Abstract
Suicide and self-harm events are elevated in psychiatric inpatient populations. In this study, health data were retrospectively collected from the medical records of 183 patients (97 civil and 86 forensic) who had resided in, or been admitted to, a public psychiatric hospital in Saskatchewan, Canada from April 1 to December 31, 2021. Descriptive and inferential analyses were conducted to estimate prevalence and correlates of (non-fatal) suicide and self-harm events, including recent and lifetime occurrences, according to patients’ health information. Nearly two-thirds (62%) of patients had any record of non-fatal suicide or self-harm events, including a lifetime history of self-harm (42%) and suicidal behavior (37%) as well as recent self-harm (24%) and suicidal (31%) thoughts or behaviors. Forensic patients were significantly more likely to have a record of suicide and self-harm events. This study emphasizes the need for further research into the course of suicidality and self-harm in psychiatric inpatients.
Introduction
Globally, it is estimated that over 700,000 people die by suicide every year and, in 2019, the global age-standardized suicide mortality rate was 9.0 per 100,000 population (equating to over 1 in 100 deaths), which was comparatively lower than the national age-standardized suicide mortality rate of 10.3 per 100,000 Canadians (World Health Organization, 2021). Given the importance of each life lost due to suicide, ideation-to-action approaches (Klonsky et al., 2018) have drawn greater attention to the (unique) mechanisms underlying the cognitive versus behavioral phases of the suicide continuum with an aim to pinpoint targets for intervention along this continuum and, ultimately, disrupt risk of suicide-related death. Ideation-to-action approaches, which have also been used to investigate self-harm processes (Melson & O'Connor, 2019), 1 were generally borne out of the fact that many more individuals will engage in suicidal behavior that does not result in death (as compared with completed suicide) and even more will think about suicide without acting on these thoughts (e.g., see Drapeau & McIntosh, 2023; Klonsky & May, 2014, 2015; Nock et al., 2008; Ten Have et al., 2009). Within the context of the general Canadian population, recent data suggest that 1 in 8 (12%) have thought about suicide, 1 in 24 (4.2%) have made suicide plans, and 1 in 32 (3.1%) have made a suicide attempt (Public Health Agency of Canada, 2023). Self-harm behaviors also continue to be problematic in Canada (especially for younger individuals), as hospitalizations for self-inflicted injury is suggested to occur at a rate of 47 per 100,000 Canadians (Yao et al., 2020). Taken together, further investigation into the nature of suicidal and self-harm thinking and behavior, especially among the most vulnerable groups in society, contributes to the global and national imperative of building a knowledge base to inform the management of suicide and self-harm.
Although death by suicide among patients hospitalized in psychiatric settings is a rare event (given one of the aims of psychiatric hospitalization is to prevent suicide), the incidence of completed suicide in psychiatric hospitals is elevated when compared with community settings as rates are reported to be anywhere from 5 to 50 times higher than in the general population (Chammas et al., 2022; Walsh et al., 2015). The high incidence of suicide in these settings is partly attributable to the criteria for psychiatric hospitalization, including known contributors of suicidal risk (e.g., severe mental disorders) and suicide and self-harm events themselves. Detection and treatment also prove to be challenging. For instance, in their study of 76 inpatient suicides, Busch et al. (2003) found that most patients who died by suicide (78%) denied having suicidal thoughts in their last assessment before the event and, of those on observation, more than half (51%) died by suicide. While the rate of suicide among psychiatric inpatients varies across jurisdictions and institutions (Chammas et al., 2022), a recent meta-analysis suggests a rate of 1 suicide per 676 (95% CI [604, 755]) admissions or 147 (95% CI [138,156]) suicides per 100,000 inpatient years (Walsh et al., 2015). Several studies have also identified variability in the incidence of completed suicide according to psychiatric diagnoses, indicating that psychotic disorders (e.g., schizophrenia) and mood disorders (e.g., bipolar and depressive disorder) are most commonly present among psychiatric inpatients who have died by suicide (Chammas et al., 2022; Walsh et al., 2015).
Self-harm and suicide attempts are also notably prevalent among adults receiving psychiatric inpatient services. For instance, current estimates suggest that anywhere between 36% and 87% of psychiatrically hospitalized persons have a history of suicide attempts, whereas the prevalence of self-harm history may range from 17% to 45%, and in either case the risk for multiple events in this population is high (Andover & Gibb, 2010; Busch et al., 2003; Horon et al., 2013; James et al., 2012; Jentz et al., 2022; Nijman et al., 1999). However, rates further vary according to civil (Andover & Gibb, 2010; Nijman et al., 1999) and forensic (Horon et al., 2013; Jentz et al., 2022) psychiatric inpatient populations. Indeed, James et al. (2012) reported that the incidence of self-harm and/or suicide attempts (43%) is highest in units that treat justice-involved individuals (i.e., forensic wards). This is supported by a study of male patients in a secure psychiatric hospital in the UK that found significant differences in the average number of self-harm incidents (threats or acts) per 30 days between civil (M = 0.06) and forensic (M = 0.21) patients (Galappathie et al., 2017).
Consistent with ideation-to-action approaches (Klonsky et al., 2018) and perspectives on the course of suicidality (Ten Have et al., 2009), which describe suicide and self-harm on a continuum from ideation to behavioral enaction, psychiatric patients with a desire for death (i.e., suicidal ideation) and capability of inflicting self-harm (i.e., presence and frequency of non-suicidal self-injury episodes) have been found to be at greatest risk of suicide attempts and completions (Andover & Gibb, 2010; Horon et al., 2013; Hubers et al., 2018). This concurs with findings on suicide attempts (Favril et al., 2022) and completions (Zhong et al., 2021) in correctional populations, as suicidal ideation and a history of self-harm (in addition to psychiatric morbidity) have been identified as the strongest risk factors for these suicidal outcomes among people in custody. With that said, justice-involved individuals are also a high-risk group for suicide (Webb et al., 2011) and suicide has been declared a leading cause of death in correctional facilities worldwide (Fazel & Baillargeon, 2011). Studies involving people in custody across several (high-income) countries have documented elevated rates of completed suicide as compared with general populations (Fazel et al., 2017), as well as note a high prevalence of suicidal ideation and suicide attempt over the life course (20–58% vs. 11–37%, respectively) and while in custody (16–40% vs. 7.5–11.9%, respectively) (Favril et al., 2020a, 2020b, 2020c; Favril & O’Connor, 2021; Favril et al., 2022; Jenkins et al., 2005; Larney et al., 2012; Stoliker et al., 2023). Therefore, psychiatric inpatients with previous or ongoing involvement in the criminal justice system represent a particularly vulnerable group for suicide and self-harm.
It is against this background in which the current study is situated. Notably, despite a growing body of research into suicide and self-harm among high-risk groups, such as psychiatric and correctional populations, studies involving these populations within the Canadian context have been scarce (e.g., Casiano et al., 2016; Correctional Investigator Canada, 2014; Sharma et al., 1998). This study explored suicide and self-harm thoughts and behaviors among civil and forensic inpatients at a public psychiatric hospital in the province of Saskatchewan to enhance the epidemiological data on this issue in Canada. Specifically, patients’ official medical records were reviewed and analyzed to provide preliminary evidence on non-fatal suicide and self-harm events in this population, including both recent and lifetime occurrences.
Methods
Setting and Data Collection
The study was conducted at a public psychiatric hospital in Saskatchewan, Canada which is a provincial mental health facility that serves the population of Saskatchewan (1.18 million people). Specifically, the hospital provides (i) short- and long-term rehabilitative psychiatric services to individuals across the province whose needs cannot be met in acute inpatient mental health centres, (ii) forensic assessment and treatment, and (iii) short- and long-term rehabilitative psychiatric services to remanded and sentenced offenders whose needs cannot be met within provincial correctional centres or acute inpatient mental health centres. The hospital has a total of 284 beds spread across seven general treatment units and three community reintegration units dedicated to the treatment of civil patients (146 beds), two units for forensic services (42 beds), and four integrated correctional units for remanded and sentenced patients requiring stabilization or treatment (96 beds). Therefore, it is a secure inpatient facility with separate units dedicated to civil and forensic patients.
Notably, the study population may be unique compared with other groups of patients (e.g., psychiatric admissions to public hospitals, psychiatric admissions to acute inpatient mental health centres, and outpatients receiving mental health services), as the psychiatric hospital involved in this study is the only facility of its kind in Saskatchewan, which provides inpatient psychiatric services to individuals living with (any) mental health symptoms or disorders that exceed the capacity of other mental health services in the province to effectively assess and treat. Therefore, this hospital admits patients from across the province with high-level and specific psychiatric needs that cannot be managed by other health services. For civil patients, they are admitted from the community or other inpatient units under a voluntary or involuntary designation according to the Mental Health Services Act (1986) for the stabilization of mental health symptoms. For forensic patients, they are admitted under the following circumstances (for which the Act also applies): court-ordered sanctions (e.g., long-term detention orders); forensic assessment (e.g., evaluation of fitness to stand trial or eligibility for the defence of not criminally responsible on account of mental disorder (NCRMD)); forensic treatment (e.g., treatment of persons found unfit to stand trial to restore fitness, treatment of NCRMD accused to improve mental health symptoms and reduce risk to public safety); and, stabilization of mental health symptoms for persons in custody in a provincial correctional centre. While some patients may be hospitalized due to suicide or self-harm events, this is not the only reason for psychiatric hospitalization at the study facility.
In April 2021, the hospital implemented a new policy and protocol for the assessment and management of suicide and self-harm, including the introduction of new screening and risk management tools. In short, all patients admitted to the hospital as of April 2021 are assessed according to a suicide screening questionnaire, which may prompt a risk assessment and management plan to match institutional safety measures and treatment targets to patients’ level of risk. 2 With the implementation of the new policy and protocol, this study was undertaken to provide foundational information on suicide and self-harm among patients at the hospital to guide future research and practice in this setting. Our study design and procedures were approved by the University of Saskatchewan’s Biomedical Research Ethics Board on November 27, 2021 (Bio 3092). As per Section 29(2) of the Health Information Protection Act (2003), personal health information used in this study did not require the consent of patients included in the sampling frame.
Data were retrospectively collected for civil (n = 97) and forensic (n = 86) patients who had resided in, or been admitted to, the hospital since the implementation of the new policy and protocol on April 1, 2021 to the study end point of December 31, 2021. Specifically, secondary health data were collected via review of patients’ electronic and paper medical records, which included admission notes, discharge summaries, a suicide screening questionnaire (non-validated), a suicide risk assessment guide/risk management plan (non-validated), the Brøset Violence Checklist (BVC) (Linaker & Busch-Iversen, 1995; Woods & Almvik, 2002; Woods et al., 2015), and the Short-Term Assessment of Risk and Treatability (START) form (Webster et al., 2006). For medical records to be included in the sample, patients had to be 18 years of age or older at the time of admission and have some level of documentation on lifetime or recent non-fatal suicide and self-harm events (i.e., indication of presence or absence of these events).
Measurement
Suicide and Self-Harm
Patients’ medical records were reviewed for lifetime history, as well as recent incidents, of non-fatal suicide and self-harm events. Lifetime history of suicidal and self-harm behavior were captured according to items from the START form and transformed into two distinct binary variables (1 = yes, 0 = no). Recent self-harm thoughts or behaviors were captured according to a single item from the suicide screening questionnaire, which asked patients “have you had any thoughts, urges, or behaviors related to harming yourself?” (1 = yes, 0 = no). Recent suicidal thoughts or behaviors were based on the aggregation of three items from the suicide screening questionnaire, which asked patients “are you thinking of suicide?”, “have you made any current plans?”, and “do you have the means to act on your plan?” (1 = yes, 0 = no). Given the protocol for administering the suicide screening questionnaire (i.e., up to once a day for four weeks following admission and as required during hospital stay), information from all forms completed for a single patient during the study period were aggregated to reflect one or more affirmative responses (vs. none) to the above suicide screening questionnaire items. In addition, “recent” non-fatal suicide and self-harm events constitute those captured during patients’ hospital stay via the suicide screening questionnaire and, therefore, may range by days, weeks, or months.
Clinical Factors
Psychiatric diagnoses were captured according to information provided in admission notes, discharge summaries, and the START form and transformed into a series of binary variables (1 = yes, 0 = no) based on the major DSM-5 classifications of mental disorders. A single patient could therefore be counted in more than one category of mental disorder diagnosis. While it is preferred to classify patients according to primary and secondary diagnoses (e.g., Galappathie et al., 2017), the medical records used in this study did not specify this information.
Other information collected from patients’ medical records included a history of childhood trauma (i.e., physical, emotional, or sexual abuse and neglect), history of involvement in the criminal justice system (e.g., charged with a Criminal Code offense, community sentence, incarceration, etc.), history of violence, substance use history, as well as vulnerability indicators (i.e., poor: social support, impulse control, and coping abilities). Each of these factors were transformed into binary variables (1 = yes, 0 = no). Given the link between hopelessness and suicidality (Horon et al., 2013; Stoliker et al., 2021), we also included a binary measure based on a single item from the suicide screening questionnaire which asked patients, “are you having any feelings of hopelessness, helplessness or depression?” (1 = yes, 0 = no). Furthermore, all patients admitted to the hospital receive ongoing assessment regarding their risk of violence, which is documented three times per 24-h period using the BVC (see Woods et al., 2015). All BVC forms completed during the study period were analyzed and scores for the total BVC, as well as its six subcategories, were calculated to create summative scales that quantify patients’ level of violence (with higher scores indicating a higher number of violence-related incidents).
Patients’ medical records also provided information on select sociodemographic characteristics (i.e., age in years, biological sex, and relationship status) and whether patients were residing in a non-custodial or custodial hospital unit (i.e., units dedicated to the treatment of civil or forensic patients, respectively).
Statistical Analysis
Data were cleaned and analyzed using the Statistical Package for the Social Sciences (SPSS version 28). Prior to descriptive and inferential analysis, a missing values analysis was conducted. Results from Little’s MCAR test demonstrated there was a range of 0–37.2% missing values across all items and, further, there was evidence to suggest these data were not missing completely at random, χ2 (2) = 41.635, p < .001. However, Multiple Imputation (MI) has been shown to correct bias and improve efficiency even with high percentages of missing data (Lee & Huber, 2021). MI was therefore used to manage missing data to reduce bias in estimates. In MI estimation, SPSS settings were configured to: have all variables act as predictors and were imputed; set constraints so that imputed values were within the range of valid scores; and perform a total of 20 imputations. All results are based on pooled estimates of the 20 imputed datasets.
Characteristics of Patients, by Total Sample and Record of Non-fatal Suicide or Self-Harm Events.
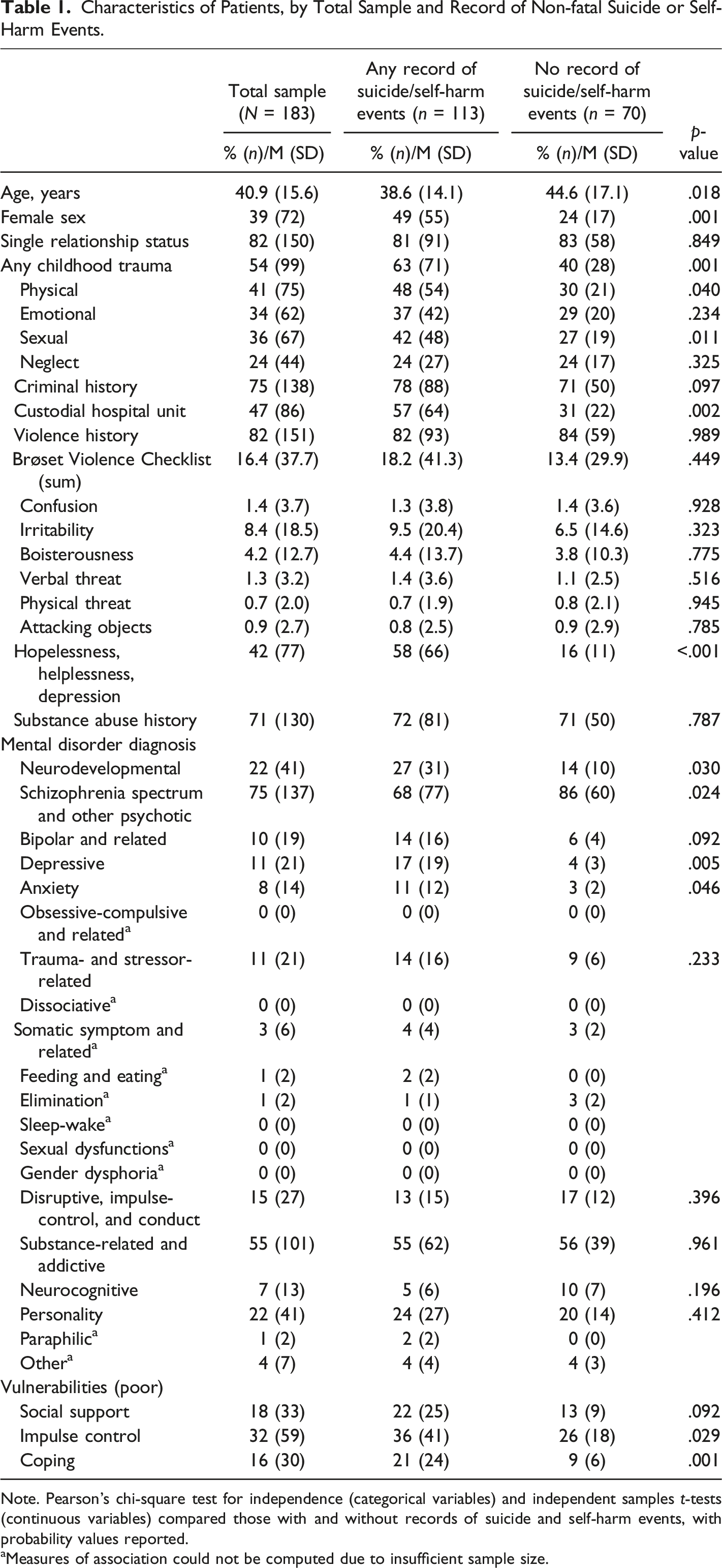
Note. Pearson’s chi-square test for independence (categorical variables) and independent samples t-tests (continuous variables) compared those with and without records of suicide and self-harm events, with probability values reported.
aMeasures of association could not be computed due to insufficient sample size.
Prevalence Estimates for Suicide and Self-Harm Status, by Select Study Variables.
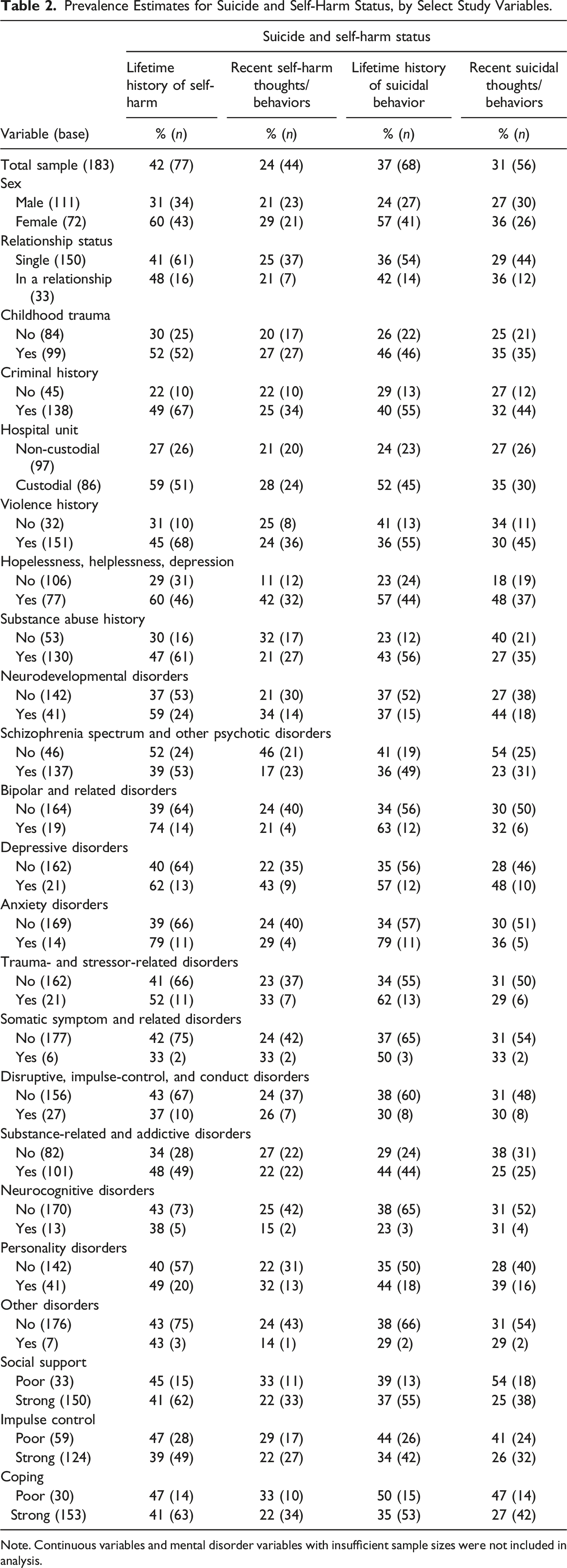
Note. Continuous variables and mental disorder variables with insufficient sample sizes were not included in analysis.
Bivariate and Multivariate Analysis for Lifetime History of Self-Harm, Compared to No History.
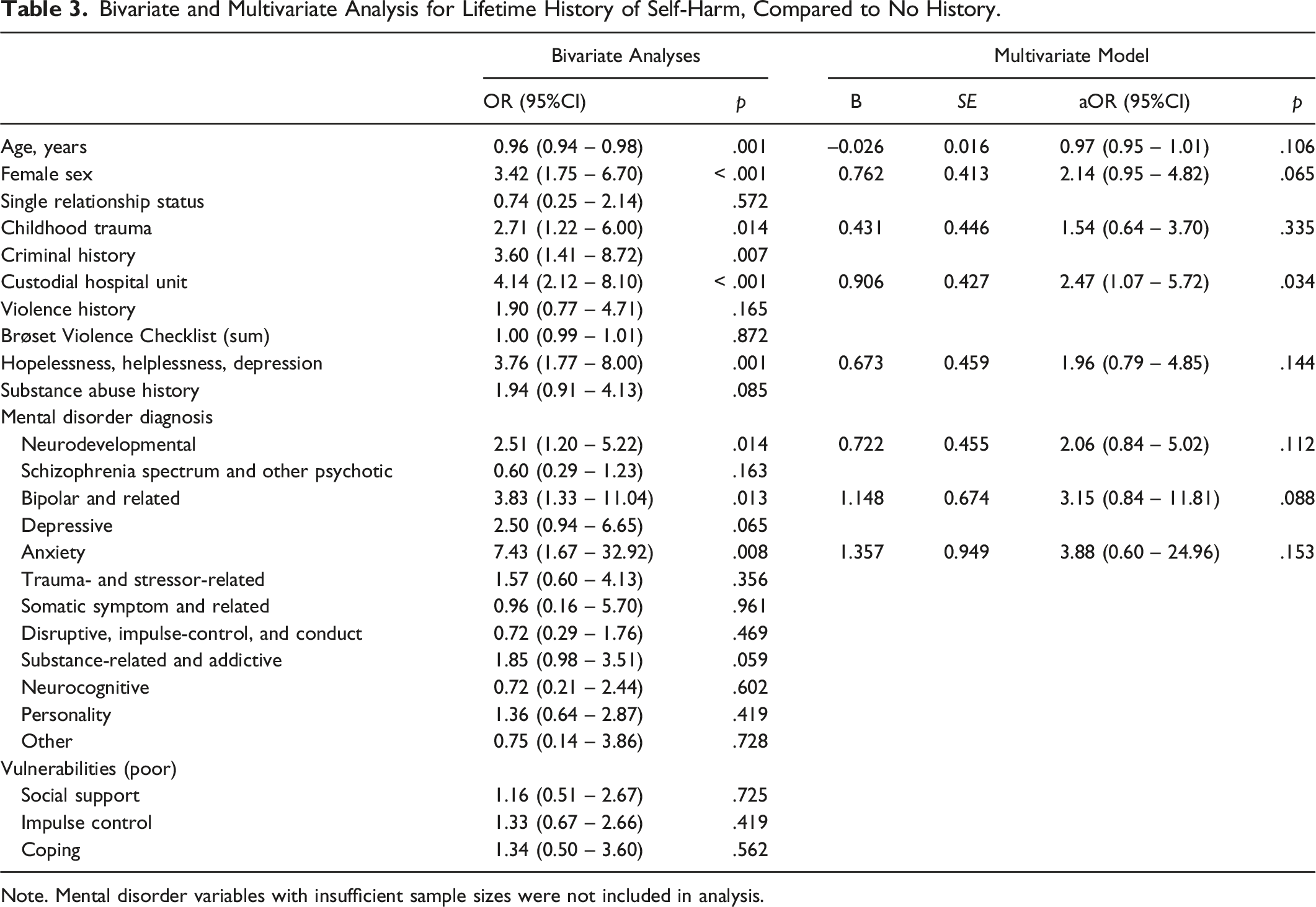
Note. Mental disorder variables with insufficient sample sizes were not included in analysis.
Bivariate and Multivariate Analysis for Lifetime History of Suicidal Behavior, Compared to No History.
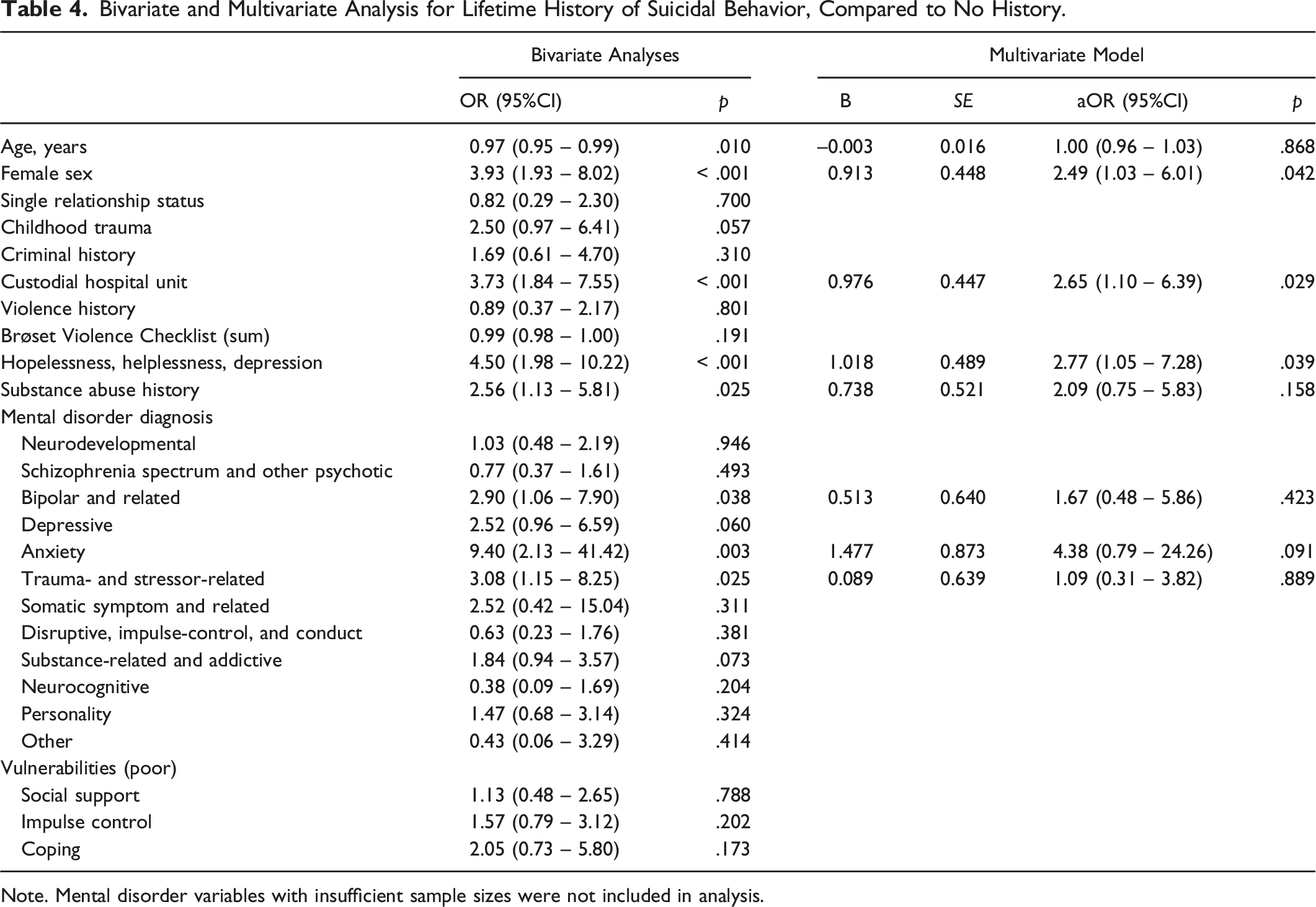
Note. Mental disorder variables with insufficient sample sizes were not included in analysis.
Results
Patient Characteristics
Table 1 presents information on patient characteristics, by total sample and suicide and self-harm status. Based on medical records for the 183 patients included in this study, the average age was 40.9 years (SD = 15.6), 39% were female, and 82% were single. Notably, 54% of patients had a recorded history of childhood trauma, 75% had a criminal history, 47% were residing in the custodial hospital unit during the study period, 82% had a history of violence, and 71% had a history of substance abuse. With respect to mental disorder diagnosis, most patients were living with a schizophrenia spectrum and other psychotic disorder (75%) followed by a substance-related and addictive disorder (55%) and neurodevelopmental or personality disorder (22%). Importantly, while the medical records that were reviewed did not disclose the reasons why patients were admitted to the study facility, records did include some information on patients’ history of admission to any provincial healthcare facility in their lifetime for a psychiatric issue. Among the 183 patients included in this study, 63% (n = 115) had been previously admitted for a psychiatric issue, 9% (n = 16) did not have a previous psychiatric admission, and 28% (n = 52) did not have any information on this admission history. Further, 15% (n = 27) had been previously admitted to a provincial healthcare facility for a suicide or self-harm event, 51% (n = 93) did not have a previous admission for this reason, and 34% (n = 63) did not have any information on this admission history.
Compared with patients with no record of suicide or self-harm events, those with a record were more likely to be younger (38.6 vs. 44.6 years), female (49% vs. 24%), experience childhood trauma (63% vs. 40%), reside in a custodial hospital unit (57% vs. 31%), have a recent record of hopelessness, helplessness, or depression (58% vs. 16%), and have poor impulse control (36% vs. 26%) and coping (21% vs. 9%). With respect to mental disorder diagnosis, patients with a record of suicide or self-harm events were more likely to be diagnosed with neurodevelopmental (27% vs. 14%), depressive (17% vs. 4%), and anxiety (11% vs. 3%) disorders, but less likely to be diagnosed with a schizophrenia spectrum or other psychotic disorder (68% vs. 86%).
Prevalence of Suicide and Self-Harm Events
Among the total sample (N = 183), 42% (95% CI [35, 49]) of patients had a lifetime history of self-harm and 24% (95% CI [18, 30]) had a record of recent self-harm thoughts or behaviors, whereas 37% (95% CI [30, 44]) had a lifetime history of suicidal behavior and 31% (95% CI [24, 37]) had a record of recent suicidal thoughts or behaviors (Table 2). Related to recent suicidal thoughts and behaviors, approximately 23% (n = 43) were thinking of suicide, 14% (n = 26) had made current plans surrounding suicide, and 14% (n = 25) had the means to act on their plan. Table 2 also presents prevalence estimates for suicide and self-harm status, disaggregated by select study variables. Overall, findings highlight that the incidence of non-fatal suicide and self-harm events is more common among patients possessing known correlates. Notably, as compared with patients without any involvement in the criminal justice system, patients with a criminal history or residing in a custodial hospital unit were more likely to have lifetime history of self-harm (49% and 59%), recent self-harm thoughts or behaviors (25% and 28%), lifetime history of suicidal behavior (40% and 52%), and recent suicidal thoughts or behaviors (32% and 35%).
Bivariate and Multivariate Regression
Lifetime History of Self-Harm Behavior
Bivariate logistic regression analyses indicate that nine variables (i.e., age, female sex, childhood trauma, criminal history, custodial hospital unit, hopelessness, neurodevelopmental disorder, bipolar and related disorder, and anxiety disorder) were significantly associated with lifetime history of self-harm (vs. no history). With respect to multivariate analysis, only one variable was independently associated with this outcome measure. Specifically, those residing in a custodial unit at the hospital (aOR = 2.47, 95% CI [1.07 – 5.72]) were more than twice as likely to have a record of self-harm history than those in a non-custodial unit.
Lifetime History of Suicidal Behavior
Bivariate logistic regression analyses indicate that eight variables (i.e., age, female sex, custodial hospital unit, hopelessness, substance abuse history, bipolar and related disorder, anxiety disorder, and trauma- and stressor-related disorder) were significantly associated with lifetime history of suicidal behavior (vs. no history). With respect to multivariate analysis, three variables were independently associated with this outcome measure. Specifically, patients who were female (aOR = 2.49, 95% CI [1.03 – 6.01]), resided in a custodial hospital unit (aOR = 2.65, 95% CI [1.10 – 6.39]), and had a recent record of feelings of hopelessness, helplessness, and depression (aOR = 2.77, 95% CI [1.05 – 7.28]) were more than twice as likely to have a lifetime history of suicidal behavior.
Discussion
This study provides greater insight into suicide and self-harm among adults receiving psychiatric inpatient services, contributing to findings from various countries and bolstering the evidence base within the Canadian context. Results indicated that a lifetime history of self-harm (42%) and suicidal behavior (37%), as well as recent self-harm (24%) and suicidal (31%) thoughts or behaviors, were comparable to the high prevalence rates found for these incidents in other studies involving psychiatrically hospitalized persons (Andover & Gibb, 2010; Horon et al., 2013; James et al., 2012; Jentz et al., 2022; Nijman et al., 1999). It is also likely that psychiatric inpatients involved in this study experienced multiple suicide and self-harm events (e.g., see Andover & Gibb, 2010; Horon et al., 2013). However, the medical records did not provide this type of information. Findings also suggest markedly higher prevalence of suicide and self-harm events among psychiatric inpatients in comparison with the general Canadian population (Public Health Agency of Canada, 2023). Though, this conclusion is tentative and future research would need to directly compare rates between psychiatric inpatients and the general population in Canada. It is also important to note that this study was conducted within the timeframe that a new policy and protocol for the assessment and management of suicide and self-harm was implemented at the hospital. Therefore, prevalence rates may be on the higher end due to greater monitoring and reporting by healthcare personnel during this period. Interestingly, inferential analyses were unable to reliably pinpoint a set of clinical factors associated with the suicide and self-harm measures (with exception to hospital unit), though this may be due to the limitations of using retrospective health data with insufficient detail.
While psychiatric and correctional populations are generally high-risk groups for suicide and self-harm (for review, see introductory section), individuals who are psychiatrically hospitalized and with criminal justice system involvement represent a particularly susceptible group. Indeed, previous research has found a greater prevalence and frequency of suicide and self-harm events among forensic patients (Galappathie et al., 2017; James et al., 2012), with some identifying alarmingly high rates of repeated suicide attempts in these patients (Horon et al., 2013). Results from this study substantiate this trend as it was found that patients with any prior involvement in the criminal justice system, and particularly those currently detained in the forensic unit, were more likely to have a record of (lifetime or recent) suicidal and self-harm thoughts or behavior. This may be related to the added distress of managing criminal matters, in addition to the associated personal and social consequences. We suggest that clinical teams be mindful of the elevated risk in these patients and consider more intensive assessment, monitoring, management, and support to adequately identify and address this risk. With that said, it is important to bear in mind the deleterious effects of environmental restrictions and controls (i.e., punitive approaches) on suicide attempts and self-harm among psychiatric inpatients (James et al., 2012), as well as the ineffectiveness of relying solely on formal observation to prevent suicidal and self-harm behavior without treating the underlying pathology and risk (Busch et al., 2003; Chammas et al., 2022).
We also suggest that strategies pertaining to the assessment and management of suicide and self-harm among psychiatric inpatients must account for the complex course and spectrum of these phenomena and, therefore, should be informed by the ideation-to-action perspective (Klonsky et al., 2018). In this case, future studies would benefit from pinpointing the dynamic and static mechanisms underlying the cognitive and behavioral phases of the suicidal and self-harm process according to the conceptualizations of ideation-to-action theories (Klonsky & May, 2015; O'Connor & Kirtley, 2018; Van Orden et al., 2010). This would help establish therapeutic targets across the suicide continuum. Related to this point, a growing body of research into suicide and self-harm among custodial populations has recently utilized the ideation-to-action framework, finding that factors associated with the development of suicidal thoughts differ from those related to the transition from suicidal thinking to behavioral enaction (Favril et al., 2020b, 2020c; Favril & O’Connor, 2021; Stoliker, 2020; Stoliker & Abderhalden, 2023; Stoliker et al., 2023) and, further, hypothesizing that shared risk factors likely play different roles in the cognitive versus behavioral spectrum of the suicide continuum (Stoliker, 2020; Stoliker et al., 2023). As such, the ideation-to-action perspective points out that prevention strategies must acknowledge the distinct processes underlying suicidal and self-harm thinking versus behavior. Indeed, a recent meta-analysis of studies in community settings highlighted that interventions that specifically target suicidal behavior (e.g., suicide safety planning) may be effective in altering one’s behavior but are unable to address suicidal ideation (Nuij et al., 2021).
A particular challenge for establishing effective strategies for the prevention of suicide and self-harm events among psychiatric inpatients relates to the complexity of identifying risk at the individual level, which has led to limited consensus on the preventive measures that should be in place in hospitals (Chammas et al., 2022). However, most would agree that a singular approach to suicide and self-harm prevention is inadequate. Chammas et al. (2022) highlighted a host of evidence-based approaches and emerging perspectives related to the prevention of suicide in psychiatric inpatients. This included the consideration of the underlying clinical dimensions of suicidality as therapeutic targets (e.g., anhedonia, psychological pain, hopelessness, aggression, impulsivity, emotion dysregulation, maladaptive decision-making, anxiety and agitation, etc.), implementing evidence-based suicide prevention training and practices for staff, securing the environment (i.e., design and safety features), as well as utilizing pharmacotherapeutic and psychotherapeutic interventions shown to reduce suicidality (for detail, see Chammas et al., 2022). Proper assessment of suicidal and self-harm thoughts and behavior is also critical, particularly for prompting appropriate responses to reduce risk (Andover & Gibb, 2010; Hubers et al., 2018). In any case, the most impactful prevention strategies will draw upon a combination of evidence-informed approaches. Further research is needed to investigate the application and effectiveness of such strategies to develop the best possible therapeutic approach for suicidal patients in psychiatric settings.
Strengths and Limitations
This study has several strengths and limitations. With respect to the former, the study was conducted at a public psychiatric hospital that provides rehabilitative services to justice-involved individuals and general community members across the province of Saskatchewan. This provided the unique opportunity to assess suicide and self-harm events for both forensic and civil psychiatric inpatients. This study also filled a major gap in terms of epidemiological data on suicide and self-harm among psychiatric inpatients within the Canadian context. Furthermore, conducting a retrospective review of medical records allowed for the inclusion of a sizable sample of patients and provided unique insight into the historical and recent health information of each patient. However, there are some drawbacks to relying solely on medical records for the purposes of research as the information is, of course, primarily intended for the administration of health services. In some cases, health documents used in this study contained limited information or were incomplete (e.g., missing data on suicide and self-harm assessments) and, while infrequent, even contained inaccuracies (e.g., for a single patient, some forms indicated a history of self-harm or suicidal behavior whereas others claimed no history). Therefore, it is important that clinical staff are aware of best practices for charting to ensure complete, detailed, and accurate information is available.
An important limitation to both research and practice is that the tools currently used to assess suicidal and self-harm thoughts and behaviors are not validated, nor do they provide critical detail. Specifically, the instruments are based on a limited number of items that do not fully capture the spectrum of suicidal and self-harm thinking and behavior (e.g., desire, plans, preparation, deterrents, means, motives, capability of inflicting self-harm, intent, frequency, chronicity, lethality, etc.). Some items even combine the cognitive and behavioral components, which is inconsistent with the ideation-to-action perspective. A lack of reliable tools for recognizing suicidal and self-harm risk may result in inaccurate assessments, leading to an underestimation or overestimation of risk and inappropriate case management (Wingate et al., 2004; see also Chammas et al., 2022). An added challenge lies within the fact that, without standardized tools, clinical staff may apply different understandings of suicide and self-harm. As such, the next phase of this research aims to implement and evaluate validated/standardized instruments that provide granular details on suicide and self-harm (e.g., see Horon et al., 2013) and, importantly, capture mechanisms theorized to underpin the suicidal and self-harm continuum. Furthermore, the data were not suited to capture levels of motivation and adherence to treatments, which could mitigate the risk of suicide and self-harm events. In addition, this study did not specifically assess the experiences of Indigenous Peoples, which is a notable limitation as rates of suicide are higher among Indigenous compared with non-Indigenous people in Canada (Kumar & Tjepkema, 2019). Future research into suicide and self-harm among psychiatric inpatients in Canada must therefore incorporate an Indigenous focus which may lead to important insights into culturally sensitive risk assessment, management, and treatment practices. Finally, while findings from our study mirror those from previous research into suicide and self-harm among civil and forensic psychiatric inpatients, results may have limited generalizability as the study population comprises patients with high-level and/or specific psychiatric needs that cannot be managed by other inpatient health services. As such, this population likely exhibits a higher level of morbidity as compared with those presenting or admitted to general hospital (including psychiatric units), acute inpatient mental health centres, or those receiving outpatient mental health services. Though, our data are unable to substantiate this claim. At any rate, findings should be interpreted with caution as they may only apply to settings that provide similar psychiatric services to civil and/or forensic inpatients.
Conclusion
With the high incidence of suicide and self-harm events among psychiatric inpatients, especially forensic patients, a focus on suicide and self-harm thoughts and behaviors represents a top priority for prevention and treatment in psychiatric settings. However, research to inform these efforts has been scarce, especially within the Canadian context. Although medical records provide valuable epidemiological data, they are unable to present the “full picture” as it relates to the development and progression of suicide and self-harm thoughts and behaviors. More research into suicide and self-harm among psychiatric (in)patients in Canada—especially which adopt a framework that acknowledges the complexity and course of suicidality and self-harm—will lead to more effective strategies for managing these issues in psychiatric settings.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
