Abstract
Anorexia Nervosa is the most deadly mental illness due to the high mortality and relapse rates after reaching remission. The systematic review investigated the effectiveness of two empirically validated interventions (Family-Based Therapy [FBT] and Adolescent-Focused Therapy [AFT]) for an adolescent or young adult living with Anorexia Nervosa to reach partial or full remission and expected weight ratios. Twelve studies published between 1994 and 2015 were evaluated and indicated that FBT resulted in significant weight gain and higher partial and full remission rates than AFT, demonstrating its superiority in treating AN in adolescents and young adult samples, in one instance, at least up to 4 years. Despite FBT and AFT delivery, a significant proportion of participants did not achieve their target weight or full remission, indicating that both treatments may not be effective in all circumstances.
Keywords
Across the globe, approximately 70 million people live with an eating disorder (McGorry, 2020). Eating disorders are serious, complex, and potentially life-threatening mental illnesses (McGorry, 2020). Anorexia Nervosa (AN) is a specific eating disorder categorised by extremely low body weight and the distorted view of the patients’ body image (American Psychiatric Association, 2013). Cognitions revolve around an excessive fear of weight gain or persistent lack of recognition of the seriousness of low body weight, evidenced by extreme dieting behaviours, which often co-occur with intense elevated exercise (American Psychiatric Association, 2013). There are two subtypes of AN: Restrictive and Binge-Eating/Purging. Rigid rules (e.g., only eating food of a specific colour) often accompany extreme dieting and undue amounts of exercise, characterising Restrictive AN (American Psychiatric Association, 2013). Whereas, Binge-Eating/Purging AN sees a person also engage in periods of over-eating, self-prompted vomiting, and abusing laxatives, diuretics, or enemas (American Psychiatric Association, 2013).
Anorexia nervosa is the most deadly mental illness as 25% of individuals that reach remission are likely to relapse, and the mortality rate is ten times higher for young people between 15 and 24 years than their same-aged peers (Arcelus et al., 2011; Keski-Rahkonen et al., 2008). Anorexia Nervosa is prevalent in up to 3.0% of adolescent females, with a lifetime prevalence of 0.3% (Arcelus et al., 2011). Male prevalence is less understood; however, clinical populations typically indicate a ratio of 10:1 female-to-male, with a lifetime prevalence up to 0.5% (American Psychiatric Association, 2013; Arcelus et al., 2011). Nevertheless, AN commonly goes undiagnosed, with only 25% of individuals experiencing body image and dieting concerns obtaining professional support (Arcelus et al., 2011).
Anorexia Nervosa Treatments
Family-Based Therapy (FBT) is an evidence-based psychotherapy incorporating family members as the focus of the treatment process. It is commonly used to treat eating disorders, centring on weight restoration (Chen et al., 2016). The FBT used today draws on Behavioural Family Systems Therapy developed by Robin and Foster (1989), where clients are seen as incompetent in meeting their biological needs. The approach encourages the client to see their strengths and individuality, simultaneously empowering parents to take control of the child’s nutrition and daily food intake to promote weight gain (Chen et al., 2016). Although FBT is the recommended first-line approach to treating AN in adolescents and young adults, concerns have been raised regarding its efficacy and replicability when treating individuals across the lifespan (Chen et al., 2016).
Alternatively, Adolescent-Focused Therapy (AFT) is an individual psychotherapy commonly used to treat eating disorders in teenagers and young adults (Lock et al., 2010). The AFT used today draws on Ego-Orientated Individual Therapy developed by Garner and Garfinkel (1984), as the client demonstrates a reduced self-concept, characterising self-control as a biological need. It explores the client’s strengths and abilities, challenging cognitive distortions concerning body image and dietary restraint in a supportive context (Lock et al., 2010). However, there is limited research exploring the efficacy of AFT and related factors influencing the likelihood of remission.
There is a plethora of research and well-established relationships concerning FBT for AN treatment and remission rates in adolescents and young adults, yet, there is limited research exploring the efficacy of AFT for the likelihood of remission. Moreover, no research has systematically examined the difference between FBT and AFT in remission rates and treatment outcomes. Therefore, the present systematic review aims to compare the efficacy of AFT and FBT in treating adolescents and young adults diagnosed with AN to reach and maintain full remission and inform psychotherapists working in the field of associated considerations. The research question for the study is: Is there a difference in the effectiveness of FBT and AFT for an adolescent or young adult living with Anorexia Nervosa to reach partial or full remission and expected weight ratios?
Method
Search Strategy
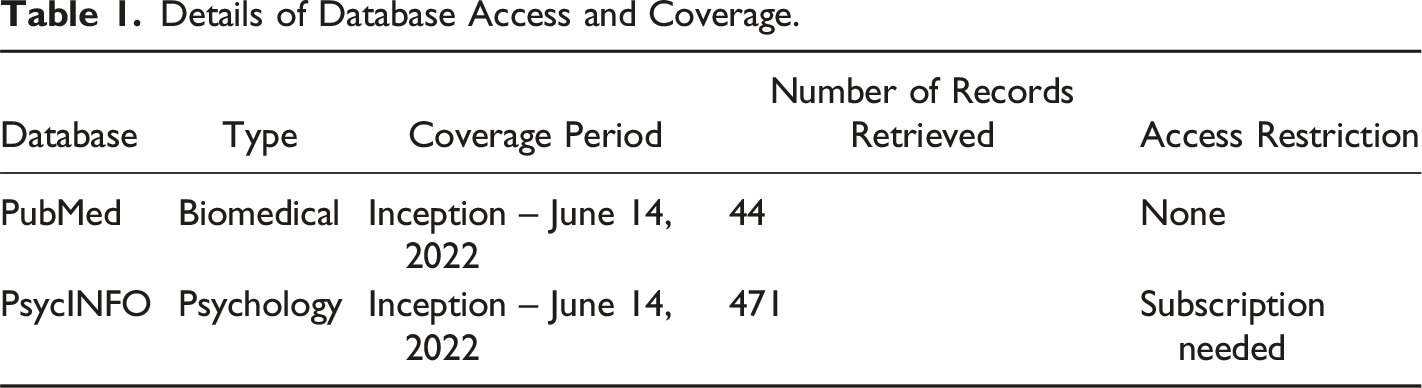
Details of Database Access and Coverage.
Eligibility Criteria
Several preconditions were determined for inclusion of a study in the present research: (1) Focus on AN as the sole eating disorder; (2) A diagnosis of AN to use psychometrically sound anthropometric or self-report measure, or interview protocols using the DSM-III-R, DSM-IV, or DSM-V, with or without the amenorrhea criteria (American Psychiatric Association, 1987; 1994; 2013); (3) Comparison of AFT and FBT in an outpatient program; (4) Participants were adolescent or young adults (11 years to 25 years old), of any gender; (5) Any date; (6) Any research design. Review articles and book chapters were excluded from the present study to explore the practical potentials and limitations of AFT and FBT on remission rates rather than exploring the theoretical constructs.
Results
Study Selection
The initial search identified 515 articles, with 288 remaining after duplicate removal. (See Figure 1). Abstract screening identified 224 articles that did not compare AFT and FBT or were either a review or book chapter. Remaining studies (n = 64) were screened by full text. Studies were removed if they did not use AFT or FBT treatments (n = 27), did not measure remission rates (n = 15), were not an outpatient program (n = 7), or participants were not within the required age range (n = 7). Of the remaining eight studies, reference lists indicated four further studies which met inclusion criteria, and these were retrieved and included in the final sample of studies (N = 12). PRISMA flowchart illustrating article selection.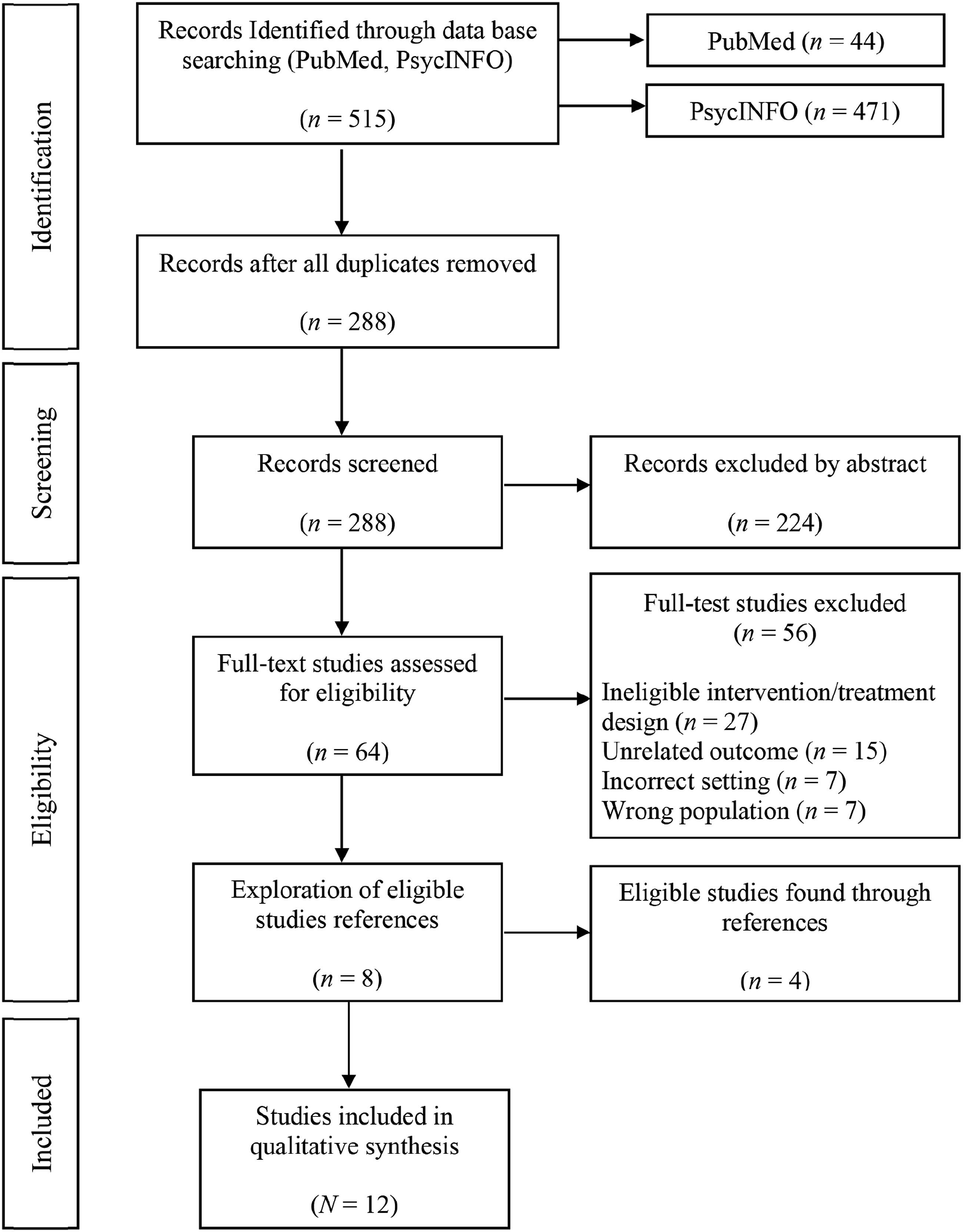
Study Characteristics
Participants
Studies in the final sample were published between 1994 and 2015. Sample sizes ranged from 22 to 121 participants, between the ages of aged 11 and 20 years old. Predominantly, participants were females (91%), followed by males (9%). All studies used randomised control trials with pre and post-testing to assess remission and associated factors.
Diagnosis
Diagnosis of AN in the studies used the DSM-III-R (n = 3) or DSM-IV (n = 9). All studies measured Body Mass Index (BMI). Also, nine studies employed the percentage of expected body weight (EBW), using the Centres for Disease Control and Prevention norms for age and gender and the Eating Disorder Examination (EDE, v12; Cooper et al., 1989; Schantz & Tsang, 2003). The remaining three studies administered the Eating Attitude Test, version 26 (EAT-26; Garner & Garfinkel, 1979), Body Shape Questionnaire (BSQ; Cooper et al., 1987), and three scales of the Eating Disorder Inventory (Garner et al., 1983).
Scales
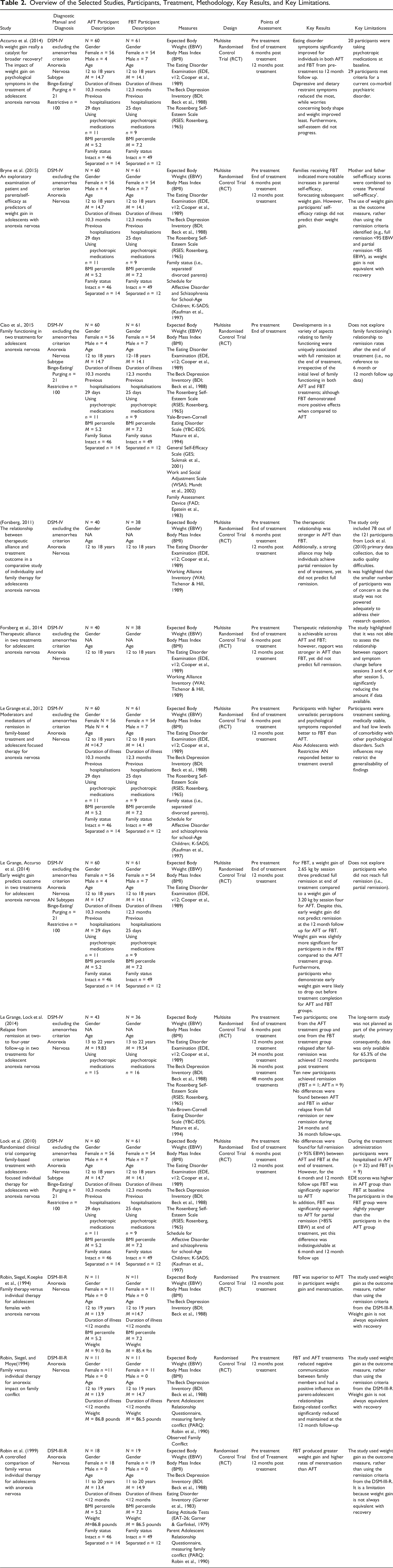
Overview of the Selected Studies, Participants, Treatment, Methodology, Key Results, and Key Limitations.
Quality Rating
The primary studies that explored weight increases or remission rates include Lock et al. (2010), Le Grange, Lock et al. (2014), and Robin, Siegel, and Moye (1994; 1999). However, most of the studies were secondary (i.e., using data from the primary studies). Each secondary study explored specific components identified in the three primary studies contributing to FBT’s and AFT’s effectiveness on adolescents and young adults diagnosed with AN reaching remission. Thus, the secondary studies add to the research and assist clinicians to identify the most effective treatment for AN. Furthermore, the three primary studies were deemed robust. All primary studies included utilised randomised control trials and sound psychometric assessments, and had a representative sample.
Discussion
The present systematic review aimed to compare the efficacy of AFT and FBT in treating adolescents and young adults diagnosed with AN to reach and maintain full remission and inform psychotherapists working in the field of factors to consider in therapy delivery.
Treatment Efficacy
Robin, Siegel, and Moye (1994) reported FBT and AFT were equally effective interventions in improving weight gain at the end of treatment. However, at the 12-month follow-up, the number of participants who met their target weight and began menstruating increased substantially for FBT and only mildly for AFT. Robin et al. (1999) results support Robin, Siegel, and Moye (1994) outcomes, indicating pronounced differences between FBT and AFT at the end of treatment, yet, FBT demonstrated meaningful improvements over AFT at the 12-month follow-up.
In comparison, Lock et al. (2010) indicated that FBT was superior to AFT at end of treatment, with significantly more participants in FBT reaching partial and full remission. Lock et al. (2010) also found at the 6-month and 12-month follow-ups, FBT remained superior to AFT for full remission; however, they were equivalent for partial remission rates. Remission rates were significantly lower than Robin, Siegel, and Moye (1994, 1999) studies. Despite the low remission rates, Lock et al. (2010) used definitive cut-off markers from the DSM-IV diagnostic criteria, as opposed to relying on BMI alone (i.e., full revision >95% EBW and partial remission >85% EBW). The differences may also result from variance among participant sizes. Lock et al. (2010) had a large sample (N = 121) and a moderate main effect when compared to the low power described in Robin, Siegel, and Moye (1994; N = 22) and Robin et al. (1999; N = 37).
Le Grange, Lock et al. (2014) tested the efficacy of FBT and AFT up to four years after Lock et al. (2010) treatments. Le Grange, Lock et al. (2014) found at the 24-month follow-up, more participants in the AFT than FBT relapsed after full remission, yet a significantly larger proportion of new participants in AFT had achieved full remission. Furthermore, relapse from full remission and new participants meeting full remission was not distinguishable between FBT and AFT treatments at the 36-month and 48-month follow-up (Le Grange, Lock et al., 2014). Le Grange, Lock et al. (2014) also explored early weight gain factors likely to predict remission at the end of treatment. They found that participants who gained a minimum of 2.65 kg by week three for FBT and 3.20 kg by week four for AFT were likely to reach partial or full remission at the end of treatment. Results highlight that early weight gain was not a predictor of partial or full remission for AFT or FBT; however, this was the only study that explored remission rates beyond the 12-month follow-up period.
Similarly, Le Grange et al., 2012 was the only study that tested the difference between baseline scores and their relationship in predicting remission. Participants with higher baseline scores benefited more from FBT than AFT, expressed by higher partial and full remission rates. Also, they compared AN subtypes and found that Binge-Eating/Purging AN responded significantly less to either treatment than Restrictive AN.
Across the primary studies, there were differences in treatment retention rates. In Robin, Siegel, and Moye’s (1994), retention rates were 100 and 82% for FBT and AFT, respectively; Lock et al. (2010) retention rates were 84% for FBT and 92% for AFT; Robin et al. (1999) retained 100% of for FBT and AFT. Regarding Robin, Siegel, Koepke et al. (1994), differences may be due to FBT requiring more treatment hours than AFT. Also, weight gain was slightly superior for participants in FBT than AFT, potentially demonstrating the difference. Alternatively, Lock et al. (2010) and Le Grange, Accurso et al. (2014) noted participants demonstrating early weight gain were likely to drop out before treatment completion; however, no patterns or differences were evident in drop-out rates between the treatments.
Furthermore, participants requiring hospitalisation during the study stopped treatment and continued when discharged. Lock et al. (2010) found more participants were hospitalised from AFT compared to FBT, with a median number of 12 and 10 days for FBT and AFT, respectively. Weight gain during hospitalisation was a median of 1.0 kg for FBT and 1.7 kg for AFT participants. In comparison, Robin et al. (1999) had higher hospital admissions rates for FBT than for AFT. Similarly, Robin, Siegel, and Moye (1994) indicated more FBT participants than AFT were hospitalised, with an average of 26.4 days. The mean days spent in hospital for Robin et al. (1999) study is unknown; however, participants were discharged when they reached 80% of their target weight; this likely inflated the results. Furthermore, most of Lock et al.'s (2010) hospitalisations occurred in the first four weeks of treatment. Le Grange, Lock et al. (2014) found that weight increases during this period predicted remission at the end of treatment, demonstrating a limitation.
External Influences on Remission Rates
Each study investigated external factors that could influence the effectiveness of FBT and AFT. Accurso et al. (2014) measured psychological symptoms of AN regarding dietary restraint, depression, and perceptions of self-esteem, body image, and weight. They found depressive and dietary symptoms significantly reduced regardless of treatment. A similar effect was found in Robin et al.’s (1999) study. Unhealthy perceptions of daily food intake notably reduced for FBT and AFT; however, at the 12-month follow-up, AFT was superior for reducing unrealistic perceptions. Nevertheless, depression scores were much higher for FBT than AFT, contrasting with Accurso et al.’s (2014) findings. Differences between the two studies may be due to differences in each treatment’s delivery protocol. For example, in FBT, the client is not considered competent enough to control their daily food intake. Instead, the parents/caregivers take on the responsibility, which may influence the client’s perceptions of self-efficacy and mental well-being (Byrne et al., 2015). Byrne et al. (2015) explored differences in adolescent and parental self-efficacy ratings at full remission. Families receiving FBT indicated notable increases in parental self-efficacy, forecasting subsequent weight gain. However, participants’ self-efficacy ratings did not predict their weight gain.
Ciao et al., 2015 measured levels of family conflict and subsequent effects on remission using data from Lock et al. (2010) primary study. Ciao et al., 2015 found developments in communication and support were associated with full remission at end of treatment, irrespective of initial level of family functioning in either treatment. In comparison, in Robin et al. (1994), AFT and FBT produced notable reductions in negative communication. Specifically, FBT demonstrated remarkably higher interactions and improvements in eating-related conflict, which were maintained at the 12-month follow-up. Although AFT’s primary focus is not on family support and connection, significant communication improvements were associated with weight increase (Robin et al., 1994).
Forsberg (2011) and Forsberg et al. (2014) compared the level of therapeutic rapport and its effect on remission. Consistently, high levels of therapeutic rapport were found across treatment groups during each period; however, the AFT group had significantly stronger alliance scores at end of treatment. Additionally, a strong therapeutic alliance was identified to predict partial remission by end of treatment, yet it did not predict full remission. Forsberg (2011) and Forsberg et al. (2014) included only 78 out of the 121 participants from Lock et al. (2010) primary study due to audio quality difficulties, highlighting limitations as they did not have adequate power to address their research question.
Conclusions
Across the three primary studies, FBT resulted in significant weight gain and higher partial and full remission rates than AFT, demonstrating its superiority in treating AN in adolescents and young adult samples, in one instance at least up to 4 years. Hence, FBT in the current sample of empirical literature demonstrates greater long-term efficaciousness in the remission of AN. However, AFT may be a suitable treatment when FBT is not feasible (e.g., there is a high family disconnect).
Despite FBT and AFT delivery, a significant proportion of participants in the three primary studies did not achieve their target weight or full remission, indicating that both treatments may not be effective in all circumstances. Additionally, the therapeutic relationship, anxiety and depression symptoms, hospitalisation, perceptions of family conflict, self-efficacy, body image, and weight influence participants’ remission across FBT and AFT. Psychology practitioners are recommended to consider including an additional therapeutic technique also known to positively influence Anorexia Nervosa weight gain and remission (e.g., Cognitive-Behaviour Therapy; Nyman-Carlsson et al., 2020).
Furthermore, there are only three primary studies, and the most recently published article is from 2010; thus, limitations arise when extrapolating data from such a small number of articles during a similar period. Such limitations are concerning, as additional factors may impact treatment nowadays (e.g., social media use and social change). Also, all primary studies were conducted in the United States of America, restricting the generalisability of treatment effects to other populations as cross-cultural considerations are not regarded. It is recommended that other research groups conduct longitudinal studies, exploring AFT and FBT’s effectiveness in attaining and maintaining remission among adolescents and young adults diagnosed with AN. Comparing the effectiveness of AFT to the current gold standard approach (FBT) may provide clients and families with a strong treatment alternative and improve remission rates by acknowledging that not all clients respond positively to all treatment approaches. Such information would aid in informing treating practitioners of AFT and FBT’s potential and limitations in reducing the prevalence and mortality associated with AN.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
