Abstract
Objectives:
Frontline essential workers face elevated risks of exposure to COVID-19 because of the interactive nature of their jobs, which require high levels of interaction with the general public and coworkers. The impact of these elevated risks on the mental health of essential workers, especially outside the health care sector, is not well studied. To address this knowledge gap, we examined correlations between perceptions of workplace risks and mental health distress among grocery store workers in Arizona.
Methods:
We collected the first statewide sample of essential workers outside the health care sector focused on mental health and well-being. A total of 3344 grocery store workers in Arizona completed an online survey in July 2020. We used multiple regression models to identify demographic and work-based correlates of mental health distress.
Results:
Levels of mental health distress among respondents were high: 557 of 3169 (17.6%) reported severe levels and 482 of 3168 (15.2%) reported moderate levels. Perceptions of workplace safety were strongly correlated with significantly reduced levels of mental health distress (ß = −1.44; SE = 0.20) and reduced perceived stress (ß = −0.97; SE = 0.16). Financially disadvantaged workers and employees aged <55 reported high levels of mental health distress. Perceptions of safety and protection in the workplace were significantly correlated with availability of safety trainings, social distancing, and policies governing customer behaviors.
Conclusions
Lacking sufficient workplace protections, grocery store employees in Arizona experienced high levels of mental health distress during the COVID-19 pandemic. Providing clear federal and state policies to employers to guide implementation of workplace protections may help reduce sources of mental health distress.
Keywords
Frontline essential workers face elevated risks of exposure to COVID-19 because of the interactive nature of their jobs, which require high levels of interaction with the general public and coworkers. 1 A healthy workforce in essential services such as health care, first responders, and retail and other services is vital to combating the COVID-19 pandemic. These frontline workers provide necessary access to consumer goods and services and represent a potential source of transmission in their communities. 2 However, the extant literature on COVID-19 exposure risks and health effects among frontline workers is predominately focused on health care workers and neglects hazards specific to other occupations in the retail and service sectors.
Retail workers are less likely than health care workers to have had previous experiences with basic infection control procedures or access to personal protective equipment (PPE). 3 They are also more likely than people in other employment sectors to be economically vulnerable, low-wage employees with low levels of education and occupational mobility. For many non–health care industries that are deemed essential, the implementation of workplace protections during the COVID-19 pandemic led to substantial transformations of both physical spaces and normative practices. Some workplaces, such as grocery stores, have also become sites of political and cultural contestation and conflict concerning public health practices, such as face mask wearing and social distancing. Recent studies suggest that grocery stores are among several transmission clusters in China4,5 and in the United States. 2 The psychological stressors associated with the transformation of retail spaces such as grocery stores are likely to be consequential for the mental health of this workforce. 6
Emerging literature on the mental health consequences of the COVID-19 pandemic suggests an increasing prevalence of mental health illness. In China, studies found that at least one-third of their study populations had moderate-to-severe mental health distress.7,8 Although studies in the United States have found comparatively lower rates of mental health distress,9,10 the literature suggests that mental health distress is likely to increase substantially as the pandemic continues. 11 Reported rates of depression and anxiety are already significantly higher among frontline health care workers than among the general US population.12,13
The mental health effects of the pandemic are potentially related to unfamiliar and challenging workplace responsibilities and the sense of uncontrollability in the absence of effective workplace protections.14 -16 Perceptions of occupational risks are correlated with effective workplace safety practices.17 -19 Workers with negative perceptions of their employers’ commitment to safety have been found to engage in more unsafe acts and to be less motivated to follow safety protocols than their peers who have more positive impressions of their employers.20,21
The increased risk of COVID-19 exposures among frontline essential workers and the associated mental health stressors are understudied, especially outside the health care sector. With millions of grocery store workers performing essential labor involving frequent interactions with customers, data are needed to track the effect of the pandemic on the well-being of this socioeconomically vulnerable workforce. 22 To address this gap in data, we examined predictors of mental health distress related to frontline essential work using a cross-sectional survey of grocery store employees during the first wave of the COVID-19 pandemic in Arizona.
Methods
Data for this project come from the Arizona Frontline Worker Survey (AFWS), a cross-sectional online survey of workers aged ≥18 in the service sector. We developed and distributed the survey in partnership with the United Food and Commercial Workers (UFCW) Local 99, representing about 24 000 workers in Arizona. All active members of the UFCW Local 99 with an email address or cellular telephone number were eligible for participation.
Survey recruitment occurred during July 2020, corresponding with the height of the COVID-19 pandemic’s initial wave in Arizona. 23 The UFCW emailed invitations in both English and Spanish to approximately 18 000 frontline workers. Of the 5400 potential participants who viewed the survey (30% contact rate) via the Qualtrics online survey platform, 3663 participants completed the survey fully and 343 participants completed the survey partially, for a 22.3% response rate. We restricted our analysis to respondents who reported working at a grocery store and for whom we had complete data for the variables of interest (n = 3344, 91.3% of total respondents). Of 3344 respondents, 3026 (90.5%) reported having regular encounters with customers. The University of Arizona Institutional Review Board approved all study protocols.
Measures
Mental Health Distress
Our primary outcome of interest for this study was mental health distress. To assess respondents’ overall mental health status, we included 2 validated measures of mental health currently used in COVID-19–related studies. The first, the 4-item version of the Patient Health Questionnaire (PHQ-4), is an ultra-short measure of anxiety and depression validated in the general US population. 24 It assesses feelings of anxiety and depression on a 4-point scale, totaling each item to produce a generalizable assessment of mental health distress ranging from normal (0-2) to mild (3-5), moderate (6-8), and severe (9-12). 25
The second measure included was the 4-item Perceived Stress Scale (PSS-4), an ultra-short assessment of perceived stress. 26 The PSS-4 measures the degree to which life situations are appraised as stressful experiences as a result of being unpredictable, uncontrollable, and overwhelming. 27 This measure assesses the frequency of these experiences within the previous month on a 5-point Likert scale ranging from never (0) to very often (4). Compared with longer perceived stress scales, the PSS-4 has sufficient internal reliability across multiple study populations.28,29
Workplace Safety Measures
To better understand changing conditions in the grocery retail workplace, we asked respondents to identify workplace modifications undertaken, including engineering controls (eg, sneeze guards or store layouts), administrative controls (eg, rules and policies governing worker and customer behavior), and PPE. We created a list of 15 potential COVID-19–related workplace practices based on our review of the emerging occupational health guidance available at the state and federal levels. A statewide mandate to wear face masks had not been instituted for Arizona at the time of the study.
Workplace safety measured the perceived possibility of exposure to COVID-19 at the workplace. We assessed participants’ sense of safety based on the question, “How safe do you feel at work during the COVID-19 pandemic?” Responses included “very safe,” “safe,” “not safe,” and “very unsafe.” For analytic purposes, we created a binomial indicator score of 0 for responses of “not safe” and “very unsafe” and 1 for “very safe” and “safe.” Of 3169 respondents to this question, 1972 (62.2%) responded “safe or very safe” (SD = 0.49; skewness = −0.51; kurtosis = −1.75).
Workplace protection measured respondents’ perceptions that their employer prioritizes employee health and safety through workplace practices and policies. We assessed participants’ sense of protection based on agreement with the statement, “My employer is doing enough to keep me safe from COVID-19,” calibrated on a 5-point Likert scale ranging from 1 (strongly agree) to 5 (strongly disagree). We similarly created a binomial measure score of 0 for responses in disagreement and 1 for responses in agreement; 52.5% (1664 of 3168) of respondents agreed that their employer was doing enough to protect them (SD = 0.50; skewness = −0.10; kurtosis = −1.91).
COVID-19
To control for participants’ personal experience of being infected with COVID-19, we asked whether they had received a positive test result for COVID-19 before completing the survey. Responses included yes, no, and I don’t know.
Demographic Measures
We examined sociodemographic characteristics, including sex (male, female), age group, race/ethnicity (non-Hispanic White, non-Hispanic American Indian/Alaska Native, non-Hispanic Black/African American, Hispanic, and other [Asian, multiracial, not identified]), and relationship status (married or cohabiting, single/widowed/divorced). We also included a modified version of the US Consumer Financial Protection Bureau’s Financial Well-Being Scale, which assesses participants’ sense of control over their finances and emphasizes economic stability. 30 Scores range from 0 to 5, where 0 represents the lowest degree of financial well-being and 5 represents the highest degree of financial well-being. We also controlled for employment status (full-time, part-time) and job tenure (<1 year, ≥1 year).
Statistical Analyses
To assess the relationship between workplace conditions and mental health, we first used binomial logistic regression models. We determined which types of workplace protections and modifications were associated with perceptions of safety and being protected by one’s employer. To control for variation in workplace experiences, we included respondents’ employment status (part-time/full-time) and job tenure (≥1 year). The 2 indicators of respondents’ risk perceptions represent distinct perspectives: 1 considers perceptions of feeling personally safe, and the other reflects perceptions of organizational measures to protect employees. Although significant (P < .001) using a 2-tailed test, the magnitude of the Pearson bivariate correlation (r = .51) between the workplace safety measure and the workplace protection measure suggested that they could be considered independently.
We then estimated 2 separate ordinary least squares (OLS) regression models to analyze the relationship between measures of mental health distress (PHQ-4 and PSS-4) and perceptions of workplace risks. The 2 workplace measures served as the key independent variables while controlling for individual-level socioeconomic factors. Although significant (P < .001), the magnitude of the bivariate correlation (r = .65) between the PHQ-4 and PSS-4 suggested sufficient independence to justify 2 separate OLS models. Although the PHQ-4 can be assessed through categorical scoring, 11 our data violated the parallel lines assumption that each increase between PHQ-4 level is equivalent. Instead, we used the full PHQ-4 scale (0-12) for the OLS model, because our data more closely approximated a normal distribution (skewness = 0.47; kurtosis = −0.95) with good scale validity (α = 0.91). The PSS-4 also demonstrated an acceptable scale validity (α = 0.72) and an acceptable normal distribution (skewness = −0.58; kurtosis = −0.26) for OLS analysis. We performed all analyses using IBM SPSS Statistics (IBM Corp).
Results
Of the 3344 grocery store workers surveyed in July 2020, 66.6% identified as female (Table 1). Most respondents (62.1%) identified as White, and 50.7% reported being married or cohabitating. The sample consisted of full-time (48.4%) and part-time (51.6%) workers, and 79.4% had been working with the same employer for ≥1 year.
Characteristics of respondents to the Arizona Frontline Worker Survey (N = 3344), Arizona, 2020 a
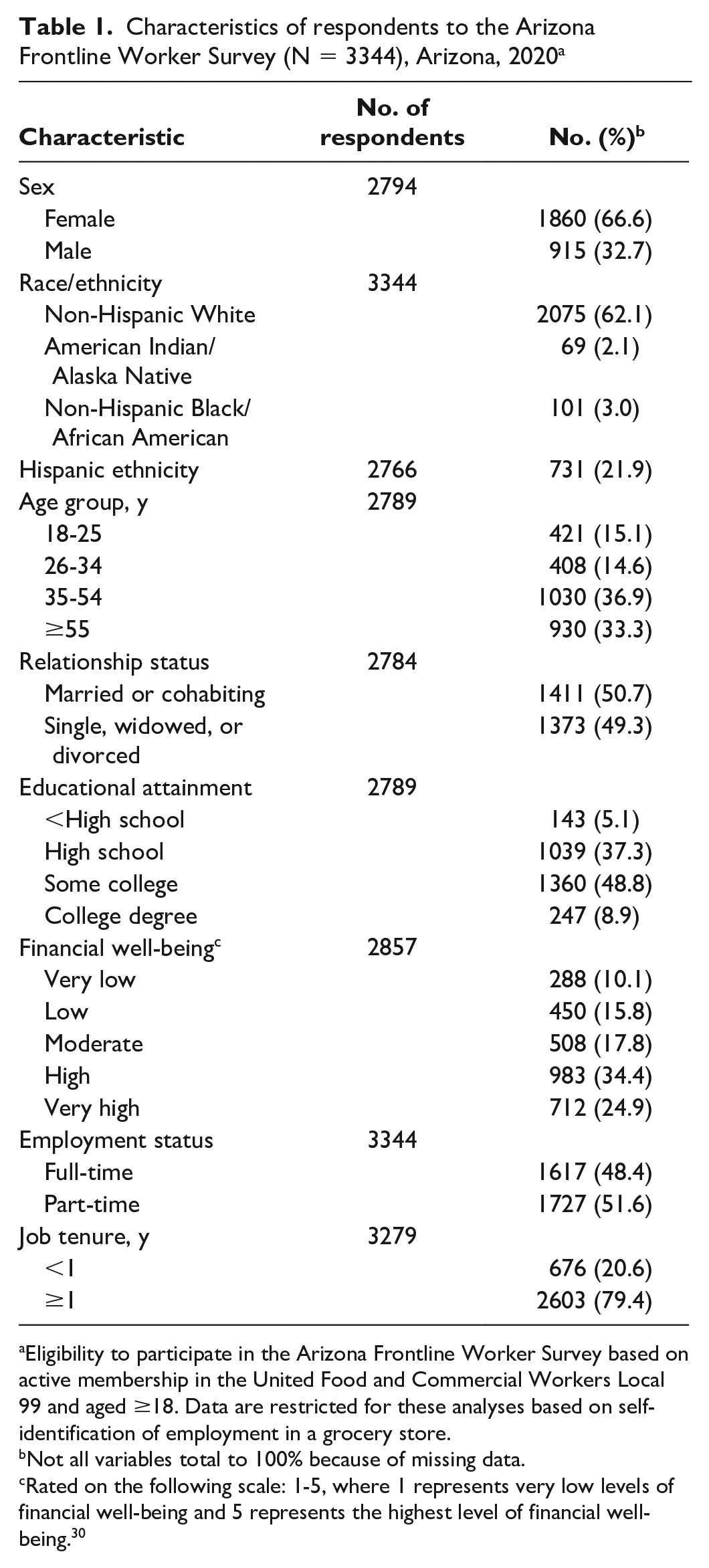

Eligibility to participate in the Arizona Frontline Worker Survey based on active membership in the United Food and Commercial Workers Local 99 and aged ≥18. Data are restricted for these analyses based on self-identification of employment in a grocery store.
Not all variables total to 100% because of missing data.
Rated on the following scale: 1-5, where 1 represents very low levels of financial well-being and 5 represents the highest level of financial well-being. 30
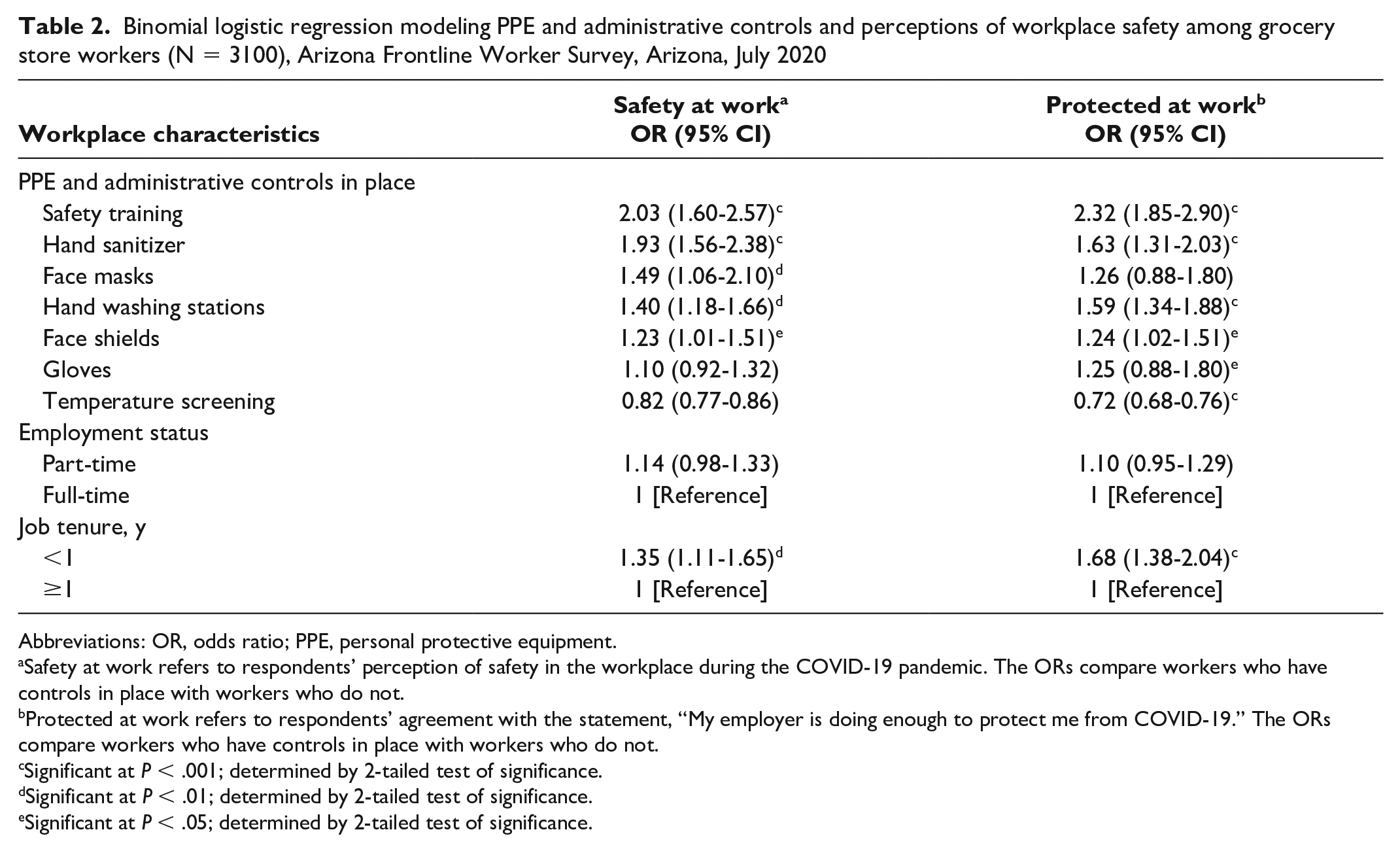
Most respondents perceived their workplace to be safe during the COVID-19 pandemic (1972 of 3169, 62.2%) and felt that their employer offered workplace protections to keep them safe (1664 of 3169, 52.5%). The largest predictor of feeling both safe and protected from COVID-19 was having access to workplace safety training. Respondents with access to safety training were twice as likely as respondents who did not have access to safety training to feel safe (odds ratio [OR] = 2.03; 95% CI, 1.60-2.57; P < .001) (Table 2). Respondents who had access to safety training were more than twice as likely as respondents who did not have access to safety training to report feeling protected at the workplace (OR = 2.32; 95% CI, 1.85-2.90; P < .001).
Binomial logistic regression modeling PPE and administrative controls and perceptions of workplace safety among grocery store workers (N = 3100), Arizona Frontline Worker Survey, Arizona, July 2020
Abbreviations: OR, odds ratio; PPE, personal protective equipment.
Safety at work refers to respondents’ perception of safety in the workplace during the COVID-19 pandemic. The ORs compare workers who have controls in place with workers who do not.
Protected at work refers to respondents’ agreement with the statement, “My employer is doing enough to protect me from COVID-19.” The ORs compare workers who have controls in place with workers who do not.
Significant at P < .001; determined by 2-tailed test of significance.
Significant at P < .01; determined by 2-tailed test of significance.
Significant at P < .05; determined by 2-tailed test of significance.
PPE and administrative controls with significant correlations to perceptions of safety included having access to hand sanitizers (OR = 1.93; 95% CI, 1.56-2.38; P < .001) and hand washing stations (OR = 1.40; 95% CI, 1.18-1.66; P < .001). Having access to face masks, face shields, and gloves was not a significant correlate of perceived safety. Correlates to feeling protected at the workplace followed a similar pattern: access to hand sanitizers (OR = 1.63; 95% CI, 1.31-2.03; P < .001) and access to hand washing stations (OR = 1.59; 95% CI, 1.34-1.88; P < .001) were both significant. Having access to face shields (OR = 1.24; 95% CI, 1.02-1.51; P = .04) and gloves (OR = 1.25; 95% CI, 0.88-1.80; P = .02) was significant but having access to face masks was not. Of the 2 employment conditions, only job tenure was significantly correlated with both outcome measures, and more strongly so for feeling protected at the workplace.
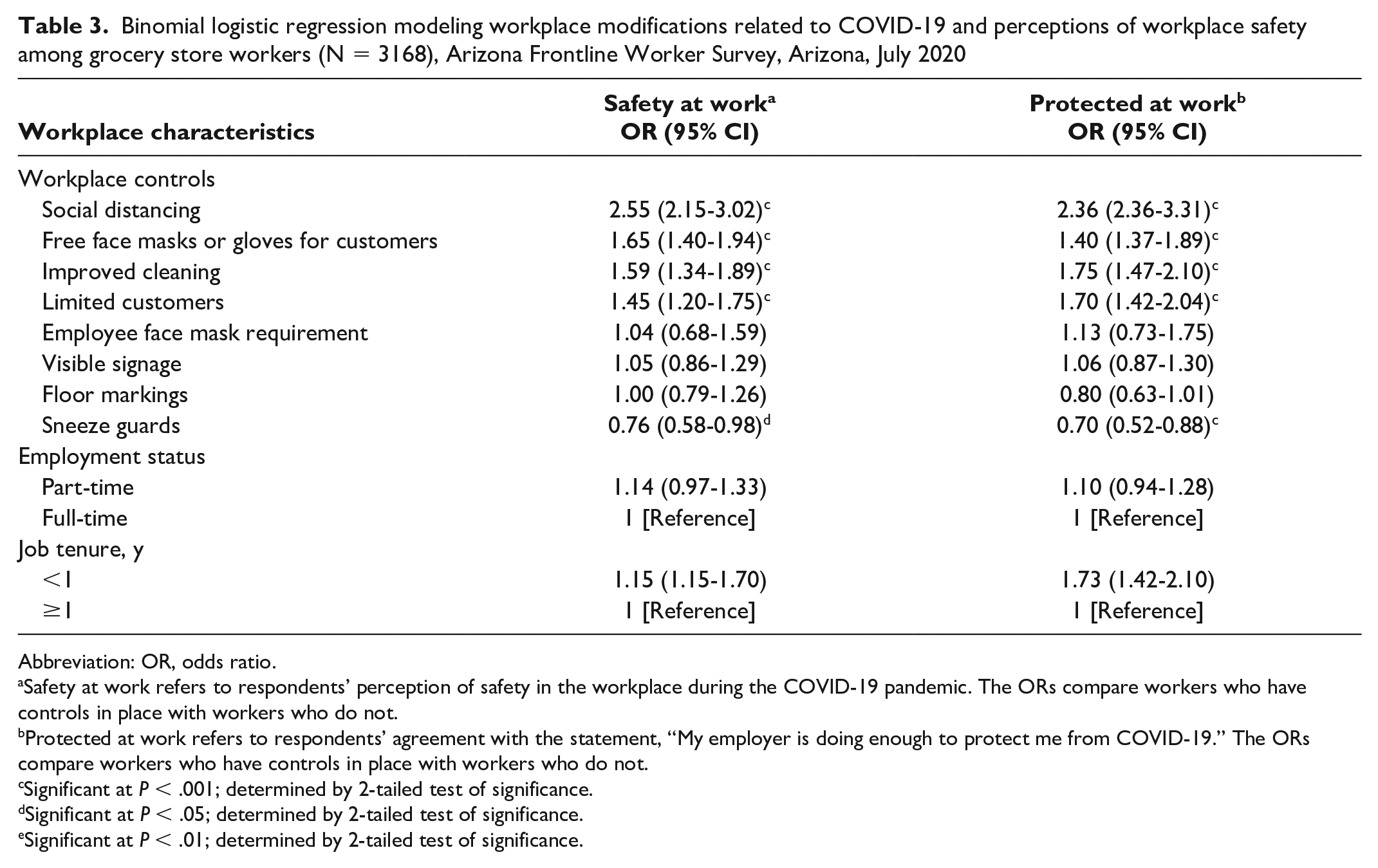
The strongest correlation observed between perception of safety and workplace protection was the requirement that customers maintain 6 feet of social distancing. Respondents reporting that their workplace required social distancing were 2.55 (95% CI, 2.15-3.02; P < .001) times more likely to feel safe at work and 2.36 (95% CI, 2.36-3.31; P < .001) times more likely to feel protected from COVID-19 at work (Table 3). For perceived safety at work, other workplace modifications with significant correlations included providing free face masks or gloves to customers entering the store (OR = 1.65; 95% CI, 1.40-1.94), modifying store hours to facilitate improved cleaning regimens (OR = 1.59; 95% CI, 1.34-1.89), and limiting the total number of customers allowed in the store at any given time (OR = 1.59; 95% CI, 1.34-1.89; all P < .001).
Binomial logistic regression modeling workplace modifications related to COVID-19 and perceptions of workplace safety among grocery store workers (N = 3168), Arizona Frontline Worker Survey, Arizona, July 2020
Abbreviation: OR, odds ratio.
Safety at work refers to respondents’ perception of safety in the workplace during the COVID-19 pandemic. The ORs compare workers who have controls in place with workers who do not.
Protected at work refers to respondents’ agreement with the statement, “My employer is doing enough to protect me from COVID-19.” The ORs compare workers who have controls in place with workers who do not.
Significant at P < .001; determined by 2-tailed test of significance.
Significant at P < .05; determined by 2-tailed test of significance.
Significant at P < .01; determined by 2-tailed test of significance.
Mental Health Distress
Scores on the PHQ-4 revealed high levels of mental health distress: 19.4% of respondents reported severe mental health distress, 16.8% reported moderate levels, 27.9% reported mild levels, and 35.9% reported normal levels. Results on the 2 PHQ-4 subscales revealed similarly high symptoms of anxiety (43.8%) and depression (33.0%). The mean score for the PSS-4 was 6.9 (SE = 3.1) on a range of 0-16.
A perception of being safe at work was significantly correlated with less mental health distress, on average lowering PHQ-4 scores by 1.4 points on a scale of 0-12. Feeling protected by one’s employer was also significantly correlated with better mental health, lowering PHQ-4 scores by 0.6 points (Table 4). However, only the perception of being safe at work was a significant predictor of lower perceived stress levels. In addition, having received a positive test result for COVID-19 was a significant predictor of higher levels of both the PHQ-4 and PSS-4.
Ordinary least squares regression modeling of mental health distress related to COVID-19 and workplace safety, Arizona, July 2020
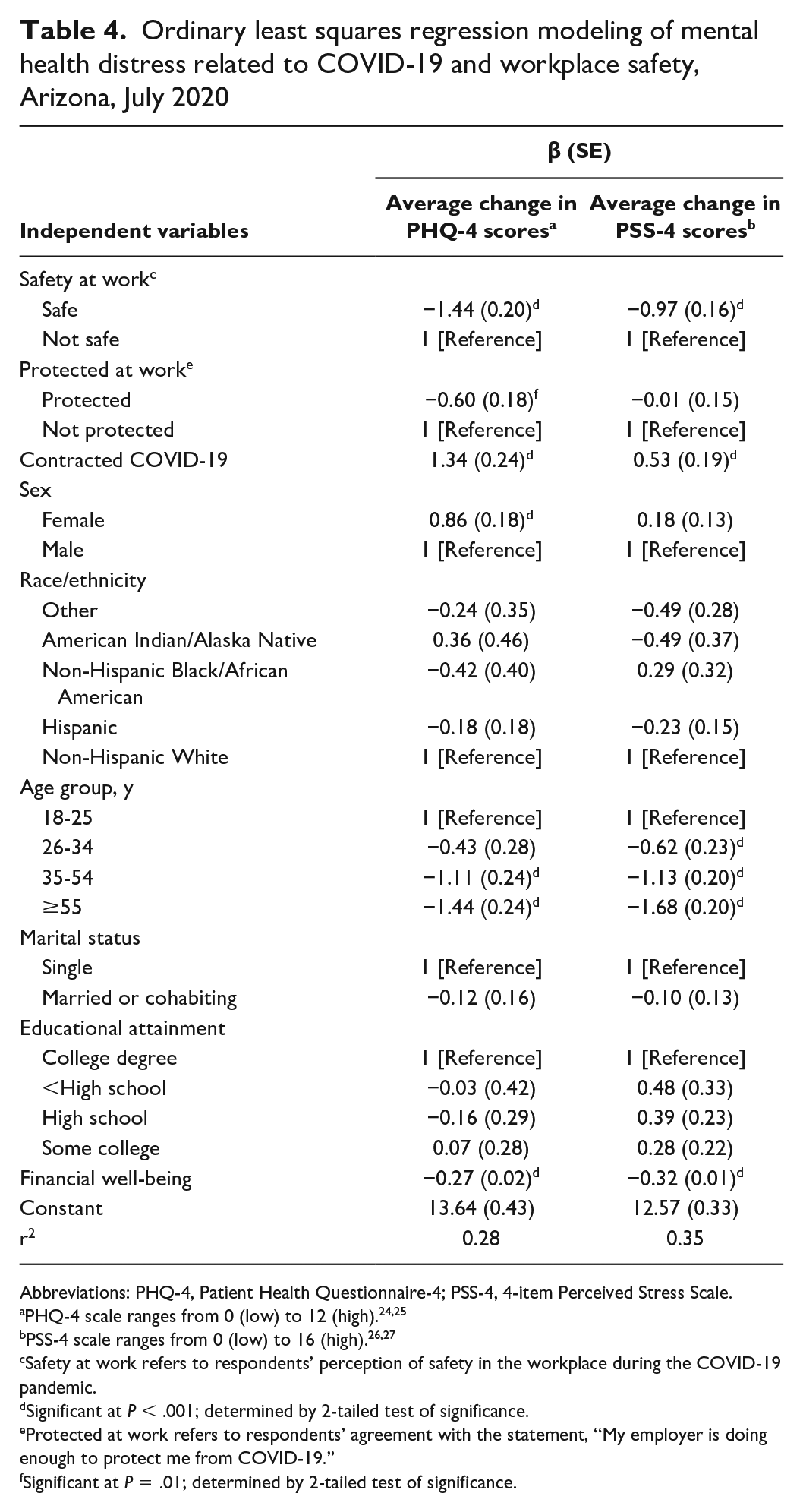

Abbreviations: PHQ-4, Patient Health Questionnaire-4; PSS-4, 4-item Perceived Stress Scale.
PHQ-4 scale ranges from 0 (low) to 12 (high).24,25
PSS-4 scale ranges from 0 (low) to 16 (high).26,27
Safety at work refers to respondents’ perception of safety in the workplace during the COVID-19 pandemic.
Significant at P < .001; determined by 2-tailed test of significance.
Protected at work refers to respondents’ agreement with the statement, “My employer is doing enough to protect me from COVID-19.”
Significant at P = .01; determined by 2-tailed test of significance.
Of the demographic control variables, only age and financial well-being were consistently significant predictors of mental health distress and perceived stress. Older respondents aged 35-54 and ≥55 were more likely than respondents aged 18-25 to report low scores on the PHQ-4 and the PSS-4, and respondents aged ≥55 were the most likely to report lower scores. Women were more likely than men to report higher levels of mental health distress as measured in the PHQ-4 but not the PSS-4. Higher levels of financial well-being were also significantly correlated with lower scores on the PHQ-4 and PSS-4.
Discussion
Our study of the effects of the COVID-19 pandemic on grocery store workers found significantly high levels of mental health distress among Arizona’s grocery store workforce. Approximately 20% of our sample reported severe levels of mental health distress on the PHQ-4 and above-average levels of stress on the PSS-4. Although these measures are both ultra-brief assessments, they have been cross-validated for their psychometric reliability.25,26 These levels of mental health distress were 3 to 4 times higher than PHQ-4 estimates of the general US adult population from 2019. Our findings were also well above contemporary estimates of mental health distress during the COVID-19 pandemic and were similar to related studies on retail workers.2,11,28,31 The retail work environment has been found to be less healthy than other occupational environments through similar self-reported measures in previous research. Our findings additionally suggest that frontline workers are at increased risk of developing behavioral health problems during the pandemic because of elevated workplace stressors. 32
Being an essential worker increases one’s risk of exposure to COVID-19, and this core vulnerability is heightened by the demographic characteristics of people in precarious occupations with little job security, such as grocery workers. Several key sociodemographic factors commonly associated with the retail workforce were significantly correlated with poor mental health outcomes, including being female, of younger age, and financially insecure, which are all consistent predictors of mental health distress. 11 These factors are mirrored in the inequities that have been seen in the COVID-19 response, from access to testing and workplace protections to vaccine distribution. 33 Because these structural inequalities that place low-income groups such as retail workers at increased risk of exposure to health and economic risks are unlikely to change, our results will likely hold true for later stages of the pandemic, if not beyond.
Although engineering controls such as sneeze guards, line barriers, and accompanying signage that are designed to separate workers from exposure risks might be more visible in work environments, our data suggest that workers’ perceptions of risk are largely determined by administrative controls that provide guidance to employees and govern customer behavior. The lack of clear federal and state guidance on face mask use and the inconsistent implementation of policies at the time of study may have contributed to the nonsignificant effect of face masks on perceptions of safety and protection. The absence of employer-initiated policies, coupled with diminishing compliance with public health recommendations, creates the potential for situations that jeopardize the well-being and safety of employees. 34 Building a sense of safety and trust in management is essential for ensuring that workers follow safety protocols and is likely a motivating factor in employees’ decisions to get vaccinated. 35
Limitations
This study had several limitations. First, our study was limited by its cross-sectional design, reliance on self-reported measures, and focus on a single state. Second, all respondents were represented by a labor union, which limited our study’s generalizability to nonunion workers. However, because unions typically promote pro-worker policies, such as access to safety training, nonunion workers who lack formal representation may be at even higher risk than union members for mental health illness. Third, although knowledge about SARS-CoV-2 transmission has increased, our core findings on the relevance of workplace trainings and the role of employer policies in protecting the physical health and, indirectly, the mental health, of employees are relevant.
Conclusions
The COVID-19 pandemic has placed grocery store workers on the front lines of essential services but left them largely ill-prepared to safely navigate their interactions with coworkers and customers, which greatly increases their risk of exposure to SARS-CoV-2. The complex situation of the grocery store worker and other employees in the retail sector needs to be considered to mitigate the long-term effects of the COVID-19 pandemic. Work environments that require frequent interactions with people outside one’s household, coupled with a lack of adequate support services, render this group vulnerable to negative physical and mental health consequences.
As the pandemic continues, coordinated, equity-based policies and worker safety initiatives are needed that place the health and safety of the employee at the center. Our study results offer insights for local and state governments that can facilitate access to safety trainings. Public health responses to the COVID-19 pandemic have largely been presented as recommendations and guidelines, placing employee mental health at risk when coworkers or customers do not comply. Both safety trainings and administrative controls increase employees’ perceptions of their employers’ commitment to their safety, which can motivate them to follow safety protocols and reduce transmission risks in the workplace. These findings further indicate the need for employer-initiated efforts and policies to ensure accessibility to the COVID-19 vaccine, as vaccination presents a form of assurance to employees in enhancing workplace safety.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: B. Mayer was supported by the Natural Hazards Center’s Quick Response Research Award Program. This program is based on work supported by the National Science Foundation (NSF award #1635593). Any opinions, findings, conclusions, or recommendations expressed in this material are those of the authors and do not necessarily reflect the views of NSF or the Natural Hazards Center.
