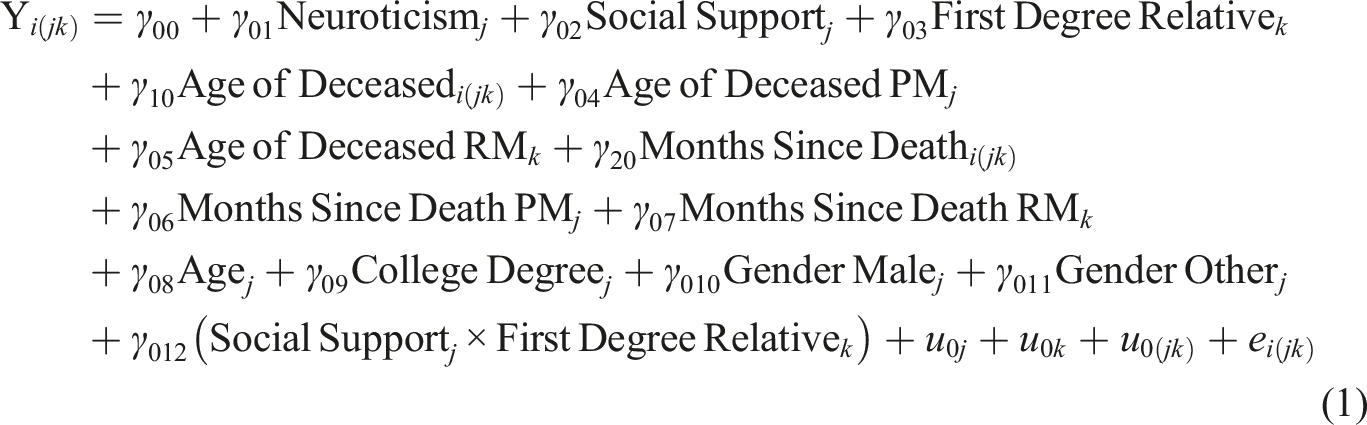Abstract
The COVID-19 pandemic left many people grieving multiple deaths and at risk for developing symptoms of complicated grief (CG). The present study is a prospective examination of the role of neuroticism and social support in the development of CG symptoms. Findings from cross-classified multilevel models pointed to neuroticism as a risk factor for subsequent CG symptoms. Social support had a stress-buffering effect, emerging as a protective factor following the loss of a first degree relative. More recent loss and younger age of the deceased were both independently associated with heightened CG symptoms. Results from the present study provide insight into heterogeneity in CG symptom development at the between-person level, and variability in CG symptoms within individuals in response to different deaths. Findings could therefore aid in the identification of those at risk for the development of CG symptoms.
Introduction
Bereavement is a universal human experience that has become increasingly common in the wake of the COVID-19 pandemic. Excess mortality attributable to the pandemic has left large swaths of the population grieving the death of one or more loved ones (Snyder et al., 2022). Despite the ubiquity of the stressor, bereavement can elicit responses that range anywhere from little or no distress to intense and prolonged suffering that can lead to significant impairment in functioning—the latter phenomenon often referred to as complicated grief (CG; Bonanno & Kaltman, 2001; Burke & Neimeyer, 2013; Shear, 2015). Where an individual falls along this continuum when faced with a specific loss is informed by a wide array of intrapersonal, interpersonal, and contextual factors. The urgent need to identify such factors has increased in light of projected increases in CG symptoms occurring as a result of the pandemic and initial evidence corroborating this effect (Eisma & Boelen, 2023; Kustanti et al., 2023). Importantly, identification of risk and protective factors must involve considering characteristics of the bereaved, the deceased, and factors unique to a given relationship (Burke & Neimeyer, 2013; Stroebe et al., 2006). In the present study, we examine how individual differences in neuroticism and social support among the bereaved, as well as factors associated with a given instance of bereavement including relatedness, length of time since death, and age of the deceased may have contributed to CG symptoms during the pandemic.
Neuroticism is a personality trait that reflects an individuals’ tendency to interpret and react strongly to negative events. Similar to the construct of negative affectivity, the trait is associated with a range of adverse psychological and physiological outcomes (Lahey, 2009). High levels of neuroticism have been associated with the development of CG symptoms following bereavement (Burke & Neimeyer, 2013; Goetter et al., 2019), including in the context of the pandemic (Breen et al., 2021; Subhasree et al., 2023). Such evidence led us to hypothesize that neuroticism would serve as a risk factor for heightened CG symptoms among the present sample. In contrast, we expected social support, a nonspecific protective factor associated with positive adaptation across multiple indicators of well-being (Holt-Lunstad, 2022), to play a role in CG outcome, independent of neuroticism. Social support is generally associated with lower CG symptoms (Burke & Neimeyer, 2013; Lobb et al., 2010), and a well-established body of work points to perceived availability of social support as a driver of its beneficial effects (Feeney & Collins, 2015; Thoits, 2011; Uchino et al., 2012). Shaped largely by past experiences of support elicitation and receipt, and early experiences of attachment, perceived availability of social support is a psychosocial resource that is relatively stable within individuals over time (Furukawa & Shibayama, 1997; Sarason et al., 1986; Thoits, 2011). As such, we hypothesized that high levels of this resource would be associated with lower CG symptoms.
While there is evidence that perceived availability of social support can prospectively protect against the development of CG symptoms, prior research has often focused on social support assessed after a loss has already occurred (Burke & Neimeyer, 2013; Stroebe et al., 2005; Van Der Houwen et al., 2010). Despite being relatively stable, perceived availability of social support can fluctuate following major stressors, often reflecting changes in support provision by one’s social network in response to the needs of the bereaved (Logan et al., 2018; Thoits, 2011). As such, perceived availability of social support assessed post-loss may be confounded with distress associated with bereavement (Lotterman et al., 2014; Robitaille et al., 2012; Schwarzer & Leppin, 1991). Discrepancies in timing of measurement may contribute to the inconsistent stress-buffering effects of social support reported in the bereavement literature (Bolger & Zee, 2019; Stroebe et al., 2005). As such, examination of how social support assessed as an intrapersonal resource may prospectively buffer against CG following loss is warranted.
Stress-buffering models are premised on the assumption that perceptions of support availability can decrease perceived threat, and increase perceived ability to cope in stressful encounters (DeLongis & Holtzman, 2005; Lazarus & Folkman, 1984). Derived from this reasoning is the hypothesis that the protective effects of social support will be most pronounced under conditions of heightened stress (Cobb, 1976; Schwarzer & Knoll, 2007). One such condition of heightened stress in the context of bereavement occurs when the death is of a first-degree relative. The death of a first-degree relative typically generates greater stress and life disruption than the death of a more distant family member or someone who is non-kin (Armstrong & Shakespeare-Finch, 2011; Fernández-Alcántara & Zech, 2017), and support is expected to be particularly important to grief outcomes under these high stress conditions. Support for a stress-buffering model would be provided by evidence that the association between social support and CG is stronger (more inversely related) when the death in question is that of a first-degree relative.
Relatedness to the deceased individual is one factor unique to a given relationship often associated with CG (Fernández-Alcántara & Zech, 2017). However, other factors unique to the deceased individual can also predict CG symptoms in the bereaved. For example, younger age of the deceased is often associated with CG symptoms (Lobb et al., 2010; Mason et al., 2020), including in the context of the pandemic (Chen & Tang, 2021; Selman et al., 2022). Similarly, the length of time that has elapsed since the death can predict CG symptoms given that in most cases, CG symptoms and other indicators of distress will alleviate as individuals adapt and adjust to changes brought on by the loss (Bonanno et al., 2002; Long & Bonanno, 2020). In the present study, we examine these factors alongside individual differences in the bereaved (social support and neuroticism), to gain a comprehensive understanding of how these variables came together to predict CG symptom development in the context of the pandemic. Our analyses provide insight into the roles of these factors in both CG variability within individuals by considering individuals’ responses to multiple deaths, and within relationship categories (e.g., friend, cousin, mother, etc.) by considering the responses of different individuals to deaths of the same relationship type. Furthermore, we examine how stress-buffering may help to explain CG outcomes by considering how a feature of the relationship to the deceased (status as a first-degree relative), may result in greater protective effects of the perceived availability of social support, a resource tied to the disposition of the bereaved. In doing so, our study answers the call for more idiographic approaches in the study of major life stressors such as bereavement (Doré & Bolger, 2018; Piper et al., 2011) while identifying potential risk factors for CG symptoms in the context of the pandemic.
Methods
The present work uses data from a longitudinal study on coping with the COVID-19 pandemic (Morstead et al., 2022; Zheng et al., 2021). Demographics, neuroticism, and perceived social support, were assessed in a baseline survey that was available beginning in March 2020. As part of the longitudinal study, a monthly survey distributed in May 2022 asked if participants had experienced the death of a loved one in the time since the COVID-19 outbreak had been declared a pandemic by the WHO (March 2020). Of 1371 respondents, 578 indicated they had experienced the death of a loved one since March, 2020. Those who responded affirmatively were sent an additional follow-up survey in June 2022 inquiring into the death (or deaths) they had experienced. This survey contained items pertaining to participants’ relationships with the deceased and experiences of grief, along with the age and date of death of the deceased individual(s). For participants who reported experiencing the loss of multiple people in their networks, survey questions were repeated with reference to each death reported (for up to five deaths). Participation in the study was voluntary and no compensation was offered. Informed consent was obtained from all participants and the study protocol was approved by the UBC Behavioural Research Ethics Board (H20-01061).
A total of 381 individuals responded to the follow-up survey and confirmed that at least one loved one had died within the specified time frame. Of these respondents, 358 remained after listwise deletion on study variables. An additional 73 respondents were excluded from the present analyses as they joined the study after having already experienced one or more deaths within the time frame examined. The final analytic sample was therefore composed of 285 participants. Apart from being slightly younger and more likely to be women, the analytic sample did not differ from non-respondents (i.e., those who experienced bereavement but did not respond to the follow-up survey; see Supplemental Table 1 for group comparisons). Of the analytic sample, 144 participants reported their experiences with more than one death. This resulted in 533 unique observations/CG scores, each reflecting the experiences of a participant with regard to a specific death. In addition to non-independence introduced by observations being nested within participants, non-independence was also induced by multiple assessments being of the same relationship-type (e.g., friend, cousin, mother, etc.). The nesting of observations within two non-hierarchically structured units (participant; n = 285, and relationship; n = 22) resulted in a cross classified data structure as depicted in Figure 1. Cross-classified multilevel data structure. Note. Figure depicts measurements of complicated grief (y) as belonging to two higher-level clustering units: Participant (j), and Relationship (k). These clustering units are treated as random factors (modelled as random intercepts) in cross-classified multilevel models.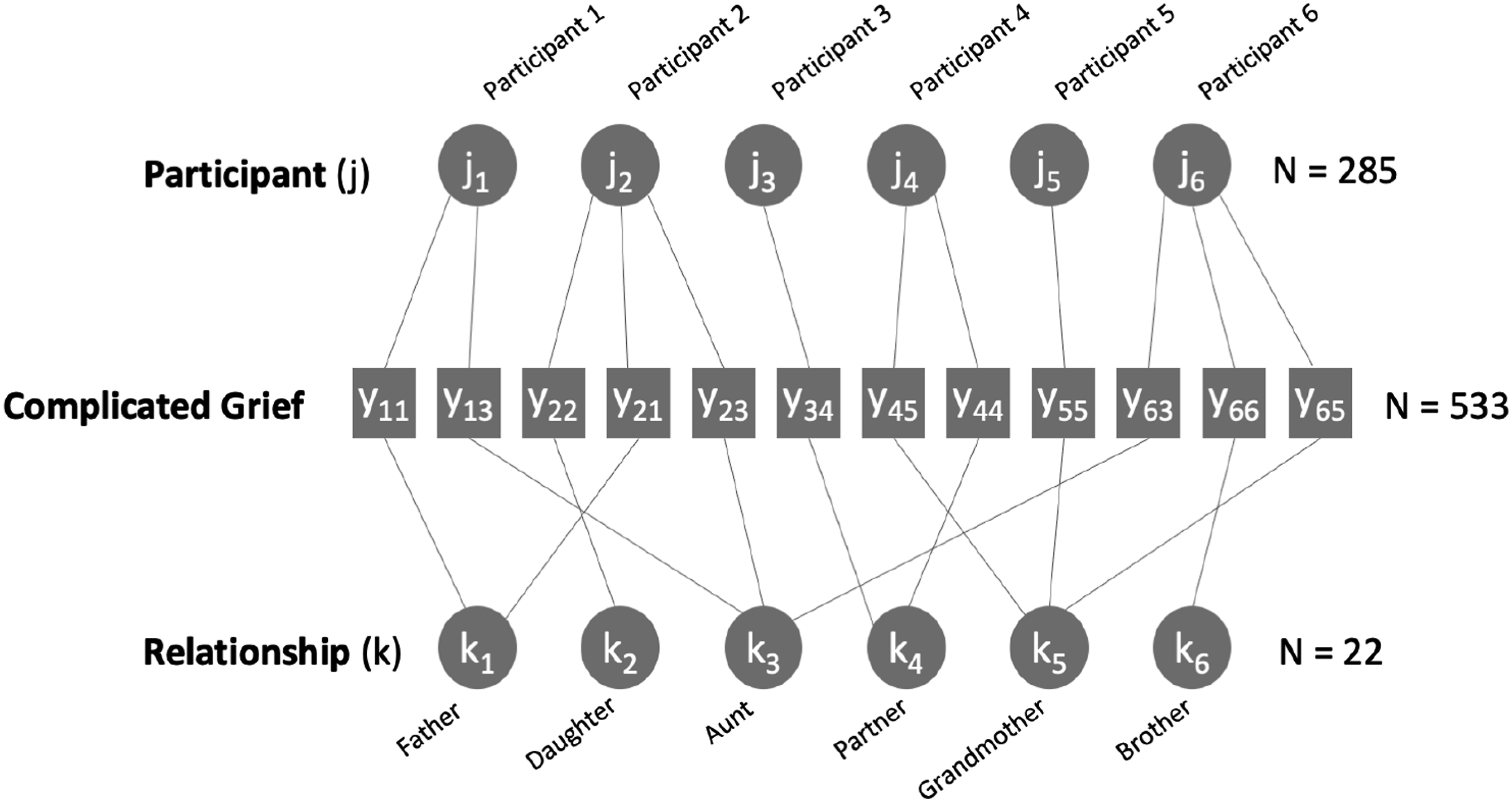
Measures
Social Support
Social support was assessed in the baseline survey using items from the Interpersonal Support Evaluation List (ISEL-12; Cohen et al., 1985). Six items were selected based on their applicability to the context of the COVID-19 pandemic, and in some cases were adapted to avoid statements that might conflict with efforts to avoid infection (such as avoiding physical contact). For example, the item “If I decide one afternoon that I would like to go to a movie that evening, I could easily find someone to go with me” was excluded. Similarly, the item “If I were sick, I could easily find someone to help me with my daily chores” was amended to read “If I were sick, I could easily find someone to help me.” Participants responded to each item on a 4-point Likert scale ranging from 1 (definitely false) to 4 (definitely true) and the mean across the six items was computed for each participant. Internal reliability of the scale (ωt) was .83.
Neuroticism
Neuroticism was assessed in the baseline survey using the 2-item neuroticism scale from the 10-item version of the Big Five Inventory (BFI-10; Rammstedt & John, 2007). Respondents were asked to rate their agreement (from 1 = strongly disagree to 5 = strongly agree) that they are someone who “gets nervous easily” and “is relaxed, handles stress well.” The latter item was reverse scored, and the mean of the items was computed to obtain a neuroticism score. The scale was chosen to reduce participant burden while retaining strong validity. The BFI-10 has been widely used, and has similar predictive validity as the full 44-item version (Rammstedt et al., 2021; Thalmayer et al., 2011). Among the present sample, internal consistency (ωt) was .69.
Degree of Relatedness
In the follow-up survey, participants were asked to provide their relationship to each individual that had died. This was assessed with a multiple-choice question consisting of a list of relationship types, and responses were used to create a binary variable indicating if the individual was a first-degree relative. This variable took the value of 1 if the participant indicated the deceased individual was their mother, father, child, brother, sister, or spouse/partner and zero if not (indicating that the individual was either a more distant relative or non-kin).
Age of Deceased
The age of each individual who died was also reported in the follow-up survey. This was assessed using a multiple-choice question with discrete age brackets but is included in the analyses as a continuous variable ranging from 1 (under 18) to 9 (85 or older). The decision to provide a range of discrete categories rather than assess age continuously was made to allow for the possibility that some participants may not have known the exact age of the individual who died (e.g., if it was someone with whom they were not particularly close).
Months Since Death
In the follow-up survey, participants were also asked to report the year and month of death for each individual that had died. From this information, the number of months that had passed since each death at the time of survey completion (June 2022) was computed. This variable was included in the analyses to account for the recency of each reported death.
Complicated Grief
CG reactions to each death were assessed in the follow-up survey using the Brief Grief Questionnaire (BGQ; Ito et al., 2012; Shear et al., 2006). The BGQ has five items, four of which reference grief in response to a specific individual (e.g., “How much are you having trouble accepting the death of ______?”). Because participants who reported multiple deaths completed the measure multiple times, the one item that does not reference a particular individual (“How much does your grief interfere with your life”) was adapted to refer to each specific loss (“How much does your grieving for ______ interfere with your life?”). The name of the deceased individual in question (provided by participants earlier in the survey) was then piped in to the blank space for each scale item. The survey software (Qualtrics) cycled through the names provided as participants progressed through multiple iterations of the items. Participants responded to the items on a 4-point Likert scale ranging from zero (not at all) to 3 (a great deal). The sum across all items was then taken to compute a scale score for each reported death. Internal consistency of the scale (ωt) was .88.
Participant Demographics
Demographic characteristics of participants including age, gender, and educational attainment were assessed in the baseline survey. In the analyses, age was included as a continuous predictor. Gender was included as a dummy coded categorical variable with three levels (men, women, other) with women as the reference category. Educational attainment was included as a binary variable with 1 indicating that the participant had obtained a 4-year bachelor’s degree in college, and zero indicative of having less than a bachelor’s degree.
Analyses
After examining univariate and bivariate statistics for study variables, we used cross-classified multilevel modelling to test study hypotheses. This approach allowed us to partition variance attributable to both sources of non-independence/clustering (participant and relationship) as well as their interaction (Goldstein, 1994; Rasbash & Goldstein, 1994). The approach also guarded against bias introduced into variance and standard error estimates by neglect to model cross classified data structures (Meyers & Beretvas, 2006). To obtain the intraclass correlation coefficients (ICCs), we first ran a model excluding all predictors. This unconditional model contained random intercepts for participant, relationship, and their interaction. Including a random component for the interaction was feasible as participants were able to report multiple deaths from within the same relationship category (e.g., if multiple friends had died). We then tested a model containing all predictors of interest (main effects model), and a model with these same predictors in addition to the hypothesized interaction (interaction model). The interaction model is presented in equation (1). We used restricted maximum likelihood (REML) to estimate all models. To compare the main effects and interaction models using a likelihood ratio test, we re-fit the models using maximum likelihood (ML) estimation. We included only random intercepts in models as including random slopes resulted in failures to converge.
In equation (1) (interaction model),
Results
Univariate and Bivariate Statistics
Participant Univariate and Bivariate Statistics.
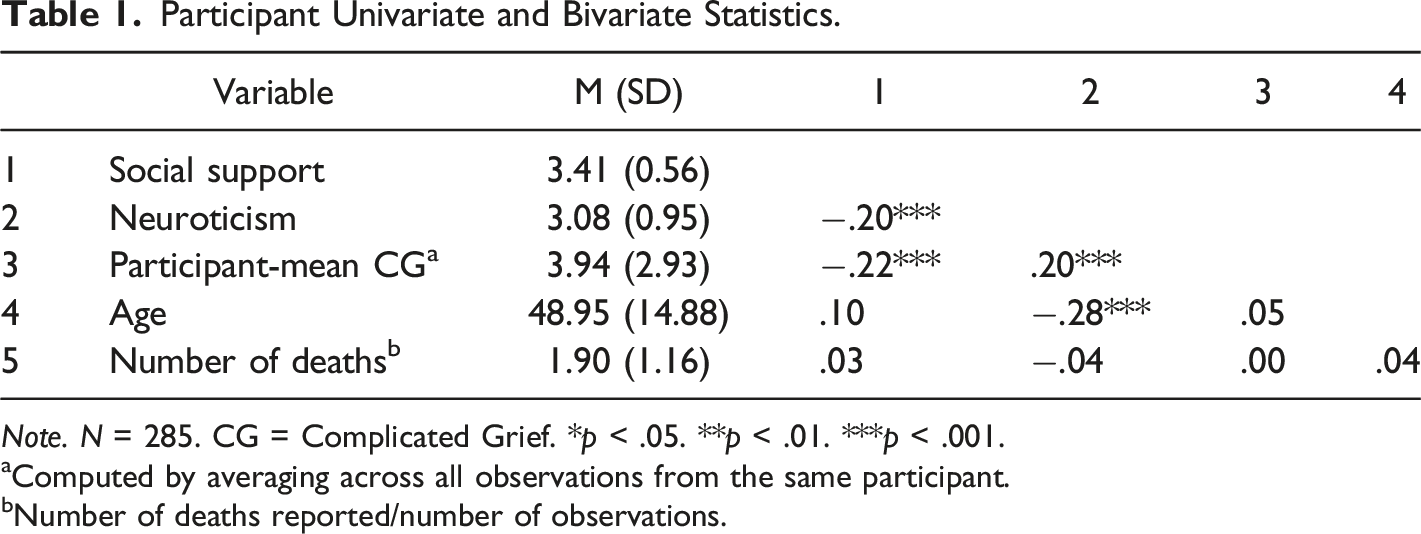
Note. N = 285. CG = Complicated Grief. *p < .05. **p < .01. ***p < .001.
aComputed by averaging across all observations from the same participant.
bNumber of deaths reported/number of observations.
Mean Complicated Grief Score Broken Down by Relationship Type.
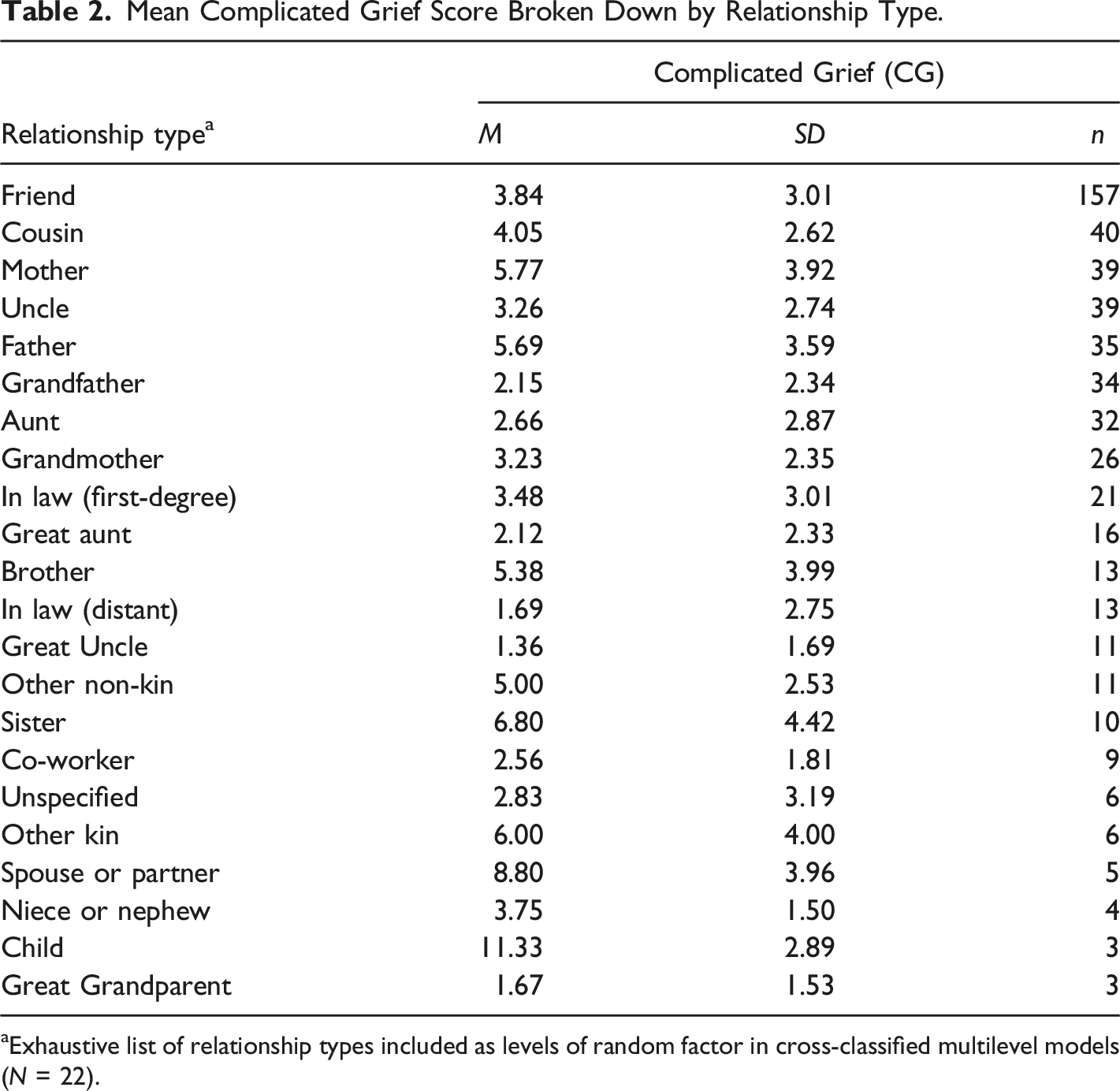
aExhaustive list of relationship types included as levels of random factor in cross-classified multilevel models (N = 22).
Multivariate Analyses
Cross-Classified Multilevel Models Predicting Complicated Grief.
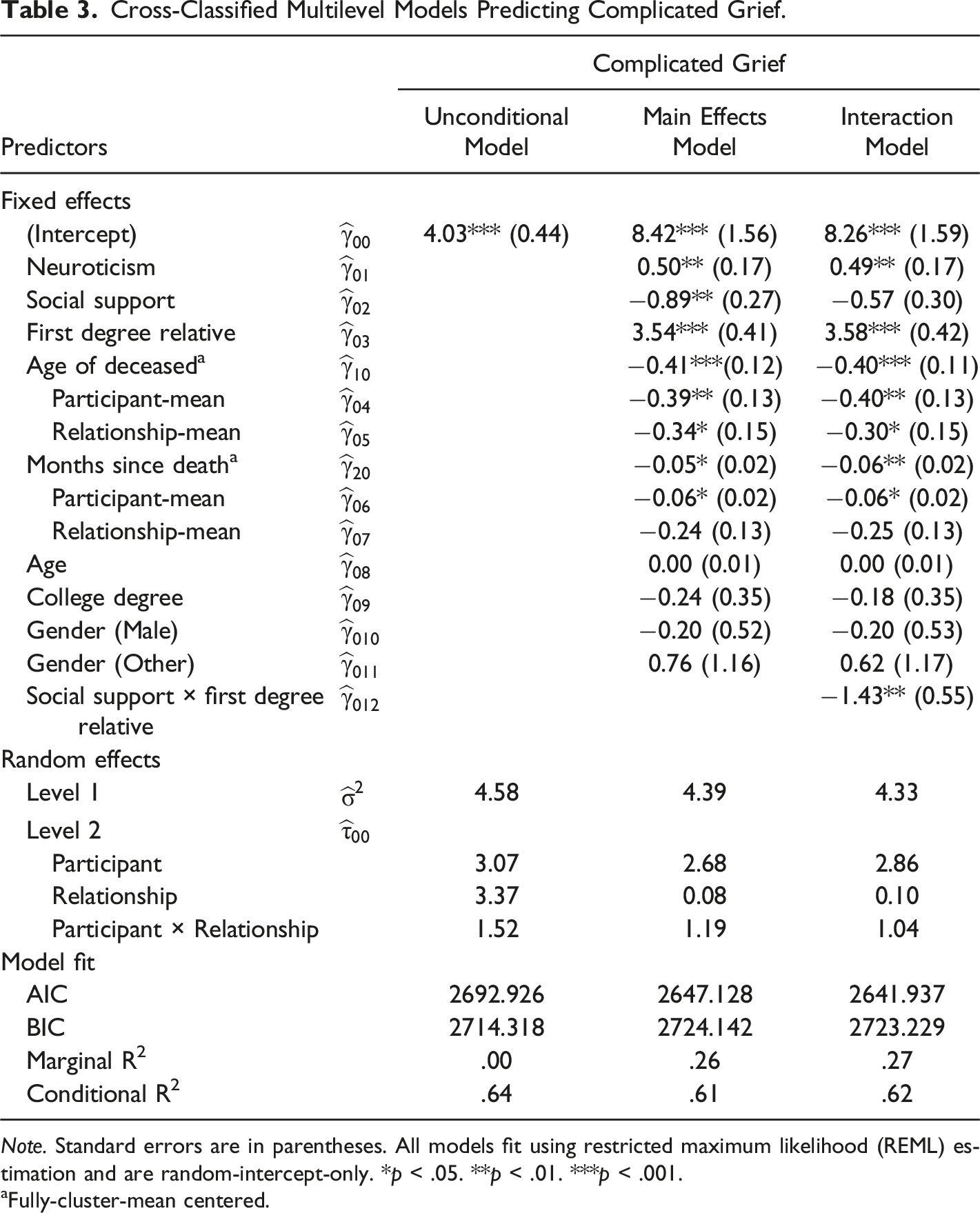
Note. Standard errors are in parentheses. All models fit using restricted maximum likelihood (REML) estimation and are random-intercept-only. *p < .05. **p < .01. ***p < .001.
aFully-cluster-mean centered.
Estimates of fixed effects from the main effects and interaction models (Table 3) indicate that, holding all other variables and random effects constant, neuroticism was significantly positively associated with CG. In addition, characteristics unique to each death—namely, age of the deceased and months since death—had independent effects on CG. Older age of the deceased was significantly associated with reduced CG at the within-cluster level (i.e., relative to the average age of the deceased individuals reported by the participant, and relative to the average age of deceased individuals of the same relationship type). Older age of the deceased was also significantly associated with reduced CG both between participants and between relationships (i.e., CG scores from participants who tended to report the deaths of older individuals, and CG scores pertaining to relationships in which the deceased tended to be older, were lower). Similarly, more time since death was significantly associated with lower CG at both the within-cluster level and between participants.
In the main effects model, social support had a significant main effect and was associated with lower CG. Degree of relatedness also exerted a main effect with first-degree relative status being a significant predictor of greater CG. The interaction model that included the product of these variables, however, resulted in significant improvement in model fit (χ2(1) = 6.38, p < .012). The interaction is depicted in Figure 2 and reveals a significant association between higher social support and less severe CG response when the deceased individual was a first-degree relative (p < .001). The effect was reduced and did not significantly differ from zero when the deceased individual was a more distant relative or non-kin (p = .06). As a sensitivity analysis, we re-ran our models including additional covariates that were not central to the study aims, but that could conceivably have contributed to CG outcomes. Specifically, we controlled for whether the cause of death was an accident or COVID-19, as well as if the participant was residing in North America. Inclusion of these variables did not change the direction or significance of the variables of interest (see Supplemental Table 2). Effect of baseline social support on complicated grief outcome moderated by degree of relatedness. Note. Social support variable is centered. Degree of relatedness is dummy coded with 1 indicating that the deceased individual was a first-degree relative. Interaction between social support and degree of relatedness is significant (p = .010).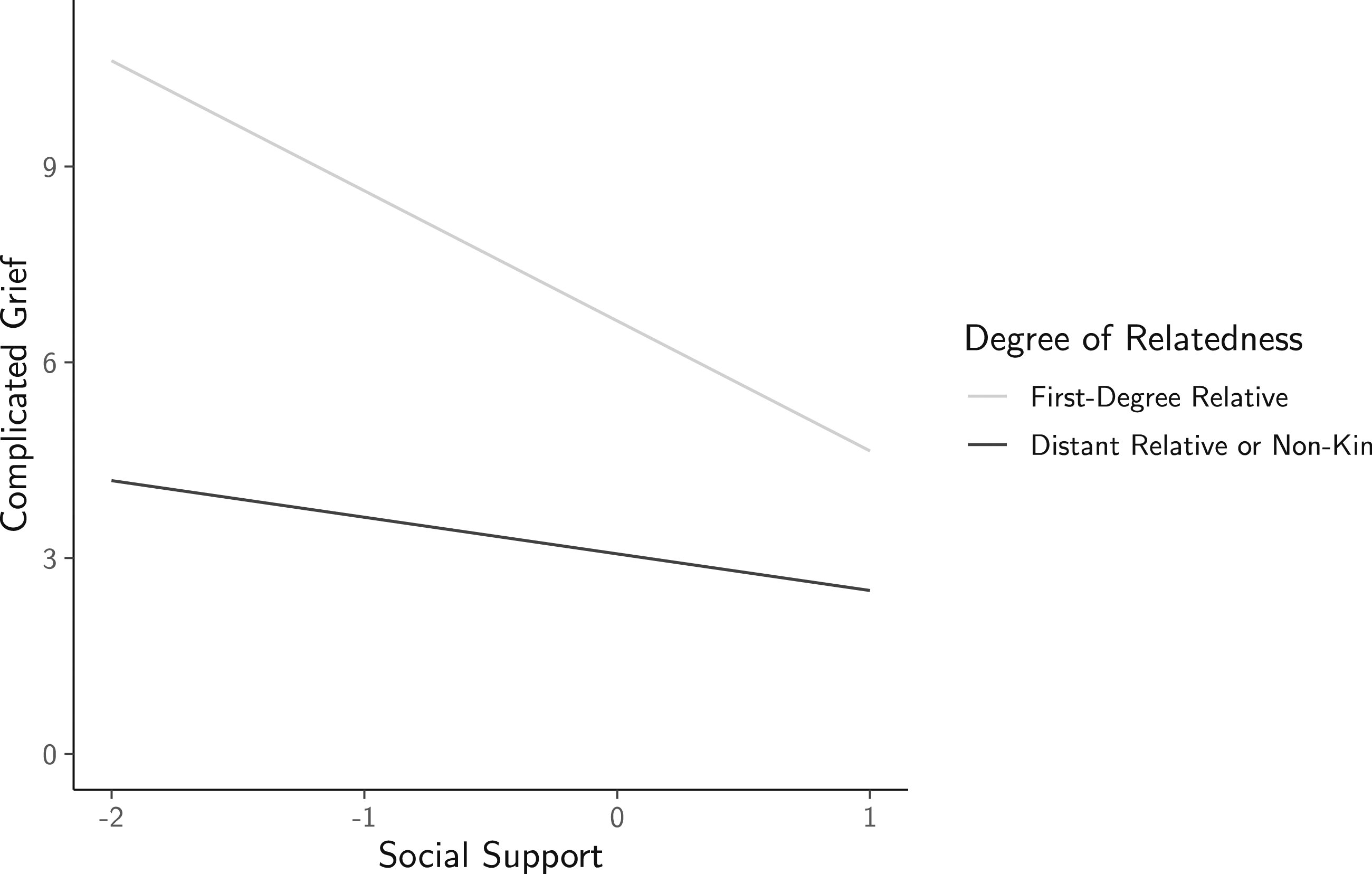
Discussion
In line with study hypotheses, neuroticism and social support emerged as psychosocial factors relevant to the development of CG symptoms in the context of the COVID-19 pandemic. Independent of phenomena characterizing unique instances of bereavement (degree of relatedness, age of the deceased, months since death), individual differences in neuroticism and social support had, respectively, prospective positive and negative associations with CG symptoms. The effects remained controlling for sociodemographic variables (i.e., age, gender, educational attainment), and in sensitivity analyses that accounted for place of residence and cause of death, increasing confidence in the observed effects.
With regard to neuroticism, our results support conceptualizations as a non-specific risk factor for a range of adverse psychological and physiological health outcomes (Lahey, 2009), including poorer psychological adaptation following loss (Kuhn & Brulé, 2019; Wijngaards-de Meij et al., 2007). As a personality trait, neuroticism is largely impervious to change over the long-term, including in response to bereavement (Bühler et al., 2023). That said, our prospective assessments guarded against the possibility that neuroticism scores reflected temporary perturbations in distress following loss (Ormel et al., 2012). Similarly, in assessing social support prior to bereavement, we were able to examine its role as an intrapersonal resource, and capture its protective effect while avoiding the conflation with distress that can occur when the construct is assessed following a major stressor such as bereavement (Thoits, 2011). For instance, an individual may elicit more support from their network if they are highly distressed by a loss, thereby temporarily inflating their perception of support availability (DeLongis & Holtzman, 2005; Hobfoll, 2010; Lazarus & Folkman, 1984). By designing our study to avoid this potential confound, our findings support the role that social support availability may play in guarding against CG symptom development post-loss. In doing so, the results also provide insight into how social support may have conferred benefit in the context of the pandemic, a time when the benefits of social support may have been less robust than in pre-pandemic contexts (Mitchell et al., 2022).
In addition to the main effect of social support, our analyses revealed a significant interaction between social support and degree of relatedness. Specifically, we found that the association between high social support and reduced CG symptoms was driven by reports of CG pertaining to the death of a first-degree relative, whereas the effect was nonsignificant when the death in question was that of a more distant relative or non-kin. This result is in line with stress-buffering models (Cobb, 1976; Schwarzer & Knoll, 2007) in that the protective effect of social support was stronger when the loss was a close relative, which has been found to be highly stressful (Armstrong & Shakespeare-Finch, 2011; Fernández-Alcántara & Zech, 2017).
In the present study we drew on the well-documented finding that the death of a close relative typically generates greater stress and upheaval than the death of a more distant relative or of someone who is non-kin (Armstrong & Shakespeare-Finch, 2011; Fernández-Alcántara & Zech, 2017). The stress-buffering effects in the present study are in line with those from a recent cross-sectional study among incarcerated individuals which similarly found a stronger protective effect of social support among those who had lost an immediate family member compared to those who had lost a more distant relative or friend (Fahmy et al., 2023). In applying this test of stress-buffering to social support assessed prospectively among a community sample, our findings expand on this work and highlight the capacity for social relatedness to serve as a factor that can be used to test stress-buffering models in bereavement contexts. This approach may help to explain the inconsistent results that have previously emerged in the literature on stress-buffering models in bereavement which often use different methods for tests of the effect. For example, approaches to examine post-bereavement adaptation in longitudinal datasets include testing interactions between social support and time or bereavement status (Anusic & Lucas, 2014; Stroebe et al., 2005). Each approach provides valuable insight into the process of bereavement and our study adds to this body of work.
In contrast to the inconsistent literature on stress-buffering in the context of bereavement, two relatively well-documented predictors of distress following loss are time since the death, and age of the deceased. In general, more time since death is associated with better adjustment (Bonanno et al., 2002; Long & Bonanno, 2020). The present work supports this pattern, and reveals that this effect not only emerges at the between-person level, but also within participants responding to multiple deaths. Similarly, our finding that younger age of the deceased was associated with heightened CG symptoms—a finding that is commonly reported in the literature (Chen & Tang, 2021; Lobb et al., 2010; Mason et al., 2020; Selman et al., 2022)—emerged both within relationship categories (i.e., compared to other reported deaths of the same relationship type), and within participants (i.e., compared to other deaths reported by the same participant). The latter finding reflects a key insight afforded by our use of cross-classified multilevel modelling using data from multiple instances of bereavement collected from the same individual. Namely, it allows for the clarification of what risk and protective factors operate at the within-person level, that can help to identify the context-specific circumstances that place an individual at risk for the development of CG symptoms. This can be contrasted with risk and protective factors that operate at the between-person level (such as neuroticism and social support), and contribute to an individuals’ risk for CG across all bereavement contexts.
A few limitations of the present study should be noted. While we found that non-respondents did not differ from respondents on psychosocial variables of interest assessed at baseline, it remains possible that characteristics associated with their experiences of bereavement played a role in their attrition. For example, those who experienced greater distress or who were more recently bereaved may have been less likely to have the time or energy to complete the follow-up survey. That said, there is little theoretical reason to suspect that the direction of the associations observed among variables would differ in this sample.
The self-selected community sample also limits the generalizability of the findings beyond the population examined. Our sample was relatively homogenous, composed primarily of women, those who were college educated, and residing in North America. Given disparate rates of bereavement between populations and within populations across demographic lines—a phenomenon that has been exacerbated by the pandemic (McGowan & Bambra, 2022)—examining the role of demographic factors and testing if the present analyses replicate among diverse populations will be crucial. In particular, considering the differing characteristics of the deaths experienced by the most vulnerable populations will be key and our study provides a framework and methodology for such examination. It is only through such analyses that universal and culturally-specific risk factors for CG can be identified.
Despite these limitations, our study sheds light on key intrapersonal and social contextual contributors to grief responses during the COVID-19 pandemic. The findings not only provide insight into the heterogeneity in CG symptom development at the between-person level, but also the variability that exists in CG symptoms within individuals in response to different deaths. Findings could therefore aid in the identification of populations at risk for the development of CG symptoms.
Supplemental Material
Supplemental Material - Predictors of Complicated Grief During the COVID-19 Pandemic: A Cross-Classified Analysis
Supplemental Material for Predictors of Complicated Grief During the COVID-19 Pandemic: A Cross-Classified Analysis by Talia Morstead, Jason D. Rights, Nancy L. Sin, and Anita DeLongis in OMEGA - Journal of Death and Dying
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Social Sciences and Humanities Research Council of Canada under grant 435-2016-1350 to AD, grant 435-2019-0608 to NLS, and by a graduate fellowship to TM.
Data Availability Statement
The data that support the findings of this study are available from the authors upon reasonable request.
Supplemental Material
Supplemental material for this article isavailable online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.