Abstract
The College of Physicians of Madrid organized an open debate on conscientious objection (CO) in the medical profession on September 14, 2022. We summarize here the main arguments discussed. CO is defined as the right to raise exceptions to the performance of legal duties when they involve a contravention of personal convictions, whether religious, moral, or philosophical. It is not insubordination. Some authors contend that any decision by elected authorities should be uniformly followed by all citizens, physicians not being an exception. However, suppressing the ethical dimension of medical care may have an unacceptable cost with harm to physicians, their patients, and ultimately society. Health professionals are not blind instruments or mere “executors.” The practice of medicine must follow the aim of the profession, namely the pursuit of the patient's good. Medical care must conform to medical ethics, which was first defined twenty-five centuries ago in the Hippocratic oath, and summarized with the triad of precepts “cure, relief, accompaniment.” Since then and particularly in light of the Nuremberg trials, most medical declarations have highlighted the duty of defending human life and the importance of CO. In modern societies, there may be medical services that are not health care, even if they are legal. Then, which comes first law or ethics? Ultimately, CO is the tool that protects the freedom of the physician to refuse to perform actions that go against the values of medical ethics. With respect to the recent Spanish laws on abortion, euthanasia, and sex re-assignment of minors, if administrators want to know who is available for a health service that raises issues of conformity to medical ethics, requesting a list of volunteers is preferable to producing an objector list. Asking for registration of conscientious objectors goes against the right to privacy and is coercive, intrusive, and abusive.
Introduction
The College of Physicians of Madrid organized an open debate on conscientious objection (CO) in the medical profession on September 14, 2022. The event was attended by more than 200 people. A short text in Spanish has recorded the major conclusions as an institutional position document (ICOMEM 2023). Herein, we report in more detail the main arguments discussed during the presentations and the final round table.
CO is defined as the right to raise objections to the performance of legal duties when they involve a contravention of personal convictions, whether religious, moral, or philosophical. It is not insubordination. The reason the citizen manifests his reluctance to follow a legal mandate must be supported by an important moral or religious argument. In other words, it is a request to be exempted from compliance with the law without intending to abolish it by providing reasonable explanations (Jones-Nosacek 2021).
Historical Perspective
A few historical testimonies may further clarify the approach to CO. Thomas Moore, Chancellor of Henry VIII, requested exemption from signing the Act of Royal Supremacy of the Anglican Church, because of his objection to the king's divorce and remarriage. For this, he was sentenced to prison in the Tower of London and beheaded in 1535 (Bolt 2013) Franz Jägerstätter, an Austrian, opposed taking up arms under the Nazi regime. He was sentenced to death in 1943 (Purtz 2009). A third and opposite case was that of Adolf Eichmann, better known as the “Butcher of Auschwitz.” He was one of those most responsible for the deaths of thousands of Jews in Nazi concentration camps. He fled to South America and resided under another name in Argentina for more than ten years. Mossad, the Israeli Secret Service, discovered and kidnapped him. He was transferred to Jerusalem, tried, and hanged in 1961. In his defense, he said that he was not a murderer; he only obeyed orders from his superiors. Taking words from Hannah Arendt considering the banality of evil, Eichmann “was not foolish, but thoughtless” (Bergen 2000).
Moore and Jägerstätter were Catholic, and they put the duty of conscience before the order of political leaders; there are many other historical figures that used CO to refuse unethical mandates (i.e., John Fisher opposed Henry VIII, Maximilian Kolbe confronted the Nazis, etc.).
By contrast, Eichmann excused himself as a person and became a bloodthirsty executioner. He defended himself saying that he just obeyed the law, claiming that the problem was the law instead of him.
The Nuremberg Trials
The trials against Nazis that followed the II World War confronted pivotal ethical considerations posited with regard to CO. The premise of the trials was that “obeying the law” was simply not enough to absolve the defendants of their moral responsibility to humanity. There is a higher standard than mere “law” (Ivy 1948). E.W. Lutzer in his book “Hitler's Cross” (Lutzer 2016) wrote: “…the moral landscape of a country is largely determined by its laws. When Hitler made the laws, Germany was molded into his own image … After Hitler was defeated, war crimes trials were held in Nuremberg to judge the guilt of Hitler's henchmen. But a dispute arose as to what laws should be used to try the accused. After all, Hitler's cronies argued, quite plausibly, that they had not broken any laws; their actions were carried out with the protection of their own legal system. They could not be accused of murder because personhood has been redefined to exclude Jews and other undesirables. These men were simply following the laws handed down by the courts of their day. As Eichmann protested before his execution, “I was simply following the laws of war and my flag.”
When a state is accountable to no one except itself, it assumes that whatever is legal is moral. The moral law is simply whatever the courts say it is. The dispute at Nuremberg was resolved when the US prosecutor Robert H. Jackson was forced to appeal to permanent values, to standards that transcended that of any particular society. He argued that “there was a ‘law above law’ that stood in judgment on the arbitrary opinions of men” (Jackson 1947).
The thrust of the Nuremberg trials was that the primacy of Natural Law supersedes a nation's temporal laws. Modern European Union, United Nations, etc., and humanitarian and political Western organizations frequently violate what they once had enshrined as a necessary requirement for ethical medicine: the duty (not merely the right) of CO.
The Hippocratic Oath and Medical Ethics Codes
Despite being ignored by many (Baumgarten and Flores 2018), it should be recalled that the Hippocratic Oath explicitly prohibits abortion and euthanasia. Almost all medical declarations in the wake of the Nuremberg trials universally acknowledged the importance of CO as well as the prohibition of abortion and euthanasia.
The Geneva Declaration of the World Medical Association states: “I will maintain the utmost respect for human life, from the time of its conception; even under threat, I will not use my medical knowledge contrary to the laws of humanity.” The explicit directive is that even if a physician is threatened with punishment, he must not violate what medical ethics mandates (World Medical Association 1948).
The British Medical Association likewise condemned abortion and euthanasia following the Nuremberg trials. The British Medical Association stated that “the greatest crime being cooperation in the destruction of life by murder, suicide and abortion” (BMJ 1947). The respect for human life at its earliest stages as espoused at the Nuremberg trials was incorporated into the foundational documents of the United Nations as well. However, it is clear the transforming view and shifts experienced about human rights and interventions in human life are acknowledged in more recent UN documents.
Democracy and CO
The three historical cases mentioned earlier in the article occurred under monarchies or dictatorships. Could they happen in democracies? In democratic societies, the rules agreed by the majority regulate the personal activity of citizens and what is lawful and what is not. However, civil laws change over time. Even democracies are not immune from manipulation. In many countries, the ability of the majority to impose a decision is only limited by an external rule of law, much like a morality sense. Recognizing the importance of the rule of law and the protection of minorities from the majority is a critical consideration in democracy.
Laws, no matter how sovereign the chambers that approve them are, must fit certain principles which, by pure logic, must be extra-legal. Law is an epiphenomenon of something that predates it: morality and ethics (Gracia 2012).
In a perfect society, ethics and laws should coincide. In Roman law, the “natural” right is expressed as the “positive” right. The doctrine of “human rights” was established in 1948, after the tremendous experience of the II World War. Any positive right is legitimate not by the mere fact of being considered legal but by a law's adherence to and respect for human rights.
CO in Medicine
None of the protagonists of the three examples cited earlier in the article were doctors. Is there anything special about CO in medicine? Being a doctor and rendering medical care have a particular consideration because of their purpose: the patient's health. In fact, until recently, most doctors graduated after reading the Hippocratic Oath, a symbolic act that emphasized and reinforced his ultimate professional duty.
What does one do when there is a conflict between civil law and the medical code of ethics? Sometimes there may be a contradiction between the duty to provide a service (civil authority) and the duty to follow one's conscience (medical duty) (Alexander 1949, 1973): contraception, sterilization, abortion, and assisted reproduction that conflict with the beginning of life; sex reassignments, and euthanasia and assisted suicide, to mention a few (Table 1).
Medical scenarios for consciencious objection.

Some authors contend that any decision by authorities elected democratically should include physicians with respect to medical procedures permitted by civil law (Savulescu 2006, Schuklenk and Smalling 2017). Suppressing what it means to be a doctor and the dimensions of medical care may have an unacceptable cost, causing harm to physicians, to their patients, and ultimately to society. Health professionals cannot be viewed as mere “executors” of patients' wishes or those of healthcare administrators (Symons 2023).
Unlike other disciplines, where there are only two actors (the administration and the citizen), in medicine three actors come into play (Figure 1). The first is the health system that dictates policies in line with laws enacted by the civil authorities. The second is the doctor, who exercises his profession in accordance with both the medical ethics code and the rule of law (Symons 2022). The third is the patient, who is increasingly enjoying autonomy in decisions regarding his health, with restrictions on the ability to decide only when the rights of others are compromised. In the time course of the last forty years, the emphasis has shifted more on the primacy of the “Health care system” over the “Physician” relative to the patient (Berwick 2023).
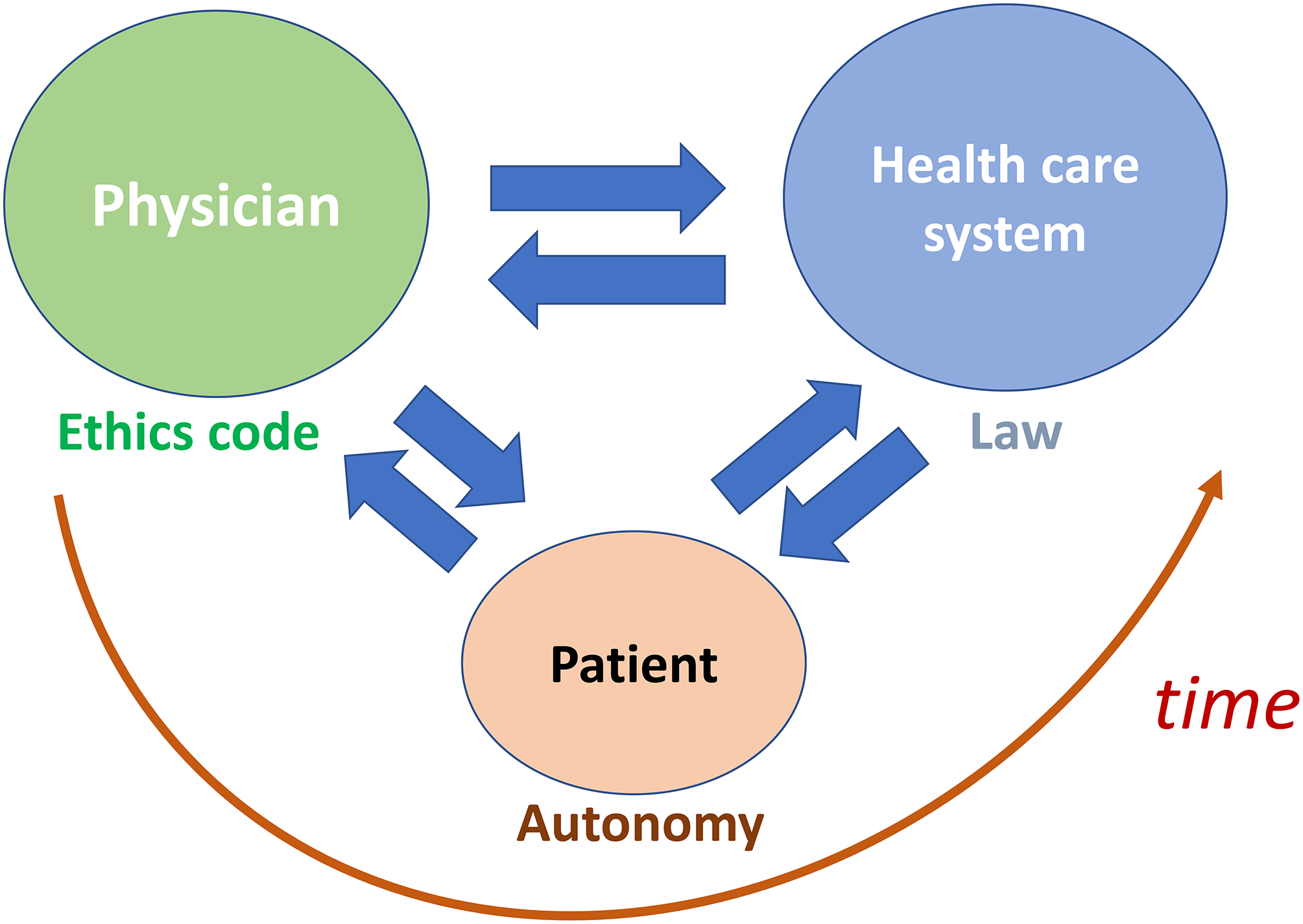
Main players and interactions in health care.
The performances of the three actors must be aligned. The doctor cannot be forced to perform a medical intervention that is contrary to medical ethics (Lopez-Guzman 2022). Otherwise, the conscience of the doctor would be violated and he would be degraded to be a blind instrument, a mere executor of decisions made by others rather than a contributing participant in care (Symons 2023).
The definitions of medicine and medical care shed light on the dimensions of the health profession. The word medicine comes from the Latin “mederi” (to cure). It is the science that aims at the prevention, diagnosis, prognosis, and treatment of diseases and health problems in humans. The WHO defines “health” as that state of complete physical, mental, and social well-being. These definitions reflect well the Hippocratic principles of the doctor's commitment to his patient: seek the cure; if not possible, relieve; and always accompany.
The comprehensive definition of health by WHO was abused by defenders of abortion seeking in the 1970s to expand ending a pregnancy until the time of birth if it harmed the “health” of the mother. Essentially, they permitted abortion at any time, claiming excuses for mental and/or social well-being. By doing so, the first right to life of the new human being was violated.
It is noteworthy that the original meaning of the definition of WHO “health” has been revived. Interestingly, VanderWeele and his colleagues at Harvard have highlighted that the complete picture of well-being lies in several areas, and seeking to do good is a major contributor to “human flourishing” (WanderWeele 2017). In the case of abortion, for example, the harmful mental consequences for the mother that voluntarily ends a pregnancy should not be discounted by the doctors in charge (Wanderweele 2023). Both are important for well-being.
The virtues of the physician were described by Edmund Pellegrino (1920–2013) (Pellegrino 2001). The search for the good of the patient (beneficence) and compassion, among others, are virtues that escape civil law. Ultimately, it is the intention of the physician that inculcates these values in his actions. For Christians and Catholics, the full dimension of medical practice is enriched by a sense of vocation for helping and healing (Pellegrino and Thomasma 1997).
To refrain from abuses appealing too much to CO, it has been said that it should be about serious matters. What is more important for patients than one's own health? If the doctor in charge is committed to providing his best care and the intervention chosen differs from the one demanded by the patient, after reasonable open discussions, one option must prevail over the other. If a patient's request is considered potentially harmful by the physician, resorting to CO is the only way for him to avoid inflicting damage while still respecting the patient's autonomy (Symons 2023).
Medical care is not a simple commodity. Article 36 of the recently published Spanish Code of Medical Ethics (Organización Médica Colegial 2022) states this clearly. Patients are entitled to much more than just any health intervention. The commitment of the physician is to the care of the patient. The doctor is not just the executor of the health service (Figure 2). In this way, the true medical act must be lawful, technically possible, and beneficial to his patient in the judgment of the physician (Gamble 2022). Ultimately, the “Physician” bears more ethical weight than the “Health Care System” relative to the patient. Hence, when democracies enact temporal civil laws that are against the code of medical ethics, physicians are not obligated by these mandates without personal responsibility.
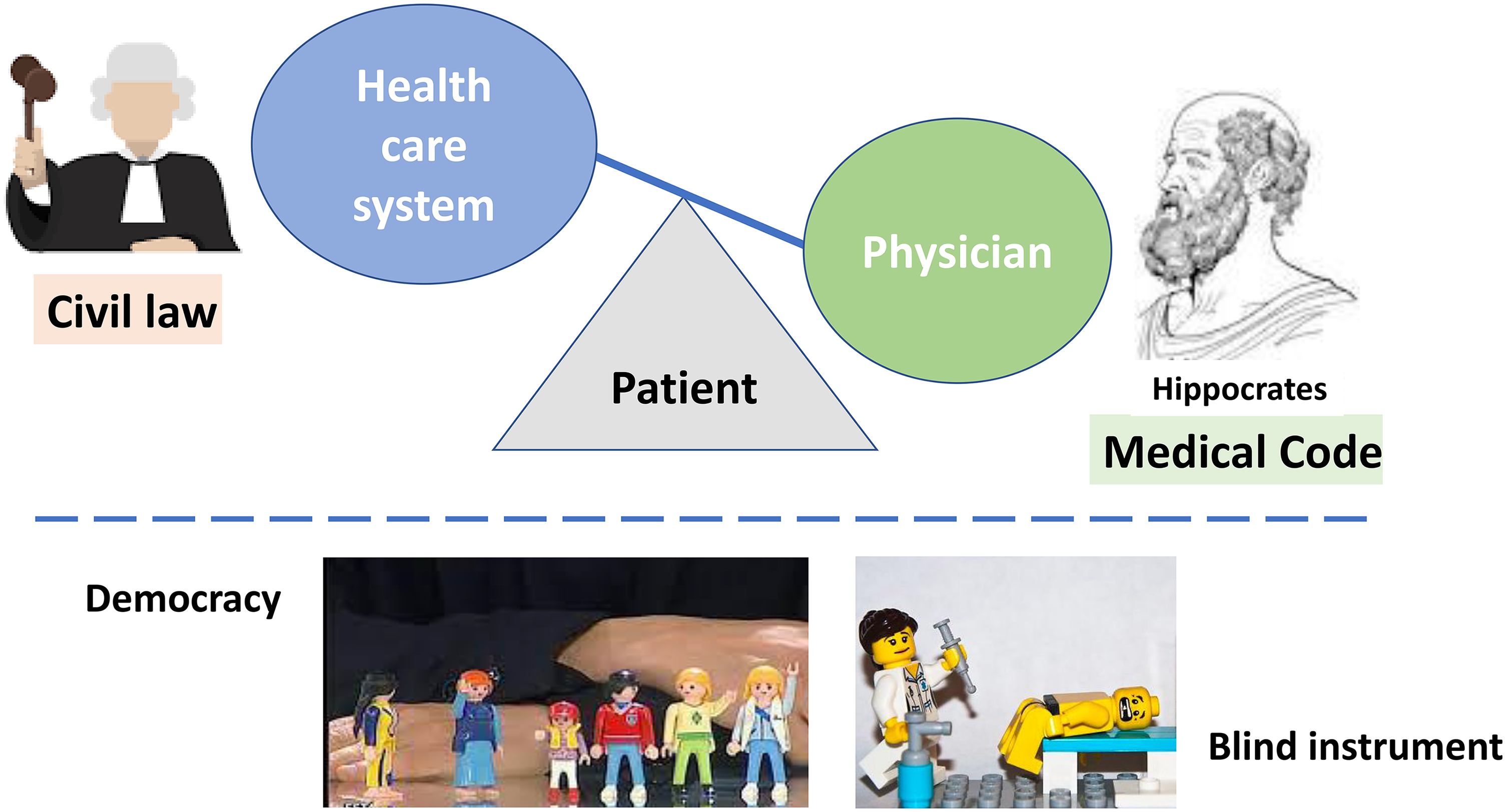
Conscientious objection–First the law or ethics? Transforming medical care into a democratic commodity.
CO by Health Care Professionals in Spain
CO is recorded as a fundamental right in Article 16 of the Spanish Constitution (Gobierno de España 1978). Accordingly, recent laws regulating abortion (Gobierno de España 2022a), euthanasia (Gobierno de España 2021), and sex re-assignation of minors (Gobierno de España 2022b) have acknowledged the access to CO, certainly with ambiguity. Furthermore, some autonomous regions have enacted laws on abortion, euthanasia, sex re-assignation of minors, care management for LGTB patients, and others that contravene CO or restrict physicians and other healthcare workers from asserting to CO. Two examples are recorded below.
In the case ARCOPOLI vs ELISABETH (TSJM 2021), a 2019 sanction to a psychotherapist, named Elisabeth, was reversed. Briefly, in her clinic, Elisabeth attended a young woman who claimed to be lesbian. She decided to provide psychotherapy as a first intervention. Thereafter, ARCOPOLI, an LGBT collective, accused Elisabeth of administering conversion therapy for homosexuality. Based on a regional law 13153/2016 of the Autonomous Community of Madrid (BOCAM 2016), she was sanctioned based on the provision that “to promote and carry out aversion or conversion therapies with the purpose of modifying the sexual orientation or gender identity of a person. For the commission of this offence, the consent given by the person undergoing such therapies shall be irrelevant.” Elisabeth, to whom the patient went freely at first, determined after interview and clinical assessment, that this patient would benefit from psychotherapy rather than other interventions trying to reinforce orientation and behavior according to her biological sex. In this case, Elisabeth expressed her CO to the LGTBIfobia law of Madrid, refusing to perform interventions that she considered harmful to her patient. She was first convicted but the Regional Supreme Court thereafter overturned the sentence.
In the case Herrera vs Junta Andalucía (TC 2015), a 2011 sanction to a pharmacist was reversed. The pharmacist Joaquín Herrera had not dispensed morning-after pills to a customer of his pharmacy in 2008. The pharmacist was sanctioned for not having a product considered essential in law 22/2007, applicable to Andalusian pharmacies. The pharmacist expressed his CO to abortion, claiming that levonorgestrel in the pill is an abortion medication. The regional government of Andalusia relied on the 2001 resolution of the case “Pichon & Sajous vs France” of the European Court of Human Rights. In such a case, the two pharmacists were convicted. The Spanish Court finally accepted the CO right of the pharmacist and he was not punished.
Ethics and Law
Conscience is a faculty of human moral psychology: the set of principles of human action that identifies us and guides our behavior. Conscience does not provide intuitive moral knowledge but rather a sense of having a moral obligation, a duty. Acting in conscience presupposes coherence between our thoughts and actions. Recognition of CO derives from recognizing the moral significance of conscience and the harm that comes from violating it (Symons 2023). Either we do what we think, or we will end up alienated, without identity, enslaved by our evil deeds.
Respect for conscience is a premise in the exercise of the medical profession because the actions that medical doctors perform are not impersonal processes. On the contrary, they are events and decisions of great personal significance. “Burnout” in patient care tasks has a lot to do with this, contributing to a large extent to potentially harmful experiences that violate moral values or beliefs. Moral damage and its relationship to the risk of physician burnout or even anxiety and depression have been assessed by a recent meta-analysis (Williamson et al. 2018).
Regarding the new euthanasia law of the Spanish government, the Spanish Bioethics Committee has made itself clear (Comité de Bioética de España 2022): the fundamental rights of the minority cannot be in the hands of the majority, which can change over time. CO is not an anomaly in a democratic system but protects against imposition and normative abuse. CO is a fundamental right, which derives from the ideological and religious freedom of Article 16 of the Spanish Constitution (Gobierno de España 1978). No law may require an individual to document CO in advance and in writing.
The doctor's opposition to a law that contravenes one's conscience begins with the objection for an individual case (and without registration); continues with dialogue with the patient/colleague; and ends with making his stance known to the responsible administration. Early registration of objectors—as proposed by the law for euthanasia approved by the current Spanish government (Gobierno de España 2021)—cannot be required because part of the physician's responsibility depends on addressing individual cases.
The American Medical Association's (AMA) Code of Medical Ethics explicitly refers to the scenario of a law that could force actions that a physician considers ethically unacceptable. “If doctors think a law violates ethical values or is unfair, they have an obligation to try to change it … In exceptional cases, ethical responsibility will be above the legal obligation” (AMA 2001). In other words, professional civil disobedience should be the response of physicians to an unethical law that intrudes on the medical profession. In some instances, such as in the sex re-assignation of minors, it is clear there is a risk of ideology prevailing over science (Hruz 2020). Sadly, it is interesting to see how some authors have manipulated the disobedience principle arguing against the Dobbs sentence (Wynia 2022). It is surprising as well that some leading medical journals have taken part in openly supporting such ideological positions (Baumgartner 2019).
The recent declaration of the World Medical Association acknowledges that CO has become the most critical issue nowadays (Parsa-Parsi 2022), as patient's autonomy and the rights of minorities are increasingly confronting the freedom of medical professionals to do what they consider best for their patients (Pellegrino, 2001).
The Collegiate Medical Organization (OMC) and the Ilustre Colegio Oficial de Médicos de Madrid. (ICOMEM) states that CO’s consideration of the new Spanish laws on euthanasia, abortion, and sex re-assignation of minors depict an unprecedented novelty in legal regulations (ICOMEM 2021, 2022, 2023). The interference with CO is unnecessary, coercive, and violates confidentiality. In order to ensure the provision of health services that go against the medical code of ethics, it is only up to the administration to request a list of available and trained personnel for this practice.
Conclusions
The practice of medicine must first follow the aim of the profession, that is, the pursuit of the patient's health. Medical care must conform to the medical code of ethics, comprising the triad of precepts “cure, relief, accompaniment.”
There may be health services that are not medical care, even if they are legal. Which comes first: law or ethics? CO is the tool that protects the freedom of the doctor to refuse to perform treatments that go against the values of medical ethics.
Is there an obligation to register as an objector, as proposed by the recent Spanish laws on euthanasia, abortion, or sex reassignment of minors? No. If administrators want to know who is available for a health service that is subject to CO, requesting a list of volunteers is preferable to mandating to produce a list of objectors. Asking for the registration of objectors goes against the right to privacy. It is coercive and intrusive and it is an abuse.
Footnotes
Acknowledgments
We would like to thank Prof. José Antonio Díez for critical reading and helpful comments on law issues.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Universidad Internacional de La Rioja (UNIR)—Citei (grant number project 005/23).
