Abstract
Adolescents bereaved by suicide and other traumatic death may experience strong grief reactions and increased risks of mental health problems and suicidal behaviour. As timely access to professional help can be critical, it is essential to understand how counselors perceive suicide bereavement in adolescents and how they work with this population. This study aimed to examine the perspectives of counselors (N = 34). Eleven participated in an individual semi-structured interview and 23 others in group interviews. Thematic analysis yielded three themes: (1) Building a relationship with the bereaved adolescent, (2) Offering support tailored to the needs of the grieving adolescent, and (3) Offering strengths-based and sustainable support. Counselors’ skills, attitudes, content-related expertise, and approaching the adolescent’s grief within their developmental context were deemed essential for building a therapeutic relationship and offering viable support. The findings may inform good practices in counseling bereaved adolescents to facilitate positive mental health outcomes.
Introduction
Many adolescents experience the death of a close person (i.e., bereavement), such as a family member or friend. Between 4% and 6% of adolescents experience the death of a parent and 78% have lost a relative or a friend before reaching age 18 (Berg et al., 2015; Burns et al., 2020). Furthermore, approximately 1 in 5 adolescents experience bereavement by suicide at some point before reaching adulthood with around 1 in 20 adolescents experiencing this loss over a 12-month period (Andriessen et al., 2017).
Bereavement in adolescence is a highly disruptive and stressful event associated with a myriad of short- and long-term consequences. Common acute grief reactions include feelings of sadness, anger, guilt, and longing (Balk, 2014). According to a contemporary grief model, the Dual-Process Model of coping with bereavement (Stroebe & Schut, 2010), grieving individuals oscillate between loss-oriented (e.g., longing for the deceased) and restoration-oriented stressors (e.g., adapting to a new role), at their own pace. Although the grief processes after any type of death appear to be similar, some grief features may be more pronounced depending on the cause of death (Jordan & McIntosh, 2011). Grief and mental health reactions after sudden or traumatic deaths, such as accidents and homicides, seem to resemble those of grief after suicide more than grief reactions after natural deaths in adolescents (Kristensen et al., 2012). Adolescents bereaved by suicide and other traumatic death may experience more intensified feelings of shock, anxiety, and self-blame, and grapple more with “why” questions and meaning-making (Andriessen et al., 2018; Feigelman et al., 2017). They are also at an increased risk of developing mental health problems such as depression, anxiety, and posttraumatic stress disorder in the first months after the bereavement as well as up to more than two years after the death (Andriessen et al., 2016; Pham et al., 2018; Stikkelbroek et al., 2016). In addition, they have higher rates of self-harm, suicide, and other forms of early mortality compared with non-bereaved adolescents (Burrel et al., 2018; Del Carpio et al., 2021).
Grief after suicide or other traumatic death extends beyond the psychological impact of bereavement on the individual adolescent (Stroebe & Schut, 2015). Adolescents usually live within their family network and bereavement often disrupts the family equilibrium. Bereaved adolescents and parents can experience concerns and struggles regarding how to support each other, and parents may particularly worry about their adolescent’s health risk behaviours, such as aggressive behaviour or substance use (Andriessen et al., 2020; Cerel et al., 2008). Furthermore, bereaved adolescents are often reluctant to share their grief experiences and they narrow their circle of close relationships. In turn, family and friends may lack skills and not know how to respond to the bereaved adolescent, resulting in adolescents receiving insufficient social support (Andriessen et al., 2018, 2019a).
Given the potentially detrimental impact of bereavement by suicide and other traumatic death on adolescents’ psychosocial health, timely access to professional help can be critical. However, most research has focused on exploring the experience and impact of bereavement in this population (Andriessen et al., 2018; Silvén Hagström, 2019). Only a few studies have evaluated bereavement interventions for children and adolescents (Krysinska et al., 2023; Ridley & Frache, 2020), support specifically for adolescents bereaved by suicide or other traumatic death (Andriessen et al., 2019b; Hung et al., 2009), or what the adolescents find helpful regarding receiving support (Andriessen et al., 2019a, 2022; Dyregrov, 2009).
To provide adequate support to adolescents bereaved by suicide and traumatic death, it is essential to understand the perspectives of counselors regarding how they perceive and approach bereavement in adolescents, and how they work with this population. While adolescents bereaved by suicide and traumatic death are often reluctant to seek counseling (Andriessen et al., 2019a; Dyregrov, 2009), establishing a therapeutic relationship with adolescent clients is crucial for the therapeutic outcomes, including preventing early dropout, and it is the counselor’s role to initiate and facilitate a therapeutic alliance (Murphy et al., 2018; Ryan et al., 2021).
The perspectives of counselors working with adolescents have been studied in other contexts, such as referral to psychotherapy (Barca et al., 2020), development of resilience (Dillard et al., 2021), online chat counseling (Dowling et al., 2014), and principles of adolescent mental health care (Platell et al., 2018). No study has examined the perspectives of counselors working with adolescents bereaved by suicide or other traumatic death. This study aimed to address this gap by exploring counselors’ views on bereavement by suicide and other traumatic death in adolescents, how they approach and support bereaved adolescents, and what forms of support they believe are helpful for this population. As such, the study contributes to the literature by providing insights into what counselors perceive as feasible, acceptable, and adequate support for this population.
Methods
Study Design and Sampling
We conducted the study according to the Consolidated Criteria for Reporting Qualitative Research (Tong et al., 2007). We recruited a purposive sample of counselors located in Australia between October 2019 and March 2020. Various (suicide) bereavement organisations, grief support services, and professional organisations of clinicians and counselors providing support to adolescents, as well as the researchers of this study, disseminated the study announcement via their mailing lists, e-newsletters, and/or social media. Eligible counselors had at least five years of professional experience with providing support to adolescents bereaved by suicide or other traumatic death. They were offered an AUD 30.00 supermarket voucher as reimbursement.
Participants could choose between taking part in a semi-structured individual telephone interview or an in-person group interview. Research has shown that individual and group interviews complement each other regarding the breadth and depth of data collected on sensitive topics (Guest et al., 2017a). Offering multiple methods also allows more potential participants to take part in qualitative research as the decision to participate is influenced by their perception of being able to contribute to the study (Heath et al., 2018). Based on the literature (Guest et al., 2017b; Malterud et al., 2016), and our experience with qualitative research in this field (e.g., Andriessen et al., 2022), we estimated the required sample size to be between 25 and 30 participants.
A total of 49 counselors contacted us and 34 (28 females, 6 males) participated in the study. Reasons for not participating were being ineligible (i.e., having less than 5 years experience, n = 11), and being unavailable (n = 4). The mean age of participants was M = 48.47 (SD = 11.35, range 26–71 years), with an average of 16 years of experience in working with bereaved adolescents (M = 15.91, SD = 8.87, range 5–37 years). About one in four had five to nine years of experience (n = 8, 24%), 12 others (35%) had 10–19 years, and 14 (41%) had more than 20 years of experience.
Participants’ professional backgrounds included (grief) counseling, social work, nursing, psychology, psychotherapy, and psychiatry, and participants had been working in various settings including services for people bereaved by suicide, grief counseling, adolescent and family mental health, school counseling, and private practice. Three participants identified as culturally and linguistically diverse (CALD) and two as First Nations. As the analysis of the final interviews did not yield new themes, we determined that the sample size was adequate.
Data Collection
We developed a semi-structured interview guide, adaptable for individual and group interviews, with open-ended questions allowing for probes and follow-up questions. The lead questions inquired about participants’ views on type and timing of the support (e.g., “In your opinion, what support should be provided to a bereaved adolescent?”, “How should the support be provided?”, “What is the role of professional vs. peer support?”, and “What are the characteristics that make support helpful?”).
Eleven counselors participated in an individual interview and 23 participated in one of six group interviews (between three and five participants per group). Researcher A conducted all interviews. The group interviews were conducted at the premises of (suicide) bereavement and mental health service providers at various locations in Australia. Individual interviews took on average 44 minutes (M = 44.09, SD = 6.85, range 34–59), and group interviews 78 minutes (M = 77.83, SD = 21.33, range 40–102). The audio-recordings of the interviews were professionally transcribed, and we checked the de-identified transcripts for accuracy.
Research Team and Reflexivity
The study was based at the Centre for Mental Health and Community Wellbeing at The University of Melbourne, a national and international leader regarding suicide and mental health research. The lead researcher, K.A., is a social worker with ample experience in qualitative bereavement research. Researcher J.S. is a medical student previously trained in public health. Researcher K.K. is an experienced research psychologist and psychotherapist. The senior researchers, D.R. and J.P. are renowned experts regarding youth mental health and suicide prevention service delivery. Several team members have lived experience of suicide. The research team met regularly to ensure consistency throughout the study.
Data Analysis
We uploaded the data in NVivo 12 (QSR, 2020), and conducted a thematic analysis (Braun et al., 2019). Two researchers (K.A. and J.S.) created a codebook based on independent analysis of three transcripts (DeCuir-Gunby et al., 2011). Next, one researcher (J.S.) coded the remaining transcripts while holding regular discussions with the lead researcher. The same two researchers analyzed the coded data through an iterative process adopting the six steps described by Braun and Clarke (2006). An inductive approach allowed us to refine and adjust the codes to capture the meaning of the data rather than its explicit content. We visualised the codes in mind maps (i.e., diagrams) as an aid to conceptualize potential themes, which we repeatedly checked against the data before deciding the themes.
Ethical Approval
The study received approval from the Human Research Ethics Committee of The University of Melbourne (#1955213). All participants provided written informed consent.
Results
Description of Themes.
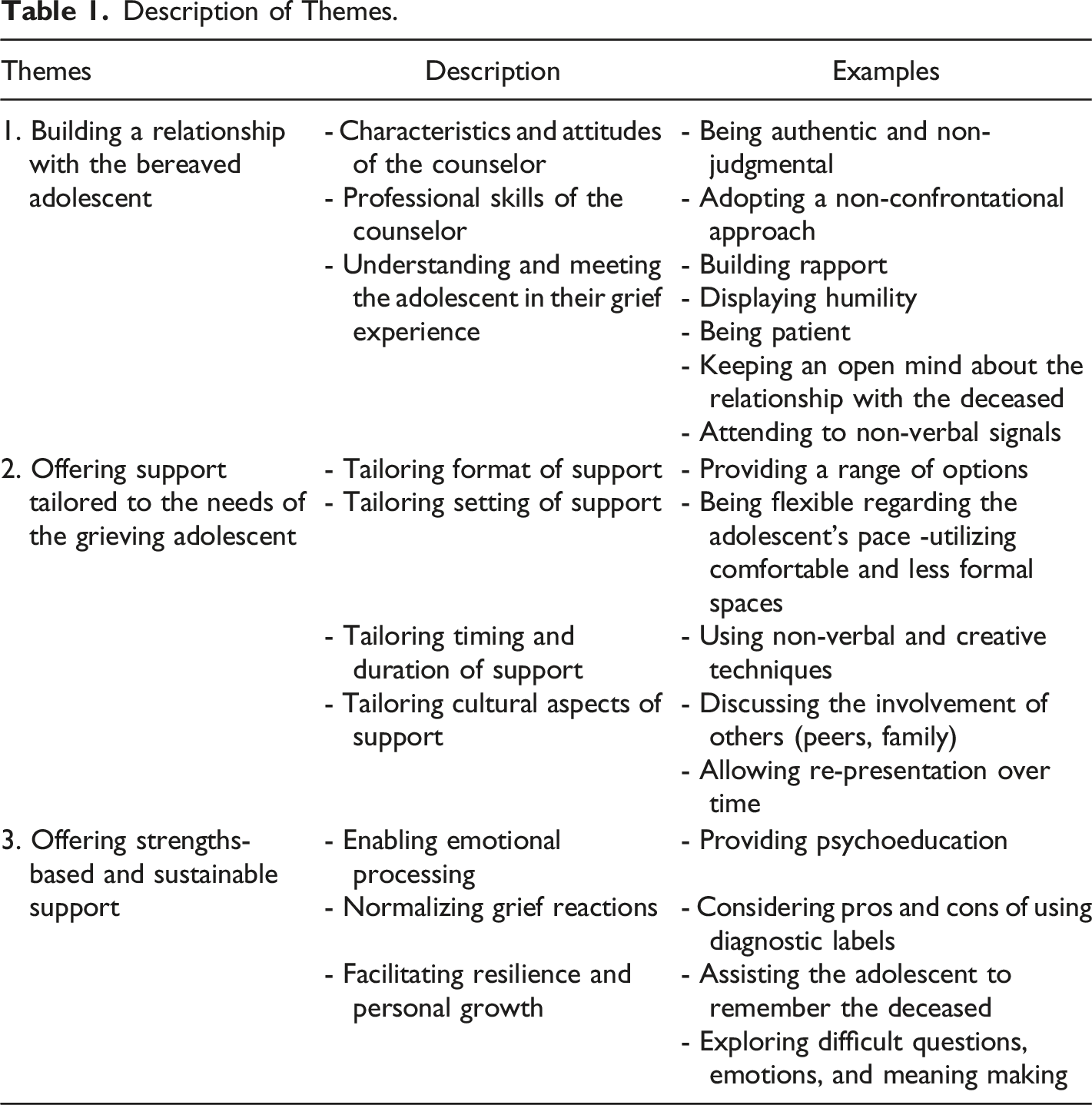
Theme 1: Building a Relationship With the Bereaved Adolescent
All participants emphasised the critical importance of establishing a personal relationship with the young client at the initial stage of the therapeutic process. They explained that, even more so than for adults, adolescents often require the formation of rapport before they can open up and share their experiences. Participants identified three main and interacting aspects of a counselor which contribute to effective relationship building: their personal characteristics and attitudes, professional skills, and their ability to understand and meet the adolescent in their grief experience. Acknowledging that relationship building is subjective in nature, many participants regarded trustworthiness of the counselor as a cornerstone to make the young person feel safe and comfortable sharing their vulnerabilities. I think they find it difficult to understand how to ask for help or what help is, and I think they are distrustful at first. It takes a lot of rapport building before you even start talking about what’s happened to make a teenager feel comfortable that you’ve come into their space and we’re going to talk about something so intimate as the loss of somebody close to them.
Most participants highlighted several elements which they believe builds a trusting relationship, such as adopting a non-judgmental attitude, and using non-confrontational techniques, such as sitting next to instead of in front of each other. Demonstrating genuine care, compassion, and empathy were also seen as vital for establishing a connection. It’s the genuine care of a person that makes a difference, that their life matters. They're saying, communicating ‘I care’.
Another central characteristic was authenticity, described as ‘being real, being authentic’. Some participants explained that adults, including counselors, often skirt around the issue of bereavement due to not knowing how to respond. They may also underestimate young people’s ability to handle the heaviness intrinsic to traumatic deaths and are, therefore, often anxious and reluctant to engage in open, honest discussions with them. Yet, participants acknowledged that sheltering the young person and not recognising their ability to cope with information can be detrimental to the relationship. But I think children cope quite well – not quite well but have a much more black and white understanding of life and death and can sometimes almost handle information more than adults can, and adolescents seem to be halfway between that. With some of them, I don’t know, but it's like they can actually handle more information than we think, and they get very confused when they know that the adults are not telling them information.
Rather than adopting a saviour mentality in which young clients are viewed as in need of rescuing, participants explained the significance of counselors displaying humility regarding their expertise and ability to aid. Participants emphasized that adolescents must be treated with the same level of respect, inclusiveness, and dignity as adults. Don’t come in with an attitude that you’ve got a piece of paper that says that ‘I’m this, this, this and I can do this, this, this’. That’s not required, it’s being a real person, not having somebody who barrels into a situation thinking that they are going to be able to fix the situation or stop the young person’s emotions.
Throughout, participants explained the critical role of gaining a mutual understanding of how the individual young person experienced their bereavement. This was conceptualised as both understanding the nuanced differences of bereavement as experienced by an adolescent as compared with an adult, and the experience of the particular young person and their context. As building rapport takes time, the counselor must be patient and adopt a gentle, paced approach. While some participants advocated for being active and gently encouraging the adolescent to engage in the process, others emphasized being comfortable sitting in silence and enabling the adolescent to engage at their own pace. Yeah, and be comfortable in allowing that young person to present however it is they need to present, not forcing conversation, not forcing any type of outcome, allowing that young person to express in whatever way they need to express, and that expression may in fact be silence. We're socially quite reluctant to engage in the silence and I think that that’s a really core part of sitting in grief with an adolescent.
In addition, most participants stated that bereavement by suicide or other traumatic death impacts upon various aspects of the adolescents’ lives and often manifests in multiple ways. They stated that counselors should engage in the process with curiosity and an open mind without imposing assumptions. This approach enabled counselors to peel back the layers of the adolescent’s experience and discover their core issues. For instance, several participants cautioned against making assumptions about the nature of the relationship with the deceased person and the impact that this would have on the adolescent’s life, as well as against making generalisations about gendered grief reactions. It all depends how attached they are to that person, like it could be a parent but they’re not close to a parent and never have been. They could be a friend who’s been their greatest lover or whatever, so it’s all about finding out the significance of that relationship. I can’t assume, you know? I think I would steer right away from gender differences in responding, instead I would say maybe they’re more introverted or extroverted, maybe they’re more this, more that, and obviously they’re talkers or they’re people you need to maybe reach out with more gestures, because they’re a bit shy. Don’t stereotype, just reach out and find out what’s the best way.
Participants explained that skilful acquisition, utilisation, and understanding of both verbal and non-verbal language are crucial skills for counselors. Participants discussed the importance of finding a common language and acquiring and utilising new forms of communication familiar to the young person. In addition, several participants raised the importance of the counselor’s ability to be sensitive to the young person’s mood and level of engagement by noticing shifts in their body language. I think the body language is really important in the counseling process. I think that being able to see the physical presentation of the young person; I think so much of it is about body language and the young person in establishing trust.
Regarding whether a counselor needs to be from the same culture or ethnicity as the adolescent client (i.e., for CALD or First Nations clients), participants expressed differing views. Some participants argued that it depends on the individual adolescent and their needs. Others advocated for involving counselors from the same cultural background as this enables some adolescents to feel more comfortable. Others emphasized the importance of being embedded within the local community rather than ethnicity per se. There’s more respect and credibility if you are a local, because people feel that you can understand the issues. Whether it’s suicide, bereavement or anything else for that matter. It just gives people more I guess comfort or maybe for them to tell their story. They don’t have to say it in a way that someone isn’t going to get it.
In summary, participants perceived building a therapeutic relationship as crucial for supporting bereaved adolescents. Counselors’ attitudes and skills such as approaching the adolescent with curiosity, an open mind, patience, authenticity, and engaging in honest and non-judgmental conversations were seen as contributing to relationship building. Understanding the adolescent’s grief experience within their developmental context and from their individual perspective was considered essential for relationship building.
Theme 2: Offering Support Tailored to the Needs of the Grieving Adolescent
Participants commonly raised the importance of adopting a ‘client-led’ approach, tailored to the needs, preferences, and capacity of the individual young person. This was considered essential due to the adolescent developmental stage, which is a time of moving away from family and gaining autonomy and independence. A key aspect of this approach is bestowing on adolescents a sense of empowerment and the ability to guide the process. Rather than offering a one-size-fits-all, adolescents should be provided with a range of options from which to choose, including the format, setting, and timing of support. A really big part of supporting adolescents is making sure that they feel empowered and not confronted, like kind of made to do something. Yeah, it’s got to be tailored to that person. Not everyone’s going to want to go on a grief camp, or sit and chat with their family. Some just want to be on their own with the counselor. It’s very varied.
Several participants described adjusting the format of support to the adolescent’s style of grieving. For instance, they explained the concept of ‘dosing’ whereby adolescents transition in and out of their grief, and how this can be incorporated by alternating between ‘traditional’ counseling and a ‘shake off’ phase. This requires counselors being flexible and acknowledging that the format of support may evolve over time. I’ve done quite a bit of sitting on the floor and maybe we would build a story out of music to their grief, but there’s points where they need a breather from it, and we’ll go make a cold drink or something and come back in. Sometimes you’ve physically got to do a bit more movement to help people move in and out of their grief so that’s dosed, I suppose.
With regards to the setting, all participants emphasised the importance of creating an environment where adolescents feel comfortable and experience as their safe ‘sharing space’. Participants described how they use less formal spaces, including nature and bushwalking. Many participants advocated for the use of creative techniques as focusing on the activity relieved pressure from the adolescent. With an adult I’ll sit in front of them, make eye contact, then I’ll start talking. With a teenager I’m more likely to sit next to them and maybe even have something in front of them like something to draw or colour with, or ask them if they’d like to take a walk, so it’s not too confrontational for them.
Many participants recognized the importance of tailoring the support in terms of who else is invited into the room. For example, participants considered the crucial role of peers as their involvement may normalize the adolescent’s experience and make them feel less ‘othered’. It also enables a shared understanding which does not need to be verbalized, thus, alleviating pressure and providing comfort. The kids who are already trying to fit in should not be different. Death makes you different. If someone dies in your family, they don’t know if anyone else has got a bereavement. To see others - I mean it’s the benefit of group isn’t it - coping or further down the track or talking about the same things. It's really validating and it helps kids.
Participants discussed if, and how, to involve the adolescent’s family in the counseling process. They noted that adolescents may not want to engage with their parents or family members either for fear of upsetting them, or because of their reactions to the death, which may decrease the adolescent’s feeling of safety. Overall, participants stressed the need to help adolescents navigate through the changing family dynamics and ensure that unrealistic expectations including parenting roles are not thrust upon them. I notice that sometimes – well not sometimes, every time, the adults have become so distressed it is quite frightening for the adolescents. They are confusing and anxious, and they are often panicking. The adolescents can absolutely feel that, and they pull away from adults because they are erratic and strange and not behaving normally.
Regarding the timing of first accessing support, participants had experienced a variety, ranging from a few days to years after the death. Several participants strongly advocated for adolescents gaining access to services early after the death. Some observed that this can lead to better outcomes and functional status in the longer term, and offering early support could introduce services that they may access in the future. Other participants cautioned that introducing services too early could deter adolescents from engaging in counseling in the future. Another participant explained that an adolescent may be in shock, necessitating practical support and survival strategies rather than bereavement counseling. If we see somebody later it’s often because they’ve had an exacerbated reaction, or they may have self-harmed, or having suicidal thoughts themselves, or they’ve stopped going to school, or things are kind of falling apart. … So I think they’re more likely to stay functioning if they get the good support in the beginning that links them in with a lot of help and care around them than just going on their own.
Several participants noted that bereaved adolescents may need to access services at a timepoint later in life due to their cognitive development. Participants explained that as adolescents mature, they are better able to fully process and understand the impact of the death on their lives which results in revisiting the grief. This enhanced understanding would often result in questioning and reconceptualizing the meaning of the bereavement experience and lead to seeking help (again). Grief is not something that I go into with a young person saying that there’s going to be recovery. They are always going to be impacted by the loss, particularly if they’re a really significant person in their life. It’s not about working that through to an end point and then being better. It’s about healing around that loss in a way and knowing that that is always going to be part of you. I have clients that they come in for the first time for counseling after four or five years and they have questions about the meaning of that loss. I would say it’s more a kind of a developmental kind of questions related with the meaning of that loss.
Many participants also explained that re-presentation at several timepoints throughout life is due to being triggered, due to life events in a family member’s life, such as a parent re-partnering, or milestones in their own lives such as partnership, marriage or births, or times of hardship, which may exacerbate the grief. Other triggers raised by participants included significant dates associated with the deceased person, such as birthdays, the death anniversary, or when the young person reaches the same age as when the person died. You might see young people re-engage at different times because grief is the kind of thing that can be re-stirred up at different life stages. So that they come back again and I actually think they probably dip in and out more than some of the work I do with adults. Kind of come for a bit and then disappear for a bit and then come back in for a bit.
In terms of the duration of support, many participants explained that there was no prescribed timeframe. Due to the lifelong impact of bereavement, participants advocated for providing young people with the option for long term care, so that they can re-engage with the service as needed. A few participants went further in stating that services should actively reach out, either randomly or intentionally, on specific dates such as anniversaries. They perceived utility in checking-in even if the young person does not respond, as the act itself demonstrates a level of care. Another participant cautioned that sustaining therapy over a long period of time can, in fact, contribute to complicating the grief response. If we haven’t heard from somebody for a little while, we’ll often just do a check in follow up to see if they’re doing okay or if they need something different from us. If you sustain therapy over too long you can actually pathologically push children, young people and family members into that more complex grief response. So, that’s got to be delicately balanced. If they come and go from therapy a little bit more, I think that’s far more appropriate. There’s got to be flexibility in what support is provided.
In sum, participants advocated that support must be tailored to the individual adolescent including the format, setting, and timing of the support, allowing them to engage with support services at their own pace and according to their needs as these may change over time. Acknowledging the agency of the bereaved adolescents, participants thought that counselors should provide them with a range of options, rather than prescribing what they should do.
Theme 3: Offering Strengths-Based and Sustainable Support
Participants articulated the myriad of benefits services can provide to adolescents. These benefits spanned the realms of enabling emotional processing, facilitating resilience and personal growth, more practical forms of help, and ensuring that the benefits are ongoing and sustainable. Many participants explained the significant value of conveying to the young person that grief is a difficult yet natural part of life. They explained how psychoeducation contributes to normalizing manifestations of grief, including somatic or behavioural issues, and intense emotions such as guilt or blame. Several participants posited that psychoeducation could allay adolescents’ worries that there is “something wrong with them”. It may instil a sense of hope and optimism by educating adolescents that there are various ways of grieving, none of which is right or wrong per se, and whilst the grieving process takes time, it will evolve to be more manageable. When people first come in, they’re feeling overwhelmed and quite chaotic and think there’s something wrong with them but actually, there isn’t. This is how they are in response to what’s happened. So, a lot of that is framing people’s experiences and assisting them to know that actually, it doesn’t feel like it, but they are okay. A lot of it’s about helping them to say ‘it’s okay’, it wasn’t your fault, and we are actually going to be able to hold that space for you to be able to ask those really hard questions.
A few participants highlighted the importance of providing psychoeducation to the family to normalize the adolescent’s manifestations of grief and reassure the family. By better recognising and understanding their own grief, parents and family members could better acknowledge the grief of their children. I’ve spoken to some mums, and it’s been a relief for them sometimes to know that ‘oh okay, my kid’s acting out, but that’s how young people express their distress. So that’s actually quite a normal thing’. It just takes some of the pressure off them.
Several participants addressed the concept of maladaptive forms of grief in the context of psychoeducation, and argued against the use of labels or diagnoses such as “prolonged grief disorder” or “complicated grief”. They did not find this language to be helpful in the counseling process. They warned that young people’s brains are still developing and maturing and, therefore, any finite diagnosis should be avoided. When it comes to young people, we’re not going to see these complex diagnostic criteria emerge early. We need to span a very broad diagnostic criteria in looking at the young people’s presentation, rather than diagnosing or trying to diagnose. I think if we do use instruments, it needs to be merely to understand preventing problems and then to track progress over time.
Other participants argued that a diagnosis could be useful when it provided benefits for the individual. For instance, it may help to clarify the individual’s circumstances and guide them towards more appropriate treatment options. Using a label may also be beneficial in securing access to additional services or funding. Another participant noted that a diagnosis may give comfort to the individual as it provides an opportunity for psychoeducation. The use of diagnosis is really only if it’s going to guide appropriate treatment. If it seems to be complicated grief, complicated by other social and emotional issues that the person might have been carrying anyway, or that might have been present in the family, or whatever, if therapy could be helpful, encourage it. There’s this idea that they don’t recognize themselves so there’s that ‘am I going mad? I’m not coping with this, I’m not doing okay’, when actually, when you put that in context, they feel a lot better with that. Because then they understand themselves a bit more.
Some participants emphasized the importance of assisting adolescents to find ways to connect with the deceased person and to remember and celebrate their life. Keeping their memory alive and maintaining a connection could contribute to finding meaning in the loss and facilitate the grief process. One of the first things I ask young people, who’ve lost someone, to do is just really simple, just to bring in photos and memorabilia so that I can get to know the person with them. In doing that, it’s like what we’ve been saying is bringing them to life. It’s creating connection and telling stories about their life, not necessarily just their deaths, but it’s what they meant. That’s I think very, very healing in the whole process.
A few participants highlighted the benefits of guiding adolescents through the journey of meaning-making and exploring both the difficult questions around why the death has occurred and what long-term impact it may have. Some participants referred to the concept of posttraumatic or personal growth. They emphasized the importance of guiding adolescents to observe and acknowledge their personal development and transformation throughout the grieving process. You’ll be forever changed from that person’s impact in your life and losing that person, and that’s okay. This will help you in other areas to understand other people’s loss or to just really appreciate the beauty of that relationship that you had with that person and to be grateful for that. It’s sort of healing around that hurt, around that person and be forever changed because of the impact of them on your world.
In summary, participants emphasized the crucial role of strengths-based counseling in processing the grief. Through psychoeducational approaches, counselors aim to normalize the adolescents’ grief reactions and enhance their understanding of what they are experiencing. This may include exploring continuing bonds with the deceased person and making meaning of the bereavement, which may facilitate personal growth in the bereaved adolescents.
Discussion
This study examined the views of counselors on how to approach and support adolescents bereaved by suicide and other traumatic death. The analysis identified three main themes: building a therapeutic relationship with the bereaved adolescent, offering tailored support, and offering strength-based and sustainable support.
Participants unequivocally considered that a therapeutic relationship built upon trust was a prerequisite for the bereaved adolescents to actively engage in the counseling process and feel safe sharing their inner world. This finding receives strong support from studies with adolescents bereaved by suicide and other traumatic death in which the young participants highlighted feeling comfortable and connected and mutual trust as key features of engaging in a helping relationship (Andriessen et al., 2019a, 2022). Although research regarding the effect of the therapeutic relationship specifically on grief outcomes is still to be conducted, bereaved adolescents, parents, and counselors in a recent Delphi consensus study, highly endorsed the value of building a therapeutic relationship in supporting bereaved adolescents (Ross et al., 2021). Systematic reviews substantiate that an effective therapeutic relationship is associated with beneficial outcomes more generally in child and adolescent mental health (Murphy & Hutton, 2018; Ryan et al., 2023).
All participants identified crucial aspects within their roles as counselors, which they perceived as contributing to relationship building with bereaved adolescents, including non-judgment, genuine care, compassion, authenticity, honesty, and professional skills. Similarly, adolescents bereaved by suicide and other traumatic death prefer being met with empathy, genuine interest, authenticity, and a non-judgmental attitude when seeking counseling (Andriessen et al., 2019a, 2022). In contrast, being met pedantically, judged, or condescendingly (Andriessen et al., 2019a; Dyregrov, 2009), or counselors acting bored or not answering questions have been reported as deterring young clients (Ryan et al., 2021). The broader child and adolescent mental health literature also stresses the importance of constructive counselor attributes (Barca et al., 2020; Kirk et al., 2023; Ryan et al., 2023), and training in interpersonal skills with adolescent clients (Murphy & Hutton, 2018).
In addition to favourable attitudes and communication skills, most participants highlighted that counselors must be able to meet the adolescent in their grief experience to establish a therapeutic relationship. This finding is highly corroborated by research with bereaved adolescents (Andriessen et al., 2019a, 2022), and a Delphi consensus study (Ross et al., 2021). The finding and the literature show that counselors must have adequate knowledge and content-related expertise specifically regarding grief after suicide and other traumatic death in this population. While grief in itself is understood as a natural reaction to a major loss (Balk, 2014; Stroebe et al., 2008), bereavement after suicide or other traumatic death constitutes a risk factor for psychosocial problems (Andriessen et al., 2016; Feigelman et al., 2017). As such, counselors need specific training and expertise to understand grief experiences within the developmental, mental health, and social context of an adolescent client.
Many participants underlined that gaining an understanding of the adolescent’s grief experience was a mutual process of counselor and client. As this process may take time, participants favoured a paced approach, with some also addressing the need to encourage the adolescent to engage in the counseling process. Studies with bereaved adolescents strongly endorse finding a balance between exercizing patience and encouraging adolescents (Dyregrov, 2009; Ross et al., 2021). The adolescent mental health literature indicates that adopting collaborative approaches, finding common ground, and validating and praising the adolescent client facilitate this engagement process (Lavik et al., 2018; Orlowski et al., 2023). Nonetheless, it has been noted that entering a counseling setting is a novel experience for adolescents, which may add to their feelings of shock and being overwhelmed by the grief (Andriessen et al., 2019a). This may, at least in part, explain why adolescents may hesitate to share their grief experiences with an unfamiliar counselor.
Views differed regarding the importance of the client sharing the same ethnic or cultural background. While no bereavement study has examined this topic, the adolescent mental health literature suggests that some young clients from ethnic minorities in Western countries may benefit from ethnic matching in counseling, as it may contribute to the client feeling safe and connected, but more high-quality studies are needed to confirm this observation (Ryan et al., 2023). Further, there is little evidence of the effect of the counselor’s gender on relationship building, contrary to stronger evidence of the positive effect of the counselor’s level of experience (Ryan et al., 2023). Perceived lack of experience has been signalled as deterring young clients bereaved by suicide (Dyregrov, 2009). Some participants in our study emphasized that being locally embedded was more important than ethnicity. Given the high exposure to suicide mortality in First Nations and CALD communities in Australia and other countries (Pollock et al., 2018; Troya et al., 2022), studies are urgently needed to enhance our understanding to better inform suicide postvention strategies in these populations.
To tailor the support to the adolescent’s needs, many participants advocated for a client-led approach. They explained that empowering the individual to guide the process was even more imperative for adolescent clients due to their developmental stage and high regard for autonomy and independence. Empowerment may counteract the lack of faith adolescents may have that things can improve (Barca et al., 2020), and strengthen the therapeutic alliance (Ryan et al., 2023). Studies with bereaved adolescents highlight the value they place on control and agency in the support provided (Andriessen et al., 2022; Breen et al., 2023; Ross et al., 2021). Rather than being told what to do, bereavement and mental health studies indicate that adolescents prefer to stay in control and receive options from which they can choose (Andriessen et al., 2022; Gibson et al., 2013, 2016; Kirk et al., 2023). Participants in our study confirmed the literature which specified that the format, setting, and timing of the support should be tailored to the needs, preferences, and capacity of the adolescent client, so that they can use the support as needed (Kirk et al., 2023; Orlowski et al., 2023; Ross et al., 2021). Importantly, as bereaved adolescents mature, they may revisit their grief experiences because their perspectives on life and death have been evolving (Oltjenbruns, 2001). Specific dates such as anniversaries may also trigger grief reactions, even after several years (Andriessen et al., 2020). Thus, bereaved adolescents must be able to access services on a flexible and long-term basis.
Within the context of tailored support, some participants referred to ‘dosing’ the support in line with the adolescent’s pace of transitioning in and out the grief. This notion is in line with contemporary understandings of grief processes as articulated by the Dual Process Model of coping with bereavement (Stroebe & Schut, 2010). The model describes how bereaved individuals oscillate between loss-oriented (e.g., feelings of sadness and longing), and restoration-oriented stressors (e.g., exploring new opportunities or finding distractions from the grief) (Stroebe & Schut, 2010). Adolescents bereaved by suicide and other traumatic death have described similar grief dynamics. They tend to share their grief with a few selected confidants (such as a specific family member, friend or counselor) and rely on others for finding distractions, such as hanging around with friends or going to school (Andriessen et al., 2018, 2020). Of note, adolescents in these studies emphasized that sharing their grief and finding distractions were equally important for coping with bereavement.
Involving others in the counseling process, especially parents/family members, appeared to be a sensitive topic eliciting nuanced reasoning from participants. Some participants highlighted how bereavement in adolescents can disrupt family relationships (Andriessen et al., 2020). They noted that adolescents are often reluctant to share their experiences with immediate family members and need the exclusive relationship with a counselor as a safe space. Others pointed at potential beneficial effects of peer support, for example, for normalizing grief reactions (Balk, 2014). Adolescents bereaved by suicide or other traumatic death participating in bereavement studies tended to prefer individual counseling and oppose sessions involving parents/family (Andriessen et al., 2022). Similarly, participants in a recent Delphi consensus study did not endorse items regarding family-based counseling; however, highly endorsed items regarding support for parents to enhance their capacity to support their bereaved adolescent (Ross et al., 2021). Moreover, systematic review of interventions for people bereaved by suicide indicated that providing support to the social environment, and specifically to parents of bereaved children and adolescents, enhances the effectiveness of the intervention, although more intervention studies with adolescents are needed (Andriessen et al., 2019b). The broader adolescent mental health literature further highlights the importance of confidentiality and privacy for adolescents (Gibson et al., 2016) and counselors openly discussing with them the possibility of involving others to mitigate breaching the adolescents’ trust (Kirk et al., 2023; Ryan et al., 2021).
Most participants advocated for strengths-based and sustainable support based on acknowledgment and validation. Psychoeducation was seen as essential in facilitating emotional processing and meaning making, normalizing the adolescent’s grief experience, and fostering resilience and personal growth. Similarly, bereaved adolescents have emphasized that educational approaches help them to understand their grief, the reactions of others, and learn skills and strategies to cope with the grief-related emotions (Andriessen et al., 2022; Breen et al., 2023; Ross et al., 2021). In this context, some participants addressed the usefulness of applying a diagnosis of complicated or prolonged grief disorder to bereaved adolescents. While views differed, most thought that it would only be useful when it informs treatment planning or provides an opportunity for psychoeducation. It has been noted that a diagnostically-led approach (i.e., a deficit-based approach) may not fit within a more holistic and strengths-based approach deemed more suitable for this population (Kirk et al., 2023).
As with our study, the broader adolescent mental health literature points at the importance of enhancing insight into one’s functioning and developing self-care skills to aid emotional and cognitive functioning (Kirk et al., 2023). The significance of these goals is deepened in the context of supporting adolescents bereaved by suicide and other traumatic death, a cohort at greater risk of experiencing more intensified negative emotions, grappling more with meaning-making, and developing suicidal behaviour and mental health problems than adolescents bereaved by other causes (Burrell et al., 2018; Feigelman et al., 2017). Nonetheless, being able to share grief experiences and find meaning in the suicide loss have been reported to contribute to posttraumatic growth in those bereaved (Levi-Belz et al., 2021), and adolescents bereaved by suicide have indicated that experiencing a death by suicide can be catalytic for positive mental health (Andriessen et al., 2018). Offering strengths-based support may contribute to such positive outcomes (Ross et al., 2021).
Limitations
The current findings should be understood within a few limitations. The study involved voluntary, mostly female participants, and relied on self-report. Although participants had ample opportunity to share their views, it is possible that some important issues were not shared. The study did not examine potential gender differences, the possible impact of ethnicity-matching of client and counselor, or the participants’ education/scholarly background. Nonetheless, we successfully recruited a purposive sample of highly experienced counselors from across the country. We used multiple recruitment channels and interview settings to ensure variation in the sample, and to collect a rich data set. Nonetheless, the study findings may not reflect the views of non-participants.
Future studies may explore particular counselor characteristics that can affect the counseling process and outcomes such as attachment style (Ryan et al., 2023), and hope for their clients (Bartholomew, 2023). Studies with counselors from First Nations and culturally diverse backgrounds may shed light on views on help-seeking across cultural groups. Further research may also examine whether counselors perceive differences in supporting bereaved adolescents between adolescents bereaved by suicide and by other traumatic death, as well as different modes of bereavement therapy for adolescents.
Implications
Counselors working in this field may benefit from training and supervision to walk the fine line between the need of adolescents for a client-led, self-paced counseling approach that acknowledges the young person’s agency, and young people’s need to receive guidance and psychoeducation from a skilled and knowledgeable counselor. The relational, therapeutic, and content-related expertise of the counselor is crucial to maintain a balance between the often-contradictory needs of bereaved adolescent clients.
This study, supported by the literature (e.g., Ryan et al., 2023), further suggests that a collaborative approach based on open communication may help to unravel and find a shared understanding of an adolescent’s grief reactions, and discuss sensitive issues such as involving others. Such an approach would also allow counselors to check in with the adolescent client on the quality of the therapeutic alliance, as the young client’s perception of the alliance is an important indicator of therapeutic outcomes (Gergov et al., 2021; Murphy & Hutton, 2018).
Conclusions
This is the first study exploring the views of counselors regarding how to approach and support adolescents bereaved by suicide and other traumatic death. It is hoped that the findings of this novel research will contribute to the scant literature in this field and serve as a source of guidance and support for counselors working with this population. Given that adolescents bereaved by suicide and traumatic death are often reluctant to seek counseling, and that establishing and maintaining a therapeutic relationship is critical in fostering engagement with and preventing early drop-out from counseling, scrutinizing this matter from counselors’ perspectives is invaluable. Furthermore, insights gained may serve to inform the development of bereavement programs and guidelines specifically designed for supporting adolescents bereaved by suicide and other traumatic death. This will contribute to improving the quality of the support they receive, and hence, their outcomes in terms of coping with grief and positive mental health.
Footnotes
Acknowledgments
We are most grateful to the participants for sharing their experiences, and to the organizations and individuals who helped with recruitment and/or hosted the focus groups, especially: The Compassionate Friends Victoria, Support After Suicide Jesuit Social Services, StandBy Support After Suicide, headspace National, Anglicare Suicide Prevention and Grief Support South Australia, Sabrina’s Reach 4 Life, and Grief Australia.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: K.A. was supported by a National Health and Medical Research Council Early Career Fellowship [GNT1157796]. J.P. was funded by a National Health and Medical Research Council Investigator Grant [GNT1173126]. The funding bodies had no role in the design of the study, the collection, analysis and interpretation of data, the writing of the report, and the decision to submit it for publication.
Data Availability Statement
Data regarding the results of this study are available from the authors upon reasonable request. Original data cannot be shared to avoid reidentification of participants.
