Abstract
End-of-life (EoL) planning and the drafting of advance care directives (ACD) are challenging for older adults. As part of a mixed study, the content of 18 semi-structured interviews with Swiss community-dwelling older adults was analyzed to investigate contextual and interactional aspects that might influence their choice to complete ACD. Results show that EoL planning vary greatly. Three types of planners were highlighted: the solo planners, the collaborative planners, and the delegators. Each represents a specific way of conceiving autonomy, the usefulness of ACD and of involving third parties in the decision-making process. Whereas for solo planners, ACD is a personal, rational affair, for collaborative planners and delegators, reflection and decisions on EoL issues are interactional and iterative processes. The results suggest that health and social care professionals would benefit from taking into consideration the various types of planning, in order to provide the best support to older adults for ACD completion.
Thanks to longer life expectancy and technological advances in the medical field, as well as legislative changes, older people – at least in some Western countries – now not only have the opportunity, but also the responsibility, to decide what they would or would not like to happen at the end of their lives. In Switzerland, for example, the Swiss Adult Protection Law, which came into effect in 2013, allows for the writing of advance care directives (ACD) and for the nomination of a therapeutic representative who will make medical decisions in the event of the person’s loss of mental faculties and/or consciousness (Vilpert et al., 2018). However, these recent opportunities are not always embraced by the people who can benefit from them. For example, in the United States, a systematic review of 150 prevalence studies indicated that 29.3% (completed end-of-life (EoL) care directives, and that 33.4% designated a surrogate (health care power of attorney) to make decisions if they become incapacitated (Yadav et al., 2017). The highest rates of completion were seen in palliative care patients (59.6%; IC95%: 41.8–75.1) and in dependent older adults living in long-term care facilities (50.1%; IC95%: 42.1–58.2). In Australia, a national health record audit of 100 organizations (general practices, hospitals, and residential aged care facilities) was carried out on advance care planning (ACP), based on the medical files of 4187 patients aged 65 and older (Buck et al., 2021). Results show that 19.3% of patients had completed the directives; the prevalence was higher in residential care facilities (28%) than hospitals (9.8%), or general practices (4.4%). How can we explain the fact that autonomy, so highly valued today in the West, particularly in biomedical ethics (Beauchamp & Childress, 2013) is not put to greater use in the drafting of ACD? In Switzerland too, only a small proportion of the population completed ACD (21.1%); rates differed significantly between the German- (25.9%), French- (6.8%) and Italian-speaking (16.5%) regions of the country (Vilpert et al., 2018). Therefore, culture seems to play a role in the decision to prepare ACD. For example, in Japan, people prefer that healthcare providers initiate discussions on the matter, and believe that family members play a crucial role in treatment decision-making (Akechi et al., 2012; Friend & Alden, 2021; Miyashita et al., 2020).
Studies looking at older adults’ general views and opinions about ACD and EoL preferences indicate that respondents have a positive attitude toward advance decisions about medical treatments, and consider them to be important, despite the relatively low rate of completion (Vilpert et al., 2018). Sociodemographic variables affecting their opinions and attitudes toward planning for EoL are: advanced age, higher education level or socioeconomic status, being unmarried or living alone, higher religiosity, cultural characteristics, perception of shorter remaining life expectancy, poor self-perceived health, personal experiences with EoL situations or death of a loved one, exposure to life-prolonging care practices (Korkmaz Yaylagul et al., 2023; Wilson et al., 2013). Most of the studies emphasize the importance of the timing and place for the discussions, and highlight the role of the family in the process (Korkmaz Yaylagul et al., 2023).
However, there are fewer studies on the personal factors that predict older adults’ decision to complete formal ACD. These studies showed that completion is positively associated with older age, multiple chronic conditions, and higher education level (Kwak et al., 2019), religiosity (Bazargan et al., 2021; Carr & Moorman, 2009), lower fear of death (Dobbs et al., 2012), knowledge regarding medical situations at the end of life (Meier et al., 2023), death of close relative or friend, having cared for a dying person (Wilson et al., 2013), and having been involved in EoL decisions for someone else (Siconolfi et al., 2021; Wilson et al., 2013).
Interpersonal factors, such as interactions with significant others and health professionals, have also been studied in research. In an Australian survey, the strongest predictor of ACD completion was having spoken to someone about it (notably a physician or one’s children), indicating that this is an important step in the EoL decision making process (Sellars et al., 2020; Siconolfi et al., 2021). On the other hand, participants who had spoken about their preferences to their partner were half (OR = .49) less likely to have completed their ACD in a formal and written way. According to Sellars et al. (2020) it is likely that respondents considered it sufficient to have verbally communicated their preferences to their partner, since he/she would be legally called upon to fulfill the role of surrogate in the event of a medical crisis. This result also reflects the widespread belief among people that their mandatary (mostly spouse or children) knows their treatment preferences, either because they have discussed it together, or simply because they consider that close relations know them well enough to know what they would like. Similarly, older adults who lived with their children were less likely to have completed written ACD than those living alone. It is interesting to note that, in a study by Bazargan et al. (2021), 50.0% of the sample said they did not discuss their wishes about EoL treatment with the person(s) who they wanted to make decisions for them if they were no longer able to do so, due to serious illness. Therefore, it is not surprising that studies report important discrepancies between older adults’ wishes for the end of their life and their relatives’ view about the elderly’s preferences (Bollig et al., 2016; Koss & Jensen, 2020; Lulé et al., 2013; Winter & Parks, 2012). Research also examined the quality of the relationship with the person most likely to become a substitute. For example, couples (18–64 years) who foresee a long and stable future together are most likely to engage in EoL planning (Moorman et al., 2014). The feeling or the fear of being or becoming a burden to others is also likely to influence EoL decisions (Roesinger et al., 2018). Finally, a recent study showed that personal/cultural values (e.g., self-reliance or interconnectedness) appear to affect a patient’s preparedness to participate in ACD discussions, and are predictors of patient preference for family involvement in ACP (Friend & Alden, 2021).
Previous studies have mostly investigated the individual variables (e.g., sociodemographic, personal experience with illness or EoL issues) that may influence willingness to make ACD. However, the end of life is rarely an individual event; it occurs within a social context of family, significant others, friends, and caregivers. Nonetheless, very little data exists on the more contextual and interactional aspects that might play a role in older adults’ choice of whether or not to complete ACD. A qualitative study is a good way of investigating such factors and their connection. This article therefore focuses on what makes older adults decide whether or not to write ACD, and on the role played by loved ones in this process.
Method
Data presented in this article stem from individual interviews carried out within a three-step (focus group, individual interview, and self-administered questionnaire), mixed design study which took place in three French-speaking states (Fribourg, Geneva, and Vaud) of Switzerland. Participants were over 65 years old – which is the threshold for retirement in Switzerland – living at home. They were first contacted through our field partners (i.e., associations of older adults, and health and social services providers) who gave them information about the study. A member of the research team contacted those willing to participate to explain the study and verify the inclusion criteria. The interviewees participated on a voluntary basis and provided written consent. At the end of the interview, participants were offered a confidential session with a geriatric psychotherapist (not a member of the research team), free of charge, should they feel the need for it. The sample was purposive in nature.
Fifteen semi-structured interviews with 18 older adults were conducted by three interviewers: three couples were interviewed jointly, according to their wishes. Saturation was deemed to be reached after 14 interviews.
Most interviews (13/15) were carried out at the home of the participants and lasted between 35 and 135 minutes. An interview guide was elaborated according to the scientific literature, the team’s professional experience, and preliminary results of the focus groups carried out with health care providers and older adults. The guide was tested through two preliminary interviews (not included in the analysis). It addressed the following topics: the definition of EoL and its meaning for interviewees; their wishes and preferences about EoL and particularly about medical treatments; any decisions they had made (which ones, context of the decisions, people involved); ACD linked to the perception of societal images of ageing, and perceived societal expectations about EoL decisions.
Field notes about the interview process, non-verbal information, and interactional aspects were written down by the interviewer as well as analytical memos concerning possible emerging themes, concepts, or aspects that would influence the research process.
Interviews were audio-taped, transcribed, and analyzed with the assistance of Atlas/Ti (version 8) using a mixed code-list (theory and data derived, constructed through regular discussions within the research team) and according to a content analysis approach. Firstly, syntheses were written for each interview according to the themes included in the interview guide or as they emerged during coding; then cross-sectional syntheses were carried out according to themes found in the literature or by meta codes emerging from the data (Gibbs, 2009). Our endeavor to establish trustworthiness was inspired by Nowell et al. (2017). Peer debriefings and team meetings allowed an audit trail to be kept and a coding framework developed. Researcher triangulation was adopted to search for themes, and personal and team diagramming (mind maps) was used to clarify and connect themes. Alternative hierarchy and negative cases were discussed. Finally, we contacted available respondents to check the fit between their reported views and the researchers’ representation of them.
Results
Participants included 13 women and 5 men, born between 1929 and 1951. Ten interviewees were married, three widowed, two divorced, and three never married. Eight out of 18 lived alone. Twelve people reported fairly good to good self-rated health (although some of them reported serious past health issues), whereas, during the interview, five people freely reported that they were suffering from a serious disease. One person gave no evaluation of her health. Occupations prior to retirement included teaching, sales, white collar work, or health services. Twelve participants were Christians (seven Catholics). They were all Swiss or European in origin.
Fourteen out of 18 interviewees saw the EoL as a period of time hindered by multiple difficulties (physical, relational, existential). Four people, on the other hand, also saw the EoL in a more positive light, as a time that offers the possibility of making an inner journey, integrating one’s life, and continuing to develop relationships and interests.
Regardless of their conception of the EoL, all interviewees expressed a clear refusal of “over-therapeutic” treatment (Castelli Dransart et al., 2022). However, not everyone had drawn up ACD. Eight interviewees had made formal arrangements, while two others had given precise instructions orally. How can we explain this discrepancy? It seems to be linked to different EoL types of planners.
End-of-Life Types of Planners and Their Characteristics.
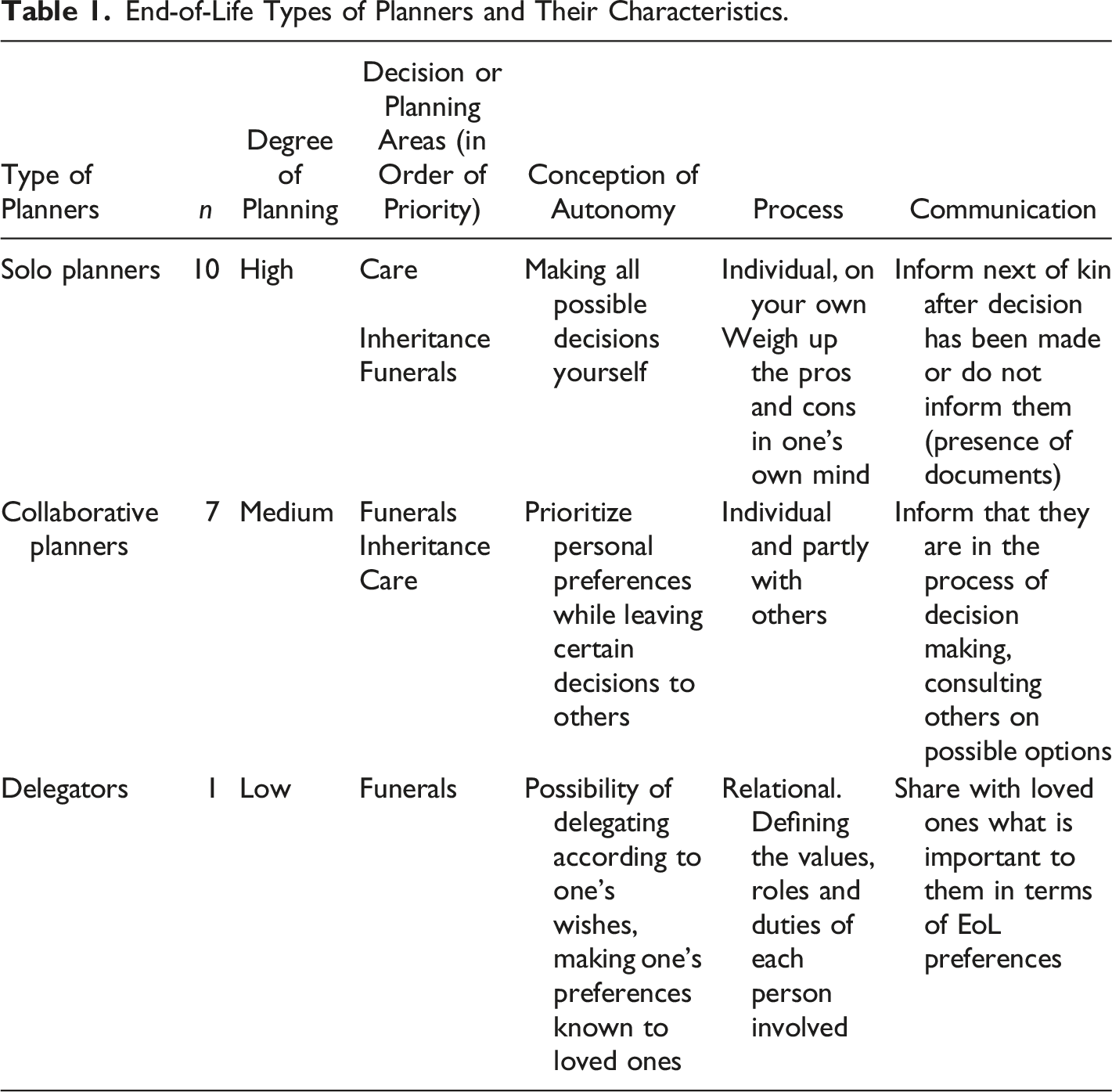
Solo Planners
Ten out of 18 interviewees were solo planners. They are characterized by a will to control their end of life as much as possible, and therefore to make precise arrangements. To do this, they anticipate everything that can be done, as long as it is important to them. They think about and make decision on all the issues involved: the treatment they want (or don’t want) at the end of their lives, the question of dependency and possible institutionalization, funeral rites, and the management of their estate after their death. Their anticipation is justified by the profound desire they feel, on one hand, to continue to be in control of their lives (and their bodies) until the end and, on the other, not to put their loved ones in delicate or even conflictual situations. Such desires take concrete form in the written and often detailed wording of their wishes, as well as in the practical organization of their implementation. The decisions and arrangements reflect, above all, their preferences. For them, autonomy means positioning themselves as individuals, taking charge of their own lives and being responsible for their own choices. They believe that it is up to them alone to determine what is right for them and what is not, and that they are free to take the necessary measures to realize their wishes. For example, HA says “I would like to die with my eyes open” (HA, p. 15), which he understands as follows: “…means remaining responsible to the end as long as you can. It means choosing, deciding and trying to do the best you can. That’s [what] open eyes [means].” (HA, p. 16)
Generally speaking, others (family members or professionals) are not directly involved in their decision-making process, with the possible exception of spouses, although the interviewees may take them into account when implementing their decisions. “[I talked] with my wife. But no, not with my children. I’m not the patriarch who rules their lives and, conversely, they’re not my guardians. On the other hand, I live with my wife. But I keep them informed…” (HA).
Decisions are therefore made privately by the person, or at most privately between the partners. There are exceptions: the wife in the OA couple became aware that her husband had drawn up ACD during the research interview. Children are generally neither involved in the decision-making process, nor consulted beforehand. They are usually informed when decisions are made, and documents drawn up: “Yes, they know (…) But we can’t say we’ve involved them. They know what we’ll do” (OA, husband).
While aware that total control over EoL issues is not assured, these people nevertheless wish to make use of the means available to them and use all their room for maneuver.
The ten solo planners share certain characteristics (at least three of the following four): a high level of education, having exercised important responsibilities in their professional lives, already faced with EoL issues, or suffering from personal health problems. This group also seems to benefit from a network of contacts developed during their professional lives, enabling them to be well-informed about ACD.
For most of the interviewees in this group, it was either a long personal experience of illness, or the concrete observation of a difficult EoL for a loved one, or their role as caregiver, that were decisive in making ACD. These experiences lead them to project themselves concretely into EoL circumstances. As a result, it seems easier for them to imagine what they might or might not feel and wish for in such circumstances.
All of these people, like HA, have said to themselves at one time or another: “I’ve got to think about putting my affairs in order, too”, so as to “avoid causing unnecessary problems and trying to ensure that things go as smoothly as possible for the heirs, or simply for the children. Death shouldn’t be an occasion for conflict”. (HA)
While decision-making may seem an eminently personal process for this type of planners, they nonetheless see making ACD and arrangements as a way to avoid creating problems for others.
Collaborative Planners
Seven interviewees adopted a more circumscribed type of planning. While they all have EoL preferences, and some of them have already made some arrangements or plan to do so in the near future, their planning does not go so far as to determine all the options, and does not settle all the details. Similarly, arrangements have not been made for all the areas potentially involved, with priority given to funerals and inheritance issues. For these interviewees, it’s important to exercise their autonomy but they consider that there are limits to what they can do or plan. On one hand, they take into account the very present notion of uncertainty about the EoL, and on the other, they keep their loved ones informed and even involve them in their reflections.
The notion of uncertainty seems to be at the heart of this type of planners. While these interviewees are willing to make a few arrangements, they systematically emphasize that life involves a great deal of the unknown/unforeseen, and that it is not totally controllable by human beings. Indeed, most want to decide, “but not too much”, as DV puts it.
Anticipating one’s death, facing it head-on, writing ACD, registering with EXIT (a Right to Die Association) – these are all steps that make sense to RO: “intellectually, I say it’s the right thing to do”, she says. Nevertheless, drawing on situations experienced by loved ones, the interviewee asserts that absolute control is not possible at the EoL, nor would it even be desirable in her eyes: “it would be horrible to control everything like that”. Her desire to make her own choices coexists with the awareness that there is an element of “irrationality” that she can live with: “There has to be a little fuzziness” (RO). RO also questions the definiteness of her wishes: “Maybe, at that time, when I’m at the end of my life, when I’m tired, when I’ve had enough, when I want someone to take care of me, to do everything for me, etc., maybe at that time, I won’t think the same” (RO).
Uncertainty is also evoked by the OE couple (born in 1938 and 1936), who would like to “finish gently at home”, but who put this possibility into perspective: “We don’t know our fate. (…) We don’t know if we’ll keep our heads or not. We don’t know and that’s better” (Couple OE).
While the couple have made some decisions about their funeral arrangements, they have not drawn up a will, as there is “nothing of value to inherit”, nor have they completed any ACD on the subject therapeutic obstinacy. While the wife maintains that preparing for one’s death, planning for the end of one’s life, is a good thing, she also believes that it should be done along broad lines: “So, you can’t have something very precise in your head either “I want this, I want that”, it’s impossible. It doesn’t make sense to me. It doesn’t make sense, that kind of project” (wife of the OE couple).
To explain her position, she offers an analogy with the game of Scrabble: “I make up a word (ed.in my mind) and, “Ah, that’ll work.” But two others still have to play. Too bad. They’ve put the pieces where I wanted to put them. But that’s the way the future is. It’s always different from what you think. We don’t know our destiny” (wife of the OE couple).
The notion of uncertainty alone does not explain these people’s relatively circumscribed planning. Not planning everything is also a way for these people to take others into account, to leave them room for maneuver or not impose constraints on them: “I think I’d rather control them (ed. the decisions), but not too much. Because once I’m gone, well, I wouldn’t want to impose on those who are left, in this case my daughters, desires that would be difficult to fulfil, such as scattering my ashes in the desert of I-don’t-know-what (…) I’d like things to be as simple as possible, given we know each other. I'd trust them to take decisions and initiatives on my behalf (…). Because I don’t think they’d make any serious mistakes. But still, to make life easier for them, I’m going to try to spell out or write down a few advance provisions” (DV).
In addition, these interviewees want to rely on healthcare professionals to help them make their decisions. For example, RO doesn’t want to decide on her own, especially in situations where her prognosis could be life-threatening: “I think that if it were a medical issue, I’d trust the doctor I know and trust (…) with his suggestions, his influence on the choice of treatment, for example. I wouldn’t trust the family for that because I think there are other things at play, which wouldn’t necessarily be the best (…). But sometimes, when you’re ill, you like to rely on someone else’s competence and not have to decide (…) we’ve gone a long way towards making patients more responsible. At some point, the patient isn’t aware of everything, and doesn’t necessarily know what to do (…). Especially in certain situations, I’d say “Listen, you’re the one who knows this, not me” (RO).
Interviewees who follow this planning logic are looking for a balance between fulfilling their personal wishes, taking into account the uncertainty associated with the end of life, and considering the situation of survivors. A number of them have actively involved children in the decision-making process, which they see as eminently relational, unlike the solo planners. As EM puts it: “In these circumstances, should you think of yourself first?”
As with the solo planners, the interviewees who subscribe to this logic have been exposed to situations that have shown them the usefulness of planning certain kind of things in order to avoid delicate situations. However, unlike the former, the collaborative planners have seen and been marked by the limits of planning. These experiences have played a decisive role in their personal reflections.
Delegators
The analyses revealed a third type of planners, although only one person belong to this. We present it here because it is clearly distinct from the other two types of planners.
DU claims to value her autonomy, which she has exercised, for example, by having chosen the treatments she underwent to cure the cancer she suffered, or by organizing her daily life as she saw fit. However, neither she nor her husband had made any concrete ACD for the end of their lives, either in terms of care or inheritance. Yet, according to the doctors, her husband is terminal and at the end of his life. Their children are aware of their financial situation and “in any case” she says, “there won’t be much to divide up”. Moreover, DU has made it clear to the children that she does not wish, nor her husband, to undergo prolonged curative treatment. However, she hasn’t given any more precise indications in terms of acceptable or unacceptable care. The reason DU hasn’t written ACD is that she feels they are better suited to people who live alone, have little family, or have poor family relationships: “It means that there are families where people don’t talk to each other, I think”. She believes that in a family where people love, trust, and communicate with each other, there’s no need to put their wishes formally in writing. She feels she can count on her children: “If there’s anything, they are the first to come and help”.
There is another reason why she does not think ACD are necessary: while she plans to rely on the medical profession to provide advice and comfort at the end of life, DU relies above all on her faith to live out her last moments. As a practicing believer, she “trusts in God” and hopes and believes that she will “receive graces as she dies”. DU also believes in an afterlife, and that she will not be alone when she dies: “So, they would say (ed. people who had near-death experiences) what we noticed every time, that is, every time, every person who had this experience, was greeted on the other side by someone from their family. “He said,” You’ll never arrive up there alone. You’ll always be welcomed by someone, different maybe, but by someone. For me, it confirmed everything I think…” (DU).
EoL control and anticipation are not at the heart for this type of planners. This participant’s autonomy consists of deciding whom to trust, in what area or under what circumstances: she has given indications of her preferences, focusing mainly on her values and the meaning she gives to her life, rather than on very precise or concrete directives. She constructs a framework within which she believes her loved ones can situate their decision-making about her. The couple assumes that their children know them, and that by virtue of the affection between them, they will know what their parents need, want or don’t want when the time comes. Autonomy here means deciding to delegate part of one’s decision-making to a third party (a relative or professional) for certain aspects, where there is room for maneuver in full awareness of the facts, and trusting in God for what one feels is beyond one’s control. To a certain extent, trust also goes hand in hand with “accepting that one is diminishing in certain respects…“: “There are some decisions you just can’t control, you see. Sometimes things change in life; things you have to change. That’s what life imposes on you. It’s not people, it’s life” (DU).
Discussion
The results of this study indicate that some older adults think about the EoL, and are prepared to some extent to discuss it, but that their reflections do not necessarily translate into firm decisions or formal arrangements in the form of written ACD. Indeed, just over half of those interviewed had formally completed written ACD. This trend was also observed in other studies, in Switzerland (Vilpert et al., 2018) and Australia (Buck et al., 2021), that indicated that only around one-fifth of people aged 65 and over have completed ACD. Our higher completion rate might be explained by the recruitment process that focused on the theme of EoL decisions and ACD among older adults.
Nevertheless, all interviewees had given some thought about the advisability of planning or making arrangements for their end of life, whether in terms of care, funeral arrangements or wills. The data from this study revealed three types of planners regarding EoL decisions: that of the solo planners, that of the collaborative planners and that of the delegators. These various types reflect different conceptions of autonomy and the role allocated to loved ones in the decision-making process.
For the solo planners, autonomy is conceived as an individual process that is predominantly rational. Making arrangements means considering one’s wishes and weighing them up against the advantages and disadvantages perceived by the individual. The decisions made were the result of personal reflection and a desire to shape the end of life to the greatest possible extent. In these cases, loved ones were not involved in the deliberation process; at most, they were informed once the decisions and arrangements had been made. These older adults were also generally unwilling to discuss their thoughts with health and social care professionals, unlike Sellars’ participants (Sellars et al., 2020). This vision of a controlled death is particularly prevalent in the upper economic strata of the population, where a culture of foresight is widely practiced, and is even perceived as an extension of “good manners” (Comby & Grossetête, 2012). Indeed, most solo planners have a high socio-educational level and have exercised significant responsibility in their professional lives. Faced with the “risks” associated with the end of life - for example, the risk of suffering, the risk of being cared for when you don’t want to be - these people (who have personally experienced illness or that of a loved one) want to be far-sighted and willingly submit to the invitation, even the social incentive, to anticipate their end of life and express their choices in this regard.
For the collaborative planners, autonomy is conceived and experienced as a contingent, interactive process. Older adults carry out their own reflections, but involve their loved ones in the process, who can play a role in determining the preferences of the planners. This situation was highlighted also in other studies (Carr & Moorman, 2009; Dening et al., 2013; Lulé et al., 2013; Winter & Parks, 2012). Some older adults find it difficult or pointless to prepare for hypothetical situations and to make decisions due to the uncertainty of future health conditions or life events (Etkind et al., 2017; Fan et al., 2019; Glaudemans et al., 2019; Korkmaz Yaylagul et al., 2023; Vilpert et al., 2018; Zhu et al., 2020). Taking this uncertainty into account is therefore a central element of this type of planners.
For the delegators, the focus is placed on personal values and meaning given at the end of life, rather than on decision-making for precise situations. Like the participants in Seymour et al. (2004) and Sellars’ study (2020), the person is open to discussing EoL issues with their loved ones, but wants them not only to be their spokespersons, but to make the decisions when the time comes because of the trust bestowed upon them. The person delegates a certain number of concrete decisions to their loved ones, particularly those concerning EoL care, as did the participants in Bazargan’s study (2021) who chose the response modality: “I trust my family to make decisions for me”. It may be that for this participant, trusting her loved ones is more comfortable both cognitively and emotionally. However, it’s important to recall that only one participant, whose husband is seriously ill, has adopted this type of planning. Consequently, confirming this type of planning in other studies will be necessary.
The qualitative results of this study are interesting in several respects. The presence of various types of planners is likely to call into question the presuppositions underlying legal frameworks and certain professional practices regarding ACD. In Switzerland, at least, these are most often based on a highly individualistic, rational vision of EoL decisions, founded on the principle that the concerned person has clear, unambiguous wishes and should fully assume their role as responsible citizens taking proactive decisions (Haesen & Shaw, 2018). Seemingly, after a rational process of weighing up advantages and disadvantages, preferences are translated into self-determined decisions recorded in written documents. However, ACP is very much influenced by uncertainty (Etkind et al., 2017; Levoy et al., 2020; Scott, 2022; Seymour et al., 2004).
The collaborative planners and delegators show that ACD are also likely to be influenced by social and relational factors. In fact, they are often the result of specific relational configurations and negotiations in which a variety of dimensions come into play, such as living conditions and resources (both material and symbolic); experiences of other people’s lives and end of life; people they can rely on, and the nature of the relationships and modes of communication they maintain with them (relatives or professionals). In fact, for the collaborative planners and the delegator, the communication with loved ones, its depth and quality is a key issue (Moorman et al., 2014; Seymour et al., 2004). In this respect, our study, like others, shows that, while they would like their loved ones to make their preferences known to the nursing staff, older adults do not often make them explicit in a concrete or in-depth way (Sellars et al., 2020). Conversations about the end of life, which are intended to ease decision-making for others, do not always result in completing formal ACP (Siconolfi et al., 2021).
Moreover, several studies point to discrepancies between older adults’ wishes for the end of their life and the perceptions of their loved ones on that matter (Bollig et al., 2016), as well as the discrepancies between older adults and their loved ones with regard the quality of life. Although interviewees repeatedly said they would like to communicate more with their loved ones on this subject, in reality, this is rarely the case. According to Siconolfi et al. (2021), the most common motivation for ACP is the desire to ease decision-making for others. In their study, it was associated with engaging in informal ACP, but not with completing formal ACP (Siconolfi et al., 2021). One potential explanation is that the motivation to reduce the burden of decision making for others is strong enough to promote conversations, but perhaps not strong enough to promote formal planning, a task that involves multiple actions. Or yet, older adults may consider that having spoken to their loved one suffices.
These results suggest that it would be desirable for professionals to take the different types of planners into account, so as to provide older adults with the best possible support (Seymour et al., 2004). Rather than inviting all of them to reflect rationally on their preferences, and record them in a formal written document, it would be preferable to know the characteristics and values, wishes and motivations of the populations concerned (Friend & Alden, 2021; Seymour et al., 2004) and to train health and social care professionals to identify the configurations of factors at work in decision-making processes (Levoy et al., 2020). Indeed, decision-making processes can take a variety of forms and, depending on people’s values and ways of functioning, may integrate various contextual and affective aspects (Friend & Alden, 2021). The diversity of logics at work in EoL planning should be matched by the diversity of support provided by professionals. Finally, it is equally important to note that the way in which ACD are framed is likely to influence the type of intervention people choose for their end of life (Park et al., 2020). It would therefore be desirable for professionals to be trained not only in the content of EoL decisions, but also in the communication and interactional aspects.
This study has some limitations. Firstly, the size and the relatively homogeneity of the sample. The interviewees had a rather similar profile: French-speaking, European culture, retirement pensions allowing them to live comfortably, if sometimes modestly, and generally satisfied with life (except for two participants), in spite of sometimes serious health problems. The second limitation includes the methods of recruitment used (through field partners and snowball effect) and the probable selection bias. The fact that only one person falls into the delegator logic could also suggest that the way researchers framed the call for participation perhaps induced a selection bias. It is possible that only those who made some kind of arrangement felt concerned by the study. In fact, professional activities of some of the co-authors suggest that the delegators are indeed present in the field, albeit in a small minority within the present sample. Another reason why delegators may be more reluctant to speak out may be the fact that this kind of planning and vision is not very much valued in Swiss society, which is heavily influenced by notions of individual responsibility and autonomy.
It would also seem necessary to carry out studies on populations less homogeneous than our own, as well as longitudinal studies. These could provide an insight into the emergence and evolution of planning intentions. Nonetheless, this study reported various types of planning adopted by older adults to make EoL decisions, and highlighted some crucial issues they face when confronted with ACD.
Footnotes
Acknowledgments
The authors wish to thank the participants, the field partners and Mrs Sabine Voélin who contributed to the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by HES-SO (Haute École Spécialisée de Suisse Occidentale) under grant HES-SO 59171/TS-RAD16-18.
