Abstract
For centuries, Black communities have responded to health discrimination and inequality by creating institutions to meet local health needs. Mid-20th-century spatial transformations helped catalyze two distinct conversations about emergency medical care. One focused on accidental death and disability in response to rising fatalities on the nation’s new highways and sprawling suburbs. Another was raised in Black communities creating their own paths toward critical care amidst racialized urban disinvestment. These conversations are fundamentally intertwined. The dominant narrative situates the origins of the emergency medical services system in the United States in the context of suburban highway development, increasing traffic fatalities, and advances in emergency medicine from wars in Korea and Vietnam. The most significant advances in emergency medical services at that time, however, came from doctors and Black paramedics in Pittsburgh organized through a local civil rights organization Freedom House Enterprises. Drawing on archival documents and secondary sources about early ambulance services along with the legislative history of the Emergency Medical Services Systems Act of 1973, this research highlights how several dimensions of contemporary emergency medical services training and standards in the United States emerged from civil rights struggles. It focuses on the pivotal role of Freedom House and its legacy for emergency medical services, and ties these together with shifts in urban planning and policy, in particular the Model Cities Program. This history illuminates the significance of pre-hospital emergency care in health equity and its implications for urban justice today.
Introduction
Economic and racial inequality are central concerns in urban theory and practice, and are acutely visible in the profound health disparities by wealth, race, and geography that characterize metropolitan areas in the United States and beyond (Arcaya and Schnake-Mahl, 2017; Kawachi and Berkman, 2003; Williams and Collins, 1995). Planning practices and land use regulations have contributed to neighborhoods that are separate and unequal by wealth and by race, with divergent levels of local resources and exposures to hazards that together have lasting impacts on health (Bullard, 1990; Corburn, 2004; Fullilove, 2004; Kramer and Hogue, 2009; Pulido, 1996; Sze, 2007; Taylor, 2014; Williams and Collins, 1995). The fields of urban planning and public health have long been intertwined (Botchwey et al., 2014; Corburn, 2004, 2007; Forsyth et al., 2010; Northridge and Freeman, 2011; Schnake-Mahl et al., 2020). Puzzlingly, however, there is little discussion in urban studies scholarship of an institution fundamental to public health and equitable health provision—emergency medical services (but see Quick et al., 2019). Emergency medical technicians (EMTs) interact directly with city residents in their communities on health issues, and emergency medical services are a crucial lever for health equity, as a service that all city residents may require at some point in their lives but that disproportionately serves low-income residents.
The lack of attention to emergency medical services in urban studies and planning research may be because this public service can seem, at first glance, distant from urban policy and land use regulation. But analysis of archival documents and legislative history reveals how the development of an emergency medical services system in the United States is intertwined with post-war shifts in urban planning and federal funding as well as the racialized transformation of the American urban form. The first highly trained paramedics in the United States were members of a community-based civil rights organization in Pittsburgh called Freedom House Enterprises, created by Black leaders including civil rights organizer James McCoy Jr in response to urban disinvestment and discrimination. They worked together with Dr Peter Safar, the anesthesiologist who pioneered cardiopulmonary resuscitation, and with medical director Dr Nancy Caroline, who went on to write the first, and still the predominant, paramedic textbook, Emergency Care in the Streets (Caroline, 1979).
Congress enacted federal legislation supporting the creation of an emergency medical services system in 1973 to operationalize advances in pre-hospital medical care. The model that Congress drew from was created in part by the members of Freedom House Enterprises in Pittsburgh’s Hill District, working with Dr Safar, Dr Caroline, and others, to address concerns about healthcare quality and access. As in the 1960s, attention to emergency medical services today can help generate new knowledge about social, political, and environmental determinants of health and serve as an important avenue through which to improve health.
Below, we briefly review literature on the intersection of urban planning and public health. We then analyze how the development of an emergency medical services system in the 1960s and 1970s was intertwined with shifts in urban development and the struggle for economic and racial justice in the United States.
Entangled from the start: Cities, ambulances, and inequality
Like most social phenomena, public health has a notable spatial structure (Arcaya et al., 2024; Brennan et al., 2025; Krieger, 2011; Sampson, 2012). The fields of public health and urban planning emerged in part in response to the spatial structure of ill-health caused by industrialization and urbanization in the 1800s, in particular to address repeated outbreaks of infectious diseases related to poor water and sanitation infrastructure in cities (Corburn, 2004). For instance, as New York City industrialized and grew in the middle of the 19th century, economic inequality widened, mortality rates climbed, and doctors and public health advocates published Sanitary Condition of the City in 1865, describing a relationship between housing, sanitation, and public health that led to state legislation establishing a Metropolitan Board of Health (Citizens’ Association of New York Council of Hygiene and Public Health, 1865).
The first superintendent of the Metropolitan Sanitary District in New York City was Edward Dalton, a doctor trained at the nation’s first public hospital, Bellevue (Oshinsky, 2016). As Dalton worked to systematize sanitary inspections in New York City, he also realized that poor residents had no reliable, rapid way of arriving at the hospital in case of severe injury or illness. Dalton pushed for the creation of an ambulance to transport acutely sick and injured patients. By 1869, Bellevue had two custom-designed horse-drawn ambulances, each staffed by a surgeon and a driver and with space for two patients lying down, described contemporaneously as a “portable emergency room” (Oshinsky, 2016: 114). Bellevue’s ambulances were followed by ambulances associated with other urban public hospitals, representative of the central role public hospitals played in developing early urban emergency medical systems (Bell, 2012).
As cities sprawled in the 20th century, the reach of the few hospital-based ambulance services was limited, and more options for the transportation of the sick and injured developed, primarily the use of morticians’ hearses or police wagons (Safar, 2001; Simpson, 2013). But the reliability of even these rudimentary services was questionable, especially for Black Americans who frequently received delayed services or were denied services altogether (Benson et al., 1972; McCormick, 1974). In the face of this discrimination, Black communities created their own lifesaving institutions, such as the Burrell Memorial Hospital in Roanoke, Virginia (founded by a group of Black physicians after their Black colleague died from being denied surgical care) and the Hunton Life Saving and First Aid Crew, formed in December 1941 to provide first aid and transportation in Roanoke. Founders of the Hunton organization noted that unequal access to emergency medical care was built into the physical infrastructure of Roanoke as Black neighborhoods were on the far side of the railroad tracks from fire stations and most hospitals, with few crossing points, delaying access (Kelly, 1996; Liu et al., 2021).
Suburbanization and urban disinvestment catalyze emergency medical services innovation
After soldiers returned from the Second World War, the 1944 Servicemen’s Readjustment Act or G.I. Bill (P.L. 78-346) provided veterans with access to subsidized mortgages for housing, but racially restrictive covenants encouraged by the Federal Housing Administration, redlining, and other discriminatory practices denied Black veterans entry to rapidly developing suburbs and mortgage financing to purchase or renovate homes even in predominantly Black neighborhoods (Katznelson, 2005; Muhammad, 2011; Steil and Charles, 2021; Taylor, 2014). As many white Americans moved to new suburban developments after the war, the Housing Act of 1949 began the process of urban renewal by providing federal financing for “slum clearance” programs. Famously described by James Baldwin as “Negro removal,” urban renewal programs generally targeted neighborhoods where Black Americans and working-class immigrants lived, often to make way for highways or other infrastructure (Fullilove, 2004; Steil et al., 2021; Sugrue, 1996; Thomas, 2013).
In 1956, President Dwight Eisenhower signed the Federal Aid Highway Act (P.L. 84-627), authorizing US$25 billion for the construction of 41,000 miles of interstate highways, subsidizing private car ownership and chipping away at robust public transportation systems (Crockett, 2018; Nall, 2018). With the federal government paying for 90% of highway construction costs, states rapidly expanded highways, tearing through poor and working-class urban neighborhoods and displacing communities of color and immigrant communities in the process (Crockett, 2018; Fullilove, 2004). Together, urban renewal, federal highway construction, and federally subsidized mortgages transformed metropolitan areas across the United States, facilitating sprawling segregation, metropolitan fragmentation, and urban inequality (Fullilove, 2004).
One consequence of this transformation of urban form was increasing rates of accidental death and disability, related in part to the growing number of vehicle miles traveled. On the 1960 presidential campaign trail, John F Kennedy labeled traffic accidents “perhaps the greatest of the nation’s public health problems,” and in 1965 consumer advocate Ralph Nader published his report on automobile safety, Unsafe at Any Speed. In its 1966 whitepaper entitled Accidental Death and Disability: The Neglected Disease of Modern Society, the National Research Council (1966: 5) called the accidental injuries that at the time were the leading cause of death in the first half of a person’s lifespan the “neglected epidemic of modern society” and “the nation’s most important environmental health problem.” The whitepaper (National Research Council, 1966: 5–6) highlighted the need for improved emergency medical services, noting that “few are adequately trained in the advanced techniques of cardiopulmonary resuscitation … or other lifesaving measures” and that “local political authorities have neglected their responsibility to provide optimal emergency medical services.” The collective attention to traffic accidents led Congress in 1966 to pass the National Traffic and Motor Vehicle Safety Act (P.L. 89-563), creating the National Highway Safety Bureau and empowering the federal government to set safety standards for motor vehicles and highways. The 1966 Act also created a Division of Emergency Treatment and Transfer of the Injured, focused on emergency medical services. That Division provided some funding to states and localities for emergency medical services but did little to require states or localities to actually provide improved pre-hospital emergency care.
At the same time, another consequence of the transformation of U.S. metropolitan areas by federal housing and highway acts was increasing urban disinvestment, and mobilization in urban communities to address continued unmet health needs.
Responding to urban disinvestment through the creation of emergency medical services programs
Black doctors and city residents knew that public health broadly and the health of Black communities in particular was intertwined with housing, transportation, and urban policy as well as discrimination in medical care, and they highlighted the negative consequences of urban inequality on Black residents’ access to healthcare, quality of care, and overall health outcomes (McBride, 1991; Nelson, 2011; Roberts, 2009; Tyner, 2006). The National Association for the Advancement of Colored People (NAACP) and the National Medical Association, the leading professional organization for Black doctors, fought for decades against medical segregation and discrimination (see e.g. Simkins v. Moses H. Cone Memorial Hospital, 323 F.2d 959 (4th Cir. 1963)). To meet the health needs of Black people in the face of discriminatory treatment, civil rights advocates and healthcare providers also pursued a parallel path of building Black-led health institutions, from the creation of Provident Hospital in Chicago in 1891, to the Black Cross Nurses of the Universal Negro Improvement Association in the 1920s, to model healthcare clinics organized by the Student Nonviolent Coordinating Committee and the Medical Committee for Civil Rights in conjunction with the 1964 Freedom Summer campaign (Nelson, 2011).
As Alondra Nelson (2011: 5) writes, “In settings where racial oppression was more commonly advanced through social abandon … and social control … than through staunch Jim Crow practices, health was a site where the stakes of injustice could be exposed and a prism through which struggles for equality could be refracted.” Black activists in the 1960s in multiple cities sought to create community-controlled institutions to meet the health needs in Black communities that were being ignored by public officials, including supporting Black residents’ health through paramedicine (Bassett, 2016; Nelson, 2011).
Freedom House Enterprise Ambulance Service
In Pittsburgh, the Lower Hill, located between downtown and the University of Pittsburgh, was the business area for Pittsburgh’s Hill District, and long home to a diverse population of immigrants including Jewish, Italian, Polish, Greek, Syrian, and Irish immigrants and their descendants, and, in the 12th century, a steadily rising share of African American residents (Handley, 2024; Hazzard, 2022). The diverse and vibrant neighborhood was a center for theatre, jazz music, and the arts. Nevertheless, when white civic and business leaders began the Allegheny Conference on Post-War Community Planning in 1943 and the Pittsburgh Urban Redevelopment Authority in 1946, they described the Hill District as deteriorated, blighted, and ripe for urban renewal (Handley, 2024; Fullilove, 2004). As urban renewal decisions were made in Pittsburgh, “[c]onspicuously absent from the picture, and from the decision-making processes, were poor people, black people, and women” (Fullilove, 2004: 60). Using federal funds from the Housing Act of 1954, city officials authorized the demolition of much of the Lower Hill in 1956 and the construction of a sports arena, delivering negligible social and economic benefits to previous residents and failing to build promised new affordable housing (Handley, 2024).
In response, the Hill District Home Owners and Tenants Association brought public officials on a tour of the Middle Hill in 1957 to challenge the claim that their neighborhood was blighted, aiming to stop the city officials from demolishing the Middle Hill and Upper Hill as they had the Lower Hill (Handley, 2024). But the city continued to procure federal funds to clear parts of the Middle and Upper Hill as well (Handley, 2024). In response, steelworker and community organizer James McCoy Jr, realtor Robert Lavelle, and businesswoman Frankie Pace created the Citizens Committee for Hill District Renewal (Glasco, 2010). Together with the United Negro Protest Committee, the Urban League, and the NAACP, the Citizens Committee for Hill District Renewal pushed for community input to influence decision making in development, and fought for the city to renovate homes rather than demolish and redevelop on a large scale (Handley, 2024). Residents created a map of their own vision of the future that contrasted the city’s plans, and reclaimed an intersection near the first round of demolition to develop “Freedom Corner,” a space to unite the community for civic engagement and collective action against urban renewal (Handley, 2024).
Even as urban renewal was uprooting residents, the Pittsburgh branch of the NAACP and its youth councils also led successful demonstrations against discrimination in other areas as well, including job discrimination in industries ranging from steel mills to construction to utilities (Collins, 2003). Representatives from the NAACP, Black churches, and other Black activist groups came together to form the United Negro Protest Committee in 1963 and elected James McCoy Jr from the Citizens Committee for Hill District Renewal to lead it (Collins, 2003). In addition to fighting employment discrimination, McCoy founded Freedom House Enterprises to create jobs within the Hill District by meeting local needs. Identifying the need for access to fresh produce as central to health and an opportunity for employment, one of the first projects was to create a mobile grocery store (Collins, 2003).
At the same time, reports circulated in the Hill District of police (who were the primary providers of hospital transport, by police “utility wagons”) not responding to medical emergencies, leading to residents of color receiving “medically inadequate” care or being denied access to needed emergency care altogether (Cheever, 1970; Edwards, 2019; Modern Hospital, 1969). In 1967, McCoy proposed the Freedom House Enterprise Ambulance Service (Freedom House). The leadership of Freedom House “figured if Freedom House could bring produce to a neighborhood that was lacking grocery stores, they could run a commercial service to transport people for hospital visits and routine checkups” (Staresinic, 2004: 33). “During the planning period, news of the project circulated in the community and resulted in several urgent requests for service” (Modern Hospital, 1969). In partnership with former ambulance attendant and community organizer Phillip Hallen, who at that time was director of the Maurice Falk Medical Fund, McCoy approached cardiopulmonary resuscitation innovator Peter Safar at the Presbyterian University-Hospital for advice on purchasing ambulances and obtaining training (Safar, 2001). The hospital agreed to provide ambulances and training as a pilot project in emergency medical services (Amato, 2019; Safar, 2001). Safar, working with medical resident Don Benson and technical director Gerald Esposito, designed an intensive nine-month training course that paired three months of classroom learning with clinical experience in the emergency room, operating room, intensive care unit, and delivery room for the members of Freedom House to treat critically ill patients, beginning in October 1967 (Amato, 2019; Safar, 2001).
Over the first two years, 44 residents of Pittsburgh’s Hill District learned how to respond to trauma, cardiac arrest, childbirth, environmental emergencies, and all manner of medical ailments (Benson et al., 1972). They learned advanced skills previously limited to doctors, including tracheal intubation, obtaining and analyzing electrocardiograms, and the administration of intravenous medications. Most of these paramedics had not finished high school, and the Pittsburgh Board of Education offered basic high-school-equivalent education as part of the training program (Modern Hospital, 1969). In the process, Freedom House and Safar developed a model of “mobile intensive care,” and the trainees became the nation’s most highly trained pre-hospital emergency medical providers (Benson et al., 1972). Unlike police or morticians, who lacked training beyond basic first aid, the Freedom House model ensured that paramedics had the medical knowledge needed to help people on scene, including by establishing intravenous access, administering a range of critical medications, using cardiac monitors, interpreting cardiac arrhythmias, defibrillating patients, intubating and ventilating patients, and providing other critical care (Cheever, 1970; Edwards, 2019; Frederick, 1972).
Local news sources highlighted the strengths of Freedom House compared to other emergency services (Cheever, 1970; Frederick, 1972). For instance, one contemporary observer noted that “[p]olice ambulance drivers are sometimes cynical about emergency calls, and occasionally turn them down,” complicated by the fact that “genuine emergencies are not always easy to diagnose” (Cheever, 1970). “The symptoms of diabetic coma, for example, closely resemble drunkenness. Freedom House ambulance drivers answer every call, even though in some areas as many as 85% of so-called emergencies are spurious” (Cheever, 1970). Police ambulances were required to transport patients to the closest hospital, even if it did not have the emergency facilities the patient needed or store their medical records (Cheever, 1970). Project manager Robert Zepfel emphasized that this could cause treatment delays and adverse patient outcomes, and “Freedom House ambulances will take patients to any hospital within reason” (Cheever, 1970). According to a study surveying 1421 patients at Presbyterian, Mercy, and Allegheny Hospital, “the level of ‘inappropriate’ prehospital care was 11% for Freedom House; the police, 62%, private ambulances and volunteer fire companies, 79%; and private cars, 77%” (Frederick, 1972: 2). In 1972, Freedom House became the first service in the county to be equipped with ongoing radio communications with a doctor, who could pass on instructions to EMTs and paramedics during emergency treatment (Frederick, 1972: 1).
As important as the high quality of its medical care, Freedom House created a sense of respect and pride in pre-hospital emergency care within the community. Hill District resident Lorraine Green recalled how many residents felt that the police, transporting Hill District residents to the hospital, did not treat them with dignity, but that that changed with Freedom House: There was a warmth there. You felt all connected … You’d see the young people and the older people waving at them and hollering at them. It was the biggest thing … I don’t think I’ll ever forget the way they made me feel. (Srikameswaran, 1997).
Seeking funding amidst urban policy shifts
The program faced many challenges, including the “reluctance of the city’s mayor to let FHE [Freedom House] provide city-wide services” and “suspected racial prejudices with white police officers eager to maintain control of ambulances city-wide” (Safar, 2001: 6). These two challenges were intertwined with the biggest obstacle Freedom House faced: funding.
The struggle to fund Freedom House reflected a larger context of political tensions between local governments and community-based advocacy organizations over federal funding. Early on, Freedom House accessed funds from the federal Office of Economic Opportunity (OEO) through Community Action Pittsburgh, one of the “community action agencies” (CAAs) that OEO supported across the country after the 1964 passage of Economic Opportunity Act (P.L. 88-452; DeFilippis, 2004; Pittsburgh Courier, 1969). “The heart of the CAA initiative was community empowerment and activism, and the underlying philosophy of the Community Action Program … was the ‘maximum feasible participation’ of community members” (DeFilippis, 2004: 41). The funding from Community Action Pittsburgh enabled Freedom House to leverage funds from private sources, and to work in partnership with the Pittsburgh Board of Education and Presbyterian University Hospital to train the first EMTs (Pittsburgh Courier, 1969).
Many mayors, however, felt threatened by the OEO bypassing city halls to give federal funds directly to local organizations emphasizing maximum feasible participation of the poor (and often challenging incumbent elected officials and their policies; DeFilippis, 2004: 41–42). Through the Demonstration Cities and Metropolitan Development Act of 1966 (P.L. 89-754), the federal government then created the Model Cities program to give money to local governments to then distribute to local community organizations for locally developed plans instead (Marrero, 2016). Grassroots groups were often faced with the decision to maintain a political identity they had formed through community action agencies and face the potential loss of federal aid, or move toward professionalized development models and seek closer partnerships with local government in order to access Model Cities funding (DeFilippis, 2004; Hetzel and Pinsky, 1969). Freedom House initially deftly navigated the shift in the federal policy landscape and received both Model Cities funding and additional local funds from Pittsburgh, which contracted with Freedom House to provide ambulance service for the Hill and Oakland neighborhoods (Long, 1971; Pittsburgh Post-Gazette, 1968). Pittsburgh Mayor Barr offered some support, noting that “The new emergency service will relieve police of many ambulance cases, thus freeing them for direct law enforcement activities” (Pittsburgh Post-Gazette, 1968). In 1969, Freedom House used federal OEO funds from the Manpower Development and Training Act as well as a US$100,000 contract with the City of Pittsburgh to expand Freedom House’s service (Stuart, 1970).
The city contract with Freedom House meant that the new ambulances provided emergency care to 4647 patients in their first year in service, including five cases of cardiac arrest where patients subsequently made a full recovery and left the hospital (Benson et al., 1972). In 1970, the Model Cities program contributed US$232,000, facilitating the expansion of the program (Frederick, 1972). At the same time that Model Cities funding was helping the ambulance service grow, however, Mayor Peter Flaherty was elected to succeed Mayor Barr and Flaherty subsequently halved the city’s contributions to US$50,000 (Stuart, 1970). Mayor Flaherty then turned ambulance services downtown back to the city police, without updating their emergency medical skills (Safar, 1975; Srikameswaran, 1997; Stuart, 1970). As Flaherty was cutting local funds, Freedom House’s OEO funds also ran out, leaving declining Model Cities Program funding and, eventually, US$25 fees from patients who could pay (McFeatters, 1969; Stuart, 1970). As a contemporaneous observer reported, “Although FHE handled sixteen percent of all the emergency calls in the City of Pittsburgh in 1972, city government continues to pay FHE only $50,000 per year. The balance of this agency’s income comes from fees paid by private patients” (McCormick, 1974).
Relying on fees from patients as local and federal funding declined was not sustainable. Nancy Caroline, the Freedom House Medical Director, commented that the city administration was “opposed to … expenditures on prehospital care,” but in March 1974 Mayor Flaherty announced that he would create a city-led ambulance service and dissolve the Freedom House service (Caroline, n.d.).
In June 1974, Pittsburgh residents, NAACP representatives, Freedom House staff, and members of other community organizations came together in the city council chambers to support the continuation of Freedom House (Flipping, 1974). As one local newspaper reported, “The mere thought of the phasing out of Freedom House has offended the citizenry of Pittsburgh who feel that it should not only be continued … but expanded throughout the entire city” (Flipping, 1974). Eugene Key, who had worked with Freedom House since its founding, “[saw] both political maneuvering and racial discrimination behind the move to phase out the Freedom House ambulance program” (Moyle, n.d.). Faced with opposition from Mayor Flaherty and loss of funding, the Freedom House ambulance service closed in 1975 (Safar, 2001). The Mayor signed a Memorandum of Agreement with Freedom House, promising to provide jobs to Freedom House paramedics without unneeded recertification, a training program to basic level for EMTs which they could retake if they failed the first time, and a course for dispatchers on working in the area—but “[o]ver the ensuing months, all of these promises were broken” (Caroline, n.d.). Some of the pioneering paramedics of Freedom House eventually worked for the new city service, and others became pioneers in emergency medical services elsewhere (Hazzard, 2022). In Caroline’s words, “I cannot escape the feeling that they were cheated somehow … How many people, not only in Pittsburgh, but all across the country, owed their lives to the pioneering work done at Freedom House over 8 years?” (Caroline, n.d.).
Building community health and social change through emergency medical services
Freedom House met communities where they were and expanded the role of hospitals and healthcare beyond their institutional walls. As Freedom House Ambulance Service director of operations Mitchell Brown put it: Sixty percent of all heart attack victims die outside the hospital … It’s great to have all that expensive equipment up there (indicating the upper floors of Presbyterian Hospital) that can transplant organs, but lives are saved out there in the vacant lot and alongside the road where there is lots of dirt and no light to work by. (Moyle, n.d.)
Freedom House transformed the provision of pre-hospital emergency care in the districts that it served and across the country. Robert Zepfel, the project director, noted, “we have had officials and health representatives of other cities visit us for the purpose of learning about the program” (Long, 1971). “In the development of Freedom House Enterprise, Inc., Ambulance Service, one hospital not only affected the social fabric of its community, but did so while improving patient care” (Modern Hospital, 1969: 93).
Not only did Freedom House meet residents’ healthcare needs; it also created jobs in a whole new role, as “paramedical life support technicians”—today’s paramedics (Stuart, 1968). Arthur Davis had not finished high school and had worked in and out of various jobs until his mother, who worked for the Opportunities Industrialization Center (which recruited for Freedom House), told him about the program (Stuart, 1968). He was in the first paramedic class and said, “I’ve got an obsession about the job … I want to help people. It makes me feel good and proud that I can sometimes save a life. And for my mother, I’m somebody” (Stuart, 1968).
David Rayzer, another student in the first paramedic class, had been working as an assistant bookbinder until he left his job when he and his wife were expecting a second child (Stuart, 1968). Through Freedom House, he trained as a paramedic and became an ambulance crew chief, while seeking an associate of arts degree in sociology at community college. Rayzer saw his status transformed into a “professional status,” “having been taught how to save lives and not to panic at the scene of an accident. I know how to control bleeding, calm people, assist a seizure patient … ” (Stuart, 1968). After the Freedom House Ambulance Service closed, Rayzer went on to complete a master’s degree in public health and continued working in the field, like many of the others who trained and worked at Freedom House (Caroline, 1977).
Beyond Pittsburgh, other civil rights organizations also began ambulance services, such as the People’s Free Ambulance Service in Winston-Salem, and as these models of community-based paramedicine emerged and succeeded, they sparked larger conversations around racial justice and reinvesting in Black communities (Hilliard 2008: 27–29; Nelson, 2011: 148; Figure 1).
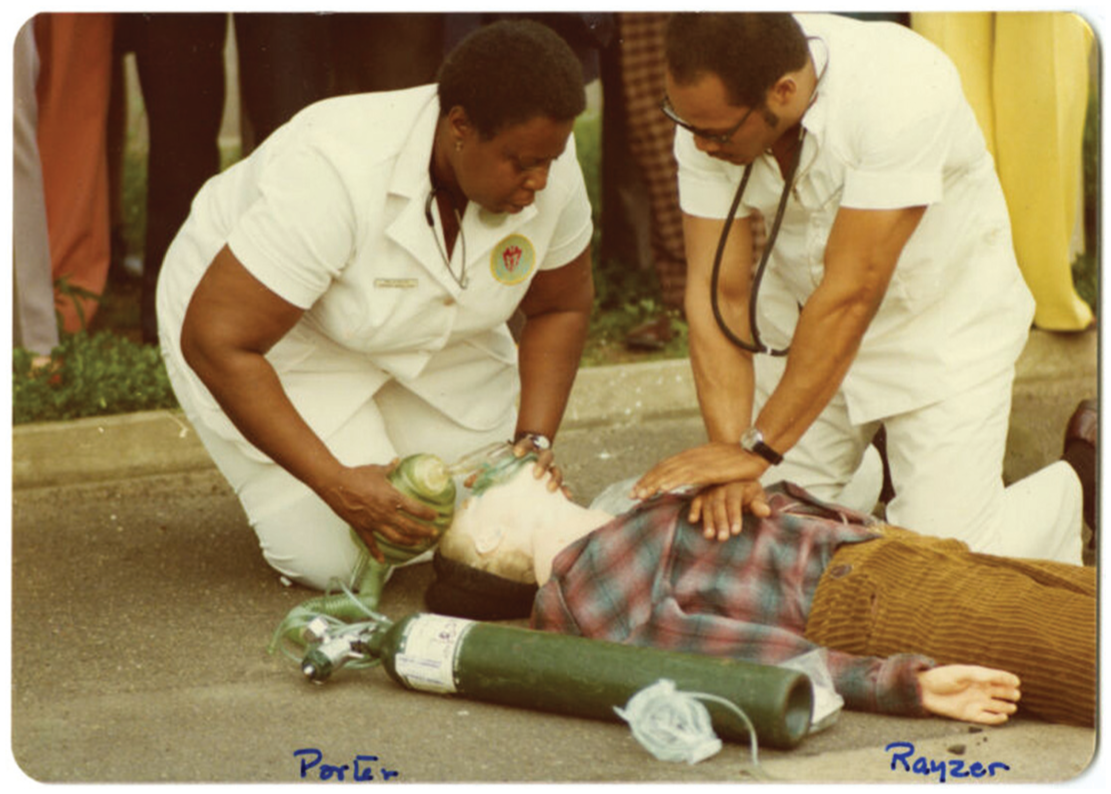
EMTs/paramedics Pearl Porter and David Rayzer during a simulated mass casualty incident.
Legacies of civil rights movements for emergency medical services
Over eight years, a total of 81 EMTs, paramedics, dispatchers, and managerial staff worked for the Freedom House ambulance service (Caroline, 1977). Many of the Freedom House employees continued to contribute to the field after the ambulance service closed, including by documenting national mobile intensive care unit guidelines and writing the model national curriculum for paramedic education (Safar, 2001). In 1973, Mitchell Brown, then technical director of Freedom House, presented the story of the ambulance service at the International Symposium on Emergency Medical Services Organization and Delivery Systems in Germany (Safar, 1975). Efforts to train paramedics similar to Freedom House began in other cities shortly after, including Dr Eugene Nagel’s creation of a paramedic program in the Miami Fire Department in 1969, Dr Leonard Cobb’s creation of a mobile coronary care unit the same year through Harborview Medical Center and the Seattle Fire Department, and Dr Walter Graf’s creation of a paramedic training program at Los Angeles’s Freeman Memorial Hospital Center in 1970. By 1971, the National Highway Traffic Safety Administration Office of Emergency Medical Services had published the first national guidelines for training EMTs, and in 1977 it published the first national guidelines for training paramedics, based on Nancy Caroline’s curriculum for Freedom House.
Creating a national emergency medical services system
Despite the advances that groups like Freedom House and the paramedic programs in Miami, Los Angeles, and Seattle were making in developing curricula and techniques for high-quality pre-hospital emergency care, most of the country still relied upon untrained morticians or police wagons into the 1970s. Senator Kennedy in 1973 emphasized that, “Nowhere is the health care crisis … more evident … than in the appalling lack of high-quality emergency medical services” (Emergency Medical Services Systems Development Act of 1973 Hearings, 1973).
Because of his experience with Freedom House, Peter Safar was invited to co-lead the National Research Council/National Academy of Sciences Committee on Emergency Medical Services and used the guidelines he drafted with Freedom House for Pittsburgh’s emergency medical services plan as the framework for new national standards and guidelines. In addition to drafting these standards and guidelines, he also played a central role in advocating to Congress for legislation supporting a more robust national system for pre-hospital care. In testimony to Congress, he highlighted disparities in treatment, emphasizing that “the best and the worst medical care can be found side by side” (Emergency Medical Services Systems Development Act of 1973 Hearings, 1973: 309).
Senator Alan Cranston of California introduced an Emergency Medical Services Systems Act in 1973, modeled in part after the structure Safar laid out to Congress based on his experiences with Freedom House. Congress approved the Act, but President Nixon vetoed it, saying that emergency medical services systems should be “a concern of State and local governments” (Nixon, 1973: iii) and opposing a provision of the bill requiring the continued operation of the remaining U.S. Public Health Service Hospitals. Withdrawing the Public Health Service Hospitals provision, Congress passed the bill again and Nixon signed it in November 1973 (P.L. 93-154).
The Act provided for new emergency medical services guidelines and funding for the planning, initial establishment, and expansion of existing systems for regional emergency medical services, and research in emergency medical techniques. The Act laid the foundation of today’s regional emergency medical service systems nationwide and it was shaped substantially by the experience of Freedom House and its early EMTs and paramedics.
Conclusion
The transformation of U.S. metropolitan areas after the Second World War through highway construction, suburbanization, and urban renewal widened already existing spatial and racial inequalities in health (Fullilove, 2001). Civil rights, Black Power, Native American, Asian American, Latinx and related struggles challenged health inequality throughout the 20th century and contributed to the rise of movements for health equity and for environmental justice (Bullard, 1990; Cole and Foster, 2001; Fernández, 2019; Molina, 2006; Nelson, 2011; Pulido, 1996; Roberts, 2009).
The transformative land use changes that urban planners and others set in motion in the mid-20th century catalyzed two seemingly separate conversations about emergency care. One focused on responses to accidental death and disability, as fatalities increased with the nation’s highway development and suburban sprawl. Another was raised by Black communities who, amidst racialized urban disinvestment and discriminatory treatment, were faced with creating their own paths toward critical prehospital care. However, these two conversations can be understood as fundamentally intertwined: the investment in highways and suburbanization was inseparable from urban disinvestment and the subsequent innovation of Freedom House. The Emergency Medical Services Systems Act of 1973 allowed for the continuation of grassroots, community-based solutions to healthcare inequality that Freedom House represented, as well as the expansion of municipal services. Incorporating the medical advancements that Peter Safar, Freedom House, and others were developing, the legislation focused on regionally controlled systems to meet federal standards.
An analysis of the history of emergency medical services reveals how intertwined these services are with urban planning and policy, as well as with economic and social inequality. The innovation of Black residents in creating community-led pre-hospital emergency care in Pittsburgh and elsewhere illuminates how the place-based nature of emergency medical services makes it a crucial vehicle for health equity and urban justice. Connecting emergency care and transportation of the sick and injured to urban planning is an understudied but essential dimension of the relationship between public health and planning. The health disparities we face today make the need for new community innovations in emergency medical services, and equitable urban planning policy to support them, as urgent now as 50 years ago.
Footnotes
Acknowledgements
In addition to the anonymous reviewers for their helpful comments, the authors thank Malhaar Agrawal and Nicholette Cameron for their outstanding research assistance; Sue Gilroy at the Schlesinger Library at Radcliffe for helping obtain access to Nancy Caroline’s papers during the Covid-19 pandemic; and Rashauna Johnson, Eve Dunbar, Will Pruitt, Darius Bost, Martha Patterson, Jesse Shipley, Andres Sevtsuk, Devin Bunten, Catherine D’Ignazio, David Hsu, Jason Jackson, Mariana Arcaya, and Alex Lam for their helpful feedback on prior drafts. The authors also thank emergency medical service providers for their continuing commitment, service, and sacrifice, day in and day out.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
