Abstract
Melanomas are the most common cancer of the eye in canines, felines and humans. The treatment approaches vary, since no gold standard exists. Therefore, this systematic review aimed to compare the treatment modalities in ocular melanoma in rabbits. Medline/PubMed, Cochrane Library, Web of Science and Embase were searched for articles published until 21 April 2021 in English, Portuguese or Spanish, reporting animal studies evaluating photodynamic therapy (PDT), laser, radiotherapy or surgical excision. Twenty-seven articles were included for the qualitative synthesis, with publication dates from 1970 to 2018. Of the selected studies, 19 used PDT, six used radiotherapy and two used laser as treatment. No studies regarding surgical therapy that met the inclusion criteria were obtained. The tumour therapy results were evaluated in a heterogeneous manner for different periods and various methods, including microscopy, angiographic, histological examination, fundoscopy, ultrasound exam and electroretinogram. The treatment modalities analysed successfully treated the ocular melanoma, with tumour necrosis being commonly observed. Despite the therapeutic efficacy shown, side effects have been reported for all the therapies. The studies showed high heterogeneity, and therefore, in the future, new studies should be carried out to increase knowledge about ocular melanoma treatment. The analysed therapies can be used successfully in the treatment of ocular melanoma, with more conservative options such as PDT presenting great potential.
Introduction
Melanomas are both the most common ocular neoplasia of melanocytic origin and the most common malignant primary intraocular tumours in canine,1,2 feline2,3 and human species. 4 Although the vast majority of ocular melanomas originate from the uvea, they may also occur on the eyelids, on the conjunctival surface, along the limbus or within the uveal tract.1,5 These tumours often show unclear limits regarding surrounding tissues, with frequent destruction of the implantation site 6 and metastatic capacity,5,7 with a significant impact on vision, comfort and longevity of companion animals. 2
Diagnosis is usually made on routine eye examination due to unspecific clinical manifestations. 8 The treatment options for ocular melanocytic neoplasia are determined by the species affected, tumour location, rate of progression and extent, as well as by the expertise and facilities available to the veterinary clinician.5,9,10 Treatment can be performed with surgery, lasers, photodynamic therapy (PDT), radiotherapy, alone or combined regimens. Chemotherapy can be used in the case of disseminated disease. Importantly, there is no gold-standard therapy, and ocular melanomas present a varied rate of response to treatment. 8
Besides its importance in veterinary medicine, eye melanoma treatments in animals are often used as models for human therapies. Animal models used in ocular melanoma research include mice, rats, rabbits, chick embryos, drosophila and zebrafish.11,12 With a key advantage over the other species employed, rabbits have larger eyes, making them favourable for the procedures and ophthalmic exams. 11 These models play an important role in cancer research, assisting in the understanding of neoplastic behaviour in vivo, as well as possible therapies,11,12 able to demonstrate efficacy and safety before clinical trials. 12
Since no gold-standard therapy exists in the treatment of eye melanoma in animals, evaluating the available therapies is of the utmost importance for veterinary guidance and to support future human research. 9 This work aimed to perform a systematic review of the literature with a qualitative comparison of the results to answer the following problem, intervention, comparison and outcome (PICO) question: ‘Which eye melanoma therapy is most effective in rabbits?’ (Table 1).
Problem, intervention, comparison and outcome (PICO) question.

Methods
This systematic review report followed the Preferred Reporting Items for Systematic Reviews (PRISMA) guidelines. 13 The PRISMA checklist is available as Supplemental Material. The review protocol is registered in Prospective International Registry of Systematic Reviews (PROSPERO) under number CRD42019146667.
Search strategy
The following databases were searched for relevant studies: MEDLINE (through PubMed), Embase, Cochrane Library and Web of Science. The initial search was conducted on 14 June 2020, and the last search was completed on 19 April 2021. The search strategy for the different databases is shown in Table 2. For all databases, the following filter was applied: articles written in English, Portuguese or Spanish. No temporal limits were applied. Two authors (T.G. and C.M.M.) independently evaluated the studies by title and abstract and selected those that met the inclusion criteria. A third reviewer (M.L.) was consulted wherever there were doubts about a study’s eligibility, and a decision was reached by consensus.
Search strategy in databases.

Inclusion and exclusion criteria
This systematic review’s inclusion criteria were: (a) studies in which the main objective was to evaluate the treatment for ocular melanoma, (b) orthotopic implantation of tumour cells in rabbit’s eyes and (c) therapeutic modalities that included PDT, laser, radiotherapy and surgery/microsurgery. Studies that did not meet the following criteria were excluded: (a) studies in which the sample included other animals or humans; (b) studies that used other forms of therapy; (c) studies reporting combined therapies; (d) heterotopic models; (e) induction of tumours other than melanoma; (f) studies in animals without tumours; (g) reviews, book chapters and conference summaries; and (h) studies that did not evaluate the therapeutic effect on ocular melanomas.
Data extraction
References (PubMed/MEDLINE and Web of Science) were managed by EndNote Web Referral Manager software (EndNote®X7; Thomson Reuters, Philadelphia, PA), and duplicate references were removed. Duplicate references from the Embase and Cochrane Library databases were handled and removed manually. For studies that met the inclusion criteria, the following information was collected: reference (author; year), animal model (strain; tumour origin; implantation site), description of treatment (initiation of treatment; type of therapy used; the form of administrations; treatment interval), clinical evaluation and histological/microscopy.
Quality assessment
The studies’ quality was evaluated by assessing the risk of bias using SYRCLE’s bias risk tool for animal studies by two independent authors (T.G. and K.C.). 14
Results
Figure 1 shows the PRISMA flow diagram of study selection, describing the process of identification, exclusion and inclusion. A total of 3058 studies were selected for analysis, with 2074 studies obtained from PubMed, 620 studies from Embase, 156 studies from Web of Science and 208 studies from Cochrane Library. Of these, 27 articles were included for the qualitative synthesis, with publication dates from 1970 to 2018. Of the selected studies, 19 used PDT as treatment,15–33 six used radiotherapy34–39 and two used laser.40,41 No studies with surgical therapy that met the inclusion criteria were obtained. The detailed information of the selected studies and results is presented in Table 3.
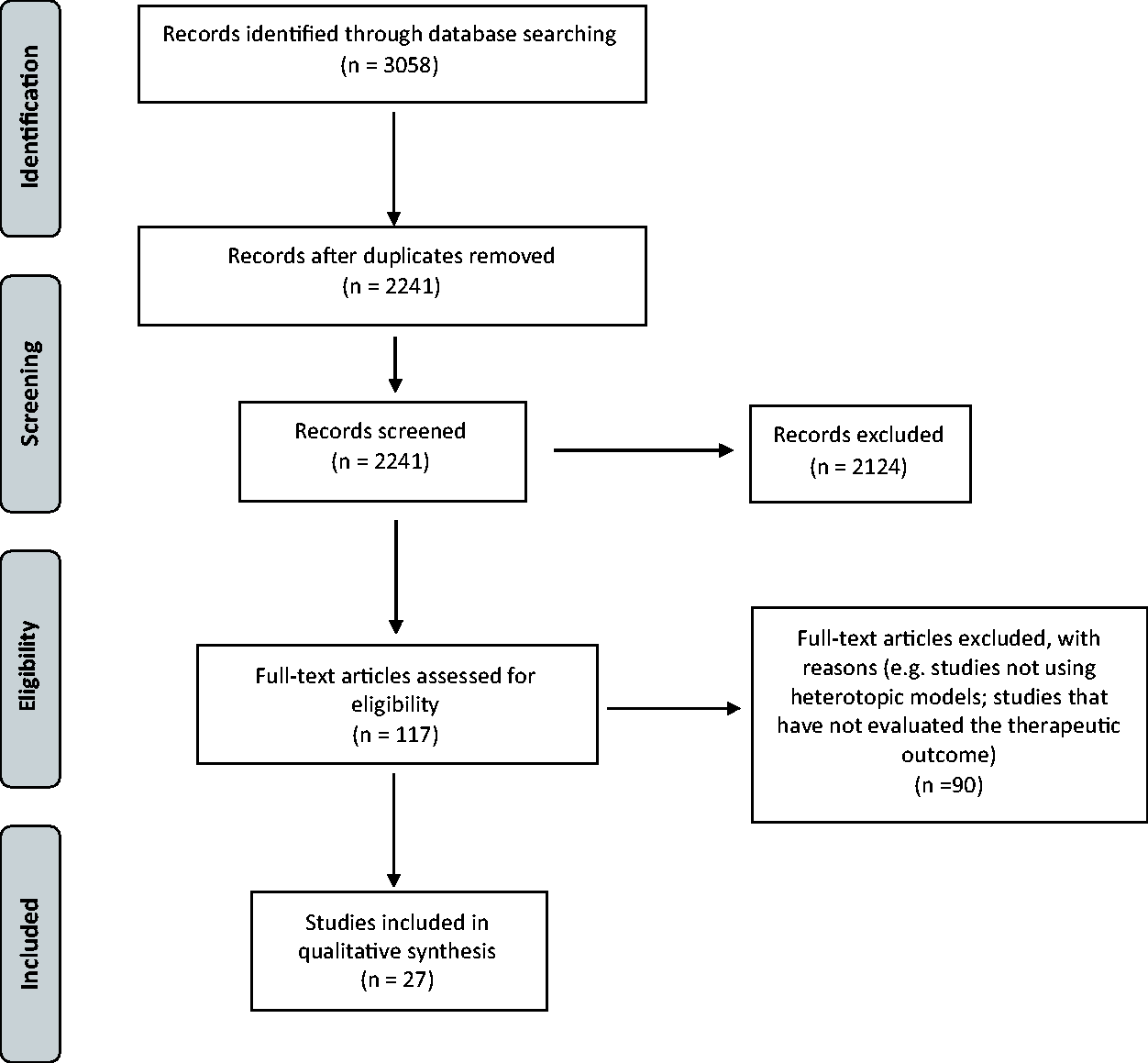
Preferred Reporting Items for Systematic Reviews (PRISMA) flow diagram of the studies selection.
Included studies details and results.

PDT: photodynamic therapy; PS: photosensitizer; AD: administration protocol; IV: intravenously; IR: irradiation; DLI: drug light interval; ST: strain; TO: tumour origin; IS: implantation site; TO: treatment onset; LT: laser type; RT: radiotherapy; NR: not reported; N: number.
Studies using PDT as a treatment have used Dutch Cross rabbits, Dutch rabbits, New Zealand albino rabbits, New Zealand white rabbits, Pigmented rabbits and chinchilla pigmented rabbits. New Zealand white rabbits, both albino and pigmented, were employed in studies with radiotherapy treatment, and New Zealand albino rabbits were used in laser studies. With regard to the origin of the tumours, murine melanoma (B16F10), Greene amelanotic hamster melanoma and human uveal melanoma (92.1MEL) were reported. Tumours were implanted in the anterior chamber, iris, subretinal space or subchoroidal space. Treatment initiation was performed within a range of 5–28 days after tumour implantation, with the tumours reaching a diameter range of 2.1–7 mm. The photosensitisers used in PDT, concentration, route of administration and activating light are shown in Table 3. The irradiation agents in radiotherapy studies and the lasers employed in laser therapy are also shown in Table 3.
Outcome of tumour therapy were evaluated by various methods, including biomicroscopy exams,17,20,21,24,26,27,30,31,33,40,41 angiographic examination15–19,21–24,26–28,31,33,40,41 histological examination,15–23,26–28,30,31,33,34,36,37,40,41 fundoscopy, 18,19,22,23,27,28,32–34,38–41 magnetic spectroscopy, 38 electron microscopy,24,29,35 ultrasound exam18,19,32,34,38,39 and electroretinogram.32,36 All treatments led to tumour inhibition.18,19,23,32 However, complete tumour destruction was not always achieved,15,17,22 with incomplete tumour necrosis 29 and tumour development in the periphery of the treated area.16,27 It was demonstrated absence of tumour growth after PDT, 31 occurring irreversible regression, 26 and tumour destruction.20,30 Until the time animals were killed to collect tissues, no tumour growth was observed. 33 No tumour cells were detected in the histological examination 21 and necrosis was present.15–24,26–33 Radiotherapy is effective, destroying melanoma. 36 Since the height of the tumour may influence its complete regression, 34 partial38,39 to total responses were observed at varying periods of days after treatment, 37 with necrosis areas of variable dimensions. 35 The energy used in laser therapy was related to therapeutic responses.40,41 Complete regression of tumours was achieved. 41 According to the laser dose, tumour necrosis was present, 41 and intact tumour cells were also found.40,41 Despite the therapeutic efficacy shown by the treatments, several side effects have been reported in different eye structures, depending on the therapy used, as described in Table 4. In terms of quality assessment, most of the studies included presented an unclear bias. The risk assessment for individual study bias is represented in Figure 2 and detailed in Supplemental Table S1.
Side effects observed after treatments.

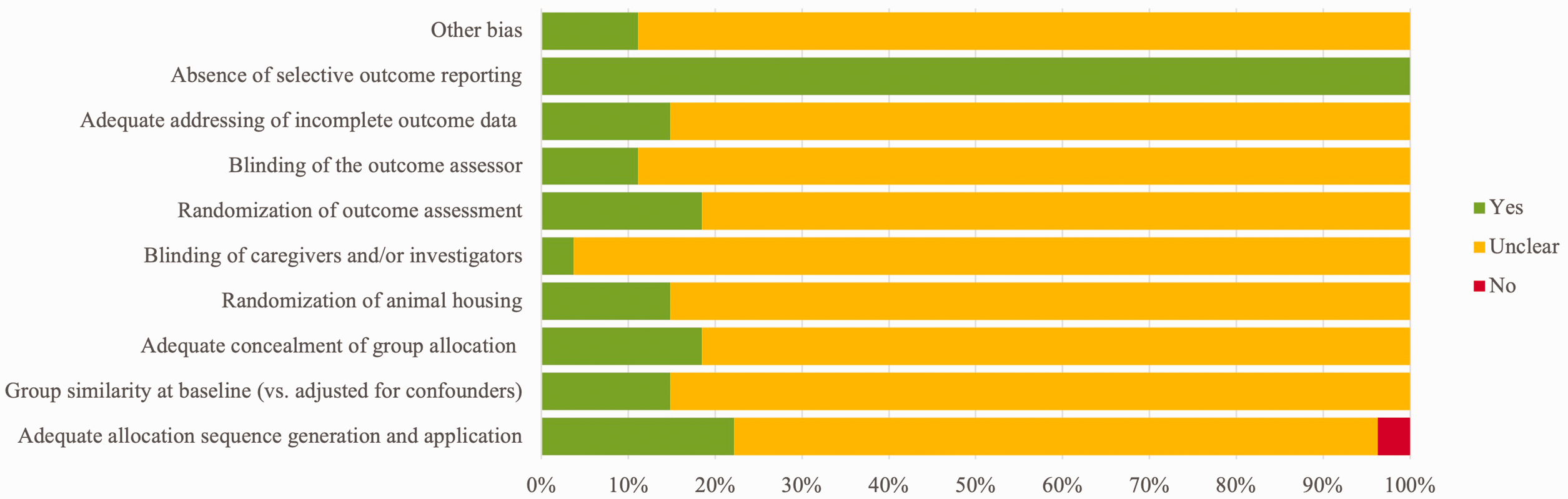
Summary of the quality assessment of the studies included in the systematic review.
Discussion
The present study’s objective was to evaluate the effectiveness of ocular melanoma treatment options in rabbits. The obtained results allow us to conclude that PDT, radiotherapy and lasers may be effective in eye melanoma. Nevertheless, complete remission was sometimes not achieved. For all treatments, the outcomes are dependent on the protocol intensity. Further studies should compare the best protocols for each treatment modality in a randomised controlled trial. A study of this nature will allow conclusions to be made over which option is the most effective.
Currently, the evidence available does not support one treatment as a gold standard for eye melanoma. Since this systematic review supports the efficacy of PDT, radiotherapy and lasers, the decision over which one to use should consider factors such as clinician preference and proficiency, financial constraints and patient health.42–44 Several animal models of ocular melanoma exist, and the decision as to which is the most appropriate is determined by factors such as cost, scientific principles, available data, the technique to be used and suitability of the model for the project. 45 For ophthalmic research, rabbits have the main advantage of larger eye size that allows for easier examination, retinal and choroidal assessment, background photography and surgical procedures, 11 as well as an accurate injection of cells in the posterior compartment and easy use of diagnostic techniques for follow-up. 46 Other advantages in choosing this species are the easy handling; short gestation, lactation and puberty cycles; the standardisation of the environment; the genetic standardisation; and the easy transplantation of tumours. Among the disadvantages are the need to live in an artificial environment, the need for a standardised diet and the execution of most experiments in animals with artificially induced diseases. 45
Rabbits are widely used in research, not only in the field of ophthalmic diseases but also in several other pathologies.47,48 The New Zealand white rabbit (albino) and American, Dutch and Californian rabbits are the most used breeds for research, representing both pigmented and albino animals. 49 Amelanotic Greene hamster melanoma cells were used in almost all revised studies, being used in 16 of the 19 PDT studies15–18,20,21,24–33 and in five of the six radiotherapy ones.34,35,37 Mus musculus melanoma cells (B16F10) were used in two PDT studies19,22 and in two laser studies.40,41 Human uveal melanoma (92.1MEL cells) were used in a PDT study. 23 One of the articles with radiotherapy classifies the cancer cells used as amelanotic epithelioid melanoma. 36 The preference for amelanotic Greene hamster melanoma cells is probably due to the success of establishing tumours in the eye, brain, testis, muscle and subcutaneous space. 50 They also grow faster after inoculation, and no immunosuppression is required in rabbits for the cells to grow. 11 Nevertheless, immunosuppression treatment was used in one study. 18
As stated, melanoma can affect any anatomical region in which melanocytes are present. 51 Ocular melanoma in dogs and cats often originate in the iris and the ciliary body, 2 and in humans, they commonly affect the choroid. 8 For the studies in this review, tumours were implanted in the iris,16–18,20,21,24–26,28,29,31anterior chamber,35–37 subretinal space 39 and subchoroidal space.15,19,22,23,27,30,32,33,38,40,41 The studies therefore represent the most common locations for ocular melanomas, for both animals and humans, making the results more comprehensive. As a suggestion for future studies, a more detailed description of the animal model used must be performed.
PDT is based on the selective retention of photosensitisers in malignant cells and the subsequent destruction of tumours by appropriate wavelength irradiation. 52 PDT largely depends on the properties of the photosensitising agent,53–55 generating photophysical and photochemical reactions, and exerting its outcomes by producing reactive oxygen species (ROS).56,57 ROS rapidly lead to significant toxicity in the target tissue microenvironment, resulting in tumour cell death by apoptosis, necrosis or autophagy. 57 Radiation exposure causes direct or indirect cellular stress due to the generation of ROS, DNA damage and damage to subcellular organelles. 58
Necrosis was the primary type of death observed after treatment.15,16,18,19,21–24,26,29,31,33,36,41 Death by necrosis caused by PDT can be accompanied by an inflammatory response, which can boost an anti-tumour immune response. 59 The results support that despite PDT not being the primary treatment option for ocular melanomas, it presents several advantages regarding the other therapies. It is the most conservative, since it has selectivity for tumour cells, and the light source can easily be applied to the eye. In the future, PDT should be assessed as a primary option for ocular melanoma treatment in animals and possibly in humans.
The included studies’ follow-up periods ranged from immediately18,19,29,40,41 to two years after treatment. 36 Since ocular melanoma can be recurrent,40,41 it will be of interest to present longer follow-ups to evaluate the long-term effects. Nevertheless, the immediate results allow the rapid effect of the treatments on tumour reduction to be verified.18,19,28,29,40,41
Inflammatory response and retinal detachment were the most common side effects, as shown in Table 4. Inflammatory response was common, contributing to tissue repair. Retinal detachment is expected, since most treatments are administered through the retina or in the proximity of this structure. Of importance, most of these complications were solved spontaneously, in a short period and without the need for additional treatment.15,18,19,26,27,32
One of the limitations observed was the heterogeneity between the studies due to different anatomical sites of the melanoma implantation, therapy intervals, time of exposure, energies and doses used, forms of evaluation, times of evaluation and times of follow-up. Also, differences exist between the numbers of studies included for each treatment, which means that the sample included in some groups is reduced, limiting the conclusions obtained. The decision to perform a systematic review aimed to reduce the heterogeneity among studies using defined inclusion and exclusion criteria, thus allowing more evidence-based conclusions. Regarding the inclusion and exclusion criteria, we opted to include all the options currently available in veterinary clinics. Additionally, PDT was included because it is a therapy with promising results that has been underused, despite the availability of commercial photosensitisers. Experimental therapies were excluded because they are not available to be used in the clinics and their efficacy is not fully established. We also decided to exclude combination studies, since they do not allow each therapy effect to be distinguished, and that would compromise the answer to the PICO question.
The present systematic review aimed to compare the available treatment modalities for ocular melanoma in rabbits. We conclude that all of the analysed therapies can be successfully used in ocular melanoma treatment, since they proved to be effective, even more conservative approaches such as PDT. Despite the therapeutic success, all modalities presented side effects, with PDT being the safest therapeutic option. The studies presented high heterogeneity. In the future, new studies should be performed to increase our knowledge of ocular treatment options.
Supplemental Material
sj-pdf-1-lan-10.1177_00236772211039333 - Supplemental material for Evaluation of eye melanoma treatments in rabbits: A systematic review
Supplemental material, sj-pdf-1-lan-10.1177_00236772211039333 for Evaluation of eye melanoma treatments in rabbits: A systematic review by Tarcísio Guerra Guimarães, Carlos Miguel Marto, Karla Menezes Cardoso, Nuno Alexandre, Maria Filomena Botelho and Mafalda Laranjo in Laboratory Animals
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This work was supported by the Foundation for Science and Technology (FCT), Portugal, through a PhD fellowship awarded to Tarcísio G. Guimarães (SFRH/BD/139319/2018). CIBB is funded by National Funds via FCT (Foundation for Science and Technology) through the Strategic Projects UID/NEU/04539/2019, UIDB/04539/2020, UIDP/04539/2020, and by COMPETE-FEDER (POCI-01-0145-FEDER-007440).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
