Abstract
We investigated the effects of cause of death (COVID-19 with an underlying medical condition vs. without) and prolonged grief disorder status (PGD present or absent) on participants’ reported public stigma towards the bereaved. Participants (N = 304, 66% women; Mage = 39.39 years) were randomly assigned to read one of four vignettes describing a bereaved man. Participants completed stigma measures assessing negative attributions, desired social distance, and emotional reactions. Participants reported significantly stronger stigmatizing responses towards an individual with PGD (vs. without PGD) across all stigma measures. There was no significant difference in stigma based on cause of death; however, stigma was reported regardless of cause of death. There was no significant interaction between cause of death and PGD on stigma. This study supports the robust finding of public stigma being reported toward an individual with PGD, suggesting these individuals are at risk of public stigma and not receiving adequate bereavement support.
Introduction
The COVID-19 pandemic, which has caused more than seven million deaths worldwide (World Health Organization [WHO], 2024), is an immense bereavement event that has severely disturbed the experience of grief and bereavement (Harrop et al., 2021). COVID-19 deaths are associated with new bereavement conditions and potential risk factors including mandated separation during the dying process and disrupted mourning rituals, which are associated with an increased risk of psychological distress, poor mental health, and impaired functioning for the bereaved (Breen et al., 2023; Lee & Neimeyer, 2022; Neimeyer & Lee, 2022). These findings provide support for early pandemic predictions, that death, dying, and bereavement experiences would be negatively impacted for bereaved individuals and their communities through intense and prolonged grief responses (Eisma et al., 2021; Mayland et al., 2020). When grief responses are intense and prolonged, a bereaved individual may be more likely to develop prolonged grief disorder (PGD).
Characterized by significant functional impairment and an invasive and persistent preoccupation with and longing for the person who died, PGD is diagnosed when intense grief symptoms endure for six (WHO, 2019) or 12 months (American Psychiatric Association, 2022) after bereavement. In addition to the distress and functional impairment of the disorder itself, PGD is associated with a decreased quality of life, suicidality, and self-injury (Lichtenthal et al., 2011; Prigerson et al., 2021). Bereaved individuals are most likely to be diagnosed with PGD when the diagnostic criteria are met within 12 months of bereavement (Boelen & Lenferink, 2022). Before the COVID-19 pandemic, approximately 10% of individuals who experienced bereavement from a natural death were at risk for meeting PGD criteria (Boelen & Smid, 2017; Lundorff et al., 2017). However, research conducted during the pandemic’s early stages suggests that bereavement from COVID-19 is associated with an increased risk of PGD (see Eisma & Boelen, 2023; Stroebe & Schut, 2021).
Research performed with COVID-19 bereaved participants from China, the United Kingdom, and the United States showed high levels of anxiety, depression, functional impairment, and dysfunctional grief (Breen et al., 2021, 2022; Lee & Neimeyer, 2022; Neimeyer & Lee, 2022; Tang & Xiang, 2021). Further research conducted with COVID-19 bereaved participants from the United Kingdom showed they experienced restrictions in interacting with loved ones, loneliness, and social isolation (Selman et al., 2022a), and those bereaved by a close relationship who reported loneliness and social isolation also experienced increased grief and support needs (Selman et al., 2022b). Experimental studies conducted with Dutch participants showed higher grief levels were experienced by those bereaved by COVID-19 than natural, but not unnatural death (Eisma et al., 2021; Eisma & Tamminga, 2022). Other similar COVID-19 studies showed cause of death was not associated with higher grief levels, suggesting increased grief symptoms may be associated with the experience of being bereaved and the unique pandemic bereavement conditions rather than COVID-19 bereavement itself (Breen et al., 2023; Gang et al., 2022).
The establishment of PGD as a mental disorder in DSM-5-TR and ICD-11 has raised concerns from researchers and clinicians that a diagnosis might pathologize grief and contribute to the stigmatization of bereaved individuals (Breen et al., 2015; Dietl et al., 2018; Lichtenthal et al., 2011). Stigma occurs when stereotyping, separation, discrimination, and status loss arise in an environment of power imbalance (Link & Phelan, 2001). Two interacting forms of stigma are public stigma and self-stigma (Eisma et al., 2019; Livingston & Boyd, 2010). Public stigma occurs when stereotypical beliefs, prejudicial reactions, and discriminatory behaviors are endorsed by the general public towards a stigmatized group, and self-stigma occurs when an individual within a stigmatized group internalizes this stigma (Corrigan & Watson, 2002). In the context of mental illness, stigma results in poor self-esteem, low self-efficacy, and reduced motivation to seek mental health support (Corrigan, 2005; Vogel et al., 2007). In the context of bereavement, public stigma results in negative attributions of the bereaved, increased desired social distance from them, and negative emotional reactions towards them (Eisma et al., 2019).
Early research indicated an association between severe grief symptoms and negative reactions towards bereaved individuals without a PGD diagnosis, including family and friends telling the bereaved they were exaggerating their grief (Johnson et al., 2009). More recently, a vignette study with German participants showed there was no difference in stigma reported towards individuals with PGD symptoms who were diagnosed with PGD, than individuals who had PGD symptoms who did not have a diagnosis of PGD (Gonschor et al., 2020). Further experimental research with Australian, Dutch, and German participants showed more stigmatizing responses through negative attributions, stronger desired social distance, and increased emotional reactions towards individuals with PGD (vs. without PGD; Dennis et al., 2022; Eisma, 2018; Eisma et al., 2019; Gonschor et al., 2020; Zammit et al., 2023).
Previous pandemics have shown a common association between infectious viruses and stigma (Demirtaş-Madran, 2020), including during the Ebola epidemic where family members bereaved by the Ebola virus reported being stigmatized within their community (Kamara et al., 2017). This appears to be the case for the COVID-19 disease as well. Studies conducted with participants from the United Kingdom showed people diagnosed with long COVID-19 reported higher levels of stigma than those without a diagnosis (Pantelic et al., 2022), while an investigation into bereavement care showed some bereaved family members reported concerns about stigma from having COVID-19 listed as the cause of death (Pearce et al., 2021). Although previous research has investigated the effect of cause of death on public stigma (Eisma et al., 2019) the results have been mixed. A systematic review of bereavement expereinces showed individuals bereaved by suicide experienced more stigmatizing responses than those bereaved by natural causes, accidents, and illness (Logan et al., 2018a). Recent experimental studies showed no significant difference between stigma reported toward individuals bereaved by suicide, homicide and natural causes, or voluntary assisted dying/medical assisted dying and long-term illness (Eisma et al., 2021; Philippkowski et al., 2021; Singer et al., 2022). A recent Australian study showed that deaths from COVID-19 elicited comparable stigma to deaths from brain hemorrhage; however, both causes elicited high levels of stigma (Zammit et al., 2023).
In the context of cause of death and stigma, an additional consideration may be the role of an underlying medical condition (UMC), including diabetes, heart failure, obesity, chronic kidney disease, and liver cirrhosis with COVID-19, due to the increased risk of negative outcomes such as intensive care admission, hospitalization, and death (Venkatakrishnan et al., 2021). However, over-emphasizing COVID-19 deaths with UMC assigns blame, devalues those affected, creates a false sense of security for the remaining population, and corrodes epidemic control measures (Gronholm et al., 2021). For those bereaved by COVID-19, the grief experience may be complicated by layers of stigma regarding bereavement, the virus, UMC, and mental illness. Therefore, with new bereavement conditions and potential risk factors negatively affecting bereavement experiences during the pandemic, including COVID-19 death with UMC and increased prolonged grief responses, it is critical that stigma be mitigated to reduce negative experiences and community division (Gronholm et al., 2021). Consequently, more research is required to understand the facets of bereavement stigma, especially in the context of the current pandemic, to ensure stigma-reduction efforts are implemented to target critical factors that will reduce the stigma barriers and enable the bereaved to seek and receive adequate support.
The aim of this research was to investigate the effects of cause of death by COVID-19 with UMC (vs. without UMC) and PGD diagnosis (with PGD vs. without PGD), on participants’ reported public stigma towards the bereaved using an experimental vignette design. We hypothesized an interaction effect between UMC and PGD, such that stigma would be intensified for an individual with PGD who was bereaved by COVID-19 with an UMC. We also hypothesized participants would report greater public stigma toward an individual bereaved by COVID-19 with UMC than without UMC and greater public stigma toward a bereaved individual with PGD than without PGD.
Method
Research Design
The design was a fully randomized factorial 2 × 2 (COVID-19 death with UMC vs. without UMC; with PGD vs. without PGD), between groups, vignette-based experiment, investigating group differences in reported public stigma according to cause of death and prolonged grief. Multiple dependent variables of stigma were used: attributes of the bereaved (competent, warm, emotionally stable, dependent, sensitive), desired social distance from the bereaved, and emotional responses towards the bereaved (anger, fear, prosocial).
Participants
Sociodemographic Characteristics of Participants (N = 304) by Groups.
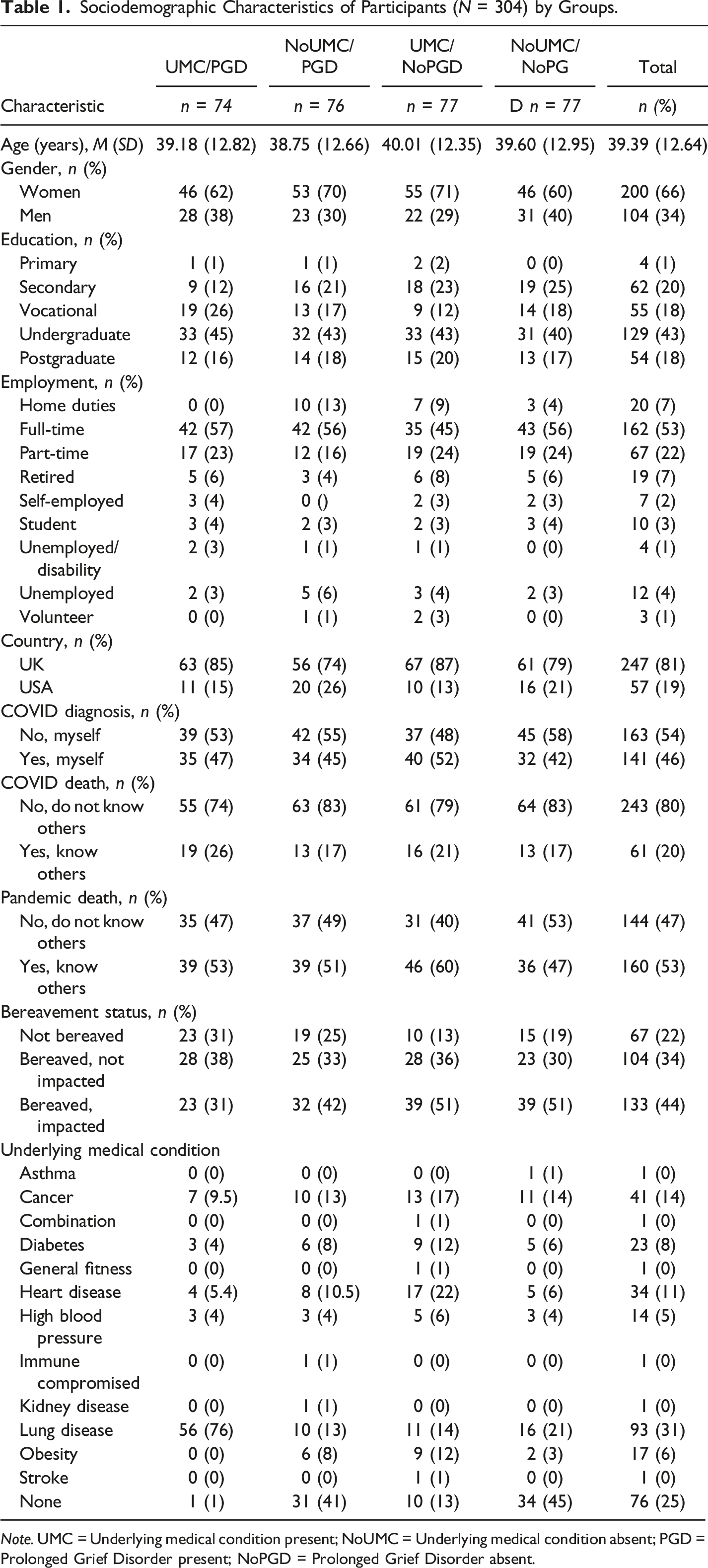
Note. UMC = Underlying medical condition present; NoUMC = Underlying medical condition absent; PGD = Prolonged Grief Disorder present; NoPGD = Prolonged Grief Disorder absent.
Measures
Demographic Questions
Participants reported their gender, age, highest education level, main employment, country of residence, personal bereavement experience and whether bereavement had a significant impact on them, their personal experience with COVID-19 bereavement, personal experience with pandemic bereavement, and personal experience with a COVID-19 diagnosis.
Vignettes
Content of Vignettes Varying Conditions of Cause of Death and PGD.
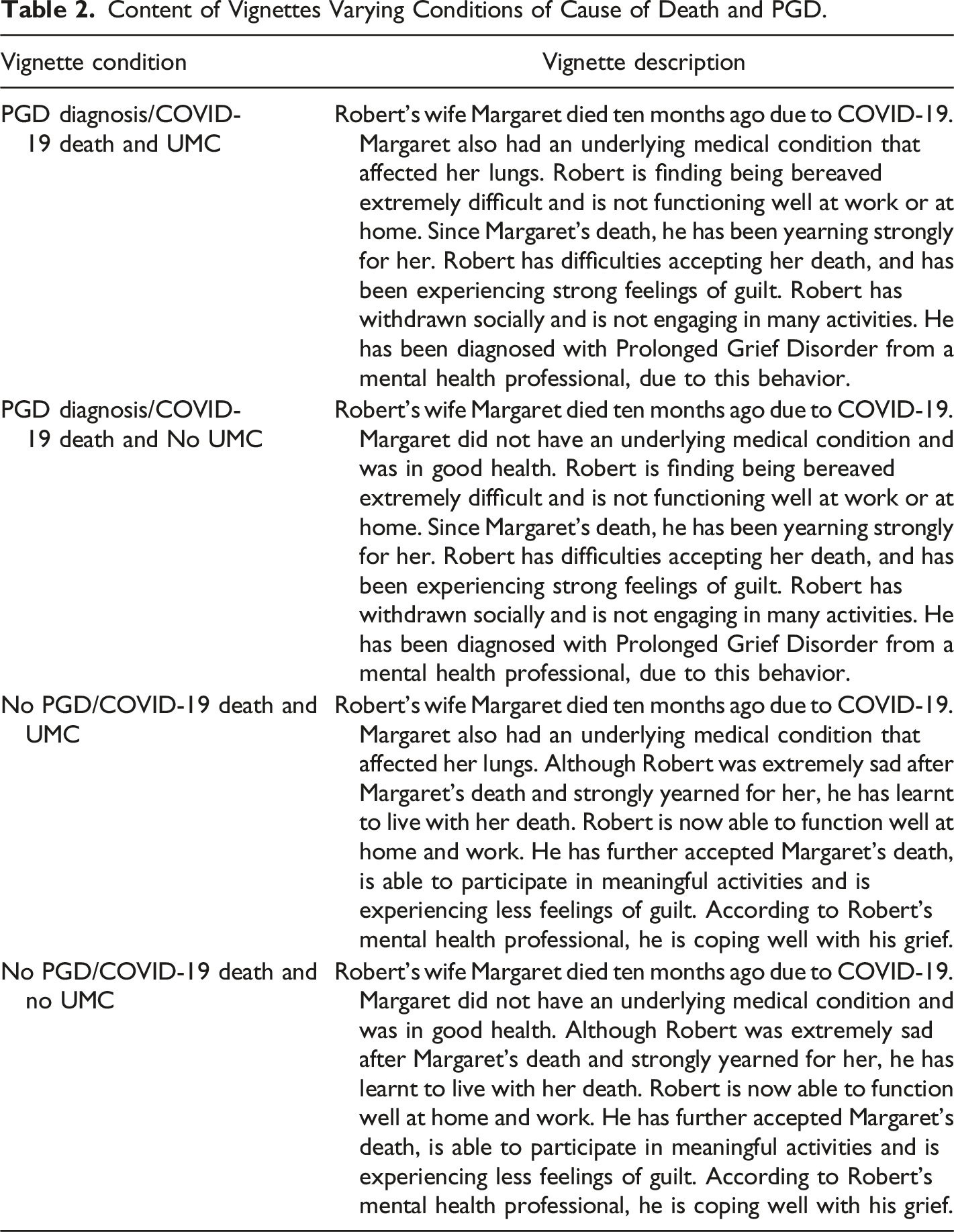

Public Stigma
Participants completed three self-report measures that assess three components of public stigma: attributions, desired social distance, and emotional reactions.
Attributions
The five Attributions items used were developed by Eisma (2018) and Eisma et al. (2021) based on Angermeyer and Matschinger’s (2003) research into public stigma and depression. Participants indicated their level of agreement with each attribute (competent, warm, emotionally stable, dependent, sensitive) assigned to Robert (e.g., “Robert is competent.”) using a 4-point Likert scale ranging from completely disagree (1) to completely agree (4) with higher scores indicating a higher level of the attribute. More stigmatizing attitudes are reported through higher scores on dependent and sensitive, and lower scores on competent, warm, and emotionally stable.
Social Distance Scale
To measure participants’ desired social distance from Robert and willingness to interact with him, the Social Distance Scale (SDS; Link et al., 1987) was used. The scale contains seven items (e.g., “how would you feel about working with someone like Robert”) and uses a 4-point Likert scale, ranging from definitely willing (1) to definitely unwilling (4), with higher scores indicating a larger desired social distance from Robert. In the current study, we adapted the measure to reflect more specific scenarios to the vignette by changing the word children to family member (e.g., “having your children marry someone like the person in the story” to “having a family member marry someone like the person in the story”) and using scoring of 1–4 rather than the original 0–3 (Penman et al., 2014). The SDS’s internal consistency was good in previous research (α = 0.85; Eisma et al., 2019), and in this study α = 0.92.
Emotional Reactions Scale
Emotional reactions toward Robert were measured using an adapted version of von dem Knesebeck et al.’s (2017) scale, with nine items assessing participants’ responses towards individuals with mental illness (Angermeyer & Matschinger, 2003). Eisma et al. (2019) developed an adapted scale by adding five items and removing one item to improve construct validity. This comprises 13 items across three subscales: anger (4 items, “I feel irritated”); prosocial emotions (4 items, “I take pity”); and fear (5 items, “I feel tense”). Participants rate each item on a 4-point Likert scale, from completely agree (4) to completely disagree (1), with higher scores indicating stronger emotional responses. The internal consistency for each subscale was demonstrated by Eisma et al. (2019; anger α = 0.82; pro-social emotion α = 0.75; and fear α = 0.85). In the current study, Cronbach’s alpha was good for each subscale (anger α = 0.91, prosocial emotion α = 0.83; and fear α = 0.84).
Manipulation check
The manipulation check was used to assess participants’ care with reading the questions and comprised two questions (“Did Margaret have an underlying medical condition?”; “Was Robert diagnosed with a mental health disorder?”).
Procedure
Ethics approval was obtained from the Human Research Ethics Office at Curtin University [HRE2021-0279]. Participants were recruited via the online Prolific platform which directed them to the Qualtrics survey where they were asked to provide consent via a check box. Each participant was randomly assigned to read one of four vignettes and asked to complete three measures to assess their response toward Robert. To conclude, participants completed the demographic questionnaire and manipulation check questions.
Data Analyses
All analyses were conducted using the Statistical Packages for the Social Science (SPSS; Version 27). The participant responses were collected from 21st June to 20th July, 2022 for 304 participants. There was no missing data. Listwise case deletions were conducted where there were not enough participants indicating gender other than woman or man to include in comparisons (n = 1).
Normality was assessed using histograms, boxplots, skewness, kurtosis, and Shapiro-Wilk tests. The histograms and boxplots indicated some univariate outliers, but none were extreme (>3 SDs) and all were retained because they were within the acceptable score range. The Shapiro-Wilk results indicated the data was not normally distributed; however, with the skewness and kurtosis statistics being mostly acceptable (z scores within ±1.96) and the large participant groups (>30), the MANOVA results could be meaningfully interpreted (Pituch & Stevens, 2016). Separate non-parametric tests (i.e., the Kruskall-Wallis ANOVA) were conducted as a measure of best practice, on variables with the most skewness and/or kurtosis Results showed statistical significance that supported the MANOVA’s interpretability. The maximum Mahalanobis Distance indicated multivariate outliers; however, Cook’s Distance indicated these were appropriate and were retained. Multicollinearity was assessed, with the correlations between dependent variables found to be appropriate. Scatterplots indicated the relationships between DVs were approximately linear. Box’s M was found to be significant at p < .001; however, with large sample sizes a MANOVA analysis is robust against this violation, and Levene’s Test of Equality of Error Variances was non-significant for all DVs except warm and sensitive, indicating equality of variance was met (Field, 2018).
To test the hypotheses, a two-way multivariate analysis of variance (MANOVA) was performed with a two-tailed significance test (α = .05). The independent variables included cause of death (COVID-19 death with UMC, COVID-19 death without UMC) and PGD diagnosis (with PGD, without PGD). The nine dependent variables were attributions (competent, warm, emotionally stable, dependent, sensitive), desired social distance, and emotional reactions (anger, fear, and pro-social). Significant MANOVA results were followed up with ANOVAs. Partial eta squared (
Results
Preliminary Findings
Prior to hypothesis testing, analyses of variance (ANOVAs) and Chi-Square tests were conducted to check participant randomization to vignettes and manipulation checks according to demographics. No significant differences were found between the four vignette groups based on: gender, χ2 (3, N = 304) = 3.30, p = .348; age, F (3, 300) = 0.14, p = .936; education level, χ2 (12, N = 304) = 10.07, p = .610; employment, χ2 (24, N = 304) = 24.46, p = .330; country of residence, χ2 (3, N = 304) = 5.48, p = .140; bereavement experience, χ2 (6, N = 304) = 11.43, p = .076; COVID-19 diagnosis (self), χ2 (3, N = 304) = 1.79, p = .618; COVID-19 death, χ2 (3, N = 304) = 2.38, p = .498, pandemic death, χ2 (3, N = 304) = 2.68, p = .443. These results indicate randomization was successful. For the manipulation check questions most participants correctly identified whether Margaret had an UMC (94%) and Robert’s PGD diagnosis (88%). As there was no difference in the resulting pattern between the full and partial samples, the findings from the full sample were reported. The nine DVs’ normality assumptions were assessed and found to be appropriate. The MANOVA’s statistical assumptions were assessed and showed they were met appropriately.
Main Findings
Means, Standard Errors, and Confidence Intervals for Stigma Variables (N = 304).
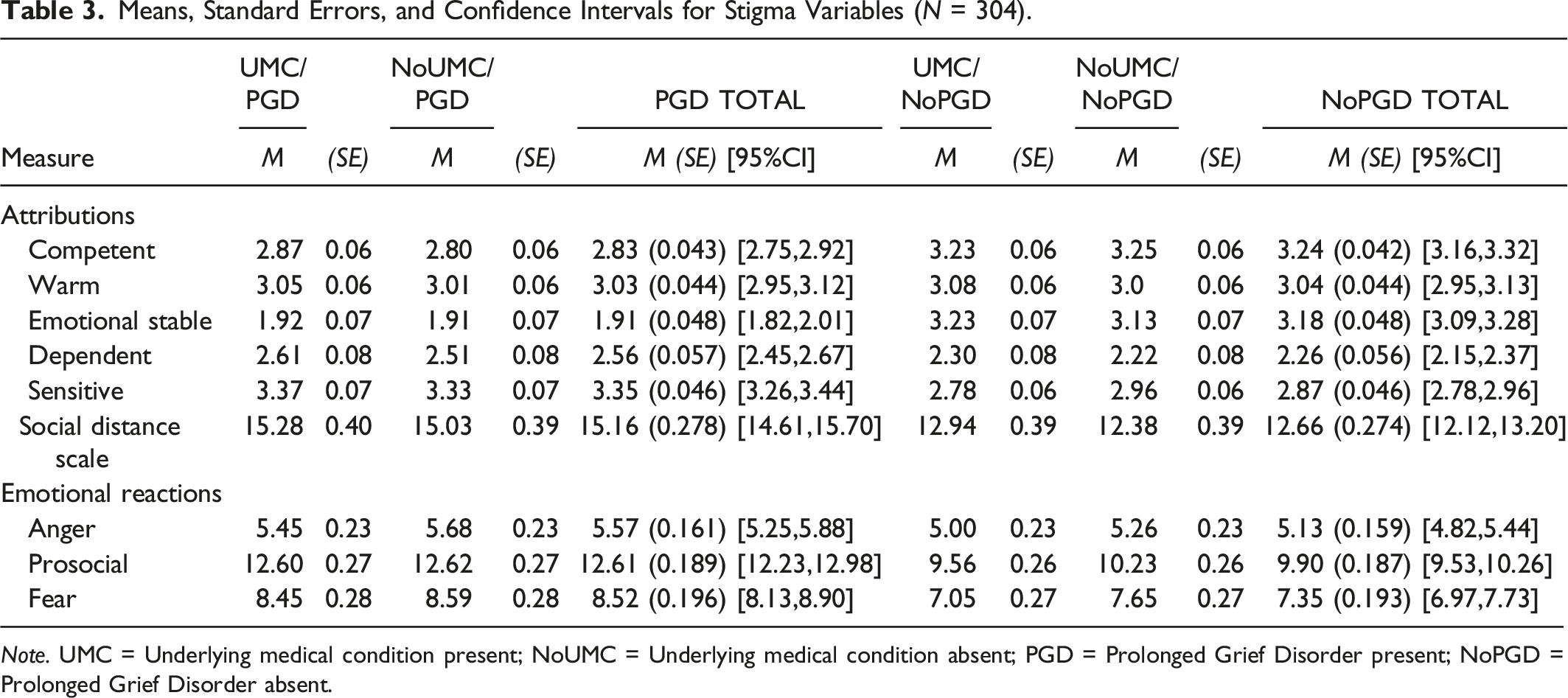
Note. UMC = Underlying medical condition present; NoUMC = Underlying medical condition absent; PGD = Prolonged Grief Disorder present; NoPGD = Prolonged Grief Disorder absent.
Contrary to our prediction, there was a non-significant interaction between cause of death (COVID-19 death with UMC/without UMC) and PGD diagnosis (with PGD/without PGD). There was a non-significant main effect for cause of death, F (9, 292) = 1.35, p = .213,
A large and significant main effect was found for PGD diagnosis, indicating that participants assigned more stigma to an individual with PGD than without PGD, F (9, 292) = 50.72, p < .001,
Discussion
This study investigated the role of UMC and PGD on public stigma toward an individual bereaved by COVID-19, using a sample of 304 English-speaking participants from the United Kingdom and the United States. Consistent with our hypothesis, participants reported significantly more public stigma towards a bereaved individual with PGD than without PGD. However, no significant interaction was found between cause of death and PGD diagnosis, and participants reported similar levels of public stigma towards individuals bereaved by COVID-19 regardless of UMC status.
Participants perceived the vignette individual with PGD as less competent and less emotionally stable than the vignette individual without PGD. Participants also reported greater desired social distance, more pro-social emotions (e.g., I am concerned about this person), and more fear toward the individual with PGD than without. This corroborates other research finding a significant main effect for PGD diagnosis on public stigma (Dennis et al., 2022; Eisma, 2018; Eisma et al., 2019; Gonschor et al., 2020), and indicates the general public may simultaneously experience feelings of desiring increased social distance, fear, and wanting to help the bereaved. This stigma finding may also indicate the general public sees the prolonged grief response as being the bereaved person’s responsibility, which aligns with mental illness stigma research showing that attributing personal responsibility for a mental illness was the most significant predictor of stigma and desired social distance (Feldman & Crandall, 2007).
In contrast to previous research (Dennis et al., 2022; Eisma, 2018; Eisma et al., 2019; Gonschor et al., 2020), participants reported similar levels of anger towards the vignettes’ individual regardless of PGD, with high mean anger scores for both groups. This suggests that it may be bereavement status that is associated with participants reporting high levels of anger toward the bereaved rather than PGD status. Indeed, research shows bereavement status alone (without a PGD diagnosis) generates high anger scores (Philippkowski et al., 2021). Also contrasting with previous research (Dennis et al., 2022; Eisma, 2018; Eisma et al., 2019; Gonschor et al., 2020), participants attributed similar levels of warmth towards bereaved individuals regardless of PGD status. This may be explained by the samples’ experience with bereavement. Almost half of our participants (44%) reported bereavement experiences rated as significantly impacting. While most comparative studies did not measure bereavement experiences, 24% of Dennis et al.’s (2022) sample reported significantly impacting bereavement, which may account for the differences in reported warmth between studies. Personal experience with grief and contact with bereaved individuals can provide individuals a better understanding of bereavement (Costa et al., 2007; Jorm & Oh, 2009), which may increase reported warmth. However, personal bereavement experience does not appear to be associated with intentions to offer bereavement support (Logan et al., 2018b) and therefore does not mean it will prevent stigmatizing responses.
Overall, participants reported more public stigma towards a bereaved individual with PGD than those without PGD. They assigned more negative attributes, desired greater social distance, and were more fearful of the individual with PGD, while simultaneously reporting a desire to help them. This implies that although people experience a desire to help the bereaved their feelings of fear may be stronger. This could potentially be due to an individual’s bereavement experience being too confronting for people to bear witness to and causing fear, therefore, the increased desired social distance may assist in reducing fear. For the bereaved individual, experiencing others as being fearful of them and socially distancing from them may create increased feelings of distress and isolation during their grief. This may leave a bereaved individual with PGD at risk of not receiving appropriate support due to stigma effects preventing them from seeking support, blocking potential supporters from offering help (Corrigan, 2005), and believing they do not require mental health support (Lichtenthal et al., 2011).
The non-significant cause of death results contrasted with our prediction, as the mean stigma scores were high for both groups, suggesting stigma was reported towards all people bereaved by COVID-19 regardless of UMC. It is possible that participants perceived a death with UMC as more similar to a natural death than a death by COVID-19 alone (Australian Institute of Health and Welfare, 2022). As previous research has shown less stigma reported towards those bereaved by natural deaths than COVID-19 and unnatural deaths (Eisma et al., 2021), this suggests participants may have perceived death by COVID-19 with UMC as a more natural death and therefore, not more stigmatizing than COVID-19 without UMC. It is also possible that no stigma differences were found as participants may hold only the deceased person responsible for their underlying medical condition rather than the bereaved, as previous research has shown that attributing personal responsibility for a mental illness was a significant predictor of stigma and lead towards desiring social distance (Feldman & Crandall, 2007), but without a comparison group who are bereaved by non-disease causes, this cannot be confirmed.
Strengths, Limitations, and Future Directions
The strengths of this research include its robust experimental design using manipulation checks, randomization of participants to vignettes, and multiple stigma measures to optimize the reliability and validity of findings. Although this study is experimental, it is also cross-sectional, and therefore inferences can only be made about the factors that cause bereavement stigma based on the experimental conditions of this study and not about the progression of stigma over time. Therefore, longitudinal research is needed to assess how participants’ perceptions of bereaved individuals develop and change over time, and what social, experiential, and psychological factors are implicated in the development, maintenance, and alteration of these perceptions.
The findings must also be considered alongside limitations to the sample, which comprised mainly highly educated women. While this demographic composition is typical across bereavement research, generalizability of the findings may be potentially limited to this population. The participants were from multiple countries which may affect bereavement stigma due to social and cultural factors; however, similar results were shown when compared to previous studies with varying western cultures, genders, and education levels (Dennis et al., 2022; Eisma, 2018; Eisma et al., 2019; Gonschor et al., 2020; Singer et al., 2022). The stigma measures were developed for mental illness and not bereavement stigma. Although PGD is a mental illness and these measures have been used in several PGD studies, they may not comprehensively measure bereavement stigma, therefore, developing a new measure should be considered to potentially assess bereavement stigma more comprehensively. Although we used measures used in previous similar studies to enable comparison of results with these studies, it is worth noting that the PGD vignettes describe the person with PGD as not functioning well at work or at home, which might have influenced participants’ ratings concerning the attributes of the bereaved, desired social distance from the bereaved, and emotional responses towards the bereaved). Additionally, cause of death (e.g., violent killings) is associated with a greater likelihood of PGD than non-violent causes (Djelantik et al., 2020), yet studies disclosing grief severity (Eisma et al., 2019) do not find such a pattern with regards to suicide. It could be that cause of death may be used by participants to infer grief levels, which may result in stigma.
There are also several factors not assessed in this study that may provide further insight into bereavement stigma. For example, more stigma is reported towards individuals who are bereaved in early adulthood than late adulthood (Philippkowski et al., 2021) and a greater social distance is desired from bereaved men than women (Gonschor et al., 2020); as such, examining these factors will be important for future work. Future vignette research could manipulate additional variables to examine the role of other factors in bereavement stigma. The UMC could also be manipulated to examine how different conditions affect stigma. Some medical conditions (e.g., obesity) are more stigmatized than others and may therefore generate greater bereavement stigma if they are implicated in the cause of death (Pearl & Schulte, 2021). Furthermore, manipulating whether the deceased had been diagnosed with long COVID-19 could be insightful, as individuals diagnosed with long COVID-19 experience more stigma than those without a diagnosis (Pantelic et al., 2022). A key future direction will be to investigate the mental health impacts of public stigma upon individuals bereaved by COVID-19 and whether it leads to self-stigma; so that the negative effects of self-stigma can also be mitigated.
Implications
The results of this study may be used to inform the development and provision of targeted support for COVID-19 bereaved individuals. Stigma towards bereaved individuals, particularly those experiencing PGD, may prevent the bereaved from seeking support and deter potential supporters from helping them. With the growing number of people bereaved during the pandemic, the number of people experiencing grief and potentially developing PGD is growing. Given that bereaved individuals who are most at risk of PGD may also be most at risk of stigma, active outreach intervention is required to ensure they are adequately supported. For example, healthcare settings could assess all bereaved individuals to determine if they have PGD symptoms, the level of bereavement care they require, and refer them to care that is available and accessible to them (Lichtenthal et al., 2024). At the same time, there is a need to implement stigma reduction programs to minimize stigma development.
Conclusions
Overall, these findings show that COVID-19 deaths are potentially stigmatizing regardless of UMC, with high levels of public stigma reported by both groups. Furthermore, this study supports the robust finding that bereaved individuals with PGD are at risk of stigmatization and this finding is generalizable across Western cultures (Dennis et al., 2022; Eisma, 2018; Eisma et al., 2019; Gonschor et al., 2020). With an increased potential risk of developing prolonged grief during the pandemic (Eisma et al., 2021), further research is required to better understand public bereavement stigma and how to increase help-seeking behaviors of the bereaved and assist with appropriate support being offered to meet their needs.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The first author was supported by a Curtin Strategic Scholarship.
