Abstract
Methamphetamine use is increasing in the Australian population. It has a known association with violent and erratic behaviour and with an increased risk of unnatural deaths. To determine whether victims of homicide have significant exposure to methamphetamine 100 randomly selected de-identified homicide cases from 2012 to 2021 were accessed from the Forensic Science SA (FSSA) Pathology Database to determine the type of homicide and whether methamphetamine was detected in the blood. A total of 76 males and 24 females were found (M:F = 3:1). Of these, 30 victims (30%) had methamphetamine detected in blood, consisting of 26 males and 4 females (M:F = 6:1; male age range 18–53 years, average 36.8 years; female age range 28–63 years average 44.8 years). Levels of methamphetamine ranged from 0.02 to 3.3 mg/L with an average of 0.64 mg/L, with the highest numbers of positive cases occurring in victims of gunshot wounds (45.5%), and the lowest in those with lethal blunt force trauma (23.5%). This study has demonstrated that victims of homicide in an Australian population are more likely to have used methamphetamine than members of the general population. The reasons for this remain unclear although involvement in a drug selling environment may be an important determinant.
Introduction
Methamphetamine is an illegal stimulant drug that gives users a feeling of euphoria associated with a surge in central nervous system dopamine levels. 1 It may also cause irritability, confusion and paranoia, and is associated with violent behaviour. For example, it has been reported that 50–73% of cases of violent and aggressive behaviour encountered by law enforcement agencies in the United States involve methamphetamine abuse. 2 In addition, methamphetamine may prevent fatigue and enhance performance, characteristics which led to German soldiers during the Blitzkrieg of WWII being supplied with 35 million tablets. It was also used by Allied and Japanese troops in that war.3,4
Methamphetamine is also associated with unnatural deaths, with increased rates of accidents (in particular vehicle crashes), suicides and homicides.5–7 In fact, it is the only drug that has been strongly linked to homicide, even compared to cocaine, alcohol, lysergic acid diethylamide (LSD), phenylcyclidine and heroin, 1 with estimates that users of methamphetamine have a nine times increased risk of committing a homicide. 8 Despite these known associations, there is limited literature on the incidence of methamphetamine use in a specific population subset, the victims of homicide. Therefore, the following study was undertaken to determine the incidence of methamphetamine use among homicide victims.
Materials and methods
100 randomly selected de-identified homicide cases from 2012 to 2021 were accessed from the Forensic Science SA (FSSA) Pathology Database. The records were reviewed and the age and sex of the victims were recorded along with the month/year of death, type of homicide and presence or absence of methamphetamine in the blood (with levels). Other drugs were recorded but not analysed as the focus of the study was purely on methamphetamine use. Cases with decomposition were excluded.
Results
A total of 76 males and 24 females were identified (M:F = 3:1). Of these, 30 victims (30%) had methamphetamine detected in blood, consisting of 26 males and 4 females (M:F = 6:1; male age range 18–53 years, average 36.8 years; female age range 28–63 years, average 44.8 years). Levels of methamphetamine ranged from 0.02 to 3.3 mg/L with an average of 0.64 mg/L. Number of cases with and without methamphetamine detection over the 10-year the study period is summarised in Figure 1. Categories of homicide with the presence or absence of methamphetamine are summarised in Table 1.
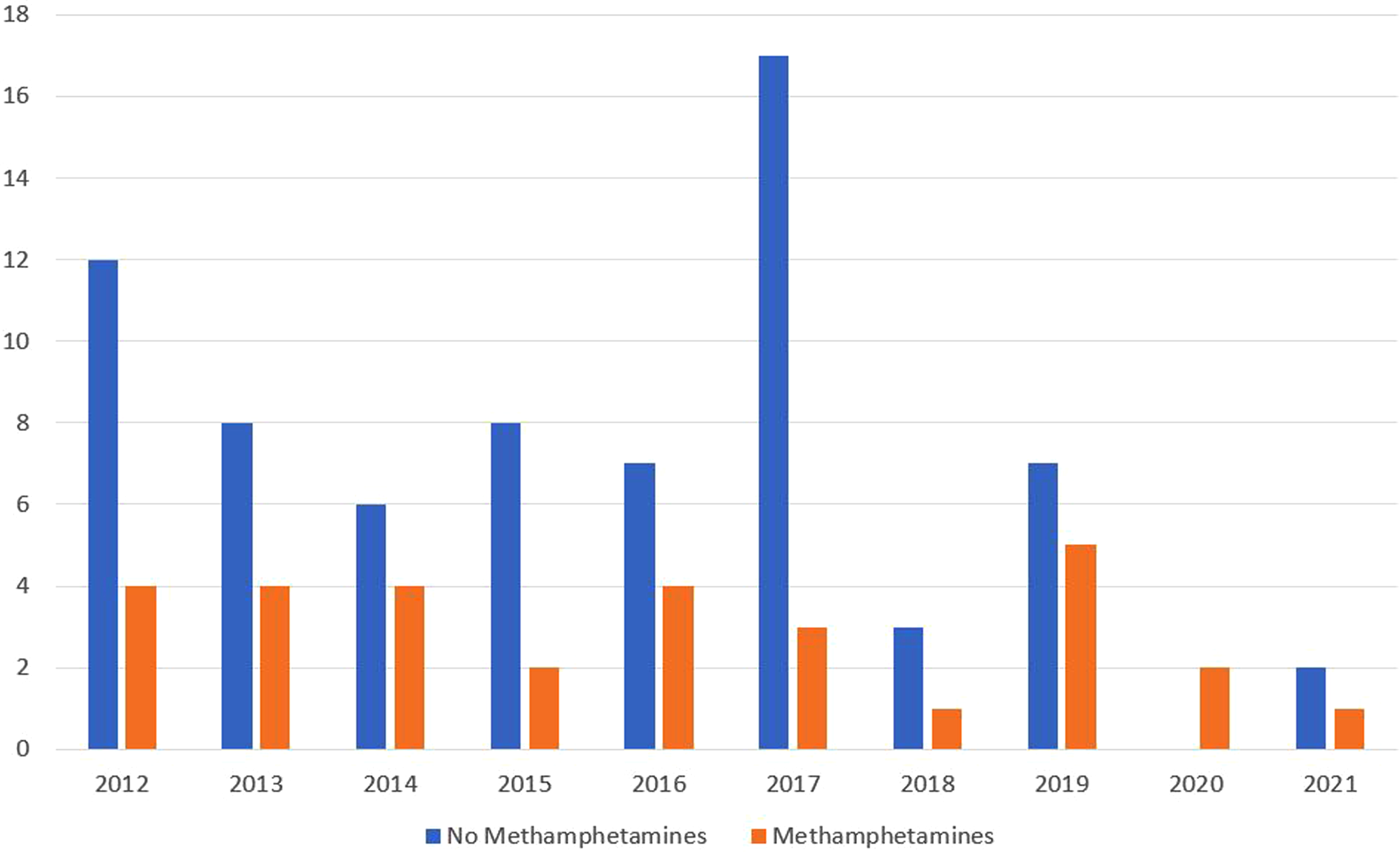
Incidence of methamphetamine detection in 100 homicide victims in South Australia over a 10-year period (2012–2021).
Numbers of homicide cases with the incidence of methamphetamine detection, by type of homicide.
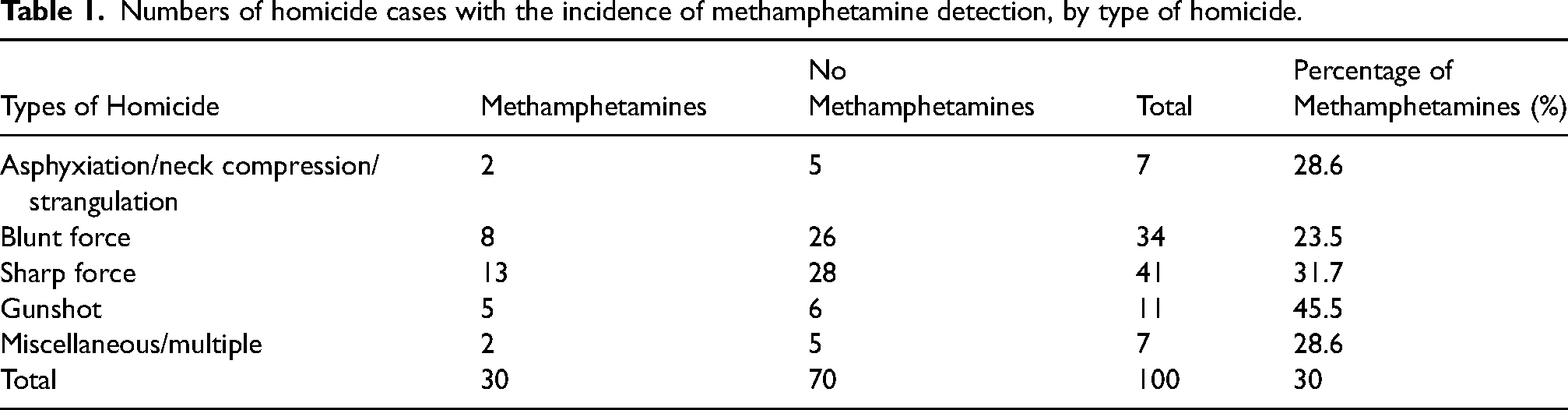
Discussion
Methamphetamine consumption is increasing in the Australian community accounting for 10% of all drug-related hospitalisations in 2019–2020, compared to 6.9% in 2015–2016. 9 There have also been changes in the demographic profile of methamphetamine users, with the mean age increasing significantly from an average of 32.6 years in 2000, to 42.2 years in 2019. Whether this reflects aging of people who use methamphetamine, increased use by older individuals, or increased detection due to greater drug screening in medicolegal cases is unclear. 10 Methamphetamine has also been detected in forensic autopsies in infants as young as one month of age, 11 and may be associated with exacerbation of underlying medical conditions such as cardiac disease and insulin-dependent diabetes mellitus.10,12
In the present study, 30% of victims of homicide had methamphetamine detected on toxicological screening of blood, which is significantly higher than in the general Australian population (30% vs 5.8%,
An Australian report on methamphetamine users showed that the majority (95%) had been victims of violence, often on multiple occasions, with 46% experiencing victimisation in the year preceding the study. 14 However, methamphetamine use was not found to be a significant risk factor for this; rather the main predictors of violent victimisation were the amount of alcohol used, the presence of antisocial behaviour and drug dealing, i.e., a major factor for being the victim of an assault was being involved in the illicit drug market. 14 Thus, although the reasons for the higher rate of methamphetamine use in the current study of victims of homicide are unclear, it may not be due to aberrant or aggressive behaviour by the victim that provoked an attack. Rather, it appears more likely given the findings from the earlier study, 14 that involvement in a drug taking/selling environment is a more significant contributing factor, posing a greater risk for lethal assault. This study has, however, demonstrated that many victims of homicide in an Australian population are likely to test positive for methamphetamine on postmortem toxicological screening.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
