Abstract
Aims: Most studies on the impact of COVID-19 have shown a decrease or no change in unassisted suicide rates, but effects on assisted suicide have not been studied. We aimed to estimate the association between the COVID-19 pandemic and both types of suicide. Methods: Between 2017 and 2021, 1280 assisted suicides and 535 unassisted suicides were recorded in three Swiss cantons. We conducted descriptive and time series analyses on monthly suicide rates, categorized by gender. Results: Among women, a decrease in assisted suicide rates was found during the acute phases of the pandemic. Among men, assisted suicide rates increased gradually from the onset of the pandemic. Regarding unassisted suicide rates, no significant change was observed in women, while in men, there was a decrease, which was larger at the end than at the onset. Conclusions: COVID-19 had contrasting effects on assisted and unassisted men and women suicide rates.
Introduction
In Switzerland in 2021, 1005 people died by unassisted suicide and 1391 by assisted suicide (Suicide et Suicide Assisté | Obsan, nd). In 2000, the rate of unassisted suicide (19.8 per 100′000 inhabitants) in the country was one of the highest in Europe but it has fallen dramatically since then and is now close to the European average (11.6 per 100'000 inhabitants) (Suicide et Suicide Assisté | Obsan, nd). Conversely, the rate of assisted suicides in Switzerland increased sharply from 1.5 per 100′000 inhabitants in 2000 to 15.8 per 100′000 in 202 (Suicide et Suicide Assisté | Obsan, nd). Assisted and unassisted suicides 1 have however different age and gender distributions. Unassisted suicides are among the most common causes of premature death after cancer and circulatory diseases and the leading cause of death among young people (Suicide et Suicide Assisté | Obsan, nd), and their rates are higher for men than for women for all ages (Office fédérale de la statistique, n.d.-b, n.d.-a), with a mean rate of 17 for men versus 6.3 for women in 2021 in Switzerland (Suicide et Suicide Assisté | Obsan, nd). On the other hand, assisted suicides have a ratio of 10 men to 13 women with the highest number of deaths occurring among those aged over 75, this age group increasing according to a recent study (Montagna et al., 2023).
The COVID-19 pandemic had major effects on many levels (e.g., economic, social, health) and its consequences on factors influencing mental health (e.g., social isolation, employment status or fear of disease) have been extensively studied (Aknin et al., 2022; Calati et al., 2021; Calderon-Anyosa & Kaufman, 2021; Eguchi et al., 2021; Isumi et al., 2020; Kahil et al., 2021; McIntyre et al., 2021; OFSP, nd; Steeg et al., 2021; Zalsman et al., 2020). In Switzerland, the Federal Statistical Office (OFS) published a report showing that the first lock-down was associated with a reduction in stress and greater satisfaction with life, but that as time went on, the population began to show signs of fatigue and other distress (BAG, nd). On the international level, at the beginning of the pandemic, experts and media warned against its major potential impacts on mental health and on suicidal behaviors (Bristol, nd; Kachaner, 2022). However regarding unassisted suicides, the majority of available publications report stability or even decrease in suicide rates compared to prepandemic years (Appleby, 2021; Botchway & Fazel, 2021; Efstathiou et al., 2021; Pathirathna et al., 2022; Pirkis et al., 2021, 2022; Webb et al., 2022). Japan is a noteworthy exception (Eguchi et al., 2021; Nakanishi et al., 2022; Radeloff et al., 2021; Sakamoto et al., 2021; Tanaka & Okamoto, 2021), where an increase in unassisted suicides was shown in all women, in young men and in men over the age of 80 (Eguchi et al., 2021; Nomura et al., 2021), suggesting that these sectors of the population have been disproportionately affected by the social and economic consequences of the pandemic (such as increased unemployment and domestic violence).
Suicide is a complex phenomenon with many determinants and previous pandemics or disasters showed a “honeymoon effect” with an initial decrease in suicides followed by a delayed increase (BAG, nd; Tanaka & Okamoto, 2021). Research should therefore continue even if the feared “suicide tsunami” did not happen.
On the other hand, possible influence of COVID-19 on assisted suicides or euthanasia 2 has hardly been covered by the media and research on this topic is scarce, with only a few articles on Canadian physician-assisted suicide data. These data showed that the acute phase of the pandemic exacerbated existing problems that is the provision of assisted suicides and limited access to applicants (Oliver et al., 2021; Wiebe et al., 2021, 2022). Regarding Switzerland, we did not identify any study on possible impact of the pandemic on assisted suicides. “EXIT Suisse romande”, 3 one of the major providers of assisted suicides in French-speaking Switzerland, reported a mandatory slowdown of its activities from March to May 2020 but increased overall activity in 2020 compared to 2019 and a sharp increase in the number of people not registered with EXIT who wanted to be helped quickly (EXIT Association pour le Droit de Mourir dans la dignité, 2021). For the year 2021, new memberships increased again as well as the number of assisted suicides performed from 369 in 2020 to 421 in 2021 (EXIT Association pour le Droit de Mourir dans la dignité, 2022), but no data on the evolution of men and women assisted suicides were published. This lack of both international and national research is surprising. Studying the changes in assisted suicide rates among men and women during the COVID-19 pandemic is crucial due to the consistent increase in these rates over the years, with women being more represented. Understanding whether the pandemic has altered this trend provides insight into its impact on end-of-life decisions and societal factors. As aforementioned older people are among the most vulnerable groups for unassisted suicides (especially men) and assisted suicides (especially women (28)) and they were deeply impacted by social isolation due to restrictions. Furthermore, the lack of resources to deal with the pandemic crisis has been associated with debates on some lives being more important than others. Older people may have felt oppressed and relegated to the background (Salinas Mengual, 2021). Knowing this, one might wonder whether the COVID-19 pandemic could have led elderly individuals to resort to assisted suicides. In Switzerland, the Swiss Federal Statistical Office publishes official data on the number and rates of suicides, the data being available until 2021 (Office fédéral de la statistique, 2022). However, to date there is no research that examined monthly evolution of suicides in the pandemic era.
In this context, we aimed to estimate the impact of COVID-19 on assisted and unassisted suicide rates by examining the monthly evolution of women and men deaths by assisted suicide in canton of Vaud, Geneva and Fribourg and by unassisted suicide in canton of Vaud from 2017 to 2021, and relating them to the COVID Stringency Index for Switzerland (KOF Stringency Indices, nd). We hypothesized a pandemic-related decrease in unassisted suicides and increase in assisted suicides with no gender-related difference. We chose to analyze the data separately by sex because research has consistently shown that there are gender-specific patterns in suicide rates, with differences in factors such as methods used, underlying mental health conditions, and social determinants. Given this evidence, we found it pertinent to examine how these sex-specific patterns may manifest during the pandemic.
By understanding how COVID-19 has influenced suicide trends, we can better prepare to deal with future public health crises. This research can guide the development of strategies and policies aimed at supporting the mental health and well-being of the population during such crisis periods.
Material and Methods
Data Source
This study was carried out with the collaboration of the University Center of Legal Medicine, Lausanne-Geneva, (“Centre universitaire romand de médecine légale” (CURML)), located on the two university hospital sites of Lausanne and Geneva. Regarding assisted suicides, the CURML Lausanne had complete data for the cantons of Vaud and Fribourg, and the CURML Geneva had complete data for the canton of Geneva, which corresponds to 1280 assisted suicides between January 01, 2017 and December 31, 2021. For unassisted suicides and due to incomplete data, we were only able to include data from the canton of Vaud between January 01, 2017 and August 31, 2021 (n = 535). We decided not to include data from canton of Geneva because data were not yet available for 2021, and we did not use data from canton of Fribourg because as of 2020, collaborations had changed and the CURML no longer had all reports of suspicious or violent deaths from the canton of Fribourg.
In Switzerland, in the case of a suspicious or violent death (including deaths by assisted suicide), the forensic pathologist is mandated by the public prosecutor’s office or the police and performs an at-the-scene examination. If, after the scene examination, the manner of death remains unclear, the public prosecutor orders a medicolegal autopsy. The role of the forensic pathologist is to determine the cause of the death. The determination of the manner of death (in the context of this study suicide/accident/natural death) is the prosecutor’s duty. “Unassisted suicide” deaths are defined according to the following criteria: (1) cases in which the scene investigation and/or the lesion mechanism is strongly suggestive of suicide in the absence of signs of intervention by third party (e.g. hanging, isolated gunshot wound to the head with the weapon found next to the body, suicide note), (2) strong anamnestic data (person known for depression, and/or history of suicide attempts), (3) people known for difficult life events for example job loss, divorce, etc. where the lesion mechanism is strongly suggestive of suicide. In cases of intoxication or drowning, suicide will be only considered if a suicide note is found or in presence of a history of previous attempts.
In Swiss law, three conditions are necessary to access assisted suicide: firstly, the person desiring death must carry out the fatal act. Secondly, this person must possess decision-making capacity. Finally, the assisting individual’s behavior must not be motivated by selfish reasons. The acceptance criteria for the EXIT association are as follows: being a member of the association, having one’s primary residence in Switzerland, being of legal age, possessing decision-making capacity, and either suffering from an incurable illness, intolerable suffering, or disabling polypathologies related to age.
Counts of suicide cases were aggregated separately by month for both types of suicide and for men and women. Monthly suicide rates for 100′000 inhabitants were then computed as the ratio between monthly suicide cases and monthly population data from the federal statistical office (STATPOP, OFS.) The rate was calculated using the respective population of the concerned canton(s).
We also used the Stringency index which measures the level of lockdown social restrictions. These are structural measures implemented to cope with the evolution of the pandemic and serve as a kind of indicator of the pandemic’s virulence. The values range from zero (=no measures) to 100 (=full lockdown). It is a composite measure based on 9 indicators: school closing, workplace closing, cancellation of public events, restrictions on gatherings, closure of public transport, stay-at-home requirements, restrictions on internal movement, international travel controls and public info campaigns. The Stringency index was rated by the KOF Swiss Economic institute (KOF Stringency Indices, nd). Daily data are available at the national level and for all individual 26 cantons of Switzerland from January 2020 onwards. Data were aggregated by month (average of daily data) and values of zero were attributed to months preceding January 2020.
The study protocol was approved by the Cantonal Commission on Ethics in Human Research (CER-VD) (authorization number ID, 2022-01,351). According to its decision, individuals who had previously refused the use of their personal data for research purposes through the general consent used in university hospitals of Lausanne, Fribourg and Geneva were removed from the database (n = 35 for assisted suicides and n = 10 for unassisted suicides).
Analyses
The months between January 2017 and February 2020 were considered as the period before the COVID-19 pandemic, and the months between March 2020 and December 2021 were considered as the COVID-19 pandemic period. First, we performed a descriptive analysis by presenting the characteristics of the individuals included in the study (number of suicides per month, suicide rate per month, mean age, age categories for men and women). Then, autoregressive integrated moving average (ARIMA) time series analyses were performed on monthly suicide rates separately for both type of suicides for each gender. Unlike traditional regression models, ARIMA models consider the dependence between observations and trends (i.e., changes in levels) over time. They allow for the modeling of three parameters (p, d, q): autoregression (p), which is the correlation between the current and previous chronological measurement points, integration (d), which is the difference between the current and previous chronological measurement points, and moving average (q), which is the correlation between the current error term and the previous error terms. These parameters can be in the non-seasonal or seasonal part of the model. One of the conditions for applying ARIMA models is the stationarity of the observations, meaning that the mean and variance of the observations are constant over time. To achieve stationarity, it may be necessary to use a difference model or adjust for deterministic trends, and/or to perform a logarithmic transformation.
The time series analyses were performed in several steps using SPSS 27 software. First, we evaluated the mean and variance of monthly suicide rates before the COVID-19 outbreak, between January 2017 and February 2020, by examining graphical representations of temporal trends. We then fitted a series of ARIMA models to determine the order of the non-seasonal and seasonal parameters p, d, and q. We also tested for deterministic trends by including the time variable (in months from the start of the series) in the models. The parameters’ order was selected based on the graphs of the autocorrelation function (ACF) and the partial autocorrelation function (PACF) and the values of the Bayesian Information Criterion (BIC). To verify whether any of a group of autocorrelations of the time series were different from zero, we used the Ljung-Box-Q test, which should not be highly significant (p > .20). We also visually inspected the residuals of the models.
These parameters were then used as the basis for fitting models estimating the effect of COVID-19 on the entire time series. Three separate models were fitted for both type of suicides and for men and women. Model 1 tested the “step” effect of COVID-19 (the variable was coded zero before March 2020 and 1 from March 2020 onwards), that is, whether there was a difference (i.e. step) in suicide rates between the pre- and the post-COVID-19 periods. Model 2 tested the “ramp” effect of COVID-19 (the variables was coded as the time in months after the onset of COVID-19 (March 2020) and coded zero for the pre-COVID-19 period from January 2017 to March 2020), that is, whether there was a gradual increase/decrease (i.e. ramp) from the onset of COVID-19 to the end of the COVID-19 period. Finally model 3 tested the effect of the Stringency index over the entire period (January 2017 to December 2021), that is, whether the stringency index was associated with unassisted suicide rates or assisted suicide rates.
Results
Descriptive Analyses
Regarding assisted suicides, between January 2017 and December 2021, 1280 deaths (60.5% women and 39.5% men) were recorded in the cantons of Vaud, Geneva, and Fribourg. The mean (standard deviation) monthly suicide rate per 100,000 inhabitants was 1.56 (0.55) among women and 1.06 (0.39) among men. The mean age (standard deviation) was 80.52 (12.13) for women and 79.39 (11.19) for men and for both genders 89% of individuals were >65 years old.
Monthly Suicide Counts and Rates From 2017 à 2021.
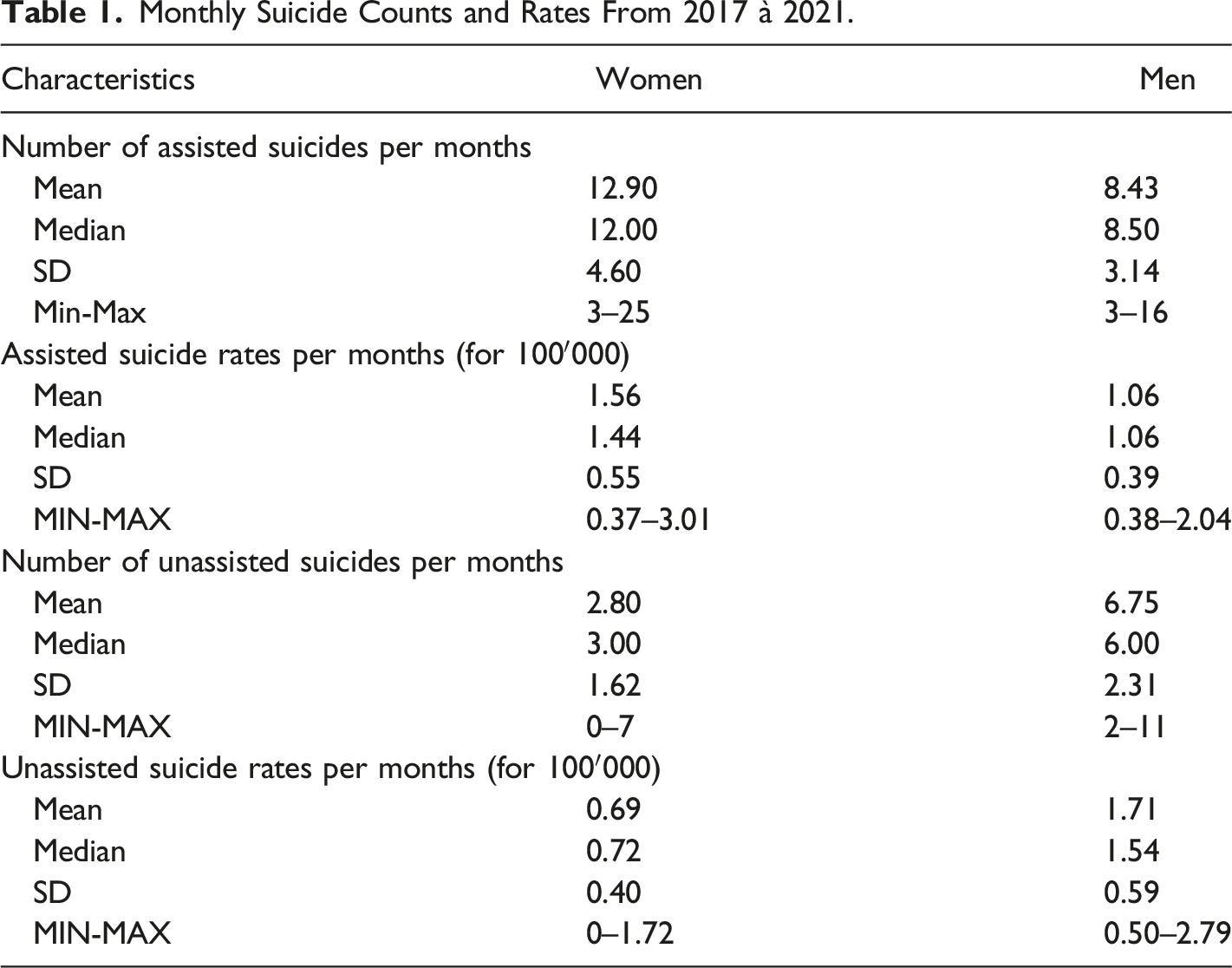
Age and Gender Characteristics of Two Types of Suicide (2017-2021).
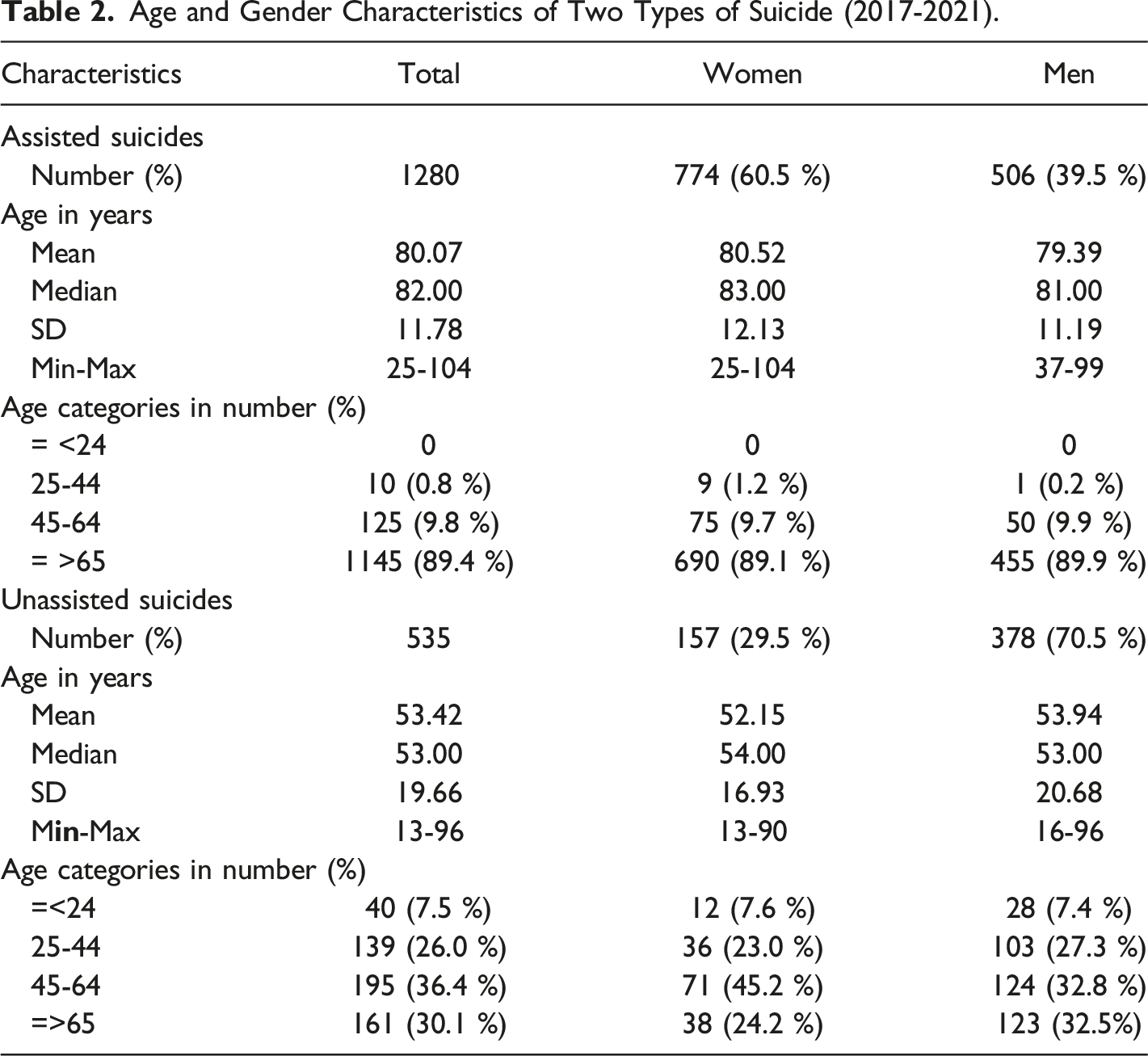
Associations with COVID-19 and Stringency Index
ARIMA Models 4 .
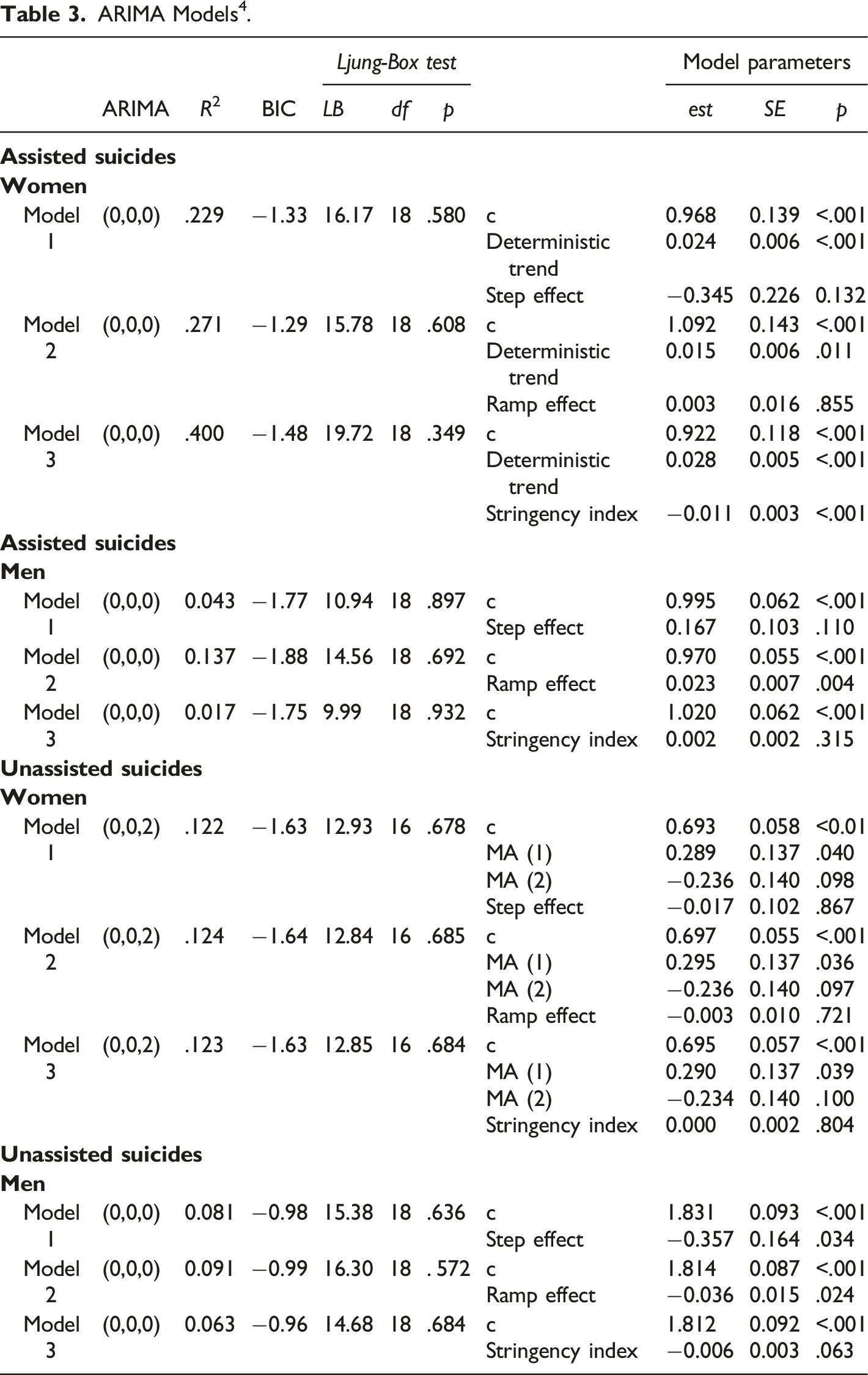
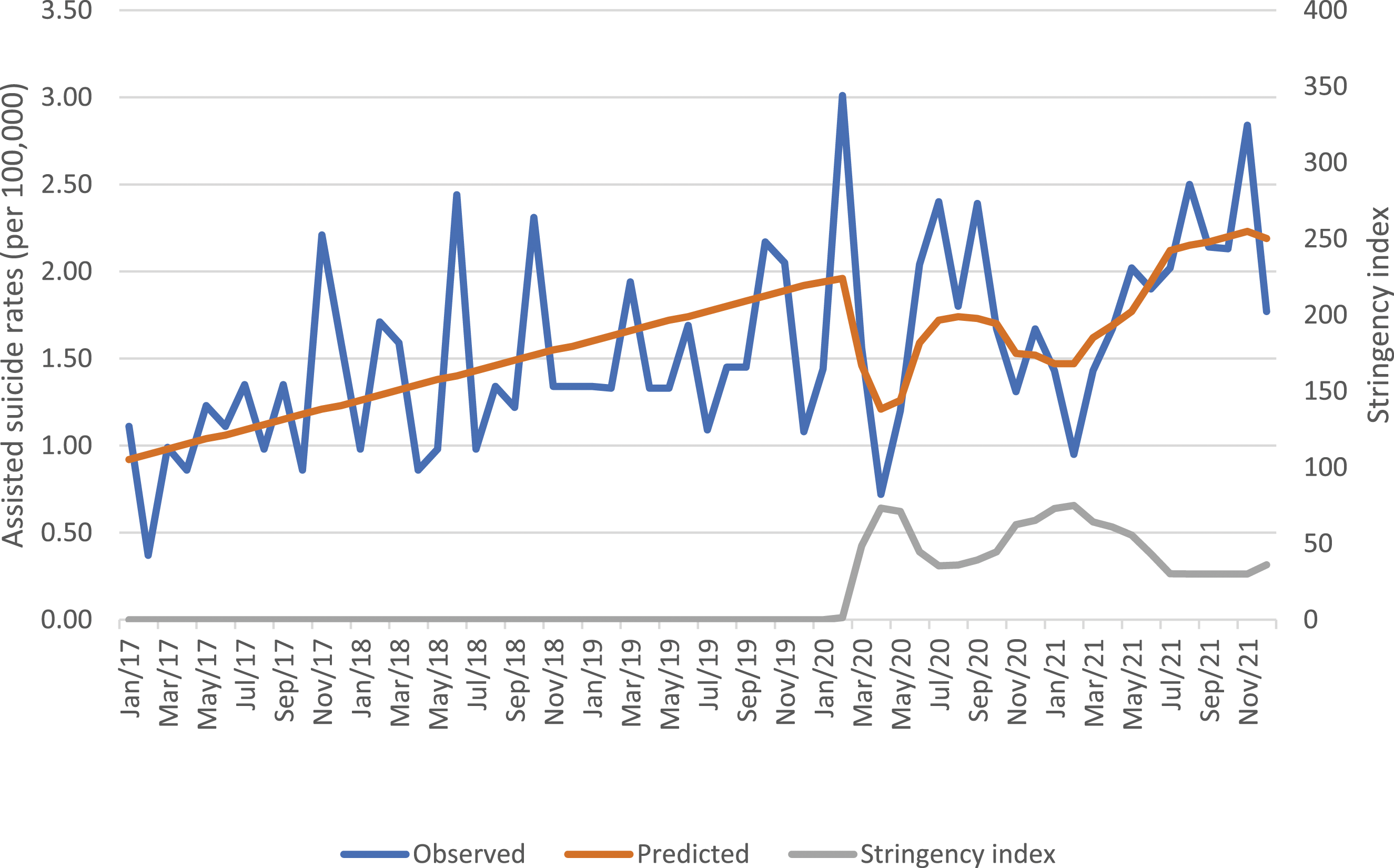
Association between stringency index and assisted suicide rates, women.
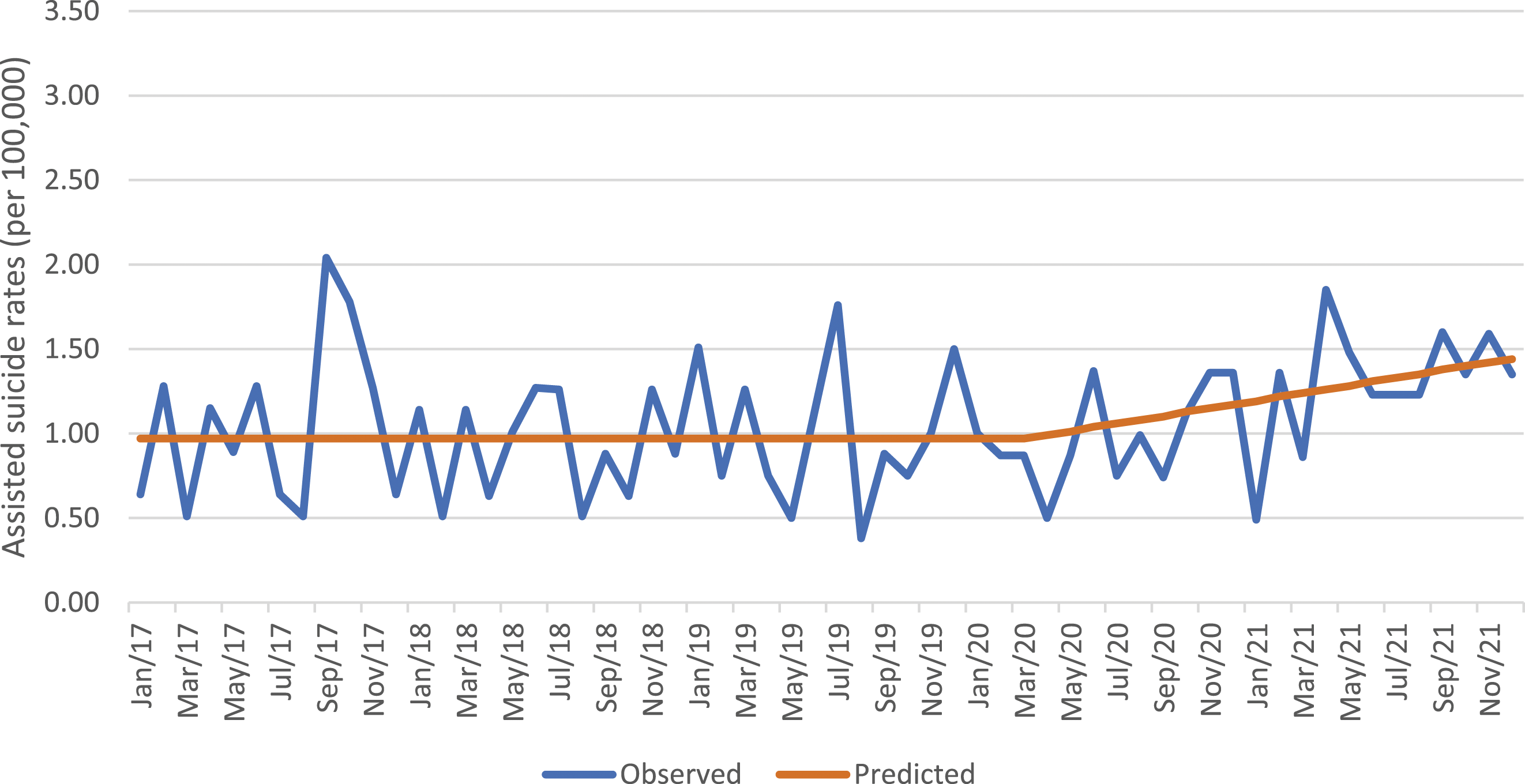
« Ramp » effect of COVID-19, assisted suicide rates, men.
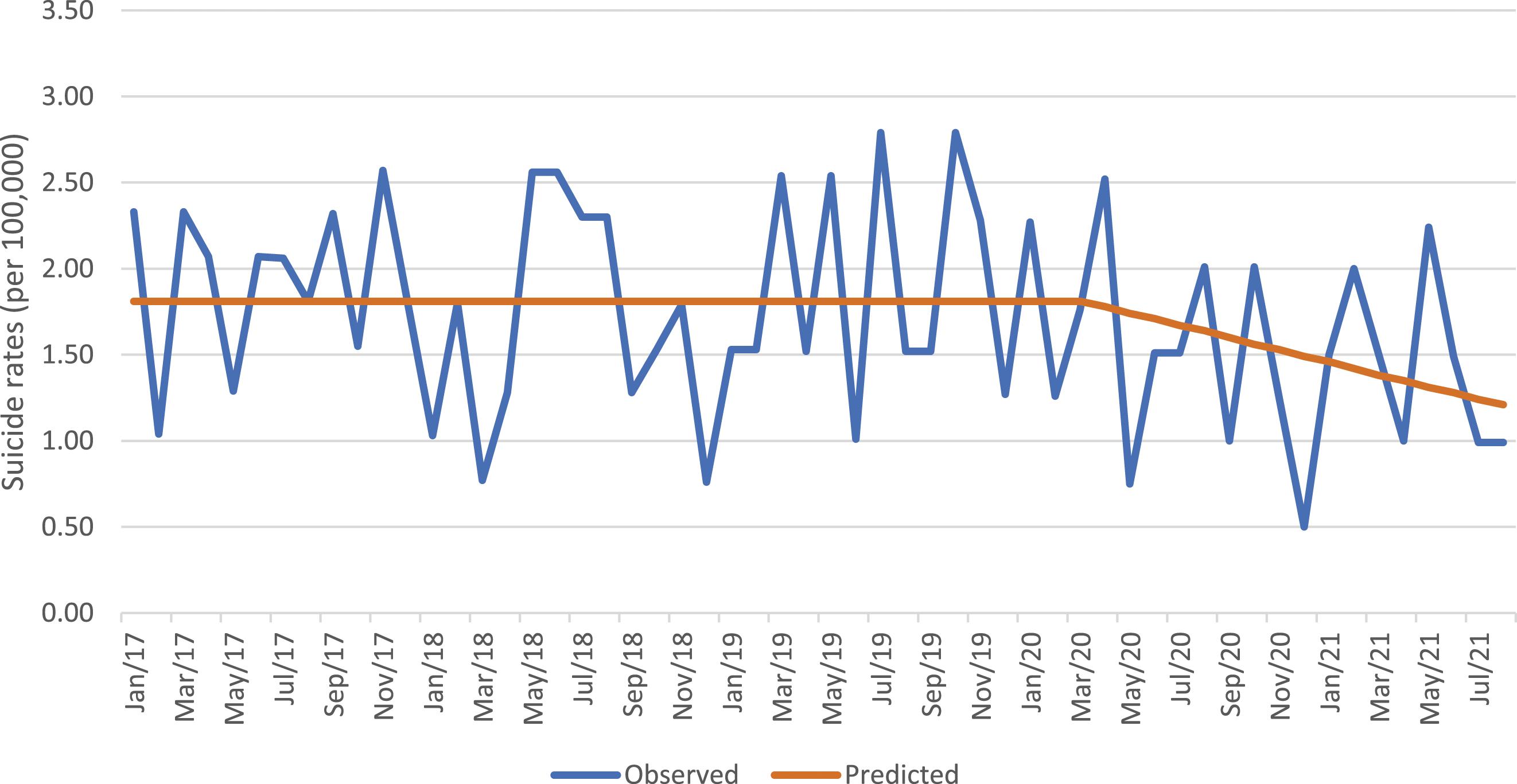
Regarding women unassisted suicide rate, none of the three models showed significant changes related to COVID-19. Among men both the “step” effect of COVID-19 (Model 1; b = −0.357, SE = 0.164, p = .034) and the “ramp” effect of COVID-19 (Model 2; b = −0.036, SE = 0.015, p = .024) were negative and significant. This result indicates that there was a decrease of 0.357 in unassisted suicide rates from the pre-COVID-19 to the post-COVID-19 period (see Figure 3), and that this decrease was gradual, corresponding to a monthly decrease of 0.036 in unassisted suicide rates starting from the onset of COVID-19 (see Figure 4). The effect of the stringency index was also negative but not significant. « Step » effect of COVID-19, unassisted suicide rates, men. « Ramp » effect of COVID-19, unassisted suicide rates, men.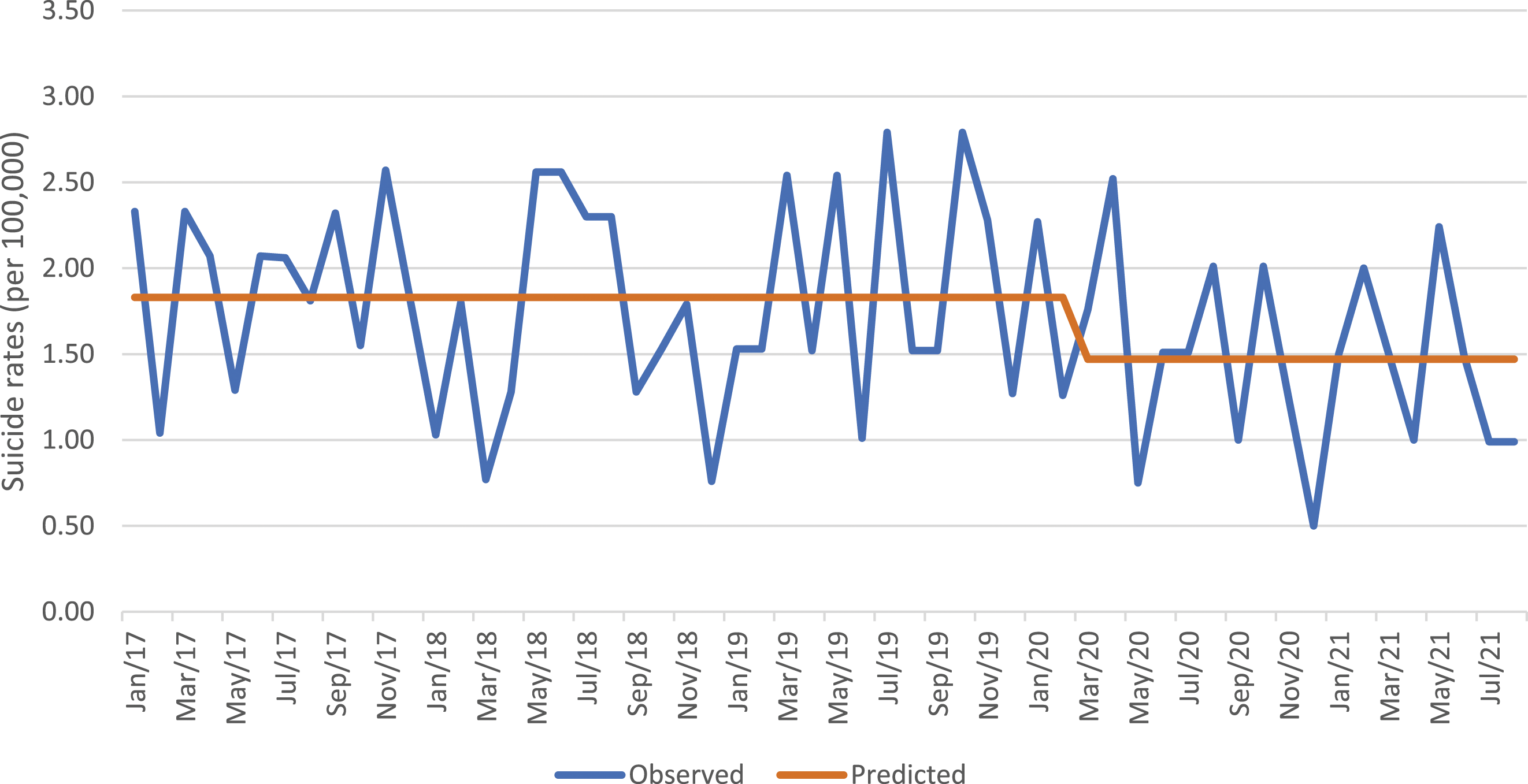
Discussion
This study sought to determine the impact of COVID-19 on women and men assisted and unassisted suicides in French-speaking cantons of Switzerland. As a reminder, “Step” effect, that is, a sudden sustained change following the onset of the COVID-19 pandemic; “Ramp” effect, that is, a change in the slope following the onset of the pandemic, and “Stringency index” effect, that is, the association with the level of lockdown policies.
For women, we found that assisted suicide rates were inversely associated with the stringency index. This suggests that assisted suicide rates were lower in the most acute phase of the pandemic where the structural were the strictest. Although not significant, the coefficients of the “step” and “ramp” effects are consistent with this interpretation. Overall, assisted suicide rates were lower (although not significantly) during the pandemic than during the pre-pandemic period (“step” effect”), and assisted suicide rates were slightly higher (although not significantly) at the end of the pandemic period than at its onset (“ramp” effect). By contrast, no significant change was observed for unassisted suicides among women. However, the non-significant results all pointed in the same direction, showing a decrease in unassisted suicide rates during the pandemic period. For men, we found a significant gradual increase in assisted suicide rates from the onset of the pandemic to the end of the covered period (“ramp” effect), both “step” and “stringency index” effects were not significant but pointed in the same direction. By contrast, for unassisted suicide rates, we found a significant decrease during the overall pandemic period compared to the pre-pandemic period that was stronger at the end of the covered period than at the onset of the pandemic. “Stringency index” effect was not significant but also showed a decrease.
The impact of COVID-19 on assisted suicides thus varied by gender: those of men increased while those of women decreased, a result raising questions. As mentioned in our introduction, more women than men usually die by assisted suicide, and rates are steadily rising in both genders (Canetto & McIntosh, 2022; Montagna et al., 2023). During the pandemic, both Canadian (Nissim & Hales, 2022; Oliver et al., 2021; Tremblay-Huet et al., 2020; Wiebe et al., 2021, 2022) and Swiss (EXIT Association pour le Droit de Mourir dans la dignité, 2021, 2022) data have shown a downward trend in the acute phases of the pandemic and an upper long-term trend for both genders, but their possible relation to COVID-19 and gender distribution were unclear. Our hypothesis was that the pandemic, which led to social isolation and significant social pressure on elderly population (Khawaja & Khawaja, 2021; Salinas Mengual, 2021) could probe them to ask more for assisted suicides. According to our results, this may be correct for men only. A previous study showed that women choose assisted suicides more than men because they are economically and socially disadvantaged, which can make them think their lives are less worthy (Canetto & McIntosh, 2022). It may be that, in the pandemic context, the burden of adverse social and economic effects increased more in men than in women and/or that men had more difficulties coping with the changes, increasing their propensity to choose to die by assisted suicide. On the other hand, previous studies showed that women have less access to care than men, are considered less deserving of care, receive poorer quality care (Canetto & McIntosh, 2022) and have fewer resources to afford expensive care (Canetto, 2017). In Switzerland, unjustified gender differences in care have also been reported (Clair et al., 2018). Our hypothesis is that it could be that the COVID-19 pandemic accentuated inequalities in access to care, but also to associations dedicated to the right to die. In such a situation (e.g. the EXIT association had to reduce its activities from March to May 2020 and had to prioritize assisted suicides of emergency cases (EXIT Association pour le Droit de Mourir dans la dignité, 2021)), men may have been more insistent about their assisted suicide and more successful in making their voices heard. These hypothesis on men assisted suicide rates increasing with COVID-19 have however to be balanced with the opposite decreasing trend we showed in men unassisted suicide. In 1995, Posner made the hypothesis that assisted suicide was likely to substitute for unassisted suicide (Posner, 1995), according to some recent studies in women (Girma & Paton, 2022). It could then be that the pandemic favored such an effect in Swiss men, which should be further explored.
Our result on the COVID-related decline in the rate of men unassisted suicides is in line with previous studies. Indeed, most of the literature showed stable or falling unassisted suicide rates for men combined during the COVID-19 pandemic in many countries (Appleby, 2021; Botchway & Fazel, 2021; Efstathiou et al., 2021; Pathirathna et al., 2022; Pirkis et al., 2021, 2022; Webb et al., 2022). On the other hand, contrary to previous existing studies (Appleby, 2021; Botchway & Fazel, 2021; Efstathiou et al., 2021; Pathirathna et al., 2022; Pirkis et al., 2021, 2022; Webb et al., 2022), we did not find any significant effect of the pandemic on women unassisted suicide rates. This might be related to our low statistical power since only 29.5% of our sample of unassisted suicides were women (N = 157). Indeed, although of small magnitude and not significant (as compared with men), the step and ramp effects of COVID-19 were negative (p-values >0.05; see Table 3). In Switzerland, a study showed that women experienced more depressive (BAG, nd) and stress (Winterthurer Institute of Health Economics (WIG) & ZHAW School of Management and Law, nd) symptoms during the pandemic, used more frequently mental health services (online platform, counselling on psychological health/personal problems, coping with everyday life, loneliness, isolation and friendship) than men (BAG, nd) and globally exhibited higher levels of distress. Furthermore, several studies in Japan showed a marked increase in the unassisted suicide rates among women (Eguchi et al., 2021; Matsumoto et al., 2021; Nomura et al., 2021; Sakamoto et al., 2021; Tanaka & Okamoto, 2021), highlighting the increase in unemployment and domestic violences among women during the pandemic (Eguchi et al., 2021; Nomura et al., 2021). This slightly reduced rate in women could thus suggest that they were more socially and economically impacted by the COVID-19 pandemic than men but further studies are needed on this topic. Furthermore, the above-mentioned possible interrelations between assisted versus unassisted suicides have to be considered. We cannot rule out the possibility that the sharper decline in the number of unassisted suicides among men is also linked to a gender-specific “shift” from unassisted to assisted suicide.
Regarding the similarities or differences between the sample and the general population in Switzerland, our average monthly suicide rates for men and women in their respective cantons (see Table 1) and data from the Federal Statistical Office (OFS) were rather similar. Assisted suicide rates for women (VD, FR, GE): 1.56 versus 1.38 (average of the 3 cantons for OFS data), assisted suicide rates for men (VD, FR, GE): 1.06 versus 1.38, unassisted suicide rates for women (VD): 0.69 versus 0.6, unassisted suicide rates for men (VD): 1.71 versus 1.6. (Suicide et Suicide Assisté | Obsan, nd). Our findings appear to be generalizable to Switzerland; however, it must be acknowledged that, due to the specificity of the cultural, judicial, and societal context, generalizability is limited to this country.
Limitations
This study has several limitations. Firstly, and as mentioned in the methods section, the suicide data are different between assisted and unassisted suicide, and do not include all French-speaking Swiss cantons. Our sample was thus reduced, and we were not able to analyse data by age, which would have been relevant to examine a possible shift from assisted to unassisted suicides, as mentioned in the discussion. Given that we saw a decrease in assisted suicides during the restrictions among women, it would have been interesting to analyze whether women who usually turn to assisted suicides would have opted for unassisted suicides when access to assisted suicides was difficult and restricted. Nor were we able to study the possible different effects of the pandemic on the young and the elderly, who are vulnerable groups. Secondly, there is still some doubt as to the classification of unassisted suicide as such, since deaths caused by less clear-cut methods such as drowning or poisoning, with no evidence of suicide, are classified as “accident”. This may have underestimated the number of unassisted suicides. However, we are not aware of any data showing that the classification of suicides may have been worsened by the pandemic and consider that our results on the research question should not have been impacted by such a bias. We did not have any additional information on suicide deaths, such as known psychiatric disorders, new social and economic pressures due to COVID-19, mental impact of the pandemic. These limitations could have influence the conclusions drawn from the study. For instance, the inability to analyze data by age limits the understanding of demographic trends in suicide rates during the pandemic, while uncertainties in the classification of unassisted suicides may affect the accuracy of reported suicide statistics. Additionally, the lack of comprehensive data on the mental health and socioeconomic factors associated with suicide limits the depth of insights into the underlying causes of changes in suicide rates observed in the study.
Conclusions
Our study is the first in Switzerland to attempt to understand the impact of COVID-19 on both assisted and unassisted suicides, and to explain any gender differences. We found a decrease in unassisted suicides and an increase in assisted suicides among men from the COVID-19 pandemic onwards, as well as a decrease in assisted suicides among women during periods of severe restrictions. The fact that these results are not similar for men and women, underlines the importance of exploring in more detail why these gender-related discrepancies occur, where they come from and how to act to avoid them. Furthermore, our results give some clues on a possible interrelation between epidemiological trends in assisted and unassisted suicide, a topic definitely deserving further investigation. They could be used to establish strategies to enhance mental health support services, improve access to resources, or implement preventative measures aimed at reducing social isolation.
Footnotes
Acknowledgements
The authors thank the CURML for the suicide data.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Notes
Author Biographies
![]() ), he has been active in research, clinical practice and teaching in mental health for the past twenty years and in suicide prevention for the past ten years. In consultation-liaison, he is interested in clinical supervision of health professionals and communication in oncology, with several ongoing projects, as well as in gender-related issues, including LGBTQI+. He leaded several scientific and public health projects on suicide prevention, which used various qualitative and quantitative methodologies and were funded by several public funds. His research focused on interventions after suicide attempts, the emotional experience of clinicians meeting suicidal patients, and completed suicides of psychiatric patients. On the clinical and teaching levels, Dr Michaud is a trainer of trainers for the module “Facing suicidal risk” and is involved in numerous courses in the field of mental health and suicide prevention (e.g. leading a Certificate of Advanced Studies (CAS) on psychoanalysis and institutions or being in the board two other CAS on (i) psychosomatic and psychosocial medicine and (ii) psycho-oncology). He regularly appears in the regional and national media for his expertise in suicide prevention. In addition to his academic and hospital clinical-based activities, he practices psychotherapy and psychoanalysis as a fellow of the Swiss psychoanalytical society.
), he has been active in research, clinical practice and teaching in mental health for the past twenty years and in suicide prevention for the past ten years. In consultation-liaison, he is interested in clinical supervision of health professionals and communication in oncology, with several ongoing projects, as well as in gender-related issues, including LGBTQI+. He leaded several scientific and public health projects on suicide prevention, which used various qualitative and quantitative methodologies and were funded by several public funds. His research focused on interventions after suicide attempts, the emotional experience of clinicians meeting suicidal patients, and completed suicides of psychiatric patients. On the clinical and teaching levels, Dr Michaud is a trainer of trainers for the module “Facing suicidal risk” and is involved in numerous courses in the field of mental health and suicide prevention (e.g. leading a Certificate of Advanced Studies (CAS) on psychoanalysis and institutions or being in the board two other CAS on (i) psychosomatic and psychosocial medicine and (ii) psycho-oncology). He regularly appears in the regional and national media for his expertise in suicide prevention. In addition to his academic and hospital clinical-based activities, he practices psychotherapy and psychoanalysis as a fellow of the Swiss psychoanalytical society.
