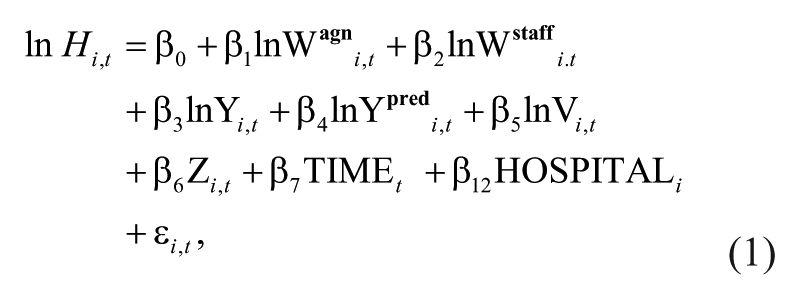Abstract
There is an ongoing debate about the reasons for the growth of temporary employment of registered nurses (RNs). Some argue that efficiency incentives to increase flexibility and reduce labor costs are the principal cause, while others point to shortages of RNs as the stronger determinant. Using hospital-level data from California’s Office of Statewide Health Planning and Development, we find a significant trend of increasing demand for agency nurses during the years of RN shortage. Demand rose with inpatient days, patient demand fluctuation, and the level of fringe benefits. Competition between hospitals and unionization, however, did not affect hospitals’ demand for temporary RNs.
Keywords
During periods of nursing shortage, hospital managers have difficulty recruiting and retaining nurses and thus often use nurses from temporary employment agencies to fill vacancies (Houseman, Kalleberg, and Erickcek 2003; LeRoy 1982; Manias et al. 2003; May, Bazzoli, and Gerland 2006). Many hospitals use both short-term daily (per diem) nurses and longer term “traveling” nurses employed by temporary employment agencies to meet staffing needs (May, Bazzoli, and Gerland 2006). Studies on nursing shortages in the United States show that growth in the use of nurses from employment agencies is associated with nurse shortages (Buerhaus, Staiger, and Auerbach 2003; May, Bazzoli, and Gerland 2006; Serratt et al. 2011). Recent estimates are that supplemental staffing accounts for more than 30 percent of total nursing hours (Bae, Mark, and Fried 2010).
Filling vacancies with temporary nurses may improve hospital services by allowing shorter waiting periods for admission while ensuring that the desired nurse-to-patient staffing ratios are met. Since the number of patients arriving in any given time period is subject to substantial variability, a considerable portion of which is unpredictable, hospitals must maintain reserve capacity to satisfy fluctuations in patient care needs (Baker et al. 2004; Carey 1998). Maintaining reserve capacity may be relatively inexpensive if hospitals have access to temporary staff, because hospitals can then avoid paying the high fixed costs of employee benefits and do not pay for unneeded hours of work. Thus, it may be cost-effective for hospitals to make use of agency personnel, even though the hourly rate is higher than baseline wages for in-house regular staff.
However, some researchers have raised safety concerns related to the use of temporary staff, citing the potential for less familiarity with hospital procedures and practices (Castle 2009; Castle and Engberg 2007; Jalonen et al. 2006; Porell et al. 1998; Roseman and Booker 1995; Weech-Maldonado et al. 2004; Yeh et al. 2007). For example, Roseman and Booker (1995) found a positive correlation between medication errors and patient days worked by temporary nurses. An increase in temporary staffing may also increase the workload of permanent staff who, in addition to dealing with their existing workload, must supervise and assist temporary nurses (Castle 2009). In such cases, the employment of temporary personnel is welfare decreasing.
In addition to employing temporary nurses to meet fluctuations in patient care needs, hospitals have engaged nurses in midterm and long-term contractual arrangements, typically through agencies that specialize in the placement of “traveling” nurses who often have a permanent residence that is not near their work assignment. These arrangements are reportedly more common when hospitals have difficulty filling vacancies for permanent positions, such as during the registered nurse (RN) shortage of 1998 to 2007. When nurse shortages are reported or perceived to be imminent, there has been federal investment in expanding nurse supply. For example, the U.S. government appropriated US$230 million in 2012 to fund nursing workforce development programs. If hospitals substitute vacant nursing positions with temporary contract nurses, mitigating the need for hospitals to develop human resource practices to recruit permanent staff, then there is little justification for government policies to encourage the training and recruitment of nurses (Long, Goldfarb, and Goldfarb 2008).
Little empirical evidence exists about the extent to which hospitals depend on temporary RNs for their nursing services, or about what factors are the most responsible for hospital demand for temporary nurse staff. In particular, the relationship between persistent nurse shortages and the employment of temporary nurses has been difficult to analyze due to limited data (Kane et al. 2007; Long, Goldfarb, and Goldfarb 2008). This study fills this gap by using hospital-level data from California for multiple years. These data include hours worked by temporary RNs, wages, and hospital and market characteristics. Our data span a period of surplus in the mid-1990s and a deep shortage that started around 1998 and peaked in the early 2000s. These data provide an opportunity to examine how shortages affect decisions made by hospitals about the ideal mix of permanent and temporary staff.
Previous Literature
The history of hospital use of temporary staffing goes back to the mid-1970s (LeRoy 1982). While time-series evidence on the national incidence of temporary nurse employment is unavailable, data from various sources suggest a growing trend of agency staffing. In a survey of hospitals conducted in 1981 by Prescott et al. (1982), 39.5 percent of hospitals in the sample used nurses from temporary employment agencies. Using data in 2001 on 1,000 hospitals nationwide, First Consulting Group, American Hospital Association (2001) reported that 56 percent of the sampled hospitals used temporary nurses. May, Bazzoli, and Gerland (2006) found that 75 percent of their surveyed hospitals used temporary staff.
There is an ongoing debate about the reasons for the growth of temporary employment. Some argue that efficiency incentives are the principal cause, while others point to shortages of RNs as the stronger determinant of temporary staffing of nurses. Proponents of the efficiency incentive theory explain that the temporary workforce has grown because firms want to increase flexibility and reduce labor costs. For example, Little and Buchan (2007) showed a trend toward employers offering more casual positions to increase their own ability to add or subtract nurses as patient volumes change. On the other hand, hospital executives and nurse managers reported that labor shortage is the major motivator for using temporary nurses (Houseman, Kalleberg, and Erickcek 2003; May, Bazzoli, and Gerland 2006).
Most research emphasizing the role of efficiency incentives has identified both competition between hospitals and the uncertainty of product demand as explanatory variables for the growth of the temporary workforce (Abraham and Taylor 1996; Baker et al. 2004; Cohany 1998; Kandel and Pearson 2001; Mobley and Magnussen 2002). Mobley and Magnussen (2002), for instance, show that interhospital competition resulting from the penetration of managed care leads hospitals to reduce staffing levels to lower labor costs. Baker et al. (2004) suggest that a hospital that expects fluctuating patient admissions is likely to use temporary staff in addition to permanent staff.
Other factors found to explain the increase in the use of temporary employees across industries include the value and extent of fringe benefits and health insurance (Abraham and Taylor 1996; Amenta 1977; Appelbaum et al. 2005; Coss 1989; Mangum, Mayall, and Nelson 1985), as well as several organizational characteristics of businesses, including whether the workforce is unionized, the size of the firm, and whether the business is located in a metropolitan area (Abraham 1990; Abraham and Taylor 1996; Davis-Blake and Uzzi 1993; Houseman 2001; Kalleberg 2000).
The use of temporary nurses can be seen as one way to overcome cost pressures and demand fluctuations in the health care industry. However, economic theories suggest that the extent to which hospitals can rely on temporary nurses for their staffing needs may depend on the local labor market. In particular, widespread persistent nursing shortages may contribute to increased temporary employment in the health care environment. Hospitals facing substantial unfilled vacancies may turn to temporary placement agencies to fill positions while recruiting permanent staff (Houseman, Kalleberg, and Erickcek 2003). Indeed, the Community Tracking Study’s nationally representative hospital survey collected data on the reasons for hiring temporary RNs from agencies; the main factor was reported to be persistent labor shortages (May, Bazzoli, and Gerland 2006).
A number of studies have surveyed hospital executives and nurse managers, who reported relying on temporaries agency staff due to labor shortages (Castle 2009; Lemow 2004; May, Bazzoli, and Gerland 2006). Most respondents in these studies did not view temporary staff as cost-effective, explaining that they have to pay a higher hourly wage to temporary RNs, in addition to administrative fees and overhead costs (May, Bazzoli, and Gerland 2006). The per-diem mark-up has been reported as ranging from 25 to 40 percent (Green 2004; Long, Goldfarb, and Goldfarb 2008). Employers also stated that they were reducing their reliance on temporary staff due to concerns over quality control, with only hospitals with severe shortages of nurses relying heavily on temporary staff (May, Bazzoli, and Gerland 2006).
One possible explanation for the link between labor shortages and agency employment is that hospitals can develop internal mechanisms to handle fluctuations in patient volume when the labor market is slack, but cannot do so when labor markets are tight. When there are a large number of workers available in a market, employers can easily form in-house, on-call worker pools. However, when labor markets are tight, workers can more easily obtain permanent employment with regular schedules, and employers find it more difficult to maintain robust flexible worker pools (Houseman, Kalleberg, and Erickcek 2003). This suggests that, during periods of perceived nurse shortage, nurse managers find it more difficult to get their regular staff RNs to work overtime, to float across units, and to be on-call. Indeed, during the last nursing shortage, First Consulting Group, American Hospital Association (2001) reported that one hospital paid permanent RNs US$6,000 bonuses to work undesirable shifts. The flexibility of temporary nurses in working shifts that are difficult would make such temporary hires attractive to hospitals during tight labor markets.
Rising vacancy rates also lower the probability that hospitals can find qualified nurses with the desired specialization and experience (Goodman-Bacon and Ono 2007). Working with a staffing agency that has access to a nationwide network of qualified nurses may help hospitals staff vacant positions without the added time and expense of recruitment (Houseman, Kalleberg, and Erickcek 2003).
Agency nurses thus fill two roles. When a hospital has a large number of unfilled vacancies, there is greater demand for agency nurses to fill these vacancies pending the recruitment of permanent staff. Nurses from agencies are also used to fill short-term staffing needs that would otherwise have been staffed by staff nurses working overtime hours or being on-call to come to work as needed. Even though employers pay a substantially greater hourly rate to use agency nurses as compared with regular employees, they save hiring time and recruitment costs that would have been required to fill either vacant permanent positions or short-term vacancies. They also save the costs associated with permanent employees, such as health care and vacation benefits.
Note that while the literature on human resource practices focuses on the demand side of the labor market, the ultimate employment of temporary nurses is simultaneously determined by both supply and demand. There is a series of papers that focuses on the supply side of the labor market to explain the growth in temporary employment (Bellemore 1998; Goodman-Bacon and Ono 2007; Houseman, Kalleberg, and Erickcek 2003; Long, Goldfarb, and Goldfarb 2008). These studies suggest that labor shortages contribute to the increase in the number of nurses who prefer temporary positions. During periods of shortages, nurses have less concern about their ability to find stable work, and thus may favor temporary positions that offer flexibility in both scheduling and the work environment. Nurses who are considering moving to a different area of clinical practice may treat temporary work as an opportunity to explore new fields (Long, Goldfarb, and Goldfarb 2008). Indeed, Goodman-Bacon and Ono (2007) found that having more vacant positions in a market increased the probability that a nurse would chose to work as a temporary nurse.
These previous studies reveal organizational and market characteristics that may explain the employment of temporary nurses. This study is the first to examine the problem empirically using hospital-level data regarding the number of temporary nursing staff, combined with organizational and market characteristics from multiple years. We leverage the panel data to control for time-invariant organizational characteristics that may determine the types of operating strategies that individual hospitals choose to adopt, as well as for time-variant market shocks.
Method
Data
To study the factors that affect demand for temporary personnel, we analyzed data from California’s Office of Statewide Health Planning and Development (OSHPD) from 1993 through 2002. The period 1993 through 1997 was marked by a surplus of RNs in California, while there was a shortage after 1998 (Buerhaus, Staiger, and Auerbach 2003; Friss 1994; Kimball and O’Neil 2002). Although the perceived shortage continued through at least 2007, we did not include data after 2002 because our findings might be confounded by the implementation of regulations mandating minimum nurse-to-patient ratios in California (Bolton et al. 2007; Donaldson et al. 2005; Mark et al. 2012; Serratt et al. 2011).
All non-Federal hospitals are required to report financial, utilization, and staffing data to OSHPD. We limited our analysis to short-term general acute care hospitals, excluding children’s, psychiatric, specialty, and long-term care hospitals. We also excluded Kaiser Foundation hospitals because they did not report staffing data in all of the years of this study.
The OSHPD Hospital Annual Financial Disclosure Reports provide data on productive hours worked by RNs, licensed vocational nurses (LVNs), unlicensed aides and orderlies, and temporary personnel. Productive hours are defined as all paid hours excluding sick, vacation, and education hours. Average hourly wages also are reported. Detailed information about the hours worked by and wages paid for registry agency personnel became available through a separate page of the survey starting in the 1992/1993 fiscal year. We analyzed data for nurses employed in daily service units, which exclude ambulatory care and ancillary services.
The OSHPD data provide other important variables including patient days, Medicare and Medicaid shares of total patient days, ownership (for-profit, not-for-profit, government, etc.), teaching status, and the amount of medical or pension benefits paid for regular staff. Data on the presence of nursing unions and the system affiliation of hospitals were obtained from unique data sets developed at the University of California, San Francisco, Center for the Health Professions. The data on regional and market characteristics are from RAND California statistics files and County Business Pattern files. Data on the annual number of nursing student graduates are from the U.S. Department of Education’s Integrated Postsecondary Education Data System (IPEDS).
We excluded from the analysis observations that had missing data for key variables. We included hospitals that closed within the time period of this study, and thus our panel is unbalanced. The final data set had 326 to 345 hospital observations per year.
Statistical Model
To investigate hospital use of agency nurse staffing, we estimated labor demand models in which demand for nursing is derived from patient needs, hospital characteristics, and structural features of the health care market (Mark, Harless, and McCue 2005; Spetz 1999). The empirical model is
where H is the work hours for agency temporary nurses, W
The dependent variables measure how much a hospital relies on temporary nurse labor. Some hospitals have zero values, because they did not employ temporary labor during the time period of this study; of the 2,109 hospital-year observations, temporary labor was not used in 506. We assigned these observations the value of one agency nurse hour, so the logarithmic-dependent variable could be calculated.
In the demand model, we included the hospital-level hourly wages of agency nurses as well as the wages of in-house RNs. In addition, fringe benefit costs were measured as the annual benefit expenses divided by the total labor expenses at the hospital; in the OSHPD data, these are not reported specifically for any labor group and thus our measure is a hospital-wide average. Patient need was measured with total patient days in daily hospital units. To control for variation in the complexity or severity of patients, we included the hospital’s case mix index from Medicare files.
In addition to the covariates stated earlier, we added a variable to measure the uncertain nature of patient volume. Although fluctuations in patient census can lead employers to increase hiring of temporary workers (Abraham and Taylor 1996; Baker et al. 2004; Houseman 2001), some portion of monthly or seasonal fluctuations in census may be anticipated by hospital administrators familiar with the patient flows of their hospitals (Baker et al. 2004; Gaynor and Anderson 1995; Friedman and Pauly 1981). It is the unpredicted portion of variation that is more likely associated with temporary work arrangements (Baker et al. 2004). To decompose the variation in patient days, we estimated forecasting regressions of the following form for each hospital year as in Friedman and Pauly (1981). The forecasting equation included three lags for inpatient days and a time trend. The measured differences between predicted variation and actual variation—that is, residuals from the regression—were used as the measure of the unexpected demand faced by each hospital:
We estimated this equation excluding data prior to 1996, due to the lag structure of the equation. Since we had a relatively short time series for each hospital (ten years), we were unable to forecast expected patient days for each hospital with the pure time series methods used by Friedman and Pauly (1981). Rather, we exploited the cross-sectional as well as the time series variation in the data to generate forecasts for expected output for each hospital by grouping the hospitals by geographic area. Adapting the method of Gaynor and Anderson (1995), hospitals that were in the same Metropolitan Statistical Area (MSA), and hospitals in non-MSA areas, were pooled. Since hospitals in the same area share common shocks specific to their market, pooling hospitals in this manner provides a reasonable approach to forecasting patient days (Gaynor and Anderson 1995).
To control for market characteristics that are associated with shifts in nurse demand, we included Health Maintenance Organization (HMO) penetration and the number of HMOs in a given county for each year. We expect these measures to capture the financial pressure placed on hospitals by managed care. Also included are urbanicity, population density per square mile, population over sixty-five in each county, and inflation-adjusted per capita income in thousands of dollars. Other covariates associated with hospital characteristics include Medicare and Medicaid shares of total patient days, ownership, teaching status, system affiliation, and whether RNs are unionized. To control for competition among hospitals, we calculated a county-level hospital Herfindahl Index, HHI = Σ si2, where si is the share of total discharges at each hospital i. 1 We included indicators for two time periods to account for changes in the overall RN labor market. One indicator was for the years 1996 to 1998, which was a period of RN surplus, and the other indicator for 2000 to 2002 represented a period of surplus; 1999 is the reference year.
Two issues might bias our results. The first concern is that some hospitals have zero values for the dependent variable. We retained these observations in our models, as described earlier, but there may be systematic differences between hospitals that use and do not use temporary labor. To formally test for the possibility of nonrandom selection, we estimated Heckman sample selection correction models to identify variables that predict the decision to use temporary labor. The selection portion of the model included all the covariates of the demand model; we could not identify any variables that might predict nonuse of temporary nurses that could be excluded from the demand equation. We found that several variables affect the likelihood of employing temporary nurses, including the number of patient days, the expected number of patient days, and some of the market characteristics. However, in the second stage, we found that the selection variables affect the likelihood of being censored out of sample but that the hypothesis that Heckman’s “lambda” is zero is accepted (p = .471). Thus, there is no strong evidence that estimates from our model are biased by the zero-value observations.
A second possible source of bias is that RN wages and temporary RN wages may be endogenous with the dependent variable of demand for temporary RNs. Instrumental variable regression can yield unbiased estimates of wage effects; in this case, we need to identify two variables that are related to the wages of permanent and temporary RNs, but are not directly related to demand for temporary RNs. We reestimated our demand equations using two instrumental variables that have been used in prior research, county unemployment rates and new graduates from RN training programs in the county (Spetz 1999; Tellez et al. 2009), both of which would be expected to affect the supply of RNs but not have a direct effect on demand. When unemployment rates are higher among the general population, there is an increased likelihood that RNs’ spouses or partners are unemployed, and thus RNs are more likely to work to ensure adequate household income. This increased supply will affect wages, but will not affect demand. RN graduations are largely determined by the resources dedicated to public colleges and universities for nursing education in prior years, because nursing education requires three to four years of study (Seago and Spetz 2002). Higher numbers of graduates will increase total supply and thus wages, but not directly affect demand. While wages might affect graduations, this relationship is lagged by at least three years and thus graduations are not contemporaneously affected by wage changes.
The first-stage equations for the Instrumental Variable (IV) estimation showed that the instruments are not strong. The F-statistic was 9.696, which does not exceed the critical Stock–Staiger value of 10, and fell well below more recent criteria established by Stock and Yogo (2005). Shea’s partial R2 had a small value (.021), which also indicates that the instruments are weak or irrelevant. These results suggest that we cannot use these instruments without conceding that they may produce biased coefficient estimates. We searched for but could not find convincing additional instruments with a higher explanatory power for wages for nurses. Thus, we present only non-IV equations and note that the results cannot be interpreted as causal.
All models were estimated in a log-linear specification using fixed effects (FE) to control for both changes that uniformly affect all hospitals over time and hospital-specific time-invariant characteristics; these results were compared with equations that did not include fixed effects. We also examined the difference between fixed effects and random effects results; in some cases, the random effects estimator produces more efficient estimates of the coefficients. However, a Hausman test to compare the fixed effects and random effects estimators indicated that the random effects estimator is not appropriate, and thus we used fixed effects.
Results
Descriptive statistics for the study sample are summarized in Table 1. The proportion of agency nurse work hours among total RN work hours averages 7 percent (SD = 0.09) and ranges from 0 to 73 percent. The mean of registry nurse wage per hour is US$36.92 (SD = 16.27) in 2002 dollars. The mean staff RN wage rate is US$24.70 (SD = 7.23). About one-fourth of hospitals have unionized nurses. The number of new graduates per county ranges from 0 to 2,767.
Summary Statistics for California Hospitals, 1996–2002.

Source. OSHPD Annual Financial Disclosure Reports 1996–2002, IPEDS completions data files, RAND California files, InterStudy, and Current Population Survey Outgoing Rotation files.
Note. All monetary values are adjusted in the 2002 term; all nurse hour and patient day variables are adjusted to reflect 365 days in a year; New RN graduates are from IPEDS completion files with the CIP code of 51.1601 (RN training program). RN = registered nurse; LVN = licensed vocational nurse; MSA = Metropolitan Statistical Area; HHI = Herfindahl Index; HMO = Health Maintenance Organization; OSHPD = Office of Statewide Health Planning and Development; IPEDS = Integrated Postsecondary Education Data System; CIP = Classification of Instructional Programs.
Table 2 presents the yearly data on the mean number of agency hours and the average proportion of agency to total RN hours. Between 1993 and 2002, the proportion of registry nurse hours increased fivefold—rising from 3.5 percent (2,051,000 hours) of total regular staff RN hours in daily services to 17.9 percent (12,497,000 hours) of total regular staff RN hours in daily services.
Registry Nurse Hours (Thousands) and the Proportion of Total RN Hours in Daily Service Units of California Hospitals.

Note. RN = registered nurse; OSHPD = Office of Statewide Health Planning and Development.
Registry hours are adjusted to reflect 365 days in a year. Many OSHPD reports begin on March 1 or September 1 as these are also starts of traditional quarters. I checked if the reporting period was 365 (or 366 in leap years) and adjusted nurse hours to calculate yearly equivalent. The formula was adjusted hours = 365/days in year * hours, where days in year is the number of days in their reporting.
Average proportion is computed as total registry nurse hours in each hospital in a given year divided by the total RN hours (RN hours plus registry nurse hours).
Table 3 presents estimates of the demand for registry nurse hours from our multivariate regressions. The regressions include data from 1996 through 2002 because the measure of the uncertainty of patient census could not be computed prior to 1996. The first two columns present generalized linear model (GLM) coefficients and standard errors, and the second two columns present the results from GLM with fixed effects. 2 Consistent with previous studies, the demand for registry nurse drops with their wages and rises with the level of fringe benefits in both the GLM and FE models. A 10 percent increase in the level of fringe benefits is associated with a 20 percent increase in the demand for temporary nurse hours in the FE model, and a greater increase in the GLM model. The volume of patients cared for at a hospital has an important effect on demand for registry RNs. In the fixed effects model, 10 percent growth in the number of inpatient days is associated with about 18 percent greater demand for temporary nurse hours. This relationship is larger in magnitude in the GLM equation (coefficient = 2.09, p < .01) than it is in the fixed effects equation (coefficient = 1.75, p < .01). The difference may be due to the effects of some unknown factor inherent to each hospital such as differences in managerial capacity, that is, the manager of hospital A (say) is well experienced or able to forecast increases in patient volume and thus hospital A does not have to hire temporary nurses to meet peak patient demands; hospital B (say) with less experienced managers does not do so. Without addressing this effect, hospital B is predicted to hire more temporary nurses by about 20.9 percent compared with hospital A as patient volumes increase by 10 percent. With addressing the effect of managerial capacity, the magnitude of the effect of changes in patient volume appears to reduce, 17.5 percent. As the predicted proportion of variation in patient volumes increases, demand for temporary nurses decreases. Conversely, demand for temporary nurses rises with patient volume fluctuation in the GLM model, which is difficult to predict. Medicaid and Medicare shares of patient days are negatively associated with temporary nurse employment in both the GLM and FE models.
Estimates of Demand for Registry Nurse Hours in Daily Services Units of California Hospitals, 1996–2002.

Source. OSHPD Annual Financial Disclosure Reports 1996–2002, RAND California files, and Managed care data, case mix index, and union data at hospital level from Spetz.
Note. GLM = generalized linear model; RN = registered nurse; LVN = licensed vocational nurse; OSHPD = Office of Statewide Health Planning and Development. The dependent variable is log(Registry nurse hours in daily service units).
p < .10. **p < .05. ***p < .01.
In general, the inclusion of fixed effects causes the coefficients of many hospital characteristics to become statistically insignificant, likely because these characteristics have primarily a cross-sectional relationship with temporary RN demand. With fixed effects, the coefficients measure the impact of a change in the characteristic for a given hospital. For example, the GLM model indicates that greater HMO penetration is associated with greater use of temporary RNs, but the fixed effects model estimates that managed care does not significantly affect the use of agency nurses. Thus, the impact of HMOs on temporary RN demand primarily occurs across hospitals based on HMO penetration, rather than for a specific hospital as its own HMO share changes. The competition between hospitals within a county market, system affiliation, rural location, a more aged population, and population density were significantly related to the use of agency nurses only in the model that did not include fixed effects. For-profit hospitals were estimated to have greater demand for temporary RNs in the GLM model, but had no significant association with demand in the fixed effects model. We did not find evidence that level of unionization affects the demand for agency nurses.
The coefficients of the time indicators in both the GLM and fixed effect models show significant changes in demand for temporary staffing as the RN labor market transitioned from surplus (1996–1998) to shortage (2000–2002). As an RN shortage emerged in 1999, demand for agency nurse hours rose by about 80 to 90 percent.
Table 4 presents estimates of the share of nursing hours provided by temporary agency nurses relative to total RN hours. The results are qualitatively similar to those for the level of temporary RN hours. Relative demand for registry nurses drops with average hourly earnings of registry nurses in both GLM and fixed effect models (p < .01). Patient fluctuations and the level of fringe benefits are positively associated with the share of nursing hours for temporary agency nurses. The use of temporary RNs was higher during the period of RN shortage than in earlier years. Medicaid and Medicare shares of patient days are negatively associated with the share of nursing hours. Unionization does not have a significant effect on the share of agency RNs.
Estimates of Relative Demand for Nursing Hours Provided by Registry Nurses.

Source. OSHPD Annual Financial Disclosure Reports 1996–2002 and various sources.
Note. The dependent variable is log(Registry nurse hours as a proportion of total RN hours in daily services units). GLM = generalized linear model; RN = registered nurse; LVN = licensed vocational nurse; OSHPD = Office of Statewide Health Planning and Development.
p < .10. **p < .05. ***p < .01.
Discussion
This study investigates changes in demand for temporary staff as the RN labor market transitioned from surplus to shortage. We found a significant trend toward higher use of agency nurses during the years of labor shortage. Agency nurse hours as a proportion of total RN hours also grew. Consistent with previous studies, these findings indicate that hospitals use temporary contract nurses to deal with RN shortages (Grumbach et al. 2001; Houseman, Kalleberg, and Erickcek 2003; Long, Goldfarb, and Goldfarb 2008; May, Bazzoli, and Gerland 2006). This may mitigate the need to raise wages for new and existing nurses during a shortage; consequently, wage growth for permanent staff RNs may be slower. Researchers and leaders in the field of nursing have raised concerns about this cycle, because it could lead to further shrinkage of the labor supply (Houseman, Kalleberg, and Erickcek 2003; May, Bazzoli, and Gerland 2006; Nevidjon and Erickson 2001).
Besides the shortage of nurses, several other forces influence hospital demand for agency nurses. Previous studies view the use of temporary workers as one way to reduce overall employment-related costs and address demand fluctuations. The present study found that high benefit expense is associated with increases in both the level and share of temporary nurses. We also found that variation in patient care demand is linked with increases in agency nurse employment.
These findings in part support the theory that hospitals use temporary nurses to overcome cost pressures in the health care industry (Abraham and Taylor 1996; Baker et al. 2004; Cohany 1998; Kandel and Pearson 2001; Mobley and Magnussen 2002). It has been hypothesized that temporary staffing arrangements are attractive to funds-constrained hospitals that are more likely to suffer from shortages, such as those that serve high shares of low-income patients (Cramer et al. 2006; Long, Goldfarb, and Goldfarb 2008; Seago et al. 2001). However, we found that district and government hospitals do not have significantly different demand for temporary staff. The demand for agency nurses was lower in hospitals that have a higher share of Medicaid and Medicare inpatient days. We also examined the influence of changes in HMO penetration, and found that it was not related to hospital employment of agency RNs, either in levels or relative to the total number of RNs.
To better understand how shortages affect decisions made by hospitals about the ideal mix of permanent and temporary staff, empirical evidence relating agency work arrangements to hospital cost should be pursued. Although using agency temporary nurse reduces hospitals’ fixed costs of employee benefits and the cost of addressing demand fluctuations, it does not necessarily follow that the use of agency nurses is cost-effective. For example, Bloom, Alexander, and Nuchols (1997) found that hiring agency temporaries involved higher operating cost, compared with overtime and float pools, due to higher administrative and overhead costs. Future studies need to examine whether the high wage costs of temporary nurses are higher for the marginal nurse hour than what would be paid for permanent staff—including costs associated with screening, training, and recruitment. Little is known about relative cost-effectiveness of temporary work arrangements, compared with internal mechanisms to improve labor efficiency such as requesting overtime work or using float pools from the regular workforce. Moreover, the quality effect of employing temporary nurses should be compared with the risk to patients of low RN staffing levels. One recent study has found no negative association between the use of supplemental nurse staffing and the quality of care, largely because maintaining adequate overall nurse staffing levels was a stronger predictor of patient safety (Aiken et al. 2007). Continued empirical research that can guide the use of agency RNs should be encouraged.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.