Abstract
RESEARCH PROBLEM & DATA
Is structural sexism associated with preventive health care use among women and men? If so, are the patterns more consistent with theories of gender norms and health behaviors or gendered power and resource allocation?
Receiving preventive health care can decrease the risk of illness and death, yet many U.S. adults do not receive the recommended preventive care procedures. This study examines state-level structural sexism as one factor potentially influencing the use of preventive care. Structural sexism is a measure of systematic gender inequality in power and resources in a given U.S. state. We argue that it likely impacts preventive health care use by influencing how individuals perform gender in their care-seeking behaviors (Figure 1a) or by affecting access to resources based on the gendered decisions of state political actors (Figure 1b).
Using data from the 2018 Behavioral Risk Factor Surveillance System, we estimate a series of gender-stratified multilevel models with individuals nested in states. The health care outcomes include dichotomous measures of whether or not individuals had received preventive care services, including cancer screenings, flu vaccinations, tests for sexually transmitted diseases, and clinician visits. The predictor of interest is a state-level measure of structural sexism, which is a composite score of inequality between men and women in political, economic, cultural, and physical/reproductive domains of society. Data for this measure were drawn from various administrative sources.
KEY FINDINGS
We find that overall, both men and women use less preventive health care in states with higher levels of structural sexism (Figure 2).
In general, these findings support the gender performance theory for men, because men are less likely to seek care in a context encouraging traditional masculine traits, and the gendered power and resource allocation theory for both men and women, because states in which women are less empowered are less likely to have health-promoting policies for all.
One finding does not follow this pattern: Men are more likely to test for prostate cancer in states with more structural sexism (Figure 2).
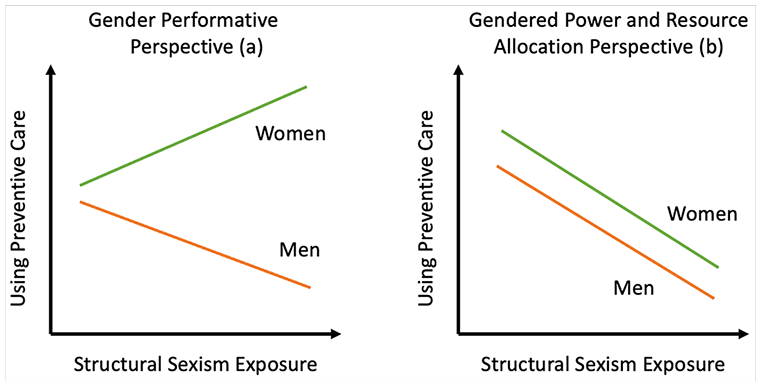
Potential Relationships between Structural Sexism and Preventive Care Use Based on Gender Theories
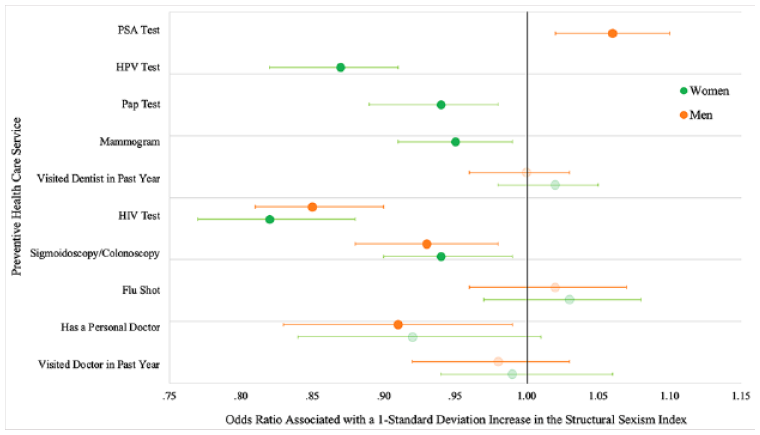
Associations between Structural Sexism and Odds of Using Preventive Health Care Services among Women and Men
POLICY IMPLICATIONS
This study identifies an important relationship between state-level structural sexism and preventive health care. Our findings suggest that policymakers can strive to increase preventive care use by targeting harmful gender norms and increasing access to health-promoting resources. For example, policies that encourage men to embrace the traditionally feminine task of care taking, such as paid parental leave, may reshape gendered expectations, thereby altering masculine behaviors like avoiding care. In addition, policymakers should embrace policies that decrease barriers to preventive care. Expanding Medicaid in all states would increase access to health insurance and health care. Policies can also tackle logistical challenges of receiving care by providing affordable childcare and accessible public transportation. By addressing underlying reasons for insufficient use of care, the United States can decrease preventable illness and death.
