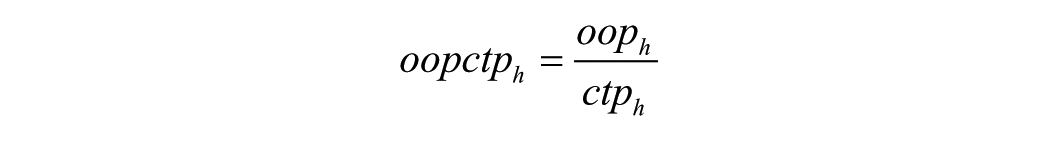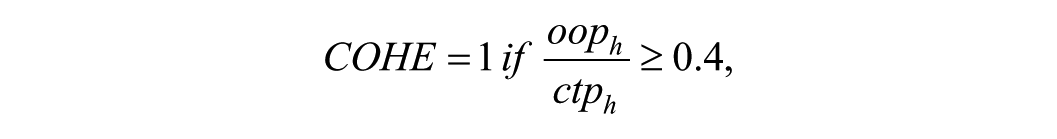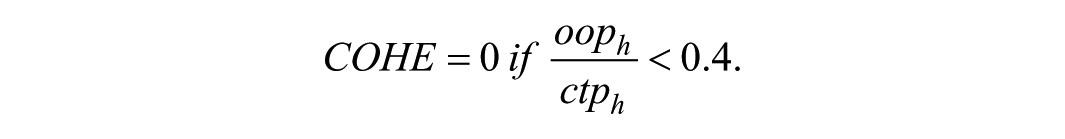Abstract
Access to affordable oral health care is central to achieving universal health coverage. While out-of-pocket expenditures can pose particular challenges for older population groups, little is known about catastrophic oral health expenditures (COHE) among people aged ≥50 y. The present study aimed to identify the extent and variation of COHE for persons aged ≥50 y from 12 European countries, for which dental expenditure data were available from the seventh wave of the Survey of Health, Ageing and Retirement in Europe. Specifically, information from 77,261 persons was included in the analysis. According to World Health Organization definitions, COHEs were calculated as out-of-pocket dental spendings exceeding 40% of the net total household expenditure on basic needs (ie, food, housing, and utilities). Descriptive and regression analyses were applied to test if COHEs at age ≥50 y differ across countries or regions and do not vary by demographic characteristics (age, gender, education, marital status, household size). On average across countries, >2.27% of study participants were identified to have COHE, with the highest observed population proportion of COHE in Spain (10.95%) and the lowest in Sweden (0.12%). Older age was associated with a significantly higher likelihood of experiencing COHE: the risk of people aged ≥70 y (2.6%) was significantly higher than for people aged 50 to 60 y (1.7%). There was a significant difference in COHE between males (1.7%) and females (2.6%). This study is the first to identify the extent and differences in COHE among people aged ≥50 y in European countries. Out-of-pocket oral health expenditures detrimentally affect older adults, with unequitable variations by gender, age, and country/region of residence. These findings are pivotal for policy makers to inform strategies to achieve equity in access to affordable oral health care.
Keywords
Introduction
The World Health Organization (WHO; 2022, 2023) emphasizes the critical need to ensure equitable access to quality oral health care without causing financial hardship. Out-of-pocket (OOP) payments, a widespread mechanism for financing oral health care, are known to create financial barriers across health systems in low-, middle-, and high-income countries (Bernabé et al 2017; Thomson et al 2023). The WHO Oral Health Action Plan highlights the importance of addressing catastrophic oral health expenditure (COHE) in the context of universal health coverage (WHO 2010; WHO 2024). COHE represents the financial burden that households face when OOP payments for oral health care surpass a certain percentage of disposable income, potentially leading to impoverishment (United Nations 2020). Populations aged ≥50 y face unique oral health and financial challenges. As people tend to keep more teeth into older age and more innovative treatment technologies become available, the complexity of care continues to increase (Kassebaum et al 2017). Multimorbidity due to aging-related systemic conditions (eg, diabetes mellitus, cardiovascular disease) complicates oral health care and may increase treatment costs (WHO 2024). The transition into retirement often results in reduced disposable income, heightening vulnerability to OOP expenditure shocks (Organisation for Economic Co-operation and Development 2018; Thomson et al 2019). Hence, dedicated attention to financial protection in oral health care for adults aged ≥50 y is justified.
As highlighted by Proaño et al (2024), significant evidence gaps persist regarding the financial hardship associated with oral health care. The review underscores methodological inconsistencies in defining financial hardship and a lack of understanding of the contextual determinants, such as variations in oral health systems and socioeconomic factors. Proaño et al (2024) emphasized that COHE is underresearched among older populations and highlighted major knowledge gaps, underscoring the relevance of this study. COHE might pose particular threats to older population groups, as the burden and complexity of oral diseases increase with age and retirement can lead to lower disposable income to cover OOP payments. Major knowledge gaps exist for the extent and determinants of COHE in older age.
Oral health plays a crucial role in overall well-being, influencing people’s ability to speak, eat, and socialize without discomfort (WHO 2024). However, reliance on OOP costs for oral health care poses significant challenges for individuals with limited disposable income (Watt et al 2019). Income disparities often determine access to dental care, as procedures not fully covered by insurance are less likely to be utilized by lower-income or uninsured individuals (Anikeeva et al 2013; Murakami et al 2014). Consequently, poorer households are more likely to seek emergency rather than preventive care (Listl 2011; Gambhir 2015). This approach not only increases avoidable suffering but also leads to higher treatment costs, exacerbating unmet oral health needs and overall financial burdens (Manski et al 2017; WHO 2023). Monitoring and evaluating COHE is critical for guiding evidence-informed policy making (OECD 2018; WHO 2024).
Against this background, the present study aimed to examine the extent and determinants of COHE among adults aged 50 y and older across 27 European countries and Israel. We hypothesize that 1) COHE does significantly vary across countries and 2) sociodemographic characteristics, such as age, gender, education, urban residence, marital status, and household size, do not significantly influence COHE risk.
Methods
Data Source
This study utilized data from the Survey of Health, Ageing and Retirement in Europe (SHARE), which is a cross-national database covering 27 European countries and Israel, containing information on health, socioeconomic status, and social and family networks of >140,000 individuals ≥50 y old (Börsch-Supan et al 2005). The study focused on wave 7 of the SHARE data, collected between 2017 and 2018, as participants in this wave were asked about their dental expenses. Statistically analyzable data on dental OOP expenditures were available for a subset of countries, and our analysis was therefore limited to the following 12 countries: Austria, Belgium, Czech Republic, Switzerland, Germany, Denmark, Spain, France, Greece, Italy, Poland, and Sweden. The remaining countries could not be included in the analysis due to the unavailability of dental expenditure data.
Conceptualization and Parametrization of Catastrophic Health Expenditures
A capacity-to-pay approach was applied to determine COHE (Thomson et al 2019). This method posits that households must allocate a minimum amount toward essential expenses such as food and housing. The denominator is calculated by subtracting the amount spent on basic necessities from the total household consumption, which was defined according to the composite household expenditure variable provided by SHARE. This approach is consistent with WHO Europe (2019) recommendations for assessing financial protection based on household consumption. Moreover, consumption is generally considered a more stable and accurate indicator of a household’s living standards than income, particularly among older or retired individuals (Meyer and Sullivan 2003). Basic needs expenditure was calculated as the sum of 3 components as available from the SHARE gv_imputations dataset: amount spent on food at home, amount spent on food outside the home, and rent and home-related expenditures. This operationalization reflects essential subsistence expenses and broadly aligns with the categories for food, housing, and utilities per the Classification of Individual Consumption according to Purpose. For the capacity-to-pay approach, the threshold was fixed to total household consumption minus the amount allocated to basic needs, resulting in a varying effective threshold across households. This study adopted the WHO’s normative spending approach for food, housing, and utilities. The denominator was calculated by subtracting the standard amount for subsistence spending on food, rent, and utilities from total household consumption (WHO Europe 2019). The basic needs used to determine the capacity to pay for health care were defined as the average spending on food, rent, and utilities per person within the 25th to 35th percentile of total consumption per person. The threshold used to identify COHE was set at 40%. This leads to an increase in COHE with increasing household consumption. Consequently, COHE is more prevalent among the poor rather than the rich, and households facing financial hardship can be identified by spending smaller OOP amounts. The calculations were based on the recommendations of a 2005 WHO report (Xu et al 2005).
Subsistence spending refers to the minimum amount of money that a household needs to spend on necessities such as food and housing. This type of spending is used as a baseline in determining the capacity of a household to pay for health care. In this study, the WHO’s normative spending approach (WHO and World Bank 2017) on food, housing, and utilities was used to define subsistence spending. The denominator was calculated as the total household consumption minus the average spending on food, rent, and utilities for the 25th to 35th percentile of total consumption per person. This approach allows for the identification of households that are experiencing financial hardship after spending relatively smaller OOP amounts on health care (WHO and World Bank 2017; Cylus et al 2018). The impact of health payments is defined as OOP expenditure expressed as percentage of a household’s capacity to pay. In this study, OOP payment is exclusively limited to expenditures related to dental care. Household capacity to pay refers to the financial ability to pay for health care and other expenses (WHO 2019). This concept is often chosen to determine catastrophic expenditures, where a household is considered to have incurred such expenditure if the amount spent on oral health care exceeds a certain percentual proportion of total household consumption. The capacity-to-pay approach considers the household’s minimum spending on basic needs such as housing and food and calculates the household’s capacity to pay for health care by subtracting this amount from the total household consumption. This approach shows that the financial ability of households to pay for health care can vary by their individual economic situations and that households with lower income and consumption are more likely to experience financial hardship as a result of health care spending (WHO and World Bank 2017; Cylus et al 2018). Households with zero or negative capacity to pay were excluded from the analysis to prevent distortion of the COHE estimates:
where ctp = capacity to pay and h = household.
Catastrophic expenditures occur when the household’s total OOP expenditure equals or exceeds the threshold of 40% of a household’s capacity to pay. COHE refers to excessive OOP payment on oral health care that results in financial hardship for a household (WHO Europe 2019). The threshold of 40% of household capacity to pay was adopted following WHO Europe (2019) recommendations, reflecting a validated level of financial burden significant enough to compromise access to other essential needs.
Spending a large proportion of one’s income on oral health care can lead to difficulties in meeting other basic needs such as food and housing. COHE is used as a benchmark for the financial burden of health care and can help identify households at risk of financial hardship as a result of their OOP costs. The concept of COHE is often calculated by the capacity-to-pay approach, which takes into account the household’s minimum spending on basic needs and calculates its capacity to pay for health care based on its remaining income or consumption (WHO Europe 2019):
Statistical Approach
Binary logistic regression analysis was employed to test our hypotheses, as stated in the Introduction. The significance level was set at alpha = 0.05, meaning that any effects with P values <0.05 were considered significant. Variables were deemed significant predictors if one category had significantly higher coefficients than any other. Missing values were replaced by imputed values from the SHARE gv_imputations dataset, which draws on multiple imputation techniques to facilitate more comprehensive analyses. Full documentation of these procedures is available via SHARE-ERIC (2024). We ran logistic regression models for nations and regions, with the binary variable COHE (yes/no) serving as the dependent variable and regions and countries as the independent variables. Linear and quadratic terms for age were included as covariates to allow for capturing nonlinear relationships between age and COHE, with use of the I() function in R to facilitate interpretation of the coefficients. Area of residence in SHARE wave 7 was categorized by respondents’ self-reported living environment based on standardized options: “big city,” “suburbs or outskirts of a big city,” “large town,” “small town or village,” and “rural area or home in the countryside.” These response categories are aligned with the standards of Eurostat and the European Union Statistics on Income and Living Conditions to ensure international comparability (Börsch-Supan et al 2013). Although the classification is based on participants’ subjective assessment, the harmonization with Eurostat definitions supports consistency across countries and facilitates cross-national analyses.
As part of the sensitivity analysis, we applied a 25% threshold to identify households experiencing particularly high financial burden from dental care. While the WHO typically recommends thresholds of 10% to 15% for general health care, the 25% cutoff has been adopted in prior research on financial protection in Europe. In line with a previous analysis on financial protection in Europe, which describes a 25% budget share threshold as a conservative lower-bound estimate of catastrophic health expenditure (Cylus et al 2018; WHO Europe 2019), we included this cutoff in our sensitivity analysis. Lower thresholds would be expected to capture a broader range of affected households (see Appendix Table 4 for details). Further methodological details are provided in the Appendix.
The reporting of this study follows recommendations of the STROBE checklist.
Results
Table 1 and the Figure show descriptive statistics for COHE by country sociodemographic characteristics. On aggregate across countries, the population proportion of COHE was 2.27%. The largest proportion was found in Spain (10.95%), while the lowest proportion was observed in Sweden (0.12%). Statistical tests were conducted to determine significance. Residing in a small town was associated with the lowest risk for COHE (0,8%), whereas living in the suburbs (1.3%), a large town (1.0%), a rural area (1.4%), or a big city (2.5%) showed higher risks.
COHEs by Sociodemographic Characteristics.
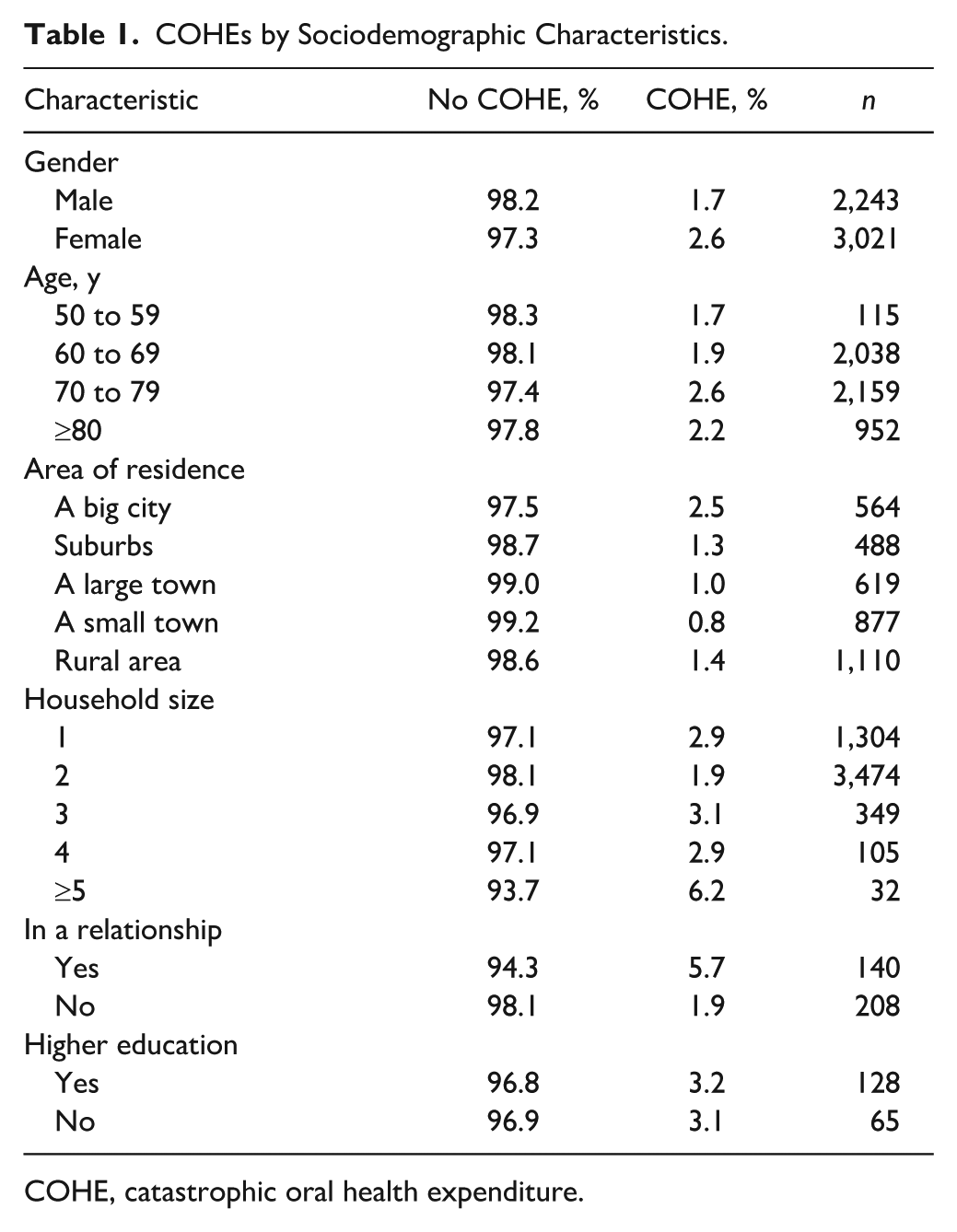
COHE, catastrophic oral health expenditure.
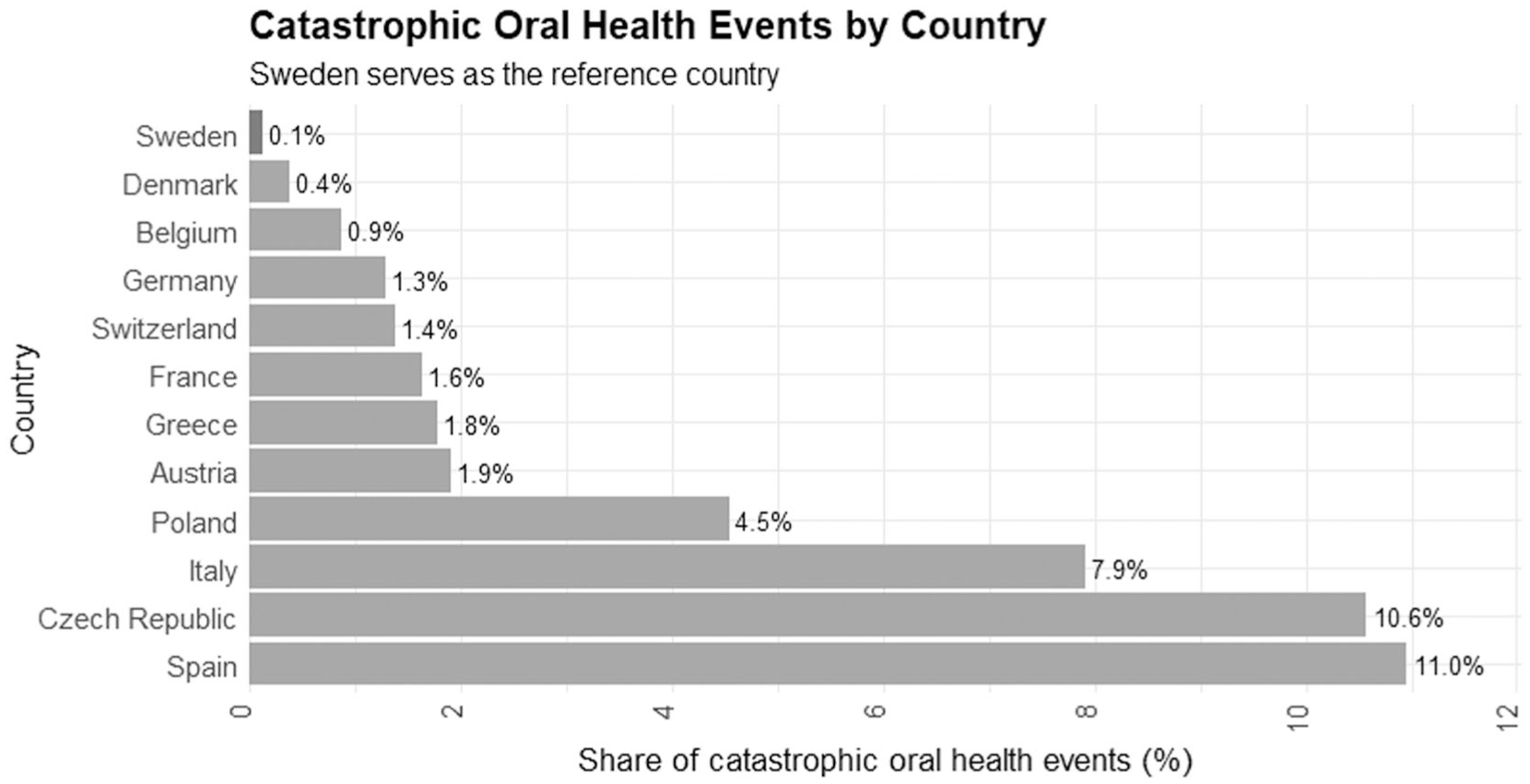
Results for countries. Catastrophic oral health events are ranked from highest to lowest by country. Spain shows the highest share of catastrophic oral health events and Sweden the lowest.
The Figure and Table 2 illustrate cross-country differences in the extent of COHE.
Logistic Regression Results to Test Cross-country Differences in COHE.
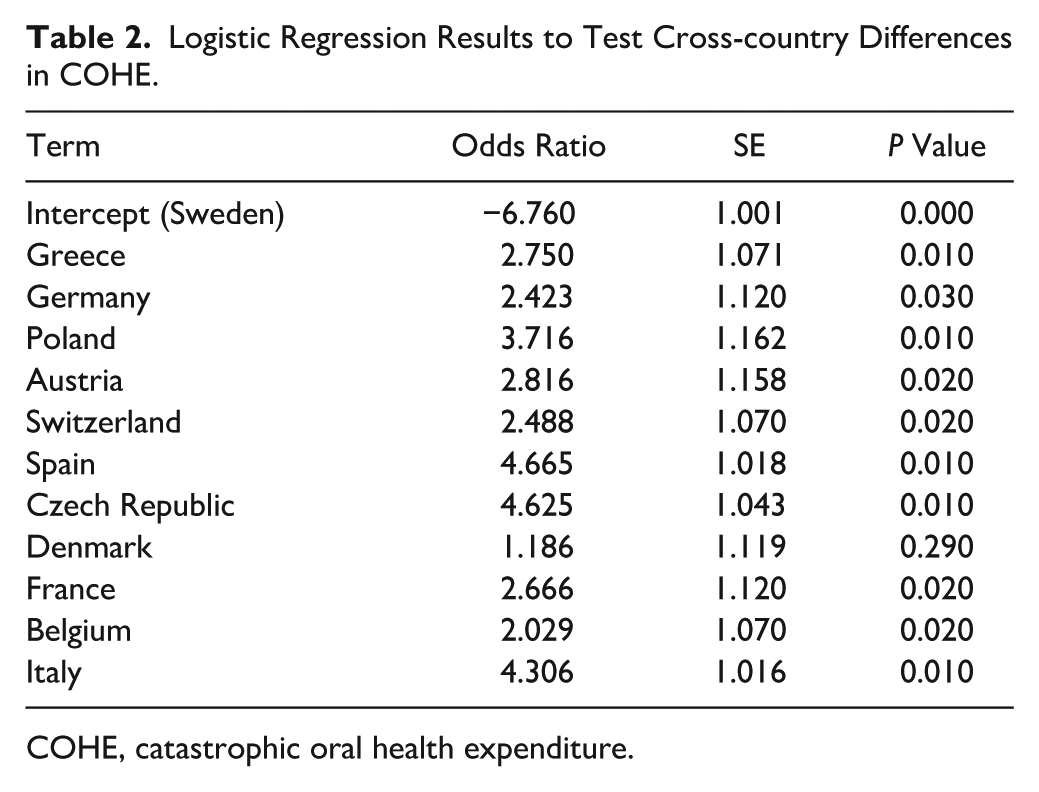
COHE, catastrophic oral health expenditure.
Table 3 shows the results from regression analysis of sociodemographic characteristics on COHEs. A significant relationship was found between age and COHE (P = 0.02), with the age group of 70 to 79 y being associated with increased COHE risk. The regression results confirm a significant nonlinear relationship between age and COHE, with the predicted probability peaking at 74 y of age. Significantly higher risks for COHE were identified for females (P = 0.030). Household size was not a significant predictor for COHE. No significant COHE difference was found for various household sizes. A higher level of education was linked to a reduced risk; however, this effect was not significant (P = 0.76). There was no significant association between living in a partnership and the prevalence of COHE.
Logistic Regression of Sociodemographic Characteristics on Catastrophic Oral Health Expenditures.
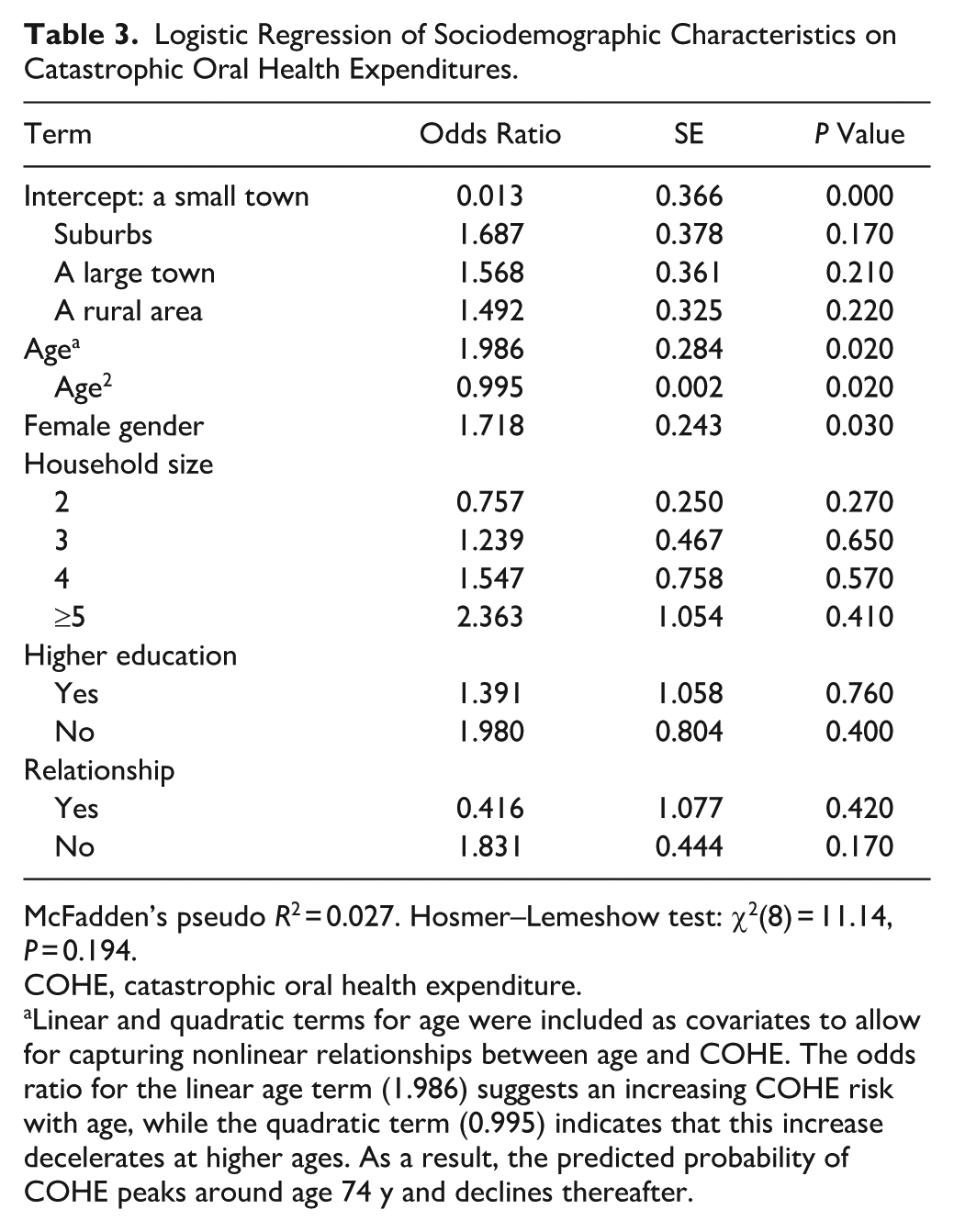
McFadden’s pseudo R2 = 0.027. Hosmer–Lemeshow test: χ2(8) = 11.14, P = 0.194.
COHE, catastrophic oral health expenditure.
Linear and quadratic terms for age were included as covariates to allow for capturing nonlinear relationships between age and COHE. The odds ratio for the linear age term (1.986) suggests an increasing COHE risk with age, while the quadratic term (0.995) indicates that this increase decelerates at higher ages. As a result, the predicted probability of COHE peaks around age 74 y and declines thereafter.
Application of the budget share approach yielded similar results (see Appendix Table 4).
Discussion
This study provides unique and novel empirical evidence on the extent of COHE among Europeans aged ≥50 y across 12 countries, highlighting vulnerable subgroups and significant cross-country disparities. Significant cross-country differences were identified, with population proportions of COHE ranging between 10.95% in Spain and 0.12% in Sweden. The likelihood of COHE was significantly higher in people aged 70 to 79 y (vs 50 to 60 and ≥80 y) and in females. COHE did not differ significantly by area of residence, education, household size, or relationship status. The substantial financial burden imposed by OOP expenditure remains a critical barrier to achieving equitable oral health outcomes in Europe. The data presented here reveal profound inequities, with low-income groups disproportionately affected by COHE. These findings underline the need to integrate dental financial protection into broader UHC strategies, systematically monitor oral health–related financial hardship, and design targeted interventions to protect high-risk older populations.
This study adds relevantly to the extant literature. Previous literature suggests that younger adults are generally less likely to experience COHE, primarily due to relatively stable income and insurance arrangements and comparably low treatment complexity (Olaisen and Manski 2024). Our finding that COHE risk increases with age supports the notion that the financial vulnerability of the population aged ≥50 y is structurally distinct from that of younger cohorts. Older adults might face increased treatment complexity due to greater retention of natural teeth, multimorbidity, and limited financial resources postretirement. This underscores the need for age-sensitive policy responses and targeted financial protection mechanisms within oral health systems. Our study further highlights cross-country differences in COHE, offering insights into the potential role of public insurance coverage in influencing such disparities. For example, Spain’s reliance on predominantly private dental services, with limited public subsidization, contrasts with Sweden’s broader insurance coverage for essential dental care (Henschke et al 2023), likely contributing to the higher observed COHE in Spain. However, in line with previous research, the present study also challenges the assumption that public dental coverage alone explains cross-country differences (Manski et al 2016; Winkelmann et al 2022). For instance, Denmark had a lower level of COHE than Germany, despite Germany having more generous public dental coverage. This suggests that other factors, such as cultural, behavioral, or systemic differences, may play a role. Higher COHE among rural residents may stem from limited dental provider availability, higher associated travel costs, and reliance on urgent rather than preventive care services (Walt et al 2008). By and large, these findings align with existing literature and stress the complexity of disentangling the precise context-specific mechanisms through which COHEs are shaped.
Our findings highlight the importance of tailored, context-specific strategies to reduce financial barriers and ensure equitable dental care. Variability in dental coverage across countries compounds these challenges, with some systems relying heavily on public or private insurance, while others shift the financial burden onto individuals. Such disparities can lead to unequal access, particularly for low-income populations and those in underserved areas (Northridge et al 2020). Policy makers should prioritize raising awareness about the importance of prevention-focused oral health care, particularly for underserved populations (National Institute of Dental and Craniofacial Research 2021). Strategies such as subsidies, tax credits, or direct financial support could alleviate treatment costs in rural and underprivileged areas while reducing the burden of advanced disease treatment and emergency dental care (Health Systems in Transition 2022). Integrated approaches that enhance access, balance costs, and promote prevention-oriented care are critical to reducing household financial burdens and achieving sustainable global oral health outcomes (Wagstaff 2008). Future policy and research should routinely include COHE indicators in health system assessments and explore context-specific changes in public dental coverage.
Recent reforms in countries such as France, Ireland, and Estonia illustrate ongoing policy-making dynamics in relation to public coverage for oral health care. France’s 100% Santé initiative eliminated copayments for some prosthetic procedures, and this led to increased denture utilization (Tubert-Jeannin et al 2025). Ireland’s Smile agus Sláinte policy aims to expand publicly funded schemes but faces challenges in ensuring sufficient workforce participation (Leavy et al 2025). Estonia has increased subsidies for older adults, people living with chronic conditions, and unemployed and lower-income groups (Laurimäe et al 2022). While long-term implications on catastrophic expenditures remain to be seen, such reforms illustrate ongoing policy dynamics with intentions to achieve UHC for oral health in European countries. Targeted strategies such as subsidies, better reimbursements, and mobile dental services can reduce OOP costs and improve access. Models such as Scotland’s Childsmile program, although designed for children, illustrate the potential of population-wide programs and could be adapted to older adults.
The present study is not without limitations. Given the previous dearth of COHE information for older population groups, the focus of the present study was on COHE among Europeans aged ≥50 y. Note that this focus implies limited comparability with other studies reporting on general catastrophic expenditure that use total health spending as the numerator. While our estimates for Spain and Czechia appear high, they are consistent with the concentration of dental costs in population subgroups and reflect a narrower focus on OOP dental expenditures. Other studies using SHARE data (eg, Jürges and Stella 2019) report lower prevalence estimates, likely due to differences in spending definitions, threshold type, and sample composition. A distribution plot (Appendix Fig. A1) has been added to illustrate the skewed distribution of dental expenditure burdens across countries. Cumulative financial hardships arising from other medical domains were not captured in the present analysis. Note that this study accounts only for individuals who can afford dental care and are negatively affected by the expenses. People who cannot afford dental care are not reflected in this study. Another limitation is the reliance on existing SHARE data, which limits the identification of detailed mechanisms for COHE. Also note that SHARE is a broad multidisciplinary survey and does not include detailed clinical oral health measures, such as the number of decayed teeth. This restricts comparing COHE with clinically measured oral health needs. Furthermore, SHARE wave 7 does not distinguish OOP costs on various types of dental treatment such that more detailed analyses were not supported by the data. Consider also that different types of dental treatment might carry different recall biases. As SHARE data are self-reported, there is a potential for recall bias, which could affect the accuracy of our estimates (Börsch-Supan et al 2013). Notwithstanding, the present study provides hitherto unavailable information about COHE among older populations in Europe, and this is highly relevant to inform policy makers.
Conclusion
The findings of the present study demonstrate substantial variations in COHE across countries and by several sociodemographic characteristics. These findings substantiate the urgency for policy makers to enact substantial changes in oral health policy making for achieving UHC. The measurement of COHE should become a routine element of health systems monitoring. The current dynamics of the WHO Oral Health Action Plan provide unique opportunities for policy recalibration toward creating a health care landscape where OOP costs are no longer a deterrent to receiving essential oral health services.
Author Contributions
J. Markeli, S. Listl, contributed to conception and design, data acquisition, analysis, and interpretation, drafted and critically revised manuscript. All authors gave final approval and agreed to be accountable for all aspects of the work.
Supplemental Material
sj-docx-1-jdr-10.1177_00220345251391189 – Supplemental material for Catastrophic Oral Health Expenditures among Europeans Aged 50 y and Older
Supplemental material, sj-docx-1-jdr-10.1177_00220345251391189 for Catastrophic Oral Health Expenditures among Europeans Aged 50 y and Older by J. Markeli and S. Listl in Journal of Dental Research
Supplemental Material
sj-docx-2-jdr-10.1177_00220345251391189 – Supplemental material for Catastrophic Oral Health Expenditures among Europeans Aged 50 y and Older
Supplemental material, sj-docx-2-jdr-10.1177_00220345251391189 for Catastrophic Oral Health Expenditures among Europeans Aged 50 y and Older by J. Markeli and S. Listl in Journal of Dental Research
Footnotes
Acknowledgements
This study was performed by using the SHARE data collection, which has been primarily funded by the European Commission through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4-CT-2006-028812), and FP7 (SHARE-PREP: No. 211909, SHARE-LEAP: No. 227822, SHARE M4: No. 261982). Additional funding from the German Ministry of Education and Research, the Max Planck Society for the Advancement of Science, the US National Institute on Aging (U01_AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_04-064, HHSN271201300071C), and various national funding sources is gratefully acknowledged (see ![]() ).
).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: All authors were funded by their own institutions to perform all work relating to the present study.
A supplemental appendix to this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.