Abstract
Studies globally have provided substantial evidence that PHC could conduct doctor-visiting behaviors, control medical expense, and improve population health. This study aimed to map how family doctor (FD) in Shanghai achieved gate-keeper goals including health management, medical expense control, and conducting ordered doctor-visiting behavior. A total of 2754 and 1995 valid questionnaires were collected in 2013 and 2016 respectively in Shanghai. The data were analyzed using structural equation modeling (SEM). Invariance analysis was also performed for 2 waves of data. We found that the coefficient of cognition on health management (β5 = 0.26,
Family doctor achieved gate-keeper goals including health management, medical expense control, and conducting ordered doctor-visiting behaviors.
“cognition-behavior-outcomes” path was found for family doctor gatekeeper role in Shanghai of China, in which cognition had a greater effect on CHSC visiting and health management than contracting with a family doctor.
The path coefficients of SEM model varied over waves suggesting that reimbursement discount was not sustainable.
Background
Family Doctor (FD) system, a Chinese characterized mode of primary health care (PHC) had been initially established since the new round of medical reform in 2009, which was set to solve accessible and affordable problem. 1 Another significant measurement in the new reform was universal coverage. 2 Five years later, the central government launched another significant document, in which FD was set to be a key strategy to achieve an ordered medical treatment system, called hierarchical diagnosis treatment system. This system was based on the PHC system, in which FD attracted residents to first-visit community health service center (CHSC) and referred those severe patients to specialists in tertiary hospitals. 3 Almost ten years later, FD system was set to be a key target to achieve “health for all” in the Healthy China 2030, in which health management was advocated and FD was respected as the main role to achieve health management for all. 4 Through the progress of PHC in China, we could capture the changes of policy goal from expense control, ordered visiting, to health for all. Indeed, World Health Organization has promoted PHC in early 1970s in Almaty Declaration. 5
Studies globally have provided substantial evidence that PHC could conduct doctor-visiting behaviors, 6 control medical expense, 7 and improve population health. 8 However, we lack a whole picture to show how we achieve those targets, and what the relationships are among those targets. Existing studies have provided evidence to contribute to this picture. Firstly, J Huang performed a longitudinal analysis based on 2 waves of survey and found that awareness of FD services was significant predictor of contracting with a FD, suggesting cognition was positively correlated with contraction behaviors of residents. 3 Secondly, their follow-up study focused on the effect of FD-contracted services and found that contracted residents were performed better in following an ordered doctor visiting behavior (first-contact CHSCs and referral to specialists via CHSCs), and performed better in health management behavior as well. Their study even suggested that contracted with a FD might have a positive effect on the health outcomes for diabetes and hypertension patients, but it was unclear for the work mechanism and paths. 9 Thirdly, Huang et al 10 further revealed that contracted residents were more likely to join non-communicable disease (NCD) focus group, which had a positive effect on self-management (including improved health knowledge, greater health awareness, more frequent engagement in health behavior, and, most importantly, greater practice of self-monitoring), and a positive effect on NCD control results. Current studies also suggested that FD contracted services could improve health by promoting health management behaviors including NCD management, health examination and exercise, though causal analysis was not performed.11-13 Fourthly, current studies compared resources used by PHC practitioners and specialists, and found that patients of PHC providers have lower levels of use, such as fewer diagnostic tests and procedures, and lower costs of care.14-16 For example, Maeseneer et al 17 examined the effect of continuing FD visiting behavior on total medical expense, and they found that provider continuity with a FD was one of the most important explanatory variables related to the total health care cost, providing evidence that first-contact and continually visit FD could control medical expense. Lastly, current studies consistently provided evidence suggesting that PHC could improve health outcomes and control medical cost at the same time. For example, international comparisons between industrialized countries suggested that the populations of countries with higher ratings of “primary care orientation” experienced better health outcomes and incurred lower health care costs than the populations of countries with lower degrees of PHC orientation.18,19
Following the current studies, we developed a theoretical model revealing the whole picture of how PHC achieved the gate-keeper role of health and medical expense management (see Figure 1). There are mainly 5 hypotheses based on previous studies: (1) Cognition is positively correlated with contraction behavior of residents; (2) contracted residents behave better in both doctor-visiting behavior and health managing behavior; (3) behave better in health management results; (4) and medical expense control; (5) better health could save medical expense. Besides, we supposed that there might be a positive relationship between cognition and behavior though existing studies did not provide direct evidence. Thus, our study aimed to integrate all these assumed factors in a coherent model that would reveal how primary care play the role in health and medical expense management.

Theoretical model.
Methods
Sampling
A longitudinal data was collected in 2013 and 2016 by questionnaire survey. The multi-stage random cluster sampling was performed to obtain 3040 individuals: in the first stage, we selected 4 neighborhood committees from each sub-street by probability-proportional-to-size sampling, 2 communities were extracted from each neighborhood committee using simple random sampling in the second stage, 38 households were selected from each community in the third stage, and we picked up 1 resident aged at least 18 years old as the ultimate participant via random drawing method of Kish table finally. A total of 2754 valid questionnaires were collected in the first wave in 2013, and the second we tracked 1995 valid individuals (72.44%) in 2016.
Measures
Cognition of FD and CHSC was measured by 3 items, including awareness the difference between CHSC and large hospitals, awareness of contact phone of the community FD, and awareness of FD contracted services. Behavior was categorized into 2 variables, that is, CHSC visiting behavior and health management behavior. The first 1 was measured by 6 items, including first-contact at CHSC preference, referral preference, referral back to CHSC, “1+1+1” group treatment, NCD visit at CHSC preference, and appointment preference before visiting CHSC. The latter was measured by 5 items, including NCD management by CHSC, self-management, NCD prevention and control services by CHSC, exercise regularly, and health examination. All items were measured on a five-point Likert scale from strongly disagree (1) to strongly agree (5). Besides, sign with FD was measured by 1 item, “have you signed with a FD? (1 = yes, 0 = no),” medical expense was measured by 1 item, “How much did you spent last year on medical treatment?,” and NCD management was measured by 1 item “How do you score your health management result? (5 = excellent, 4 = good, 3 = fair, 2 = poor, 1 = very poor).”
Exploratory factor analysis (EFA) was performed and showed that 2 factors, 2 factors and 3 factors were extracted respectively for cognition, CHSC visiting and health management by principle components method (Figure 1). Then, confirmatory factor analysis was performed and showed that those structure model could be ideally supported by the investigation data.
Data analysis
We performed the measurement model first, and we deleted some observed variables whose factor loadings were below 0.45 suggested by Bentler and Wu. 20 We assured that all latent variables had at least 2 measurement variables, according to Kenny. 21 Reliability and Validity were then performed to make sure the item reliability and the convergent validity for each construct and the discriminant validity among constructs. Then the final SEM Model was completed which combined measurement model and construct model. We used indicators of chi-square test, GFI, AGFI, NFI, IFI, TLI, CFI, Standardized RMR, and RMSEA to examine the goodness of model fit. And invariance of multi-group confirmative factor analysis and multi-group structural equation model were also performed for 2 waves of data comparison. SPSS Amos was used for SEM in the dataset. All parameters were estimated using maximum likelihood.
Results
Data Description
Though we have 2 waves of data, the characteristics kept in stable. Thus, we pooled the data to describe the sample characteristics. Among the respondents, the average age was 55.13, 61.10% were females, 76.17% got married, 28.57% had a bachelor’s degree, 95.82% had a Shanghai Hukou (household registration), and 93.56% were covered in social medical insurance schemes (Table 1).
General Characteristics of the Sample.

Reliability and Validity
Composite reliability (CR), and average variance extracted (AVE) were used to assess convergent validity. 22 The CR values was around 0.60 as we used self-created items to construct latent variable, and values of AVE were greater than 0.40, which were not that reliable and convergent compared with early developed and repeatedly practice scales but also acceptable. 23 The discriminant validity showed that correlations among constructs were all below the square root of AVE for all construct suggesting a well discriminant validity. Thus, convergent validity and discriminant validity were supported (Tables 2 and 3).
Reliability and Convergent Validity.

Discriminant Validity.

Model Fit
After measurement model reliability and validity test, we constructed the structural model. The fit indices of the research model were calculated as GFI = 0.993, AGFI = 0.986, NFI = 0.976, IFI = 0980, TLI = 0.966, CFI = 0.980, SRMR = 0.024 and RMSEA = 0.033, which were all satisfied with experience value standard, suggesting this structural model achieved an acceptable level, suggesting that this model could be supported by the total sample. The X2/
Model Fit Indexes.
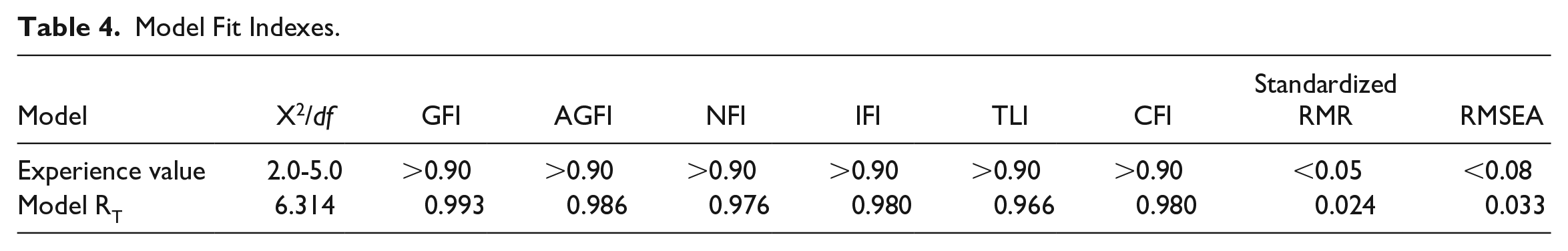
SEM Analysis
All factor loading parameters were larger than 0.45 and significant, and all error terms (1-SMC) were also significant as well. In the structural path model, we found cognition had a significant positive effect on sign with FD behavior (β1 = 0.67,

The SEM model of FD gate-keeper role path.
Invariance Analysis
We compared 2 waves of survey data with the same SEM model, and found the measurement weights seemed consistent except for the effect of sign with FD on health management, of CHSC visiting on health management, and of health management on medical expense (Table 5). The path loadings were not significant in 2016 anymore. And we further performed 6 models to conduct the invariance analysis. The Model fit indexes were all acceptable (Table 6), however, the significant
Parameter Estimates of SEM Model among 2 Wave-Samples.

Multigroup Invariance Test on Model R among 2 Samples of Waves.

Discussion
China implemented FD system since 2009, a Chinese mode of PHC, and ambitious goals were set by the government, that is, to conduct ordered doctor-visiting behaviors, to achieve health for all by health management, and to control medical expense. Ten years have passed, it is still unclear whether FD has achieved these goals and how. We collected data since 2013 in Shanghai, the pilot city to practice FD in China, and performed SEM to test our research question in the conceptual model.
We found cognition was a significant predictor of FD-contraction behavior which also affected residents’ doctor visiting behavior and health management behavior significantly. Previous studies provided evidence that cognition was the most significant predictor of signing behavior. Huang et al 9 examined the effect of cognition on signing with a FD, and found that those with high awareness of FD contract services were 21.674 times that of the low awareness ones to sign with a FD based on multivariate analysis. The effect of cognition on health behavior was also widely discussed. Kiviniemi et al 25 presented a framework and empirical evidence for complex relations between cognition in predicting health behavior, and found that interplay between affect and cognition drives health behavior. One opinion is that health education is an effective and efficient method to improve health knowledge. Zhu et al 26 provided empirical evidence that health education has overall positive effects on changing exercise behavior. The other opinion argues that education, 1 significant measure of socioeconomic status, 27 is the structural factor affecting health knowledge, cognition and behavior. Johnston et al 28 found that the mediating effects of health behaviors accounted in the short run for around a quarter and in the long run for around a third of the entire effect of education on health. And substantial evidence showed that health behavior was the mediator between cognition and health outcomes.29,30
The impact of cognition on health management (β5 = 0.26,
SEM model also showed that first-contact at CHSC had a positive effect on health management by FDs (β6 = 0.30,
The gate-keeper role of medical expense control was significant in first-contact (β10 =
Limitation
There are some limitations of this study. Firstly, a theoretical model is lacked, as the path of FD’s gate-keeper role has never been mapped by evidence-based model in Shanghai, China. Instead, we constructed a conceptual model based on existing studies. Secondly, some variable is not accurate in this study especially the medical expense variable. We used self-reported medical expense variable as it is difficult to get access to official dataset from the government.
Conclusion
We mapped the path of how FDs in Shanghai achieved the gate-keeper goals in Shanghai, China for the first time by SEM. The conceptual model was tested and showed a “cognition-behavior-outcomes (health and medical expense)” path of FD’s gate-keeper role on health management, medical expense control and ordered doctor-visiting behavior conducting. Our study also suggested that we have a long way to go to consolidate FD contracted services rather than reimbursement discount.
Footnotes
Acknowledgements
We thank the students from sociology and social work department, Fudan University, for visiting the selected residents as investigators. We especially appreciate the investigators for the second wave survey, as it is quite difficult to revisit the selected residents 3 years later; We thank Ma Li, and Li Yun for their support and cooperation as survey assistants.
Ethics Approval and Consent to Participate
This study was approved by the Academic Ethics Committee of Shanghai Pudong Institute for Health Development (approved number is PDWSL2013-1). All participants were asked to provide written consent before participating in this survey. Data were stored and processed anonymously.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by Leading Personnel Training Program of Pudong New Area Health System (PWRl2020-05), Leading Personnel Training Program of Pudong New Area Health System (PWRL2017-05) and the National Natural Science Foundation of China (71904145).
