Abstract
• There is promising evidence that psychedelic-assisted psychotherapy may be a powerful new treatment approach for mortality-related distress • Less is known about the possible benefits of psychedelics for people experiencing grief
• This scoping review demonstrates that there is not a strong evidence base at this time to guide clinical recommendations for applying psychedelics to the problem of grief following loss from advanced illness at this time. • Across the few empirical studies identified, there were generally positive outcomes reported in terms of grief symptom reduction, and few reported adverse or negative outcomes
• Further empirical research with clear theoretical conceptualizations of grief and anticipated mechanisms of action is needed to informal clinical recommendationsKey statements
What is already known about the topic?
What this Paper adds
Implications for practice, theory or policy
Introduction
Public interest in the field of psychedelics is rapidly growing. Annual publications on psychedelics have increased by 1300% over the past two decades (Lewis et al., 2023), with clinical trials exploring the effectiveness of psychedelic-assisted psychotherapy to treat a range of mental health conditions (Horton et al., 2021). Within palliative care, there is evidence that psychedelic-assisted psychotherapy may be a powerful new treatment approach for mortality-related distress (e.g., demoralization, hopelessness, or existential distress) (Agin-Liebes et al., 2020; Beaussant et al., 2021; Ross, 2018; Yaden et al., 2022), for which there are few evidence-based recommendations or targeted interventions (Vehling & Kissane, 2018). Despite these promising findings, most psychedelics remain controlled substances not approved for clinical use. Further research is needed to inform policy and clinical use (Beaussant et al., 2020). While most work in the field of psychedelic-assisted psychotherapy in end-of-life care focuses on those experiencing advanced illness, there have been calls to explore the impact of psychedelic-assisted psychotherapy on family caregiver grief, both while they care for the dying person (Gold et al., 2023) and after the person has died (Beaussant et al., 2021; Rosa et al., 2022).
Grief
Humans have long attended to the deaths of significant others, with every culture and religion providing some guidance on how to come to terms with the death of meaningful individuals (Klass & Goss, 1999). The experience of grief is influenced by culture (Klass, 1999). Rather than searching for one universal conceptualization of grief, as biomedical clinicians working in a multicultural context, we acknowledge there are many griefs, and we seek to understand Western grief scholarship while recognizing other social constructions of grief.
From a Western perspective, grief is commonly described as the natural, personal reaction to loss, especially after the death of a person of significance (Johannsen et al., 2019). Unique to each person, grief responses do not follow predefined stages (Szuhany et al., 2021). Grief often includes distressing and painful emotions (e.g., anger, yearning), thoughts focused on disbelief or confusion, changes to behavioural patterns, and physical sensations (e.g., dizziness, headaches) (CAMH, 2024). Over time, most individuals adjust to the loss and find ways to cope with their grief (Jordan & Litz, 2014; Prigerson et al., 2009; Szuhany et al., 2021). However, up to 10% of bereaved individuals may experience prolonged and profound loss-related distress (Maciejewski et al., 2016).
A systematic review examining psychological interventions for grief in adults found that some individual interventions for people with high baseline symptoms showed promising results in relieving depressive and post traumatic distress symptoms (Johannsen et al., 2019). However, ‘gold standard’ grief interventions show little evidence of improving anxiety symptoms or quality of life (Johannsen et al., 2019). With psychedelic-assisted psychotherapy demonstrating promising results for treating a range of mental health conditions, some clinicians and scholars are examining what psychedelics can do for those experiencing grief.
Due to uncertainty about the evidence informing the burgeoning field of grief and psychedelics, we conducted a scoping review in order to explore the extent of the literature, summarize the evidence, and inform future research (Tricco et al., 2016). Therefore, this scoping review examines what is known about the application of psychedelics for people experiencing grief after a death due to advanced illness (e.g., metastatic cancer). Given the history of the study of both grief and psychedelics outside of medical research, by “what is known” we are referring to scholarship on this topic across a wide range of disciplines (e.g., medicine, psychology, social sciences).
Method: Scoping Review
This scoping review followed Arskey and O’Malley’s methodological framework (Arksey & O'Malley, 2005), with additional suggestions made by Levac et al. (2010). Reporting of this scoping review follows the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) to promote transparency and consistency.
Stage 1: Identifying the Research Question
The primary research question this scoping review sought to answer is: what is “known'' about using psychedelics to attend to grief following death due to advanced illness? Secondary questions focused on understanding the proposed mechanisms of action that could explain why psychedelics might be helpful for supporting people through both “normal” grief as well as the challenges that come with prolonged grief. Secondary questions included: which psychedelics in combination with which types of support have been tried or promoted?; with which patients?; with which intended or achieved outcomes?; and with what proposed mechanisms of action?
Stage 2: Identifying the Relevant Studies
Prior to developing a protocol, our team searched the literature broadly to explore the intersection of grief and psychedelics. Next, in collaboration with a research librarian/information specialist (MA) at the University Health Network, we developed a protocol (this was not registered but can be accessed upon request). A search strategy was iteratively developed. The strategy was trialed in Ovid Medline, with two researchers reviewing the first 200 records to determine fit with the purpose of this review. Searches were then conducted in the databases Ovid Medline, Embase and PsycINFO, ProQuest Sociological Abstracts, Web of Science, ClinicalTrials.gov, and International Clinical Trials Registry Platform. The initial results were downloaded in April 2023, with updated searches run in December 2023. Appropriate subject headings and keywords for psychedelics and grief or loss in the context of advanced illness were used for each database. The limited number of results led to a mingled concept structure of psychedelics AND grief OR caregiver OR surviving loved ones. Embase was the exception to this concept structure given initial results were predominantly irrelevant. Consequently, the structure used in Embase was psychedelics AND grief AND caregiver OR surviving loved ones, which led to more relevant results. No limits or filters were applied. For complete strategies, see Supplemental Data.
Stage 3: Study Selection
Records were eligible if they met the following criteria: (1) focused on individuals over age 18; (2) relevant to grief experienced following death from advanced illness; and (3) discussed the use of psychedelics to address grief, including prolonged and/or normative grief. Records were excluded if they: (1) focused exclusively on grief from traumatic loss (e.g., suicide, miscarriage); or (2) focused on interventions aimed at grieving healthcare clinicians.
EndNote 20 was used for reference management, de-duplication (Bramer et al., 2016), and removal of non-English titles and abstracts. Covidence (Covidence Systematic Review Software, 2023) was used for study selection. At the title and abstract screen, two reviewers independently screened all records using the eligibility criteria. To improve consistency, the team met to review inclusion criteria and pilot screen 10 titles and abstracts, discussing the screening process, criteria, and ambiguities. The resulting agreement at the title and abstract screen was 98.3%. Discrepancies were resolved by consensus. At the full-text screen, two reviewers independently screened all articles based on the eligibility criteria. To improve consistency, the team pilot screened two full-texts. Reasons for exclusion included wrong patient population, no use of psychedelics, and insufficient conceptualization of grief. The resulting agreement at the full-text screen was 85.5%. Discrepancies were resolved by consensus. Results of the study selection are presented in the PRISMA flow diagram (Figure 1), which follows standard guidelines and terminology in that a “record” refers to a bibliographic entry (e.g., title and/or abstract) from a database search, while a “report” is the full-text document. PRISMA flow diagram. https://www.prisma-statement.org/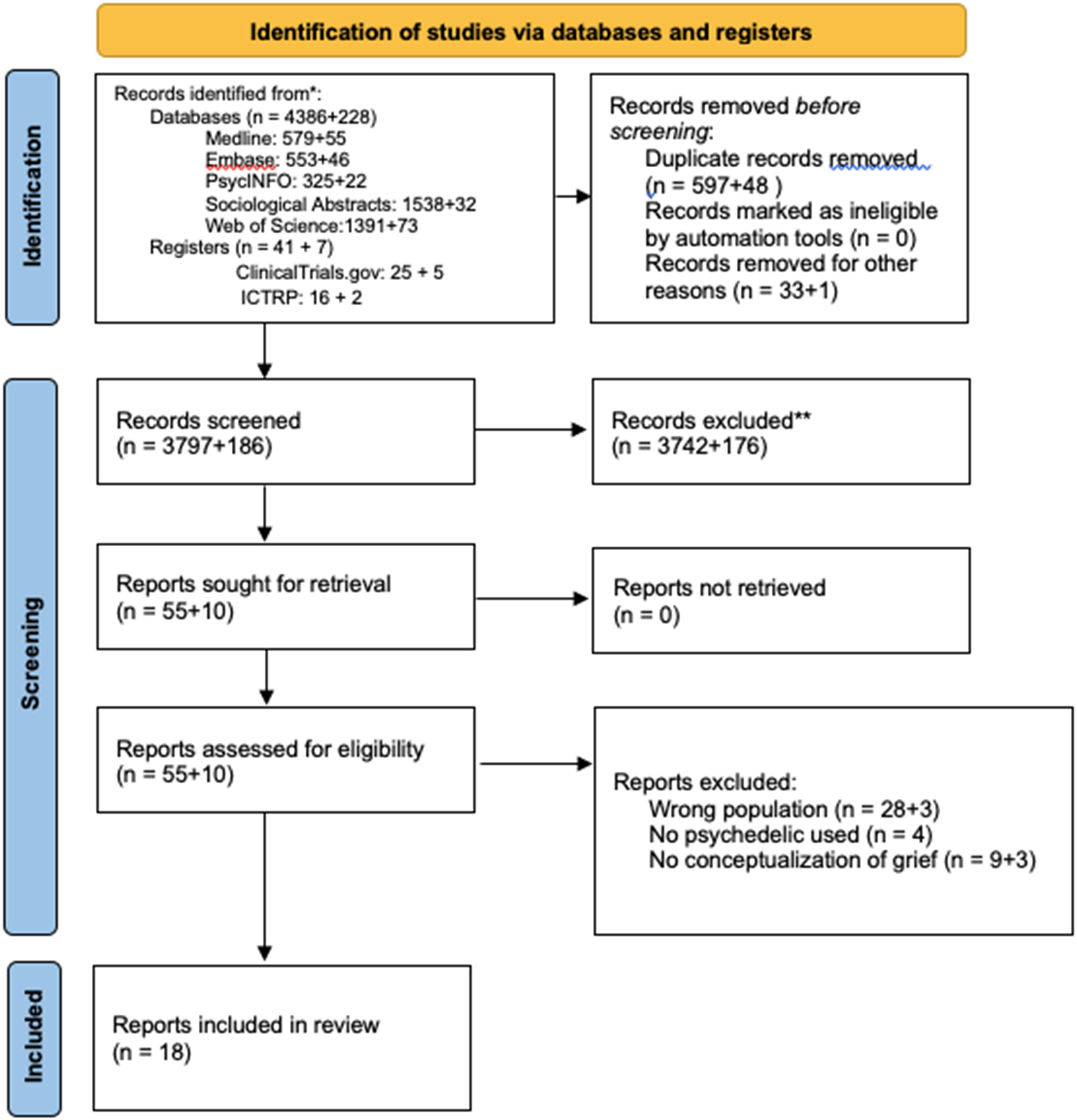
Stage 4: Charting the Data
Data Extraction Table
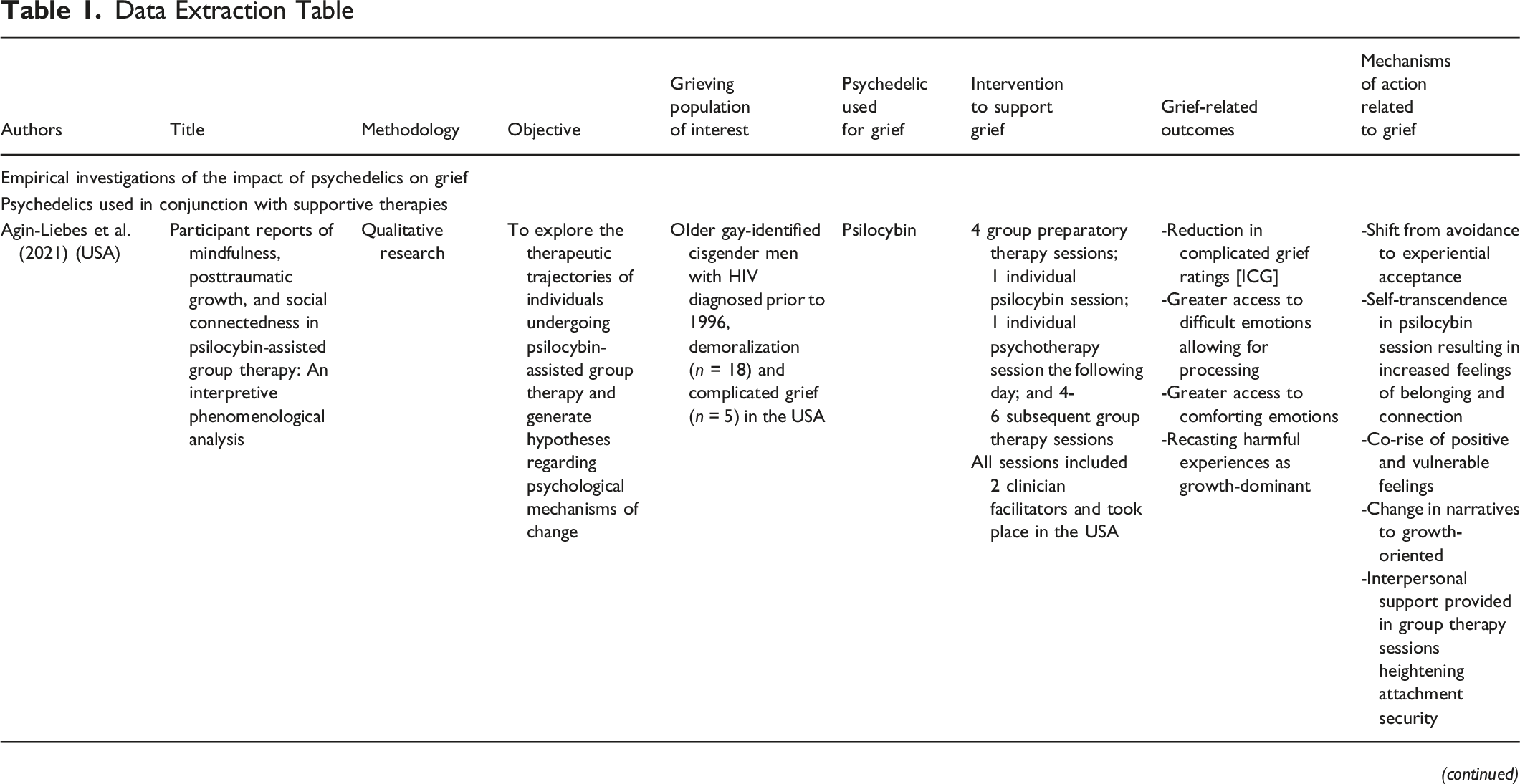
Stage 5: Collating, Summarizing, and Reporting the Results
Team members (CC, DR, SH) each reviewed the data, summarizing and descriptively analyzing the data extraction table with a focus on answering the research questions. Due to the heterogeneity of frameworks, patients, settings, approaches, and outcomes across reports, it proved unhelpful to organize our findings in this decontextualized way. The team then descriptively analyzed each report based on our research questions, noting critiques, similarities, and differences between reports. These descriptive accounts, including the final data extraction table, were finalized through consensus, and the results were interpreted through group discussion and reflection with attention to our overall objectives and clinical experience.
Results
Eighteen eligible records were identified (see Figure 1 for the PRISMA flow diagram). Of these eighteen records, seven have a central focus on investigating the impact of psychedelics to attend to grief (Agin-Liebes et al., 2021; González, 2023; González et al., 2019, 2020, 2022; Low & Earleywine, 2024; Morton, 2023), with four describing the use of psychedelics with accompanying supports (e.g., therapy, a retreat), and three describing psychedelic experience without explicit structured support. The remaining 11 reports contained brief paragraphs on the connection between psychedelic therapies and grief. Our results begin with a summary of methodological approaches, followed by a description of the conceptualizations of grief and theoretical frameworks applied. We then report on what is known about using psychedelics to attend to grief resulting from death due to advanced illness.
Methodological Approaches
We identified seven empirical studies explicitly investigating the impact of psychedelics on grief. These reports include two qualitative research studies (Agin-Liebes et al., 2021; Morton, 2023) and five quantitative studies including a cohort study (González et al., 2020), a cross-sectional study (Low & Earleywine, 2024), one mixed-methods cross-sectional retrospective study (González et al., 2019) and one mixed-methods case study (González et al., 2022), and a non-randomized controlled trial study protocol (González, 2023).
The other 11 reports include one scoping review (Houle et al., 2021) and one narrative review (Maia et al., 2023), four socio-cultural explorations of the intersection of psychedelics and grief, a historical analysis (Dyck, 2019), a subjective account and cultural critique in a book chapter (Isfahani-Hammond, 2020), two ethnographies of Indigenous practices (Shepard, 1998; Shepard Jr., 2002), and five expert opinion and commentary articles (Adrian & Spence, 2022; Beaussant et al., 2021; Johnston et al., 2023; Rosa et al., 2022; Whinkin et al., 2023).
Conceptualizations of Grief and Theoretical Frameworks
A challenge in answering our primary research question was the diversity of perspectives across publications in terms of conceptualizing grief. Several papers made no explicit reference to theory informing the author(s)’s approach. Where specific perspectives were cited, these included: biological (neuropharmacology (Maia et al., 2023), botany (Shepard, 1998; Shepard Jr., 2002)); psychological (attachment theory, humanistic psychology, dual process theory, post-traumatic growth (González et al., 2019)); philosophical (constructivism (González, 2023; González et al., 2022)); spiritual (mysticism, the sacred, transcendence); and cultural/anthropological perspectives (shamanism, the Matsigenka worldview, (Shepard, 1998; Shepard Jr., 2002) “feminist-vegetarian interpretations”(Isfahani-Hammond, 2020)).
The included reports also varied in their psychological conceptualizations of grief. With respect to Western psychological theories, González et al. (2019; 2022) cited the dual process model (Stroebe & Schut, 1999), the constructs of posttraumatic growth (Tedeschi & Calhoun, 2004) and continuing bonds (Field, 2006; Russac et al., 2002), the constructivist approach to grief and grief therapy (Neimeyer, 2006; Neimeyer & Sands, 2011), and meaning reconstruction theory (Neimeyer, 2012; 2015a). A non-Western conceptualization of grief was invoked by Shepard (Shepard Jr., 2002), namely the notion that it is the dead who grieve the living. Many authors acknowledged certain features of normative grief, including the tasks of acceptance and moving on (Dyck, 2019; González et al., 2019). Little was included regarding how normative grief should be supported, with the exception of González’s (González, 2023) study that aims to treat adults experiencing grief in order to prevent Persistent Complex Bereavement Disorder and Prolonged Grief Disorder. Many studies distinguished between normative and pathological grief. However, with respect to the latter, various frameworks and language were used. The terms “pathological”, “prolonged”, “persistent complex” and “complicated” were all used to denote an emotional process distinct from normative grief. Across the included publications, it was commonly implied or stated explicitly that pathological grief warrants treatment.
What is “Known” About Using Psychedelics to Attend to Grief following Death due to Advanced Illness?
Ayahuasca
Ayahuasca was used in all four of the Gonazalez et al. studies (González, 2023; González et al., 2019, 2020, 2022). However, only in the mixed-methods case study (González et al., 2022) and the non-randomized controlled trial (González, 2023) is ayahuasca used as part of a psychotherapeutic intervention designed specifically to prevent Prolonged Grief Disorder. In the mixed-methods case study (González et al., 2022), the therapeutic approach and mechanisms of action explored are relevant to this body of literature; restorative retelling (Neimeyer & Rynearson, 2022) was employed following the participant’s ayahuasca sessions, with the aim of helping the participant “assimilate” the experience and subsequently reorganize their internal world or schemas (a process referred to as “accommodation”). Following the intervention, the participant no longer met criteria for complicated grief. The authors hypothesize that ayahuasca facilitates the emergence of psychological content that helps participants adapt to grief. The participant was noted to “connect with the presence of her mother” during the ayahuasca session(s), highlighting the potential relevance of continuing bonds theory (Klass et al., 1996) to psychedelic therapy for grief. Furthermore, the experience of “contact” with her mother was felt to facilitate a shift in the participant’s “internal working model” of her mother, and this shift was felt to be “the most relevant aspect in [the] participant’s adaptation of grief” (González et al., 2022). The authors suggest such psychological shifts may be understood through the lens of attachment theory, noting, “fostering a secure attachment with the deceased is the objective of various contemporary techniques employed in grief therapy” (Jordan & Neimeyer, 2012; Kosminsky & Jordan, 2016; Neimeyer, 2015b, 2022).
In the non-randomized controlled trial study protocol (González, 2023), the intervention described involves constructivist psychotherapy sessions, one preparation session, and two integration sessions following two ayahuasca administrations (0.75 mg/kg DMT) that take place after the 3rd and 6th therapeutic sessions. The two control groups include (1) constructivist psychotherapy only, and (2) no treatment. Mechanisms of action will be determined by measuring the following at baseline, post-intervention, and at 3 months follow-up: change in grief severity, prevalence of Persistent Complex Bereavement Disorder and Prolonged Grief Disorder, quality of life, posttraumatic growth, avoidance, meaning-made, consistency of self beliefs, subjective effects of ayahuasca, and acceptance or avoidance-promoting effects of ayahuasca.
In the retrospective study, González et al. (2019) explored the potential effects of ayahuasca on grief by comparing experiences of 30 participants who had taken ayahuasca with 30 participants who attended peer-support grief groups (González et al., 2019). Seventy percent of participants in the ayahuasca group had experienced loss due to illness, versus only 43.3% in the peer support group. People who used ayahuasca reported lower levels of grief post-test than people in the control group (p < .001). All of the ayahuasca participants believed their experience had a very positive (25/30) or positive (5/30) influence on their grieving process. Subjectively, ayahuasca participants reported feelings of peace and acceptance of death via emotional confrontation and release; recollection of forgotten memories with the deceased or the experience of an “autobiographical review” from another point of view; and contact with the deceased during the ayahuasca experience. The emotional confrontation during the ayahuasca experience, while often painful, was hypothesized to promote feelings of peace and acceptance via the integration of the loss into the patient’s life history. Recollection of forgotten memories, the authors suggest, may “facilitate the redefinition of their relationship with the deceased and of their own life history.” Notably, the authors claim contact with the deceased and maintenance of the bond may offer “the greatest therapeutic impact.”
The prospective, observational cohort study reported on the course of grief related to the loss of a loved one among 50 participants (39 of whom completed the study) who attended a retreat centre in Peru to participate in Indigenous Shipibo ayahuasca ceremonies (González et al., 2020). Most participants experienced loss from a naturally foreseeable death. Subjects participated in one of a range of retreats which were not designed specifically to support those experiencing grief. A significant decrease in grief severity was observed at all time points following participation in the ayahuasca ceremonies (p < .001), and effect sizes were large at all time points. Ratings of quality of life in physical health, psychological health, and social relationships all improved significantly and endured at 12 months following the retreat. The proposed mechanisms of change – acceptance (i.e., the positive formulation of experiential avoidance) and decentering (i.e., the capacity to observe one’s thoughts and feelings in a detached manner) – both significantly improved after the retreat (p < .001), with improvements noted at all timepoints. The authors propose that acceptance and decentering mediate the improvement of grief symptoms.
Ayahuasca was discussed in two literature reviews citing the work of González et al. (2019, 2020), (Houle et al., 2021; Maia et al., 2023) as well as in a subjective account of an adult child grieving the death of their parents (Isfahani-Hammond, 2020). The author noted that ayahuasca facilitated contact with the deceased, which helped create a renewed sense of connection and “tenderness”.
Psilocybin
Psilocybin is explored in the interpretive phenomenological analysis conducted by Agin-Liebes et al. following a group therapy intervention for the treatment of demoralization among long-term AIDS survivor men (Agin-Liebes et al., 2021). Five of the 18 participants in the trial experienced “complicated grief” related to numerous losses during the AIDS epidemic. The therapeutic approach of the group therapy sessions was not discussed in detail. Among those who reported grief at baseline (n = 5), there were significant reductions in complicated grief following the intervention. Subjectively, participants reported greater access to and ability to process emotions during the psilocybin experience, including grief. More generally, participants described an enhanced capacity for meta-awareness; increased emotion processing and regulation capacity, along with enhanced emotional/experiential acceptance; and increased transcendence and dissolution of self-boundaries, leading to increased feelings of connectedness. The authors described how the therapy facilitated the appreciation of past traumatic experiences as vehicles for growth through changing “from automatic to mindful modes of processing” and from trauma-dominant to growth-dominant narratives.
In a phenomenological qualitative study, Morton investigated the subjective experiences of seven individuals who used psilocybin to process grief after losing a “loved one” (Morton, 2023). Three of the participants had experienced loss due to illness, two to suicide, one to murder/suicide, and one to a car accident. The time between loss and psychedelic experience ranged from less than a year to 13 years. The psilocybin experience was identified as important, with respondents describing resolution of internal conflict, feelings of connectedness, and experiential acceptance of emotions during the experience. In terms of outcomes attributed to psilocybin, participants described increased awareness of thought patterns and self-compassion, increased comfort with mortality and loss, and increased spirituality/belief in life after death. The study also reported an improvement in depressive symptoms and reduced feelings of numbness after loss among participants. Morton drew parallels between these outcomes and the goals of complicated grief therapy, suggesting that psilocybin could serve as a useful complement (Morton, 2023). A spiritual dimension was also described, with participants reporting an enhanced spiritual outlook after the psilocybin experience that helped them address feelings of death anxiety and existential distress associated with bereavement.
Psilocybin use for grief was described in a recent update on new palliative care interventions (Whinkin et al., 2023) as well as a reflective opinion piece (Adrian & Spence, 2022), both of which discuss a ceremonial retreat model in Jamaica where psilocybin is provided to bereaved parents under supervision from physicians and therapists from the US, Canada, and Jamaica (where psilocybin is legal). Some of the parent participants are described as having lost a child suddenly, i.e. to overdose, suicide, accident, or murder. The intervention involves a group ceremony in which participants are invited to “[open] up, [share] stories, [refine] goals, [and revisit] ‘the worst pain of their lives'” with staff support. The retreats aim to support grieving parents in spiritual, psychological, and existential struggles around the death of their children. Adrian & Spence hypothesize that the mechanisms by which grieving parents might benefit from such an approach include experiential acceptance of suffering, meaning-making from suffering, and forging connections and community with others who have experienced similar losses (Adrian & Spence, 2022).
Other
The cross-sectional study conducted by Low and Earleywine (2024) surveyed a group of 363 individuals who had used a psychedelic substance in the context of bereavement. Most participants endorsed using the psychedelic within 5 years of bereavement in order to address their symptoms of grief. Most respondents went through the experience alone, in a single session (57.6%). The most common psychedelic used was psilocybin, followed by lysergic acid diethylamide (LSD), 3,4-methylenedioxymethamphetamine (MDMA), ketamine, peyote, dimethyltryptamine (DMT), mescaline, salvia, ayahuasca, phencyclidine (PCP) and ibogaine. Most participants reported significant improvements in grief symptoms after their psychedelic experience. Half of these participants reported functional impairment prior to their experience, and less than a third continued to report impairment after. The authors observed a positive correlation between emotional breakthroughs during the psychedelic experience – defined as the overcoming of difficult feelings or memories leading to relief, as measured by the Emotional Breakthrough Inventory (EBI) (Roseman et al., 2019) – and improvement in grief symptoms. Conversely, challenging experiences were negatively correlated with improvement in grief symptoms. Notably, 11% of participants reported worsening symptoms of grief after taking psychedelics.
In Shepard’s ethnographic studies of grief among the Matsigenka people of Hayapaari, Peru, “psychoactive plants” (some of which contain DMT) are reported to treat symptoms of grief persisting beyond cultural norms (that is, beyond the three days allotted for grieving within Matsigenka culture) (Shepard, 1998; Shepard Jr., 2002). Specifically, “ergot compounds…with diverse psychoactivity and diverse physiological activities (noted vasoconstrictors)” are described, along with “pungent tobacco snuff” taken intranasally, or “kaokirontsi” (eye cleanser) medicines that “[sting and burn] the eyes” to control negative emotions that are socially disruptive.
In a review of the history of psychedelics and end-of-life care, Dyck (Dyck, 2019) discusses the case of Aldous Huxley, the famous writer, philosopher, and psychedelic thinker, who supported the death of his wife, Maria Nys, who also studied philosophy and mysticism. Drawing on their psychedelic experiences (notably with mescaline and LSD), Huxley guided Nys to move towards peace in her final moments. As Dyck describes, Nys died surrendering her life without struggle, which was a great comfort that reportedly decreased Huxley’s experience of grief.
Finally, several papers reference the potential use of psychedelics for grief among caregivers of patients who are dying (Beaussant et al., 2021), older adults experiencing grief related to the deaths of spouses and friends (Johnston et al., 2023), and family caregivers of people with serious illness, including parents of young children (Rosa et al., 2022). How psychedelics could support these potential outcomes is not explored in depth in these articles.
Discussion
Main Findings of this Review
This review demonstrates that there is little that can be definitively stated about the benefits of psychedelics to attend to grief following death from advanced illness. The empirical papers included employed a variety of qualitative and quantitative methodologies, although none employed a randomized controlled design that might allow for more definitive conclusions to be drawn about treatment efficacy. That said, positive outcomes were generally reported in terms of grief symptom reduction, with few reported adverse or negative outcomes. Higher rates of poor outcomes (i.e., no improvement or worsened grief symptoms after psychedelics) were reported more among recreational users studied by Low and Earleywine (2024) than among participants in the ceremonial ayahuasca context studied by González et al. (2019). In Low and Earleywine’s (2024) study, worse outcomes among recreational users were associated with more challenging experiences, and most respondents reported using psychedelics alone. While the authors described their sample as recreational users, more than 80% of participants reported having used psychedelics with an intention to address grief. These findings highlight the potential importance of psychological support, whether offered in a clinical or ceremonial milieu.
What this Study Adds
Despite the lack of strong evidence on which to make recommendations or conclusions, based on the number of papers on this topic, there is clearly interest in this approach and growth in research applying psychedelics to the problem of grief.
Several mechanisms of action were proposed by which psychedelics might reduce grief symptoms or enhance grief therapy. Numerous papers suggested that psychedelics facilitate access to, emergence of, and, importantly, acceptance of previously avoided and distressing emotional material. In Low and Earleywine’s (2024) survey study, emotional breakthrough was positively correlated with improved grief symptoms. Several papers suggest that psychedelics promote relational connectedness, including via contact with the deceased during the psychedelic experience itself. Morton found that some participants reported improvements in grief as a function of “increased spirituality and belief in life after death (Morton, 2023)”.
Other cultural or spiritual rituals, psychotherapies, or interventions may be able to stimulate similar shifts but in a slower or more subtle fashion. Studying the combination of psychedelics and other practices known to support those experiencing grief could prove fruitful, especially if there are strong theoretical or empirical reasons for particular combinations. This strategy is being employed by González et al. (2022) in their upcoming non-randomized clinical trial, which compares ayahuasca in combination with constructivist psychotherapy for grief against constructivist psychotherapy alone, with an additional control group that will receive no treatment.
Tying the possible mechanisms of change identified in this scoping review to prominent psychological theories of grief or grief therapies can help researchers develop targeted interventions as well as hypotheses about change mechanisms that can be tested empirically. For example, the finding that psychedelics facilitate acceptance is noteworthy, as acceptance has long been identified as an important task for those experiencing grief (Kübler-Ross, 1969; Worden, 1996). Next, reconnecting with the presence of the deceased – a feature common to the ayahuasca experience, as noted by González et al. (2019; 2022), – also appears significant and suggests the potential relevance of continuing bonds theory (Klass et al., 1996) to psychedelic-assisted psychotherapy for grief. Relatedly, connection with the presence of the deceased during the psychedelic experience may also promote a new representation or internal working model of the loved one, which highlights the relevance of attachment theory (Bowlby, 1982). Finally, the possibility that psychedelics may support the grieving process by altering metaphysical beliefs (e.g. about the persistence of life after death) raises the potential relevance of Letheby’s Metaphysical Belief Theory (Letheby, 2024), which argues that when psychedelics reduce the fear of death, they do so by inducing or increasing non-physicalist beliefs.
Methodological Critiques and Considerations
The papers identified in this review used a wide variety of research methodologies, addressed different types of loss in different populations, and examined different treatment approaches in different settings with a variety of psychedelic compounds. Perhaps what is most striking about this review is this variety, and the convergence of different epistemologies, ontologies, cultures, paradigms, and interests. The diversity of theories and grief conceptualizations, sometimes within a single paper, highlights the many approaches and interests aimed at both psychedelic and grief studies. This diversity complicates the synthesis of this material and highlights potential conflicts that may arise based on differing values and priorities. However, it also creates potential for added richness and depth. As Dyck (Dyck, 2019) points out, “psychedelic experiences invoke a variety of reactions that often rely on a more expansive vocabulary to render them meaningful, whether that vocabulary borrows from a spiritual realm, an anthropological one, or a philosophical dimension” (p. 5), and the literature on grief has a similar history.
The interests driving the rapid growth in this field may include a wish to address suffering with a novel and promising approach, but may also include other interests, such as profit motives, interest in elevating “alternative” approaches to mental health and healing, and the interests of individual researchers (e.g., power, prestige, etc.). There is often a creative interplay between motives that nonetheless may lead to important discoveries and advancements. There is also, however, the risk of creating an industry around problematizing normative distress or creating iatrogenic issues such as those seen with the opioid crisis or prescription of antidepressants (Whitaker, 2010). At this early stage – as grief is being conceptualized as a potential target for psychedelic-assisted psychotherapy – there is an opportunity to consider the interests driving this work with a critical eye. Numerous authors have explored these dynamics with respect to grief, including whether it ought to be considered a normative human experience, how it ought to be supported, and where the line may be between normative and “pathological” grief (Aftab, 2024; Zachar et al., 2023). Similarly, there is a growing field of critical psychedelic studies that can inform these issues as they relate to the development and study of psychedelic-assisted psychotherapy (Devenot, 2024; Hauskeller & Schwarz, 2023).
In many of the papers reviewed, psychedelics were used by non-clinicians in non-clinical settings (or by individuals without formal support), rather than by healthcare providers in hospitals or clinics. Many papers were written by authors without clear expertise in the problem of grief. As this field grows, we will likely see further tensions between “medical” (or “expert”) versus “lay” practitioners, and “normal” versus “abnormal” conditions. Again, there may be valuable and novel directions arising from these tensions, but also potential harm if new and “unproven” treatments are hastily promoted without the input of experienced clinicians, experts, or individuals with long histories and established practices using psychedelic and related substances for healing (Celidwen et al., 2023; Urrutia et al., 2023). Here we should note our position as academic clinicians and researchers who tend to give weight to evidence-based medicine and the kind of knowledge it generates. However, we also acknowledge that this apparatus has significant limitations and technical biases, preferring methods such as randomized controlled trials that are challenging to conduct with complex interventions like psychotherapies (Gupta, 2014) and especially psychedelic-assisted psychotherapy (Schenberg, 2021). We also acknowledge the inherent biases in this form of knowledge-making that ignores or dismisses Indigenous knowledge and ways of knowing that could inform clinical approaches to psychedelic use, both in the area of grief and beyond (Hauskeller et al., 2023; Marcus & Dakwar, 2023; Williams et al., 2022).
Strengths and Limitations
Strengths of this scoping review include working with an information specialist to design and carry out the search strategy, employing a diverse team with experience conducting scoping reviews, and adhering to PRISM-ScR. Limitations include consulting databases focused on medicine, health sciences, psychology, social sciences, and interdisciplinary health studies, while omitting the anthropological or religious studies literature. Our scoping review protocol was not registered in advance. This review is also limited by the quality of the included reports. For example, while our aim was to explore what is known about using psychedelics to attend to grief following death due to advanced illness, many of the included reports looked at other types of losses (e.g., loss due to suicide, other sudden death, or accidental death). We did not exclude reports that included discussion of grief following these other kinds of loss, provided that there was also discussion about grief following loss due to advanced illness. The amount of psychedelic research published is rapidly growing, and it is possible that a similar scoping review in the next few years will lead to clearer conclusions and recommendations.
Conclusion
This scoping review, exploring what is known about using psychedelics to attend to grief following death due to an advanced illness, found that there is not a strong evidence base upon which to make clinical recommendations at this time. The literature is informed by different epistemologies, ontologies, and paradigms, as well as theories, models, and psychological concepts, adding a layer of complexity and a challenge for consensus building. That said, our findings do suggest potential positive impact of psychedelics in supporting people experiencing grief when offered in appropriate contexts with adequate psychological support. Our recommendations for future research, given the diversity of perspectives noted, are for authors and researchers to: (1) explicitly situate their work within theoretical traditions; (2) comment on their background, position, and interests in order to assist with the interpretability of their work; and (3) clearly describe their study population (i.e., what kinds of loss have participants experienced) and consider the particular psychological needs of people who have experienced different kinds of losses. Finally, and more generally, it would significantly strengthen research in this field if experts in grief joined with experts in psychedelic medicine in the development of grief-focused psychedelic interventions and in the associated research.
Supplemental Material
Supplemental Material - Exploring what is Known About Using Psychedelics to Attend to Grief Following Death due to Advanced Illness: A Scoping Review
Supplemental Material for Exploring what is Known About Using Psychedelics to Attend to Grief Following Death due to Advanced Illness: A Scoping Review by Daniel Rosenbaum, Celina Carter, Brandon A. Cirella, Matthew Cho, Melanie Anderson, and Sarah Hales in OMEGA - Journal of Death and Dying
Footnotes
Authors Contributions
All authors drafted, revised, and approved the final version of this article. Authors DR, CC, and SH contributed to the concept, design, acquisition, analysis, and interpretation of data. MA contributed to the design and data acquisition. Authors BC and MC contributed to data analysis, and BC provided editorial support.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by a grant from an anonymous not-for-profit donor to the UHN Foundation.
Data Availability Statement
Full preliminary search results can be made available upon request.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
