Abstract
This article focuses on the end-of-life experiences of migrants and non-migrants from young to old, who died in a Canadian cosmopolitan city in the years preceding the COVID-19 pandemic. Based on interviews with over one hundred relatives of as many deceased, the authors discuss end of life issues, namely access to palliative care and medical assistance in dying. The data indicate unequal access to care at the intersection of several factors, including type of disease, patient’s age, uncertainty of their prognosis, and migrant/non-migrant status. While being young and having cancer were undeniably associated with the provision of care (curative and palliative), those who did not benefit from palliative care tended to be social minorities in the local society and suffered from diseases with ambiguous prognosis. The right to “Die with dignity” is fundamental, with or without palliative care and regardless of where the end of life takes place.
Keywords
Introduction
In 2017, Erina, a 40-year-old Canadian originally from Southeast Asia, was diagnosed with advanced ovarian cancer with little hope of recovery. The diagnosis followed a recent mastectomy for breast cancer, after two years of chemotherapy. Notwithstanding the support received at a leading hospital, Erina made the decision to stop treatment. Although she was in pain, she refused all medication and received no home care. Despite being a devout Muslim, Erina wanted to ask for medical assistance in dying, but her family, especially her mother, discouraged her from doing so. A month and a half later, she died at home, attended by her mother.
This death took place in Montreal, a plural city, where 34% of the population is immigrant (i.e. born outside of Canada, from a wide range of countries) and where religious, ethnic and, more inclusively, cultural diversity is prevalent. While literature (Kaye et al., 2019; Migala & Flick, 2018) shows that diversity affects access to and quality of care at the end of life, other elements intrinsic to social structures and organizations shape its contours: access to the health care system and to adequate needs-based care, biomedical technologies, types of illnesses and expectations, interpersonal relationships, age, gender, etc.
Beyond diversity issues, the rights of people facing the end of their lives have been legislated to make care more accessible to the broader population. This « dying with dignity » (Gouv. du Québec, 2012:11) stems from a law enacted in Quebec in 2015 stating that everyone nearing the end of their life has the right to receive care that is appropriate to their needs, regardless of their illness, age, region of residence, or place of care. In this context, what does the end-of-life experiences of people such as Erina and her loved ones reveal? What kind of care can Montrealers (by birth or adoption) expect to receive in the event of major illness with a poor prognosis? What affects their access to care?
In an effort to shed light on what “dying with dignity” entails and the issues that arise at the end of life, this article examines the experiences of migrants, children of migrants, and non-migrants from young to old who died in Montréal in the years preceding the COVID-19 pandemic. The authors discuss end-of-life trajectories and the elements that promote or hinder access to palliative care in a context of social and cultural diversity. The data and narratives presented here form a set of synchronic and diachronic scenes of experiences of dying intersected by movement between place and type of care, while taking into account the age group of the person facing the end of their life, the type of illness (or leading one), his or her group identity, religion, and language proficiency. A discussion of the findings follows, highlighting tensions between life now and sustaining life as well as differences in access to palliative care and medical assistance in dying (MAID).
Background
Medicine of the Incurable?
Despite the changing epidemiological portrait of illness due to medical advances (Carr & Luth, 2019) according to which chronic illnesses now constitute most of the public health landscape, acute illness remains central to medicine. In so doing, it generally focuses on curative activity through a variety of approaches that aim at totally or partially curing patients so that they may continue to live for variable lengths of time. Furthermore, as Krawczyk (2021) suggests, fighting disease involves both uncertainty and hope, and the way the health care system is organized remains dependent on this. However, chronic illnesses have the particularity of being incurable and as a result, people who suffer from such diseases live and die with them. This médecine de l’incurable (medicine of the incurable) (Mino et al., 2008) is a kind of rescue medicine that allows patients to live better (or less poorly) with disease. In so doing, palliative care, also known as supportive care or comfort care, is part of a set of practices aimed at health-related quality of life (Radbruch et al., 2020), that is, symptoms, well-being, and end-of-life medical care.
Notwithstanding these goals for better quality of life, many people see palliative care as the cessation of active treatment and the equivalent of death, whereas members of palliative care teams see it as a multidimensional practice (Mino & Moulin, 2021). Palliative care thus takes on different meanings depending on who is receiving or providing it. In addition, medical assistance in dying (also known as euthanasia) is a new medical practice in Quebec, available to terminally ill people with unbearble suffering. However, there are tensions between the philosophies of palliative care and those of MAID especially regarding whether MAID falls within or outside the scope of palliative care. While aiming to relieve suffering, palliative care supports the patient until (natural) death occurs, whereas MAID shortens life and is the result of the patient’s choice. Some may see this as the dying person taking control of their death and a growing pluriformity in religious and secular beliefs around death (van der Geest, 2021). Others question the legitimacy of shortening a person’s life, as it runs counter to certain interpretations of various religious dogmas (Inthorn et al., 2015; Schweda, Schicktanz et al., 2017).
Access (and Lack of Access) to Palliative Care
Even though public policies promote access to palliative care, inequalities persist (Stajduhar et al., 2019). In Quebec, eligibility criteria restrict universal access to palliative care due to limited health and social services resources and an aging population. This generates processes of prioritization of patients according to elements outside the patient’s control, such as the manifestation of acute symptoms, pain, or the presence of a poor or guarded prognosis associated with cancer in particular (Philip et al., 2019). In fact, in order to receive palliative care in a hospital unit or palliative care home in Quebec, the ill person must have a guarded prognosis of three months or less. This prognosis is more difficult to establish for diseases with uncertain outcomes, such as chronic illnesses or multiple conditions. As for home care, it is for people for whom strictly curative treatments are no longer appropriate.
These administrative and organizational barriers affect the entire population. However, some people with a precarious status, migrants, or racialized individuals encounter difficulties in accessing services. The resulting low use of formal health care services appears to be more a matter of constraints than choice (Brotman & Ferrer, 2015): lack of knowledge of the local language and services, cost and inflexibility of services, restrictions associated with migrant status and lastly, prejudice on the part of health care professionals (Torres et al., 2016).
When it comes to palliative care, studies of Canadians suffering from cancer have shown that migrants are more likely to receive aggressive care than supportive care compared to longer-term residents (Chu et al., 2021). An age-based rationale also comes into play among adult cancer patients: individuals between the ages of 45 and 75 are more likely to receive palliative care compared to those who are younger or older (CIHI, 2018). Finally, lack of awareness and negative representations of palliative and end-of-life care among both the general population and health care providers (Hawley, 2017), non-recognition of life that ends (Cable-Williams a& Wilson, 2017), and the desire, often by families, to continue curative treatments (Fortin & Lessard, 2021) are all factors in late access or non-access to this type of care.
Together, these phenomena result in the often (very) short-term stays of the dying person in dedicated end-of-life care spaces (Sercu et al., 2018) and a significant number of people dying in hospitals without access to palliative care (Walter, 2020).
Different Trajectories of Dying
The emergence and consolidation of palliative care have fostered the development of an (secular) idea that dying and death can be experienced in a “good” and “dignified” way. The place of death has become central to this image (Collier & Broom, 2021), with home perceived as the ideal place, in contrast with the hospital, which represents a technical, depersonalized, even inhuman death in the collective imagination (Driessen et al., 2021). This good death can be part of an individual or collective experience, of kinship or community (Soom Ammann et al., 2016). It can also be expressed differently depending on the position of the ill person within the family (child, parent, spouse, brother, or sister), gender, age, or social background. It is part of a trajectory, an accumulation of experiences and states of being.
These perspectives co-exist with a plurality of religious traditions, a dynamic societal context resulting from mobility and migratory movements (Foner et al., 2019), and the social transformations that accompany the globalization of exchanges of all kinds. Culture, understood as a variable set of values, beliefs and ways of being that take on meaning in a situated relational context (Cuche, 2001), plays a role in shaping practices and perspectives on dying, death, and care. This context involves close ties (family, relatives), but also relations to institutions, between migrants and non-migrants.
More than 60 years ago, Glaser and Strauss (1964) spoke of the different social value of the dying, particularly with regard to ethnicity. Closer to home, Králová (2021) reiterates status inequalities and the impact of these inequalities on the experience of care, despite the dynamism and agency of those involved. Following these paths, our exploration of dying, palliative care and MAID attempts to highlight the common experiences recounted by loved ones of the deceased, but also the particular experiences that reveal, each in their own way, the enactment of palliative and end-of-life care. This being said, Montreal’s diversity cannot be reduced to migration (although sustained by population movement), encompassing historically and politically constituted relationships of gender, age, religion (and spirituality), social status, as well as ethnicity.
In light of these trajectories, the issues of care and access to care are connected to those of dying in a context of social, cultural, and religious diversity and, more broadly, to the end-of-life experiences of sick people in all age groups.
Methods
This paper draws on the testimonies of loved ones (usually a family member) who supported a relative at the end of their life in the year preceding the interview. These testimonies, collected between 2017 and 2019 in Montréal (Quebec, Canada), provide an account of end-of-life experiences of 119 people, from young to old, through semi-structured individual interviews. We documented the end-of-life trajectories of migrants, children of migrants, and non-migrants, and the challenges their loved ones encountered along the way. These were “long” interviews (between 60 and 120 minutes) in which the themes central to our study were addressed from different angles at various points.
In order to account for experiences of care in health care settings and institutions but also capture diverse trajectories, a variety of recruitment methods were used, including posters in our university and local businesses in neighborhoods that were targeted for their diversity, recurrent visits to various organizations and religious institutions, advertisements in neighborhood newspapers, and flyers that were distributed in places such as subway station exits and popular Montréal festivals. We also contacted health care institutions and organizations in the Montréal area.
The results shared in this paper stem from both descriptive and thematic analysis of our data, in regards to palliative and end of life care, places of care, types of illness, age group of the deceased and socio-cultural variables in regards to gender, place of origin (migrant/non-migrant), religious affiliation and language proficiency. The data were analyzed both intra-corpus (within each age group) and across them, shedding light on the intricate relationship between age, type of illness, care and migrant/non-migrant trajectories.
Distribution of the Deceased According to Age Group, Gender, and Origin.
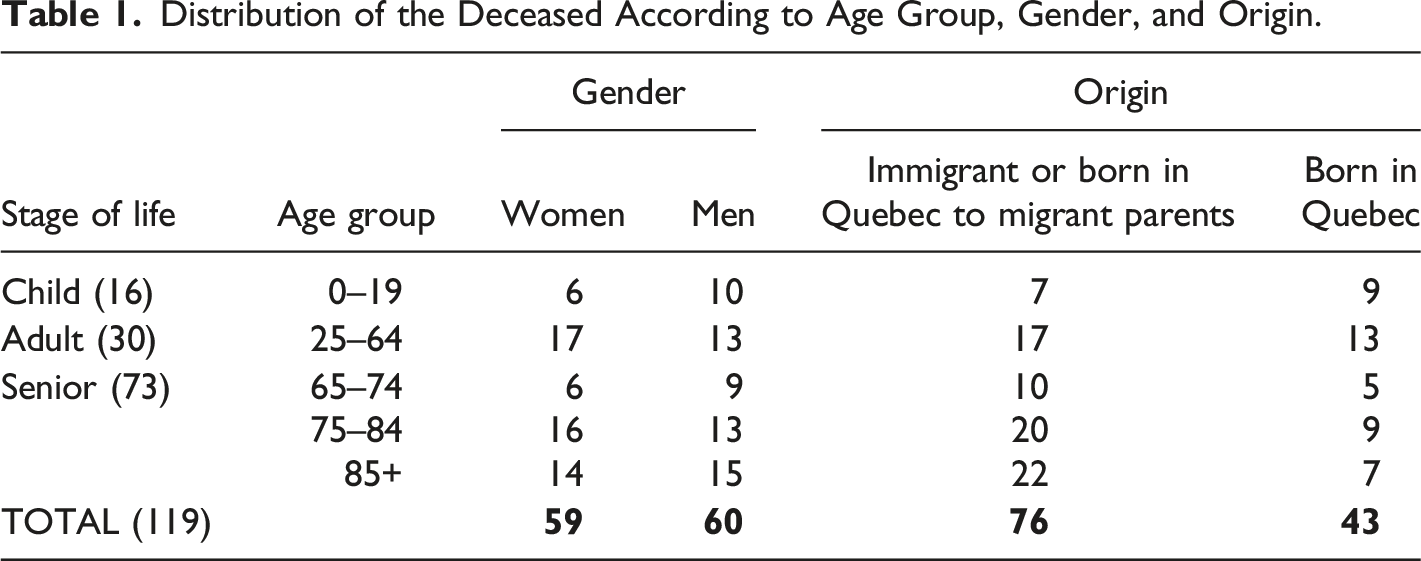
Type of Care and Illness According to Age Group.
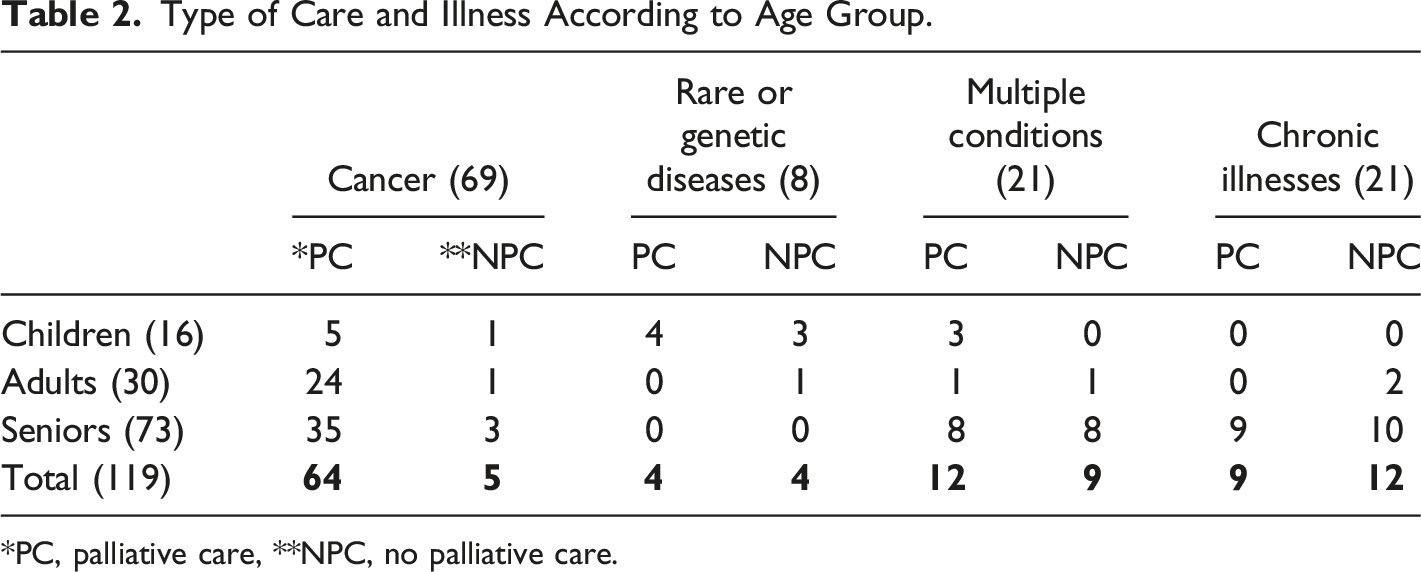
*PC, palliative care, **NPC, no palliative care.
Findings
Places of Care, Places of Death, from Young to Old
Places of care (whether palliative or curative) and places of death may differ. Eighty-nine of the deceased received comfort care (47 men and 43 women) and 30 died without it (13 men and 17 women). As shown in Table 2, the vast majority of palliative care recipients had cancer. When palliative care is provided at home, its duration seems to go beyond active dying (i.e., the last moment of life, which can be a matter of hours or days depending on the individual). Many receive such care for several weeks or even months. Receiving palliative care at home does not, however, ensure dying at home, as the majority of people who receive palliative home care die in a special care or regular unit in a hospital. In contrast, people who stay in a special care unit for longer periods of time often do not receive palliative care at home.
Two observations stand out: (1) the older people were, the less access they had to comfort care; (2) the majority of those who did not receive comfort care were migrants: 36% of migrants did not receive palliative care compared to 7% of non-migrants. Let us frame these findings from young to old.
The Children
As revealed by the children’s trajectories, the last stage of the disease led to specialized care in a respite home for children, a pediatric hospital, or at home. In all, 12 children received palliative care, including one at the very end of life (at home). Of these, 6 died at a respite home (also a palliative care hospice), 2 died at home (supported by a palliative home care team) and the remaining four died in a hospital. Of the children who did not receive palliative care, 3 died in a hospital (1 in the emergency room, 2 in intensive care), and 1 child died at home.
With one exception, care was spread out over a period of weeks, months, or even a year. The type of disease (see Table 2) seems to have influenced whether or not palliative care was received, as 3 of the 4 children who did not receive such care had genetic diseases. The fourth had cancer. Palliative care was offered to all 4 children, but the parents turned it down. They refused it because they did not accept their child’s terminal condition, associating palliative care with end-of-life care. Being a migrant, a child of migrant parents, or a non-migrant did not have any bearing on whether or not the children received palliative care. Nor did religious denomination, as the families who wished to maintain a curative approach until the end of their child’s life (Protestant, atheist or of personal spiritual beliefs) did not differ in terms of religion from the parents who opted for a palliative approach (Catholic, Muslim, atheist, Buddhist, Protestant or other). The only child, Alexia (age 10, Canadian born to migrant parents from Central America) who died in the emergency room did so under difficult conditions. Suffering from a rare genetic disease, with no physical autonomy, she was at her maternal grandparents’ home when she stopped breathing. The grandparents called emergency services and asked them to come to their home. Alexia was taken to the hospital where the do not resuscitate (DNR) forms (previously filled out by the child’s mother and father) were not respected and the parents, as other members of the family, were immediately questioned by police. While any suspicion of ill-treatment by the family members having subsequently been ruled out by the authorities, the death of this child was traumatic for her relatives, not because of the death itself (which was foreseeable in the medium term), but because they were (wrongly) blamed for her sudden death.
The Adults
The adults whose stories we collected received care in different (not mutually exclusive) settings (at home, at a private residence or hospital). The care trajectories were not linear; there was a lot of back and forth between locations depending on the progression of the disease. Unlike the children who received palliative care, the types of services the adults received differed in terms of the duration of care (we will return to this a little later). Nevertheless, a certain similarity emerges in that 24 of the 25 people who received palliative care (including 13 migrants) had cancer. In general this disease brings together seasoned care teams, often with many resources and well-defined care protocols. Only one person (a migrant with multiple health problems) of the remaining five adults received palliative care (see Table 2).
Like Erina (the 25th adult with cancer), those who did not receive palliative care (5) were all migrants or descendants of migrants. Four of them died in an intensive care unit (the fifth person died at home). In 3 of the stories, however, the deaths were unexpected (the individuals who died had multiple conditions). Among those who received palliative care (25), 14 died in hospital palliative care units and 5 in other units, 3 died in a palliative care home and 2 died at home.
Adult palliative care was provided, for varying lengths of time, at home or in a private residence, but more frequently in hospitals. Unlike the children, in almost half of the stories, palliative care was received at the same time as curative care. As for those who discontinued curative care (in favor of palliative care), the decisions were mainly motivated by the harmful side effects of the treatments or their (perceived) ineffectiveness.
Again, migrant/non-migrant status did not seem to play a role, with regard to access to palliative care for a well-defined disease such as cancer. The duration of such care varied from a few days to a few months. For those who received palliative care at the same time as curative care, the duration—although variable—was rather long (often several months) and resulted in a continuum of care from home to hospital. Those who received palliative care over a shorter period of time (ranging from a few days to 3 weeks) received it only in a hospital (the same is true among the seniors). And in this setting, those who experienced palliative care in wards other than palliative care units did so in a sporadic way and often short duration (48 hours or less).
The adults who did not receive palliative care, were all migrants and suffered from diseases other than cancer with the exception of Erina. As for faith and access (or lack of access) to palliative care, those who did not receive palliative care were Muslim, Catholic and atheist. As for the adults having received palliative care, they shared a wide range of faiths (Catholic, atheist, personal spirituality, Protestant, Jewish, Buddhist, or other.
The Seniors
Seniors accounted for more than half of the documented narratives. Like the adult group, they received care in a variety of settings (at home, in a hospital [dedicated or general unit], or in a long-term care facility). These settings were not mutually exclusive, and the duration of care varied. Fifty-two seniors received palliative care, of which 35 had cancer (see Table 2). Their care trajectories are multiple as was movement from one place to another. Palliative care at home was generally provided for a longer period of time (several weeks or even months) than in a hospital (usually a few days to a week) or long-term care home (a few hours, days, or sometimes weeks). The remaining older adults (21) who did not receive palliative care had similar end-of-life situations: they had a disease other than cancer, were over 75 years old, and were migrants.
Distribution of Seniors Who Received Palliative Care, Categorized According to Type of Illness and Place of Death.
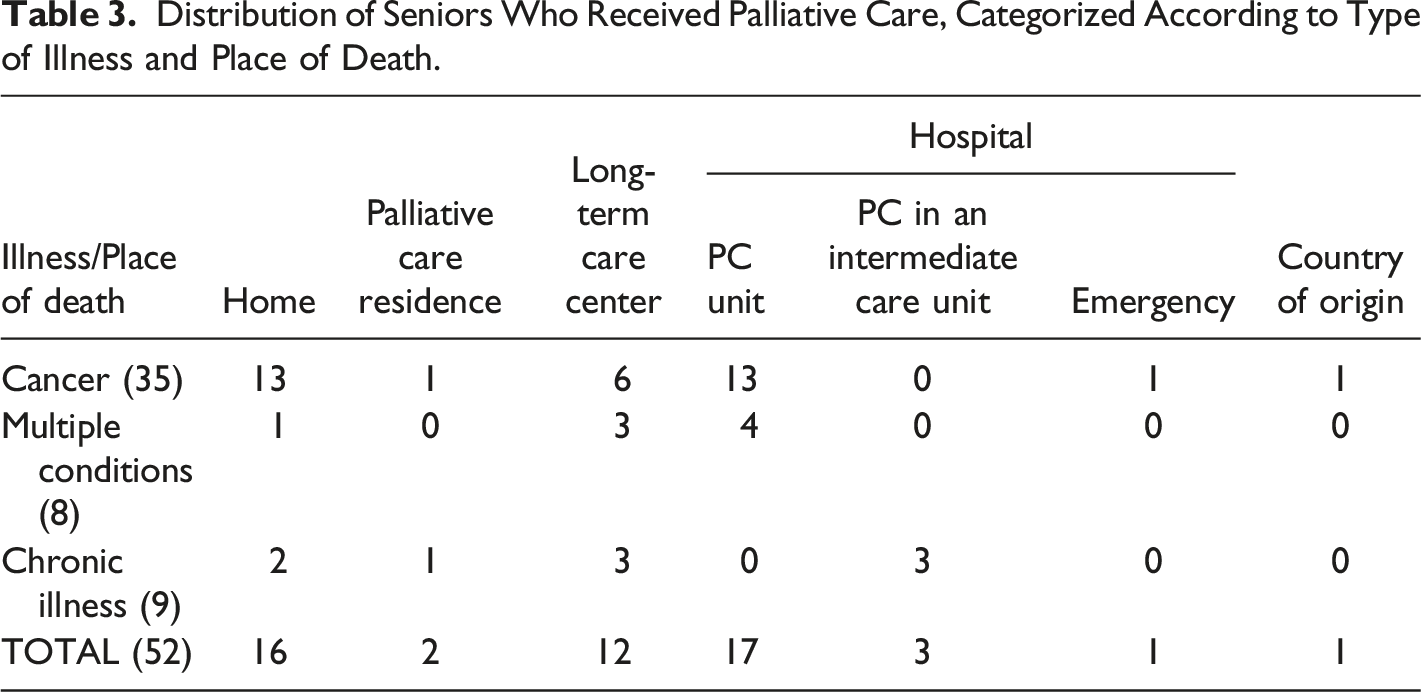
Distribution of Seniors Who did Not Receive Palliative Care, Categorized According to Type of Illness and Place of Death.
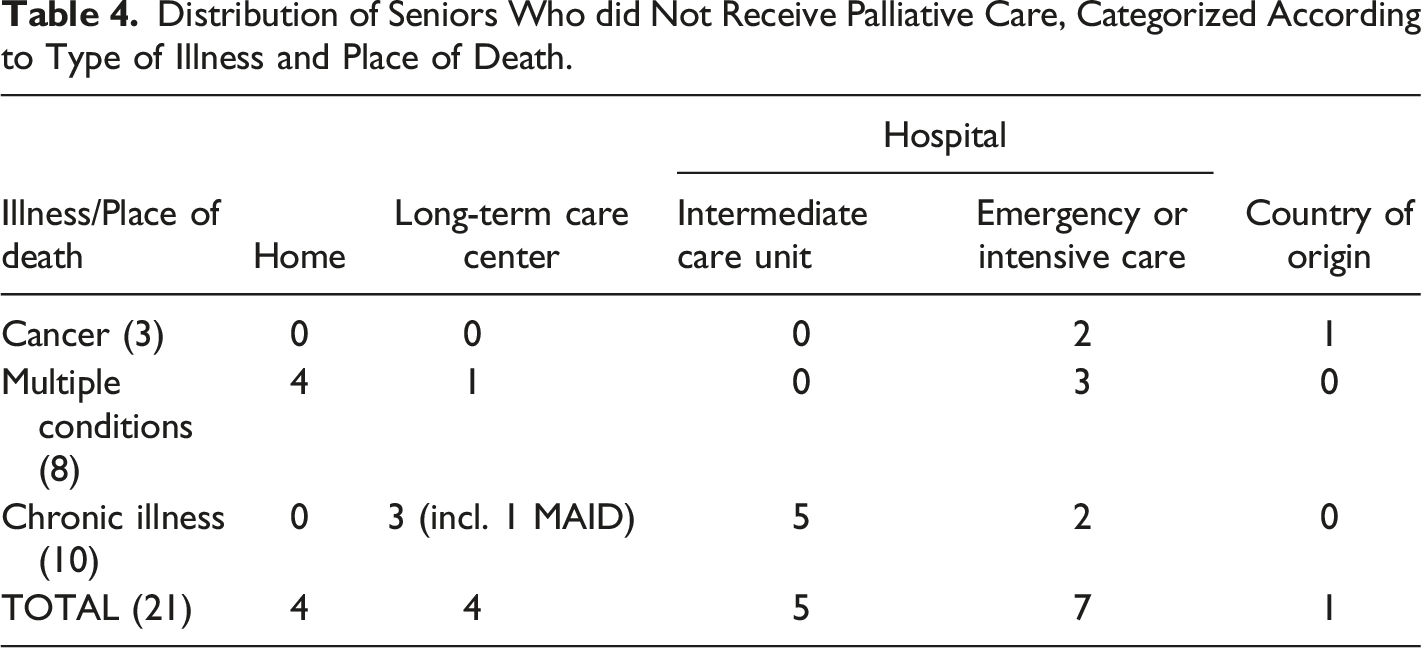

For the seniors with multiple conditions (out of a total of 16 seniors who did not have access to palliative care), the trajectory of the disease was marked by a long decline, punctuated by acute episodes requiring hospital care. Once again, most of these seniors did not get a clear prognosis. Their deaths were often described as sudden by their families; three died in a hospital (emergency or intensive care) and one died in long-term care. The other four elderly people with multiple conditions died at home, three without care for various reasons (migratory status limiting access to care, lack of available care matching the person’s needs, mistrust of health services).
The case of Da Xia’s mother is an example of an end of life without care and is a reminder of how migrant (or minority) status combined with an undefined illness can lead to a tragic death. Da Xia assisted her 81-year-old mother (both Asian born) in her final years. She spoke limited French and had been hospitalized several times due to difficulties with mobility and undernourishment. Da Xia, herself a worker in Quebec’s public health system, made several attempts to obtain home care for her mother. After a year’s wait, Da Xia turned to the private health care sector. In addition to what was perceived as a lack of support from the public health care system, Da Xia recounted the many hardships her mother faced, which added to her distress and exhaustion (as a caregiver). Her mother’s life ended abruptly: she died alone, in her own home, without receiving any care.
The disease trajectories of the seniors with advanced chronic diseases were similar to those of seniors with multiple conditions who experienced a long decline punctuated by acute episodes requiring hospital stays. As was the case for the seniors who had cancer or multiple conditions, the majority of the seniors with chronic illnesses were not yet deemed to be at the end of their lives and died following yet another intervention or transfer. These seniors died in intensive care, in regular hospital care, or in long-term care facilities.
Beyond the type of illness and the age of the individuals (the youngest seniors mostly had cancer, while other diseases were more common among those who were older), it is worth noting that all but one of the seniors who did not receive palliative care were migrants. With two exceptions (older adults who had moved to Canada less than five years ago), all of the 20 foreign-born seniors were Canadian citizens and had been in Quebec for more than 20 years. The issue of immigration status and access to public medical services was therefore relevant only for two seniors who had arrived recently, one of whom chose to return to his country of origin to die, and the other who chose to die in Montreal without formal care. Although the latter’s grand-daugther (age 58, European migrant) found the experience very difficult, she talks of her grand-father’s death (age 96, European migrant) as peaceful, away from curative medicine.
Finally, with regard to religion, besides the predominance of the Catholic faith, the seniors in our study had a variety of religious affiliations (Orthodox, Protestant, Buddhist, Muslim, Jewish, Hindu, Jehovah’s Witness, atheist and personal spirituality). However, among those who did not receive palliative care, religions other than Catholicism are proportionately more prevalent, whereas among seniors who did receive palliative care, the Catholic religion predominates.
Beyond the presence or absence of palliative care, how does MAID fit into the trajectories of care and end-of-life situations that were documented?
Medical Assistance in Dying (MAID)
At the time of our study, MAID was a recent medical practice in Quebec, legalized in 2015 (2016 in Canada) and restricted to adults. Of all the end-of-life experiences documented in our study, eight adults (7.8%) were granted MAID, while nine applicants were denied it. In comparison, 3 % of all deaths in Quebec were MAID in 2020 (with an increase of 4.7% in 2021 and 6.1% in 2022, Institut de la statistique du Québec, 2023) whereas 9% of the MAID requests were declined (Santé Canada, 2021).
The Adults
Among the adults in our study, Dalila (age 54), Camille (age 41), and Sylvie (age 64), all of whom had cancer, applied for and received MAID in a hospital setting. They were all Quebecers of French-Canadian descent (and therefore part of the majority group in our study). As Dalila’s husband recalls, Dalila chose MAID shortly after having lost her own father to cancer. He found it difficult to acknowledge her choice, hoping that she would outplay her bleak prognosis. In time and with much talk, witness to her suffering, he came to share her choice. They left the house (for the hospital), with a simple bag containing pajamas and lipstick. Dalila died surrounded by her family.
Another member of the majority group, a 54-year-old cancer patient, was initially refused MAID but was offered it later in the course of his illness. However, the patient refused it, opting instead for palliative sedation.
Three other adults (all of whom were migrants) also wanted MAID, although they did not actually request it from their caregivers. Unlike Dalila, Camille, and Sylvie, these individuals had their choice challenged by their relatives. Angelo (age 43, South American born), who had HIV and amyotrophic lateral sclerosis (ALS) and lived in a long-term care facility, wanted to apply for MAID. However, it conflicted with his sister’s religious (Catholic) beliefs. In the end, Angelo did not proceed with his application. Nicoleta (age 56, European migrant) had cancer and was being cared for at home. Her husband was strongly opposed to MAID because it went against his Jewish faith. As a result, Nicoleta did not follow through on her wishes despite having expressed them on more than one occasion. Finally, the same was true for Erina (age 40) whose mother strongly opposed MAID due to religious (Muslim) reasons.
The Seniors
Among the older adults, 5 people (migrant and non-migrant of Catholic faith or atheist) requested and received MAID: two men and three women who had cancer, ALS or a degenerative disease. For example, after four years of treatment for thyroid cancer, Suzanne (age 82, non-migrant) was able to receive MAID, without difficulty and with the support of a palliative care team, at home surrounded by her family. Differently, Yves (age 74, non-migrant with a chronic pulmonary disease as well as lung cancer) declined palliative care over medical assistance in dying (MAID). According to his partner, Yves associated palliative care and pain management to a loss of connectedness while MAID offered a “conscious” death, without suffocation (Yves’ fear). Nevertheless, MAID was granted once Yves left the hospital for a long-term care facility, after two refusals from the oncology medical team.
With regard to the unfulfilled requests for MAID, five seniors (four women and one man, four of whom were migrants) requested it, but did not receive it for a variety of reasons: the treating physician refused to support the request, other care was offered to better alleviate the pain, the person didn’t have access to public health care due to their temporary migratory status, and one woman (in the majority) requested it very late and died within a few hours of the request. Finally, one woman (a migrant) died before MAID (which had been granted) could be administered.
MAID as Care
In light of these experiences, the question of whether MAID is palliative care or something on its margins remains unanswered. Yet, while altering life trajectories, MAID remains care at the end of life (Buchbinder, 2018). Some relatives are completely in favor of it, others firmly resist it, and still others are opposed to it, making the patient’s intention to use it null and void. Although they were not opposed to it, some relatives expressed their reticence about MAID, not because the moment of death was chosen (upsetting the “natural” order of things), but rather because MAID shortened the amount of time they could spend with their loved one. For certain, the decision to move towards MAID (or to refrain from it as Erina’s story shows) is rarely an individual one, and takes place within a collective, mostly family members. Among younger patients, it is more common to discuss the issue with a spouse, while older people tend to discuss it with their children and grandchildren.
The family members who were in favor of MAID did so because they wanted to see an end to their loved one’s suffering. Conversely, the relatives who opposed MAID cited religious reasons (all religions combined) and were all migrants. For some, MAID runs contrary to the hope of a cure, while for others, MAID was seen as an obstacle to accepting the death to come, an acceptance that goes hand in hand with the uncertainty brought about by serious illness.
Of all the MAID applicants, many were recipients of palliative care. In other words, most of those who applied for MAID did not oppose palliative and end-of-life care to euthanasia. For some, the request for MAID was made in continuity with palliative care, while for others the request for MAID was a parallel, separate process.
Discussion
In a social, health, and legal context that stresses the importance of access to end-of-life care and “dying with dignity”, our study reveals unequal access to such care. Some people received palliative care over a long period of time, while others did not have access to it, or they only had access to it for a short period. Our study places this unequal access to care at the intersection of several phenomena, including type of illness, age, ability (or inability) to identify a terminal condition (uncertain prognosis), and the patient’s migrant background.
Care Across Various Age Groups and Places
Having a disease such as cancer makes it easier to access palliative care. It is a well-defined disease whose trajectory is often informed by conclusive data. Conversely, access to resources for non-oncology patients and, in particular, older adults, is unequal. Such diseases are long-term, often disabling, progressive, and slower. Certainly, unparalleled resources are available for health care services for young people, which is perhaps the opposite of what is available for the older adults (although it must be noted that in the context of our study, children with genetic and rare diseases received active care until they died). Most adults also received palliative care, especially when they had cancer and non-migrant status. This disparity between the care provided to young people and that which was or was not provided to seniors challenges the “distinction between those who deserve or are worth treating, and those who do not deserve or are not worth treating […]” raised by the philosopher Frederic Worms (2012, 29 – our translation). This gap reveals the differential value accorded to age groups and the care trajectories they entail (Fortin et al., 2023).
Life now?
The ability or inability to identify that a patient’s condition is deteriorating is also a factor in access to palliative care. Some relatives declined the offer of palliative care (largely associated with end-of-life) because they were unaware of or unwilling to accept their relative’s deteriorating condition. The refusal to accept that death is approaching is as common among parents of children with a grim prognosis as it is among relatives of adults and seniors. The whole issue of death is at play and to what extent it is conceivable—often more so for relatives than for the patient themself (Bluebond-Langner, 1978; Kirby et al., 2018). This nonrecognition can also be seen among some caregivers, who do not consider or do not want to consider that the patient is “there yet.” Despite advanced illness, hope of recovery remains a strong factor in the direction of care (Wrigley, 2019).
For many, palliative care is associated with imminent death despite a philosophy of providing the best possible care now. This latter view seems to be more common in home care, where the people in this study received palliative care over a longer period of time, in the final months and weeks of their lives (and illness) in comparison to hospital palliative care, especially in non-palliative care units such as intensive care or emergency. And as our study shows significant movement toward the end of life, from the home to the hospital in particular, this movement translates into dying “in action.” In fact, frequent transitions between various institutions do not encourage comprehensive care that lasts over time. Too often associated with the end of life, the very notion of palliative care as long-term support is obscured.
Difference in Access to Palliative Care for Adult and Senior Migrants
Diversity (social, cultural, and religious) as expressed in this study raises the question of the scope of minority status in our health care institutions, as migrants constitute the vast majority of people who did not receive palliative care. While this difference in access was not salient among children, it was more pronounced among adults and seniors, especially among those who had a disease other than cancer. Furthermore, those who received few services throughout the end-of-life stage were mainly migrants.
Understanding this difference in access is a complex issue. Although only a few people stated that they spoke neither French nor English, all of them were supported (in navigating health care services) by a relative who was comfortable communicating in one of the two languages. Access to palliative care in this context should therefore not be considered solely in terms of the relationship between the provision of care and the sick person but also in terms of the relationship between the person nearing the end of their life and their relatives, and perhaps also between the relatives and the health care professionals providing care (Durivage et al., forthcoming).
With regard to access to public health services, migration and residency status had little impact in our study, as only two people (one senior and one adult) had temporary status and therefore did not have access to public health care. However, it is plausible that migration status played an indirect role, as many of the seniors moved to Quebec to be closer to their relatives (Le Gall et al., 2021). Many did not enter the job market and lived with their children, where they helped take care of the home and their grandchildren. This leads us to question family members’ level of awareness of the health care services available to seniors nearing the end of their lives, as many of them seemed to be unaware of such services. Among adults and seniors, being non-native appears to be a factor that influences access to palliative care. However, once people access palliative care, our study does not show any differences between migrants and non-migrants in terms of length of service or quality of care.
The issue of unequal access to care certainly colors dying trajectories. We have seen elsewhere how the voices of patients and their families are unequally represented in various health care contexts (Fortin & Maynard, 2018) as not all have the same capacity to voice their concerns or to be heard. Beyond a migrant or non-migrant status, we could argue that all migrants are not equal in regards to the local majority. In the field of ethnic relations and in the context of plural societies, DeRudder and Taboada-Leonetti (2019) refer to national and cultural minorities and, more broadly, to the processes of social differentiation and hierarchization according to origin and culture, that foster racial, ethnic, religious, regional and national minorities. In this regard, migrants (and Canadians born to migrant parents) from western Europe for example may be more at ease with Quebec’s health-care system (and wider institutions, norms and practices) than migrants from the Antilles, Asia or East Africa. The social recognition of an individual, the space they occupy, and the value of this space within a given environment, as well as the mastery of local customary codes and different levels of ability to access services, all play a role in the course of the patient’s illness and their relationship with health care institutions. This issue of resources is reminiscent of the work of Glaser and Strauss (1964) cited earlier, on the variable social value accorded to a patient based on their age in particular, but also on their origins.
As for religious affiliation, it does not explicitly appear to play a role in access (or lack of access) to palliative care. However, religious affiliation does have an impact on the trajectories of requests for MAID, as such requests may be questioned by family members and in fine, abandoned by the patient out of respect for those who see it as a major breach of dogma. Certain religious traditions (or trend within a given tradition) believe that euthanasia should not be legal, but support relieving all forms of an individual’s suffering (Inthorn et al., 2015). Others, on the other hand, give absolute priority to the sacredness of life, a principle that surpasses that of individual self-determination. Discontinuation of treatment—not only euthanasia—is viewed as an “active” gesture that shortens life and is therefore considered unacceptable (Schicktanz et al., 2010). But religious traditions and degree of observance are not the only factors, as the notion of choosing to shorten life is a recent development in the local society that raises concerns among certain relatives (of all faiths) who find it difficult to accept a premature farewell.
Dying at home, with support and care, is also a question of resources. Public home care teams do a much-appreciated job (the families who received this type of care stated so unanimously). Nonetheless, dying at home involves social and economic resources that are not available to everyone.
Conclusion
The purpose of this article was to explore access to palliative care and MAID for Montrealers (whether born in Montréal or elsewhere) and to identify what shapes such access. It is apparent that age group and main illness are drivers of access to palliative care, with young people and cancer patients most likely to have access to care that combines curative and palliative perspectives. Being a migrant was a common denominator for those who did not receive end-of-life care. An array of reasoning shed partial light on this intricate result, from lack of knowledge of the available health care services to an incapacity to mobilize these resources or to choose not to. As noted earlier though, once palliative care is accessed, there is no difference in quality of care between migrants and non-migrants. Among those who did receive such care, the home as a place of care seemed to facilitate a more long-term approach, beyond active dying. Regardless of the type of care (and the inequality of access to it, especially for older adults), moving from one institution to another at the very end of life remains, whether by choice or necessity.
Beyond the units dedicated to the end of life, the hospital remains a place where many people die. Dying at home requires considerable resources, which some families and people facing the end of their lives—with or without prognosis—may lack. Could we therefore conclude that, regardless of the place where care is provided, connectedness with health care providers are key elements in “dying with dignity”? Perhaps the relationship that arises from care is more significant than the care itself whether curative or palliative? Unequal access to palliative care is no less important as is the right to “die with dignity”, with or without palliative care regardless of where end of life takes place.
Footnotes
Acknowledgments
The End-of-life Experiences in a Plural Montréal study includes researchers and practitioners from diverse backgrounds (![]() ): S. Fortin, J. Le Gall, I. Olazabal, G. Mossière, L. Rachédi, and P. Durivage in close collaboration with M. E. Samson, S. Lessard, B, Mathiot, T. Bytyqi, and S. Ouadfel, and earlier, J. Fuentes Bernal, P. Gagnon, V. Kayayan, É. Develey, C. Goglio, J. Simard, and M. Cliche-Galarza. A. Simard, M. Drolet, C. Sigouin, and J. Desrochers complete the team with their expertise in health care environments. We sincerely thank all our colleagues, without whom this study would not have been the same.
): S. Fortin, J. Le Gall, I. Olazabal, G. Mossière, L. Rachédi, and P. Durivage in close collaboration with M. E. Samson, S. Lessard, B, Mathiot, T. Bytyqi, and S. Ouadfel, and earlier, J. Fuentes Bernal, P. Gagnon, V. Kayayan, É. Develey, C. Goglio, J. Simard, and M. Cliche-Galarza. A. Simard, M. Drolet, C. Sigouin, and J. Desrochers complete the team with their expertise in health care environments. We sincerely thank all our colleagues, without whom this study would not have been the same.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Social Sciences and Humanities Research Council of Canada (SSHRC, 2017–2022), grant no. (435-2017-0678).
Ethical Statement
Author Biographies
