Abstract
End-of-life doulas (EOLDs) provide non-medical, holistic support to individuals at or near the end-of-life. However, understanding of the factors that enable EOLDs to provide effective support remains limited. This scoping review examines existing literature on the EOLD role and synthesises key components, mapping them onto a logic model. A systematic search was conducted using relevant keywords across five databases. Seventeen articles met the inclusion criteria for the final analysis, all conducted within high-income countries. Key findings highlight the importance of timely referrals, which enable EOLDs to provide relational, person-centred support that promotes the wellbeing of both patients and carers. The review also identifies broader societal benefits, including improved death literacy. The resulting logic model offers a timely and foundational framework to guide discussions on integrating EOLDs into health and social care systems. Further research is recommended to refine the logic model, explore EOLD practices across diverse global contexts, and assess potential cost-benefit implications.
Background
End-of-life care systems are complex and non-linear, spanning health, medical, care, and social support pathways, influenced by ever-shifting cultural norms and societal values shaping how people are born, live, and die. With worldwide advances in medicine and technology, coupled with ageing populations, there is increased demand and pressure on social, primary care, and community care services (Morin et al., 2016; Sallnow et al., 2022; Sleeman et al., 2019). Increasing numbers of individuals require sustained care and support throughout their lives, particularly at the end-of-life (Bone et al., 2018; Etkind et al., 2017).
It is well documented that palliative care is a human right (Gwyther et al., 2009; Pask et al., 2022) to provide physical, emotional and practical support that can improve patient outcomes, reduce acute hospital care admissions, and support people to die in their preferred place (Sleeman et al., 2021); however, this remains a neglected global issue (Horton, 2018; Peeler et al., 2024; World Health Organisation, 2021). People with social and economic vulnerabilities often have less knowledge and access to quality end-of-life care (Stajduhar et al., 2019) as do ethnic minority groups (Pask et al., 2022; Tobin et al., 2021), people living in rural areas (Cai and Lalani, 2022), and people with social circumstances that make them vulnerable (Care Quality Commission, 2016). Finding ways to address preventable suffering and provide integrated, person-centred care and support is pressing in the face of this crisis.
The end-of-life doula (EOLD) role has developed in part in response to these trends and challenges (Rawlings et al., 2019). Working in people’s homes, hospitals, care homes, and hospices, EOLDs may liaise with health and social care practitioners, advocating for the patient if necessary, and providing person-centred support when health and social care services are not always available (Murphy, 2021) which may continue into bereavement (Fersko-Weiss, 2017; Fukuzawa and Kondo, 2017). This is not a new role, nor is it specific to the Global North. Garces- Foley (2022) traces historical roots of the vigiler, companion, and doulas in the United States. Conisbee (2025) recounts ‘Watchers’ in the UK, primarily women, cognisant of the dying process, providing comfort, and gathering the community or family to the bedside of the dying person. This role was recognised up until the mid-19th century, when it was usurped by predominantly male medical professional expertise. In low-to-middle income countries, non-medicalised end-of-life care may be delivered through locally led community volunteers, traditional healers, or hospital/home-based palliative programs (MacRae et al., 2020). The roles, similar to doulas include holistic home-based care, psychological support, and spiritual guidance. Stonington (2020, p. 120) in his ethnographic account of end-of-life care in Northern Thailand relates some similarities to his training as a doula in the USA ‘putting the dying person in the driver’s seat of his or her own deaths’. Ntizimira (2023), founder of the Safari Concept, presents a palliative care approach grounded in the Ubuntu philosophy of “I am because we are.” Supporting communication between healthcare practitioners and families in African countries, and using animal archetypes, the approach highlights non-medical, person-centred care rooted in collective identity and community echoing principles comparable to those underpinning EOLD support.
Despite increasing global interest, statistics on the number of EOLDs, certified organisations, and people who have employed an EOLD remain unknown (Hahn and Ogle, 2022). This may be unsurprising considering that there are variations in the name, and EOLDs may work independently of any organisation. The International End of Life Doula Association INELDA (nd) lists doulas available in several countries including Czech Republic, Germany, Ireland, Italy, Japan, New Zealand, Russia, UK, Mexico, Canada, and the USA; however, EOLD practices in the Global South are less documented in academic literature.
Like birth and postpartum doulas, EOLDs seek to address the non-medical needs of the person and their supporting others (Fukuzawa and Kondo, 2017); however, despite an increasing interest in EOLDs, there are significant gaps in our knowledge. This includes the need to better understand the role and work of doulas, outcomes for those dying and their carers, and broader impacts on service delivery.
At the time of writing, three published reviews have focussed on the EOLD role. Yoong et al. (2022) conducted a scoping review to better understand the role, regulatory impact, and training of EOLDs. They identified thirteen articles and concluded that EOLDs take on diverse roles and forms of support (psychological, spiritual, and practical), offering a continuous presence throughout the end-of-life. Common and specific roles, as a companion and advocate, were identified across three phases: pre-death, active dying and post-death. The authors identified EOLDs as having the potential to bridge gaps in end-of-life care, provide a continuum of support, whilst complementing other health services, but noted a level of confusion among health and social care professionals and the public in understanding what an EOLD was. They suggested further research to explore the views and perspectives of healthcare professionals working with EOLDs and evaluating the outcomes of supported patients. These findings chime with a systematic review conducted by Rawlings et al. (2019) to explore the role of EOLDs and implications for care, health systems, and delivery. They found a paucity of formal research in this area and minimal understanding of the EOLD role and implications on service delivery. Nonetheless, they too suggested the potential utility of EOLDs in providing care directed by the dying person, to complement existing services. Similarly, Thompson and Utz (2024) in their integrative review included 25 articles and summarised emergent themes including the application, identity and perception of the role, concluding that more research is needed to understand how EOLDs could be integrated within policy and practice settings. A nationwide survey of palliative care organizations in Germany found that only 5.6% used EOLD support, yet 17 of these 18 organizations recommended it to other institutions (Volberg et al., 2025).
Research Objectives
There remains limited information on the necessary framework, context, and factors to help the EOLD role become recognised and integrated into end-of-life and palliative care settings. The purpose of this review was to identify and scope the published international literature on EOLDs, with a specific focus on the mechanisms by which they are likely to achieve successful outcomes for individuals supported by EOLD (‘patients’), and their supporting others (‘carers’). The objective was to develop an evidence-informed logic model; a visual representation of inputs, activities, and outputs, which, if achieved, can lead to desired outcomes and any longer-term impacts (Kellogg Foundation, 2004). Logic models have been used within reviews to help identify how a programme works, or might work, identifying relevant outcomes and helping to communicate findings to stakeholders within policy and practice settings (Kneale et al., 2015; Prendergast et al., 2023, 2024).
Methodology
As the EOLD role is an emergent field with a nascent evidence base, an exploratory and iterative process was required. Therefore, a scoping review was chosen involving a transparent and systematic method across a range of study designs (Arksey and O’Malley, 2005; Levac et al., 2010). Here we followed the process described by Arksey and O’Malley (2005), which involved the following stages: • Identifying and refining research questions • Searching databases for relevant literature • Selecting the literature • Charting data • Reporting the results.
We referred to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Scoping Review extension (PRISMA-ScR) checklist (Tricco et al., 2018) to underpin the process and report on the findings (see Supplemental file 1).
Identifying the Research Question
The authors are part of a working group of researchers and academics based in Wales, one of whom is an end-of-life doula. All are engaged in roles working with people affected by end-of-life issues, in professional and/or voluntary capacities, and have been involved in workshops or participatory research with the public. The research question: “What is known about the role of the EOLD and the associated outcomes for patients, carers, and EOLDs?” emerged through discussions with health and social care practitioners, and people affected by end-of-life, including people bereaved and unpaid carers. These highlighted a need for relational, person-centred, and consistent support for the patient and carers, at the end-of-life.
To address this question, the following objectives were further identified: (i) map key components of the EOLD role, (ii) capture associated outcomes to three groups: patients, carers, and EOLD, and (iii) produce a logic model illustrating the inputs, activities, outputs, outcomes, context, and assumptions associated with the role.
Inclusion/Exclusion Criteria
The scoping review included literature on EOLDs supporting any patient and/or their carer. We aimed to be inclusive regarding the role, and recognising the diversity of terminology, we consistently refer to the term end-of-life (EOLD) throughout. We included the following keywords ‘death midwife’, ‘soul midwife’ ‘death doula’, ‘death worker’ ‘end of life doula’. The search string and ProQuest results can be found in Supplemental file 2.
To ensure relevance to current health and social care policy and practice, we included literature spanning the previous 10 years (January 2014–August 2024). There were no geographical restrictions; however, due to limited resources, we only included English language articles.
We excluded reviews from the final selection to avoid double-counting of literature, and letters, opinion pieces, editorials, and theses.
Search Strategy, Data Extraction and Screening
Following the Joanna Briggs Institute method for scoping reviews (Peters et al., 2021) we performed an initial search in ProQuest to identify relevant articles and index terms. A systematic literature search was conducted using five databases: ProQuest (20 databases), PubMed, Scopus, CINAHL, and Web of Science (Supplemental File 1). A grey literature search was conducted on Google, and the first five pages were screened for inclusion. We also searched reference lists of included articles and cited references. The searches were conducted between June and August 2024. We screened articles and included those that reported on the role of EOLDs with substantial reference to inputs required for EOLDs to operate, the activities of EOLDs, and/or the outputs and any outcomes detailed for the patients, carers, and/or the EOLDs themselves.
Search Outcome
A total of 252 records were identified and uploaded onto Mendeley, where 136 duplicates were removed. Two authors screened the titles and abstracts, and 67 articles that did not meet the inclusion criteria were excluded. Potentially relevant studies were retrieved to read in full. Identifying relevant literature was iterative and refined through discussion and reflection. The authors (LP and RS) initially screened the titles and abstracts. Any disagreements were discussed and resolved. Reasons for exclusions are reported in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews) (PRISMA-ScR) detailed in the PRISMA flow diagram (Figure 1). Flow Diagram of Study Selection Protocol (Based on PRISMA 2020 Flow Diagram, Tricco et al., 2018)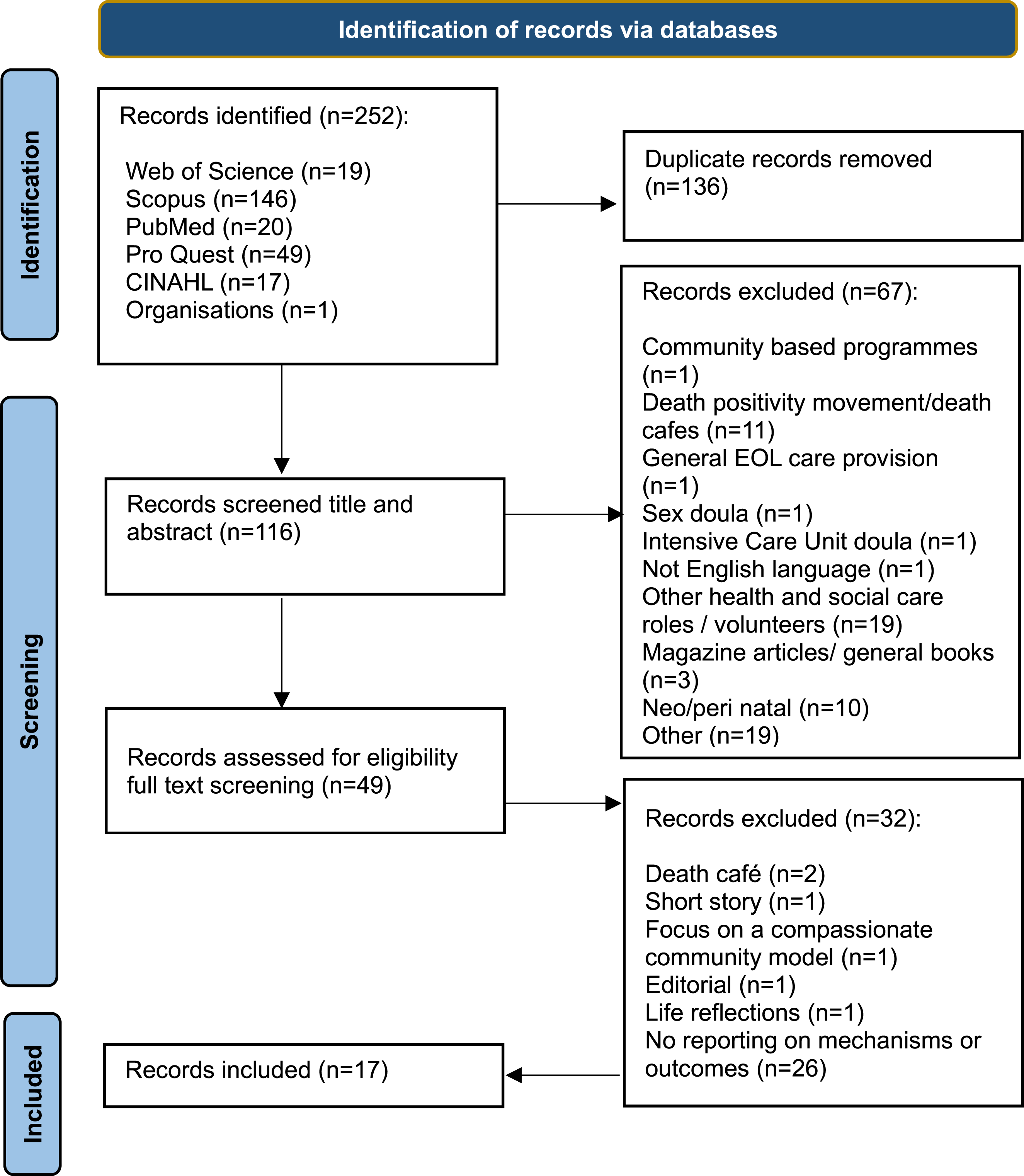
Charting the Data
We extracted the data related to EOLD roles. We used the logic model components: inputs, activities, outputs, and perceived or reported outcomes as coding categories applied across all texts. One author (LP) completed the initial charting, which was then checked for consistency and relevance by a second author (RS). The research team discussed these categories to ensure a shared understanding of what should be included under each component, and the rationale for inclusion.
The data were charted into the following categories (see Table 1 for summary of studies): • Reference (author/year, journal, publication, country) • Study aims/objectives. • Any reported inputs, activities, and outputs related to the role, and associated outcomes for patient, carers, or EOLDs, and potential longer-term impacts. • Context and assumptions under which EOLDs are expected to function. Details of Included Articles
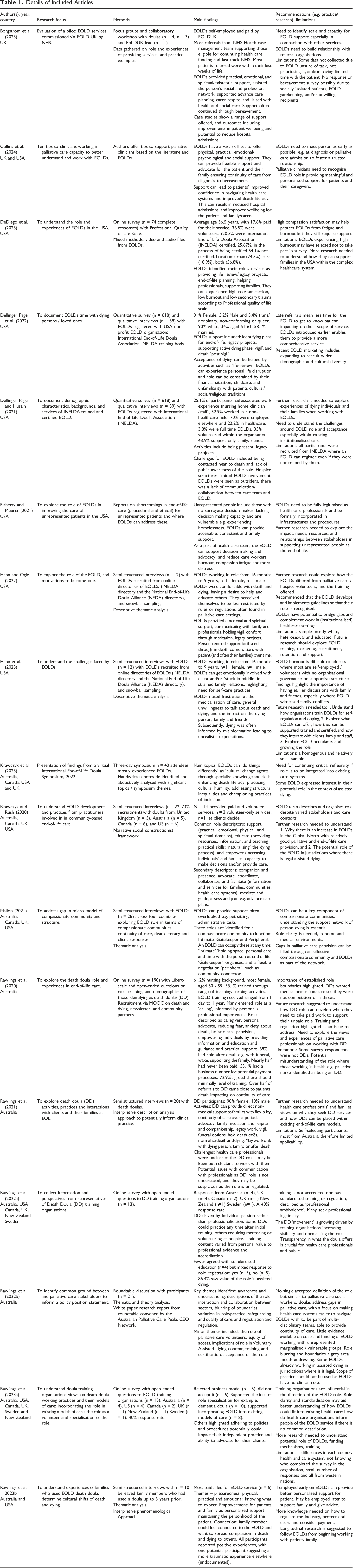
Collating, Summarising, and Reporting the Results
The data aligned with logic model components were collated. These were the inputs and activities required for the EOLD role, and resulting outputs leading to outcomes. Additionally, the model incorporates contextual and influencing factors, including underlying assumptions (Renger and Titcomb, 2002).
Results
A total of 17 articles were identified as suitable for inclusion. The literature was diverse with varying aims and methods. All articles reflected a Global North perspective: six articles were USA-based, three from Australia, with a further seven including data from more than one country, including USA, Australia and/or UK and Canada (see Table 1).
One author (Rawlings) was listed as a first author in six articles. Most articles reported on perspectives of EOLDs, including reporting from events attended by EOLDs (Krawczyk et al., 2023; Rawlings et al., 2022a), and focus groups (Borgstrom et al., 2023). One article reported on perspectives of family members who received EOLD services, using semi-structured interviews (Rawlings et al., 2023b). Three articles reflected upon EOLD practice: Flaherty and Meurer (2021) explored the potential of improving care of unrepresented patients, Collins et al. (2024) reported suggestions for clinicians in palliative and end-of-life care, and Mallon (2021) explored the role within compassionate communities. Four articles reported on two distinct studies focusing on different aspects (Dellinger Page and Husain, 2021; Dellinger Page et al., 2022) and (Hahn et al., 2023; Hahn and Ogle, 2022).
Logic Model Components
The logic model components derived from the literature linking the inputs, or resources and activities, to the anticipated outcomes are detailed in Figure 2 and described in more detail here. Logic Model Informed by the Literature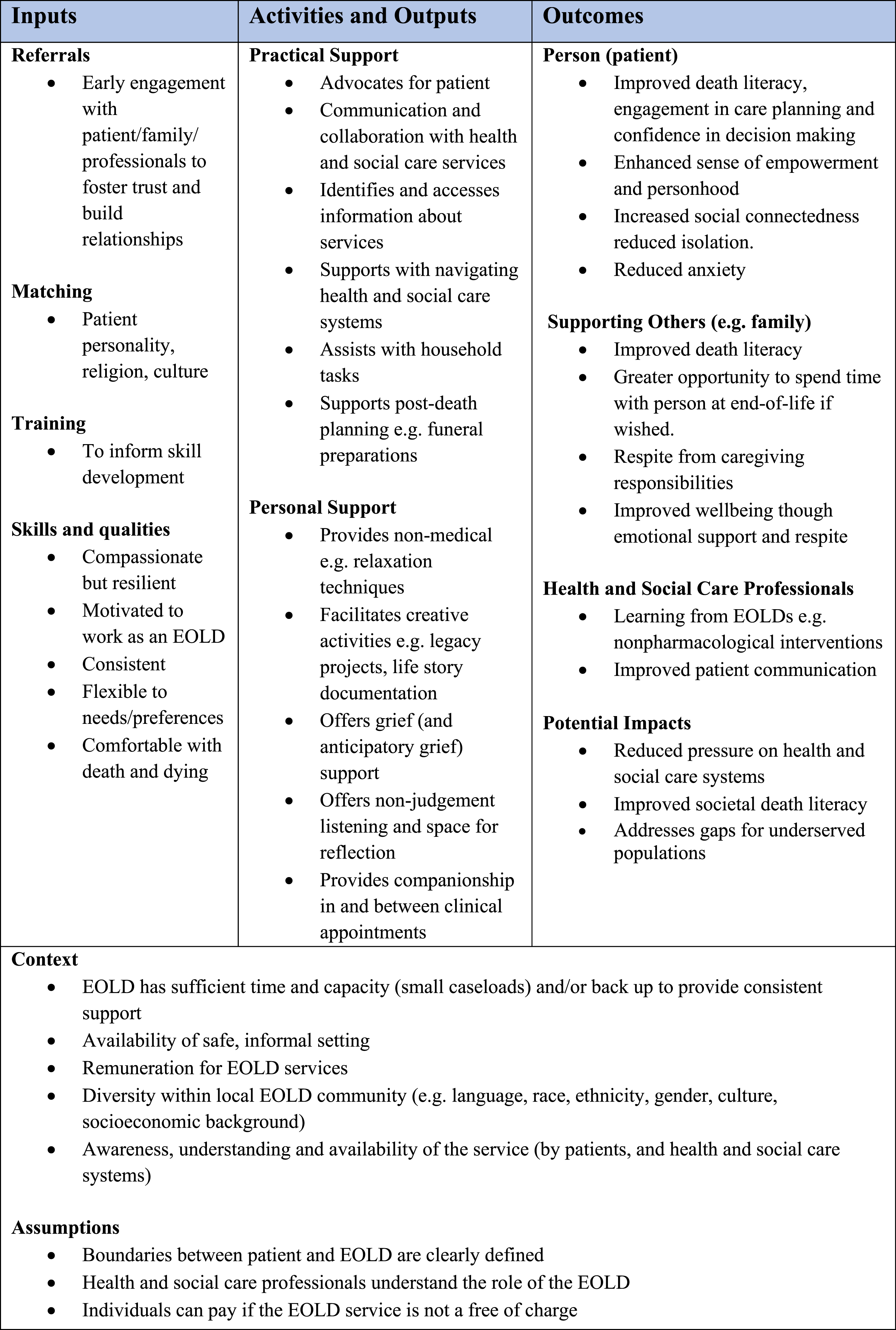
Inputs
Inputs refer to the resources required for EOLDs to support people and are therefore foundational to the subsequent activities, outputs, and outcomes. These were identified as referrals, matching, training, and skills, and qualities needed.
Referrals
Early referrals, close to diagnosis or at the beginning of the patient’s palliative care, were recommended to allow time to foster trust between the EOLD, patient and, if relevant, those close to them (Collins et al., 2024; Rawlings et al., 2023b). Building links and collaborations with potential referral organisations was reported as essential, requiring time, knowledge of, and trust in EOLD support (Borgstrom et al., 2023; Dellinger Page et al., 2022). Rawlings et al. (2020) noted that over half of the EOLDs in their study received referrals in the patient’s last days of life. A late referral, as the person was close to death, limited the relational support that could be provided (Dellinger Page et al., 2022), which could be a single phone call (Krawczyk et al., 2023). Reasons for late referrals were described as varied, with a key element being a stigma around death. As Dellinger Page et al. (2022, p. 14) suggested, a cultural reluctance to talk about death and dying, resulted in people contacting an EOLD only when the patient was close to death: The bias of death that everybody has, it’s not talked about. Families haven’t talked about it. This has not been set up for success for them…But culturally, and it’s not just America, culturally people don’t like to talk about death.
Referrals to EOLDs could be received informally via ‘word of mouth’, for example, from individuals who had a previous positive experience of EOLD support; referrals were also reported to be from hospital palliative care teams, funeral directors, hospice care, and therapists (DeDiego et al., 2023). However, before deciding whether to employ an EOLD, families often enquired about the service from health professionals (Rawlings et al., 2020). EOLDs were commissioned by the NHS (UK) in one pilot study, with most patients referred from Health Case Management Teams who can provide support for people during the last weeks of life (Borgstrom et al., 2023).
Matching
Collins et al. (2024) noted that EOLDs should ideally be matched with the patient and, if relevant, their family to build rapport, understand patient preferences and cultural values, and foster trust. It was also observed by Hahn et al. (2023, p. 8) that if there was no connection with the patient/family, the EOLD could easily be dismissed: “Not everyone will like you, we have to realize that”. Flaherty and Meurer (2021) emphasised the need for EOLDs to recognise “signifiers” of patient preferences, such as tattoos or jewellery, especially in the context of offering tailored support for more marginalised individuals, such as those experiencing homelessness. The need for ‘cultural alignment’ to match the patient appropriately with the EOLD was recognised in a roundtable discussion of EOLD stakeholders (Rawlings et al., 2022b). Furthermore, matching EOLDs’ specific skills with patient populations, such as people living with dementia, was perceived to enhance the fit and effectiveness of care (Rawlings et al., 2023a; Borgstrom et al., 2023). However, Borgstrom et al. (2023) noted that matching was largely pragmatic, based on the availability and location of the EOLD.
Skills and Qualities
EOLDs require a non-medical skillset to provide physical, practical, psychological/emotional, and social support. Commonly reported skills were practising emotional intelligence, active listening, compassionate communication, and being non-judgmental (Borgstrom et al., 2023; Collins et al., 2024). These skills developed over time, with knowledge and experience that were not easily quantified. Crucially, EOLDs required the flexibility to be responsive to people’s needs (Borgstrom et al., 2023; Dellinger Page et al., 2022; Rawlings et al., 2020), having a collaborative mindset (Collins et al., 2024) and being aware of additional support services that could benefit the patient (Krawczyk et al., 2023).
Some EOLDs regarded their skills in delivering person-centred support as presenting learning opportunities for health professionals (Hahn et al., 2023). For example, being skilled in practicing ‘cultural humility’ and reflecting any power imbalances and bias inherent in medical practices (Krawczyk et al., 2023). However, with many EOLDs reported as having a professional background in healthcare, predominantly nursing, having medical skills could potentially blur the lines of delivering non-clinical advice and support (Rawlings et al., 2023b).
Many EOLDs were described as personally motivated to be an EOLD, wanting to help and educate the public and professionals about death and dying, and perceiving the role as a calling: To tell you the truth, I think to be a doula is kind of like not just a job, but it’s your life because everyone has people who have died and they all when they find out you’re a doula, they all want to talk about it. It’s kind of a sacred being a sacred…sacred keeper of, of end of-life. (Hahn and Ogle, 2022, p. 9)
Due to the personal investment, EOLDs described themselves as having to be prepared emotionally, physically, and spiritually for the unpredictability of death, as well as able to understand their own, as well as their clients’ limits (Hahn et al., 2023).
Training
Training for the EOLD role was diverse, involving facilitators from a range of backgrounds, from palliative care-trained nurses to those with relevant personal experience. This included self-directed learning and skill development supported by organisations and other EOLDs (Borgstrom et al., 2023; Rawlings et al., 2020). As Rawlings et al. (2020) noted, training could last two days or longer and consist of more than one training course. In one study 72% of EOLDs surveyed agreed there should be a minimal level of training (Rawlings et al., 2020). Despite such variation in mode and method of training, it was widely considered that training ensured that EOLDs did not blur role boundaries in adhering to providing non-medical support: Therefore, what we say to doulas is if you are a nurse, and you’re going to be practicing as a nurse, and you’re going to also be doula-ing, then you need to be uber clear with your clients that you’re, you know, talking to them about your services, that you have nursing services and you have doula services and that they need to be billed separately. (Rawlings et al., 2022b, p. 15)
The benefits and limitations of formalising the role through training and licensing were noted as subject to continuing discussion. For example, certified training, as well as accreditation and regulatory oversight, was regarded by some EOLDs as being potentially restrictive to practice: Well, if we’re going to be reimbursed by insurance then there’s going to start being regulation and licensing and all that stuff is going to begin to limit us just as it limited hospice. And we really don’t want that. We as a group are pushing back real hard on that. (Dellinger Page et al., 2022, p. 519)
Rawlings et al. (2022a, p. 8) argued that EOLD training organisations are a ‘driving force’ in the industry; however, they observed inconsistencies across training and courses which led to some concern amongst EOLDs: I am concerned about the cults of personality that arise from many Australian training courses that are run by one person. This is further enhanced by closed FB (Facebook) groups, the blurring of lines between what is offered as doula work per se, and what is considered essential by individual trainers.
Activities
Activities were identified as the specific actions conducted by EOLDs, which subsequently generated outputs. These were typically influenced by the patient's individual circumstances. Support could be delivered online, over the phone or in person. The observation of there being no typical day was reflected on by Hahn and Ogle (2022, p. 10): It really depends on where the person is in their own journey. Right - and their own timeline. So, they could be calling me 7 months before. They could be calling me a week before a month before, and that person is not going to be the same person that they were 7 months ago. So many factors are about their physical being, their mental being, and spiritual being.
Nonetheless, some common themes were evident, encompassing practical and personal support.
Practical Support
EOLDs were frequently described as advocates for patients and, in some instances, their families. This involved attentively listening to their concerns, acting upon their wishes, and encouraging them to ask questions that were important to their care and decision-making: I’d say, for me, emotional support was huge. And also, legal knowledge. Legal support, and I suppose it comes under emotional support, just knowing, coaching me in how to speak to the medical staff so that I didn’t come across as hysterical. I’d ring them up and burst into tears, saying, “Sorry.” But then I’d collect myself, and say my little speech, and then they’d understand what I was talking about, which was really good, because I’d been coached’. (Family member in Rawlings et al., 2023b, p. 7)
Flaherty and Meurer (2021) reported that an EOLD could advocate for patients with no supporting family/friends, identifying and communicating their preferences to health professionals. Moreover, in practicing cultural humility, that is, engaging with patients in a reflective way to understand the cultural context, values and concerns, EOLDs could facilitate improved communication between healthcare providers and patients (Borgstrom et al., 2023; Collins et al., 2024; Rawlings et al., 2020).
Activities also included co-ordinating and assisting with practical tasks: shopping, laundry, and helping with pets, resulting in precious time not spent on chores (Borgstrom et al., 2023; DeDiego et al., 2023; Dellinger Page et al., 2022; Rawlings et al., 2020). These activities could continue even after the person had died, where the EOLD could remain with the family (Borgstrom et al., 2023; DeDiego et al., 2023; Rawlings et al., 2023b) and provide practical support for example, assisting in organising or conducting a funeral (Rawlings et al., 2021), and helping to navigate often complex systems encountered at the end-of-life (Rawlings et al., 2022a).
The literature revealed that EOLDs were able to source and share relevant information with the patient such as supporting organisations available in the area. Additionally, they could attend medical appointments with the patient to provide an avenue for reflection and recall (Collins et al., 2024; Rawlings et al., 2020). As one doula noted: So, one of the things I really liked about end-of-life doula work is going to medical appointments with people. I'm quite happy to translate medical speak into plain English. I'm quite happy to translate a client's questions and fears and wishes to a medical practitioner… I think advocacy is really, really important. (Rawlings et al., 2020, p. 578)
Without constraints of time, EOLDs were identified as well positioned to focus entirely on the patient without distraction (Borgstrom et al., 2023; Collins et al., 2024; Rawlings et al., 2020): Health service providers are in and out within a set time limit. Basically, nurses are in for half an hour to an hour a day, changing pic lines, checking vitals, giving medication, etc. PSWs (Personal Support Workers) are in for maybe half an hour to an hour per day, washing or bathing, getting them dressed and up into a chair …I do everything else. (EOLD Respondent in Rawlings et al., 2020, p. 16) So, they've got someone that's bringing that continuity, because every other team including their pall team, drop off, the medical team. So, I think you know that to me is a crucial point. (EOLD Respondent in Rawlings et al., 2022b, p. 14)
However, whilst maintaining a closeness to the patient, Collins et al. (2024) referred to EOLDs providing an ‘outside perspective’, summed up by an EOLD in Dellinger Page et al. (2022, p. 17): It takes an outside perspective sometimes to offer these points of view and these tools, which everybody kind of knows them, but when you’re in the midst of dealing with the chaos and confusion, the dying process, because it often is on so many different levels.
Personal Support
In supporting the spiritual and emotional needs of patients and their family/unpaid carers, the EOLD could help them understand their illness and navigate any anticipatory grief (Collins et al., 2024). Active listening was central to the role, facilitating continuous dialogue and reflection with the patient and/or carers to adapt to the patient’s changing needs and/or preferences over time. This could involve encouraging conversations about death as well as discussions on advance care planning (Borgstrom et al., 2023; Collins et al., 2024; Krawczyk et al., 2023). Providing a platform to address concerns such as fears, anxieties, and end-of-life goals, activities with the patient could include art legacy projects, life review work and mindfulness-based approaches (Collins et al., 2024; Hahn and Ogle., 2022).
Towards the end-of-life, the EOLD was noted as being vigilant of small changes in the patient, and attentive to emotional changes of those supporting them (Dellinger Page et al., 2022). Providing information and/or options (Rawlings et al., 2022b), they could explain the signs of dying, supporting the family member with knowledge of what to expect – the physical processes and required tasks to enable a ‘good death’ (Rawlings et al., 2023b). The family might not know what to ask; therefore, the EOLD could inform them of what was possible, for example, in supporting a death at home, or what happened after death, in the context of laws and jurisdictions (Rawlings et al., 2023b).
It was stressed throughout the literature that EOLDs would attend to the whole person and not their illness. This could be through activities focusing on their past life, such as legacy work but also significantly, a focus on their living in the present to maintain their personhood: The individuals who are dying sometimes just see the end date. I want them to know that even with this diagnosis, they still have a future. (Hahn and Ogle, 2022, p. 12)
Outcomes
Outcomes represent the intended goals of EOLDs, as experienced by, or reported for patients, carers, and EOLDs.
Outcomes for the Patient
Key aims of EOLDs across the literature were to improve patients’ end-of-life care, support health and social care professionals and any individuals supporting the patient to facilitate a ‘good death’ (Collins et al., 2024). In receiving consistent person-centred or relational-centred support, the reported outcomes for patients and carers included feeling empowered due to experiencing agency and control (Collins et al., 2024; Dellinger Page et al., 2022; Rawlings et al., 2023b). For patients otherwise unsupported with no social networks, family or friends, an EOLD could improve their wellbeing by fostering social connectedness, potentially leading to improved quality of life and ensuring that they had the choice not to die alone (Collins et al., 2024; Rawlings et al., 2023b). Additional outcomes included increased self-worth and confidence, and a better understanding of their condition and how to manage it (Borgstrom et al., 2023), thus reducing anxiety, fatigue, and depression, and lessening any emotional burden associated with end-of-life decision making (Collins et al., 2024).
Outcomes for Family/Supporting Others
It was suggested that caregiver strain could be alleviated through the emotional and practical support provided by EOLDs (Collins et al., 2024). An unpaid carer, such as a family member, was likely to experience meaningful respite with peace of mind, knowing that the person they cared for was being looked after by the EOLD (Borgstrom et al., 2023; Rawlings et al., 2023b). They could also feel better prepared and in control, knowing what to expect over time, such as physical deterioration, and be aware of the pragmatic tasks required to support the patient nearing death (Rawlings et al., 2023b). Furthermore, they could feel more confident in supporting decision making alongside the patient when assisted by the EOLD who was equipped with the knowledge and resources to assist in navigating healthcare systems (Collins et al., 2024). Resulting outcomes were described as feeling heard, empowered, involved, and less anxious following EOLD support (Borgstrom et al., 2023).
In Rawlings et al. (2023b, p. 7) bereaved family members reported that the EOLD had helped them to communicate their preferences: Prepared. I think I’ve said it. Yeah, prepared is. . . I mean, I do really appreciate the fact that she coached me in how to speak to specialists, doctors, and even carers. I did have, when he died, I really wanted to wash his body and wrap him. I didn't want. They kept saying, “Have you rung the funeral place yet?” And (DD) had said, “Just tell them you’ll do it in your own time. Your own time. Your own time.”
Outcomes for EOLDs
EOLDs appeared to be motivated to pursue the role, with their identity closely tied to it as a ‘way of being’ (Borgstrom et al., 2023). They reported feeling rewarded in supporting a positive death experience (DeDiego et al., 2023; Dellinger Page et al., 2022). However, where other services were not seen to understand their role fully, EOLDs could feel disrespected (Borgstrom et al., 2023; Hahn and Ogle, 2022). Additionally, they might not always recognise the emotional toil of their work, or when they have ‘done a good job’ (Borgstrom et al., 2023, p. 23). Secondary losses were also described where EOLDs worked closely with patients, family, and colleagues, as one EOLD described in Hahn et al. (2023, p. 7): ‘It’s hard to step into it with your whole heart, knowing that you will just continue to say goodbye to people’. This highlighted the importance of EOLDs practicing self-care and implementing strategies to manage the work’s emotional impact (Borgstrom et al., 2023).
Impacts (Longer Term Outcomes)
Wider impacts stemming from outcomes were suggested in the literature. Where the EOLD held a series of sensitive conversations with the patient about what mattered to them, they were likely to document advance care plans stating preferred place of death, potentially avoiding unwanted overtreatment and/or hospital admissions and potentially reducing healthcare expenditures. Additionally, with the EOLD focusing on the patient’s psychosocial needs, health providers could prioritise the patient’s medical care (Borgstrom et al., 2023; Collins et al., 2024; Flaherty and Meurer, 2021).
Many EOLDs were reported as challenging a dominant medicalised discourse of ‘fixing and curing’ (Hahn et al., 2023; Krawczyk et al., 2023) through community discussion via death cafes and other community events (Mallon, 2021; Rawlings et al., 2021). Additionally, individuals with positive experiences of an EOLD were likely to facilitate discussions that mitigated misinformation and unrealistic expectations about what happens at the end-of-life (Rawlings et al., 2023b). Rawlings et al. (2023b) refer to family members becoming more death literate following their experiences with EOLDs, and in sharing with others, potentially contributing to the ‘reshaping the death system’.
Context and Framing Assumptions
The context, wider environment, and underlying assumptions that enable EOLDs to successfully operate within the varying nodes of the end-of-life ecosystem are key elements of the logic model. Key components were agreement on remuneration, role clarity, EOLD capacity, standardisation and diversity of role.
Remuneration
Determining if, and how EOLD services were paid for was an area of contestation. Some received financial payment as agreed prior to starting and as a set rate (Collins et al., 2024). However, in a survey of EOLDs in Australia, 49.4% had never been paid, with others reporting in-kind payments (Rawlings et al., 2019). Elsewhere, EOLDs spoke of healthcare as a socio-economic issue, suggesting that the service should be provided free of charge or on a sliding scale (Krawczyk et al., 2023). Rawlings et al. (2023a, p. 5) noted that some EOLDs they interviewed felt uncomfortable charging for their services: We’re talking about people that don’t have a lot of money in a lot of cases and I have a sliding scale. It’s not about money. It is about people.
Where remuneration was perceived to reflect service professionality, there remained uncertainty about how much to charge, particularly when the EOLD was recruited close to a death (Dellinger Page et al., 2022). Rawlings et al. (2022a) found that six of thirteen EOLD organisations perceived volunteering as devaluing the role which should be viewed as a trained profession, whilst the remainder saw this as personal choice. Within the USA, Dellinger Page et al. (2022) explained how health insurance companies only reimburse services provided by qualified medical providers (training, expertise, and certification) therefore excluding EOLDs.
Certification/Standardisation
The issue of formal licensing and oversight was a concern described as potentially impacting role delivery (Dellinger Page et al., 2022). Flaherty and Meurer (2021) noted that if EOLDs were recognised as legitimate healthcare professionals and incorporated into USA procedures and structures this would demonstrate their competency. Rawlings et al. (2021, p. 582) referred to some EOLDs conflicted about role regulation, noting that remaining uncertified could contribute to a lack of trust: Double-edged sword, isn’t it? in some ways to have like code of conduct, professional membership to something, that professional support, yes. On the other hand, if it becomes to rule and restrictive… I can see the benefits of it but I can also see the downfall of it in some ways.
Rawlings et al. (2022a) explored the views of thirteen EOLD training organisations internationally and found that the majority did not support a standardised business model. Eight organisations supported integrating the EOLD role into existing care models, while others cautioned that embedding it within organisational policies and structures might limit their capacity to advocate for patients. Opinions on regulating the role were evenly divided.
Dellinger Page et al. (2022) noted that the apparent ambiguity and non-universal structure of the EOLD role was a weakness, but also a strength, offering flexibility and diversity. Attendees of an EOLD symposium in Krawczyk et al. (2023) discussed this polarisation of views, with some seeing role credibility and visibility as attainable through certification and standardisation, while others believed this could lead to poor training and unaccredited certification. Some form of regulation was perceived to be inevitable if EOLD services became in demand, and necessary in supporting patients who are vulnerable and open to exploitation (Rawlings et al., 2020).
The challenges posed by unregulated EOLDs without standardised training were reflected in a roundtable discussion in Australia (Rawlings et al., 2022b, p. 16): But I feel like we’re amongst friends. I think we’ve got to pose the challenge, who’s not here? You know, where are the Mavericks, who will stand out and actually do their own thing? Because in many ways they’re the ones who will, maybe not tarnish, but taint the reputation of doulas, if they stay out of the tent. And so how do we bring them into the room? I think that’s probably an ongoing conversation.
Role Clarity
Many EOLDs perceived their role not to be fully understood by the public and professionals, exacerbated by the lack of standardisation and a common role descriptor (Rawlings et al., 2023a). Stakeholders involved in palliative care similarly expressed the need to better understand the role within the sector (Rawlings et al., 2022b). In some cases, EOLDs referred to medical teams viewing them as ‘outsiders’, leading to a lack of communication and collaboration between themselves and healthcare professionals (Dellinger Page et al., 2022), a sentiment reported elsewhere: I spoke to one GP and she was quite disgruntled about what I’m doing. She said, ‘Well, I think what you're doing is all a load of crap “Palliative care manages all that. They don't need you guys”. (Rawlings et al., 2021, p. 579)
Conveying the EOLD role and remit to patients and professionals was essential, in that they were to support and not replace healthcare professionals (Collins et al., 2024).
Some EOLDs expressed the need for health and social care professionals to have a better understanding, and acceptance of the EOLD role: You guys deliver specialist care, and I can't do my job without you. I just want to walk alongside you and collaborate with you so that together we can actually make a difference to the people that we're there to serve (Rawlings et al., 2022b, p. 14)
Capacity
EOLDs were reported to have more flexibility to provide tailored and consistent support due to fewer organisational rules and regulations than health and social care professionals. However, they too relied on having adequate capacity and resources (Borgstrom et al., 2023), for example in supporting between one to three patients at one time (Hahn and Ogle, 2022; Rawlings et al., 2021). In a study by Rawlings et al. (2019) while over half of EOLDs reported having backup support in case they were unavailable, whilst 67% did not collaborate with other EOLDs.
Diversity of EOLDs
A key benefit of EOLDs was their potential to support minoritised groups who may otherwise be unrepresented, enabling them to have a more positive end-of-life experience. Ideally, the EOLD demographic should reflect the socially and culturally diverse population they aspire to support (Collins et al., 2024). However, EOLDs were described as majority female (91.4%) (Dellinger Page et al., 2022), mostly white, with an average age of 50 years (Rawlings et al., 2019; Krawczyk et al., 2023). Most were college educated, and potentially better positioned to take on the voluntary and part-time EOLD role: There’s a lot of discussion about (how) diversity and inclusion is at the heart of EOLD organisations and practice. Whilst we strive for this in practice, the reality is that the vast majority of our members and practising EOLDs are white, middle-class women. (Krawczyk and Rush, 2020, p. 8)
Dellinger Page et al. (2022) suggested marketing to appeal for EOLDs from more diverse cultural and demographic backgrounds and bring EOLD services to underserved populations, although how this might be achieved was not stated explicitly.
Discussion
The primary objective of this review was to identify the mechanisms through which EOLDs function and the associated outcomes for patients, carers, and EOLDs to inform a preliminary logic model framework. This has illustrated how EOLDs could benefit patients and carers, and fit alongside health and social care providers, helping to meet current challenges in palliative and end-of-life care support. With services facing growing pressure the emotional, spiritual, and informational support for patients and their families is often under-addressed in healthcare systems. This can be due to systemic pressures such as staffing levels, support and time constraints leading to work-related stress (Cedar and Walker, 2020). EOLDs can provide continuous support which may extend to the patient’s network, into bereavement. They do not replace medical or nursing expertise but add a “missing layer, acting as an expert family member, a mentor or facilitator and a source of information and guidance” (Elliott, 2011, p. 30). Flexibility, advocacy, being present and taking time with the patient are assets identified as important by service providers and patients including those marginalised nearing the end-of-life (Petruik et al., 2025). In supporting patients with no advocate, they could be part of an equity-focused health initiative in reducing inequalities and improving outcomes.
End-of-life care has been suggested as being too medicalised (Sallnow et al., 2022). EOLDs may, through their practice, challenge death system norms, such as where someone can die, be cared for, and post-death arrangements. The role can potentially contribute to improved death literacy at an individual and societal level ‘the knowledge and skills that people need, to make it possible to gain access to, understand, and make informed choices about end-of-life and death care options’ (Leonard et al., 2020, p. 1). Moreover, EOLDs can attend to emotional, physical, spiritual, and psychological distress associated with a loss of dignity, social isolation, and loss of control, agency, and purpose identified as common reasons to request assisted dying (Royal College of Nursing, 2016).
Nonetheless, contexts and assumptions affecting the role development, recognition, and its wider implementation include contested views as to whether EOLDs should be integrated within health and social care systems, and issues of standardisation, certification, as well as remuneration. These are intersecting tensions that the EOLD community acknowledges themselves. This issue lends itself to further discussion of how the role could complement existing services, and where it could be situated, between social work practice and volunteer companionship for example.
This review highlights some important gaps in the research and practice, summarised in Box 1. Clearly, more research is needed to understand the ‘scale and capacity’ of EOLDs to support other services, and their training and support needs (Borgstrom et al., 2023, p. 24). Healthcare professional perspectives are lacking despite the inferences made in the literature of lessening their burden and helping them to focus on their tasks (Rawlings et al. 2019), and little is known about the views and experiences (good or bad) of those who have been supported by an EOLD (Rawlings et al. 2019; Rawlings et al., 2023b). Furthermore, despite claims of patient-centred support, any differences in support needed and outcomes across settings (such as a home, hospice or hospital) and urban and more rural areas are lacking, and peer-reviewed studies in Global South settings remains notably scarce. It would be useful to explore differences in role establishment and activities in the context of the legal and welfare regimes, for example, with assisted dying legal in some jurisdictions.
• Are matching processes considered across EOLD practices and if so, how are these achieved? • To what extent, and how, are EOLDs recruited to reflect diversity and bring specialised expertise (e.g., in dementia or learning disability)? • What are the perspectives and experiences of health and social care professionals who have worked alongside an EOLD? • How can equitable access to EOLDs be ensured, so that support is not only available and accessible to individuals who are able to pay? • Is there a desire for EOLD support in the UK, and if so, by whom? • What evidence supports the suggestion that EOLDs can influence the culture and discourse surrounding death, dying, and bereavement, and improve people’s levels of death literacy? • Can the EOLD role demonstrate cost-effectiveness through measurable improvements in the quality of end-of-life care and other outcomes valued by patients, carers, and health and social care professionals? • What differences exist in EOLD practices between countries and health systems globally, and how might these inform learning opportunities for wider recognition and integration of EOLDs into health systems?Box 1. Suggestions for further research
This logic model can serve as a useful focal point for further discussion. However, informed by evidence of only 17 articles and with only high-income countries represented, further framework development will be an iterative and cumulative process relying on knowledge from multiple stakeholders (Funnell and Rogers, 2011). Therefore, the suggested next step will be to refine the model through consultation and collaboration with stakeholders, including health and social care professionals, EOLDs, and people who have had experience with an EOLD.
Limitations
There are known limitations of the scoping review process. The literature, whilst peer reviewed, was not subject to quality appraisal, which limits the robustness of the findings. Six of the studies were written by the same author, and this offers a limited evidence base. The review included English-language publications, and relevant studies published in other languages are missing, which could add to the work in this emerging area. Only high-income countries were identified, possibly due to the English language limitations, and therefore this review reflects only the cultural, social norms, and health system of countries with Western, more medicalised models of care. Future research could expand the search strategy to include traditional healers or grief workers.
This is a fast-growing area of interest, with publications relating to EOLD research increasing (Bochanova and Mikhaylova, 2025). Whilst we conducted forward and backwards citation searching to be as comprehensive as possible, it is possible that we have missed some sources that may have been relevant. Additionally, the review relied on the reviewer subjectivity in identifying articles with data relevant to the criteria of the logic model. This may have introduced bias into interpretation. However, we attempted to mitigate this with a second reviewer.
Logic models may exclude the myriads of complex factors involved in interventions (Gov.uk, 2018) subject to changes in assumptions about how EOLDs might work, evolving population needs and preferences, and health and social care contexts. However, this is the first logic model presented of EOLDs to assist in further conversations with all stakeholders to explore how the role could be included within policy and practice settings. It is likely that the EOLD role will generate continued interest, especially in relation to changing health and social care contexts for example, their potential to support people in jurisdictions where assisted dying is legal (Parliament, 2024).
Conclusions
Whilst the EOLD role continues to evolve, it could present an important response to the changing norms and challenges associated with end-of-life care. This scoping review highlights the significant potential of EOLDs by systematically identifying, synthesising, and mapping their activities, outputs, and range of outcomes for patients, supporting others (family/ unpaid carers), and EOLDs themselves. These findings provide a foundation for developing a framework of core components and contextual considerations essential for considering effective integration of EOLDs into end-of-life and palliative care.
Supplemental Material
Supplemental Material - Mapping the Role of the End-Of-Life Doula: A Scoping Review and Logic Model Framing
Supplemental Material for Mapping the Role of the End-Of-Life Doula: A Scoping Review and Logic Model Framing by Louise Prendergast, Roiyah Saltus, Jane Depledge in OMEGA - Journal of Death and Dying
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
