Abstract
Attempts to analyze respiratory function of the laryngectomized patient with tests such as spirometry and plethysmography have been described in the literature, highlighting however substantial difficulties. Oscillometry, through the forced oscillation technique (FOT), measures the mechanical properties of the respiratory system minimizing the problems related to the patient's lack of compliance. This methodology has never been applied to these patients and therefore represents a new perspective in the analysis of respiratory function.
Introduction
Laryngeal cancer is the second most common respiratory neoplasm after lung cancer and a total laryngectomy is required at certain stages of the disease. 1 The surgery involves the total separation of the air-digestive tracts (no longer air communication between nose-mouth-pharynx and the respiratory system), allowing the patient to breathe exclusively through the artificial stoma.
Over time, this feature results in both functional and structural changes of the tracheo-broncho-alveolar system 2 which probably exacerbate or add to respiratory diseases such as Chronic Obstructive Pulmonary Disease (COPD). 3
Attempts to analyze respiratory function with tests such as spirometry and plethysmography have been described in the literature, highlighting the substantial difficulty in performing the test by individuals and applying the aids to the stoma of the laryngectomized patient. 4 Oscillometry, also known as Forced Oscillation Technique (FOT), measures the mechanical properties of the respiratory system during quiet tidal breathing, by the application of an oscillating pressure signal minimizing the problems related to the patient's lack of compliance.
As far as we know, this methodology has never been applied to the analysis of the respiratory function of patients undergoing total laryngectomy.
Case presentation
We selected a 68-year-old patient who underwent total laryngectomy in 2017 for extensive laryngeal cancer. At the time of enrollment, the patient was in good general condition, had no relevant comorbidities and was a user of stoma covers and Heat-and-Moisture Exchanger (HME) for pulmonary rehabilitation.
An adapter produced with Polyamide 12 (PA 12) in 3D printing (dimensions: 158 mm-Length, 22 mm-Width1, 35 mm-Width2, 2 mm-Thickness) was used to connect the oscillometer filter to a Provox® XtraBase® Adhesive Base Plates (Figure 1a-b); in this way, it was possible to eliminate any loss of flow as well as in the general population through the use of the nasal clip.
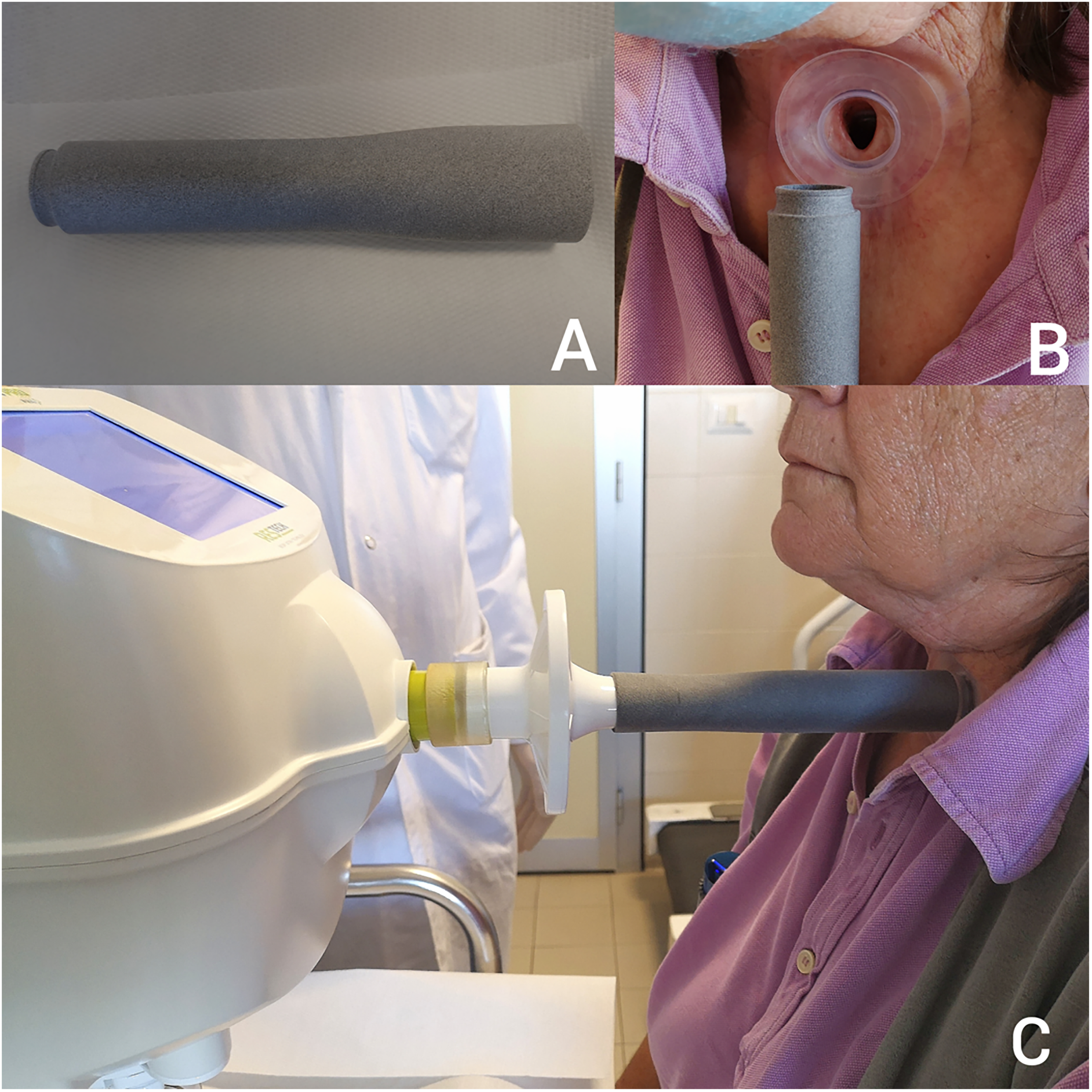
The figure shows the adapter made in 3D printing (a); a detail on the coupling mechanism to the adhesive base plates (b); the adapter-filter system connected to the oscillometer during the test (c).
After obtaining the informed consent to the procedure, the patient was subjected to serial FOT measurements with the Resmon™ Pro Full (Restech, Milano, It.) machine (Figure 1c).
The test was conducted on 5 measurements by auto-calibrating the oscillometer filter with and without the adapter generating a different impedance (Z) of the filter: of these, the software considered acceptable two measurements with an adapter and two without, excluding the fifth calibration which reported a slight impedance discrepancy (0.75 cmH2O/(L/s) vs the 0.74 of the other two measurements with an adapter.
Each test, including instrument calibration and computerized analysis, lasted between 3 and 4 min, highlighting the simplicity and quickness of the procedure even in laryngectomized patients.
The results reflected the patient's physiological respiratory function without alterations of the traces, both by auto-calibrating the filter with the adapter or without; in fact, the resistance and reactance curves assumed overlapping trends thanks to the software installed on the instrumentation that automatically considers the impedance difference to be null once connected to the patient for the execution of the exam (Figure 2a-b).

The tests showed resistance and reactance values within the normal limits, highlighting inconsistent variations of the results by calibrating the filter respectively without (a) and with (b) the 3D adapter.
To guarantee the quality of the test, in accordance with the technical standards for respiratory oscillometry, 5 a coefficient of variation (CV) of less than 10% was considered acceptable as shown in Table 1.
The table shows the coefficients of variation (cv) of the measurements after filter calibration both with and without adapter. In all measurements the CV is always less than 10%.

Discussion and conclusion
As far as we know, this is the first attempt to measure pulmonary function through FOT in laryngectomized patients. These results demonstrate the adequacy and reproducibility of this technique, consistently with our expectations. The analysis showed that the R5 and X5 values (respectively resistance and reactance of the bronchoalveolar system stimulated at a frequency of 5Hz) were within the range identified by the analysis program for age, weight, height and BMI. The instrumentation reported as acceptable all the measurements performed, probably thanks to the efficiency of the hermetic system generated with the 3D printed adapter. Through these measures, it could be possible to use and standardize this method to analyze not only the physiological conditions of the bronchoalveolar system of these patients but also the pathological changes in order to intervene promptly.
The limits of this study are related to the single patient analyzed, who does not allow a statistical analysis for the purpose of interpersonal reproducibility. Furthermore, the patient was specifically selected in good health and without bronchopulmonary problems; this has allowed us to certify the reliability of the method in objectively physiological clinical conditions.
The authors, by extending the sample of this research, hope to stimulate the scientific community to investigate the diagnostic and therapeutic implications of this innovative method.
Indeed, in consideration of the numerous reports provided by patients on the exacerbation of breathing difficulties under exertion, this test would also be ideal in the search for obstructive diseases after bronchial provocation tests and pharmacodynamic reversibility tests.
Although further research on this topic is certainly necessary, the authors are confident that the verification of these hypotheses can lead to better management the laryngectomized patients to improve their quality of life.
Footnotes
Acknowledgments
The authors are grateful to Atos Medical for the support in developing the adapter in 3D printing.
Ethics statement
All the clinico-pathologic investigations detailed in the manuscript have been conducted in accordance with the Declaration of Helsinki and its later amendments or comparable ethical standards.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
