Abstract
Perioperative arrhythmias may be induced by an imbalance between sympathetic and parasympathetic activities owing to excessive mental and physical stress. To date, no studies have been conducted on intravenous sedation (IVS) during dental procedures in a serious dental anxiety patient with atrioventricular junctional rhythm (AVJR). We describe herein the management of IVS in an outpatient with dental phobia who experienced the AVJR followed by vasovagal reflex (VVR) during dental care. A 26-year-old woman with serious dental anxiety was scheduled for dental extraction under intravenous conscious sedation. A II-lead electrocardiogram revealed AVJR following sinus rhythm. Immediately afterwards, she experienced VVR with dimmed vision, cold sweat, hypotension, and bradycardia. She was made to relax in the supine position, which restored hemodynamics to normal, and sinus rhythm followed. She was optimally sedated with midazolam 4 mg and uneventfully treated under a preparation of intravenous atropine, and hemodynamic and respiratory statuses were closely monitored to ensure spontaneous breathing without any signs of AVJR or cardiorespiratory disorders. Finally, flumazenil 0.5 mg was administered, and she recovered without re-sedation or prolonged sedation. The autonomic nervous system and endocrine system are closely related in order to control the stress responses. The present case suggests that an electrocardiographic change such as AVJR is induced by an imbalance of autonomic activity owing to excessive psychosomatic stress and is considered as a possible prodromal sign of VVR as the dental procedures are likely to be stressful for some patients.
Keywords
Introduction
Perioperative arrhythmias may be induced by an imbalance between sympathetic and parasympathetic activity due to excessive mental and physical stress or general anesthesia.1,2 Herein, we discuss the management of intravenous sedation (IVS) for an outpatient with serious dental anxiety who experienced the atrioventricular junctional rhythm (AVJR) followed by vasovagal reflex (VVR) during dental procedures. The present study patient represents a rare or unusual case of AVJR incidence prior to the start of IVS.
Case presentation
A 26-year-old woman with dental phobia was scheduled to undergo extraction of bilateral maxillary and mandibular first premolars under intravenous conscious sedation. Preoperative electrocardiogram (ECG) indicated normal sinus rhythm (Figure 1). An intravenous line was secured as painlessly as possible under non-invasive monitoring of II-lead ECG, blood pressure (120/72 mmHg), heart rate (91 beats per minute; bpm), and oxygen saturation (SpO2, 99%). The ECG revealed AVJR without visible P waves following sinus rhythm. Immediately afterwards, she experienced VVR with cold sweat, dimmed vision, hypotension (59/27 mmHg), and bradycardia (50 bpm). She had no loss of consciousness or respiratory depression with normal SpO2 (97%). She was made to relax in the supine position under a preparation of intravenous atropine along with oxygenation which restored sinus rhythm, normal hemodynamics (blood pressure: 104/55 mmHg, heart rate: 76 bpm), and good general condition. The ECG record during VVR following AVJR could not be promptly obtained under the situation of emergency care and was obtained only after recovering to sinus rhythm as a result (Figure 2).

Preoperative 12-lead ECG indicating normal sinus rhythm.
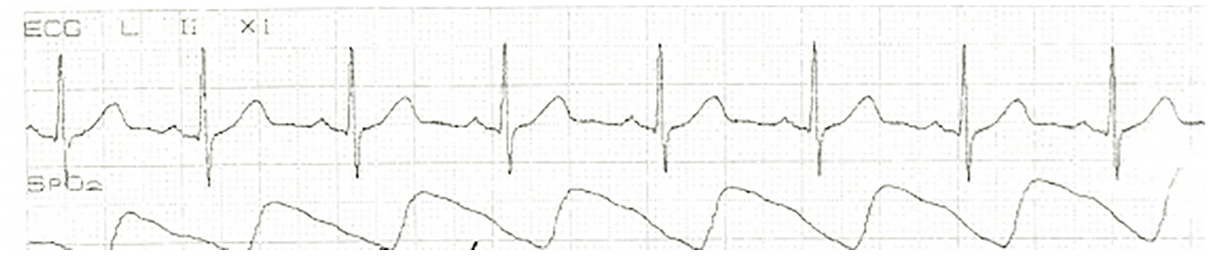
II-lead ECG after recovering to sinus rhythm.
For induction and maintenance of sedation, midazolam (total dose: 4 mg) was administered under the guidance of the first author, a certified dental anesthesiology specialist. The patient was optimally sedated (Ramsay sedation score: 3) 3 and uneventfully treated under local anesthesia with administration of 2% lidocaine containing adrenaline without any signs of AVJR, cardiovascular disorders, and respiratory depression. Her blood pressure (92–100/46–50 mmHg), heart rate (71–86 bpm), and SpO2 (99%–100%) were stable without any other electrocardiographic changes throughout the procedure. Clinical recovery from sedation after administration of flumazenil 0.5 mg was satisfactory with regard to postoperative physiological homeostasis and locomotor functions, without any re-sedation or prolonged sedation (Figure 3).

Perioperative management record. The patient experienced an occurrence of AVJR followed by transient vasovagal reflex prior to the start of intravenous sedation. Supine position and oxygenation under a preparation of intravenous atropine restored sinus rhythm, normal hemodynamics, and good general condition. She was optimally sedated and uneventfully treated without any signs of AVJR, cardiovascular disorders, and respiratory depression.
Discussion
Dental patients are likely to experience excessive anxiety, fear, and tension before the treatment. Patients with previous aversive painful experiences or preconception about pain during dental surgery are particularly susceptible to such psychological stress.4,5 Such dental phobia, recognized by the World Health Organization, is a common but noteworthy problem in the dental clinics. 6 Once the patients consult a dental doctor, they can be exposed to a stressful ambulatory environment of dento-oral surgery. Therefore, psychological or hemodynamic disorders such as VVR, hyperventilation syndrome, hypertension, or arrhythmia due to stress-induced sympathetic hyperactivity or sympathetic/parasympathetic imbalance are of special concern in dental care. In this regard, IVS can be a safe and beneficial strategy to provide the patients with stabilization of emotion and hemodynamics and to prevent VVR in patients with dental phobia. On the other hand, dental anxiety test before treatment may be reliable and useful to recognize three classes (mild; moderate; severe) of dental phobia. 6 In addition, it is pointed out that while the friendly approach to patients, the use of audiovisual devices for relaxation, and so forth are evaluated as the different methods to overcome dental phobia, IVS with administration of benzodiazepines is also considered as the only solution to obtain the effective treatment for the patient.6,7 With respect to IVS, among the benzodiazepines, midazolam is commonly and appropriately administered in dental surgical procedures and is safe, convenient, and has a relatively short recovery profile, 8 as applied satisfactorily in the present patient. Moreover, flumazenil can promptly antagonize the effects of benzodiazepines for a controlled reversal of residual sedation; however, it has a shorter elimination half-life of active metabolite than other benzodiazepines. 9 From this perspective, the re-sedation needs to be carefully observed throughout the postoperative period.
It is essential to carry out the careful systemic management under perioperative ECG monitoring particularly in the present patient with serious dental anxiety. Because, we should keep in mind and understand the possible ECG findings to indicate some signs of psychosomatic stress-induced VVR. In the light of the perioperative electrocardiographic changes, AVJR occurs in association with high vagotonia caused by psychological stress. 10 Consequently, it is necessary to focus on the diverse stressors as patients may develop stress even from the time of intravenous line cannulation, prior to the start of IVS. In AVJR, regarding isorhythmic atrioventricular dissociation, the P waves and QRS complexes are generated by different pacemakers, and atrial excitation occurs more slowly than ventricular one. The P–P intervals become equal to the R–R intervals when the atria and ventricles can beat at the same rate due to intrinsic rhythmicity. 11 The P waves that do not lead to ventricular conduction remain within the QRS complexes, during the refractory periods immediately before the QRS complexes, on the ST segments or on the T waves. With respect to the atrioventricular nodal rhythm, in which the atrioventricular junction acts as a pacemaker with its own intrinsic rhythm, the P waves disappear or appear following the QRS complexes due to retrograde conduction. 11 The transient disappearance of the P waves in the present patient is considered to be the electrocardiographic change that indicates the latency of the P waves disappearing within the QRS complexes.
The sinus node and atrioventricular node are mainly controlled by the right vagus nerve and by the left vagus nerve, respectively. Accordingly, the imbalance between sympathetic and parasympathetic activity may be a factor bringing about AVJR. A vagotonia stimulates the vasomotor center in the brainstem through the vagal afferent branch, resulting in the cardiovascular disorders such as bradycardia and severe hypotension due to vasodilation leading to a loss of consciousness.12,13 The symptoms associated with VVR include dimmed vision (prodrome), nausea, cold sweat, facial pallor, etc. The preoperative examination in the present patient showed no abnormalities in the ECG and electrolytes, and there was no medical history of cardiovascular diseases likely to cause AVJR. As the present patient complained of dimmed vision immediately after the AVJR, and the associated symptoms of VVR improved along with the return to sinus rhythm, we infer that a parasympathetic dominance due to imbalance of autonomic activity induced the AVJR as a prodromal sign of VVR with excessive dental anxiety. Therefore, we surmise that AVJR did not occur during the IVS as the autonomic balance was well maintained by the optimal sedation effect.
The AVJR can manifest as an electrocardiographic change based on the background of the balance between surgical invasion and anesthetic depth during general anesthesia.11,14 From this viewpoint, we consider that the imbalance of autonomic activity is closely related to the above-mentioned clinical background under the influence of the neuroendocrine system on homeostasis during surgery. Clinically, it is essential to differentially diagnose the underlying diseases that may cause AVJR or other cardiac conduction disorders. Furthermore, if the AVJR, such as an isorhythmic atrioventricular dissociation or atrioventricular nodal rhythm, persists during general anesthesia or IVS, a reduction in the left ventricular end-diastolic volume, due to lack of atrial kick, results in decreased cardiac output followed by hypotension. The absence of atrial contraction has been found to be associated with a 15% decrease in cardiac output. 15 The AVJR accompanied by bradycardia and hypotension due to vagotonia requires administration of atropine and vasopressors such as etilefrine or ephedrine, or transcutaneous external pacing as needed, especially during general anesthesia or IVS.16,17 Therefore, the clinical diagnosis of the possible causes of AVJR is important for an appropriate treatment.
Conclusion
The present case suggests that the AVJR induced by the imbalance of autonomic activity is a possible prodromal sign of VVR. We should reacknowledge and closely monitor perioperative electrocardiographic changes due to systemic disorders such as VVR in patients with dental phobia exposed to excessive psychosomatic stress. For stress-free management in dental procedures, it might be also worthwhile to take advantage of the patient-first perioperative care such as an assessment of dental anxiety score, a considerate approach to patients, and some devices that lead to relaxation, in case of judging IVS practice.
Footnotes
Authors’ contributions
Hajime Shimoda drafted the manuscript and Tetsu Takahashi revised the manuscript. Both authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
