Abstract
Objectives:
Fentanyl overdose deaths are a critical public health issue in the United States. Rhode Island, an early epicenter of the fentanyl crisis, has seen fentanyl overdose deaths increase 30-fold since 2009. In response, harm reduction tools such as fentanyl test strips (FTSs) have been introduced to help people who use drugs (PWUD) detect fentanyl in their substances. We analyzed FTS use among PWUD in Rhode Island from 2021 through 2023 and identified characteristics associated with their use.
Methods:
We conducted a pooled cross-sectional analysis using aggregate data from the Rhode Island Harm Reduction Surveillance System. We used bivariate Pearson χ2 tests to assess the relationship between past-month FTS use and demographic and behavioral characteristics. Because analyses were limited to unadjusted comparisons, these findings are exploratory and hypothesis generating.
Results:
Of 498 survey respondents, most identified as male (n = 328; 65.9%), non-Hispanic White (n = 204; 41.0%), straight (n = 400; 80.3%), and aged 25 to 44 years (n = 288; 57.8%). The most frequently reported substances used were crack (n = 355; 71.3%), cocaine (n = 219; 44.0%), and fentanyl/heroin (n = 196; 39.4%). Only 31.7% of individuals reported FTS use in the past 30 days. FTS use was significantly associated with age, race and ethnicity, witnessing an overdose, possessing naloxone, and recent fentanyl/heroin use (all
Conclusions:
Despite FTS distribution efforts and overdose risk, FTS uptake in Rhode Island was low. Future research should assess barriers to FTS adoption and consider integrating FTS distribution within naloxone programs.
Illicitly manufactured fentanyl has greatly accelerated the trajectory of opioid overdose deaths in the United States. As a potent synthetic opioid typically used for pain relief following surgical procedures, fentanyl is structurally similar to morphine, but it is estimated to be approximately 50 to 100 times more potent. 1 Because of its high potency, only a small amount (as little as 2 mg) can lead to overdose and death. 2 Illicitly manufactured fentanyl may be mixed with other drugs (eg, heroin, cocaine) either intentionally or unintentionally during production, distribution, and use.3,4 People who use drugs (PWUD) may be unaware of the presence of fentanyl in their drugs, substantially increasing the risk of unintentional overdose and fueling a public health crisis nationwide. 5
In response to this public health crisis, harm reduction interventions have been implemented to promote awareness of the drug supply, safety behaviors, and linkage to care among PWUD. For example, fentanyl test strips (FTSs; ie, lateral-flow chromatographic immunoassay test strips) allow users to easily test for the presence of fentanyl and a small number of fentanyl analogs in their drugs. 6 FTS use is associated with an increase in taking safety precautions, such as using smaller amounts, trying a test dose first, not using alone, and having someone present with naloxone.7-11 FTSs are also affordable (~$1 each), can be used privately, and have demonstrated high sensitivity and specificity.6,12,13 However, FTSs have certain limitations; they can detect only the presence of fentanyl, not its quantity or potency; they cannot differentiate between fentanyl and stronger fentanyl analogs if detected (eg, carfentanil); and they may give false-negative test results because of cross-reactivity or the uneven distribution of fentanyl within a sample.14-17 In addition to these technical limitations, both social and structural barriers influence FTS uptake. Drug-related stigma, concerns about potential negative consequences from law enforcement, mistrust of health care or harm-reduction services, or prior experiences of discrimination may discourage some people from using drug-checking equipment. 7 At the structural level, laws regulating the possession and distribution of drug-checking equipment, including FTSs, as well as the funding and authorization of harm-reduction services, vary widely across the United States, restricting access to FTS and creating structural barriers to optimal FTS access.
In Rhode Island, the early epicenter of the US fentanyl crisis, the number of fentanyl overdose deaths increased substantially, from 7 in 2009 to 226 in 2018. 18 In response, FTSs were legalized in Rhode Island in 2018, and more than 50 000 FTSs have since been distributed.19,20 In 2019, the state achieved a 5% decrease in fentanyl overdose deaths; however, the COVID-19 pandemic escalated overdose risk during 2020-2021. 18 The number of overdose deaths nationally and in Rhode Island stabilized in 2022 and 2023 and declined in 2024, reflecting ongoing harm-reduction efforts, such as expanded distribution of naloxone and FTSs as well as treatment and recovery programs and drug supply dynamics. 18 As overdose mortality begins to plateau, understanding whether and how PWUD are engaging with available harm-reduction tools such as FTSs becomes increasingly important to sustain progress. Substantial gaps exist regarding the extent of FTS uptake and the characteristics of PWUD using them. Our study builds on prior analyses from 2021-2022,21,22 which indicated that 32.5% of PWUD who participated in the survey reported overdosing in the past 12 months and 67.4% reported witnessing an overdose. We analyzed statewide use of FTS among PWUD in Rhode Island during 3 years (2021-2023) and identified key characteristics associated with use to inform future harm-reduction strategies.
Methods
Data Source and Collection
The Rhode Island Harm Reduction Surveillance System (HRSS) was launched in 2020 through a partnership between the Rhode Island Department of Health (RIDOH) and The Miriam Hospital to survey PWUD in Rhode Island. 21 HRSS collects information on demographic characteristics, substance use, health care access, overdose experiences, and harm-reduction behaviors. Our analysis used data from January 1, 2021, through December 31, 2023.
Eligible participants were Rhode Island residents aged ≥18 years who provided verbal consent and had self-repor-ted illicit drug use (other than marijuana) in the previous 30 days. The study team primarily recruited participants through targeted canvassing at syringe distribution programs, harm-reduction outreach programs, and street outreach in overdose hotspots. Participants completed anonymous surveys in person or by telephone, and the study team compensated participants with $25 in cash. Although the survey was anonymous, we generated a unique 8-digit code (based on initials and birth date) for each participant and cross-checked to minimize duplicate participation. Because the HRSS did not systematically record the number of individuals approached or who declined participation, we could not calculate a survey response rate. The study team collected and stored all HRSS survey data through the Research Electronic Data Capture (REDCap) tool. This work, based on deidentified aggregate data, is considered public health surveillance and was reviewed and exempted by the RIDOH Institutional Review Board (IRB) and approved by the Miriam Hospital IRB (committee no. 218820). The Ethics Committee of the RIDOH IRB waived the need for ethics approval and patient consent for the collection, analysis, and publication of the retrospectively obtained and deidentified data for this noninterventional study. Survey items were developed in collaboration with community partners.
Data Analysis
This pooled cross-sectional quantitative analysis used deidentified, aggregate (cross-tabulated) data from the HRSS provided by RIDOH. We assessed recent FTS use using a single survey question: “In the past 30 days, how often did you test a new ‘batch’ of drugs for fentanyl with a fentanyl test strip?” We operationalized responses as a binary variable: respondents who answered “always,” “most of the time,” or “some of the time” were categorized as FTS users, and respondents who answered “never” were categorized as nonusers. We excluded responses such as “other,” “prefer not to answer,” or any missing values.
We generated descriptive statistics to summarize demographic and behavioral characteristics, including age, sex assigned at birth, education level, race and ethnicity, sexual orientation, housing status, health insurance, nonprescribed substances used, and witnessing an overdose or possessing naloxone in the past 12 months. For nonprescribed substances used, polysubstance use was defined as self-reported use of ≥2 substances in the past 30 days. Certain categories with low counts were combined to adhere to RIDOH’s Small Numbers Reporting Policy; these included age (grouped into 5 categories) and education level (grouped into 3 categories). The dataset consisted of frequency tables rather than individual records; therefore, analyses were restricted to bivariate analyses using the Pearson χ2 test, and multivariable modeling could not be performed. We set significance at
Results
The HRSS collected survey responses from 498 unique individuals from 2021 through 2023 (Table 1). Most participants identified as male (n = 328; 65.9%), non-Hispanic White (n = 204; 41.0%), and straight (n = 400; 80.3%) and were aged 25 to 44 years (n = 288; 57.8%), with a relatively stable age distribution across survey years. Education levels varied: 30.5% (n = 152) had not completed high school, 40.2% (n = 200) had a high school diploma or General Educational Development, and 28.5% (n = 142) had completed some college or graduated from college. Nearly three-quarters of participants (n = 366; 73.5%) reported experiencing some form of housing instability, and only 5.8% (n = 29) lacked health insurance. Polysubstance use was common (89.4%); participants reported using crack (n = 355; 71.3%), cocaine (n = 219; 44.0%), fentanyl/heroin (n = 196; 39.4%), methamphetamine (n = 131; 26.3%), and opioid pain medications (n = 83; 16.7%). Approximately two-thirds (67.1%; n = 334) had witnessed an overdose in the past 12 months, and more than three-quarters (n = 386; 77.5%) reported having naloxone in the past 12 months. Across all 3 study years, only 158 (31.7%) participants reported using an FTS in the past 30 days. Reported FTS use increased from 25.2% in 2021 to 38.5% in 2022 and then declined to 31.5% in 2023.
Characteristics of participants in the Rhode Island Harm Reduction Surveillance System (N = 498), 2021-2023a,b
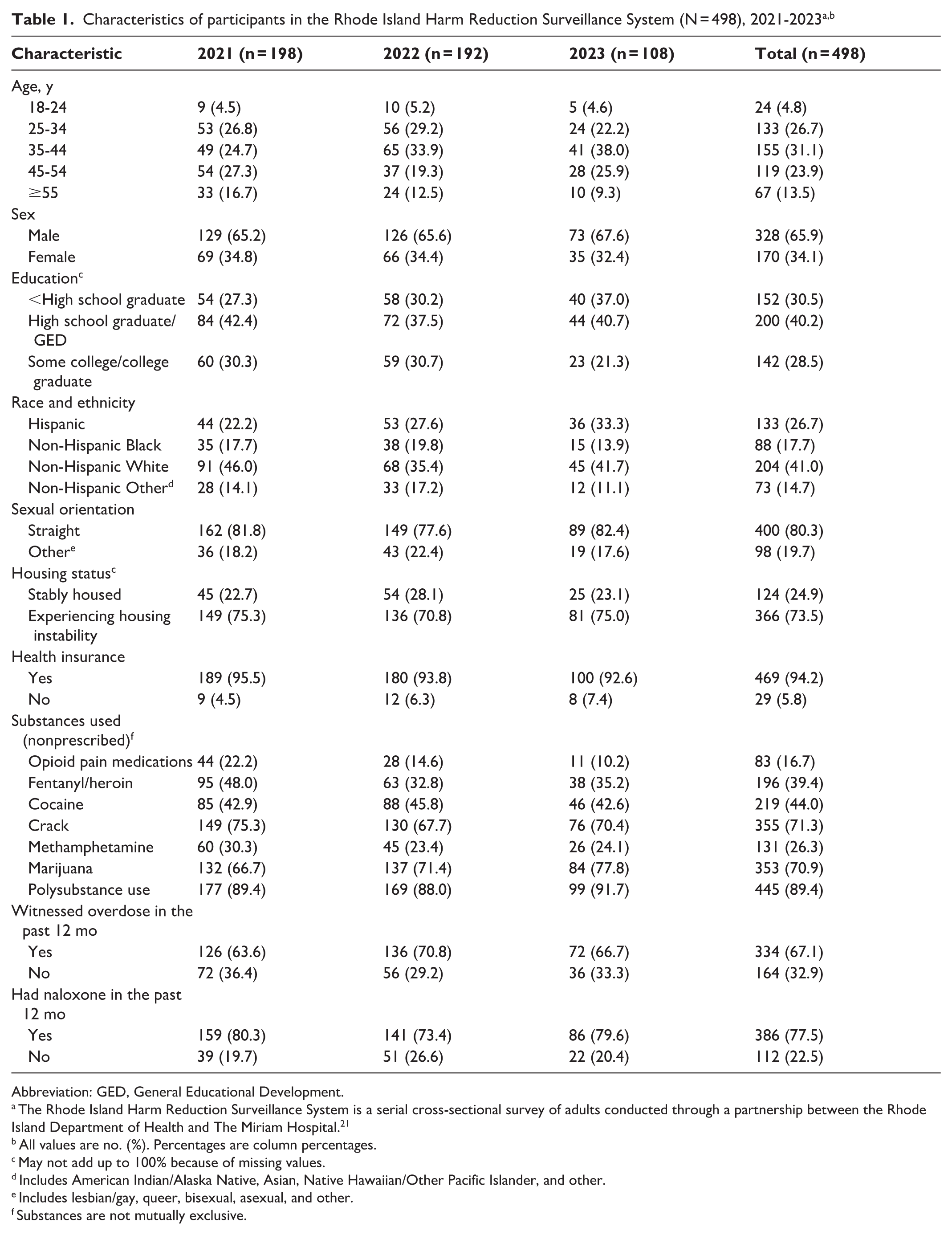
Abbreviation: GED, General Educational Development.
The Rhode Island Harm Reduction Surveillance System is a serial cross-sectional survey of adults conducted through a partnership between the Rhode Island Department of Health and The Miriam Hospital. 21
All values are no. (%). Percentages are column percentages.
May not add up to 100% because of missing values.
Includes American Indian/Alaska Native, Asian, Native Hawaiian/Other Pacific Islander, and other.
Includes lesbian/gay, queer, bisexual, asexual, and other.
Substances are not mutually exclusive.
Bivariate analyses revealed several significant associations with FTS use in the past 30 days (Table 2). Age was significantly associated with FTS use (
Demographic and behavioral characteristics of participants in the Rhode Island Harm Reduction Surveillance System (N = 498), by use of fentanyl test strips (FTSs), 2021-2023a,b
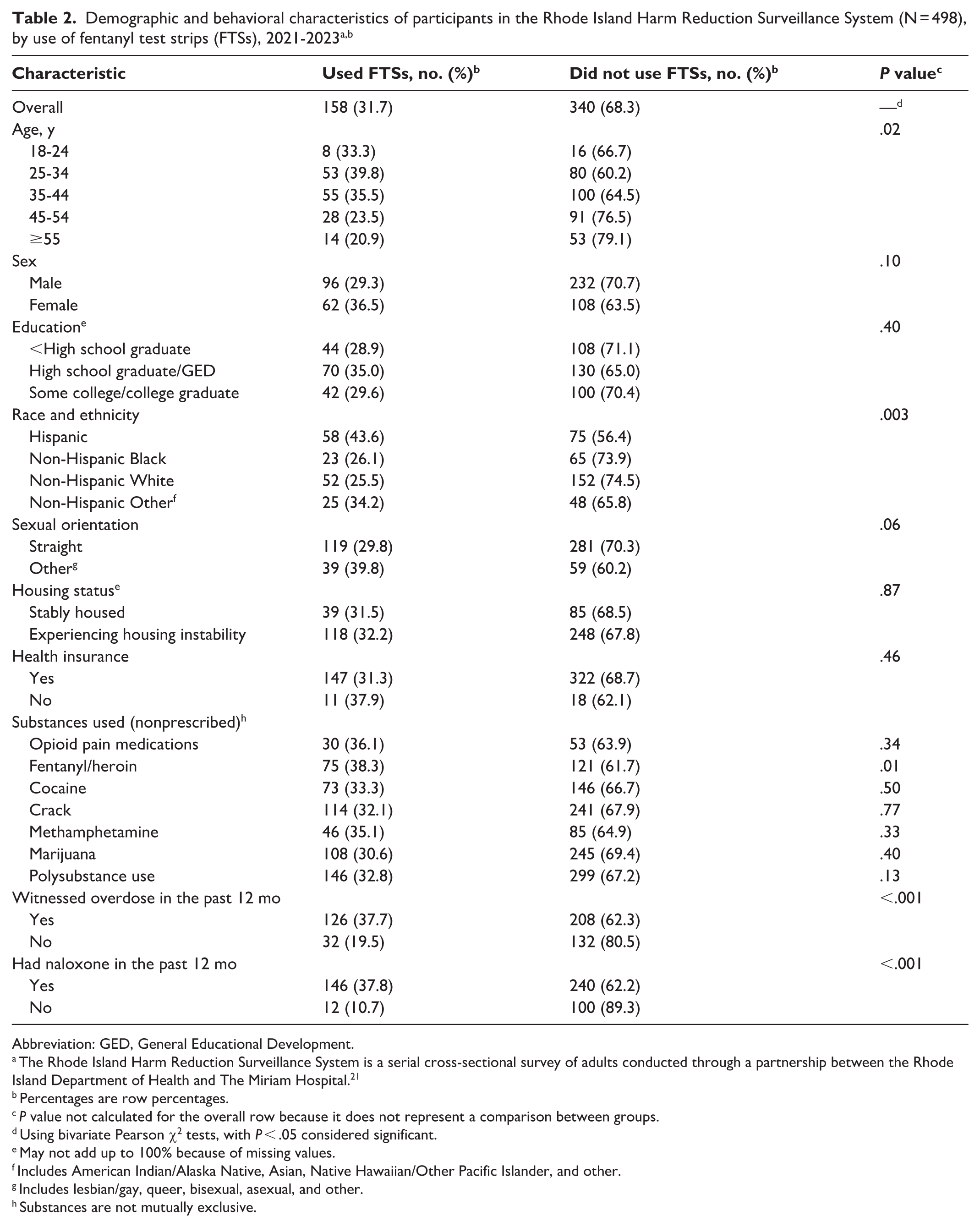
Abbreviation: GED, General Educational Development.
The Rhode Island Harm Reduction Surveillance System is a serial cross-sectional survey of adults conducted through a partnership between the Rhode Island Department of Health and The Miriam Hospital. 21
Percentages are row percentages.
Using bivariate Pearson χ2 tests, with
May not add up to 100% because of missing values.
Includes American Indian/Alaska Native, Asian, Native Hawaiian/Other Pacific Islander, and other.
Includes lesbian/gay, queer, bisexual, asexual, and other.
Substances are not mutually exclusive.
Witnessing an accidental overdose in the past 12 months was significantly associated with FTS use (
Discussion
This pooled analysis examined FTS use in Rhode Island among PWUD from 2021 through 2023. Despite at least 3 years of legalization and distribution efforts across the state, fewer than one-third of surveyed participants (31.7%) reported FTS use in the past 12 months, indicating an opportunity for improvement. These findings are consistent with a previous study 23 that reported 26.1% past-month and 50.3% lifetime FTS use among a separate sample in Rhode Island from 2020 through 2023. Building on that previous analysis, this study used statewide surveillance data, providing newer, population-level insight into FTS uptake among diverse harm-reduction and outreach settings in Rhode Island. Only a few studies have examined FTS uptake outside Rhode Island, with varying results. One study in San Francisco found that 45.4% of a sample of people who inject drugs had used FTSs in the past year. 24 In contrast, another study conducted in Kentucky, New York, and Ohio found that 56.6% of surveyed PWUD reported using FTSs in the past 30 days. 25 While these studies have many methodological differences, they suggest that FTS uptake is suboptimal and could be improved by addressing gaps in existing outreach efforts, potential barriers to access or use (eg, distance to harm-reduction services, difficulties interpreting results), or other factors (eg, stigma, legal barriers) that shape the lack of widespread adoption.
We found significant differences in recent FTS use across demographic groups. Age was significantly associated with FTS use, with the highest rates of use among people aged 25 to 44 years and the lowest rates of use among people aged ≥45 years. This finding aligns with previous research, which found that FTS users were significantly younger on average (aged 40 y) than nonusers. 23 The consistent concentration of FTS use among people in their late 30s and early 40s across both studies may suggest that this group has a greater awareness of FTSs, willingness to use FTSs, or more experience engaging with harm-reduction services than younger or older PWUD do.
Racial and ethnic disparities were also evident. Hispanic PWUD had the highest rate of FTS use (43.6%), followed by PWUD of non-Hispanic Other race and ethnicity (34.2%), non-Hispanic Black PWUD (26.1%), and non-Hispanic White PWUD (25.5%). This result was somewhat unexpected and differed from much of the existing literature, which has found that non-Hispanic White PWUD are more likely to use FTSs than Hispanic and non-Hispanic Black PWUD.11,24,25 Our findings may reflect recent outreach efforts in Rhode Island that have successfully engaged Hispanic communities in harm-reduction services.
People who had witnessed an overdose or possessed naloxone in the past 12 months were significantly more likely to report recent FTS use than people who had not witnessed an overdose or possessed naloxone in the past 12 months. Similar findings were observed in a previous study, suggesting that individuals embedded in networks at higher risk of fentanyl exposure, overdose, or drug-related harms and associated services may be more aware of fentanyl-related risks or more motivated to engage in harm-reduction services than individuals not embedded in these networks. 23 Past literature also links FTS use to engagement in multiple harm-reduction services, including naloxone use.26,27 Given this finding, existing naloxone distribution sites could serve as locations for FTS expansion and drug supply education. FTS use was also significantly higher among people who reported recent fentanyl/heroin use than among people who did not report recent fentanyl/heroin use, which may reflect harm-reduction engagement but could also indicate FTS use primarily for confirming drug contents rather than avoiding exposure.
Limitations
This study had several limitations. First, self-reported data may be subject to recall or social desirability bias, primarily because the survey was administered by interview. Second, the study population represents a convenience sample that was heavily recruited from urban settings at elevated risk of overdose and fentanyl exposure and may not fully represent all PWUD in Rhode Island. Because recruitment primarily occurred in these settings, the sample could overrepresent PWUD with greater engagement in harm-reduction services and overdose prevention activities. Third, data from 2021 through 2023 do not capture more recent trends. Fourth, using aggregate data poses many analytical limitations and prevents the ability to conduct multivariable analyses. As a result, all reported associations are unadjusted and may be influenced by confounding among correlated demographic and behavioral factors. Some subgroups had small sample sizes and should be interpreted with caution. These findings should be interpreted as descriptive rather than causal and useful for generating hypotheses for future research on FTS use among PWUD. Fifth, a temporal mismatch occurred between the outcome (FTS use in the past 30 days) and several correlates (witnessing an overdose or possessing naloxone in the past 12 months). This asymmetry limited causal interpretation and may have introduced reverse causation. Sixth, operationalizing FTS use as a binary variable may have obscured important nuances, such as discrepancies between people who always use FTSs and people who use FTSs occasionally. Seventh, racial differences should be interpreted cautiously because the non-Hispanic Other category aggregated multiple small racial and ethnic groups, and race and ethnicity represent socially assigned exposures to structural inequities rather than biological differences. Finally, because the aggregated dataset combined some response categories to adhere to small numbers policies, ordinal analyses could not be performed. Despite these limitations, this study provides valuable insights into patterns of FTS use and related behaviors among PWUD in Rhode Island.
Conclusions
FTS use in the past 30 days was significantly associated with age, race and ethnicity, overdose exposure, naloxone possession, and recent fentanyl/heroin use. High rates of FTS use were reported among people aged 25 to 44 years, Hispanic people, those who had witnessed an overdose or possessed naloxone in the past year, and those who used fentanyl/heroin recently. Additional research using robust measures and multivariable methods is needed to confirm these patterns and evaluate the effectiveness of FTS implementation strategies.
Despite these patterns, the overall uptake of FTSs in Rhode Island is low compared with uptake in other states. Expanding access to FTSs and increasing education and awareness about FTS use are critical. Public health agencies could consider leveraging naloxone distribution sites as locations for FTS distribution and outreach and actively engaging populations with low rates of FTS use. Further research should explore barriers to FTS adoption, such as cost, convenience, testing technique, and perceived utility, as well as effective and sustainable models for expanding access to drug-checking services, inclusive of FTS and other emerging drugs of public health concern.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Rhode Island Department of Health. J.N.P. was supported by the COBRE on Opioids and Overdose (P20GM125507). Its contents are solely the responsibility of the authors and do not necessarily represent the official views of our funders.
