak of 2020 (Figure 1). 2019 and 2020 sexually transmitted diseases reporting overlayed with 2020 COVID-19 reporting, Maricopa County.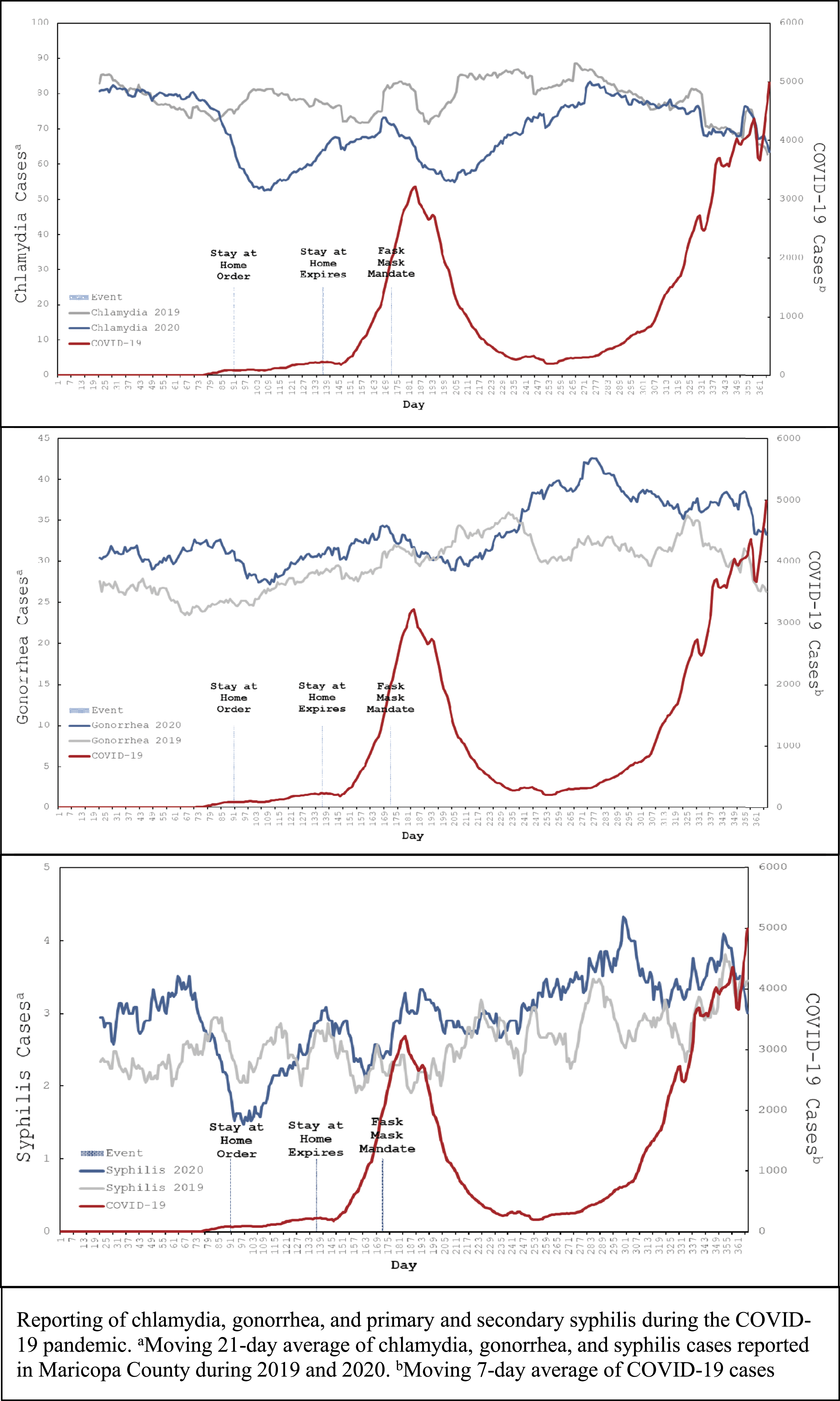
Countywide Chlamydia
Daily Median STD Reporting and STD Clinic Attendance During Pre-Lockdown, Lockdown, and Post-Lockdown, Maricopa County 2020.

Note. IQR: interquartile range; STD: sexually transmitted diseases, MCDPH STD: Maricopa County Public Health Department Sexually Transmitted Diseases.
Note—Italicized gonorrhea in males represents subcategory of clients seeking provider visits.
*Denotes statistical significance at P < .05.
Countywide Syphilis
During the Pre-Lockdown, Lockdown, and Post-Lockdown timeframes in 2020, Maricopa County reported median daily primary and secondary syphilis case counts of 2 (IQR, 1–4), 2 (IQR, 1–4), and 3 (IQR, 1–5), respectively. There was no significant difference in syphilis reporting among these 3 timeframes (P = .1311) (Table 1).
Countywide Gonorrhea
During the Pre-Lockdown, Lockdown, and Post-Lockdown timeframes in 2020, Maricopa County reported median daily gonorrhea case counts of 34 (IQR, 16–41), 34 (IQR, 18–39), and 39 (IQR, 20–47), respectively (Table 1). There was a significant difference in reporting of gonorrhea among these 3 timeframes (P = .0068) (Table 1). Pairwise comparisons showed a statistically significant difference between the Pre-Lockdown and Post-Lockdown periods during which median daily reporting increased 15% (P = .0031). Lockdown and Post-Lockdown comparison was also significant during which median daily case counts increased 15% (P = .0099).
Clinic Attendance and STD Diagnoses
During the Pre-Lockdown, Lockdown, and Post-Lockdown timeframes in 2020, the MCDPH STD Clinic served a median daily count of 92 (IQR, 79–101), 65 (IQR, 59–75), and 92 (IQR, 83–99) clients through express testing, respectively. There was a significant difference in express testing attendance among these 3 timeframes (P < .0001) (Table 1). Pairwise comparisons showed a statistically significant difference between the Pre-Lockdown and Lockdown periods during which median daily express testing attendance decreased 29% (P < .0001). Lockdown and Post-Lockdown comparison was also significant during which median daily express testing attendance increased 42% (P < .0001).
During the Pre-Lockdown, Lockdown, and Post-Lockdown timeframes in 2020, the MCDPH STD Clinic served a median daily count of 40 (IQR, 35–46), 35 (IQR, 31–45), and 42 (IQR, 36–46) clients through provider visits, respectively. There was a significant difference in provider visit attendance among these 3 timeframes (P = .0265) (Table 1). Pairwise comparisons showed a statistically significant difference between the Lockdown and Post-Lockdown periods during which median daily provider visits increased 20% (P = .0103).
Overall, during the Lockdown period, there were a total of 2,994 express test and 1,257 provider visits. Additionally, 415 cases of chlamydia, 328 cases of gonorrhea, and 65 cases of primary and secondary syphilis were diagnosed and/or offered treatment and partner services directly at the MCDPH STD Clinic.
Secondary Analysis
For provider visit attendance among male gonorrhea cases during the Pre-Lockdown, Lockdown, and Post-Lockdown timeframes in 2020, the MCDPH STD Clinic served a median daily case count of 4 (IQR, 3–6), 5 (IQR, 3–7), and 5 (IQR, 4–7), respectively. There was no significant difference in attendance among these 3 timeframes (P = .0846) (Table 1).
Discussion
During the Stay-at-Home Order, Maricopa County observed a significant decrease in daily chlamydia case reporting. Changes in gonorrhea and syphilis case reporting were not significant. Following the expiration of the Stay-at-Home Order, countywide STD case reporting rebounded to Pre-Lockdown levels. From Lockdown to Post-Lockdown, both countywide chlamydia and gonorrhea case reporting increased significantly. Syphilis case reporting similarly increased although was not significant.
Consistent with the changes in countywide STD reporting during the Stay-at-Home Order, the MCDPH STD Clinic observed a significant decrease in express testing attendance. The clinic also observed a non-significant decrease in provider visit attendance. Following the expiration of the Stay-at-Home Order, the clinic observed significant increases in both express testing and provider visit attendance.
As the largest single provider for STD testing and treatment in Maricopa County, the MCDPH STD Clinic is the largest single contributor to countywide STD case reporting. As described in this report, the STD Clinic observed declines in clinic attendance during the 2020 lockdown months of the COVID-19 pandemic. Given the diverse patient population served by the clinic, these results may be generalizable to other outpatient clinics offering sexual health services in the Central Phoenix area. These findings, concurrent to the statistically significant declines in STD reporting observed at the county level, suggest that STD services in other clinical settings were also not accessed at rates seen prior to the onset of the COVID-19 pandemic. These findings suggest disruptions in uptake of STD services and missed opportunities for prevention counseling, diagnosis, treatment, and contact tracing.
While the cause of the decline in STD reporting is likely multifactorial, several factors are important to consider. Fear of coronavirus infection may possibly have contributed to changes in sexual behavior by deterring sexual activity; evidence on this matter is mixed. Despite some researchers finding decreased self-reported sexual encounters during COVID-19 measures, others have demonstrated no changes in risky sexual behaviors among specific populations.11,12 Moreover, researchers have also documented significant increases in frequency of sexual intercourse during the pandemic. 13 Evidence therefore is unclear on whether reduced sexual transmission played a large role in the observed decreases in STD reporting.
In this study, as a proxy for STD incident infection and transmission during periods prior to and during lockdown, we evaluated gonorrhea in males given the symptomatic nature of this infection. We found MCDPH provider visits for this STD remained the same suggesting that unprotected sexual activity and sexual transmission may have remained unchanged during the lockdown. This finding is consistent with the countywide reporting of gonorrhea which similarly did not change from Pre-Lockdown to Lockdown.
As demonstrated in this report, the MCDPH STD Clinic experienced lower volumes of STD testing and provider visits during COVID-19 lockdown measures. These results support those documented in routine STD clinics and centers outside the United States, where similar decreases in testing have been observed.12,14 Emerging evidence in Oregon, California, and Georgia is also consistent with the declines in STD reporting observed in this report.15-17 Some researchers have documented starker declines in STD testing among asymptomatic clients when compared to symptomatic cases. 18 The findings in this study are consistent with this notion given the largest decrease in STD reporting was observed among chlamydial cases, which are largely detected through routine screenings. Furthermore, the largest decline in clinic attendance was observed in express testing, which provides STD testing to asymptomatic clients. Decline in provider visits was likely less pronounced due to symptomatic patients requiring immediate care. Despite this evidence, further studies are necessary to assess this association.
Limitations should be considered when interpreting these data. First, although the MCDPH STD Clinic remained open during the lockdown period and throughout the pandemic, telemedicine services were not available. It is possible that routine clients may have sought syndromic management from other private providers through telemedicine visits during this period, a practice supported by CDC recommendations. 19 This may have contributed to decreased STD clinic attendance. However, decreased STD reporting observed at the County level suggests reduced uptake of STD testing and diagnostic services additionally occurred in other clinical settings. People receiving care through telemedicine may have furthermore been prescribed empiric oral treatment based on symptoms without laboratory diagnosis and case reporting.
Second, during September 2020, the CDC announced a shortage of STD diagnostic test kits and laboratory supplies. 19 In response, the MCDPH STD Clinic prioritized extragenital testing among symptomatic cases in high-risk populations. This disruption in STD testing, concurrent with ongoing empiric treatment without laboratory diagnosis and etiologic diagnosis, may have resulted in fewer reported cases during the Post-Lockdown period.
Last, average daily case counts for countywide syphilis in this study were low leading to small differences in daily averages. Small effect size and limited sample size may therefore have contributed to low power in detecting differences between timeframes. Additionally, data from the MCDPH STD Clinic may not be generalizable to other clinical settings outside of Maricopa County. As a publicly funded organization, the clinic provides low-cost services to individuals in the Central Phoenix area. Persons attending the clinic pay $20 for testing, treatment, and partner services. Results may therefore not be generalizable to clinics servicing individuals of differing socioeconomic status.
Despite the decreases in STD reporting, Maricopa County still observed high frequencies of STDs during the Lockdown. Maintaining MCDPH STD clinic operations resulted in 415 people with chlamydia, 328 with gonorrhea, and 65 with primary and secondary syphilis receiving testing, diagnosis, treatment, and/or partner services interviews directly at the MCDPH STD Clinic. Had the MCDPH STD Clinic closed during the Lockdown, these individuals would not have received access to low-cost, timely STD services (testing, treatment, and partner services). These results, in the wake of COVID-19, highlight the value of maintaining access to STD services during public health emergencies.
In conclusion, declines in STD reporting were observed countywide during the Lockdown period. Concurrent to the declines in attendance observed at the MCDPH STD Clinic, the findings in this report support the notion that decreased testing and treatment during the COVID-19 pandemic contributed to overall declines in STD reporting. Reduced testing and treatment may lead to increased transmission, particularly among asymptomatic individuals. As Maricopa County data show, STD case counts are quickly returning to pre-COVID-19 historic highs. The temporal trend of incident STDs in Maricopa County and other communities will need to be continually monitored relative to STD service access and uptake as part of the evolving COVID-19 pandemic.
Footnotes
Acknowledgments
We thank Dr. Renuka Khurana, Corinne Velasquez, and Dr. Haron Siringi for their support and guidance in the completion of this study. We thank Christina Mrukowicz and Jennifer Collins for their support and contributions in countywide COVID-19 data acquisition.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
CDC Disclaimer
The views expressed in this manuscript are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
